Abstract
Objective:
Assess the effect of increasing pulse oximetry targets on incidence of pulmonary hypertension in very low birthweight premature infants.
Study Design:
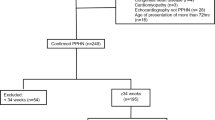
Retrospective cohort study comparing pulmonary hypertension incidence among three cohorts of premature infants exposed to varying oxygen saturation targets (Cohort 1: n=459, 1 May 2009 to 30 April 2011, 85–94%; Cohort 2: n=474, 1 May 2011 to 31 May 2013, 88–94%; Cohort 3: n=387, 1 June 2013 to 31 May 2015, 90–95%). Subjects had birth weight <1500 g and gestational age 23–32 weeks. Chi-square, Kruskall–Wallis and Anderson–Darling tests were used, as well as multivariable logistic regression.
Results:
Incidence of pulmonary hypertension declined with higher oxygen saturation targets (19.0% Cohort 1, 7.9% Cohort 2, 9.6% Cohort 3, P<0.001). Other parameters were largely not different between cohorts though rates of chorioamnionitis and prenatal steroids increased and oxygen use, inhaled nitric oxide use, necrotizing enterocolitis and patent ductus arteriosus ligation decreased over time.
Conclusion:
Higher oxygen saturation targets for very low-birthweight premature infants were associated with reduced rates of pulmonary hypertension in this retrospective cohort study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Khemani E, McElhinney DB, Rhein L, Andrade O, Lacro RV, Thomas KC et al. Pulmonary artery hypertension in formerly premature infants with bronchopulmonary dysplasia: clinical features and outcomes in the surfactant era. Pediatrics 2007; 120: 1260–1269.
Mirza H, Ziegler J, Ford S, Padbury J, Tucker R, Laptook A . Pulmonary hypertension in preterm infants: prevalence and association with bronchopulmonary dysplasia. J Pediatr 2014; 165: 909–914.
Bhat R, Salas A, Foster C, Carlo W, Ambalavanan N . Prospective analysis of pulmonary hypertension in extremely low birth weight infants. Pediatrics 2012; 129: e682–e689.
Slaughter JL, Pakrashi T, Jones DE, South AP, Shah TA . Echocardiographic detection of pulmonary hypertension in extremely low birthweight infants with bronchopulmonary dysplasia requiring prolonged positive pressure ventilation. J Perinatol 2011; 10: 635–640.
Berenz A, Vergales JE, Swanson JR, Sinkin RA . Evidence of early pulmonary hypertension is associated with increased mortality in very low birthweight infants. Am J Perinatol 2017; 34 (8): 801–807.
Martin RJ, Di Fiore JM, Walsh MC . Hypoxic episodes in bronchopulmonary dysplasia. Clin Perinatol 2015; 42: 825–838.
Mourani PM, Ivy DD, Gao D, Abman SH . Pulmonary vascular effects of inhaled nitric oxide and oxygen tension in bronchopulmonary dysplasia. Am J Respir Crit Care Med 2004; 170: 1006–1013.
Gitto E, Pellegrino S, Aversa S, Romeo C, Trimarchi G, Barberi I et al. Oxidative stress and persistent pulmonary hypertension of the newborn treated with inhaled nitric oxide and different oxygen concentrations. J Matern Fetal Neonatal Med 2012; 25: 1723–1726.
Lakshminrusimha S, Swartz DD, Gugino SF, Ma CX, Wynn KA, Ryan RM et al. Oxygen concentration and pulmonary hemodynamics in newborn lambs with pulmonary hypertension. Pediatr Res 2009; 66: 539–544.
Lakshminrusimha S, Russell JA, Steinhorn RH, Ryan RM, Gugino SF, Morin FC 3rd et al. Pulmonary arterial contractility in neonatal lambs increases with 100% oxygen resuscitation. Pediatr Res 2006; 59: 137–141.
Lakshminrusimha S, Russell JA, Steinhorn RH, Swartz DD, Ryan RM, Gugino SF et al. Pulmonary hemodynamics in neonatal lambs resuscitated with 21%, 50%, and 100% oxygen. Pediatr Res 2007; 62: 313–318.
Wedgwood S, Steinhorn RH . Role of reactive oxygen species in neonatal pulmonary vascular disease. Antioxid Redox Signal 2014; 21: 1926–1942.
Manja V, Saugstad OD, Lakshminrusimha S . Oxygen saturation targets in preterm infants and outcomes at 18–24 months: a systematic review. Pediatrics 2017; 139: e20161609.
Manja V, Lakshminrusimha S, Cook DJ . Oxygen saturation target range for extremely preterm infants: a systematic review and meta-analysis. JAMA Pediatr 2015; 169: 332–340.
Polin R, Bateman D . Oxygen-saturation targets in preterm infants. N Engl J Med 2013; 368: 22.
Cummings JJ, Polin RA, AAP Committee on Fetus and Newborn.. Oxygen targeting in extremely low birth weight infants. Pediatrics 2016; 138: e20161576.
Chow LC, Wright KW, Sola A, CSMC Oxygen Administration Study Group.. Can changes in clinical practice decrease the incidence of severe retinopathy of prematurity in very low birth weight infants? Pediatrics 2003; 111: 339–345.
Carlo W, Finer N, Walsh M, Rich W, Gantz M, Laptook A et alSUPPORT Study Group of the Eunice Kennedy Shriver NICHD Neonatal Research Network.. Target ranges of oxygen saturation in extremely preterm infants. N Engl J Med 2010; 363: 1959–1969.
Manley BJ, Kuschel CA, Elder JE, Doyle LW, Davis PG . Higher rates of retinopathy of prematurity after increasing oxygen saturation targets for very preterm infants: experience in a single center. J Pediatr 2016; 168: 242–244.
Schmidt B, Whyte RK, Shah PS, Abbasi S, Bairam A, Harrold J et alCanadian Oxygen Trial (COT) Group.. Effects of targeting higher or lower oxygen saturations in centers with more versus less separation between median saturations. J Pediatr 2016; 178: 288–291.
STOP-ROP Multicenter Study Group. Supplemental therapeutic oxygen for prethreshold retinopathy of prematurity (STOP-ROP), a randomized, controlled trial. I: primary outcomes. Pediatrics 2000; 105: 295–310.
Inomata K, Taniguchi S, Yonemoto H, Inoue T, Kawase A, Kondo Y . Lower early postnatal oxygen saturation target and risk of ductus arteriosus closure failure. Pediatr Int 2016; 58: 1153–1157.
Tarnow-Mordi W, Stenson B, Kirby A, Juszczak E, Donoghoe M, Deshpande S et alBOOST-II Australia and United Kingdom Collaborative Groups.. Outcomes of two trials of oxygen-saturation targets in preterm infants. N Engl J Med 2016; 374: 749–760.
Sylvester JT, Shimoda LA, Aaronson PI, Ward JP . Hypoxic pulmonary vasoconstriction. Physiol Rev 2012; 92: 367–520.
Dunham-Snary KJ, Wu D, Sykes EA, Thakrar A, Parlow LR, Mewburn JD et al. Hypoxic pulmonary vasoconstriction: from molecular mechanisms to medicine. Chest 2017; 151: 181–192.
Semenza GL . Oxygen sensing, hypoxia-inducible factors, and disease pathophysiology. Annu Rev Pathol 2014; 9: 47–71.
Kylhammar D, Rådegran G . The principal pathways involved in the in vivo modulation of hypoxic pulmonary vasoconstriction, pulmonary arterial remodeling and pulmonary hypertension. Acta Physiol 2017; 219: 728–756.
Olsen IE, Groveman MS, Lawson ML, Clark RH, Zemel BS . New intrauterine growth curves based on United States Data. Pediatrics 2010; 125: e214–e224.
Naguib M, Kanaan U, Simon D, Guglani L . Risk factors for development of pulmonary hypertension in infants with bronchopulmonary dysplasia:systematic review and meta-analysis. Paediatr Respir Rev 23: 27–32.
Rudolph AM The ductus arteriosus and persistent patency of the ductus arteriosus. Congenital Diseases of the Heart: Clinical-Physiological Considerations. Future Publishing Company, Inc.: New York, 2001, pp 155–196.
Acknowledgements
We appreciate and benefitted from the help and support of Dr Reese Clark, the research department at Mednax, and Courtney McCracken, PhD.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Dr Kanaan and Ms Huckaby receive research support but no personal remuneration from Eli Lilly and Company and from the Association for Pediatric Pulmonary Hypertension (a non-profit research organization supported by Actelion Pharmaceuticals, Ltd.). The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kanaan, U., Srivatsa, B., Huckaby, J. et al. Association of unit-wide oxygen saturation target on incidence of pulmonary hypertension in very low birthweight premature infants. J Perinatol 38, 148–153 (2018). https://doi.org/10.1038/jp.2017.166
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.166
This article is cited by
-
Oxygen desaturations in the early neonatal period predict development of bronchopulmonary dysplasia
Pediatric Research (2019)