Abstract
The aim of this study was to analyze the Furin–TNF-α-converting enzyme (TACE)–amphiregulin (AREG)-IL-6/IL-8 secretion pathway in non-neoplastic human salivary gland epithelial cells (SGECs) stimulated with anti-Ro/SSA autoantibodies (Abs). We examined whether anti-Ro/SSA Abs-mediated TACE activation is responsible for AREG activation. As recent studies have demonstrated that AREG could induce proinflammatory cytokines secretion in epithelial cells, we discuss how TACE-mediated AREG shedding, caused by anti-Ro/SSA Abs treatment, could have a critical role in TNF-α-induced IL-6 and IL-8 secretion by SGEC. Furthermore, the effects of TNF-α blockade on AREG expression and TNF-α–AREG-mediated IL-6 and IL-8 secretion were evaluated. We have discovered that the upregulation of AREG occurs through TNF-α produced after anti-Ro/SSA Abs uptake via Fcγ receptors. Biological drug adalimumab and the gene silencing technique were used to study the AREG–IL-6/IL-8 secretion pathway, demonstrating that (i) adalimumab-mediated TNF-α blocking and TNF -α gene silencing provoke a significant decrease of proinflammatory cytokines production and AREG expression in anti-Ro/SSA Abs-treated SGEC; (ii) AREG gene silencing has a potent inhibitory effect on TNF-α-induced IL-6 and IL-8 secretion in SGEC treated with anti-Ro/SSA Abs; (iii) an inspection of the kinetics of cytokine production after exogeni TNF-α and AREG addition, and the use of cycloheximide in the presence of exogenous TNF-α as stimulant, clarified that TNF-α induces IL-6 and IL-8 secretion through AREG.
Similar content being viewed by others
Main
Cytokines have a central role in the regulation of immunity and dysregulation of the cytokine network contributes to both systemic and exocrine manifestations of Sjögren's syndrome (SS), a systemic chronic inflammatory autoimmune disorder, that affects secretory organs such as the salivary and lachrymal glands.1 Proinflammatory cytokines, most notably interleukin (IL)-6, IL-8 and tumor necrosis factor (TNF)-α have been found in functionally and structurally damaged areas of the salivary glands and have been implicated in the disease pathogenesis.2, 3, 4, 5, 6
Anti-TNF-α agents have been successfully introduced for the treatment of chronic inflammatory diseases and the strategies to block TNF-α have revolutionized the therapeutic approaches.7 Among the biological agents that neutralise the activity of TNF-α, adalimumab (Humira; Abbott Laboratories) is the first fully human (100% human peptide sequences) therapeutic monoclonal antibody (mAb) that blocks TNF-α and is currently being evaluated as clinical trial.7, 8, 9 The impaired interaction with receptors prevents TNF-α-mediated cellular responses and modulates the activity of other TNF-α-regulated proinflammatory cytokines.7
The membrane bound precursor of TNF-α is processed to the soluble active component by the metalloproteinase TNF-α-converting enzyme (TACE).10, 11 The essential step for the activation of TACE is proteolytic processing by Furin, a proprotein convertase, at a characteristic motif, which is located between the prodomain and the metalloproteinase domain.12 Extensive in vitro data indicate that various members of the ADAMs family of cell surface enzymes, including TACE, are responsible for the release of epidermal growth factor receptor (EGFR) ligands, as amphiregulin (AREG).13, 14, 15 AREG is synthesized as membrane-bound precursor that requires metalloproteinase-mediated proteolytic cleavage to produce the soluble, mature form,16 and is expressed from a variety of cells including human keratinocytes.17, 18, 19
Various reports have shown that AREG enhances the production of several proinflammatory cytokines,20, 21, 22 and, recently, it was demonstrated that TACE-mediated AREG shedding may have a critical role in the secretion of proinflammatory cytokines by human epithelial cells induced by TNF-α.20, 23
We previously demonstrated a dose-dependent increase of TACE expression in anti-Ro/SSA Abs-treated human salivary gland epithelial cells (SGEC) followed by internalization, prodomain shedding and activation of TACE protein. Adalimumab treatment brought TACE expression to levels than those observed in untreated SGEC, suggesting that this biological drug could be efficacious in preventing TACE activation caused by anti-Ro/SSA Abs.24, 25, 26
Our present hypothesis explores first, whether anti-Ro/SSA Abs-mediated TACE activation is responsible for AREG activation. As recent studies have demonstrated that AREG could induce proinflammatory cytokines secretion in epithelial cells,20, 21, 22 as second step, we discuss how TACE-mediated AREG shedding, caused by anti-Ro/SSA Abs treatment, could have a critical role in TNF-α-induced IL-6 and IL-8 secretion by SGEC. Finally, we evaluate the effect of adalimumab and gene silencing on AREG expression and on TNF-α-AREG-mediated proinflammatory IL-6 and IL-8 secretion.
MATERIALS AND METHODS
Autoantibodies
Anti-Ro/SSA antibodies are found in ∼80% of patients with SS and anti-La/SSB antibodies are present in approximately 40% of patients with SS. As these autoantibodies have the same effects on SGEC,27, 28, 29, 30, 31, 32 we choose to use in this study anti-Ro/SSA Abs because they were isolated more easily from SS sera. Anti-Ro/SSA Abs were purified from a pool of Sjögren IgG fractions obtained from 20 ml of sera of 25 SS patients (n=25; mean age 48.3 years). All patients fulfilled the American–European Consensus Group Classification criteria for SS.33 None of the patients examined met the clinical or serological criteria for additional connective tissue disease. None of the patients suffered from acute viral or bacterial infections at the time of the study. Informed consent for studies involving human subjects was obtained and the studies were conducted according to the tenets of the Declaration of Helsinki.
Anti-Ro/SSA Abs were purified using human Ro/SSA antigen–Sepharose 4B affinity columns as described.34 The Abs obtained were concentrated to 200 μg/ml by the ultrafiltration method and used at concentrations of 50 μg/ml in the experimental procedures. The experiments carried out were repeated for the number indicated in the figure legends. Autoantibodies preparations resulted free of endotoxin contamination, as assessed by a Limulus amebocyte assay (Sigma, St Louis, MO, USA). IgG from healthy subjects (HIgG) were obtained from control asymptomatic volunteers (n=27; mean age 43.7 years).
Microdissection and Primary Explant Culture
Cultures of salivary gland epithelial cells (SGEC) were derived from labial minor salivary gland (LSG) biopsies obtained from 12 healthy individuals awaiting removal of salivary mucoceles from the lower lip. Informed consent from the patients and approval by the local ethics committee were obtained. The HIgG had no complaints of oral dryness, no autoimmune disease and normal salivary function. Labial minor glands were harvested from the lower lip under local anesthesia through normal mucosa. The explant outgrowth technique35 was applied to establish SGEC cultures from limited amounts of glandular tissue. The cells were isolated from the labial glands by microdissection and collagenase (Worthington Diagnostic Division, Millipore, freehold, NJ, USA) digestion in physiological saline containing 1 mm Ca2+. After dispersal, cells were resuspended in McCoy's 5a modified medium supplemented with 10% fetal bovine serum, 1% antibiotic solution, 2 mM L-glutamine, 20 ng/ml epidermal growth factor (EGF, Promega, Madison, WI, USA), 0.5 μg/ml insulin (Novo, Bagsvaerd, Denmark) and incubated at 37°C, 5% CO2 in air. Contaminating fibroblasts were selectively removed by treatment of the cultures with 0.02% EDTA. The epithelial origin of cultured cells was routinely confirmed by staining with mAbs against epithelial-specific markers, including the various cytokeratins and epithelial membrane antigens and the absence of myoepithelial, fibroblastoid and lymphoid markers, using immunocytochemistry as previously described.36, 37
Evaluation of Furin, TACE and AREG Expression
Cell Treatment
SGEC were collected from culture media by centrifugation at 250 × g and resuspended at 1 × 106 cells/ml in McCoy's 5a modified medium. Cell suspensions (105 cells/well) were added to each well of a six-well plate (Thomas Scientific, Swedesboro, NJ, USA) and allowed to incubate for 24 h at 37°C under 5% CO2. After incubation, cells were washed and treated as follows: (1) IgG fractions extracted from sera of healthy donors dissolved in McCoy's 5a (HIgG, 50 μg/ml) for 48 h; (2) anti-Ro/SSA Abs (50 μg/ml) dissolved in McCoy's 5a for 48 h; (3) exogenous TNF-α (500 pg/ml) for 8–72 h; (3) exogenous AREG (700 pg/ml) for 8–72 h; (4) pre-treatment with protein synthesis inhibitor cycloheximide (CHX; 10 ìg/ml) for 30 min followed by exogenous TNF-α (500 pg/ml) addition for 48 h.
Gene Expression Analysis
To determine the TACE, Furin and AREG mRNA expression, total RNA was extracted from variously treated SGEC using the TRI reagent (Sigma). We treated 2 μg of RNA with DNase I (GIBCO, Life Technologies, Carlsbad, CA, USA) before the reverse transcription with Moloney murine leukemia virus reverse transcriptase (GIBCO) in the presence of RNaseOUT (GIBCO) and used 1/10 of cDNA preparation for each PCR. PCR was performed in a 50-μl reaction mixture composed of 2 μ M of each sense and antisense primer, 1 × PCR buffer, 2.4 mM MgCl2, 0.2 mM each dNTP, 10 μl of transcribed cDNA and 0.04 U/μl Taq DNA polymerase. After initial denaturation at 94°C for 5 min, 35 cycles were performed (denaturation at 94°C for 30 s, annealing at 62°C for 30 s, 58°C for 30 s and 59°C for 30 s, respectively, for Furin, TACE and AREG, and extension at 72°C for 1 min) followed by 10 min at 72°C. Equal amounts of PCR products were run on a 1.5% agarose gel containing ethidium bromide. The expected size of PCR products is 480 bp for GADPH, 210 bp for Furin, 295 bp for TACE and 495 bp for AREG. See the list of PCR primers designed according to published sequences (reference source: http://www.ncbi.nlm.nih.gov) in the Table 1.
Sequencing and Sequence Analysis
Densitometric analysis, performed by gel image software (Bio-Profil Bio-1D; ltf Labortechnik GmbH, Wasserburg, Germany), was carried out to quantify mRNA expression levels by determining the intensity values for each band relative to GADPH (internal control for lane loading). Results were averaged from five sets of independent experiments and expressed as arbitrary units. The identity of each PCR product was confirmed by the size and by direct sequencing of the amplified cDNA eluted from the gel.
Quantitative Real-Time PCR Assay
Total RNA from cultured cells were prepared and reverse transcription was conducted as described above. TaqMan expression assays, including fluorescent probes, forward and reverse primers for human TACE, Furin and AREG (Assays-On-Demand, Applied Biosystems, Foster City, CA, USA), and the internal control gene β-2 microglobul (part n°4326319E; β2M) were purchased from Applied Biosystems. All other reagents used in real-time PCR assays were purchased from the same manufacturer. Real-time quantitative PCR was performed in a 96-well microtiter plate with an ABI PRISM 7700 (Applied Biosystems). Each reaction contained 5 μl of cDNA template, 2.5 μl of 20 × probes and primers mixture, 12.5 μl of TaqMan Universal PCR Master Mix, No AmpErase UNG (Applied Biosystems), in a total volume of 25 μl. Reactions were amplified for 40 cycles (65°C for 5 min and 95°C for 10 min, followed by 40 denaturation cycles at 95°C for 15 s and annealing/extension at 60°C for 30 s, 58°C for 30 s and 58°C for 1 min, respectively, for Furin, TACE and AREG). The threshold was determined as 10 times the s.d. of the baseline fluorescence signal. The cycle number at the threshold was used as the threshold cycle (Ct). The different expression of mRNA in untreated and treated samples was deducted from 2−ΔΔCt where ΔΔCt=ΔCt anti-Ro/SSA Abs treated cells—ΔCt untreated cells/HIgG-treated cells.
Proteins Expression Analysis
Furin, TACE and AREG protein levels were determined in treated and untreated control cells. We adopted two approaches to investigate proteins expression in SGEC, in the absence or presence of anti-Ro/SSA Abs stimulation, western blot and flow cytometry. For western blot, SGEC were washed twice, detached, collected and centrifuged at 600 × g for 10 min. The supernatant was removed and the pellet was incubated with lysis buffer (1% (v/v) Triton X-100, 20 mM Tris-HCl, 137 mM NaCl, 10% (v/v) glycerol, 2 mM EDTA, 1 mM phenylmethylsulfonyl fluoride, 20 μ M leupeptin hemisulfate salt, 0.2 U/ml aprotinin) for 30 min on ice. After incubation, the obtained lysates were centrifuged at 12 800 × g for 10 min; the protein concentration in the supernatant was spectrophotometrically determined by Bradford's protein assay, and the lysates were subjected to SDS-polyacrylamide gel electrophoresis. Proteins (25 μg/lane) and prestained standards (BioRad Laboratories, Hercules, CA, USA) were loaded on 10% SDS-polyacrylamide precast gels. After electrophoresis, the resolved proteins were transferred from gel to nitrocellulose membranes. A blot buffer (20 mM Tris/150 mM glycine, pH 8, 20% (v/v) methanol) was used for gel and membrane saturation and blot. The blot conditions were the following: 200 mA (constant amperage), 200 V for 110 min. Blots were then blocked by phosphate-buffered saline (PBS) pH 7.2 with 0.1% (v/v) Tween-20, 5% w/v non-fat dried milk for 1 h and washed three times with 0.1% (v/v) Tween-20 PBS 1 × . Membranes were incubated for 90 min with rabbit anti-human Furin polyclonal antibody (pAb), goat anti-human TACE pAb (both from Santa Cruz Biotechnology, Santa Cruz, CA, USA), mouse anti-human AREG mAb (R&D Systems, Minneapolis, MN USA), and for 30 min with the relative secondary antibodies-HRP conjugates (Santa Cruz Biotechnology). Proteins recognized by the antibodies were revealed using chemoluminescence luminal reagent (Santa Cruz Biotechnology) according to the protocol. The β-actin protein level was determined by western blot and used as protein loading control. Flow cytometric analysis was performed to reveal Furin, intracellular active TACE, and AREG in treated and untreated SGEC. SGEC were incubated with anti-human Furin–phycoerythrin (PE) mAb, anti-human TACE-PE mAb and biotinylated anti-human amphiregulin antibody (from R&D Systems). For AREG detection streptavidin-RPE (STAR4A, Serotec, Oxford, UK) was used. Proteins expression was analyzed by a Becton Dickinson (BD, Becton Dickinson, Germany) FACSCanto II flow cytometer and BD FACS Diva software. Values are given as percentages of positive cells.
Enzyme-Linked Immunosorbent Assay (ELISA) Method for the Quantification of Shedded AREG
ELISA on conditioned medium was carried on cells grown in six-well plates. An AREG DuoSet ELISA from R&D Systems was used to measure AREG mean concentrations. High-binding ELISA plates were coated with 3 μg/ml MAB262 monoclonal AREG antibody in sterile PBS overnight at room temperature. Absorbance was measured on a VERSAmax microplate reader (Molecular Devices, Silicon Valley, CA, USA). Sampling was carried out in triplicate.
Proinflammatory Cytokines Determinations
Il-6 and Il-8 levels were determined in treated and untreated cells. We adopted RT-PCR, real-time PCR, ELISA and western blot to investigate cytokines expression in SGEC. For RT-PCR, after the initial denaturation at 94°C for 5 min, 35 cycles were performed (denaturation at 94°C for 30 s, annealing at 60°C for 30 s, 59°C for 30 s, respectively, for IL-6 and IL-8, and extension at 72°C for 1 min) followed by 10 min at 72°C. Equal amounts of PCR products were run on a 1.5% agarose gel containing ethidium bromide. The expected size of PCR products is 398 bp for IL-6, and 300 bp for IL-8. See the list of PCR primers in the Table 1. Real-time PCR was performed as described above. For amplification 40 cycles (65°C for 5 min and 95°C for 10 min, followed by 40 denaturation cycles at 95°C for 15 s and annealing/extension at 62°C and 58°C for 1 min, respectively, for Il-6 and IL-8) were performed. The different expression of cytokines mRNA in untreated and treated samples was deducted from 2−ΔΔCt where ΔΔCt=ΔCt anti-Ro/SSA Abs treated cells—ΔCt untreated cells/HIgG treated cells. The culture supernatants from cells maintained for 48 h in the absence or presence of anti-Ro/SSA Abs (50 μg/ml) were tested for IL-6 and IL-8 protein concentrations using commercial ELISA kits (R&D Systems). Each measurement was performed in triplicate, and the average value was recorded as pg/ml. The detection level was 0.70 pg/ml for IL-6 and, for IL-8, ranged from 1.5–7.5 pg/ml. For western blot, membranes were incubated with mouse anti-human IL-8 mAb and mouse anti-human IL-6 mAb (both from R&D systems), and with the relative secondary antibodies-HRP conjugates (Santa Cruz Biotechnology). The β-actin protein level was used as protein loading control.
Evaluation of Fcγ Receptors Block Effect on ProInflammatory Cytokines Production
To examine the role of Fcγ receptors on IL-6 and IL-8 production induced by anti-Ro/SSA Abs, SGEC were treated with Fc fragments from human IgG (Chemicon, Temecula, CA, USA) at a concentration of 200 μg/ml for 2 h at 37°C, to block Fcγ receptors. At the end of the incubation period, anti-Ro/SSA (50 μg/ml) were added and the cells were incubated for 48 h. The culture supernatants were tested for IL-6 and IL-8 protein concentrations using commercial ELISA kits (R&D Systems). Each measurement was performed in triplicate, and the average value was recorded as pg/ml. The detection level was 0.70 pg/ml for IL-6 and, for IL-8, ranged from 1.5–7.5 pg/ml.
TNF-α and AREG Synthesis Inhibition
First we used a biological drug to inhibit TNF-α production by anti-Ro/SSA Abs treated-SGEC as the following treatment: anti-Ro/SSA autoAbs (50 μg/ml) plus adalimumab (50 μg/ml) for 48 h. Second, for TNF-α and AREG genes silencing in SGEC, transfection of 21-nucleotide siRNA duplexes (Ambion, Austin, TX, USA) was carried out. Briefly, SGEC cultured in McCoy's 5a modified medium were transfected with siRNA for TNF-α and AREG using the siPORT NeoFX transfection agent (Ambion). The siRNAs were mixed and diluted in OPTI-MEM1 medium to a final concentration of 30 nM/well. siRNA/transfection agent was dispensed into culture plates as directed by the manufacturer. The highest efficiencies in silencing target genes were obtained by using mixtures of siRNA duplexes targeting different regions of the genes of interest. A positive control using GAPDH siRNA (Ambion) and a negative control with no known sequence similarity to human genes, were included. Silencing was observed by mRNA quantification.
Kinetics of Proinflammatory Cytokine Production
For the study of kinetics of IL-6 and IL-8 production, cell-free supernatants were collected after SGEC had been stimulated with exogenous TNF-α (Sigma) and exogenous AREG (Sigma) for 8, 16, 24, 48, 72 h. Stimulating concentrations used in experiments were: TNF-α, 500 pg/ml and AREG, 700 pg/ml. The culture supernatants were tested for IL-6 and IL-8 protein concentrations using commercial ELISA kits as above described.
Statistics
The data were analyzed for normality using the Wilks Shapiro Test. Differences in means for paired observations were analysed by Student's t-test. In all instances values of P<0.05 were considered statistically significant.
RESULTS
Furin, TACE and AREG Genes are Overexpressed in Anti-Ro/SSA Abs-Treated SGEC
The expression of Furin, TACE and AREG genes was studied by semiquantitative RT-PCR and real-time PCR. Primary human SGEC cultures, established from biopsies of LSG, were treated with human anti-Ro/SSA Abs (50 μg/ml) for a period of 48 h. As shown in Figure 1a, after anti-Ro/SSA treatment, a clear upregulation of Furin, TACE and AREG gene expression was observed. As depicted in Figure 1b, densitometric analysis, normalized against that of GADPH, revealed that in anti-Ro/SSA Abs-treated cells, the expression of Furin was upregulated about 2.5-fold, the expression of TACE increased remarkably of about 2.8-fold and AREG gene expression increased about 3.2-fold in comparison with untreated control cells. The upregulation of each gene was statistically significant (P<0.01).
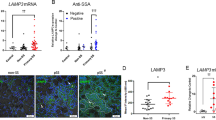
Semiquantitative RT-PCR and real-time PCR for Furin, TACE and AREG genes expression. (a) RT-PCR analysis of Furin, TACE and AREG mRNA extracted from SGEC treated with anti-Ro/SSA autoantibodies. M, marker; control, untreated SGEC; HIgG, SGEC treated with IgG fractions extracted from sera of healthy donors; anti-Ro, SGEC treated with anti-Ro/SSA autoantibodies. RT-PCR of GADPH was used as control. Band intensities were analyzed by densitometry (b). (c) Real-time PCR for Furin, TACE and AREG genes expression. Representative histograms of mRNA levels of Furin, TACE and AREG in untreated SGEC (control), SGEC treated with healthy IgG (HIgG), anti-Ro/SSA autoantibodies (anti-Ro). The mRNA levels of the housekeeping gene, β-2 microglobulin, were quantified between untreated control cells and variously treated cells (data represent the mean±s.e. of five independent experiments).
These changes are in agreement with results monitored by real-time PCR (Figure 1c, that showed a significant increase (P<0.01) of the mRNA expression of Furin, TACE and AREG in anti-Ro/SSA Abs-treated cells (2.8±1.2, 2.76±0.3 and 2.9±0.3 times, respectively) when compared with those in control/HIgG-treated SGEC. No differences in the relative gene expression were detectable between untreated control SGEC and SGEC treated with IgG extracted from sera of healthy donors (healthy IgG).
Anti-Ro/SSA Abs Induce Furin Overexpression Correlated with TACE and AREG Activation
Representative images obtained from flow cytometry of SGEC exposed to 50 μg anti-Ro/SSA Abs are shown in Figure 2a. The expression of Furin (panel A) was increased from 50.8%±1.7 of the control value to 94.4%±1.4 (P<0.01) of treated SGEC. Simultaneously, intracellular TACE expression analysis (panel B) revealed that after anti-Ro/SSA Abs treatment, an increase of intracellular TACE (98%±1.56 versus 69.4%±1.94 for untreated control cells) was observed (P<0.01). The expression of AREG (panel C) followed a similar trend (25%±1.3 for untreated control SGEC versus 68%±1.5 for anti-Ro/SSA Abs-treated SGEC, P<0.01). Western blot analysis (Figure 2b) provided results largely in accordance to those of flow cytometric analysis. In the western blot of Furin, the band appeared at a little over 97 kDa. Figure 2 illustrates the significant accumulation of Furin protein in response to anti-Ro/SSA Abs after 48 h of stimulation. This result indicates that Furin can be induced by autoantibodies at both the mRNA and the protein level. For the TACE protein, anti-Ro/SSA Abs treatment induces the appearance of a TACE processed form devoid of the prodomain (80 kDa). Western blot analysis, performed with a biotinylated affinity-purified anti-human AREG antibody on SGEC lysates, allowed us to detect a band of 50 kDa corresponding to the form of AREG described in epithelial cells.38 In concordance with the upregulation of AREG mRNA levels, in anti-Ro/SSA Abs-treated SGEC, a significant increase of AREG band intensity was observed in comparison with untreated control SGEC and SGEC treated with HIgG. Then, we analysed whether the upregulation of AREG gene and protein expression in anti-Ro/SSA Abs-treated SGEC translates into an increased quantity of active shedded AREG. To detect secreted (shedded) AREG, we used an AREG-specific ELISA. The results showed a strong increase in the concentration of secreted AREG as a response to autoantibodies treatment (Figure 2c). Our results showed that SGEC secrete 600 pg/ml AREG into the medium/105 cells after a 48 h period of treatment with anti-Ro/SSA Abs. Taken together, these data underlined that AREG is overexpressed at the message level as well as the membrane and secreted protein levels in anti-Ro/SSA Abs-treated SGEC.
Analysis of Furin, TACE and AREG expression in anti-Ro/SSA Abs-treated SGEC. (a) Flow cytometric analysis of Furin, TACE and AREG expression in SGEC after anti-Ro/SSA Abs treatment. Examples of flow cytometric images from one representative experiment. (A) Furin expression analysis in untreated and anti-Ro/SSA or HIgG-treated SGEC; (B) intracellular active TACE expression analysis in untreated and anti-Ro/SSA or HIgG-treated SGEC; (C) AREG expression analysis in untreated and anti-Ro/SSA or HIgG-treated SGEC. (b) Western blot analysis of Furin, TACE and AREG proteins expression in SGEC treated or not with anti-Ro/SSA. Immunoblotting gave rise to bands of the expected size (97 kDa for Furin, 80 kDa for active TACE and 50 kDa for AREG). β-Actin was used as protein loading control. (c) Detection of soluble AREG by ELISA. Secreted AREG was detected by ELISA in the conditioned medium. Control, untreated SGEC; HIgG, SGEC treated with IgG fractions extracted from sera of healthy donors; anti-Ro, SGEC treated with anti-Ro/SSA autoantibodies. (Data represent the mean±s.e. of four independent experiments).
Anti-Ro/SSA-Dependent IL-6 and IL-8 Production
The levels of IL-6 and IL-8 genes transcription were analyzed by RT-PCR and real-time PCR. Figure 3a and b showed that anti-Ro/SSA Abs induced SGEC to express high levels of mRNA that encode proinflammatory cytokines IL-6 and IL-8. No IL-6 and IL-8 genes expression was detectable in untreated control SGEC or in SGEC treated with HIgG. We then evaluated whether the protein level was also raised. To measure IL-6 and IL-8 production, cytokines were quantified by a specific ELISA (Figure 3d). As for gene expression, autoantibodies tested determined IL-6 and IL-8 production by SGEC. Western blot (Figure 3c) analysis performed with a biotinylated affinity-purified anti-human IL-6 and IL-8 antibodies on anti-Ro/SSA treated SGEC lysates allowed us to detect a band of 28 kDa for IL-6 and a band of 64 kDa for IL-8, whereas no bands were observed in unstimulated SGEC or in HIgG-stimulated SGEC. To demonstrate that the IL-6 and IL-8 production occurs through the anti-Ro/SSA uptake via the Fcγ receptors, SGEC were pretreated with the Fc fragment of IgG to block Fcγ receptors. ELISA assay (Figure 4a and b) demonstrated that the addition of the exogenous Fc fragment determines a reduction of proinflammatory cytokines release by anti-Ro/SSA-treated SGEC.
Induction of mRNA expression and release of IL-6 and IL-8 from SGEC. SGEC were exposed to 50 ìg/ml of anti-Ro/SSA Abs for 48 h. Control, untreated SGEC; HIgG, SGEC treated with IgG fractions extracted from sera of healthy donors; anti-Ro, SGEC treated with anti-Ro/SSA autoantibodies. (a) RT-PCR analysis of IL-6 and IL-8 mRNA extracted from untreated SGEC or SGEC treated with anti-Ro/SSA autoantibodies/HIgG. M, marker; RT-PCR of GADPH was used as control. (b) Real-time PCR for IL-6 and IL-8 genes expression. The mRNA levels of the housekeeping gene, β-2 microglobulin, were quantified between untreated control cells and cells variously treated. (c) Western blot analysis of IL-6 and IL-8 proteins expression in SGEC treated or not with anti-Ro/SSA. Immunoblotting revealed bands of 28 kDa and 64 kDa, respectively, for IL-6 and IL-8. β-actin was used as protein loading control (43 kDa). (d) SGEC Il-6 and IL-8 release detected by specific ELISA assays. (Data represent the mean±s.e. of five independent experiments).
Effect of Fcγ receptors block by Fc fragments from human IgG on IL-6 and IL-8 secretion. Pretreatment of SGEC with Fc fragments from human IgG decreases the concentration of IL-6 (a) and IL-8 (b) induced by anti-/Ro/SSA Abs measured by ELISA assay. Control, untreated SGEC; anti-Ro, SGEC treated with anti-Ro/SSA autoantibodies; anti-Ro+Fc, SGEC treated with anti-Ro/SSA autoantibodies plus Fc fragments from human IgG. (Data represent the mean±s.e. of three independent experiments).
TNF-α Block by Adalimumab and Gene Silencing Affects AREG Expression and IL-6 and IL-8 Secretion
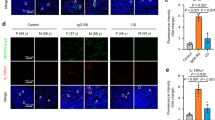
In many cases, in which epithelial cells produce cytokines, their levels of production may be much increased after exposure to other cytokines.39 To study the involvement of TNF-α in IL-6 and IL-8 secretion from anti-Ro/SSA Abs-treated SGEC and the potential therapeutic effect of adalimumab on proinflammatory cytokines secretion we added adalimumab to anti-Ro/SSA-treated SGEC to block TNF-α. When SGEC were treated with anti-Ro/SSA Abs plus adalimumab a notably decreased of IL-6 and IL-8 secretion was observed and the levels were reported to that observed in untreated SGEC (Figure 5a). To confirm data obtained with adalimumab addition, we used the siRNA-mediated gene silencing technique. We used siRNA to knock down the expression of TNF-α (Figure 5b and c) and evaluate the effects on IL-6 and IL-8 production. ELISA assay (Figure 5d) demonstrated that TNF-α gene silencing caused a significant decrease (P<0.05) of cytokines production.
Effect of TNF-α block by adalimumab and gene silencing on AREG expression and IL-6 and IL-8 secretion. (a) ELISA analysis of IL-6 and IL-8 secretion in SGEC after anti-Ro/SSA Abs plus Adalimumab treatment. (b) SGEC were transfected with TNF-α siRNA. TNF-α gene expression was measured by semiquantitative RT-PCR. Negative, negative controls with sequence similarity to no known human; anti-Ro, TNF-α mRNA production in anti-Ro/SSA Abs treated SGEC; anti-Ro+TNF-α siRNA, TNF-α gene silencing in anti-Ro/SSA Abs treated SGEC; mRNA expression of the housekeeping gene, GADPH, was used as internal control. (c) PCR products were densitometrically analyzed after standardizing the amount of amplification product according to the expression of the housekeeping gene GADPH. Results were averaged from four sets of independent experiments and expressed as arbitrary units. The identities of the amplified fragments were confirmed by sequencing. (d) Effect of TNF-α gene silencing on IL-6 and IL-8 production detected by ELISA. (e) Flow cytometric analysis of the effect of TNF-α block by adalimumab and gene silencing on AREG expression.
Then the involvement of AREG in TNF-α-induced IL-6 and IL-8 secretion in human salivary gland epithelial cells treated with anti-Ro/SSA autoantibodies was investigated. As it has not yet been well established whether TNF-α is a regulator of AREG activation, we used Adalimumab and siRNA specifically directed against TNF-α mRNA to evaluate the effect of TNF-α block on AREG expression. After adalimumab treatment, AREG levels in anti-Ro/SSA Abs treated-SGEC were reported to that observed in untreated control cells (32.3%±1.45, for AREG in anti-Ro/SSA Abs plus adalimumab-treated SGEC versus 25%±1.3 for AREG in untreated cells). (Figure 5e). Notably, treatment of SGEC with Adalimumab alone did not affect the AREG levels in comparison with untreated control cells (26.1%±1.76 for adalimumab-treated SGEC versus 25%±1.3 for AREG in untreated cells). TNF-α gene silencing resulted in a significant decrease of AREG expression (Figure 5e) in anti-Ro/SSA Abs plus TNF-α siRNA-treated SGEC (29.7%±1.47 for anti-Ro/SSA Abs plus TNF-α siRNA-treated SGEC versus 68%±1.5 for anti-Ro/SSA Abs-treated SGEC, P<0.01) restoring expression to the basal level observed in unstimulated cells. To test whether TNF-α-induced IL-6 and IL-8 secretion is mediated by the activation of AREG, SGEC were treated with siRNA that were specifically targeted against the AREG mRNA transcript, to block AREG signal transduction (Figure 6a and b). Similarly to TNF-α knock down, AREG gene silencing inhibited the TNF-α-induced IL-6 and IL-8 secretion (Figure 6c and d) in SGEC treated with anti-Ro/SSA Abs, suggesting that TNF-α induces IL-6 and IL-8 secretion through AREG.
Silencing effect of AREG siRNA on proinflammatory cytokines production. SGEC were transfected with AREG siRNA. AREG gene expression was measured by semiquantitative RT-PCR (a). Negative, negative controls with no known sequence similarity to human genes; anti-Ro, AREG mRNA production in anti-Ro/SSA Abs treated SGEC; anti-Ro+AREG siRNA, AREG gene silencing in anti-Ro/SSA Abs treated SGEC; mRNA expression of the housekeeping gene, GADPH, was used as internal control. (b) PCR products were densitometrically analyzed after standardizing the amount of amplification product according to the expression of the housekeeping gene GADPH. (c) ELISA determination of the effect of AREG gene silencing on IL-6 and IL-8 production. (d) Real-Time analysis of the effect of AREG gene silencing on cytokines expression.
Kinetic of IL-6 and IL-8 Production
To further confirm that TNF-α induces IL-6 and IL-8 secretion through AREG, the kinetic of IL-6 and IL-8 cytokines production by SGEC was determined using exogeni TNF-α and AREG as stimulants (Figure 7a and b). Cytokines concentrations were determined at 8, 16, 24, 48, 72 h after addition of the stimulants to the cultures. The concentrations of the cytokines studied increased rapidly within the first 16 h of stimulation with TNF-α and AREG. The concentrations of IL-6 and IL-8 reached their peak value at 24 h when SGEC were treated with exogenous AREG. When the stimulant was exogenous TNF-α, IL-6 and IL-8 concentrations peaked at 48 h. After this time, cytokine concentrations declined gradually.
Kinetics of IL-6 and IL-8 production by SGEC in response to exogeni TNF-α and AREG. SGEC were incubated with stimulants, and cell-free supernatants were collected at 8, 16, 24, 48, 72 h. IL-6 and IL-8 in supernatants were quantified by ELISA test. (Data represent the mean±s.e. of four independent experiments).
CHX Decreases ProInflammatory Cytokines Production
To further address the question whether AREG regulation occurs directly through TNF-α, CHX, a protein synthesis inhibitor, was used in the presence of exogenous TNF-α as stimulant and the effect on AREG mRNA expression by SGEC was evaluated (Figure 8).
CHX effect on AREG mRNA and IL-6 and IL-8 secretion. After cells were pretreated with CHX for 30 min, exogenous TNF-α was added. Total RNA was analyzed for the content of AREG mRNA (a). These experiments were repeated twice with similar results. PCR products were densitometrically analyzed after standardizing the amount of amplification product according to the expression of the housekeeping gene GADPH (b). Results were expressed as arbitrary units. The identities of the amplified fragments were confirmed by sequencing. For ELISA assay, cell-free supernatants were collected and IL-6 (c) and IL-8 (d) were quantified. (Data represent the mean±s.e. of six independent experiments).
CHX addition results in increased expression of AREG mRNA (panel A and B) suggesting that the mechanism through which TNF-α upregulates AREG is direct and does not require de novo protein synthesis. As concern the effect of CHX on IL-6 and IL-8 release from exogenous TNF-α-treated SGEC, a marked decrease of proinflammatory cytokines production was observed (panel C and D). As in control SGEC, AREG is present in a percentage of 25%, (Figure 2a, panel C), when the cells were treated with exogenous TNF-α plus CHX, a low production of IL-6 and IL-8 was still detectable. This is probably because of the shedding of AREG by the exogenous TNF-α added.
DISCUSSION
Our previous studies investigated on the pathogenic role of anti-nuclear autoantibodies, characterizing SS and primarily directed against a number of antigenic proteins coupled to small RNA molecules. We demonstrated that autoantibodies can access SGEC via Fcγ receptors, transmembrane receptors that recognize the Fc part of the IgG, and lead to various functional cellular alterations.27, 30, 34 SGEC express the receptors for TNF-α and produce the cytokine TNF-α after anti-Ro/SSA Abs internalization.29, 31, 39 The actual study results provide more information about the proinflammatory cytokines production by SGEC after autoantibodies treatment, demonstrating that cells release IL-6 and IL-8 in response to anti-Ro/SSA Abs. Furthermore, one of the possible mechanism through which IL-6 and IL-8 production occurs, is mediated by the anti-Ro/SSA Abs uptake via the Fcγ receptors, as demonstrated by the block of Fcγ receptors through exogenously added Fc fragment of IgG, that determined a marked reduction of proinflammatory cytokines production in anti-Ro/SSA Abs-treated SGEC.
As previously demonstrated, in human SGEC, anti-Ro/SSA Abs determine, the prodomain shedding and activation of TACE, and a regulation of TACE expression by the TNF-α antagonists, such as adalimumab, was proven.24, 25, 26 In this research, we first evaluated whether anti-Ro/SSA Abs regulate the expression of Furin, responsible for TACE activation. In autoimmune diseases, a correlation between autoantibodies production and Furin expression has not previously been investigated. To our knowledge, our report provides the first observation of a relation between the regulation of Furin and the pathogenic role of autoantibodies, demonstrating an increase of Furin expression determined by anti-Ro/SSA Abs treatment correlated to the increased intracellular active TACE.
Extensive data show that various members of the ADAMs family, including TACE, are responsible for the release of all EGFR ligands, as AREG.14 In autoimmune diseases, characterized by a chronic inflammatory state, an overexpression of AREG occurs. AREG expression is enhanced in systemic lupus erythematosus and idiopathic thrombocytopenic purpura patients,40 in psoriasis41 and in rheumatoid arthritis, in which AREG overexpression is associated with synovial membrane inflammation.42 In accordance with our experiments, anti-Ro/SSA Abs treatment of SGEC led to an AREG gene and protein overexpression and a strong increase in the concentration of secreted AREG was observed as a response to autoantibodies treatment.
Other investigators reported that AREG overexpression is followed by the production of several proinflammatory cytokines20, 21, 22, 40, 41, 42 in autoimmune disorder. EGFR inhibition decreased the protein expression of IL-6 by adipose tissue macrophages, reducing the proinflammatory state,22 and TNF-α stimulates airway smooth muscle cells to express many proinflammatory mediators such as IL-6, chemokines, growth factors and adhesion molecules known to be involved in asthma.23 As regards the link between AREG, TNF-α and cytokines secretion, recent works have demonstrated that an anti-AREG neutralizing antibody inhibits the effect of TNF-α and exogenously added AREG stimulates IL-8 secretion, suggesting that TNF-α-induces IL-8 secretion through AREG.20
Patients with SS have an upregulated production of proinflammatory cytokines. Serum levels of IL-6 are elevated, mRNA for IL-6 are detectable in salivary gland biopsies,2 and the frequency of IL-6-secreting cells is increased in peripheral blood.4 IL-6 together with TNF-α seem to be directly associated with inflammation of the gland as these two cytokines are overexpressed in the saliva of SS patients.43 Significantly increased levels of IL-1α, IL-6, IL-8, TNF-α and TGF-β1 RNA transcripts were found in the conjunctival epithelium of SS patients as compared with controls.3, 5
In the light of these observations, the involvement of AREG in TNF-α-induced IL-6 and IL-8 secretion in healthy human salivary gland epithelial cells treated with anti-Ro/SSA Abs was investigated in this study. In these experiments, we found an increase of AREG mRNA expression in anti-Ro/SSA Abs-treated SGEC. Data obtained for AREG gene expression were confirmed by AREG protein concentration analysis and a strong increase in the concentration of secreted AREG was visualized as a response to autoantibodies treatment We also demonstrated that TNF-α gene silencing cause a significant decrease of cytokines release and AREG levels, suggesting the possibility that AREG overexpression and IL-6 and IL-8 production are directly induced by TNF-α. To clarify the mechanisms of these proinflammatory cytokines release, AREG involvement in TNF-α-induced IL-6 and IL-8 production was investigated. SGEC were treated with siRNA specifically targeted against the AREG mRNA transcript to block AREG signal transduction and AREG gene silencing had a potent inhibitory effect on TNF-α-induced IL-6 and IL-8 secretion in SGEC treated with anti-Ro/SSA Abs. The kinetics of IL-6 and IL-8 release, following exogenously added TNF-α and AREG, confirmed that TNF-α induces IL-6 and IL-8 secretion through AREG. In fact, the concentrations of IL-6 and IL-8 reached their peak value at 24 h when SGEC were treated with exogenous AREG and at 48 h when the stimulant was exogenous TNF-α.
The response we observed in the presence of CHX is also consistent with the hypothesis that AREG regulation occurs directly through TNF-α. CHX, in the presence of exogenous TNF-α as stimulant, results in increased expression of AREG mRNA suggesting that the mechanism through which TNF-α upregulates AREG is direct and does not require de novo protein synthesis. As concern the effect of CHX on IL-6 and IL-8 release from exogenous TNF-α-treated SGEC, a marked decrease of proinflammatory cytokines production was observed.
Taken together, these observations suggest the possibility that anti-Ro/SSA autoantibodies, penetrating cells through Fcγ receptors, determine overexpression of the proprotein convertase Furin in this system. This is responsible for shedding and activation of TACE that, in turn, determine the production of active TNF-α. TNF-α directly induces upregulation of AREG expression that stimulates SGEC to secrete the proinflammatory cytokines IL-6/IL-8.
Biological agents are promising therapies for SS, even if this promising effect must be confirmed in larger randomized controlled clinical trials. TNF-α targeting treatment could not be proven to be of benefit in reducing the complaints of SS patients. In the serum of several autoimmune patients human anti-human antibodies against biological agents were detectable after anti-TNF-α biological drugs administration and this could be one of the probably explanation for the clinical evidence of lack of efficacy of anti-TNF-α treatment in SS patients in which treatment effects were monitored.44 Than, currently available humanized antibodies are promising, but need further study. Interestingly, in the current research, we found that when SGEC were treated with anti-Ro/SSA Abs plus adalimumab, AREG levels were reported to that observed in control cells and a notably decreased of IL-6 and IL-8 secretion was observed. Thus, adalimumab, seems to have, in our experimental model, an anti-inflammatory effect, confirming our preliminary observation regarding the regulation of TACE expression by Adalimumab.24, 25, 26
The above findings suggest that the Furin–TACE–AREG–proinflammatory cytokines axis may be one of the intracellular mechanisms involved in the salivary glands inflammatory response in SS and could be of importance to clarify the lymphoproliferative disorders observed in this autoimmune disease. Regulation exerted by anti-TNF-α biological drugs on proinflammatory cytokines production might be of beneficial effect in inflammatory and autoimmune diseases. TNF-α interaction with anti-TNF-α agents will contribute to understanding the bases of clinical efficacy of these promising treatment modalities.
Change history
02 June 2011
In this retraction statement, the authors of the article agreed to withdraw this article because the data on the basal expression of proteins analyzed in this work have been published in another journal. The retraction of the article obviously does not preclude the possibility that the new data reported in the article, and never submitted to any journal, such as modulation of the protein expression by biological drug or the role played by Fc gamma receptors in this modulation, can be subject to some one journal for possible publication. The authors also state that no fraud was committed, but prefer to withdraw the article to avoid problems that could result from this unfortunate incident.
References
Roescher N, Tak PP, Illei GG . Cytokines in Sjögren's syndrome. Oral Dis 2009;15:519–526.
Fox RI, Kang HI, Ando D, et al. Cytokine mRNA expression in salivary gland biopsies of Sjogren's syndrome. J Immunol 1994;152:5532–5539.
Cuello C, Palladinetti P, Tedla N, et al. Chemokine expression and leucocyte infiltration in Sjögren's syndrome. Br J Rheumatol 1998;37:779–783.
Halse A, Tengnér P, Wahren-Herlenius M, et al. Increased frequency of cells secreting IL-6 and IL-10 in peripheral blood of patients with primary Sjogren's syndrome. Scand J Immunol 1999;49:533–538.
Pflugfelder SC, Jones D, Ji Z, et al. Altered cytokine balance in the tear fluid and conjunctiva of patients with Sjögren's syndrome keratoconjunctivitis sicca. Curr Eye Res 1999;19:201–211.
Boras VV, Cikes N, Lukac J, et al. The significance of salivary and serum interleukin 6 and basic fibroblast growth factor levels in patients with Sjogren's syndrome. Coll Antropol 2004;28:305–309.
Ackermann C, Kavanaugh A . Tumor necrosis factor as a therapeutic target of rheumatologic disease. Expert Opin Ther Targets 2007;11:1369–1384.
Furst DE, Schiff MH, Fleischmann RM, et al. Adalimumab, a fully human anti tumor necrosis factor-alpha monoclonal antibody, and concomitant standard antirheumatic therapy for the treatment of rheumatoid arthritis: results of STAR (Safety Trial of Adalimumab in Rheumatoid Arthritis). J Rheumatol 2003;30:2563–2571.
Horiuchi T, Mitoma H, Harashima SI, et al. Transmembrane TNF-{alpha}: structure, function and interaction with anti-TNF agents. Rheumatology (Oxford) 2010;49:1215–1228.
Black RA, Rauch CT, Kozlosky CJ, et al. A metalloproteinase disintegrin that releases tumour-necrosis factor-α from cells. Nature 1997;385:729.
Moss ML, Jin SL, Becherer JD, et al. Cloning of a disintegrin metalloproteinase that processes precursor tumour-necrosis factor-α. Nature 1997;385:733.
Srour N, Lebel A, McMahon S, et al. TACE/ADAM-17 maturation and activation of sheddase activity require proprotein convertase activity. FEBS Lett 2003;554:275–283.
Sunnarborg SW, Hinkle CL, Stevenson M, et al. Tumor necrosis factor-alpha converting enzyme (TACE) regulates epidermal growth factor receptor ligand availability. J Biol Chem 2002;277:12838–12845.
Hinkle CL, Sunnarborg SW, Loiselle D, et al. Selective roles for tumor necrosis factor alpha-converting enzyme/ADAM17 in the shedding of the epidermal growth factor receptor ligand family: the juxtamembrane stalk determines cleavage efficiency. J Biol Chem 2004;279:24179–24188.
Sahin U, Weskamp G, Kelly K, et al. Distinct roles for ADAM10 and ADAM17 in ectodomain shedding of six EGFR ligands. J Cell Biol 2004;164:769–779.
Sanderson MP, Dempsey PJ, Dunbar AJ . Control of ErbB signaling through metalloprotease mediated ectodomain shedding of EGF-like factors. Growth Factors 2006;24:121–136.
Barnard JA, Graves-Deal R, Pittelkow MR, et al. Auto- and cross-induction within the mammalian epidermal growth factor-related peptide family. J Biol Chem 1994;269:22817–22822.
Chung E, Cook PW, Parkos CA, et al. Amphiregulin causes functional downregulation of adherens junctions in psoriasis. J Invest Dermatol 2005;124:1134–1140.
Morita S, Shirakata Y, Shiraishi A, et al. Human corneal epithelial cell proliferation by epiregulin and its cross-induction by other EGF family members. Mol Vis 2007;13:2119–2128.
Chokki M, Mitsuhashi H, Kamimura T . Metalloprotease-dependent amphiregulin release mediates tumor necrosis factor-alpha-induced IL-8 secretion in the human airway epithelial cell line NCI-H292. Life Sci 2006;78:3051–3057.
Yamane S, Ishida S, Hanamoto Y, et al. Proinflammatory role of amphiregulin, an epidermal growth factor family member whose expression is augmented in rheumatoid arthritis patients. J Inflamm 2008;5:5.
Prada PO, Ropelle ER, Mourão RH, et al. EGFR tyrosine kinase inhibitor (PD153035) improves glucose tolerance and insulin action in high-fat diet-fed mice. Diabetes 2009;58:2910–2919.
Amrani Y, Ammit AJ, Panettieri RA Jr . Tumor necrosis factor receptor (TNFR) 1, but not TNFR2, mediates tumor necrosis factor-α-induced interleukin-6 and RANTES in human airway smooth muscle cells: Role of p38 and p42/44 mitogen-activated protein kinases. Mol Pharmacol 2001;60:646–655.
Sisto M, Lisi S, Lofrumento DD, et al. Induction of TNF-alpha-converting enzyme-ectodomain shedding by pathogenic autoantibodies. Int Immunol 2009;21:1341–1349.
Sisto M, Lisi S, Lofrumento DD, et al. TNF blocker drugs modulate human TNF-alpha-converting enzyme pro-domain shedding induced by autoantibodies. Immunobiology 2009 (in press).
Lisi S, Sisto M . Effects of biological drug adalimumab on tumour necrosis factor-alpha-converting enzyme activation. Immunol Cell Biol 2010;88:297–304.
Lisi S, Sisto M, Soleti R, et al. Fcgamma receptors mediate internalization of anti-Ro and anti-La autoantibodies from Sjögren's syndrome and apoptosis in human salivary gland cell line A-253. J Oral Pathol Med 2007;36:511–523.
Sisto M, Lisi S, Lofrumento D, et al. Autoantibodies from Sjögren's syndrome trigger apoptosis in salivary gland cell line. Ann N Y Acad Sci 2007;1108:418–425.
Sisto M, Lisi S, D’Amore M, et al. Anti-Ro and anti-La autoantibodies induce TNF-alpha production by human salivary gland cells: an in vitro study. Reumatismo 2007;59:221–226.
Lisi S, D’Amore M, Lofrumento D, et al. Modulation of the Fcgamma receptors induced by anti-Ro and anti-La autoantibodies: observations in salivary gland cells. Rheumatol Int 2008;28:943–948.
Sisto M, D’Amore M, Caprio S, et al. Tumor necrosis factor inhibitors block apoptosis of human epithelial cells of the salivary glands. Ann NY Acad Sci 2009;1171:407–414.
Lisi S, Sisto M, Lofrumento D, et al. Regulation of mRNA caspase-8 levels by anti-nuclear autoantibodies. Clin Exp Med 2010;10:199–203.
Vitali C, Bombardieri S, Jonsson R, et al. Classification criteria for Sjögren's syndrome: a revised version of the European criteria proposed by the American-European Consensus Group. European Study Group on Classification Criteria for Sjögren's Syndrome. Ann Rheum Dis 2002;61:554–558.
Sisto M, Lisi S, Castellana D, et al. Autoantibodies from Sjögren's syndrome induce activation of both the intrinsic and extrinsic apoptotic pathways in human salivary gland cell line A-253. J Autoimmun 2006;27:38–49.
Sens DA, Hintz DS, Rudisill MT, et al. Explant culture of human submandibular gland epithelial cells: evidence for ductal origin. Lab Invest 1985;52:559–567.
Kapsogeorgou EK, Dimitriou ID, Abu-Helu RF, et al. Activation of epithelial and myoepithelial cells in the salivary glands of patients with Sjögren's syndrome: high expression of intercellular adhesion molecule-1 (ICAM 1) in biopsy specimens and cultured cells. Clin Exp Immunol 2001;124:126–133.
Kapsogeorgou EK, Moutsopoulos HM, Manoussakis MN . Functional expression of a costimulatory B7.2 (CD86) protein on human salivary gland epithelial cells that interacts with the CD28 receptor, but has reduced binding to CTLA4. J Immunol 2001;166:3107–3113.
Brown CL, Meise KS, Plowman GD, et al. Cell surface ectodomain cleavage of human amphiregulin precursor is sensitive to a metalloprotease inhibitor. Release of a predominant N-glycosylated 43-kDa soluble form. J Biol Chem 1998;273:17258–17268.
Sisto M, D’Amore M, Scagliusi P, et al. Selective TNF-alpha gene silencing attenuates apoptosis in human salivary gland epithelial cells. Int J Immunopathol Pharmacol 2008;21:1045–1047.
Ishii T, Onda H, Tanigawa A, et al. Isolation and expression profiling of genes upregulated in the peripheral blood cells of systemic lupus erythematosus patients. DNA Res 2006;112:1–11.
Bhagavathula N, Nerusu KC, Fisher GJ, et al. Amphiregulin and epidermal hyperplasia: amphiregulin is required to maintain the psoriatic phenotype of human skin grafts on severe combined immunodeficient mice. Am J Pathol 2005;166:1009–1016.
Davies MR, Harding C J, Raines S, et al. Nurr1 dependent regulation of pro-inflammatory mediators in immortalised synovial fibroblasts. J Inflamm 2005;25:2–15.
Vucicevic Boras V, Brailo V, Lukac J, et al. Salivary interleukin-6 and tumor necrosis factor alpha in patients with drug-induced xerostomia. Oral Dis 2006;12:509–511.
Meijer JM, Pijpe J, Bootsma H, et al. The future of biologic agents in the treatment of Sjögren's syndrome. Clin Rev Allergy Immunol 2007;32:292–297.
Acknowledgements
This work was supported by grant (no. 20216000056) from the Italian Ministry for Universities and Research. We are grateful to MVC Pragnell, BA, for critical reading of this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Sisto, M., Lisi, S., Lofrumento, D. et al. Blockade of TNF-α signaling suppresses the AREG-mediated IL-6 and IL-8 cytokines secretion induced by anti-Ro/SSA autoantibodies. Lab Invest (2010). https://doi.org/10.1038/labinvest.2010.168
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/labinvest.2010.168