Key Points
-
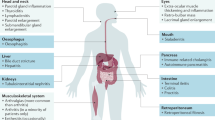
IgG4-related disease represents a chronic inflammatory disorder characterized by various systemic organ dysfunctions, such as IgG4-associated dacryoadenitis and sialadenitis (also called Mikulicz disease) and type 1 autoimmune pancreatitis
-
The disease is associated with elevated serum levels of IgG4 and specific histopathological features, including abundant IgG4+ plasmacyte infiltration, and storiform fibrosis and obliterative phlebitis in the inflamed organs
-
IgG4-related disease is also associated with a predominantly type 2 T-helper-cell cytokine profile, and infiltration of regulatory T cells is considered to be involved in the disease pathogenesis
-
Comprehensive systemic and organ-specific diagnostic criteria have been defined for IgG4-related disease in Japanese populations, although criteria that classify the disease in other populations are not available at present
-
Examination for systemic organ failure and screening for underlying malignancies is important during the diagnosis and follow-up of IgG4-related disease
-
Glucocorticoids are effective in the treatment of IgG4-related disease, but the rate of relapse after tapering or discontinuing glucocorticosteroids is high
Abstract
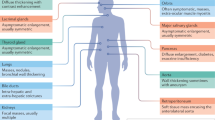
Recognition of IgG4-related disease as an independent chronic inflammatory disorder is a relatively new concept; previously, the condition was thought to represent a subtype of Sjögren's syndrome. IgG4-related disease is characterized by elevated serum levels of IgG4 and inflammation of various organs, with abundant infiltration of IgG4-bearing plasma cells, storiform fibrosis and obliterative phlebitis representing the major histopathological features of the swollen organs. The aetiology and pathogenesis of this disorder remain unclear, but inflammation and subsequent fibrosis occur due to excess production of type 2 T-helper-cell and regulatory T-cell cytokines. The disease can comprise various organ manifestations, such as dacryoadenitis and sialadenitis (also called Mikulicz disease), type 1 autoimmune pancreatitis, kidney dysfunction and lung disease. Early intervention using glucocorticoids can improve IgG4-related organ dysfunction; however, patients often relapse when doses of these agents are tapered. The disease has also been associated with an increased incidence of certain malignancies. Increased awareness of IgG4-related disease might lead to consultation with rheumatologists owing to its clinical, and potentially pathogenetic, similarities with certain rheumatic disorders. With this in mind, we describe the pathogenic mechanisms of IgG4-related disease, and outline considerations for diagnosis and treatment of the condition.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Stone, J. H., Zen, Y. & Desphande, V. IgG4-related disease. N. Engl. J. Med. 366, 539–551 (2012).
Uchida, K., Masamune, A., Shimosegawa, T. & Okazaki, K. Prevalence of IgG4-related disease in Japan based on nationwide survey in 2009. Int. J. Rheumatol. http://dx.doi.org/10.1155/2012/358371.
Kanno, A. et al. Nationwide epidemiological survey of autoimmune pancreatitis in Japan. Pancreas 41, 835–839 (2012).
von Mikulicz, J. Über eine eigenartige symmetrische Erkrankung der Tränen- und Mundspeicheldrüsen, in Beiträge zur Chirurgie: Festschrift gewidmet Theodor Billroth [German]. 610–630 (F. Enke, Stuttgart, 1892).
Mikulicz, J. Über eine eigenartige symmetrische Erkrankung der. Tränen und Mundspeicheldrüsen [German]. Med. Classics 2, 137–164 (1937).
Schaffer, A. J. & Jacobsen, A. W. Mikulicz's syndrome: a report of ten cases. Am. J. Dis. Child. 34, 327–346 (1927).
Sjögren, H. Zur Kenntnis der Keratoconjunctivitis Sicca. (Keratitis filiformis bei Hypofunktion der Tränendrüsen) [German]. Acta Ophthalmol. (Suppl. 2), 1–151 (1933).
Morgan, W. S. & Castleman, B. A clinicopathologic study of “Mikulicz's disease.” Amer. J. Pathol. 29, 471–503 (1953).
Morgan, W. S. The probable systemic nature of Mikulicz's disease and its relation to Sjögren syndrome. N. Engl. J. Med. 251, 5–10 (1954).
Yamamoto, M. et al. Elevated IgG4 concentrations in serum of patients with Mikulicz's disease. Scand. J. Rheumatol. 33, 432–433 (2004).
Yamamoto, M. et al. Clinical and pathological differences between Mikulicz's disease and Sjögren syndrome. Rheumatology (Oxford) 44, 227–234 (2005).
Yamamoto, M. et al. A new conceptualization for Mikulicz's disease as an IgG4-related plasmacytic disease. Mod. Rheumatol. 16, 335–340 (2006).
Sarles, H., Sarles, J. C., Muratore, R. & Guien, C. Chronic inflammatory sclerosis of the pancreas—an autonomous pancreatic disease? Am. J. Dig. Dis. 6, 688–698 (1961).
Case records of the Massachusetts General Hospital. Weekly clinicopathological exercises. Case 6–1982 A 55-year-old man with eight months of obstructive jaundice. N. Engl. J. Med. 306, 349–358 (1982).
Kawaguchi, K. et al. Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum. Pathol. 22, 387–395 (1991).
Toki, F. et al. An unusual type of chronic pancreatitis showing diffuse irregular narrowing of the entire main pancreatic duct on ERCP—A report of four cases. Endoscopy 24, 640 (1992).
Yoshida, K. et al. Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig. Dis. Sci. 40, 1561–1568 (1995).
Hamano, H. et al. High serum IgG4 concentrations in patients with screlosing pancreatitis. N. Engl. J. Med. 344, 732–738 (2001).
Hamano, H. et al. Hydronephrosis associated with retroperitoneal fibrosis and sclerosing pancreatitis. Lancet 359, 1403–1404 (2002).
Zamboni, T. et al. Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch. 445, 552–563 (2004).
Notohara, K., Burgart, L. J., Yadav, D., Chari, S. & Smyrk, T. C. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am. J. Surg. Pathol. 27, 1119–1127 (2003).
Park, D. H., Kim, M. H. & Chari, S. T. Recent advances in autoimmune pancreatitis. Gut 58, 1680–1689 (2009).
Yamamoto, M. et al. A case of Mikulicz's disease complicated by autoimmune pancreatitis, in which impaired glucose tolerance was improved by glucocorticoid treatment [Japanese]. Nihon Rinsho Meneki Gakkai Kaishi 28, 349–356 (2005).
Kamisawa, T. et al. A new clinicopathological entity of IgG4-related autoimmune disease. J. Gastroenterol. 38, 982–984 (2003).
Kamisawa, T. & Okamoto, A. Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J. Gastroenterol. 41, 613–625 (2006).
Yamamoto, M. et al. A new conceptualization for Mikulicz's disease as a Systemic IgG4-related Plasmacytic Syndrome (SIPS) [abstract]. Scand. J. Rheumatol. 37 (Suppl. 123), 38 (2008).
Masaki, Y. et al. Proposal for a new clinical entity, IgG4-positive multi-organ lymphoproliferative syndrome: Analysis of 64 cases of IgG4-related disorders. Ann. Rheum. Dis. 68, 1310–1315 (2009).
Umehara, H. et al. A novel clinical entity, IgG4-related disease (IgG4-RD): general concept and details. Mod. Rheumatol. 22, 1–14 (2012).
Umehara, H. et al. Comprehensive diagnostic criteria for IgG4-related disease (IgG4-RD), 2011. Mod. Rheumatol. 22, 21–30 (2012).
Stone, J. H. et al. Recommendations for the nomenclature of IgG4-related disease and its individual organ system manifestations. Arthritis Rheum. 64, 3061–3067 (2012).
Deshpande, V. et al. Consensus statement on the pathology of IgG4-related disease. Mod. Pathol. 25, 1181–1192 (2012).
Kawa, S. et al. HLA DRB10405-DQB10404 haplotype is associated with autoimmune pancreatitis in the Japanese population. Gastroenterology 122, 1264–1269 (2002).
Park, D. H. et al. Substitution of aspartic acid at position 57 of the DQβ1 affects relapse of autoimmune pancreatitis. Gastroenterology 134, 440–446 (2008).
Ota, M. et al. Two critical genes (HLA-DRB1 and ABCF1) in the HLA region are associated with the susceptibility to autoimmune pancreatitis. Immunogenetics 59, 45–52 (2007).
Umemura, T. et al. Genetic association of Fc receptor-like 3 polymorphisms with autoimmune pancreatitis in Japanese patients. Gut 55, 1367–1368 (2006).
Chang, M. C. et al. T-cell regulatory gene CTLA-4 polymorphism/haplotype association with autoimmune pancreatitis. Clin. Chem. 53, 1700–1705 (2007).
Umemura, T. et al. Association of autoimmune pancreatitis with cytotoxic T-lymphocyte antigen 4 gene polymorphisms in Japanese patients. Am. J. Gastroenterol. 103, 588–594 (2008).
Ota, M. et al. Polymorphism in the KCNA3 gene is associated with susceptibility to autoimmune pancreatitis in the Japanese population. Dis. Markers 31, 223–229 (2011).
Frulloni, L. et al. Identification of a novel antibody associated with autoimmune pancreatitis. N. Engl. J. Med. 361, 2135–2142 (2009).
Holtet, T. L. et al. Tetranectin, a trimeric plasminogen-binding protein C-type lectin. Protein Sci. 6, 1511–1515 (1997).
Watanabe, T. et al. Involvement of activation of Toll-like receptors and nucleotide-binding oligomerization domain-like receptors in enhanced IgG4 responses in autoimmune pancreatitis. Arthritis Rheum. 64, 914–924 (2012).
Watanabe, T. et al. Toll-like receptor activation in basophils contributes to the development of IgG4-related disease. J. Gastroenterol. 48, 247–253 (2013).
Kiyama, K. et al. Serum BAFF and APRIL levels in patients with IgG4-related disease and their clinical significance. Arthritis Res. Ther. 14, R86 (2012).
Tsuboi, H. et al. Analysis of IgG4 class switch-related molecules in IgG4-related diseases. Arthritis Res. Ther. 14, R171 (2012).
van der Zee J. S., van Swieten, P. & Aalberse, R. C. Inhibition of complement activation by IgG4 antibodies. Clin. Exp. Immunol. 64, 415–422 (1986).
Jefferis, R. in The Human IgG Subclasses (ed. Shakib, F.) 15–30 (Pergamon Press, Oxford, 1990).
Aalberse, R. C. & Schuurman, J. IgG4 breaking the rules. Immunology 105, 9–19 (2002).
Aalberse, R. C., Stapel, S. O., Schuurman, J. & Rispens, T. Immunoglobulin G4: an odd antibody. Clin. Exp. Allergy 39, 469–477 (2009).
van der Neut Kolfschoten, M. et al. Anti-inflammatory activity of human IgG4 antibodies by dynamic Fab arm exchange. Science 317, 1554–1557 (2007).
Ozdemir, C., Kucuksezer, U. C., Akdis, M. & Akidis, C. A. Mechanisms of immunotherapy to wasp and bee venom. Clin. Exp. Allergy 41, 1226–1234 (2011).
Kawa, S. et al. A novel immunoglobulin-immunoglobulin interaction in autoimmunity. PLoS ONE 3, e1637 (2008).
Takahashi H. et al. The immunology and clinical characteristics of IgG4-related diseases. J. Autoimmun. 39, 93–96 (2012).
Aparisi, L. et al. Antibodies to carbonic anhydrase and IgG4 levels in idiopathic chronic pancreatitis: relevance for diagnosis of autoimmune pancreatitis. Gut 54, 703–709 (2003).
Okazaki K. et al. Autoimmune-related pancreatitis is associated with autoantibodies and a TH1/TH2-type cellular immune response. Gastroenterology 118, 573–581 (2000).
Asada, M. et al. Identification of a novel autoantibody against pancreatic secretory trypsin inhibitor in patients with autoimmune pancreatitis. Pancreas 33, 20–26 (2006).
Zen, Y. et al. TH2 and regulatory immune reactions are increased in immunoglobulin G4-related sclerosing pancreatitis and cholangitis. Hepatology 45, 1538–1546 (2007).
Tanaka, A. et al. TH2 and regulatory immune reactions contribute to IgG4 production and the initiation of Mikulicz's disease. Arthritis Rheum. 64, 254–263 (2012).
Maehara, T. et al. Interleukin-21 contributes to germinal center formation and immunoglobulin G4 production in IgG4-related dacryoadenitis and sialoadenitis, so-called Mikulicz's disease. Ann. Rheum. Dis. 71, 2011–2019 (2012).
Nakashima, H. et al. An amplification of IL-10 and TGF-β in patients with IgG4-related tubulointerstitial nephritis. Clin. Nephrol. 73, 385–391 (2010).
Tsuboi, H. et al. Analysis of IgG4 class switch-related molecules in IgG4-related disease. Arthritis Res. Ther. 14, R171 (2012).
Yamamoto, M., Takahashi, H. & Shinomura, Y. Mikulicz's disease and the extraglandular lesions. Curr. Immunol. Rev. 7, 162–171 (2011).
Nakatani, K., Nakamoto, Y. & Togashi, K. Utility of FDG PET/CT in IgG4-related systemic disease. Clin. Radiol. 67, 297–305 (2012).
Cheuk, W., Yuen, H. K. & Chan, J. K. Chronic sclerosing dacryoadenitis: part of the spectrum of IgG4-related sclerosing disease? Am. J. Surg. Pathol. 31, 643–645 (2007).
Kitagawa, S. et al. Abundant IgG4-positive plasma cell infiltration characterizes chronic sclerosing sialadenitis (Küttner's tumor). Am. J. Surg. Pathol. 29, 783–791 (2005).
Shimizu, M. et al. Sonographic diagnosis for Mikulicz disease. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 108, 105–113 (2009).
Ito, T. et al. Characteristics of pancreatic diabetes in patients with autoimmune pancreatitis. J. Dig. Dis. 12, 210–216 (2011).
Irie, H. et al. Autoimmune pancreatitis: CT and MR characteristics. AJR Am. Roentgenol. 170, 1323–1327 (1998).
Yamamoto, M. et al. A case of Mikulicz's disease (IgG4-related plasmacytic disease) complicated by autoimmune hypophysitis. Scand. J. Rheumatol. 35, 410–411 (2006).
Chan, S. K., Cheuk, W., Chan, K. T. & Chan, J. K. IgG4-related screlosing pachymeningitis: a previously unrecognized form of central nervous system involvement in IgG4-related sclerosing disease. Am. J. Surg. Pathol. 33, 1249–1252 (2009).
Pasquali, T., Schoenfield, L., Spalding, S. J. & Singh, A. D. Orbital inflammation in IgG4-related sclerosing disease. Orbit 30, 258–260 (2011).
Sogabe, Y. et al. Pathological findings of intraorbital nerve enlargement in IgG4-related ophthalmic disease. Jpn. J. Ophthalmol. 56, 511–514 (2012).
Dahlgren, M., Khosroshahi, A., Nielsen, G. P., Deshpande, V. & Stone, J. H. Riedel's thyroiditis and multifocal fibrosclerosis are part of the IgG4-related systemic disease spectrum. Arthritis Care Res. (Hoboken) 62, 1312–1318 (2010).
Watanabe, T. et al. Clinical features of a new disease concept, IgG4-related thyroiditis. Scand. J. Rheumatol. 42, 325–330 (2013).
Tsushima, K. et al. Pulmonary involvement of autoimmune pancreatitis. Eur. J. Clin. Invest. 39, 714–722 (2009).
Matsui, S. et al. Immunoglogulin G4-related lung disease: clinicoradiological and pathological features. Respirology 18, 480–487 (2013).
Uchiyama-Tanaka, Y. et al. Acute tubulointerstitial nephritis associated with autoimmune-related pancreatitis. Am. J. Kidney Dis. 43, e18–e25 (2004).
Saeki, T. et al. Clinicopathological characteristics of patients with IgG4-related tubulointerstitial nephritis. Kidney Int. 78, 1016–1023 (2010).
Vaglio, A., Salvarani, C. & Buzio, C. Retroperitoneal fibrosis. Lancet 367, 241–251 (2006).
Zen, Y. et al. Retroperitonel fibrosis: a clinicopathological study with respected to immunoglobulin G4. Am. J. Surg. Pathol. 33, 1833–1839 (2009).
Kasashima, S. & Zen, Y. IgG4-related inflammatory abdominal aortic aneurysm. Curr. Opin. Rheumatol. 23, 18–23 (2011).
Chiba, K. et al. Clinical features of 10 patients with IgG4-related retroperitoneal fibrosis. Intern. Med. 52, 1545–1551 (2013).
Qian, Q., Kashani, K. B. & Miller, D. V. Ruptured abdominal aortic aneurysm related to IgG4 periaortitis. N. Engl. J. Med. 361, 1121–1123 (2009).
Yoshimura, Y. et al. IgG4-associated prostatitis complicating autoimmune pancreatitis. Intern. Med. 45, 897–901 (2006).
Sato, Y. et al. Systemic IgG4-related lymphadenopathy: a clinical and pathologic comparison to multicentric Castleman's disease. Mod. Pathol. 22, 589–599 (2009).
Deshpande, V. et al. Subclassification of Autoimmune pancreatitis: a histologic classification with clinical significance. Am. J. Surg. Pathol. 35, 26–35 (2011).
Zen, Y. & Nakanuma, Y. IgG4-related disease: a cross-sectional study of 114 cases. Am. J. Surg. Pathol. 34, 1812–1819 (2010).
Zen, Y. et al. Retroperitoneal fibrosis: a clinicopathologic study with respect to immunoglobulin G4. Am. J. Surg. Pathol. 33, 1833–1839 (2009).
Zen, Y. et al. IgG4-related lung and pleural disease: a clinicopathologic study of 21 cases. Am. J. Surg. Pathol. 33, 1886–1893 (2009).
Shrestha, B. et al. Distinctive pulmonary histopathology with increased IgG4-positive plasma cells in patients with autoimmune pancreatitis: report of 6 and 12 cases with similar histopathology. Am. J. Surg. Pathol. 33, 1450–1462 (2009).
Deshpande, V. et al. IgG4-associated cholangitis: a comparative histological and immunophenotypic study with primary sclerosing cholangitis on liver biopsy material. Mod. Pathol. 22, 1287–1295 (2009).
Cheuk, W. et al. Ocular adnexal lymphoma associated with IgG4+ chronic sclerosing dacryoadenitis: a previously undescribed complication of IgG4-related sclerosing disease. Am. J. Surg. Pathol. 32, 1159–1167 (2008).
Cornell, L. D. et al. Pseudotumors due to IgG4 immune-complex tubulointerstitial nephritis associated with autoimmune pancreatocentric disease. Am. J. Surg. Pathol. 31, 1586–1597 (2007).
Kasashima, S. et al. Inflammatory abdominal aortic aneurysm: close relationship to IgG4-related periaortitis. Am. J. Surg. Pathol. 32, 197–204 (2008).
Geyer, J. T. et al. Chronic sclerosing sialadenitis (Küttner tumor) is an IgG4-associated disease. Am. J. Surg. Pathol. 34, 202–210 (2010).
Shimizu, Y. et al. Necessity of early intervention for IgG4-related disease—delayed treatment induces fibrosis progression. Rheumatology (Oxford) 52, 679–683 (2013).
Yamamoto, M. et al. Value of serum IgG4 in the diagnosis of IgG4-related disease and in differentiation from rheumatic disease and other disease. Mod. Rheumatol. 22, 419–425 (2012).
Yamamoto, M. et al. Analysis of serum IgG subclasses in Churg–Strauss syndrome—the meaning of elevated serum levels of IgG4. Intern. Med. 49, 1365–1370 (2010).
Sato, Y. & Yoshino, T. IgG4-Related Lymphadenopathy. Int. J. Rheumatol. http://dx.doi.org/10.1155/2012/572539.
Kamisawa, T. et al. Pancreatic cancer with a high serum IgG4 concentration. World J. Gastroenterol. 14, 6225–6228 (2006).
Shimosegawa, T. et al. The amendment of the Clinical Diagnostic Criteria in Japan (JPS2011) in response to the proposal of the International Consensus of Diagnostic Criteria (ICDC) for autoimmune pancreatitis. Pancreas 41, 1341–1342 (2012).
Kawano, M. et al. Proposal for diagnostic criteria for IgG4-related kidney disease. Clin. Exp. Nephrol. 15, 615–626 (2011).
Ohara, H. et al. Clinical diagnostic criteria of IgG4-related sclerosing cholangitis 2012. J. Hepatobilliary Pancreat. Sci. 19, 536–542 (2012).
Chari, S. T. et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin. Gasrtroenterol. Hepatol. 4, 1010–1016 (2006).
Kwon, S., Kim, M. H. & Choi, E. K. The diagnostic criteria for autoimmune chronic pancreatitis: it is time to make a consensus. Pancreas 34, 279–286 (2007).
Otsuki, M. et al. Asian diagnostic criteria for autoimmune pancreatitis: consensus of the Japan–Korea Symposium on Autoimmune Pancreatitis. J. Gastroenterol. 43, 403–408 (2008).
Shimosegawa, T. et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas 40, 352–358 (2011).
Raissaian, Y. et al. Diagnosis of IgG4-related tubulointerstitial nephritis. J. Am. Soc. Nephrol. 22, 1343–1352 (2011).
Yamamoto, M. et al. Beneficial effects of steroid therapy for Mikulicz's disease. Rheumatology (Oxford) 44, 1322–1323 (2005).
Nishimori, I. et al. Influence of steroid therapy on the course of diabetes mellitus in patients with autoimmune pancreatitis: findings from a nationwide survey in Japan. Pancreas 32, 244–248 (2006).
Yamamoto, M. et al. Relapse patterns in IgG4-related disease. Ann. Rheum. Dis. 71, 1755 (2012).
Takahashi, H. et al. Long-term follow-up of IgG4-related disease presenting with lacrimal and salivary gland involvement [abstract 1917]. Arthritis Rheum. 64 (Suppl. 10), S814 (2012).
Matsushita, M., Ikeura, T., Fukui, T., Uchida, K. & Okazaki, K. Refractory autoimmune pancreatitis: azathioprine or steroid pulse therapy? Am. J. Gastroenterol. 103, 1834 (2008).
Khosroshahi, A. et al. Rituximab for the treatment of IgG4-related disease: lessons from 10 consecutive patients. Medicine (Baltimore) 91, 57–66 (2012).
Murakami, J. et al. Recurrence of IgG4-related disease following treatment with rituximab. Mod. Rheumatol. http://dx.doi.org/10.1007/s10165-012-0738-2.
Yamamoto, M. et al. Efficacy of rituximab and other immunosuppressants for IgG4-related disease [abstract]. Ann. Rheum. Dis. 71 (Suppl. 3), 290 (2012).
Hart, P. A. et al. Long-term outcomes of autoimmune pancreatitis: a multicenter, international analysis. Gut http://dx.doi.org/10.1136/gutjnl-2012-303617.
Shiokawa, M. et al. Risk of cancer in patients with autoimmune pancreatitis. Am. J. Gastroenterol. 108, 610–617 (2013).
Yamamoto, M. et al. Risk of malignancies in IgG4-related disease. Mod. Rheumatol. 22, 414–418 (2012).
Author information
Authors and Affiliations
Contributions
M. Yamamoto researched the data for the article, decided on the content and wrote the manuscript. H. Takahashi and Y. Shinomura made substantial contributions to review/editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Yamamoto, M., Takahashi, H. & Shinomura, Y. Mechanisms and assessment of IgG4-related disease: lessons for the rheumatologist. Nat Rev Rheumatol 10, 148–159 (2014). https://doi.org/10.1038/nrrheum.2013.183
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2013.183
This article is cited by
-
IgG4 related pericardium and lung disease in pediatric patient complicated with fatal massive hemoptysis: a case report and review of literature
Pediatric Rheumatology (2023)
-
The differential diagnosis of IgG4-related disease based on machine learning
Arthritis Research & Therapy (2022)
-
New biomarkers for the diagnosis of pleural effusion
The Egyptian Journal of Bronchology (2022)
-
Pathogenic roles and therapeutic potential of the CCL8–CCR8 axis in a murine model of IgG4-related sialadenitis
Arthritis Research & Therapy (2021)
-
Congruent microbiome signatures in fibrosis-prone autoimmune diseases: IgG4-related disease and systemic sclerosis
Genome Medicine (2021)