In the Clinic
Optical imaging can be used in a variety of applications in clinical practice to aid diagnosis and treatment of diseases across a wide array of medical disciplines, including cardiology, gastroenterology, oncology and ophthalmology. Optical techniques can provide clinicians and surgeons with real-time morphological and physiological information in health and disease. In fact, optical imaging has a broad range of uses in diagnostic medicine, from screening and health monitoring to applications during surgery or treatment.
One of the most common optical devices in clinical practice is the endoscope, which is used to examine an organ or cavity. Endoscopy is widely used in gastroenterology for the diagnosis and monitoring of a number of gastrointestinal diseases, including colorectal cancer, coeliac disease and inflammatory bowel disease (IBD) — a chronic inflammatory condition of the gastrointestinal tract with two main clinical entities, Crohn’s disease and ulcerative colitis. When it comes to gastrointestinal disease ‘seeing is believing’ and endoscopy remains a cornerstone of the management of patients with these conditions. Endoscopic devices are used to confirm pathologies along the entire gastrointestinal tract, one prime example of its use is for the diagnosis and monitoring of patients with IBD. As noted in the Nature Outlook on IBD, published in December 2016, it can be a debilitating condition and the disease incidence continues to increase. As discussed in a Review by Walsh et al., patients with IBD undergo endoscopic assessments throughout their disease course, from the initial diagnosis to monitoring disease activity and severity (including monitoring for signs of colorectal cancer, which patients with IBD have an increased risk of). Moreover, mucosal healing, as determined by endoscopy, has emerged as an important treatment goal and clinical trial end point in IBD.
Endoscopy is evolving and, as noted by Joshi & Wang, confocal laser endomicroscopy enables high-resolution imaging of the gastrointestinal tract, collecting histology-like images that provide an instantaneous ‘optical biopsy’. Increasingly, advanced endoscopes are multifunctional, enabling multimodal imaging or indeed combining bioelectronics and therapeutic approaches (Lee et al). A further step forward in the evolution of endoscopic screening is to combine molecular imaging using fluorescent probes with standard endoscopy. This integrated approach has particular promise for the early detection of neoplasia, as described by Burggraaf et al. and a related commentary. 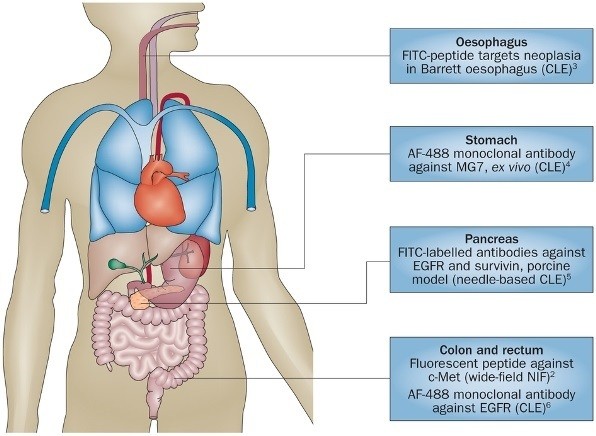
One medical specialty in which optical imaging has a key role in diagnosis and treatment is cardiology. Cardiac imaging utilises a variety of techniques, with an expanding role for photonics and combinations of optical techniques. 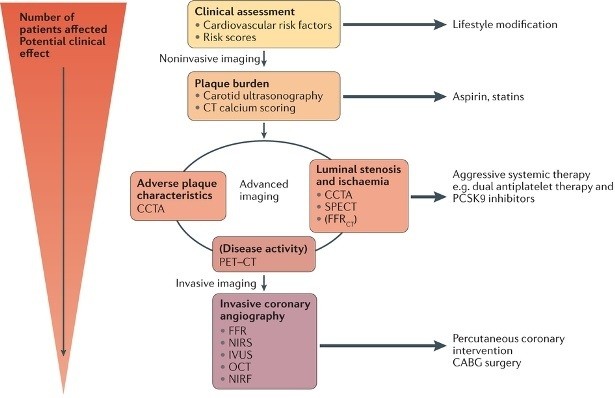
Atherosclerosis is a thickening and loss of elasticity of the arterial walls that is associated with the formation of atherosclerotic plaques, which can restrict the blood flow. Although atherosclerosis can be asymptomatic for many decades, it is considered a dynamic process, and when the condition progresses, it can lead to a number of serious cardiovascular diseases (CVDs) and outcomes, including coronary heart disease and heart attack. As such, optical techniques such as optical coherence tomography can be used for close monitoring of the progression and classification of atherosclerotic coronary plaques. As discussed in the Review by Dweck et al., optical diagnostics could help identify patients at high risk of CVD as well as guide clinical management to ultimately reduce the risk of serious cardiovascular events.
In addition to its diagnostical relevance, information gathered with optical techniques can also help guide the surgeon in their procedures. Minimally invasive surgery in fact would not be possible without the laparoscope, which typically comprises a light source to illuminate the operative field and a camera or digital device to relay images to the surgeon. Large incisions can be avoided with this approach, with laparoscopic surgery having many advantages over open surgery (including faster recovery time, reduced postoperative pain and bleeding, and reduced scarring) and being widely applied in urology, gastroenterology and gynaecology. For example, 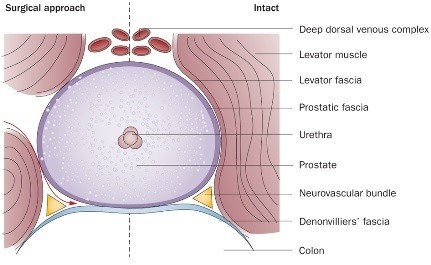 Fried and Burnett describe how novel optical technologies (including optical coherence tomography and spectroscopy) could be used to identify, map and preserve the carvernous nerves during radical prostatectomy in a bid to preserve erectile function after surgical removal of the prostate gland.
Fried and Burnett describe how novel optical technologies (including optical coherence tomography and spectroscopy) could be used to identify, map and preserve the carvernous nerves during radical prostatectomy in a bid to preserve erectile function after surgical removal of the prostate gland.

