Key Points
-
Populations of T cells that are specific for tumour-associated antigens can be expanded to generate large numbers of cells and transferred into tumour-bearing hosts, a process known as adoptive cell transfer (ACT)-based immunotherapy.
-
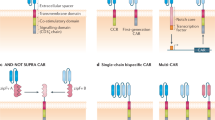
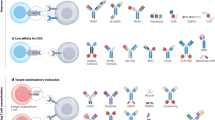
T cells can be genetically engineered to express αβ T cell receptors (which recognize MHC-restricted peptide antigens) or chimeric antigen receptors, which are antibody-like structures capable of recognizing structures on the surface of tumour cells or tumour-associated cells.
-
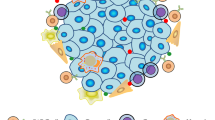
Tumours are complex masses that comprise numerous cell types, including transformed cells as well as non-transformed stromal cells and immune cells (such as myeloid cells and various T cell subsets).
-
Transformed cells (tumour cells) express mutated genes and genes that are normally epigenetically repressed in most adult tissues, and these genes can trigger tumour masses to grow uncontrollably, resist death and invade tissues. The products of these genes can be targeted by immunotherapy.
-
ACT can be improved by destroying host elements that interfere with the function of tumour-specific T cells. This can be accomplished using lymphodepletion mediated by chemotherapy or total-body irradiation.
-
The differentiation state of tumour-specific T cells affects the efficacy of T cell-based immunotherapy. 'Younger', less-differentiated T cells are more effective than cells that have fully acquired effector functions.
-
DNA sequencing might be useful in the identification of targetable neo-antigens expressed by tumours.
-
New combinations of ACT-based immunotherapy with 'targeted therapies' offer promising new directions.
Abstract
Immunotherapy based on the adoptive transfer of naturally occurring or gene-engineered T cells can mediate tumour regression in patients with metastatic cancer. Here, we discuss progress in the use of adoptively transferred T cells, focusing on how they can mediate tumour cell eradication. Recent advances include more accurate targeting of antigens expressed by tumours and the associated vasculature, and the successful use of gene engineering to re-target T cells before their transfer into the patient. We also describe how new research has helped to identify the particular T cell subsets that can most effectively promote tumour eradication.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Deguine, J., Breart, B., Lemaitre, F., Di Santo, J. P. & Bousso, P. Intravital imaging reveals distinct dynamics for natural killer and CD8+ T cells during tumor regression. Immunity 33, 632–644 (2010).
Kochenderfer, J. N. et al. Eradication of B-lineage cells and regression of lymphoma in a patient treated with autologous T cells genetically engineered to recognize CD19. Blood 116, 4099–4102 (2010).
Brentjens, R. J. et al. Safety and persistence of adoptively transferred autologous CD19-targeted T cells in patients with relapsed or chemotherapy refractory B-cell leukemias. Blood 118, 4817–4828 (2011).
Rosenberg, S. A. et al. Durable complete responses in heavily pretreated patients with metastatic melanoma using T-cell transfer immunotherapy. Clin. Cancer Res. 17, 4550–4557 (2011).
Porter, D. L., Levine, B. L., Kalos, M., Bagg, A. & June, C. H. Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N. Engl. J. Med. 365, 725–733 (2011).
Robbins, P. F. et al. Tumor regression in patients with metastatic synovial cell sarcoma and melanoma using genetically engineered lymphocytes reactive with NY-ESO-1. J. Clin. Oncol. 29, 917–924 (2011). This study provides evidence that gene-engineered T cells can treat other solid tumour histologies (in this case, metastatic synovial cell sarcoma), in addition to melanoma.
Kochenderfer, J. N. et al. B-cell depletion and remissions of malignancy along with cytokine-associated toxicity in a clinical trial of anti-CD19 chimeric-antigen-receptor-transduced T cells. Blood 8 Dec 2011 (doi:10.1182/blood-2011-10-384388). References 2, 3, 5 and 7 demonstrate the therapeutic power of genetically engineered T cells in the treatment of CD19+ lymphoma.
Baitsch, L. et al. Exhaustion of tumor-specific CD8 T cells in metastases from melanoma patients. J. Clin. Invest. 121, 2350–2360 (2011).
Ahmadzadeh, M. et al. Tumor antigen-specific CD8 T cells infiltrating the tumor express high levels of PD-1 and are functionally impaired. Blood 114, 1537–1544 (2009).
Offringa, R. Antigen choice in adoptive T-cell therapy of cancer. Curr. Opin. Immunol. 21, 190–199 (2009).
Restifo, N. P. et al. Identification of human cancers deficient in antigen processing. J. Exp. Med. 177, 265–272 (1993).
Restifo, N. P. et al. Loss of functional β2-microglobulin in metastatic melanomas from five patients receiving immunotherapy. J. Natl Cancer Inst. 88, 100–108 (1996).
Schreiber, R. D., Old, L. J. & Smyth, M. J. Cancer immunoediting: integrating immunity's roles in cancer suppression and promotion. Science 331, 1565–1570 (2011).
Matsushita, H. et al. Cancer exome analysis reveals a T-cell-dependent mechanism of cancer immunoediting. Nature 482, 400–404 (2012).
van der Bruggen, P. et al. A gene encoding an antigen recognized by cytolytic T lymphocytes on a human melanoma. Science 254, 1643–1647 (1991).
Parkhurst, M. R. et al. T cells targeting carcinoembryonic antigen can mediate regression of metastatic colorectal cancer but induce severe transient colitis. Mol. Ther. 19, 620–626 (2011).
Bos, R. et al. Balancing between antitumor efficacy and autoimmune pathology in T-cell-mediated targeting of carcinoembryonic antigen. Cancer Res. 68, 8446–8455 (2008).
Overwijk, W. W. & Restifo, N. P. Autoimmunity and the immunotherapy of cancer: targeting the “self” to destroy the “other”. Crit. Rev. Immunol. 20, 433–450 (2000).
Overwijk, W. W. et al. gp100/pmel 17 is a murine tumor rejection antigen: induction of “self”-reactive, tumoricidal T cells using high-affinity, altered peptide ligand. J. Exp. Med. 188, 277–286 (1998).
Kawakami, Y. et al. Cloning of the gene coding for a shared human melanoma antigen recognized by autologous T cells infiltrating into tumor. Proc. Natl Acad. Sci. USA 91, 3515–3519 (1994).
Johnson, L. A. et al. Gene therapy with human and mouse T-cell receptors mediates cancer regression and targets normal tissues expressing cognate antigen. Blood 114, 535–546 (2009).
Palmer, D. C. et al. Effective tumor treatment targeting a melanoma/melanocyte-associated antigen triggers severe ocular autoimmunity. Proc. Natl Acad. Sci. USA 105, 8061–8066 (2008).
Yeh, S. et al. Ocular and systemic autoimmunity after successful tumor-infiltrating lymphocyte immunotherapy for recurrent, metastatic melanoma. Ophthalmology 116, 981–989 (2009).
Davies, M. A. & Samuels, Y. Analysis of the genome to personalize therapy for melanoma. Oncogene 29, 5545–5555 (2010).
Walia, V., Mu, E. W., Lin, J. C. & Samuels, Y. Delving into somatic variation in sporadic melanoma. Pigment Cell Melanoma Res. 25, 155–170 (2012).
Gilchrest, B. A. Molecular aspects of tanning. J. Invest. Dermatol. 131, e14–e17 (2011).
Robbins, P. F. et al. A mutated β-catenin gene encodes a melanoma-specific antigen recognized by tumor infiltrating lymphocytes. J. Exp. Med. 183, 1185–1192 (1996).
Brenner, M. K. & Heslop, H. E. Adoptive T cell therapy of cancer. Curr. Opin. Immunol. 22, 251–257 (2010).
Kenter, G. G. et al. Vaccination against HPV-16 oncoproteins for vulvar intraepithelial neoplasia. N. Engl. J. Med. 361, 1838–1847 (2009).
Anders, K. et al. Oncogene-targeting T cells reject large tumors while oncogene inactivation selects escape variants in mouse models of cancer. Cancer Cell 20, 755–767 (2011).
Zhang, J. et al. A novel retinoblastoma therapy from genomic and epigenetic analyses. Nature 481, 329–334 (2012).
Hofmann, O. et al. Genome-wide analysis of cancer/testis gene expression. Proc. Natl Acad. Sci. USA 105, 20422–20427 (2008).
Almeida, L. G. et al. CTdatabase: a knowledge-base of high-throughput and curated data on cancer-testis antigens. Nucleic Acids Res. 37, D816–D819 (2009).
Baylin, S. B. & Jones, P. A. A decade of exploring the cancer epigenome — biological and translational implications. Nature Rev. Cancer 11, 726–734 (2011).
Guo, Z. S. et al. De novo induction of a cancer/testis antigen by 5-aza-2′-deoxycytidine augments adoptive immunotherapy in a murine tumor model. Cancer Res. 66, 1105–1113 (2006).
Wargo, J. A. et al. Recognition of NY-ESO-1+ tumor cells by engineered lymphocytes is enhanced by improved vector design and epigenetic modulation of tumor antigen expression. Cancer Immunol. Immunother. 58, 383–394 (2009).
Simpson, A. J., Caballero, O. L., Jungbluth, A., Chen, Y. T. & Old, L. J. Cancer/testis antigens, gametogenesis and cancer. Nature Rev. Cancer 5, 615–625 (2005).
Chinnasamy, N. et al. A TCR targeting the HLA-A*0201-restricted epitope of MAGE-A3 recognizes multiple epitopes of the MAGE-A antigen superfamily in several types of cancer. J. Immunol. 186, 685–696 (2011).
Ruffell, B. et al. Leukocyte composition of human breast cancer. Proc. Natl Acad. Sci. USA 8 Aug 2011 (doi:10.1073/pnas.1104303108).
Engels, B., Rowley, D. A. & Schreiber, H. Targeting stroma to treat cancers. Semin. Cancer Biol. 22, 41–49 (2012).
Kraman, M. et al. Suppression of antitumor immunity by stromal cells expressing fibroblast activation protein-α. Science 330, 827–830 (2010).
Chinnasamy, D. et al. Gene therapy using genetically modified lymphocytes targeting VEGFR-2 inhibits the growth of vascularized syngenic tumors in mice. J. Clin. Invest. 120, 3953–3968 (2010).
Shrimali, R. K. et al. Antiangiogenic agents can increase lymphocyte infiltration into tumor and enhance the effectiveness of adoptive immunotherapy of cancer. Cancer Res. 70, 6171–6180 (2010).
Chung, A. S., Lee, J. & Ferrara, N. Targeting the tumour vasculature: insights from physiological angiogenesis. Nature Rev. Cancer 10, 505–514 (2010).
Fefer, A. Immunotherapy and chemotherapy of Moloney sarcoma virus-induced tumors in mice. Cancer Res. 29, 2177–2183 (1969).
Greenberg, P. D., Cheever, M. A. & Fefer, A. Eradication of disseminated murine leukemia by chemoimmunotherapy with cyclophosphamide and adoptively transferred immune syngeneic Lyt-1+2− lymphocytes. J. Exp. Med. 154, 952–963 (1981). An important and remarkable landmark paper that describes in significant detail the scientific foundations of lymphodepletion prior to adoptive immunotherapy using what are now known as CD4+ T cells.
Rosenberg, S. A. & Terry, W. D. Passive immunotherapy of cancer in animals and man. Adv. Cancer Res. 25, 323–388 (1977).
Wang, M. et al. Active immunotherapy of cancer with a nonreplicating recombinant fowlpox virus encoding a model tumor-associated antigen. J. Immunol. 154, 4685–4692 (1995).
Palmer, D. C. et al. Vaccine-stimulated, adoptively transferred CD8+ T cells traffic indiscriminately and ubiquitously while mediating specific tumor destruction. J. Immunol. 173, 7209–7216 (2004).
Chen, P. W. et al. Therapeutic antitumor response after immunization with a recombinant adenovirus encoding a model tumor-associated antigen. J. Immunol. 156, 224–231 (1996).
Bronte, V. et al. IL-2 enhances the function of recombinant poxvirus-based vaccines in the treatment of established pulmonary metastases. J. Immunol. 154, 5282–5292 (1995).
Cormier, J. N. et al. Enhancement of cellular immunity in melanoma patients immunized with a peptide from MART-1/Melan A. Cancer J. Sci. Am. 3, 37–44 (1997).
Leitner, W. W. et al. Alphavirus-based DNA vaccine breaks immunological tolerance by activating innate antiviral pathways. Nature Med. 9, 33–39 (2003).
Ying, H. et al. Cancer therapy using a self-replicating RNA vaccine. Nature Med. 5, 823–827 (1999).
Overwijk, W. W. et al. Vaccination with a recombinant vaccinia virus encoding a “self” antigen induces autoimmune vitiligo and tumor cell destruction in mice: requirement for CD4+ T lymphocytes. Proc. Natl Acad. Sci. USA 96, 2982–2987 (1999).
Rosenberg, S. A. et al. Tumor progression can occur despite the induction of very high levels of self/tumor antigen-specific CD8+ T cells in patients with melanoma. J. Immunol. 175, 6169–6176 (2005).
Irvine, K. R. et al. Enhancing efficacy of recombinant anticancer vaccines with prime/boost regimens that use two different vectors. J. Natl Cancer Inst. 89, 1595–1601 (1997).
Rao, J. B. et al. IL-12 is an effective adjuvant to recombinant vaccinia virus-based tumor vaccines: enhancement by simultaneous B7–1 expression. J. Immunol. 156, 3357–3365 (1996).
Irvine, K. R. et al. Recombinant virus vaccination against “self” antigens using anchor-fixed immunogens. Cancer Res. 59, 2536–2540 (1999).
Irvine, K. R., Rao, J. B., Rosenberg, S. A. & Restifo, N. P. Cytokine enhancement of DNA immunization leads to effective treatment of established pulmonary metastases. J. Immunol. 156, 238–245 (1996).
Carroll, M. W. et al. Construction and characterization of a triple-recombinant vaccinia virus encoding B7–1, interleukin 12, and a model tumor antigen. J. Natl Cancer Inst. 90, 1881–1887 (1998).
Schlom, J. Recent advances in therapeutic cancer vaccines. Cancer Biother. Radiopharm. 27, 2–5 (2012).
Rosenberg, S. A., Yang, J. C. & Restifo, N. P. Cancer immunotherapy: moving beyond current vaccines. Nature Med. 10, 909–915 (2004).
Klebanoff, C. A., Acquavella, N., Yu, Z. & Restifo, N. P. Therapeutic cancer vaccines: are we there yet? Immunol. Rev. 239, 27–44 (2011). An update on recent vaccine trials showing that although current therapeutic cancer vaccines can extend survival in some studies (by months, not years), they are rarely if ever curative.
Kantoff, P. W. et al. Sipuleucel-T immunotherapy for castration-resistant prostate cancer. N. Engl. J. Med. 363, 411–422 (2010). Although criticized by some for the trial design, this study nevertheless served as a key basis for the FDA licensing of sipuleucel-T (Provenge; Dendreon).
Itzhaki, O. et al. Establishment and large-scale expansion of minimally cultured “young” tumor infiltrating lymphocytes for adoptive transfer therapy. J. Immunother. 34, 212–220 (2011).
Besser, M. J. et al. Clinical responses in a phase II study using adoptive transfer of short-term cultured tumor infiltration lymphocytes in metastatic melanoma patients. Clin. Cancer Res. 16, 2646–2655 (2010).
Klebanoff, C. A. et al. Determinants of successful CD8+ T-cell adoptive immunotherapy for large established tumors in mice. Clin. Cancer Res. 17, 5343–5352 (2011).
Khong, H. T. & Restifo, N. P. Natural selection of tumor variants in the generation of “tumor escape” phenotypes. Nature Immunol. 3, 999–1005 (2002).
Ogino, S., Galon, J., Fuchs, C. S. & Dranoff, G. Cancer immunology-analysis of host and tumor factors for personalized medicine. Nature Rev. Clin. Oncol. 8, 711–719 (2011).
Stratton, M. R. Exploring the genomes of cancer cells: progress and promise. Science 331, 1553–1558 (2011).
Louis, C. U. et al. Antitumor activity and long-term fate of chimeric antigen receptor-positive T cells in patients with neuroblastoma. Blood 118, 6050–6056 (2011).
Kochenderfer, J. N., Yu, Z., Frasheri, D., Restifo, N. P. & Rosenberg, S. A. Adoptive transfer of syngeneic T cells transduced with a chimeric antigen receptor that recognizes murine CD19 can eradicate lymphoma and normal B cells. Blood 116, 3875–3886 (2010).
Kerkar, S. P. et al. Genetic engineering of murine CD8+ and CD4+ T cells for preclinical adoptive immunotherapy studies. J. Immunother. 34, 343–352 (2011).
Abad, J. D. et al. T-cell receptor gene therapy of established tumors in a murine melanoma model. J. Immunother. 31, 1–6 (2008).
Morgan, R. A. et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 314, 126–129 (2006).
Pule, M. A. et al. Virus-specific T cells engineered to coexpress tumor-specific receptors: persistence and antitumor activity in individuals with neuroblastoma. Nature Med. 14, 1264–1270 (2008).
Recombinant DNA Advisory Committee. Human gene transfer protocols. National Institutes of Health [online], (2011).
Varela-Rohena, A. et al. Control of HIV-1 immune escape by CD8 T cells expressing enhanced T-cell receptor. Nature Med. 14, 1390–1395 (2008).
Sadelain, M., Brentjens, R. & Riviere, I. The promise and potential pitfalls of chimeric antigen receptors. Curr. Opin. Immunol. 21, 215–223 (2009).
Morgan, R. A. et al. Case report of a serious adverse event following the administration of T cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol. Ther. 18, 843–851 (2010).
Baeuerle, P. A. & Itin, C. Clinical experience with gene therapy and bispecific antibodies for T cell-based therapy of cancer. Curr. Pharm. Biotechnol. 14 Feb 2012 [epub ahead of print].
Choi, B. D. et al. Bispecific antibodies engage T cells for antitumor immunotherapy. Expert Opin. Biol. Ther. 11, 843–853 (2011).
Merhavi-Shoham, E., Haga-Friedman, A. & Cohen, C. J. Genetically modulating T-cell function to target cancer. Semin. Cancer Biol. 22, 14–22 (2011).
Gattinoni, L. et al. A human memory T cell subset with stem cell-like properties. Nature Med. 17, 1290–1297 (2011).
Stephan, M. T. et al. T cell-encoded CD80 and 4–1BBL induce auto- and transcostimulation, resulting in potent tumor rejection. Nature Med. 13, 1440–1449 (2007).
Charo, J. et al. Bcl-2 overexpression enhances tumor-specific T-cell survival. Cancer Res. 65, 2001–2008 (2005).
Pegram, H. J. et al. Tumor-targeted T cells modified to secrete IL-12 eradicate systemic tumors without need for prior conditioning. Blood 21 Feb 2012 (doi:10.1182/blood-2011-12-400044).
Kerkar, S. P. et al. IL-12 triggers a programmatic change in dysfunctional myeloid-derived cells within mouse tumors. J. Clin. Invest. 121, 4746–4757 (2011).
Kerkar, S. P. et al. Tumor-specific CD8+ T cells expressing interleukin-12 eradicate established cancers in lymphodepleted hosts. Cancer Res. 70, 6725–6734 (2010).
Peng, W. et al. Transduction of tumor-specific T cells with CXCR2 chemokine receptor improves migration to tumor and antitumor immune responses. Clin. Cancer Res. 16, 5458–5468 (2010).
Bendle, G. M. et al. Lethal graft-versus-host disease in mouse models of T cell receptor gene therapy. Nature Med. 16, 565–570 (2010). An important paper that explores in significant detail the consequences of 'mispairing' of transduced TCR α- and β-chains.
Rosenberg, S. A. Of mice, not men: no evidence for graft-versus-host disease in humans receiving T-cell receptor-transduced autologous T cells. Mol. Ther. 18, 1744–1745 (2010).
Vatakis, D. N. et al. Antitumor activity from antigen-specific CD8 T cells generated in vivo from genetically engineered human hematopoietic stem cells. Proc. Natl Acad. Sci. USA 108, e1408–e1416 (2011).
Ha, S. P. et al. Transplantation of mouse HSCs genetically modified to express a CD4-restricted TCR results in long-term immunity that destroys tumors and initiates spontaneous autoimmunity. J. Clin. Invest. 120, 4273–4288 (2010).
Jorritsma, A., Schotte, R., Coccoris, M., de Witte, M. A. & Schumacher, T. N. Prospects and limitations of T cell receptor gene therapy. Curr. Gene Ther. 11, 276–287 (2011).
Brentjens, R., Yeh, R., Bernal, Y., Riviere, I. & Sadelain, M. Treatment of chronic lymphocytic leukemia with genetically targeted autologous T cells: case report of an unforeseen adverse event in a phase I clinical trial. Mol. Ther. 18, 666–668 (2010).
Di Stasi, A. et al. Inducible apoptosis as a safety switch for adoptive cell therapy. N. Engl. J. Med. 365, 1673–1683 (2011). This paper describes a highly effective means of rapidly deleting gene-engineered T cells in the event of toxicity.
North, R. J. Cyclophosphamide-facilitated adoptive immunotherapy of an established tumor depends on elimination of tumor-induced suppressor T cells. J. Exp. Med. 155, 1063–1074 (1982).
Cheever, M. A., Greenberg, P. D. & Fefer, A. Specificity of adoptive chemoimmunotherapy of established syngeneic tumors. J. Immunol. 125, 711–714 (1980).
Bronte, V. et al. Identification of a CD11b+/Gr-1+/CD31+ myeloid progenitor capable of activating or suppressing CD8+T cells. Blood 96, 3838–3846 (2000).
Wrzesinski, C. et al. Hematopoietic stem cells promote the expansion and function of adoptively transferred antitumor CD8 T cells. J. Clin. Invest. 117, 492–501 (2007).
Wrzesinski, C. et al. Increased intensity lymphodepletion enhances tumor treatment efficacy of adoptively transferred tumor-specific T cells. J. Immunother. 33, 1–7 (2010).
Dudley, M. E. et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 298, 850–854 (2002).
Dudley, M. E. et al. Adoptive cell therapy for patients with metastatic melanoma: evaluation of intensive myeloablative chemoradiation preparative regimens. J. Clin. Oncol. 26, 5233–5239 (2008).
Gabrilovich, D. I., Ostrand-Rosenberg, S. & Bronte, V. Coordinated regulation of myeloid cells by tumours. Nature Rev. Immunol. 12, 253–268 (2012).
Bronte, V. et al. Apoptotic death of CD8+ T lymphocytes after immunization: induction of a suppressive population of Mac-1+/Gr-1+ cells. J. Immunol. 161, 5313–5320 (1998). One of the first descriptions of the suppressive myeloid subset later known as MDSCs.
Seung, L. P., Rowley, D. A., Dubey, P. & Schreiber, H. Synergy between T-cell immunity and inhibition of paracrine stimulation causes tumor rejection. Proc. Natl Acad. Sci. USA 92, 6254–6258 (1995). This paper describes a classic experiment demonstrating that depletion of GR1+ cells can enhance tumour immunotherapy.
Gattinoni, L. et al. Removal of homeostatic cytokine sinks by lymphodepletion enhances the efficacy of adoptively transferred tumor-specific CD8+ T cells. J. Exp. Med. 202, 907–912 (2005).
Paulos, C. M. et al. Microbial translocation augments the function of adoptively transferred self/tumor-specific CD8+ T cells via TLR4 signaling. J. Clin. Invest. 117, 2197–2204 (2007).
Antony, P. A. et al. CD8+ T cell immunity against a tumor/self-antigen is augmented by CD4+ T helper cells and hindered by naturally occurring T regulatory cells. J. Immunol. 174, 2591–2601 (2005).
Kastenmuller, W. et al. Regulatory T cells selectively control CD8+ T cell effector pool size via IL-2 restriction. J. Immunol. 187, 3186–3197 (2011).
Antony, P. A. & Restifo, N. P. CD4+CD25+ T regulatory cells, immunotherapy of cancer, and interleukin-2. J. Immunother. 28, 120–128 (2005).
Bluestone, J. A. The yin and yang of interleukin-2-mediated immunotherapy. N. Engl. J. Med. 365, 2129–2131 (2011).
Gattinoni, L. et al. Acquisition of full effector function in vitro paradoxically impairs the in vivo antitumor efficacy of adoptively transferred CD8+ T cells. J. Clin. Invest. 115, 1616–1626 (2005).
Gattinoni, L., Powell, D. J. Jr, Rosenberg, S. A. & Restifo, N. P. Adoptive immunotherapy for cancer: building on success. Nature Rev. Immunol. 6, 383–393 (2006).
Sallusto, F. & Lanzavecchia, A. Memory in disguise. Nature Med. 17, 1182–1183 (2011).
Klebanoff, C. A., Gattinoni, L. & Restifo, N. P. CD8+ T-cell memory in tumor immunology and immunotherapy. Immunol. Rev. 211, 214–224 (2006).
Palmer, D. C. & Restifo, N. P. Suppressors of cytokine signaling (SOCS) in T cell differentiation, maturation, and function. Trends Immunol. 30, 592–602 (2009).
Hinrichs, C. S. et al. Adoptively transferred effector cells derived from naive rather than central memory CD8+ T cells mediate superior antitumor immunity. Proc. Natl Acad. Sci. USA 106, 17469–17474 (2009).
Hinrichs, C. S. et al. Human effector CD8+ T cells derived from naive rather than memory subsets possess superior traits for adoptive immunotherapy. Blood 117, 808–814 (2011).
Klebanoff, C. A. et al. Central memory self/tumor-reactive CD8+ T cells confer superior antitumor immunity compared with effector memory T cells. Proc. Natl Acad. Sci. USA 102, 9571–9576 (2005).
Klebanoff, C. A. et al. IL-15 enhances the in vivo antitumor activity of tumor-reactive CD8+ T cells. Proc. Natl Acad. Sci. USA 101, 1969–1974 (2004).
Berger, C. et al. Adoptive transfer of effector CD8+ T cells derived from central memory cells establishes persistent T cell memory in primates. J. Clin. Invest. 118, 294–305 (2008). An important study in non-human primates showing that cells derived from central memory T cells are more persistentthan those derived from effector memory T cells.
Wang, X. et al. Engraftment of human central memory-derived effector CD8+ T cells in immunodeficient mice. Blood 117, 1888–1898 (2011).
Chapuis, A. et al. Transferred melanoma-specific CD8+ T cells persist, mediate tumor regression, and acquire central memory phenotype. 5 Mar 2012 (doi:10.1073/pnas.1113748109). References 122 and 126 show that central memory T cells mediate superior antitumour immunity compared with effector memory T cells in murine systems.
Zhang, Y., Joe, G., Hexner, E., Zhu, J. & Emerson, S. G. Host-reactive CD8+ memory stem cells in graft-versus-host disease. Nature Med. 11, 1299–1305 (2005).
Gattinoni, L. et al. Wnt signaling arrests effector T cell differentiation and generates CD8+ memory stem cells. Nature Med. 15, 808–813 (2009).
Mackall, C. L., Fry, T. J. & Gress, R. E. Harnessing the biology of IL-7 for therapeutic application. Nature Rev. Immunol. 11, 330–342 (2011).
June, C. H., Bluestone, J. A., Nadler, L. M. & Thompson, C. B. The B7 and CD28 receptor families. Immunol. Today 15, 321–331 (1994).
Ji, Y. et al. Repression of the DNA-binding inhibitor Id3 by Blimp-1 limits the formation of memory CD8+ T cells. Nature Immunol. 12, 1230–1237 (2011).
Hinrichs, C. S. et al. IL-2 and IL-21 confer opposing differentiation programs to CD8+ T cells for adoptive immunotherapy. Blood 111, 5326–5333 (2008).
Singh, H. et al. Reprogramming CD19-specific T cells with IL-21 signaling can improve adoptive immunotherapy of B-lineage malignancies. Cancer Res. 71, 3516–3527 (2011).
Gattinoni, L., Ji, Y. & Restifo, N. P. Wnt/β-catenin signaling in T-cell immunity and cancer immunotherapy. Clin. Cancer Res. 16, 4695–4701 (2010).
Gattinoni, L., Klebanoff, C. A. & Restifo, N. P. Pharmacologic induction of CD8+ T cell memory: better living through chemistry. Sci. Transl. Med. 1, 11ps12 (2009).
Pardoll, D. M. & Topalian, S. L. The role of CD4+ T cell responses in antitumor immunity. Curr. Opin. Immunol. 10, 588–594 (1998).
Xie, Y. et al. Naive tumor-specific CD4+ T cells differentiated in vivo eradicate established melanoma. J. Exp. Med. 207, 651–667 (2010).
Quezada, S. A. et al. Tumor-reactive CD4+ T cells develop cytotoxic activity and eradicate large established melanoma after transfer into lymphopenic hosts. J. Exp. Med. 207, 637–650 (2010).
Mumberg, D. et al. CD4+ T cells eliminate MHC class II-negative cancer cells in vivo by indirect effects of IFN-γ. Proc. Natl Acad. Sci. USA 96, 8633–8638 (1999).
Corthay, A. et al. Primary antitumor immune response mediated by CD4+ T cells. Immunity 22, 371–383 (2005).
Martin-Orozco, N. et al. T helper 17 cells promote cytotoxic T cell activation in tumor immunity. Immunity 31, 787–798 (2009).
Muranski, P. et al. Tumor-specific Th17-polarized cells eradicate large established melanoma. Blood 112, 362–373 (2008).
Muranski, P. et al. Th17 cells are long lived and retain a stem cell-like molecular signature. Immunity 35, 972–985 (2011).
Frankel, T. L. et al. Both CD4 and CD8 T cells mediate equally effective in vivo tumor treatment when engineered with a highly avid TCR targeting tyrosinase. J. Immunol. 184, 5988–5998 (2010).
Yee, C. Adoptive therapy using antigen-specific T-cell clones. Cancer J. 16, 367–373 (2010).
Hunder, N. N. et al. Treatment of metastatic melanoma with autologous CD4+ T cells against NY-ESO-1. N. Engl. J. Med. 358, 2698–2703 (2008).
Nakayamada, S., Takahashi, H., Kanno, Y. & O'Shea, J. J. Helper T cell diversity and plasticity. Curr. Opin. Immunol. 15 Feb 2012 (doi:10.1016/j.coi.2012.01.014).
Nishimura, T. et al. The critical role of Th1-dominant immunity in tumor immunology. Cancer Chemother. Pharmacol. 46, S52–S61 (2000).
Muranski, P. & Restifo, N. P. Adoptive immunotherapy of cancer using CD4+ T cells. Curr. Opin. Immunol. 21, 200–208 (2009).
Zou, W. & Restifo, N. P. TH17 cells in tumour immunity and immunotherapy. Nature Rev. Immunol. 10, 248–256 (2010).
Muranski, P. & Restifo, N. P. Does IL-17 promote tumor growth? Blood 114, 231–232 (2009).
Hinrichs, C. S. et al. Type 17 CD8+ T cells display enhanced antitumor immunity. Blood 114, 596–599 (2009).
Yen, H. R. et al. Tc17 CD8 T cells: functional plasticity and subset diversity. J. Immunol. 183, 7161–7168 (2009).
Boni, A. et al. Adoptive transfer of allogeneic tumor-specific T cells mediates effective regression of large tumors across major histocompatibility barriers. Blood 112, 4746–4754 (2008).
Restifo, N. P. & Bachinski, M. Imagining a cure: for cancer patients, close is not good enough. The Scientist April 2011, 28–29 (2011).
Blank, C. U., Hooijkaas, A. I., Haanen, J. B. & Schumacher, T. N. Combination of targeted therapy and immunotherapy in melanoma. Cancer Immunol. Immunother. 60, 1359–1371 (2011).
Klebanoff, C. A. et al. Programming tumor-reactive effector memory CD8+ T cells in vitro obviates the requirement for in vivo vaccination. Blood 114, 1776–1783 (2009).
Overwijk, W. W. et al. Tumor regression and autoimmunity after reversal of a functionally tolerant state of self-reactive CD8+ T cells. J. Exp. Med. 198, 569–580 (2003).
Restifo, N. P. Can antitumor immunity help to explain “oncogene addiction”? Cancer Cell 18, 403–405 (2010).
Rakhra, K. et al. CD4+ T cells contribute to the remodeling of the microenvironment required for sustained tumor regression upon oncogene inactivation. Cancer Cell 18, 485–498 (2010). A paper that explores the immunological consequences of oncogene withdrawal.
Sumimoto, H., Imabayashi, F., Iwata, T. & Kawakami, Y. The BRAF–MAPK signaling pathway is essential for cancer-immune evasion in human melanoma cells. J. Exp. Med. 203, 1651–1656 (2006).
Boni, A. et al. Selective BRAFV600E inhibition enhances T-cell recognition of melanoma without affecting lymphocyte function. Cancer Res. 70, 5213–5219 (2010).
DuPage, M., Mazumdar, C., Schmidt, L. M., Cheung, A. F. & Jacks, T. Expression of tumour-specific antigens underlies cancer immunoediting. Nature 482, 405–409 (2012).
Staveley-O'Carroll, K. et al. Induction of antigen-specific T cell anergy: an early event in the course of tumor progression. Proc. Natl Acad. Sci. USA 95, 1178–1183 (1998).
Hung, K. et al. The central role of CD4+ T cells in the antitumor immune response. J. Exp. Med. 188, 2357–2368 (1998).
Kryczek, I. et al. Human TH17 cells are long-lived effector memory cells. Sci. Transl. Med. 3, 104ra100 (2011).
Acknowledgements
This work was supported by the Intramural Research Program of the Center for Cancer Research, US National Cancer Institute (NCI), National Institutes of Health. The authors would like to thank C. Klebanoff, L. Gattinoni, C. Hinrichs and P. Muranski for discussions about T cell differentiation, M. Bachinski for editorial help, E. Tran for critically reading the manuscript, and all the members of the translational immunology team at the NCI, especially J. C. Yang, P. F. Robbins, R. A. Morgan, R. M. Sherry, S. Feldman, M. Parkhurst, M. Hughes, G. Phan and U. Kammula.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Tumour-infiltrating lymphocyte
-
(TIL). A member of the heterogeneous population of T cells found in a tumour. TILs are characterized by a diversity of phenotypes, antigen specificities, avidities and functional characteristics. TIL populations can be activated and expanded ex vivo and re-infused into the tumour-bearing host.
- Interleukin-2
-
(IL-2). A T cell growth factor that is capable of triggering the expansion of both effector T cell and regulatory T cell populations. IL-2 is used to treat patients with melanoma and as a part of some ACT-based treatment regimes.
- Adoptive cell transfer
-
(ACT). The administration of tumour-specific lymphocytes (obtained from the patient (autologous) or from a donor (allogeneic)) following a lymphodepleting preparative regimen.
- Lymphodepletion
-
The use of total-body irradiation or cytotoxic drugs to deplete the lymphoid compartment in a patient.
- Myeloid-derived suppressor cells
-
(MDSCs). A group of immature CD11b+GR1+ cells (which include precursors of macrophages, granulocytes, dendritic cells and myeloid cells) that are produced in response to various tumour-derived cytokines. These cells have been shown to induce tolerance in tumour-associated CD8+ T cells.
- Cross-priming
-
The ability of certain antigen-presenting cells to load peptides that are derived from exogenous antigens onto MHC class I molecules. This property is atypical, because most cells exclusively present peptides from their endogenous proteins on MHC class I molecules.
- Immunoediting
-
A process by which the immune system of a host may alter the gene expression of an emerging tumour, such that the most immunogenic epitopes are removed or 'edited', thereby facilitating tumour escape from immune recognition.
- Carcinoembryonic antigen
-
A protein found in fetal gastrointestinal tissue that can be upregulated in some gastrointestinal cancers and can serve as a marker of tumour burden.
- Objective clinical responses
-
The response evaluation criteria in solid tumours (RECIST) define an objective response as a 30% reduction in the sum of the longest diameters of measurable tumour lesions when comparing post-treatment with pretreatment values. The World Health Organization criteria define an objective response to be a 50% reduction in the sum of the products of perpendicular diameters of measurable lesions. In both sets of criteria, no new lesions can appear. Perhaps the most important clinical end point is benefit from a treatment based on increased survival time, although this can only be assessed using controlled patient cohorts.
- Driver mutations
-
A nonsense mutation in a gene that causes a cancer cell to have a survival and/or growth advantage.
- Cancer–testis antigens
-
(Also known as cancer germline antigens). A class of >100 proteins that are expressed by many human cancers but not by normal adult tissues except in the testes and fetal ovaries. These antigens include CTAG1, MAGEA3 and SSX1.
- Complementarity-determining regions
-
Short amino acid sequences found in the variable domains of antigen receptor proteins that recognize an antigen and therefore provide the receptor with its specificity for that particular antigen.
- Directed evolution
-
A cyclic sequence of steps (including modification, selection and amplification) that is used, typically in vitro, to enrich for proteins or nucleic acids that show properties that are desired by the researcher but that are not necessarily found in nature.
- Chimeric antigen receptors
-
(CARs). Antigen receptors that contain sequences from more than one source, such as an antibody molecule, a T cell receptor signalling chain, and an activating motif.
- Homeostatic proliferation
-
A process of activation and proliferation of leukocytes in the lymphopenic environment. T cell homeostatic proliferation is driven by T cell receptor interactions with self-peptide–MHC complexes and T cell responsiveness to cytokines such as interleukin-7 (IL-7), IL-15 and possibly IL-21.
- Recombination-activating genes
-
These genes (Rag1 and Rag2) are expressed by developing lymphocytes. Mice that are deficient in either RAG protein fail to produce B and T cells owing to a developmental block in the gene rearrangement that is required for antigen receptor expression.
- Allelic exclusion
-
A mechanism that ensures that a lymphocyte expresses antigen receptors of only a single specificity at its cell surface. This is an integral step in the clonal commitment of a lymphocyte lineage.
- Cytokine storm
-
A sudden surge in the circulating levels of pro-inflammatory cytokines, such as interleukin-1, interleukin-6, tumour necrosis factor and interferon-γ. Clinically, this can result in hypotension, acute renal failure, poor pulmonary function and even death.
- Central memory T cell
-
(TCM cell). An antigen-experienced CD8+ T cell that lacks immediate effector function but is able to mediate rapid recall responses. These cells also rapidly develop the phenotype and function of effector memory T cells after re-stimulation with antigen. TCM cells retain the migratory properties of naive T cells and therefore circulate through the secondary lymphoid organs.
- Effector memory T cell
-
(TEM cell). A terminally differentiated T cell that lacks lymph-node-homing receptors but expresses receptors that enable it to home to inflamed tissues. TEM cells can exert immediate effector functions without the need for further differentiation.
- Telomere
-
The segment at the end of chromosome arms, which consists of a series of repeated DNA sequences (TTAGGG in all vertebrates) that regulate chromosomal replication at each cell division.
- Allogeneic
-
Inter-individual genetic variation at the MHC locus. In a partially matched transplant, for example, some MHC molecules are shared by the donor and recipient, but in addition the donor has some MHC molecules that the recipient does not.
- TH2 cells
-
(T helper 2 cells). A subset of CD4+ T cells that has an important role in humoral immunity and in allergic responses. TH2 cells express the transcription factors GATA3 and STAT6 and produce cytokines such as interleukin-4 (IL-4), IL-5, IL-9 and IL-13, which regulate IgE synthesis, eosinophil proliferation, mast cell proliferation and airway hyperresponsiveness, respectively. A TH2 cell pattern of cytokine expression is observed in allergic inflammation and in parasitic infections, conditions that are both associated with IgE production and eosinophilia.
- TH1 cells
-
(T helper 1 cells). A subset of CD4+ T cells that expresses the transcription factor T-bet and is associated with cell-mediated immunity. TH1 cells provide help for cytotoxic T cell responses by secreting high concentrations of interleukin-2, tumour necrosis factor and interferon-γ. They may also promote immunopathology in certain autoimmune diseases, such as multiple sclerosis and rheumatoid arthritis.
- TH17 cells
-
(T helper 17 cells). A subset of CD4+ T helper cells that produce interleukin-17 (IL-17) and that are thought to be important in antibacterial and antifungal immunity and may also have a role in autoimmune diseases. Their generation involves IL-23 and IL-21, as well as the transcription factors RORγt and STAT3.
Rights and permissions
About this article
Cite this article
Restifo, N., Dudley, M. & Rosenberg, S. Adoptive immunotherapy for cancer: harnessing the T cell response. Nat Rev Immunol 12, 269–281 (2012). https://doi.org/10.1038/nri3191
Published:
Issue Date:
DOI: https://doi.org/10.1038/nri3191
This article is cited by
-
An engineered influenza virus to deliver antigens for lung cancer vaccination
Nature Biotechnology (2024)
-
Effects of Chemotherapy on the Immune System: Implications for Cancer Treatment and Patient Outcomes
Naunyn-Schmiedeberg's Archives of Pharmacology (2024)
-
Newly developed 3D in vitro models to study tumor–immune interaction
Journal of Experimental & Clinical Cancer Research (2023)
-
Adoptive neoantigen-reactive T cell therapy: improvement strategies and current clinical researches
Biomarker Research (2023)
-
Reprogramming T cell differentiation and exhaustion in CAR-T cell therapy
Journal of Hematology & Oncology (2023)