Key Points
-
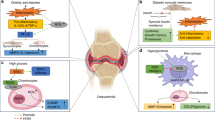
Osteoarthritis (OA) is an active disease of the whole joint that is subject to both local and systemic regulation
-
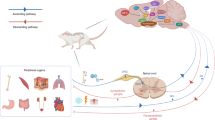
The nervous system controls key aspects of joint pathophysiology by regulating circadian rhythms, the hypothalamic–pituitary–adrenal axis, and metabolic and inflammatory pathways
-
Ageing, obesity and chronic inflammation interfere with the brain–joint axis (including the circadian system), which compromises joint homeostasis and increases susceptibility to OA
-
Circadian clocks in the central brain and peripheral joint tissues temporally coordinate local physiology to the daily rhythmic environment (light–dark, feeding–fasting, body temperature regulation and mechanical loading cycles)
-
Environmental or genetic disruption to the biological timing system might be a novel risk factor for OA susceptibility
-
Targeting the nervous system or circadian system could provide novel therapeutic avenues for OA
Abstract
Osteoarthritis (OA) is a prevalent and debilitating joint disease for which ageing, obesity and chronic inflammation are known risk factors. The central, peripheral and autonomic nervous systems are essential in all metabolic systems, and emerging evidence suggests a role for these systems in OA. In the past few years, metabolic diseases, such as obesity or diabetes, have been linked to disruption of circadian rhythms that are tightly regulated by the nervous system, whereas inflammatory and autoimmune diseases are known to be linked to disruption of the cholinergic vagus nerve reflex. Interestingly, metabolism, inflammation and circadian rhythms have all been linked to the development and progression of OA. This article reviews current knowledge of the direct and indirect roles of the nervous system and circadian system in the initiation and/or progression of OA, and highlights the directions for future research in this emerging field.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hoy, D. G. et al. Reflecting on the global burden of musculoskeletal conditions: lessons learnt from the global burden of disease 2010 study and the next steps forward. Ann. Rheum. Dis. 74, 4–7 (2015).
Vos, T. et al. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380, 2163–2196 (2012).
Goldring, M. B. & Berenbaum, F. Emerging targets in osteoarthritis therapy. Curr. Opin. Pharmacol. 22, 51–63 (2015).
Bijlsma, J. W., Berenbaum, F. & Lafeber, F. P. Osteoarthritis: an update with relevance for clinical practice. Lancet 377, 2115–2126 (2011).
Heilbronn, L. K. & Campbell, L. V. Adipose tissue macrophages, low grade inflammation and insulin resistance in human obesity. Curr. Pharm. Des. 14, 1225–1230 (2008).
Duncan, B. B. et al. Low-grade systemic inflammation and the development of type 2 diabetes: the atherosclerosis risk in communities study. Diabetes 52, 1799–1805 (2003).
Yusuf, E. et al. Association between weight or body mass index and hand osteoarthritis: a systematic review. Ann. Rheum. Dis. 69, 761–765 (2010).
Courties, A., Gualillo, O., Berenbaum, F. & Sellam, J. Metabolic stress-induced joint inflammation and osteoarthritis. Osteoarthritis Cartilage 23, 1955–1965 (2015).
Huang, Z. & Kraus, V. B. Does lipopolysaccharide-mediated inflammation have a role in OA? Nat. Rev. Rheumatol. 12, 123–129 (2016).
Sohn, D. H. et al. Plasma proteins present in osteoarthritic synovial fluid can stimulate cytokine production via Toll-like receptor 4. Arthritis Res. Ther. 14, R7 (2012).
Kyrkanides, S. et al. Osteoarthritis accelerates and exacerbates Alzheimer's disease pathology in mice. J. Neuroinflamm. 8, 112 (2011).
Verzijl, N. et al. Crosslinking by advanced glycation end products increases the stiffness of the collagen network in human articular cartilage: a possible mechanism through which age is a risk factor for osteoarthritis. Arthritis Rheum. 46, 114–123 (2002).
Loeser, R. F. Aging and osteoarthritis: the role of chondrocyte senescence and aging changes in the cartilage matrix. Osteoarthritis Cartilage 17, 971–979 (2009).
Berenbaum, F. Osteoarthritis as an inflammatory disease (osteoarthritis is not osteoarthrosis!). Osteoarthritis Cartilage 21, 16–21 (2013).
Tracey, K. J. Physiology and immunology of the cholinergic antiinflammatory pathway. J. Clin. Invest. 117, 289–296 (2007).
Cermakian, N. & Sassone-Corsi, P. Multilevel regulation of the circadian clock. Nat. Rev. Mol. Cell Biol. 1, 59–67 (2000).
Gamble, K. L., Berry, R., Frank, S. J. & Young, M. E. Circadian clock control of endocrine factors. Nat. Rev. Endocrinol. 10, 466–475 (2014).
Roenneberg, T. & Merrow, M. Circadian clocks — the fall and rise of physiology. Nat. Rev. Mol. Cell Biol. 6, 965–971 (2005).
Takahashi, J. S., Hong, H.-K., Ko, C. H. & McDearmon, E. L. The genetics of mammalian circadian order and disorder: implications for physiology and disease. Nat. Rev. Genet. 9, 764–775 (2008).
Yoo, S. H. et al. PERIOD2::LUCIFERASE real-time reporting of circadian dynamics reveals persistent circadian oscillations in mouse peripheral tissues. Proc. Natl Acad. Sci. USA 101, 5339–5346 (2004).
Balsalobre, A. et al. Resetting of circadian time in peripheral tissues by glucocorticoid signaling. Science 289, 2344–2347 (2000).
Pezuk, P., Mohawk, J. A., Wang, L. A. & Menaker, M. Glucocorticoids as entraining signals for peripheral circadian oscillators. Endocrinology 153, 4775–4783 (2012).
Reddy, A. B. et al. Glucocorticoid signaling synchronizes the liver circadian transcriptome. Hepatology 45, 1478–1488 (2007).
Herzog, E. D. & Muglia, L. J. You are when you eat. Nat. Neurosci. 9, 300–302 (2006).
Damiola, F. et al. Restricted feeding uncouples circadian oscillators in peripheral tissues from the central pacemaker in the suprachiasmatic nucleus. Genes Dev. 14, 2950–2961 (2000).
Sladek, M. et al. Insight into the circadian clock within rat colonic epithelial cells. Gastroenterology 133, 1240–1249 (2007).
Le Minh, N., Damiola, F., Tronche, F., Schutz, G. & Schibler, U. Glucocorticoid hormones inhibit food-induced phase-shifting of peripheral circadian oscillators. EMBO J. 20, 7128–7136 (2001).
Buhr, E. D., Yoo, S. H. & Takahashi, J. S. Temperature as a universal resetting cue for mammalian circadian oscillators. Science 330, 379–385 (2010).
Hut, R. A. & Van der Zee, E. A. The cholinergic system, circadian rhythmicity, and time memory. Behav. Brain Res. 221, 466–480 (2011).
Gillette, M. U. et al. Role of the M1 receptor in regulating circadian rhythms. Life Sci. 68, 2467–2472 (2001).
Liu, C. & Gillette, M. U. Cholinergic regulation of the suprachiasmatic nucleus circadian rhythm via a muscarinic mechanism at night. J. Neurosci. 16, 744–751 (1996).
Kalsbeek, A. et al. Circadian rhythms in the hypothalamo–pituitary–adrenal (HPA) axis. Mol. Cell. Endocrinol. 349, 20–29 (2012).
Nader, N., Chrousos, G. P. & Kino, T. Interactions of the circadian CLOCK system and the HPA axis. Trends Endocrinol. Metab. 21, 277–286 (2010).
Spies, C. M., Straub, R. H., Cutolo, M. & Buttgereit, F. Circadian rhythms in rheumatology — a glucocorticoid perspective. Arthritis Res. Ther. 16, S3 (2014).
Straub, R. H., Bijlsma, J. W., Masi, A. & Cutolo, M. Role of neuroendocrine and neuroimmune mechanisms in chronic inflammatory rheumatic diseases — the 10-year update. Semin. Arthritis Rheum. 43, 392–404 (2013).
Meulenbelt, I. et al. Identification of DIO2 as a new susceptibility locus for symptomatic osteoarthritis. Hum. Mol. Genet. 17, 1867–1875 (2008).
Hinoi, E. et al. Up-regulation of per mRNA expression by parathyroid hormone through a protein kinase A-CREB-dependent mechanism in chondrocytes. J. Biol. Chem. 281, 23632–23642 (2006).
Jänig, W. Sympathetic nervous system and inflammation: a conceptual view. Auton. Neurosci. 182, 4–14 (2014).
Abboud, F. M. In search of autonomic balance: the good, the bad, and the ugly. Am. J. Physiol. Regul. Integr. Comp. Physiol. 298, R1449–R1467 (2010).
Rosas-Ballina, M. & Tracey, K. J. Cholinergic control of inflammation. J. Intern. Med. 265, 663–679 (2009).
Liu, Y. et al. Activation of α7 nicotinic acetylcholine receptors prevents monosodium iodoacetate-induced osteoarthritis in rats. Cell. Physiol. Biochem. 35, 627–638 (2015).
Takarada, T. et al. Interference by adrenaline with chondrogenic differentiation through suppression of gene transactivation mediated by Sox9 family members. Bone 45, 568–578 (2009).
Jenei-Lanzl, Z. et al. Norepinephrine inhibition of mesenchymal stem cell and chondrogenic progenitor cell chondrogenesis and acceleration of chondrogenic hypertrophy. Arthritis Rheumatol. 66, 2472–2481 (2014).
Lai, L. P. & Mitchell, J. β2-adrenergic receptors expressed on murine chondrocytes stimulate cellular growth and inhibit the expression of Indian hedgehog and collagen type X. J. Cell. Biochem. 104, 545–553 (2008).
Mitchell, J., Lai, L. P., Peralta, F., Xu, Y. & Sugamori, K. β2-adrenergic receptors inhibit the expression of collagen type II in growth plate chondrocytes by stimulating the AP-1 factor Jun-B. Am. J. Physiol. Endocrinol. Metab. 300, E633–E639 (2011).
Vignon, E., Broquet, P., Mathieu, P., Louisot, P. & Richard, M. Histaminergic H1, serotoninergic, beta adrenergic and dopaminergic receptors in human osteoarthritic cartilage. Biochem. Int. 20, 251–255 (1990).
Opolka, A., Straub, R. H., Pasoldt, A., Grifka, J. & Grassel, S. Substance P and norepinephrine modulate murine chondrocyte proliferation and apoptosis. Arthritis Rheum. 64, 729–739 (2012).
Fonseca, T. L. et al. Double disruption of α2A- and α2C-adrenoceptors results in sympathetic hyperactivity and high-bone-mass phenotype. J. Bone Miner. Res. 26, 591–603 (2011).
Mauro, L. J., Wenzel, S. J. & Sindberg, G. M. Regulation of chick bone growth by leptin and catecholamines. Poult. Sci. 89, 697–708 (2010).
Gossan, N. et al. The circadian clock in murine chondrocytes regulates genes controlling key aspects of cartilage homeostasis. Arthritis Rheum. 65, 2334–2345 (2013).
Honda, K. K. et al. Different circadian expression of major matrix-related genes in various types of cartilage: modulation by light-dark conditions. J. Biochem. 154, 373–381 (2013).
Andersson, M. L. et al. Diurnal variation in serum levels of cartilage oligomeric matrix protein in patients with knee osteoarthritis or rheumatoid arthritis. Ann. Rheum. Dis. 65, 1490–1494 (2006).
Kong, S. Y. et al. Diurnal variation of serum and urine biomarkers in patients with radiographic knee osteoarthritis. Arthritis Rheum. 54, 2496–2504 (2006).
Jubiz, W., Canterbury, J. M., Reiss, E. & Tyler, F. H. Circadian rhythm in serum parathyroid hormone concentration in human subjects: correlation with serum calcium, phosphate, albumin, and growth hormone levels. J. Clin. Invest. 51, 2040–2046 (1972).
Okubo, N. et al. Parathyroid hormone resets the cartilage circadian clock of the organ-cultured murine femur. Acta Orthop. 86, 627–631 (2015).
Kanbe, K., Inoue, K., Xiang, C. & Chen, Q. Identification of clock as a mechanosensitive gene by large-scale DNA microarray analysis: downregulation in osteoarthritic cartilage. Mod. Rheumatol. 16, 131–136 (2006).
Bass, J. Circadian topology of metabolism. Nature 491, 348–356 (2012).
Guo, B. et al. Catabolic cytokines disrupt the circadian clock and the expression of clock-controlled genes in cartilage via an NFsmall ka, CyrillicB-dependent pathway. Osteoarthritis Cartilage 23, 1981–1988 (2015).
Dudek, M. et al. The chondrocyte clock gene Bmal1 controls cartilage homeostasis and integrity. J. Clin. Invest. 126, 365–376 (2016).
Dudek, M. & Meng, Q. J. Running on time: the role of circadian clocks in the musculoskeletal system. Biochem. J. 463, 1–8 (2014).
Gundberg, C. M., Markowitz, M. E., Mizruchi, M. & Rosen, J. F. Osteocalcin in human serum: a circadian rhythm. J. Clin. Endocrinol. Metab. 60, 736–739 (1985).
Hassager, C., Risteli, J., Risteli, L., Jensen, S. B. & Christiansen, C. Diurnal variation in serum markers of type I collagen synthesis and degradation in healthy premenopausal women. J. Bone Miner. Res. 7, 1307–1311 (1992).
Grundberg, E. et al. Systematic assessment of the human osteoblast transcriptome in resting and induced primary cells. Physiol. Genomics 33, 301–311 (2008).
Maronde, E. et al. The clock genes Period 2 and Cryptochrome 2 differentially balance bone formation. PLoS ONE 5, e11527 (2010).
Fu, L., Patel, M. S., Bradley, A., Wagner, E. F. & Karsenty, G. The molecular clock mediates leptin-regulated bone formation. Cell 122, 803–815 (2005).
Samsa, W. E., Vasanji, A., Midura, R. J. & Kondratov, R. V. Deficiency of circadian clock protein BMAL1 in mice results in a low bone mass phenotype. Bone 84, 194–203 (2016).
Komoto, S., Kondo, H., Fukuta, O. & Togari, A. Comparison of β-adrenergic and glucocorticoid signaling on clock gene and osteoblast-related gene expressions in human osteoblast. Chronobiol. Int. 29, 66–74 (2012).
Fujihara, Y., Kondo, H., Noguchi, T. & Togari, A. Glucocorticoids mediate circadian timing in peripheral osteoclasts resulting in the circadian expression rhythm of osteoclast-related genes. Bone 61, 1–9 (2014).
Yeung, C. Y. et al. Gremlin-2 is a BMP antagonist that is regulated by the circadian clock. Sci. Rep. 4, 5183 (2014).
McDearmon, E. L. et al. Dissecting the functions of the mammalian clock protein BMAL1 by tissue-specific rescue in mice. Science 314, 1304–1308 (2006).
Bunger, M. K. et al. Progressive arthropathy in mice with a targeted disruption of the Mop3/Bmal-1 locus. Genesis 41, 122–132 (2005).
Brown, S. A., Pagani, L., Cajochen, C. & Eckert, A. Systemic and cellular reflections on ageing and the circadian oscillator: a mini-review. Gerontology 57, 427–434 (2011).
Khapre, R. V., Kondratova, A. A., Susova, O. & Kondratov, R. V. Circadian clock protein BMAL1 regulates cellular senescence in vivo. Cell Cycle 10, 4162–4169 (2011).
Turek, F. W. et al. Obesity and metabolic syndrome in circadian Clock mutant mice. Science 308, 1043–1045 (2005).
Brown, S. A., Schmitt, K. & Eckert, A. Aging and circadian disruption: causes and effects. Aging 3, 813–817 (2011).
Davidson, A. J., Yamazaki, S., Arble, D. M., Menaker, M. & Block, G. D. Resetting of central and peripheral circadian oscillators in aged rats. Neurobiol. Aging 29, 471–477 (2008).
Sellix, M. T. et al. Aging differentially affects the re-entrainment response of central and peripheral circadian oscillators. J. Neurosci. 32, 16193–16202 (2012).
Pagani, L. et al. Serum factors in older individuals change cellular clock properties. Proc. Natl Acad. Sci. USA 108, 7218–7223 (2011).
Shane Anderson, A. & Loeser, R. F. Why is osteoarthritis an age-related disease? Best Pract. Res. Clin. Rheumatol. 24, 15–26 (2010).
Green, C. B., Takahashi, J. S. & Bass, J. The meter of metabolism. Cell 134, 728–742 (2008).
Shi, S. Q., Ansari, T. S., McGuinness, O. P., Wasserman, D. H. & Johnson, C. H. Circadian disruption leads to insulin resistance and obesity. Curr. Biol. 23, 372–381 (2013).
Zhuo, Q., Yang, W., Chen, J. & Wang, Y. Metabolic syndrome meets osteoarthritis. Nat. Rev. Rheumatol. 8, 729–737 (2012).
Janich, P. et al. Human epidermal stem cell function is regulated by circadian oscillations. Cell Stem Cell 13, 745–753 (2013).
Bhosale, A. M. & Richardson, J. B. Articular cartilage: structure, injuries and review of management. Br. Med. Bull. 87, 77–95 (2008).
Kc, R. et al. Environmental disruption of circadian rhythm predisposes mice to osteoarthritis-like changes in knee joint. J. Cell. Physiol. 230, 2174–2183 (2015).
Matsushita, T. et al. The overexpression of SIRT1 inhibited osteoarthritic gene expression changes induced by interleukin-1β in human chondrocytes. J. Orthop. Res. 31, 531–537 (2013).
Matsuzaki, T. et al. Disruption of Sirt1 in chondrocytes causes accelerated progression of osteoarthritis under mechanical stress and during ageing in mice. Ann. Rheum. Dis. 73, 1397–1404 (2014).
Gabay, O. et al. Increased apoptotic chondrocytes in articular cartilage from adult heterozygous SirT1 mice. Ann. Rheum. Dis. 71, 613–616 (2012).
Gabay, O. et al. Sirtuin 1 enzymatic activity is required for cartilage homeostasis in vivo in a mouse model. Arthritis Rheum. 65, 159–166 (2013).
Chang, H.-C. & Guarente, L. SIRT1 mediates central circadian control in the SCN by a mechanism that decays with aging. Cell 153, 1448–1460 (2013).
Ramsey, K. M. et al. Circadian clock feedback cycle through NAMPT-mediated NAD+ biosynthesis. Science 324, 651–654 (2009).
Nakahata, Y. et al. The NAD+-dependent deacetylase SIRT1 modulates CLOCK-mediated chromatin remodeling and circadian control. Cell 134, 329–340 (2008).
Nakahata, Y., Sahar, S., Astarita, G., Kaluzova, M. & Sassone-Corsi, P. Circadian control of the NAD+ salvage pathway by CLOCK-SIRT1. Science 324, 654–657 (2009).
Asher, G. et al. SIRT1 regulates circadian clock gene expression through PER2 deacetylation. Cell 134, 317–328 (2008).
Eckel-Mahan, K. & Sassone-Corsi, P. Metabolism control by the circadian clock and vice versa. Nat. Struct. Mol. Biol. 16, 462–467 (2009).
la Fleur, S. E. & Serlie, M. J. The interaction between nutrition and the brain and its consequences for body weight gain and metabolism; studies in rodents and men. Best Pract. Res. Clin. Endocrinol. Metab. 28, 649–659 (2014).
Ruiter, M. et al. The daily rhythm in plasma glucagon concentrations in the rat is modulated by the biological clock and by feeding behavior. Diabetes 52, 1709–1715 (2003).
Ando, H. et al. Rhythmic messenger ribonucleic acid expression of clock genes and adipocytokines in mouse visceral adipose tissue. Endocrinology 146, 5631–5636 (2005).
Bodosi, B. et al. Rhythms of ghrelin, leptin, and sleep in rats: effects of the normal diurnal cycle, restricted feeding, and sleep deprivation. Am. J. Physiol. Regul. Integr. Comp. Physiol. 287, R1071–R1079 (2004).
Accili, D. et al. The mind and the belly: a glance at how the nervous system directs metabolism. Diabetes Obes. Metab. 16, 1–3 (2014).
Bellet, M. M. & Sassone-Corsi, P. Mammalian circadian clock and metabolism — the epigenetic link. J. Cell Sci. 123, 3837–3848 (2010).
Kohsaka, A. et al. High-fat diet disrupts behavioral and molecular circadian rhythms in mice. Cell Metab. 6, 414–421 (2007).
Lane, N. E. et al. Tanezumab for the treatment of pain from osteoarthritis of the knee. N. Eng. J. Med. 363, 1521–1531 (2010).
European Medicines Agency. clinicaltrialsregister.eu, https://www.clinicaltrialsregister.eu/ctr-search/search?query=2014-004805-34 (2014).
European Medicines Agency. clinicaltrialsregister.eu, https://www.clinicaltrialsregister.eu/ctr-search/search?query=2015-001136-37 (2015).
Levine, Y. A. et al. Neurostimulation of the cholinergic anti-inflammatory pathway ameliorates disease in rat collagen-induced arthritis. PLoS ONE 9, e104530 (2014).
Zitnik, R. J. Treatment of chronic inflammatory diseases with implantable medical devices. Ann. Rheum. Dis. 70, i67–i70 (2011).
Simoni, A. et al. A mechanosensory pathway to the Drosophila circadian clock. Science 343, 525–528 (2014).
Feillet, C. A. et al. Lack of food anticipation in Per2 mutant mice. Curr. Biol. 16, 2016–2022 (2006).
Hughes, A. T. & Piggins, H. D. Feedback actions of locomotor activity to the circadian clock. Prog. Brain Res. 199, 305–336 (2012).
Zhang, R., Lahens, N. F., Ballance, H. I., Hughes, M. E. & Hogenesch, J. B. A circadian gene expression atlas in mammals: implications for biology and medicine. Proc. Natl Acad. Sci. USA 111, 16219–16224 (2014).
Hirota, T. et al. Identification of small molecule activators of cryptochrome. Science 337, 1094–1097 (2012).
Solt, L. A. et al. Regulation of circadian behaviour and metabolism by synthetic REV-ERB agonists. Nature 485, 62–68 (2012).
Meng, Q. J. et al. Ligand modulation of REV-ERBα function resets the peripheral circadian clock in a phasic manner. J. Cell Sci. 121, 3629–3635 (2008).
Meng, Q. J. et al. Entrainment of disrupted circadian behavior through inhibition of casein kinase 1 (CK1) enzymes. Proc. Natl Acad. Sci. USA 107, 15240–15245 (2010).
Kaur, G., Phillips, C., Wong, K. & Saini, B. Timing is important in medication administration: a timely review of chronotherapy research. Int. J. Clin. Pharm. 35, 344–358 (2013).
Levi, F., Le Louarn, C. & Reinberg, A. Timing optimizes sustained-release indomethacin treatment of osteoarthritis. Clin. Pharmacol. Ther. 37, 77–84 (1985).
Gautron, L., Elmquist, J. K. & Williams, K. W. Neural control of energy balance: translating circuits to therapies. Cell 161, 133–145 (2015).
Acknowledgements
F.B.'s work is supported by the Arthritis Foundation R&D (ROAD: Research on Osteoarthritic Diseases) and by the French Society of Rheumatology. Q.-J.M's work is supported by Arthritis Research UK and the Medical Research Council (UK).
Author information
Authors and Affiliations
Contributions
F.B. and Q.-J.M. researched the data for the article, contributed equally to discussions of its content, wrote the manuscript, and undertook review or editing of the manuscript before submission.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Berenbaum, F., Meng, QJ. The brain–joint axis in osteoarthritis: nerves, circadian clocks and beyond. Nat Rev Rheumatol 12, 508–516 (2016). https://doi.org/10.1038/nrrheum.2016.93
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2016.93
This article is cited by
-
Hypertension contributes to exacerbated osteoarthritis pathophysiology in rats in a sex-dependent manner
Arthritis Research & Therapy (2023)
-
Rhythm disturbance in osteoarthritis
Cell Communication and Signaling (2022)
-
Soluble CCR2 gene therapy controls joint inflammation, cartilage damage, and the progression of osteoarthritis by targeting MCP-1 in a monosodium iodoacetate (MIA)-induced OA rat model
Journal of Translational Medicine (2022)
-
The role of HIF proteins in maintaining the metabolic health of the intervertebral disc
Nature Reviews Rheumatology (2021)
-
Clocking in to immunity
Nature Reviews Immunology (2018)