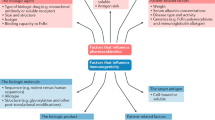
Key Points
-
Monoclonal antibodies and fusion proteins induce the formation of antidrug antibodies (ADAs), the occurrence and magnitude of which differs between chimeric antibodies, fully humanized antibodies and fusion proteins
-
The clinical implication of ADAs are unclear, although ADAs are known to cause secondary drug failure
-
Consensus definitions of primary and secondary non-response are lacking, as are evidence-based recommendations on how to guide biologic therapy on the basis of drug level and immunogenicity
-
Testing for ADAs or serum trough drug levels might be indicated in some situations of primary and secondary treatment failure and could prompt changes in dosing or therapeutic agent
-
When switching from an anti-TNF drug (originator) to a biosimilar of that originator, one has to take into consideration that ADAs against the originator will crossreact with the biosimilar, causing treatment failure
-
More information regarding the immunogenicity of the different TNF antagonists and improved ADA testing systems could lead to the development of an immune-pharmacologic strategy for the individualized treatment of rheumatoid arthritis
Abstract
The availability of monoclonal antibodies has revolutionized the treatment of an increasingly broad spectrum of diseases. Inflammatory diseases are among those most widely treated with protein-based therapeutics, termed biologics. Following the first large-scale clinical trials with monoclonal antibodies performed in the 1990s by rheumatologists and clinical immunologists, the approval of these agents for use in daily clinical practice led to substantial progress in the treatment of rheumatic diseases. Despite this progress, however, only a proportion of patients achieve a long-term clinical response. Data on the use of agents blocking TNF, which were among the first biologics introduced into clinical practice, provide ample evidence of primary and secondary treatment inefficacy in patients with rheumatoid arthritis (RA). Important issues relevant to primary and secondary failure of these agents in RA include immunogenicity, methodological problems for the detection of antidrug antibodies and trough drug levels, and the implications for treatment strategies. Although there is no strong evidence to support the routine estimation of antidrug antibodies or serum trough levels during anti-TNF therapy, these assessments might be helpful in a few clinical situations; in particular, they might guide decisions on switching the therapeutic biologic in certain instances of secondary clinical failure.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Rothe, A., Power, B. E. & Hudson, P. J. Therapeutic advances in rheumatology with the use of recombinant proteins. Nat. Clin. Pract. Rheumatol. 4, 605–614 (2008).
Cantarovich, D. et al. Treatment of acute kidney rejection episodes with monoclonal antibody directed against IL2 receptor: a pilot study. Transplant. Proc. 21, 1785–1786 (1989).
Cantarovich, D. et al. Anti-IL2 receptor monoclonal antibody (33B3.1) in prophylaxis of early kidney rejection in humans: a randomized trial versus rabbit antithymocyte globulin. Transplant. Proc. 21, 1769–1771 (1989).
Horneff, G., Burmester, G. R., Emmrich, F. & Kalden, J. R. Treatment of rheumatoid arthritis with an anti-CD4 monoclonal antibody. Arthritis Rheum. 34, 129–140 (1991).
Elliott, M. J. et al. Randomised double-blind comparison of chimeric monoclonal antibody to tumour necrosis factor α (cA2) versus placebo in rheumatoid arthritis. Lancet 344, 1105–1110 (1994).
Kremer, J. M. et al. Long-term safety, efficacy and inhibition of radiographic progression with abatacept treatment in patients with rheumatoid arthritis and an inadequate response to methotrexate: 3-year results from the AIM trial. Ann. Rheum. Dis. 70, 1826–1830 (2011).
Sfikakis, P. P. The first decade of biologic TNF antagonists in clinical practice: lessons learned, unresolved issues and future directions. Curr. Dir. Autoimmun. 11, 180–210 (2010).
Weinblatt, M. E. et al. Adalimumab, a fully human anti-tumor necrosis factor α monoclonal antibody, for the treatment of rheumatoid arthritis in patients taking concomitant methotrexate: the ARMADA trial. Arthritis Rheum. 48, 35–45 (2003).
Keystone, E. C. et al. Once-weekly administration of 50 mg etanercept in patients with active rheumatoid arthritis: results of a multicenter, randomized, double-blind, placebo-controlled trial. Arthritis Rheum. 50, 353–363 (2004).
Weinblatt, M. E. et al. A trial of etanercept, a recombinant tumor necrosis factor receptor:Fc fusion protein, in patients with rheumatoid arthritis receiving methotrexate. N. Engl. J. Med. 340, 253–259 (1999).
Finckh, A., Simard, J. F., Gabay, C., Guerne, P. A. & SCQM physicians. Evidence for differential acquired drug resistance to anti-tumour necrosis factor agents in rheumatoid arthritis. Ann. Rheum. Dis. 65, 746–752 (2006).
van Dartel, S. A. et al. Difference in the risk of serious infections in patients with rheumatoid arthritis treated with adalimumab, infliximab and etanercept: results from the Dutch rheumatoid arthritis monitoring (DREAM) registry. Ann. Rheum. Dis. 72, 895–900 (2013).
Iannone, F. et al. Longterm retention of tumor necrosis factor-α inhibitor therapy in a large Italian cohort of patients with rheumatoid arthritis from the GISEA registry: an appraisal of predictors. J. Rheumatol. 39, 1179–1184 (2012).
Flendrie, M., Creemers, M. C., Welsing, P. M., den Broeder, A. A. & van Riel, P. L. Survival during treatment with tumour necrosis factor blocking agents in rheumatoid arthritis. Ann. Rheum. Dis. 62 (Suppl. 2), ii30–ii33 (2003).
Hetland, M. L. et al. Direct comparison of treatment responses, remission rates, and drug adherence in patients with rheumatoid arthritis treated with adalimumab, etanercept, or infliximab: results from eight years of surveillance of clinical practice in the nationwide Danish DANBIO registry. Arthritis Rheum. 62, 22–32 (2010).
Fafá, B. P. et al. Drug survival and causes of discontinuation of the first anti-TNF in ankylosing spondylitis compared with rheumatoid arthritis: analysis from BIOBADABRASIL. Clin. Rheumatol. 34, 921–927 (2015).
Carmona, L., Gómez-Reino, J. J. & BIOBADASER Group. Survival of TNF antagonists in spondylarthritis is better than in rheumatoid arthritis. Data from the Spanish registry BIOBADASER. Arthritis Res. Ther. 8, R72 (2006).
Biggioggero, M. & Favalli, E. G. Ten-year drug survival of anti-TNF agents in the treatment of inflammatory arthritides. Drug Dev. Res. 75, S38–S41 (2014).
Duclos, M. et al. Retention rates of tumor necrosis factor blockers in daily practice in 770 rheumatic patients. J. Rheumatol. 33, 2433–2438 (2006).
Schiff, M. H., von Kempis, J., Goldblum, R., Tesser, J. R. & Mueller, R. B. Rheumatoid arthritis secondary non-responders to TNF can attain an efficacious and safe response by switching to certolizumab pegol: a phase IV, randomised, multicentre, double-blind, 12-week study, followed by a 12-week open-label phase. Ann. Rheum. Dis. 73, 2174–2177 (2014).
Navarro Coy, N. C. et al. The 'Switch' study protocol: a randomised-controlled trial of switching to an alternative tumour-necrosis factor (TNF)-inhibitor drug or abatacept or rituximab in patients with rheumatoid arthritis who have failed an initial TNF-inhibitor drug. BMC Musculoskelet. Disord. 15, 452 (2014).
Fransen, J. & van Riel, P. L. The disease activity score and the EULAR response criteria. Clin. Exp. Rheumatol. 23, S93–S99 (2005).
Emery, P. Optimizing outcomes in patients with rheumatoid arthritis and an inadequate response to anti-TNF treatment. Rheumatology (Oxford) 51 (Suppl. 5), v22–v30 (2012).
Weyand, C. M. & Goronzy, J. J. Ectopic germinal center formation in rheumatoid synovitis. Ann. NY Acad. Sci. 987, 140–149 (2003).
van Vollenhoven, R. F. Switching between anti-tumour necrosis factors: trying to get a handle on a complex issue. Ann. Rheum. Dis. 66, 849–851 (2007).
Talotta, R. et al. Paradoxical expansion of Th1 and Th17 lymphocytes in rheumatoid arthritis following infliximab treatment: a possible explanation for a lack of clinical response. J. Clin. Immunol. 35, 550–557 (2015).
Souto-Carneiro, M. M. et al. Alterations in peripheral blood memory B cells in patients with active rheumatoid arthritis are dependent on the action of tumour necrosis factor. Arthritis Res. Ther. 11, R84 (2009).
Klaasen, R., Wijbrandts, C. A., Gerlag, D. M. & Tak, P. P. Body mass index and clinical response to infliximab in rheumatoid arthritis. Arthritis Rheum. 63, 359–364 (2011).
Arnott, I. D. R., McNeill, G. & Satsangi, J. An analysis of factors influencing short-term and sustained response to infliximab treatment for Crohn's disease. Aliment. Pharmacol. Ther. 17, 1451–1457 (2003).
Potter, C. et al. Association of rheumatoid factor and anti-cyclic citrullinated peptide positivity, but not carriage of shared epitope or PTPN22 susceptibility variants, with anti-tumour necrosis factor response in rheumatoid arthritis. Ann. Rheum. Dis. 68, 69–74 (2009).
Mugnier, B. et al. Polymorphism at position-308 of the tumor necrosis factor α gene influences outcome of infliximab therapy in rheumatoid arthritis. Arthritis Rheum. 48, 1849–1852 (2003).
Viatte, S. et al. Association of HLA-DRB1 haplotypes with rheumatoid arthritis severity, mortality, and treatment response. JAMA. 313, 1645–1656 (2015).
Criswell, L. A. et al. The influence of genetic variation in the HLA-DRB1 and LTA-TNF regions on the response to treatment of early rheumatoid arthritis with methotrexate or etanercept. Arthritis Rheum. 50, 2750–2756 (2004).
Plant, D. et al. Genome-wide association study of genetic predictors of anti-tumor necrosis factor treatment efficacy in rheumatoid arthritis identifies associations with polymorphisms at seven loci. Arthritis Rheum. 63, 645–653 (2011).
Plant, D., Wilson, A. G., Barton, A. Genetic and epigenetic predictors of responsiveness to treatment in RA. Nat. Rev. Rheumatol. 10, 329–337 (2014).
Lee, Y. H. & Bae, S. C. Associations between PTPRC rs10919563 A/G and FCGR2A R131H polymorphisms and responsiveness to TNF blockers in rheumatoid arthritis: a meta-analysis. Rheumatol. Int. 36, 837–844 (2016).
Cui, J. et al. Genome-wide association study and gene expression analysis identifies CD84 as a predictor of response to etanercept therapy in rheumatoid arthritis. PLoS Genet. 9, e1003394 (2013).
Fabris, M. et al. The TTTT B lymphocyte stimulator promoter haplotype is associated with good response to rituximab therapy in seropositive rheumatoid arthritis resistant to tumor necrosis factor blockers. Arthritis Rheum. 65, 88–97 (2013).
Lutt, J. R. & Deodhar, A. Rheumatoid arthritis: strategies in the management of patients showing an inadequate response to TNFα antagonists. Drugs 68, 591–606 (2008).
Montes, A. et al. Rheumatoid arthritis response to treatment across IgG1 allotype — anti-TNF incompatibility: a case-only study. Arthritis Res. Ther. 18, 63 (2015).
Tabrizi, M. A., Tseng, C.-M. L. & Roskos, L. K. Elimination mechanisms of therapeutic monoclonal antibodies. Drug Discov. Today 11, 81–88 (2006).
Keizer, R. J., Huitema, A. D., Schellens, J. H. & Beijnen, J. S. Clinical pharmacokinetics of therapeutic monoclonal antibodies. Clin. Pharmacokinet. 49, 493–507 (2010).
Souto, A., Maneiro, J. R. & Gómez-Reino, J. J. Rate of discontinuation and drug survival of biologic therapies in rheumatoid arthritis: a systematic review and meta-analysis of drug registries and health care databases. Rheumatology (Oxford) 55, 523–534 (2016).
Kang, J. H. et al. Drug survival rates of tumor necrosis factor inhibitors in patients with rheumatoid arthritis and ankylosing spondylitis. J. Korean Med. Sci. 29, 1205–1211 (2014).
Agarwal, S. K. et al. Predictors of discontinuation of tumor necrosis factor inhibitors in patients with rheumatoid arthritis. J. Rheumatol. 35, 1737–1744 (2008).
Hyrich, K. L., Watson, K. D., Silman, A. J. & Symmons, D. P. Predictors of response to anti-TNF-α therapy among patients with rheumatoid arthritis: results from the British Society for Rheumatology Biologics Register. Rheumatology (Oxford) 45, 1558–1565 (2006).
Anderson, P. J. Tumor necrosis factor inhibitors: clinical implications of their different immunogenicity profiles. Semin. Arthritis Rheum. 34 (Suppl. 1), 19–22 (2005).
Tracey, D., Klareskog, L., Sasso, E. H., Salfeld, J. G. & Tak, P. P. Tumor necrosis factor antagonist mechanisms of action: a comprehensive review. Pharmacol. Ther. 117, 244–279 (2008).
Deora, A. et al. Transmembrane TNF-dependent uptake of anti-TNF antibodies. MAbs 9, 680–695 (2017).
Atzeni, F. et al. Investigating the potential side effects of anti-TNF therapy for rheumatoid arthritis: cause for concern? Immunotherapy 7, 353–361 (2015).
Bremmer, M., Deng, A. & Gaspari, A. A mechanism-based classification of dermatologic reactions to biologic agents used in the treatment of cutaneous disease. Part 1. Dermatitis 20, 182–192 (2009).
Vultaggio, A., Maggi, E. & Matucci, A. Immediate adverse reactions to biologicals: from pathogenic mechanisms to prophylactic management. Curr. Opin. Allergy Clin. Immunol. 11, 262–268 (2001).
Leach, M. W. et al. Immunogenicity/hypersensitivity of biologics. Toxicol. Pathol. 42, 293–300 (2014).
Vultaggio, A. et al. Anti-infliximab IgE and non IgE antibodies and induction of infusion-related severe anaphylactic reactions. Allergy 65, 657–661 (2010).
Vultaggio, A. & Castells, M. C. Hypersensitivity reactions to biologic agents. Immunol. Allergy Clin. North Am. 34, 615–632 (2014).
Hart, M. H. et al. Differential effect of drug interference in immunogenicity assays. J. Immunol. Methods 372, 196–203 (2011).
Shankar, G. et al. Recommendations for the validation of immunoassays used for detection of host antibodies against biotechnology products. J. Pharm. Biomed. Anal. 48, 1267–1281 (2008).
Krieckaert, C., Rispens, T. & Wolbink, G. Immunogenicity of biological therapeutics: from assay to patient. Curr. Opin. Rheumatol. 24, 306–311 (2012).
Aarden, L., Ruuls, S. R. & Wolbink, G. Immunogenicity of anti-tumor necrosis factor antibodies-toward improved methods of anti-antibody measurement. Curr. Opin. Immunol. 20, 431–435 (2008).
Van Stappen, T., Brouwers, E., Vermeire, S. & Gils, A. Validation of a sample pretreatment protocol to convert a drug-sensitive into a drug-tolerant anti-infliximab antibody immunoassay. Drug Test. Anal. 9, 243–247 (2017).
Bian, S., Ferrante, M. & Gils, A. Validation of a drug-resistant anti-adalimumab antibody assay to monitor immunogenicity in the presence of high concentrations of adalimumab. AAPS J. 19, 468–474 (2017).
Van Stappen, T. et al. Clinical relevance of detecting anti-infliximab antibodies with a drug-tolerant assay: post hoc analysis of the TAXIT trial. Gut http://dx.doi.org/10.1136/gutjnl.2016-313071 (2017).
Bourdage, J. S., Cook, C. A., Farrington, D. L., Chain, J. S. & Konrad, R. J. An affinity capture elution (ACE) assay for detection of anti-drug antibody to monoclonal antibody therapeutics in the presence of high levels of drug. J. Immunol. Methods 327, 10–17 (2007).
van Schie, K. A. et al. The antibody response against human and chimeric anti-TNF therapeutic antibodies primarily targets the TNF binding region. Ann. Rheum. Dis. 74, 311–314 (2015).
Wolbink, G. J. et al. Development of antiinfliximab antibodies and relationship to clinical response in patients with rheumatoid arthritis. Arthritis Rheum. 54, 711–715 (2006).
Radstake, T. R. et al. Formation of antibodies against infliximab and adalimumab strongly correlates with functional drug levels and clinical responses in rheumatoid arthritis. Ann. Rheum. Dis. 68, 1739–1745 (2009).
de Vries, M. K. et al. Decreased clinical response to infliximab in ankylosing spondylitis is correlated with anti-infliximab formation. Ann. Rheum. Dis. 66, 1252–1254 (2007).
de Vries, M. K. et al. Inefficacy of infliximab in ankylosing spondylitis is correlated with antibody formation. Ann. Rheum. Dis. 66, 133–134 (2007).
van Schouwenburg, P. A. et al. Adalimumab elicits a restricted anti-idiotypic antibody response in autoimmune patients resulting in functional neutralisation. Ann. Rheum. Dis. 72, 104–109 (2013).
Bartelds, G. M. et al. Clinical response to adalimumab: relationship to anti-adalimumab antibodies and serum adalimumab concentrations in rheumatoid arthritis. Ann. Rheum. Dis. 66, 921–926 (2007).
Bartelds, G. M. et al. High levels of human anti-human antibodies to adalimumab in a patient not responding to adalimumab treatment. Ann. Rheum. Dis. 65, 1249–1250 (2006).
de Vries, M. K. et al. Decreased clinical response to adalimumab in ankylosing spondylitis is associated with antibody formation. Ann. Rheum. Dis. 68, 1787–1788 (2009).
Pouw, M. F. et al. Key findings towards optimising adalimumab treatment: the concentration-effect curve. Ann. Rheum. Dis. 74, 513–518 (2015).
Kneepkens, E. L. et al. Lower etanercept levels are associated with high disease activity in ankylosing spondylitis patients at 24 weeks of follow-up. Ann. Rheum. Dis. 74, 1825–1829 (2015).
Chen, D. Y. et al. Significant associations of antidrug antibody levels with serum drug trough levels and therapeutic response of adalimumab and etanercept treatment in rheumatoid arthritis. Ann. Rheum. Dis. 74, e16 (2015).
de Vries, M. K. et al. Immunogenicity does not influence treatment with etanercept in patients with ankylosing spondylitis. Ann. Rheum. Dis. 68, 531–535 (2009).
Kneepkens, E. L. et al. Golimumab trough levels, antidrug antibodies and clinical response in patients with rheumatoid arthritis treated in daily clinical practice. Ann. Rheum. Dis. 73, 2217–2219 (2014).
Reich, K. et al. Successful treatment of moderate to severe plaque psoriasis with the PEGylated Fab' certolizumab pegol: results of a phase II randomized, placebo-controlled trial with a re-treatment extension. Br. J. Dermatol. 167, 180–190 (2012).
Fleischmann, R. et al. Efficacy and safety of certolizumab pegol monotherapy every 4 weeks in patients with rheumatoid arthritis failing previous disease-modifying antirheumatic therapy: the FAST4WARD study. Ann. Rheum. Dis. 68, 805–811 (2009).
Maini, R. N. et al. Therapeutic efficacy of multiple intravenous infusions of anti-tumor necrosis factor α monoclonal antibody combined with low-dose weekly methotrexate in rheumatoid arthritis. Arthritis Rheum. 41, 1552–1563 (1998).
Garcês, S., Demengeot, J. & Benito-Garcia, E. The immunogenicity of anti-TNF therapy in immune-mediated inflammatory diseases: a systematic review of the literature with a meta-analysis. Ann. Rheum. Dis. 72, 1947–1955 (2013).
Maneiro, J. R., Salgado, E. & Gomez-Reino, J. J. Immunogenicity of monoclonal antibodies against tumor necrosis factor used in chronic immune-mediated inflammatory conditions: systematic review and meta-analysis. JAMA Intern. Med. 173, 1416–1428 (2013).
Krieckaert, C. L., Nurmohamed, M. T. & Wolbink, G. J. Methotrexate reduces immunogenicity in adalimumab treated rheumatoid arthritis patients in a dose dependent manner. Ann. Rheum. Dis. 71, 1914–1915 (2012).
Burmester, G. R. et al. Efficacy and safety of ascending methotrexate dose in combination with adalimumab: the randomised CONCERTO trial. Ann. Rheum. Dis. 74, 1037–1044 (2015).
Vogelzang, E. H. et al. Adalimumab trough concentrations in patients with rheumatoid arthritis and psoriatic arthritis treated with concomitant disease-modifying antirheumatic drugs. Ann. Rheum. Dis. 74, 474–475 (2015).
Jani, M., Barton, A., Warren, R. B., Griffiths, C. E. & Chinoy, H. The role of DMARDs in reducing the immunogenicity of TNF inhibitors in chronic inflammatory diseases. Rheumatology (Oxford) 53, 213–222 (2014).
Smolen, J. S. et al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2013 update. Ann. Rheum. Dis. 73, 492–509 (2014).
Singh, J. A. et al. 2015 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 68, 1–25 (2016).
Bunescu, A., Seideman, P., Lenkei, R., Levin, K. & Egberg, N. Enhanced Fcγ receptor I, αMβ2 integrin receptor expression by monocytes and neutrophils in rheumatoid arthritis: interaction with platelets. J. Rheumatol. 31, 2347–2355 (2004).
Joseph, A., Munroe, K., Housman, M., Garman, R. & Richards, S. Immune tolerance induction to enzyme-replacement therapy by co-administration of short-term, low-dose methotrexate in a murine Pompe disease model. Clin. Exp. Immunol. 152, 138–146 (2008).
Sandborn, W. J. Preventing antibodies to infliximab in patients with Crohn's disease: optimize not immunize. Gastroenterology 124, 1140–1145 (2003).
Rutgeerts, P. et al. Efficacy and safety of retreatment with anti-tumor necrosis factor antibody (infliximab) to maintain remission in Crohn's disease. Gastroenterology 117, 761–769 (1999).
Present, D. H. et al. Infliximab for the treatment of fistulas in patients with Crohn's disease. N. Engl. J. Med. 340, 1398–1405 (1999).
Hanauer, S. B. et al. Maintenance infliximab for Crohn's disease: the ACCENT I randomised trial. Lancet. 359, 1541–1549 (2002).
Ducourau, E. et al. Antibodies toward infliximab are associated with low infliximab concentration at treatment initiation and poor infliximab maintenance in rheumatic diseases. Arthritis Res. Ther. 13, R105 (2011).
Rutgeerts, P. et al. Comparison of scheduled and episodic treatment strategies of infliximab in Crohn's disease. Gastroenterology 126, 402–413 (2004).
Mitchison, N. A. Induction of immunological paralysis in two zones of dosage. Proc. R Soc. Lond. B Biol. Sci. 161, 275–292 (1964).
Mease, P. J. et al. Comparative effectiveness of biologic monotherapy versus combination therapy for patients with psoriatic arthritis: results from the Corrona registry. RMD Open 1, e000181 (2015).
Favalli, E. G., Biggioggero, M., Marchesoni, A. & Meroni, P. L. Survival on treatment with second-line biologic therapy: a cohort study comparing cycling and swap strategies. Rheumatology (Oxford) 53, 1664–1668 (2014).
Chatzidionysiou, K. et al. Effectiveness of TNF inhibitor switch in RA: results from the national Swedish register. Ann. Rheum. Dis. 74, 890–896 (2015).
Hyrich, K. L. et al. Outcomes after switching from one anti-tumor necrosis factor α agent to a second anti-tumor necrosis factor α agent in patients with rheumatoid arthritis: results from a large UK national cohort study. Arthritis Rheum. 56, 13–20 (2007).
Lequerré, T. et al. Switching from an anti-TNF monoclonal antibody to soluble TNF-receptor yields better results than vice versa: an observational retrospective study of 72 rheumatoid arthritis switchers. Joint Bone Spine 82, 330–337 (2015).
Mpofu, S., Fatima, F. & Moots, R. J. Anti-TNF-α therapies: they are all the same (aren't they?). Rheumatology (Oxford) 44, 271–273 (2005).
Levy, R. A. et al. Biology of anti-TNF agents in immune-mediated inflammatory diseases: therapeutic implications. Immunotherapy 8, 1427–1436 (2016).
Buch, M. H. et al. True infliximab resistance in rheumatoid arthritis; a role for lymphotoxin α? Ann. Rheum. Dis. 63, 1344–1346 (2004).
Finckh, A. et al. Which subgroup of patients with rheumatoid arthritis benefits from switching to rituximab versus alternative anti-tumour necrosis factor (TNF) agents after previous failure of an anti-TNF agent? Ann. Rheum. Dis. 69, 387–393 (2010).
Finckh, A. et al. B cell depletion may be more effective than switching to an alternative anti-tumor necrosis factor agent in rheumatoid arthritis patients with inadequate response to anti-tumor necrosis factor agents. Arthritis Rheum. 56, 1417–1423 (2007).
Du Pan, S. M., Scherer, A., Gabay, C. & Finckh, A. Differential drug retention between anti-TNF agents and alternative biological agents after inadequate response to an anti-TNF agent in rheumatoid arthritis patients. Ann. Rheum. Dis. 71, 997–999 (2012).
Emery, P. et al. Rituximab versus an alternative TNF inhibitor in patients with rheumatoid arthritis who failed to respond to a single previous TNF inhibitor: SWITCH-RA, a global, observational, comparative effectiveness study. Ann. Rheum. Dis. 74, 979–984 (2015).
Frederiksen, M. T. et al. Antibodies against infliximab are associated with de novo development of antibodies to adalimumab and therapeutic failure in infliximab-to-adalimumab switchers with IBD. Inflamm. Bowel Dis. 20, 1714–1721 (2014).
Ben-Horin, S. et al. Cross-immunogenicity: antibodies to infliximab in remicade-treated patients with IBD similarly recognise the biosimilar remsima. Gut 65, 1132–1138 (2016).
Yoo, D. H. et al. A randomized, double-blind, parallel-group study to demonstrate equivalence in efficacy and safety of CT-P13 compared with innovator infliximab when coadministered with methotrexate in patients with active rheumatoid arthritis: the PLANETRA study. Ann. Rheum. Dis. 72, 1613–1620 (2013).
Rosas, J. et al. Clinical relevance of monitoring serum levels of adalimumab in patients with rheumatoid arthritis in daily practice. Clin. Exp. Rheumatol. 32, 942–948 (2014).
Chen, D. Y. et al. Drug trough levels predict therapeutic responses to dose reduction of adalimumab for rheumatoid arthritis patients during 24 weeks of follow-up. Rheumatology (Oxford) 55, 143–148 (2016).
Liefferinckx, C. et al. Infliximab trough levels at induction to predict treatment failure during maintenance. Inflamm. Bowel Dis. 23, 1371–1381 (2017).
European Medicines Agency. Guideline on immunogenicity assessment of monoclonal antibodies intended for in vivo clinical use. European Medicines Agency http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2012/06/WC500128688.pdf (2012).
Freeman, K. et al. Clinical effectiveness and cost-effectiveness of use of therapeutic monitoring of tumour necrosis factor alpha (TNF-α) inhibitors (LISA-TRACKER® enzyme-linked immunosorbent assay (ELISA) kits, TNF-α Blocker ELISA kits and Promonitor® ELISA kits) versus standard care in patients with Crohn's disease: systematic reviews and economic modelling. Health Technol. Assess. 20, 1–288 (2016).
Acknowledgements
The authors sincerely thank Martina Seidel for instrumental help with the preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Both authors researched data for article, made substantial contributions to discussion of content, wrote the article and undertook review and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Kalden, J., Schulze-Koops, H. Immunogenicity and loss of response to TNF inhibitors: implications for rheumatoid arthritis treatment. Nat Rev Rheumatol 13, 707–718 (2017). https://doi.org/10.1038/nrrheum.2017.187
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2017.187
This article is cited by
-
A Real-World Effectiveness Study Using a Mobile Application to Evaluate Early Outcomes with Upadacitinib in Rheumatoid Arthritis
Rheumatology and Therapy (2023)
-
Silence of S1PR4 Represses the Activation of Fibroblast-like Synoviocytes by Regulating IL-17/STAT3 Signaling Pathway
Inflammation (2023)
-
Pan American League of Associations for Rheumatology recommendations for the management of axial spondyloarthritis
Nature Reviews Rheumatology (2023)
-
The second decade of anti-TNF-a therapy in clinical practice: new lessons and future directions in the COVID-19 era
Rheumatology International (2022)
-
sTNFRII-Fc modification protects human UC-MSCs against apoptosis/autophagy induced by TNF-α and enhances their efficacy in alleviating inflammatory arthritis
Stem Cell Research & Therapy (2021)