Abstract
T cells are involved in the pathogenesis of many diseases. To exert a pathological effect, T cells enter the tissues. We show that the determination of their entry site requires isolation of the respective T cell population, injection into genetically un-manipulated animals, and identification of the cells in vivo at various time points after injection. We indicate variables influencing in vivo migration experiments artificially, and outline how resulting problems can be either avoided or taken into account. Reviewing experiments performed according to the outlined criteria reveals two types of migration patterns for T cell subsets in vivo: 1) Naïve and memory T cells enter lymphoid and non-lymphoid organs in comparable numbers, but selectively accumulate in lymphoid tissues over time, 2) Effector T cells, too, enter lymphoid and non-lymphoid organs in comparable numbers. However, most of them die within 24 hours. Depending on the presence of cytokines, chemokines and extracellular matrix compounds they are able to survive, thereby preferentially accumulating in their target tissues. This information might help to understand the role of migration in the pathogenesis of T cell mediated diseases.
Similar content being viewed by others
Introduction
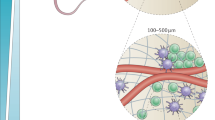
T cells are involved in the pathogenesis of many diseases that can affect almost all organ systems (Fig. 1). Although other cells such as macrophages and B cells in combination with genetic and acquired factors influence these illnesses, T cells play a dominant role (Mackay, 2000). For example, in inflammatory bowel disease, T helper cells are required for the disease to develop (Elson et al, 1998; Strober et al, 1998). In addition, T cells from patients with Crohn’s disease show hyperreactivity toward autologous intestinal flora (Duchmann et al, 1995). Depletion of T helper cells, as during progression of coincident HIV infection, can lead to remission of Crohn’s disease (Pospai et al, 1998).
Examples of diseases with known or suspected T-cell involvement and their prevalence. Indicated are affected organs, name of disease, and the respective prevalence. The data are from Mackay (2000), Holdsworth et al (1999), and Robert and Kupper (1999) and references summarized therein.
To exert a pathologic effect, T cells leave the blood and enter the tissues. During this process, T cells have to adhere to and then transmigrate through the vascular endothelium of the target organ. The molecular mechanisms that regulate this step are therefore of considerable clinical interest. It is known that the adhesion of T cells to endothelium is a multistep process (Butcher, 1991). Often molecules of the selectin family reduce the high speed of the free-flowing T cells in the blood and mediate loose attachment to the endothelium (Campbell and Butcher, 2000; Drillenburg and Pals, 2000). Then chemokines activate molecules of the integrin family on T cells. The activated integrins mediate firm adhesion to the endothelium, and the interaction of T-cell integrins with endothelial molecules of the Ig superfamily leads to the subsequent migration of T cells into the tissue.
Although the general principle of this interaction seems to apply to all sites where T cells leave the circulation, the molecules that mediate adhesion at local sites vary for the different T-cell subsets and for the different types of endothelium (Campbell and Butcher, 2000; Drillenburg and Pals, 2000). Therefore, it was postulated that by sequential interaction of a variety of adhesion molecules and chemokine receptors, T-cell subsets would be targeted specifically to certain organs, very much like the “area code” ensures that a telephone call reaches the correct recipient (Springer, 1994). On the basis of this model, the target organ of blood T cells is often inferred by comparing adhesion molecule and chemokine expression on blood T cells with in situ distribution of their ligands on blood vessel endothelium. However, it is now clear that the situation in vivo is even more complex. For example, it has recently been shown that chemokines have a dual role during entry. On the one hand, they mediate firm adhesion of T cells to the endothelium of blood vessels, thereby facilitating T-cell entry. On the other hand, they can interfere with rolling, thereby preventing T-cell entry (Grabovsky et al, 2002). In addition, in vivo the function of adhesion molecules can be strongly influenced by alterations in blood flow (Finger et al, 1996; Ohtsuka et al, 1993), acid base balance, anemia (Melder et al, 2000), nitric oxide production (Hokari et al, 1998), fever (Wang et al, 1998), acute phase proteins (Xu et al, 1995), and drugs (Diaz-Gonzalez and Sanchez-Madrid, 1998; Termeer et al, 1998).
This demonstrates that the delineation of T-cell migration routes in vivo cannot be deduced from expression analysis of adhesion molecules and chemokine receptors. Instead, it requires injection and identification of the respective T-cell population in vivo. In this article, we outline the most important factors that artificially influence the outcome of in vivo migration experiments and indicate how they can be avoided or, if not possible, can be taken into account. In addition, the traffic of naïve, effector, and memory T cells is outlined on the basis of reviewing in vivo migration experiments that meet the outlined criteria. This information might help those who are new in the field to design and conduct in vivo migration experiments successfully. Furthermore, it allows readers who are interested in the field to identify both strong and weak parts of in vivo migration experiments. This is important for the interpretation of migration data and the subsequent conclusion regarding the role of migration in the pathogenesis of T-cell–mediated diseases.
Important Considerations When Studying T-Cell Migration In Vivo
General principles that critically determine the quality of experiments investigating the migration of T cells in vivo are outlined (summarized in Table 1). Problems that complicate in vivo migration experiments cannot always be avoided, but they should be recognized and taken into account in the design and interpretation of experiments (Hall, 1985). For more details, the reader is referred to additional literature in the field (Ford, 1983; Hamann and Rebstock, 1993; Pabst et al, 1993).
Source
In most migration studies, T cells are isolated from cell suspensions prepared from splenic and lymph node tissue and are injected intravenously. Lymphoid tissues contain lymphocyte populations that are sessile and never leave the node (eg, many B cells within the germinal center). It is not known whether they also contain sessile T-cell populations. During migration through lymphoid tissues, which lasts approximately 24 hours (Westermann et al, 2001a), T and B cells temporarily either up- or down-regulate the expression of adhesion molecules (Luettig et al, 2001; Milicevic et al, 2001), and they absorb surface molecules from other cell types (Flugel et al, 2001; Hwang et al, 2000). These changes are reversed before leaving the tissue. Thus, it is very likely that cell suspensions prepared from lymphoid tissues contain T cells that would not leave the organ at that time point. They are forced into the blood, although they are not yet prepared. This suggests that such T cells do not show a normal migration pattern. Indeed, when in sheep the migration properties of T cells obtained from cell suspensions of mesenteric lymph nodes were compared with that of T cells spontaneously leaving the mesenteric lymph nodes (T cells obtained from the efferent lymph), remarkable differences were observed (Reynolds et al, 1982). Consequently, whenever possible, spontaneously migrating T cells should be used for migration experiments, which can be obtained from blood and lymph only. Nevertheless, recent experiments indicate that lymphocytes from blood and lymph also differ in their migration properties (Young et al, 1997), which should be considered in the experimental design.
Label
Numerous cell-labeling techniques have been developed to trace T cells in vivo, including radioisotopes (51Cr) (Fossum et al, 1983b), fluorochromes (FITC), bromodeoxyuridine (Pabst et al, 1993), and green fluorescent protein-engineered T cells (Flügel et al, 1999). All of these techniques are hampered by possible side effects, which can be minimized by using, for example, the appropriate dosage (Rolstad and Toogood, 1978). Some of the outlined problems could be avoided by the use of congenic animal strains. The genetic difference between donor and recipient allows an easy identification of the injected T cells both by flow cytometry (Bell and Sparshott, 1990) and by immunohistochemistry (Westermann et al, 1996) without previous labeling (green fluorescent protein-engineered T cells are much more difficult to demonstrate by immunohistochemistry). In addition, the congenic “label” is not diluted after multiple cell divisions. However, even under these conditions, the migratory properties of lymphocytes can be damaged by inappropriate in vitro handling (Ford et al, 1984). Therefore, it is necessary to control these adverse effects, which can be done by monitoring three parameters: (a) recovery: a total recovery between 80% and 90% of the injected T cells shows that the cells have been handled appropriately during the labeling procedure (Westermann et al, 1994); a lower recovery indicates that the cells have been damaged during in vitro handling, (b) lymph node entry: because only intact T cells are able to enter lymph nodes via high endothelial venules, the presence of T cells within lymph nodes shows that they are not damaged (approximately 5% of the injected cells are usually found in mesenteric lymph nodes 24 hours after injection [Smith and Ford, 1983]), (c) liver localization: damaged T cells are preferentially found in the liver, and more than 20% of the injected cells found in the liver at any time point after injection usually indicate severe cell damage (Smith and Ford, 1983).
These values are representative for migration experiments using naïve and memory T cells. Because approximately 70% of injected effector T cells physiologically die within 24 hours (summarized in Westermann et al, 2001a), a low recovery rate, few cells in lymph nodes, and high numbers in the liver are normal for this T-cell subset. Thus, analysis of recovery and of the number of injected cells in lymph nodes and liver should be included in migration studies to estimate the influence of the labeling and handling procedure on the migration of T cells.
Injection
For investigating the systemic distribution of migrating T cells, they should be injected intravenously. Intravenous injection is the only way to know exactly how many injected cells are reaching the circulation and are therefore available for entering the various organs. Intraperitoneal application of T cells complicates the experiment (Flugel et al, 2001): T cells first have to leave the peritoneal cavity into the blood and lymph before they are distributed to the various tissues. It is difficult to determine how many T cells are really reaching the blood. This number varies from animal to animal, significantly complicating the analysis. Similarly, retro-orbital application of labeled cells has the disadvantage of not allowing the researcher to know how many of the injected cells are reaching the circulation (Williams and Butcher, 1997). For a long time, it was assumed that the high numbers of lymphocytes in the lung early after intravenous injection represent a passive retention of damaged cells in the first capillary bed. By injecting labeled lymphocytes intra-arterially, it was shown that the labeled lymphocytes accumulated early after injection in the lung, too, although this time the lung was the second capillary bed that the labeled lymphocytes had to pass (Binns et al, 1981). This clearly shows that the high number of lymphocytes in the lung immediately after injection represents an active process that retains living cells.
As a rule, it can be stated that few labeled cells should be injected in a small volume over a long time. By simultaneously injecting a small number of labeled lymphocytes together with a variable number of unlabeled lymphocytes, it has been shown that the distribution of labeled lymphocytes is not altered, although up to 109 lymphocytes are co-injected (Heslop and Hardy, 1971). In our experience, satisfactory results are obtained by injecting approximately 5 × 107 T cells in 2 ml of saline over 2 minutes intravenously into a 200-g rat.
Recipient
T-cell migration has often been investigated in vivo using genetically manipulated mice that lack an adhesion molecule or chemokine receptor. However, in knockout mutants, the absence of the molecule in question may not be the only difference affecting T-cell migration in vivo compared with wild-type animals. For example, in a recent study that investigated the migration of T cells lacking the chemokine receptor CCR7, T-cell entry into the lymph nodes was reduced (Forster et al, 1999). The conclusion was that CCR7 is important for lymph node entry. However, compared with wild-type animals, the T cells used for the migration studies not only lacked CCR7 but also showed a significantly reduced number of l-selectin–positive T cells (wild-type 95% compared with knockout 65% [Forster et al, 1999]). Therefore, it is unclear whether the cause of the reduced T-cell entry into the lymph nodes is the missing chemokine receptor, reduced l-selectin expression, or a third unknown factor. Moreover, T cells take twice as long to migrate through the T-cell area of a lymph node possessing a reduced number of endogenous T cells when compared with migration through a normal node (Fossum et al, 1983b; Stekel et al, 1997). T-cell survival also depends on the number of endogenous T cells (Pilling et al, 2000). Although the cellularity of lymphoid tissues is often altered in mutant mice (eg, Chaplin and Fu, 1998), this change in cellular composition is seldom taken into account in the interpretation of T-cell migration studies. Such changes in mutant animals may be the reason that in some situations a blocking antibody directed against an adhesion molecule and the genetic lack of the same molecule have different consequences for the traffic of leukocytes (Doerschuk et al, 1996).
Thus, it is necessary to confirm the results obtained in genetically manipulated animals (eg, absence of CCR7) by following the fate of injected T cells (eg, either CCR7 high or CCR7 low) in unmanipulated recipients to define their functional role during migration in vivo. In our experience, six to eight recipient animals should be analyzed per time point to account for the variability that is normal for in vivo migration experiments.
Analysis
Several Organs. T cells continuously enter lymphoid and nonlymphoid organs (summarized in Westermann et al, 2001a). Therefore, observing only the organ of interest might lead to wrong conclusions. For example, in a recent study, the distribution of naïve lymphocytes was compared with a population enriched for lymphocytes specific for a certain antigen (Finke and Acha-Orbea, 2001). It was found that the antigen-specific population localized three times more frequent in the tissue presenting the respective antigen than naïve lymphocytes. This could have led to the conclusion of preferential migration induced by the antigen. However, the authors also presented the data of 10 other organs showing that the antigen-specific lymphocytes migrated into them in higher numbers (up to 20 times) than into the tissue presenting the antigen (Finke and Acha-Orbea, 2001). Thus, analysis of several organs helps in the appreciation of the biologic meaning of lymphocyte localization in the organ of interest.
Several Time Points. T cells are able to enter and exit tissues many times. This is in contrast to granulocytes, which enter a tissue only once and then die. Thus, an accumulation of T cells in a given tissue can be due to an increased entry, a reduced exit, or both. For differentiating from among these possibilities, several time points after injection of labeled cells must be studied. A convenient time point to study entry into tissues is 30 minutes after injection. At this time, the T cells have had enough time to adjust themselves in the recipient and to enter the tissues (Ager, 1994; Fossum et al, 1983a). However, the time elapsed after injection is too short to allow significant exit from most tissues. The rate of exit is more difficult to determine. A direct approach is to cannulate efferent lymphatic vessels (Hall and Morris, 1965). This procedure is not always feasible because of the small size of lymphatic vessels in many species and because T cells leave many organs not only via the efferent lymphatic vessels but also via the venous circulation. An indirect approach to analyze the exit phase is the determination of the organ distribution of labeled T cells 2 hours and 24 hours after injection. These time points account for the fact that T cells leave some organs fast (eg, the lungs) and some organs slowly (eg, lymph nodes). By comparing these two time points with the entry phase (0.5 hours after injection), it is possible to infer exit kinetics. In addition, to improve the analysis further, two more time points should be included. Approximately 48 to 96 hours after injection, the labeled T cells have equilibrated with the endogenous population, and it is possible to determine their distribution in a steady-state situation (Westermann et al, 2001a).
Background Values. After injection of labeled T cells, the label may detach from the cell. The maximal level of such background activity can be estimated, for example, by labeling lymphocytes radioactively, killing them, and then injecting them. For the radioactive isotope 51Cr, the background activity differs in the various organs and can range between 0.5% and 3% of the injected dosage (Finke and Acha-Orbea, 2001). Thus, when using 51Cr-labeled lymphocytes, it is difficult to design experiments in which differences between 0.5% and 3% of the injected dosage can be taken as significant for two groups (Austrup et al, 1997). This problem could be avoided when investigating the migration of T cells by quantitative immunohistochemistry. Here it is possible to detect as few as 1 labeled T cell in 100,000 endogenous cells (Westermann et al, 1996). Injected cells are identified using a microscope, thereby allowing the differentiation between living and dead cells, but this technique is time consuming and it is difficult to determine the absolute number of injected cells contained by the whole organ. With new techniques (eg, two-photon imaging [Miller et al, 2002]), it is possible to follow the traffic of labeled lymphocytes real time within the intact organ (eg, lymph node). However, one should bear in mind that for such examination, blood flow, lymph flow, and innervation are disrupted, and oxygen has to be supplied artificially, factors that might severely affect the observed migration patterns (Stoll et al, 2002; von Andrian, 2002). Quantitative immunohistochemistry performed at several time points after injection lacks these disadvantages; however, with this technique, it is not possible to follow single T cells over time.
Interpretation
The interpretation of the results obtained in experiments that investigate the migration of T cells in vivo is influenced by many factors. Here, only two issues that tend to be overlooked in many studies are raised.
Data Presentation. Many studies have investigated whether two T-cell populations differ in their migration pattern. Thus, two populations are radioactively labeled and injected, and the radioactivity in various organs is determined. In many studies, the radioactivity is given as “percentage of recovered radioactivity.” Here, the values for the two populations can be compared only when the total recovery for each population is almost identical. A direct comparison of the two T-cell populations is possible when the radioactivity is indicated as “percentage of injected radioactivity” because it also accounts for cell death that might occur after injection. The importance of this point is underlined by the following example. Naïve T cells are thought to migrate preferentially through lymphoid tissues. During activation, it is assumed that effector T cells alter their migration properties dramatically and now migrate through preferentially nonlymphoid tissues. This view seems to be confirmed when the distribution of the two populations is analyzed 24 hours after injection. Naïve T cells prevail in lymph nodes and spleen, whereas in all other organs, more effector T cells are found (Fig. 2A). However, the data are presented as “percentage of recovered radioactivity.” It has long been known that approximately 70% of the effector cells die within 24 hours (summarized in Westermann et al, 2001a). If this is taken into account and the same data are given as “percentage of injected radioactivity,” then a completely different picture arises (Fig. 2B). Now naïve T cells prevail in 7 of 11 organs, including many nonlymphoid organs. Furthermore, effector T cells are found in lymphoid and nonlymphoid organs in approximately comparable numbers. Specifically, when indicated as “percentage of recovered radioactivity,” it seems that effector T cells localize approximately three times more efficiently into the bone marrow as compared with naïve T cells (Fig. 2A, red arrow). However, choosing the appropriate presentation, it becomes obvious that naïve T cells migrate into the bone marrow in higher numbers than effector T cells (Fig. 2B, green arrow). Thus, for the biologic relevant interpretation of those data, not only their distribution but also their survival in vivo have to be considered. Therefore, the data should be presented as “percentage of injected radioactivity.”
Migration of naïve and effector T cells in vivo: Impact of data presentation. Radioactively labeled naïve and effector T cells are injected intravenously and analyzed 1 day later. A, If the data are presented as “percentage of recovered radioactivity,” then naïve T cells (blue bars) prevail in lymph nodes and spleen, whereas in all other organs, effector T cells (green bars) are more numerous. For example, approximately three times more effector T cells are found in the bone marrow compared with naïve T cells (red arrow). B, If the same data are presented as “percentage of injected radioactivity,” then naïve T cells (blue bars) are predominant in 7 of 11 organs, including many nonlymphoid organs. Furthermore, naïve T cells migrate into the bone marrow in higher numbers than effector T cells (green arrow). Rat thoracic duct lymphocytes (consisting mainly of T cells) were labeled either with 51Cr (resting T cells) or with 125I (activated T cells) and injected into the rat tail vein. One day later, the recipient was thoroughly perfused to remove contaminating blood in the various organs and the radioactivity of the different tissues was determined and expressed as indicated (data derived from Rannie and Donald (1977) and from Hamann et al (2000) for the small intestine).
Biologic Implication of “Small Percentages”. One day after injection of naïve T cells, approximately 40% of the injected T cells are found in lymph nodes, whereas only approximately 0.004% are found in the brain, the other organs ranging between these two extremes (Fig. 2B). This localization pattern has been confirmed by many groups (Smith and Ford, 1983) not only for naïve T cells but also for helper and cytotoxic T cells (Bell et al, 1995), memory T cells (Bell et al, 1995), and B cells (Fossum et al, 1983a, 1983b). Often the 0.004% of the injected naïve T cells found in the brain is considered to be background activity rather than meaning that naïve T cells enter the brain for physiologic reasons. However, recent animal experiments using different techniques also demonstrate that not only activated but also naïve T cells are able to enter the brain (Krakowski and Owens, 2000). Moreover, with the use of immunohistochemistry, T cells have been identified in brain parenchyma of healthy, untreated mice with an intact blood-brain barrier (Raivich et al, 1998). Even the low percentage of labeled T cells found after injection in the rat brain might be of biologic significance. Assuming that after injection a percentage of labeled T cells comparable to that found in animal experiments are found in the human brain would mean that approximately 20 million T cells pass through the brain each day (0.004% of 5 × 1011 T cells leaving the blood each day to enter the tissues). Given a frequency of T cells specific for a certain antigen of approximately 1 in 5000 T cells (Kearney et al, 1994; Merkenschlager et al, 1988), even the brain might be “surveyed” by sufficient T cells to allow the recognition of each available antigen specificity more than 4000 times per day. Additional studies are necessary to analyze in more detail the extent to which the different regions within a single organ are included in the migration pathways of the different T-cell subsets. To our knowledge, no study has unequivocally demonstrated the complete absence of naïve T cells from any organ. Thus, with the exception of tissues such as cartilage, cornea, and lens (normally not supplied by blood at all), all organs are continuously transmigrated by naïve T cells. As a result of the huge number of T cells leaving the blood each day into the tissues, small percentages found in the tissues after injection indicate surprisingly high numbers of transmigrating T cells.
Identification of Molecules Regulating T-Cell Migration
Analysis of in vitro cell adhesion assays and of in vivo expression of adhesion molecules and chemokine receptors has been instrumental for the identification of molecules involved in the regulation of T-cell traffic. The following sections outline important characteristics of both approaches, which are helpful for the interpretation of the data obtained by these techniques.
In Vitro Cell Adhesion Assay
Most in vitro adhesion assays measure only adhesion. It is known, however, that normally no more than 30% of the adherent cells migrate through the endothelium (Fig. 3, left panel [Bjerknes et al, 1986]). Thus, the usual type of in vitro adhesion assay, as well as intravital microscopy, cannot be assumed to provide information on whether an adherent cell migrates into the tissue (Walter et al, 1995; Warnock et al, 2000). Even an in vitro assay in which transmigration is also measured does not fully reflect the in vivo situation as shown by the following two examples:
Presence of adequate adhesion molecule: Differences for T-cell adhesion in vitro and in vivo. In vitro (left): T cells expressing the adequate adhesion molecule bind to the endothelial cells in vitro and are able to transmigrate. In vivo (right): Although T cells express the adequate adhesion molecules, they might not be able to adhere to the endothelium and to transmigrate because they are prevented from reaching the appropriate vascular bed. One possible reason is that T cells are retained in the lung.
(A) When T cells do not express the respective adhesion molecule, they will not adhere and therefore not migrate through the endothelium. Despite the same basic situation in vivo (absence of the adhesion molecule for the relevant ligand), adhesion to and migration through the endothelium may be possible because already adherent platelets (Diacovo et al, 1996), lymphocytes (Jutila and Kurk, 1996), and neutrophils (Bargatze et al, 1994) function as “bridging molecules” and facilitate adhesion and thereby transmigration.
(B) It is widely assumed that effector T cells poorly enter lymph nodes because l-selectin, which is necessary for lymph node entry, is down-regulated during activation of these cells (Dailey, 1998). However, when activated lymphocytes are directly infused into the artery supplying the lymph node, they migrate into the tissue in numbers comparable to those of resting lymphocytes (Sedgley and Ford, 1976). Thus, a reduced availability (eg, as a result of retention in the lung; Fig. 3, right panel) and not decreased l-selectin expression is a likely cause for the poor entry of activated T cells into lymph nodes.
In Vivo Analysis of the Expression of Adhesion Molecules and Chemokine Receptors
Often the analysis of in vivo expression data leads to conclusions that are in contrast to that of in vivo migration experiments (summarized in Westermann et al, 2001b). Although the molecular mechanisms that mediate these unexpected results still await clarification, several principal arguments may help to explain them:
(A) The demonstration of T cells within a tissue expressing an adhesion molecule that has been shown in vitro to bind to the locally expressed ligand is often taken as evidence to infer a functional role of that molecule during entry. However, it is known that adhesion molecules can be up-regulated on T cells after migration into the tissue (Pitzalis et al, 1996; Seiter et al, 1998). This process may be induced by factors that are characteristic of the respective microenvironment (Dailey, 1998; Shibahara et al, 2000). Therefore, analysis of adhesion molecule and ligand expression only does not allow differentiating between two scenarios: Are T cells within a certain tissue because they express certain adhesion molecules, or do T cells express certain adhesion molecules because they are within a certain tissue (“hen and egg problem”)? In addition, the presence of well-developed tight junctions between endothelial cells is often taken as evidence that lymphocytes are prevented from transmigration. However, there are now indications that in vivo leukocytes mainly use the transcellular rather than the paracellular route (summarized in Kvietys and Sandig, 2001), showing that the presence of tight junctions as such cannot be taken to conclude an impeded migration.
(B) In vivo, most adhesion molecules bind not only to one but to several ligands. For example, l-selectin binds not only to ligands expressed by the endothelium of peripheral lymph nodes but also to ligands expressed by the endothelium of Peyer’s patches (Berlin et al, 1995) and inflamed skin (Tang et al, 1997). Similarly, the integrin α4β7 mediates binding not only to MAdCAM-1 expressed by gut endothelium but also to vascular cell adhesion molecule-1 expressed by peripheral lymph node endothelium (Berlin-Rufenach et al, 1999). From analysis of the expression pattern only, it is not possible to decide which organ will be entered by the T cells in vivo.
(C) It is difficult to decide what a high and low expression of an adhesion molecule means in functional terms in vivo. For example, in children who are born with a complete absence of CD18 (leukocyte adhesion deficiency), leukocyte entry into the tissues is severely impaired, and these children experience severe infections and many die very early. However, children who have a CD18 expression of as low as 2% of the normal value show a much milder clinical course (Etzioni et al, 1999). Similarly, even 5% of the normal expression restores l-selectin function considerably (von Andrian et al, 1995). Furthermore, integrins and CD44 both occur in active and inactive conformations (Hourihan et al, 1993; Toyama-Sorimachi et al, 1993). Most antibodies used to identify these molecules do not differentiate between functional and nonfunctional forms of adhesion molecules. Thus, expression levels determined by such antibodies do not correlate with the ability to adhere to endothelium.
These examples clearly show that the results of both approaches (ie, in vitro adhesion assay and in vivo expression analysis) need confirmation regarding their proposed function in vivo.
Migration Routs of Naïve, Effector, and Memory T Cells In Vivo
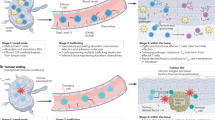
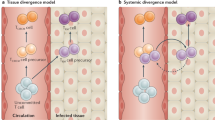
Investigating the migration of labeled T-cell subsets in vivo has revealed two principally different distribution patterns (Fig. 4). (A) Naïve T cells enter lymphoid and nonlymphoid organs in comparable numbers. They have a long life span and are able to complete many rounds of migration. As a result of their long transit time through lymphoid tissues (eg, lymph nodes approximately 24 hours), they accumulate in these tissues over time (Westermann et al, 1994). (B) After activation in lymphoid organs, the generated effector T cells are short-lived and their survival depends on cytokines, chemokines, and extracellular matrix compounds experienced during activation (Bode et al, 2001). From the site of generation, effector T cells are homogeneously distributed into lymphoid and nonlymphoid organs (Fig. 4). Depending on the milieu they face in these tissues (eg, absence or presence of characteristic cytokines, chemokines, and extracellular matrix compounds), effector T cells either die or survive. Because the milieus of the drainage area and the draining lymph node are comparable, this mechanism provides a way to target effector T cells selectively into the drainage area of the lymph node in which they were generated (ie, the region through the pathogen is invading the organism) (Bode et al, 2001). Comparably, the selective accumulation of T-cell precursors in the thymus, of T cell lymphomas in the skin, and of tumor metastasis in specific organs is probably due to selective survival and proliferation in the appropriate microenvironment rather than to selective entry into these sites. We have indications that freshly generated memory T cells are distributed like effector T cells (Bode et al, 2002). In contrast, mature memory T cells show a migration pattern that is comparable to that of naïve T cells (Westermann et al, 2001a).
Two principally different migration patterns can be identified when following the migration routes of labeled naïve, effector, and memory T cells. A, Naïve T cells enter lymphoid and nonlymphoid organs. They have a long life span and continuously leave the organs and enter them again. Because the time needed for migrating through the lymphoid organs, especially the lymph nodes, is longer than through other organs, cohorts of naïve T cells selectively accumulate in lymph nodes to initiate immune responses. B, After generation in lymph nodes, effector T cells have a short live span and are homogeneously distributed into lymphoid and nonlymphoid organs. Depending on the presence of characteristic cytokines, chemokines, and extracellular matrix compounds they, are able to survive and to proliferate thereby accumulating in their target tissues.
Conclusion
Investigating the migration of labeled lymphocytes in vivo is essential for defining T-cell traffic routes. Organ-specific entry has been proposed for several T-cell populations (for naïve and memory T cells (Mackay et al, 1990); for central memory and effector memory T cells (Sallusto et al, 1999); for skin- and gut-seeking T cells [Campbell and Butcher, 2000]); however, the in vivo migration experiments have either failed to demonstrate organ-specific entry or are still missing (summarized in Westermann et al, 2001b). Instead, in vivo migration studies have revealed organ-specific survival of T cells during their effector stage. Identifying the molecules that govern T-cell distribution in vivo will allow their modification to enhance desired immune responses and to diminish unwanted ones.
“The difficulties introduced by such phenomena [which complicate the design of in vivo migration experiments] cannot always be avoided but they can be recognized and taken into account in both the design and interpretation of experiments. Like the bunkers in a golf course they contribute a good deal to the fun; they are a challenge to the participants, and a source of endless amusement to the informed observer.” —Joe Hall (Hall, 1985)
References
Ager A (1994). Lymphocyte recirculation and homing: Roles of adhesion molecules and chemoattractants. Trends Cell Biol 4: 326–333.
Austrup F, Vestweber D, Borges E, Löhning M, Bräuer R, Herz U, Renz H, Hallmann R, Scheffold A, Radbruch A, and Hamann A (1997). P- and E-selectin mediate recruitment of T-helper-1 but not T-helper-2 cells into inflamed tissues. Nature 385: 81–83.
Bargatze RF, Kurk S, Butcher EC, and Jutila MA (1994). Neutrophils roll on adherent neutrophils bound to cytokine-induced endothelial cells via L-selectin on the rolling cells. J Exp Med 180: 1785–1792.
Bell EB and Sparshott SM (1990). Interconversion of CD45R subsets of CD4 T cells in vivo. Nature 348: 163–166.
Bell EB, Sparshott SM, and Ager A (1995). Migration pathways of CD4 T cell subsets in vivo. The CD45RC-subset enters the thymus via alpha4/VCAM-1 interaction. Int Immunol 7: 1861–1871.
Berlin C, Bargatze RF, Campell JJ, von Andrian UH, Scabo MC, Hasslen SR, Nelson RD, Berg EL, Erlandsen SL, and Butcher EC (1995). Alpha 4 integrins mediate lymphocyte attachment and rolling under physiologic flow. Cell 80: 413–422.
Berlin-Rufenach C, Otto F, Mathies M, Westermann J, Owen M, Hamann A, and Hogg N (1999). Lymphocyte migration in LFA-1 deficient mice. J Exp Med 189: 1467–1478.
Binns RM, Blakeley D, and Licence ST (1981). Migration of fluoresceinated pig lymphocytes in vivo: Technical aspects and use in studies of autologous and homologous cell survival for up to three weeks. Int Arch Allergy Appl Immunol 66: 341–349.
Bjerknes M, Cheng H, and Ottaway CA (1986). Dynamics of lymphocyte-endothelial interactions in vivo. Science 231: 402–405.
Bode U, Sahle A, Sparmann G, Weidner F, and Westermann J (2002). The fate of effector T cells in vivo is determined during activation and differs for CD4(+) and CD8(+) cells. J Immunol 169: 6085–6091.
Bode U, Sparmann G, and Westermann J (2001). Gut-derived effector T cells circulating in the blood of the rat: Preferential re-distribution by TGFbeta-1 and IL-4 maintained proliferation. Eur J Immunol 31: 2116–2125.
Butcher EC (1991). Leukocyte-endothelial cell recognition: Three (or more) steps to specificity and diversity. Cell 67: 1033–1036.
Campbell JJ and Butcher EC (2000). Chemokines in tissue-specific and microenvironment-specific lymphocyte homing. Curr Opin Immunol 12: 336–341.
Chaplin DD and Fu Y (1998). Cytokine regulation of secondary lymphoid organ development. Curr Opin Immunol 10: 289–297.
Dailey MO (1998). Expression of T lymphocyte adhesion molecules: Regulation during antigen-induced T cell activation and differentiation. Crit Rev Immunol 18: 153–184.
Diacovo TG, Puri KD, Warnock RA, Springer TA, and von Andrian UH (1996). Platelet-mediated lymphocyte delivery to high endothelial venules. Science 273: 252–255.
Diaz-Gonzalez F and Sanchez-Madrid F (1998). Inhibition of leukocyte adhesion: An alternative mechanism of action for anti-inflammatory drugs. Immunol Today 19: 169–172.
Doerschuk CM, Quinlan WM, Doyle NA, Bullard DC, Vestweber D, Jones ML, Takei F, Ward PA, and Beaudet AL (1996). The role of P-selectin and ICAM-1 in acute lung injury as determined using blocking antibodies and mutant mice. J Immunol 157: 4609–4614.
Drillenburg P and Pals ST (2000). Cell adhesion receptors in lymphoma dissemination. Blood 95: 1900–1910.
Duchmann R, Kaiser I, Hermann E, Mayet W, Ewe K, and Meyer zum Buschenfelde KH (1995). Tolerance exists towards resident intestinal flora but is broken in active inflammatory bowel disease (IBD). Clin Exp Immunol 102: 448–455.
Elson CO, Cong Y, Brandwein S, Weaver CT, McCabe RP, Mahler M, Sundberg JP, and Leiter EH (1998). Experimental models to study molecular mechanisms underlying intestinal inflammation. Ann NY Acad Sci 859: 85–95.
Etzioni A, Doerschuk CM, and Harlan JM (1999). Of man and mouse: Leukocyte and endothelial adhesion molecule deficiencies. Blood 94: 3281–3288.
Finger EB, Puri KD, Alon R, Lawrence MB, von Andrian UH, and Springer TA (1996). Adhesion through L-selectin requires a threshold hydrodynamic shear. Nature 379: 266–269.
Finke D and Acha-Orbea H (2001). Differential migration of in vivo primed B and T lymphocytes to lymphoid and non-lymphoid organs. Eur J Immunol 31: 2603–2611.
Flugel A, Berkowicz T, Ritter T, Labeur M, Jenne DE, Li Z, Ellwart JW, Willem M, Lassmann H, and Wekerle H (2001). Migratory activity and functional changes of green fluorescent effector cells before and during experimental autoimmune encephalomyelitis. Immunity 14: 547–560.
Flügel A, Willem M, Berkowicz T, and Wekerle H (1999). Gene transfer into CD4+ T lymphocytes: Green fluorescent protein-engineered, encephalitogenic T cells illuminate brain autoimmune responses. Nat Med 5: 843–847.
Ford WL (1983). The preparation and labelling of lymphocytes. In: Weir DM, editor. Handbook of experimental immunology, 2nd ed. Oxford: Blackwell, 23.
Ford WL, Allen TD, Pitt MA, Smith ME, and Stoddart RW (1984). The migration of lymphocytes across specialized vascular endothelium. VIII Physical and chemical conditions influencing the surface morphology of lymphocytes and their ability to enter lymph nodes. Am J Anat 170: 377–390.
Forster R, Schubel A, Breitfeld D, Kremmer E, Renner-Muller I, Wolf E, and Lipp M (1999). CCR7 coordinates the primary immune response by establishing functional microenvironments in secondary lymphoid organs. Cell 99: 23–33.
Fossum S, Smith ME, and Ford WL (1983a). The migration of lymphocytes across specialized vascular endothelium. VII The migration of T and B lymphocytes from the blood of the athymic, nude rat. Scand J Immunol 17: 539–549.
Fossum S, Smith ME, and Ford WL (1983b). The recirculation of T and B lymphocytes in the athymic, nude rat. Scand J Immunol 17: 551–557.
Grabovsky V, Dwir O, and Alon R (2002). Endothelial chemokines destabilize L-selectin-mediated lymphocyte rolling without inducing selectin shedding. J Biol Chem 277: 20640–20650.
Hall J (1985). The study of circulating lymphocytes in vivo: A personal view of artifice and artifact. Immunol Today 6: 149–152.
Hall JG and Morris B (1965). The origin of the cells in the efferent lymph from a single lymph node. J Exp Med 121: 901–911.
Hamann A, Klugewitz K, Austrup F, and Jablonski-Westrich D (2000). Activation induces rapid and profound alterations in the trafficking of T cells. Eur J Immunol 30: 3207–3218.
Hamann A and Rebstock S (1993). Migration of activated lymphocytes. Curr Top Microbiol Immunol 184: 109–124.
Heslop BF and Hardy BE (1971). The distribution of 51Cr-labeled syngeneic and allogeneic lymph node cells in the rat. Transplantation 11: 128–134.
Hokari R, Miura S, Fujimori H, Tsuzuki Y, Shigematsu T, Higuchi H, Kimura H, Kurose I, Serizawa H, Suematsu M, Yagita H, Granger DN, and Ishii H (1998). Nitric oxide modulates T-lymphocyte migration in Peyer’s patches and villous submucosa of rat small intestine. Gastroenterology 115: 618–627.
Holdsworth SR, Kitching AR, and Tipping PG (1999). Th1 and Th2 T helper cell subsets affect patterns of injury and outcomes in glomerulonephritis. Kidney Int 55: 1198–1216.
Hourihan H, Allen TD, and Ager A (1993). Lymphocyte migration across high endothelium is associated with increases in alpha 4 beta 1 integrin (VLA-4) affinity. J Cell Sci 104: 1049–1059.
Hwang I, Huang JF, Kishimoto H, Brunmark A, Peterson PA, Jackson MR, Surh CD, Cai Z, and Sprent J (2000). T cells can use either T cell receptor or CD28 receptors to absorb and internalize cell surface molecules derived from antigen-presenting cells. J Exp Med 191: 1137–1148.
Jutila MA and Kurk S (1996). Analysis of bovine gammadelta T cell interactions with E-, P-, and L-selectin characterization of lymphocyte on lymphocyte rolling and the effects of O-glycoprotease. J Immunol 156: 289–296.
Kearney ER, Pape KA, Loh DY, and Jenkins MK (1994). Visualization of peptide-specific T cell immunity and peripheral tolerance induction in vivo. Immunity 1: 327–339.
Krakowski AM and Owens T (2000). Naive T lymphocytes traffic to inflamed central nervous system, but require antigen recognition for activation. Eur J Immunol 30: 1002–1009.
Kvietys PR and Sandig M (2001). Neutrophil diapedesis: Paracellular or transcellular? News Physiol Sci 16: 15–19.
Luettig B, Sponholz A, Heerwagen C, Bode U, and Westermann J (2001). Recent thymic emigrants (CD4+) continuously migrate through lymphoid organs: Within the tissue they alter surface molecule expression. Scand J Immunol 53: 563–571.
Mackay CR, Marston WL, and Dudler L (1990). Naive and memory T cells show distinct pathways of lymphocyte recirculation. J Exp Med 171: 801–817.
Mackay IR (2000). Science, medicine, and the future: Tolerance and autoimmunity. BMJ 321: 93–96.
Melder RJ, Yuan J, Munn LL, and Jain RK (2000). Erythrocytes enhance lymphocyte rolling and arrest in vivo. Microvasc Res 59: 316–322.
Merkenschlager M, Terry L, Edwards R, and Beverly PCL (1988). Limiting dilution analysis of proliferative responses in human lymphocyte populations defined by the monoclonal antibody UCHL1: Implications for differential CD45 expression in T cell memory formation. Eur J Immunol 18: 1653–1661.
Milicevic NM, Lüttig B, Trautwein C, Wüstefeld T, Mähler M, Jecker P, Wonigeit K, and Westermann J (2001). Splenectomy of rats selectively reduces LFA-1 and ICAM-1 expression on B cell subsets in blood and lymph nodes. Blood 98: 3035–3041.
Miller MJ, Wei SH, Parker I, and Cahalan MD (2002). Two-photon imaging of lymphocyte motility and antigen response in intact lymph node. Science 296: 1869–1873.
Ohtsuka A, Ando J, Korenaga R, Kamiya A, Toyama-Sorimachi N, and Miyasaka M (1993). The effect of flow in the expression of vascular adhesion molecule-1 by cultured mouse endothelial cells. Biochem Biophys Res Commun 193: 303–310.
Pabst R, Binns RM, Rothkötter HJ, and Westermann J (1993). Quantitative analysis of lymphocyte fluxes in vivo. Curr Top Microbiol Immunol 184: 151–159.
Pilling D, Akbar AN, Shamsadeen N, Scheel-Toellner D, Buckley C, and Salmon M (2000). High cell density provides potent survival signals for resting T-cells. Cell Mol Biol 46: 163–174.
Pitzalis C, Cauli A, Pipitone N, Smith C, Barker J, Marchesoni A, Yanni G, and Panayi GS (1996). Cutaneous lymphocyte antigen-positive T lymphocytes preferentially migrate to the skin but not to the joint in psoriatic arthritis. Arthritis Rheum 39: 137–145.
Pospai D, Rene E, Fiasse R, Farahat K, Beaugery L, Lammens P, Reimund C, Duclos B, Le Quintrec Y, Vandercam B, and Mignon M (1998). Crohn’s disease stable remission after human immunodeficiency virus infection. Dig Dis Sci 43: 412–419.
Raivich G, Jones LL, Kloss CU, Werner A, Neumann H, and Kreutzberg GW (1998). Immune surveillance in the injured nervous system: T-lymphocytes invade the axotomized mouse facial motor nucleus and aggregate around sites of neuronal degeneration. J Neurosci 18: 5804–5816.
Rannie GH and Donald KJ (1977). Estimation of the migration of thoracic duct lymphocytes to non-lymphoid tissues. A comparison of the distribution of radioactivity at intervals following i v transfusion of cells labelled with 3H, 14C, 75Se, 99mTc, 125I and 51Cr in the rat. Cell Tissue Kinet 10: 523–541.
Reynolds J, Heron I, Dudler L, and Trnka Z (1982). T-cell recirculation in the sheep: Migratory properties of cells from lymph nodes. Immunology 47: 415–421.
Robert C and Kupper TS (1999). Inflammatory skin diseases, T cells, and immune surveillance. N Engl J Med 341: 1817–1828.
Rolstad B and Toogood E (1978). Toxicity of Na251CrO4 when used to label rat lymphocytes. J Immunol Methods 21: 271–276.
Sallusto F, Lenig D, Forster R, Lipp M, and Lanzavecchia A (1999). Two subsets of memory T lymphocytes with distinct homing potentials and effector functions. Nature 401: 708–712.
Sedgley M and Ford WL (1976). The migration of lymphocytes across specialized vascular endothelium. I The entry of lymphocytes into the isolated mesenteric lymph-node of the rat. Cell Tissue Kinet 9: 231–243.
Seiter S, Schadendorf D, Tilgen W, and Zoller M (1998). CD44 variant isoform expression in a variety of skin-associated autoimmune diseases. Clin Immunol Immunopathol 89: 79–93.
Shibahara T, Si-Tahar M, Shaw SK, and Madara JL (2000). Adhesion molecules expressed on homing lymphocytes in model intestinal epithelia. Gastroenterology 118: 289–298.
Smith ME and Ford WL (1983). The recirculating lymphocyte pool of the rat: A systematic description of the migratory behaviour of recirculating lymphocytes. Immunology 49: 83–94.
Springer TA (1994). Traffic signals for lymphocyte recirculation and leukocyte emigration: The multistep paradigm. Cell 76: 301–314.
Stekel DJ, Parker CE, and Nowak MA (1997). A model of lymphocyte recirculation. Immunol Today 18: 216–221.
Stoll S, Delon J, Brotz TM, and Germain RN (2002). Dynamic imaging of T cell-dendritic cell interactions in lymph nodes. Science 296: 1873–1876.
Strober W, Ludviksson BR, and Fuss IJ (1998). The pathogenesis of mucosal inflammation in murine models of inflammatory bowel disease and Crohn disease. Ann Intern Med 128: 848–856.
Tang MLK, Hale LP, Steeber DA, and Tedder TF (1997). L-Selectin is involved in lymphocyte migration to sites of inflammation in the skin. J Immunol 158: 5191–5199.
Termeer CC, Weiss JM, Schöpf E, Vanscheidt W, and Simon JC (1998). The low molecular weight dextran 40 inhibits the adhesion of T lymphocytes to endothelial cells. Clin Exp Immunol 114: 422–426.
Toyama-Sorimachi N, Miyake K, and Miyasaka M (1993). Activation of CD44 induces ICAM-1/LFA-1-independent, Ca2+, Mg2–independent adhesion pathway in lymphocyte-endothelial cell interaction. Eur J Immunol 23: 439–446.
von Andrian UH (2002). Immunology. T cell activation in six dimensions. Science 296: 1815–1817.
von Andrian UH, Hasslen SR, Nelson RD, Erlandsen SL, and Butcher EC (1995). A central role for microvillous receptor presentation in leukocyte adhesion under flow. Cell 82: 989–999.
Walter S, Micheel B, Pabst R, and Westermann J (1995). Interaction of B and T lymphocyte subsets with high endothelial venules in the rat: Binding in vitro does not reflect homing in vivo. Eur J Immunol 25: 1199–1205.
Wang WC, Goldman LM, Schleider DM, Appenheimer MM, Subjeck JR, Repasky EA, and Evans SS (1998). Fever-range hyperthermia enhances L-selectin-dependent adhesion of lymphocytes to vascular endothelium. J Immunol 160: 961–969.
Warnock RA, Campbell JJ, Dorf ME, Matsuzawa A, McEvoy LM, and Butcher EC (2000). The role of chemokines in the microenvironmental control of T versus B cell arrest in Peyer’s patch high endothelial venules. J Exp Med 191: 77–88.
Westermann J, Ehlers E-M, Exton MS, Kaiser M, and Bode U (2001a). Migration of naive, effector, and memory T cells: implications for the regulation of immune responses. Immunol Rev 184: 20–37.
Westermann J, Engelhardt B, and Hoffmann J (2001b). Migration of T cells in vivo: Molecular mechanisms and clinical implications. Ann Intern Med 135: 279–295.
Westermann J, Persin S, Matyas J, van der Meide P, and Pabst R (1994). Migration of so-called naive and memory lymphocytes from blood to lymph in the rat: The influence of interferon gamma on the circulation pattern. J Immunol 152: 1744–1750.
Westermann J, Smith T, Peters U, Tschernig T, Pabst R, Steinhoff G, Sparshott SM, and Bell EB (1996). Both activated and nonactivated leukocytes from the periphery continuously enter the thymic medulla of adult rats: Phenotypes, sources and magnitude of traffic. Eur J Immunol 26: 1866–1874.
Williams MB and Butcher EC (1997). Homing of naive and memory T lymphocyte subsets to Peyer’s patches, lymph nodes, and spleen. J Immunol 159: 1746–1752.
Xu L, Badolato R, Murphy WJ, Longo DL, Anver M, Hale S, Oppenheim JJ, and Wang JM (1995). A novel biologic function of serum amyloid A induction of T lymphocyte migration and adhesion. J Immunol 155: 1184–1190.
Young AJ, Marston WL, Dessing M, Dudler L, and Hein WR (1997). Distinct recirculating and non-recirculating B-lymphocyte pools in the peripheral blood are defined by coordinated expression of CD21 and L-selectin. Blood 90: 4865–4875.
Acknowledgements
We thank M. Peter (Hannover, Germany) for help in preparing the figures.
This study was supported by the Deutsche Forschungsgemeinschaft (We 1175/5-1) and the Volkswagenstiftung (I/78068).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Westermann, J., Söllner, S., Ehlers, EM. et al. Analyzing the Migration of Labeled T Cells In Vivo: An Essential Approach with Challenging Features. Lab Invest 83, 459–469 (2003). https://doi.org/10.1097/01.LAB.0000062852.80567.90
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1097/01.LAB.0000062852.80567.90
This article is cited by
-
Challenges for labeling and longitudinal tracking of adoptively transferred autoreactive T lymphocytes in an experimental type-1 diabetes model
Magnetic Resonance Materials in Physics, Biology and Medicine (2019)