Abstract
It is conceived that specific combinations of periodontal bacteria are associated with risk for the various forms of periodontitis. We hypothesized that such specificity is also related to human cause-specific death rates. We tested this hypothesis in a representative sample of the US population followed for a mean duration of 11 years and found that two specific patterns of 21 serum antibodies against periodontal bacteria were significantly associated with increased all-cause and/or diabetes-related mortalities. These data suggested that specific combinations of periodontal bacteria, even without inducing clinically significant periodontitis, may have a significant impact on human cause-specific death rates. Our findings implied that increased disease and mortality risk could be transmittable via the transfer of oral microbiota, and that developing personalized strategies and maintaining healthy oral microbiota beyond protection against periodontitis would be important to manage the risk.
Similar content being viewed by others
Introduction
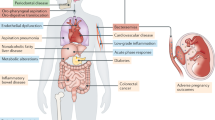
Mucosal surfaces, including the oral mucosa, are colonized by a complex and dynamic microbial ecosystem called “microbiota” that has important implications for human health and disease1,2. While more epidemiological evidence is warranted, periodontal microbiota has been identified as a causative agent of periodontitis, which is one of the most prevalent diseases in human population3,4. Interestingly, some animal and human observational evidence supports that periodontitis is not just an oral, in situ disease. The disease also contributes to several systemic diseases including diabetes and cardiovascular diseases (CVD)5,6,7,8,9. The chronic inflammatory processes of periodontitis are considered to be responsible for the etiologies10. In the oral cavity, the inflammatory and immunologic reactions following periodontitis induce the production of pro-inflammatory cytokines resulting in the breakdown of periodontal epithelium and connective tissues2,11. Systematically, the chronic trickling of periodontal microbiota into the systemic bloodstream elicits a systemic inflammation response resulting in elevated levels of various inflammatory mediators and cross-reactive systemic antibodies, which promote risk for many systemic diseases12,13,14,15. Importantly, it has been shown that the increased periodontitis-related all-cause and CVD mortalities are comparable with, but independent of, diabetes-related mortality16,17,18,19,20,21,22,23,24,25.
Results from a recent clinical trial, the Diabetes and Periodontal Therapy Trial (DPTT), do not support the use of nonsurgical periodontal treatment in patients with diabetes and periodontitis for the purpose of lowering levels of glycated hemoglobin (HbA1c)26. However, it is important to note that the trial did not evaluate the changes of periodontal microbiota after periodontal treatment. Studies have demonstrated that the re-development of oral microbiota was so rapid that the abundance of many pathogenic bacterial species exceeded the baseline values in two days after periodontal treatment27. It is likely that the failure to benefit from periodontal treatment was due to the failure to establish a commensal microbiota after the treatment.
It is believed that complex interactions between specific periodontal pathogens and different bacterial combinations are more relevant to periodontitis than are individual species28,29,30. We therefore hypothesize that a similar phenomenon exists in the association between periodontal microbiota and mortality rates. To test our hypothesis, we related 21 serum immunoglobulins G (IgGs) against periodontal bacteria to the rates of all-cause, diabetes-related, and hypertension-related mortalities in a death cohort from a representative sample of the US population, the Third National Health and Nutrition Examination Survey (NHANES III).
Methods
Study cohort
The NHANES III was performed between 1988 and 1994 by the National Center for Health Statistics (NCHS)31. It is a cross-sectional nationwide health survey of 33994 non-institutionalized US residents aged 2 months and older using a stratified multistage probability sampling design to sample a representative cohort of the US general population. The survey protocol was approved by the Institutional Review Board of the Centers for Disease Control and Prevention. All participants gave written informed consent. This study has been conducted according to the principles expressed in the Declaration of Helsinki.
All available sera from NHANES III (1988–1994) participants 40+ years old (n = 8153) were tested for the presence and level of 21 IgG antibodies against a broad panel of periodontal bacteria using a rapid checkerboard immunoblotting technique32,33. We excluded persons with missing IgG data, history of diabetes, heart attack, stroke, or cancers. Participants on immunomodulatory medications or corticosteroids were also excluded from our study. Among non-smokers, other tobacco product users such as chewing tobacco, cigar, and pipe and cotinine level >15 ng/ml were also excluded. We used the linked mortality-follow-up data through December 31, 2011 for these NHANES III participants and identified 1908 deaths (Table 1). The mean follow-up time to death was 10.9 years. A death was coded diabetes-related if ICD-9 code ‘250’ or ICD-10 codes ‘E10 thru E14’ was coded in the entity-axis multiple cause of death codes. For hypertension-related death, it was ICD-9 codes ‘401’ or ‘403’ or ICD-10 codes ‘I10’ or ‘I12’. Among this death cohort, 113 deaths were diabetes-related and 240 deaths were hypertension-related.
Serum immunoglobulins G against periodontal bacteria
The following bacterial strains were used to prepare whole cell antigenic extracts for determining the levels of 21 IgG antibodies by means of the “checkerboard” immunoassay: Aggregatibacter actinomycetemcomitans ATCC strains #43718, #29523 and #33384; Porphyromonas gingivalis ATCC #33277 and #53978; Tannerella forsythia ATCC#43037 (TF); Treponema denticola OMGS#3271 (TD); Campylobacter rectus ATCC#33238 (CR); Eubacterium nodatum ATCC#33099 (EN); Prevotella intermedia ATCC#25611 (PI); Prevotella nigrescens ATCC#33563 (PN); Prevotella melaninogenica ATCC#25845 (PM); Fusobacterium nucleatum ATCC#10953 (FN); Micromonas micros ATCC #33270 (MM); Selenomonas noxia ATCC#43541 (SN); Eikenella corrodens ATCC#23834 (EC); Capnocytophaga ochracea ATCC#33624 (CO); Streptococcus intermedius ATCC#27335 (SI); Streptococcus oralis ATCC#35037 (SO); Streptococcus mutans ATCC#25175 (SM); Veillonella parvula ATCC#10790 (VP); and Actinomyces naeslundii ATCC#49340 (AN). To assess the level of antibody to Porphyromonas gingivalis, a mixed suspension of ATCC strains #33277 and #53978 (PGMX) was used. For the assessment of antibody to Aggregatibacter actinomycetemcomitans, a mixed suspension of three strains (ATCC#43718, #29523 and #33384; AAMX) was used as well as individual preparations from Aggregatibacter actinomycetemcomitans serotype a (ATCC strain #29523, AA29) and serotype b (ATCC strain #43718, AAY4).
Detailed laboratory procedures have been described elsewhere and summarized in Fig. 1 32. Briefly, each bacterial colony was cultivated on a Trypticase soy agar plate supplemented with 5% sheep blood. After 2 days of incubation period, colonies were harvested and suspended in phosphate buffered saline (PBS, pH 7.4), and sequentially sonicated on ice for 10 seconds with a micro-ultrasonic cell disrupter (Kontes, Vineland, NJ). The optical density of each suspension was adjusted to 1.0 at 600 nm, using a spectrophotometer (Ultrospec III, Parmacia, Sweden). The qualifications of the antigens have been validated with enzyme-linked immunosorbent assay (ELISA)32. The whole cell antigenic extracts derived from each of the above species and protein A standards were immobilized on nitrocellulose membranes. Serially diluted (1/250, 1/500 and 1/1000) serum from each subject as well as human IgG standards (250 ng/ml and 125 ng/ml) were loaded perpendicularly to the bacterial extracts, and were allowed to interact. After several washing steps, membranes were incubated with Fab fragments of anti-human IgG conjugated with horseradish-peroxidase and a horseradish-peroxidase substrate. The chemiluminescent signal was assessed in a LumiImagerTM Workstation. Signals were compared to the ones generated by the protein A and human IgG standards and expressed in a scale of 0 to 9. Whenever signal was present at several serum dilutions, the signal generated by the highest dilution was used to represent the particular patient’s antibody titer.
Flow diagram summarizes experimental procedures for checkerboard immunoassay.
Whole cell bacterial antigenic extracts were used for determining the levels of IgG antibodies. The whole cell antigenic extracts and protein A standards were immobilized on nitrocellulose membranes. Serially diluted (1/250, 1/500 and 1/1000) serum from each subject as well as human IgG standards (250 ng/ml and 125 ng/ml) were loaded perpendicularly to the bacterial extracts, and were allowed to interact. After several washing steps, membranes were incubated with Fab fragments of anti-human IgG conjugated with horseradish-peroxidase and a horseradish-peroxidase substrate. The chemiluminescent signal was assessed in a LumiImagerTM Workstation. Signals were compared to the ones generated by the protein A and human IgG standards and expressed in a scale of 0 to 9. Whenever signal was present at several serum dilutions, the signal generated by the highest dilution was used to represent the particular patient’s antibody titer. IgG: immunoglobulin G.
All assessed antibody titer levels are reported in the units of μg/ml in this data release. The mean (+/−standard error (SE)) of the coefficients of variation (CVs) for replicates within an assay averaged 7.3 (+/−2.3%)32. The CVs of the assay run on different days for serum antibody to a range of subgingival species averaged 10.1 (+/−2.1%) using the beaded protein A matrix preparation and 16.1 (+/−4.4%) using protein A solution directly on the membrane. Antibody present at levels >5 μg/ml were detectable in all replicates of each sample.
Serum levels of vitamin C, vitamin E, lutein/zeazanthin, and C reactive protein
Details about the procedures and quality control systems for the determination of serum levels of vitamin C, vitamin E (alpha-tocopherol), lutein/zeazanthin, and C reactive protein (CRP) in the NHANES III have been described elsewhere34,35. In brief, vitamin C levels were measured by high-performance liquid chromatography (HPLC) with an electrochemical detector. Levels of vitamin E and lutein/zeazanthin were measured by using isocratic HPLC with detection at two different wavelengths. Serum CRP was measured with an automated Behring Nephelometer Analyzer System (Behring Diagnostics, Inc, Somerville, NJ).
Assessment of periodontal health
Details of the oral health component of the NHANES III are published elsewhere36. The NHANES III periodontal measurements included periodontal probing depth (PPD), gingival recession and bleeding on probing (BOP). Clinical attachment loss (CAL) was calculated as the sum of the recession and PPD. To measure these periodontal measurements, the teeth in each participant were divided into two maxillary and two mandibular halves and measurements were taken from two sites per tooth (mid-buccal and mesio-buccal) for all teeth (excluding third molars) in one randomly chosen upper and lower quadrant. We employed continuous periodontal parameters for mean number of tooth sites that bled on probing (mBOP) and mean CAL (mCAL).
Statistical methods
We summarized our analysis process in Fig. 2. First, because the distributions of the 21 IgG antibody levels showed positively skewed, before performing further analysis we first took a natural log for each of the IgG variables (Step 1 in Fig. 2). The log-transformed IgG variables were tested for normality and showed no significant deviations. These log(IgG) variables were used in further analysis.
Statistical analysis consists of six steps.
Step 1: Log-transformation. Step 2: Periodontal microbiota patterns by partial least squares regression. Step 3: Pattern (latent factor) score calculation. Step 4: Pattern score percentile ranking. Step 5: Periodontal microbiota patterns and mortalities association analysis. Step 6: Periodontal microbiota patterns and clinical periodontal measurements association analysis.
We first explored the associations between 21 individual IgG variables and total, diabetes-related, and hypertension-related mortalities (Supplementary Figure 1a–c, respectively). Although we entered the 21 IgG variables into the model at the same time, due to the highly collinearity among the 21 IgG variables, residual confounding remained being an issue. Therefore, the results were not used in making our conclusion. Furthermore, we aimed to assess the combined effect of the 21 highly correlated IgG antibodies on mortality rates. To achieve this objective, we used partial least squares (PLS) regression to assemble the 21 highly collinear IgG variables into another 21 uncorrelated factors (latent factors) that describe maximum correlation between the 21 IgG variables and two mortality variables (diabetes-related and hypertension-related mortalities) (Step 2 in Fig. 2). Each PLS-derived latent factor can be considered as a specific periodontal microbiota pattern. According to the PLS analysis, a pattern score for each of the latent factors can be calculated for every study subjects. A pattern score was calculated by summarizing the 21 log(IgG) variables weighted by their corresponding loadings derived from the PLS analysis (Step 3 in Fig. 2). A higher loading indicates a more important contribution of the specific IgG to the pattern score. Therefore, a pattern score for each of the latent factors represented a specific combination of periodontal bacteria. Next, we ranked and grouped our study subjects into 100 equal-sized subgroups (i.e. percentiles) according to each of the pattern scores and assigned the percentiles as the values for latent factor score percentile variables (Step 4 in Fig. 2). Using Cox proportional hazard models, the latent factor score percentile variables were then individually related to cause-specific mortality rates (Step 5 in Fig. 2). To evaluate if periodontal measurements, mBOP and mCAL (see Assessment of periodontal health section), are related to the latent factors, we run a linear regression using either mBOP or mCAL as the dependent variable and each of the individual latent factor score percentile variables as the independent variable (Step 6 in Fig. 2).
The following were considered as covariates in our regression analysis: age, sex, race, education level, smoking status, body mass index (BMI, computed from weight and height; Kg/m2), drinking alcohol (at least 12 drinks in the past 12 months), and serum levels of CRP, vitamin C, vitamin E, and lutein/zeaxanthin. However, we also examined the results derived from models without including vitamin C, vitamin E, and lutein/zeaxanthin variables. The results were similar and led to the same conclusion with the results from models including the three variables.
Our analyses were performed using SAS® SURVEY procedures (version 9.3; SAS Institute Inc, Cary, NC), which take into account of the complex sampling design used in NHANES III and yield unbiased SE and confidence interval (CI) estimates. We used P < 0.05 to denote statistical significance and all tests were two-sided.
Results
Characteristics of death cohorts
Table 1 shows the baseline characteristics of our study death cohort consisting of 1908 deaths, including 113 diabetes-related deaths and 240 hypertension-related deaths, after 10.9 years of follow-up in the NHANES III. Compared with non-diabetes-related deaths, diabetes-related deaths had higher BMI and lower serum levels of lutein/zeaxanthin (Table 2). There were marginally significant (0.05 < P < 0.1) differences in age, sex, race, and serum levels of CRP between the two groups. In terms of hypertension-related deaths (Table 3), they had significantly higher BMIs and tended to be non-Hispanic black than non-hypertension-related deaths. They also tended to be females but did not reach the significant level.
Partial least squares regression
As described in the Statistical methods section, using the PLS technique we reduced the 21 highly collinear IgG variables to a smaller set of uncorrelated latent factors. We decided to focus on the top five latent factors (Factors 1–5) derived from our PLS analysis because they met our preset criterion of accounting for over 70% of total variation in the 21 IgG variables. It is to say that we used PLS regression to reduce the 21 highly collinear IgG variables into five uncorrelated factors (latent factors) that described maximum correlation between independent (the 21 IgG) variables and dependent (mortality) variables. Factor 1 accounted for the largest variation (0.79%) in the two mortality variables (diabetes-related and hypertension-related mortalities) but only for a small variation (5.40%) in the 21 IgG variables. Factor 3 accounted for the largest variation (38.30%) in the 21 IgG variables followed by Factor 2 (17.89%), and they accounted for 0.13% and 0.29% respectively in the two mortality variables. Factor 4 and Factor 5 accounted for only small amounts of variations both in the 21 IgG variables (5.12% and 3.37% respectively) and in the two mortality variables (0.24% and 0.16% respectively).
Table 4 shows the PLS model effect loadings of the 21 IgG variables in each latent factor (Factor). A higher loading indicates a more important contribution of the specific IgG to the Factor, which represents a specific combination of periodontal microbiota. Accordingly, a pattern score for each of the Factors can be calculated for every study subjects by summarizing the 21 log(IgG) variables weighted by their corresponding loadings.
Factor 1 featured heavy loadings (≥0.2) in the IgGs against PGMX, PI, PN, and the three AA strains, but lower loadings (≤−0.2) in the IgGs against TF, EC, EN, VP, SN, and TD. Interestingly, PG, PI, PN, and the three AA strains have been shown to be strongly associated with periodontitis and our analysis also indicated that Factor 1 suggests active periodontitis (see Table 5). Factor 2 featured low loadings in all IgGs except the IgG against PGMX although the loading for PGMX was small (0.02); in other words, it featured a relatively high loading only in the IgG against PGMX. This data is consistent with that PG can serve as a keystone pathogen in periodontitis. The two latent factors were significantly associated with all-cause and/or diabetes-related mortalities (see Figs 3 and 4).
Cox proportional hazard regression analysis relating five partial least squares latent factors to all-cause death rate.
Models were adjusted for age, sex, race, education level, smoking status, body mass index, drinking alcohol (at least 12 drinks in the past 12 months), and serum levels of C reactive protein, vitamin C, vitamin E and lutein/zeaxanthin, and the sampling weights in the Third National Health and Nutrition Examination Survey. IgG: immunoglobulin G. PLS: partial least squares. HR: hazard ratio. CI: confidence interval.
Cox proportional hazard regression analysis relating five partial least squares latent factors to diabetes-related death rate.
Models were adjusted for age, sex, race, education level, smoking status, body mass index, drinking alcohol (at least 12 drinks in the past 12 months), and serum levels of C reactive protein, vitamin C, vitamin E and lutein/zeaxanthin, and the sampling weights in the Third National Health and Nutrition Examination Survey. IgG: immunoglobulin G. PLS: partial least squares. HR: hazard ratio. CI: confidence interval.
Factor 3 featured high loadings in all IgGs, especially (≥0.2) the IgG against PGMX, TF, the three AA strains, SO, CR, EC, EN, SI, VP, SN, TD, and SM. Factor 3 can be considered as an enhanced host immune responses resulting in high levels in all of the 21 IgGs.
Factor 4 featured low loadings in most IgGs except the IgGs against SO, MM, EN, SI, AN, and SM. Factor 5 were heavily loaded (≥0.2) in IgGs against PN, CO, PM, and SM, but featured lower loadings (≤−0.2) in IgGs against the three AA strains, CR, EC, EN, and AN. In contrast to Factor 1, Factor 4 featured low loadings in the IgGs against PGMX, PI, PN and the three AA strains and Factor 5 featured low loadings in the IgGs against PGMX, PI, and the three AA strains. Therefore, Factor 4 and Factor 5 can be considered as two reflections of Factor 1 in terms of the loadings for the characteristic bacterial antibodies.
Serum immunoglobulin G patterns and clinical periodontal measurements
As defined in the Assessment of periodontal health section, BOP can be considered as a sign of periodontal inflammation and CAL can be considered as a measure of the extent of the periodontal support that has been destroyed around a tooth. We used mean BOP (mBOP) as a surrogate to the activity of periodontitis and mean CAL (mCAL) as a surrogate to the overall periodontal destruction (severity) for a subject. Table 5 shows the relationships between the two periodontal measurements and the five latent factors. Accordingly, we described Factor 1 as an indicator of “active periodontitis”, Factor 2 as an indicator of “no clinically significant periodontitis”, Factor 3 as an indicator of “inactive periodontitis”, Factor 4 as an indicator of “inactively protective against periodontitis”, and Factor 5 as an indicator of “actively protective against periodontitis”.
Serum immunoglobulin G patterns and mortalities
In our Cox regression analysis, we found that, per percentile increased in Factor 2 score, there was a 0.2% increase in total mortality rate (hazard ratio (HR) = 1.002; 95% CI: 1.000 to 1.004); in other words, compared with people in the lowest percentile of Factor 2 score, those in the highest percentile of Factor 2 score had 20% higher all-cause mortality rate (Fig. 3). Further adjustment for the status of diabetes-related mortality did not change the results. There were marginally significantly (P = 0.08 and P = 0.0995, respectively) lower all-cause mortality rate per percentile increased in Factor 4 score and Factor 5 score (HRs = 0.998). In our diabetes-related mortality analysis (Fig. 4), we found that higher scores in either Factor 1 or Factor 2 were significantly associated with high rates of death due to diabetes-related causes; per percentile increased in the scores was related to a 1.1% increase in diabetes-related death. In other words, compared with people in the lowest percentile of Factor 1 or Factor 2 score, those in the highest percentile of Factor 1 or Factor 2 score had over one-fold higher rate of death due to diabetes-related causes. No significant relationship was noted between hypertension-related mortality and any of the five pattern scores (Fig. 5).
Cox proportional hazard regression analysis relating five partial least squares latent factors to hypertension-related death rate.
Models were adjusted for age, sex, race, education level, smoking status, body mass index, drinking alcohol (at least 12 drinks in the past 12 months), and serum levels of C reactive protein, vitamin C, vitamin E and lutein/zeaxanthin, and the sampling weights in the Third National Health and Nutrition Examination Survey. IgG: immunoglobulin G. PLS: partial least squares. HR: hazard ratio. CI: confidence interval.
Discussion
In this study, we found that two baseline serum IgG patterns, Factor 1 and Factor 2, were significantly associated with higher all-cause and/or diabetes-related mortality rates among people without history of diabetes, CVD, and cancers. While only Factor 2 was related to all-cause mortality, both Factor 1 and Factor 2 were related to diabetes-related mortality. To our best knowledge, this is the first data showing that specific oral microbiota may have an impact on the rate of death in humans.
Different from most studies in human microbiota, which measure bacterial DNA to evaluate the quantities and species of microbiome, we used serum IgGs against periodontal bacteria in this study. Serum IgGs reflected human systemic response to the corresponding periodontal bacteria and studies have shown that individual periodontal bacterial quantities were significantly correlated with corresponding serum antibody levels37. Therefore, the serum IgG levels can be considered as host-related phenotypes of periodontal microbiota.
Our analysis showed that, although the two mortality-related IgG patterns that we characterized featured several bacteria, which were also featured in periodontitis-related complexes, they were in different combinations. It seemed that different bacterial combinations have different impacts on human health. For example, Socransky et al. identified five microbial complexes, which were repeatedly found together in subgingival biofilm28. Among these, the “red complex”, consisting of PG, TF, and TD, is considered the most pathogenic microbial complex for periodontitis38. Our Factor 1 (an indicator of active periodontitis; see Table 5) featured heavy loadings in the IgGs against PGMX, PI, PN, and the three AA strains, all of which were strongly associated with periodontitis28. However, unlike Socransky’s red complex, our Factor 1 featured low loadings in the IgGs against TF and TD. Similarly, our Factor 2 (an indicator of no clinically significant periodontitis) featured a relatively high loading (with a small value of loading factor of 0.02, see Table 4) only in the IgG against PGMX but low loadings in all the other IgGs, including the two IgGs against TF and TD. Interestingly, our findings coincide with the hypothesis of PG as a keystone pathogen. It is conceived that the mere presence of a keystone pathogen, even at very low colonization levels, can modulate host response in ways that alter the amount and composition of subgingival microbiota, thereby triggering adverse effects on human health29,39. It has been demonstrated in a murine periodontal model that the introduction of PG, even at low numbers, in cooperation with other dysbiotic bacteria led to a marked acceleration in pathological alveolar bone loss, but PG alone failed to induce periodontitis39. Importantly, our findings from Factor 1 and Factor 2 also, respectively, suggested that active periodontitis may increase diabetes-related death rate, and that, even without clinically significant periodontitis, the presence of PG at very low colonization levels increase total and diabetes-related death rate. It seemed that the elimination of PG is crucial in reducing risk for both periodontitis and mortality.
Despite of featuring high loadings in all of the 21 IgGs, we did not find an association between Factor 3 and mortalities. As Factor 3 indicating an inactive periodontitis, it was likely that Factor 3 reflected an enhanced host immune responses resulting in a periodontal bacterial consortium which was constrained to a homeostasis. It was also noteworthy that, in contrast with Factor 1, which featured heavy loadings in the IgGs against PGMX, PI, PN and the three AA strains and showed a significant association with diabetes-related mortality but no association with total mortality, Factor 4 (featuring low loadings in the IgGs against PGMX, PI, PN and the three AA strains) and Factor 5 (featuring low loadings in the IgGs against PGMX, PI, and the three AA strains) suggested protective against total mortality but no association with diabetes-related mortality. Our data provided self-consistent evidence that the suppression of this specific bacterial combination, PGMX, PI, and the three AA strains, may be beneficial. However, studies have suggested that a specific combination of periodontal bacterial species may have important implication on a human disease only in a particular population29. Our findings in a representative US cohort may be different from those in other populations.
Our findings collaborated with previous observations that periodontitis, a result of polymicrobial infection, increased the risk for several major diseases, such as diabetes, CVD, cancers40,41,42,43, and mortalities as well16,17,18,19,20,21,22,23,24,25. The etiologies may involve several pathological consequences leading to uncontrolled inflammation, such as elevated levels of systemic proinflammatory cytokines14,44,45, oxidative stress46,47, formation of advanced glycation end products48, disturbed microbe-host nutrition and metabolism interaction49,50,51, etc. These mechanisms may be responsible not only for the initiation but also for the promotion and progression of the diseases as well, and thus lead to higher death rates. However, it has been shown that periodontal microbial interactions are complex and that numerous genes related to motility, metabolism, and virulence in one bacterium are differentially regulated in the presence of others29,52,53. The detailed mechanisms relating specific combinations of periodontal bacteria to specific diseases or death rates warrant further study. The information would be valuable in developing personalized therapeutic and prevention strategies.
The strengths of this study included a prospective study in a representative cohort of the US population, standardized collection of risk factor information and periodontal examinations to minimize the influence of confounding factors and misclassifications. However, the ascertainment of cause-specific death in the NHANES III may not comprehensive enough, especially for the hypertension-related death used in this study. The limited number of diabetes-related deaths in our study resulted in inadequate sample sizes for some analyses. Among the 1908 apparently healthy study subjects, 1792 (93.9%) had missing information for taking cholesterol lowing medications. This hindered us in addressing the potential confounding issue, especially for our analysis on the hypertension-related mortality. Although serum IgGs are considered to reflect chronic, intermittent exposure54, the one-time measurement at baseline may not reflect a long-term exposure to dynamic periodontal microbiota.
In conclusion, our analysis suggested that specific combinations of periodontal bacteria, even without inducing clinically significant periodontitis, may have a significant impact on human cause-specific death rates. More mechanistic and human observational studies are needed before a clinical trial could be implemented to confirm our findings. If an etiological relationship of specific periodontal microbiota to death rates is established, increased mortality could be transmittable via the transfer of oral microbiota. In that case, developing personalized strategies and maintaining a healthy oral microbiota, beyond that against periodontitis, would be important to manage the increased mortality risk.
Additional Information
How to cite this article: Chiu, C.-J. et al. Associations between Periodontal Microbiota and Death Rates. Sci. Rep. 6, 35428; doi: 10.1038/srep35428 (2016).
References
Honda, K. Porphyromonas gingivalis sinks teeth into the oral microbiota and periodontal disease. Cell Host Microbe. 10, 423–425 (2011).
Darveau, R. P. Periodontitis: a polymicrobial disruption of host homeostasis. Nat Rev Microbiol. 8, 481–490 (2010).
Burt, B. & Research Science and Therapy Committee of the American Academy of Periodontology. Position paper: epidemiology of periodontal diseases. J Periodontol. 76, 1406–1419 (2005).
Chapple, I. L. Time to take periodontitis seriously. BMJ. 348, g2645 (2014).
Rosenstein, E. D., Greenwald, R. A., Kushner, L. J. & Weissmann, G. Hypothesis: the humoral immune response to oral bacteria provides a stimulus for the development of rheumatoid arthritis. Inflammation. 28, 311–318 (2004).
Kozarov, E. V., Dorn, B. R., Shelburne, C. E., Dunn, W. A. J. & Progulske-Fox, A. Human atherosclerotic plaque contains viable invasive Actinobacillus actinomycetemcomitans and Porphyromonas gingivalis. Arterioscler Thromb Vasc Biol. 25, e17–18 (2005).
Genco, R., Offenbacher, S. & Beck, J. Periodontal disease and cardiovascular disease: epidemiology and possible mechanisms. J Am Dent Assoc. 133, 14S-22S (2002).
Chapple, I. L., Genco, R. & Working group 2 of the joint EFP/AAP workshop. Diabetes and periodontal diseases: consensus report of the Joint EFP/AAP Workshop on Periodontitis and Systemic Diseases. J Periodontol. 84, S106–112 (2013).
Demmer, R. T. et al. Periodontal Bacteria and Prediabetes Prevalence in ORIGINS: The Oral Infections, Glucose Intolerance, and Insulin Resistance Study. J Dent Res. 94, 201S–211S (2015).
Southerland, J. H., Taylor, G. W., Moss, K., Beck, J. D. & Offenbacher, S. Commonality in chronic inflammatory diseases: Periodontitis, diabetes, and coronary artery disease. Periodontol 2000 40, 130–143 (2006).
Birkedal-Hansen, H. Role of cytokines and inflammatory mediators in tissue destruction. J Periodontal Res 28, 500–510 (1993).
Schenkein, H. A. & Loos, B. G. Inflammatory mechanisms linking periodontal diseases to cardiovascular diseases. J Clin Periodontol 40, S51–S69 (2013).
Choi, H. M., Han, K., Park, Y. G. & Park, J. B. Associations Among Oral Hygiene Behavior and Hypertension Prevalence and Control: The 2008 to 2010 Korea National Health and Nutrition Examination Survey. J Periodontol 86, 866–873 (2015).
Lalla, E. & Papapanou, P. N. Diabetes mellitus and periodontitis: a tale of two common interrelated diseases. Nat Rev Endocrinol. 7, 738–748 (2011).
Noble, J. M. et al. Serum IgG antibody levels to periodontal microbiota are associated with incident Alzheimer disease. PLoS One. 9, e114959 (2014).
Sharma, P., Dietrich, T., Ferro, C. J., Cockwell, P. & Chapple, I. L. Association between periodontitis and mortality in stages 3-5 chronic kidney disease: NHANES III and linked mortality study. J Clin Periodontol. 43, 104–113 (2016).
Saremi, A. et al. Periodontal disease and mortality in type 2 diabetes. Diabetes Care. 28, 27–32 (2005).
Albert, D. A. et al. Diabetes and oral disease: implications for health professionals. Ann N Y Acad Sci. May, 1255, 1251–1215 (2012).
Li, Q. et al. Oral disease and subsequent cardiovascular disease in people with type 2 diabetes: a prospective cohort study based on the Action in Diabetes and Vascular Disease: Preterax and Diamicron Modified-Release Controlled Evaluation (ADVANCE) trial. Diabetologia. 53, 2320–2327 (2010).
Kshirsagar, A. V. et al. Periodontal disease adversely affects the survival of patients with end-stage renal disease. Kidney International 75, 746–751 (2009).
Chen, L. P. et al. Relationship between periodontal disease and mortality in patients treated with maintenance hemodialysis. Am J Kidney Dis. 57, 276–282 (2011).
de Souza, C. M. et al. Association among oral health parameters, periodontitis, and its treatment and mortality in patients undergoing hemodialysis. J Periodontol 85, E169–E178 (2014).
Garcia, R. I., Krall, E. A. & Vokonas, P. S. Periodontal disease and mortality from all causes in the VA Dental Longitudinal Study. Ann Periodontol 3, 339–349 (1998).
Xu, F. & Lu, B. Prospective association of periodontal disease with cardiovascular and all-cause mortality: NHANES III follow-up study. Atherosclerosis 218, 536–542 (2011).
Linden, G. J. et al. All-cause mortality and periodontitis in 60–70-year-old men: a prospective cohort study. J Clin Periodontol 39, 940–946 (2012).
Engebretson, S. P. et al. The effect of nonsurgical periodontal therapy on hemoglobin A1c levels in persons with type 2 diabetes and chronic periodontitis: a randomized clinical trial. JAMA. 310, 2523–2532 (2013).
Uzel, N. G. et al. Microbial shifts during dental biofilm re-development in the absence of oral hygiene in periodontal health and disease. J Clin Periodontol. 38, 612–620 (2011).
Socransky, S. S., Haffajee, A. D., Cugini, M. A., Smith, C. & Kent, R. L. J. Microbial complexes in subgingival plaque. J Clin Periodontol 25, 134–144 (1998).
Torrungruang, K., Jitpakdeebordin, S., Charatkulangkun, O. & Gleebbua, Y. Porphyromonas gingivalis, Aggregatibacter actinomycetemcomitans, and Treponema denticola/Prevotella intermedia Co-Infection Are Associated with Severe Periodontitis in a Thai Population. PLoS One. 10, e0136646 (2015).
Lourenço, T. G. et al. Microbial signature profiles of periodontally healthy and diseased patients. J Clin Periodontol. 41, 1027–1036 (2014).
US Government Printing Office. Series 1,1. DHHS publication (PHS) 94 1308. ed. (National Center for Health Statistics) (Washington, DC, 1994).
Sakellari, D., Socransky, S. S., Dibart, S., Eftimiadi, C. & Taubman, M. A. Estimation of serum antibody to subgingival species using checkerboard immunoblotting. Oral Microbiol Immunol. 12, 303–310 (1997).
Dye, B. A. et al. Serum antibodies to periodontal bacteria as diagnostic markers of periodontitis. J Periodontol. 80, 634–647 (2009).
Gunter, E. W., Lewis, B. G. & Koncikowski, S. M. ed (National Center for Environmental Health Centers for Disease Control and Prevention, and National Center for Health Statistics.) (Atlanta, GA., 1996).
Gunter, E. W. & McQuillan, G. Quality control in planning and operating the laboratory component for the Third National Health and Nutrition Examination Survey. J Nutr. 120, 1451–1454 (1990).
Drury, T. F. et al. An overview of the oral health component of the 1988–1991 national health and nutrition examination survey (NHANES III-Phase 1). J Dent Res 75, 620–630 (1996).
Pussinen, P. J. et al. Periodontal pathogen carriage, rather than periodontitis, determines the serum antibody levels. J Clin Periodontol. 38, 405–411 (2011).
Suzuki, N., Yoneda, M. & Hirofuji, T. Mixed red-complex bacterial infection in periodontitis. Int J Dent. 2013, 587279 (2013).
Hajishengallis, G. et al. Low-abundance biofilm species orchestrates inflammatory periodontal disease through the commensal microbiota and complement. Cell Host Microbe. 10, 497–506 (2011).
Taylor, G. W. Bidirectional interrelationships between diabetes and periodontal diseases: an epidemiologic perspective. Ann Periodontol. 6, 99–112 (2001).
Slocum, C., Kramer, C. & Genco, C. A. Immune dysregulation mediated by the oral microbiome: potential link to chronic inflammation and atherosclerosis. J Intern Med. 280, 114–128 (2016).
Zeng, X. T. et al. Periodontal Disease and Incident Lung Cancer Risk: A Meta-Analysis of Cohort Studies. J Periodontol. 87, 1158–1164 (2016).
Whitmore, S. E. & Lamont, R. J. Oral bacteria and cancer. PLoS Pathog. 10, e1003933 (2014).
Hajishengallis, G. Periodontitis: from microbial immune subversion to systemic inflammation. Nat Rev Immunol. 15, 30–44 (2015).
Slocum, C. et al. Distinct lipid a moieties contribute to pathogen-induced site-specific vascular inflammation. PLoS Pathog. 10, e1004215 (2014).
Bullon, P., Newman, H. N. & Battino, M . Obesity, diabetes mellitus, atherosclerosis and chronic periodontitis: a shared pathology via oxidative stress and mitochondrial dysfunction? Periodontol 2000 64, 139–153 (2014).
Varela-López, A., Quiles, J.L., Cordero, M., Giampieri, F. & Bullón, P. Oxidative Stress and Dietary Fat Type in Relation to Periodontal Disease. Antioxidants (Basel). 4, 322–344 (2015).
Katz, J. et al. Expression of the receptor of advanced glycation end products in gingival tissues of type 2 diabetes patients with chronic periodontal disease: a study utilizing immunohistochemistry and RT-PCR. J Clin Periodontol. 32, 40–44 (2005).
Wang, Z. et al. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature. 472, 57–63 (2011).
Arimatsu, K. et al. Oral pathobiont induces systemic inflammation and metabolic changes associated with alteration of gut microbiota. Sci Rep. 4, 4828 (2014).
Chapple, I. L. et al. Adjunctive daily supplementation with encapsulated fruit, vegetable and berry juice powder concentrates and clinical periodontal outcomes: a double-blind RCT. J Clin Periodontol. 39, 62–72 (2012).
Loozen, G. et al. Inter-bacterial correlations in subgingival biofilms: a large-scale survey. J Clin Periodontol 41, 1–10 (2014).
Sarkar, J., McHardy, I. H., Simanian, E. J., Shi, W. & Lux, R. Transcriptional responses of Treponema denticola to other oral bacterial species. PLOS One 9, e88361 (2014).
Noble, J. M. et al. Periodontitis is associated with cognitive impairment among older adults: analysis of NHANES-III. J Neurol Neurosurg Psychiatry. 80, 1206–1211 (2009).
Acknowledgements
Any opinions, findings, conclusions, or recommendations expressed in this publication are those of the authors and do not necessarily reflect the views or policies of the U.S. Department of Agriculture, nor does mention of trade names, commercial products, or organizations imply endorsement by the US Government. Financial support for this project has been provided by the RO1EY021826 (C.-J.C.), RO1EY013250 and RO1EY021212 (A.T.) from the National Institutes of Health, and the United States Department of Agriculture under agreements, 1950–5100–060–01A. We thank Yu-Hsuan Chiu for her help with proofreading this manuscript.
Author information
Authors and Affiliations
Contributions
C.-J.C. raised the hypothesis, designed the study, directed and performed the statistical analysis and drafted the manuscript. M.-L.C. helped conceive of the hypothesis, searched for related literature, and helped draft the manuscript. A.T. participated in study coordination, provided administrative and technical support and review of the manuscript. All authors read and approved the final manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Chiu, CJ., Chang, ML. & Taylor, A. Associations between Periodontal Microbiota and Death Rates. Sci Rep 6, 35428 (2016). https://doi.org/10.1038/srep35428
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep35428
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.