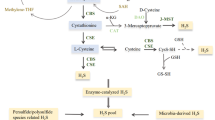
Abstract
We previously showed that H2 acts as a novel antioxidant to protect cells against oxidative stress. Subsequently, numerous studies have indicated the potential applications of H2 in therapeutic and preventive medicine. Moreover, H2 regulates various signal transduction pathways and the expression of many genes. However, the primary targets of H2 in the signal transduction pathways are unknown. Here, we attempted to determine how H2 regulates gene expression. In a pure chemical system, H2 gas (approximately 1%, v/v) suppressed the autoxidation of linoleic acid that proceeds by a free radical chain reaction and pure 1-palmitoyl-2-arachidonyl-sn-glycero-3-phosphocholine (PAPC), one of the major phospholipids, was autoxidized in the presence or absence of H2. H2 modified the chemical production of the autoxidized phospholipid species in the cell-free system. Exposure of cultured cells to the H2-dependently autoxidized phospholipid species reduced Ca2+ signal transduction and mediated the expression of various genes as revealed by comprehensive microarray analysis. In the cultured cells, H2 suppressed free radical chain reaction-dependent peroxidation and recovered the increased cellular Ca2+, resulting in the regulation of Ca2+-dependent gene expression. Thus, H2 might regulate gene expression via the Ca2+ signal transduction pathway by modifying the free radical-dependent generation of oxidized phospholipid mediators.
Similar content being viewed by others
Introduction
Molecular hydrogen (H2) was originally thought to behave as an inert gas in mammalian cells; however, our previous studies showed that this is not always the case1, demonstrating that H2 neutralizes the hydroxyl radical (·OH) and peroxynitrite (ONOO–) inside cells and acts as a novel antioxidant to protect the cells against oxidative stress1,2. Inhalation of 1%–4% (v/v) H2 gas is effective for the treatment of ischemia/reperfusion injuries1,3,4. Recently, inhalation of 1.3% H2 gas from a premixed gas was shown to protect neurons in a cardiac arrest model5. However, the mechanism of how such a low concentration of H2 exerts the positive effects is not known.
Numerous studies have strongly suggested that H2 has the potential for a variety of therapeutic and preventive applications6,7. In addition to extensive animal experiments, more than 10 clinical studies examining the efficacy of H2 have been reported6,7, including double-blinded clinical studies in patients with Parkinson’s disease and rheumatism8,9. Based on these studies, the field of hydrogen medicine is rapidly growing.
Subsequently, H2 was shown to exhibit multiple functions, including anti-inflammatory, anti-apoptotic, anti-allergic and antioxidant activities, as well as regulation of differentiation and energy metabolism6,7. To exert multiple functions in addition to anti-oxidative roles, H2 regulates various signal transduction pathways and the expression of many genes6,7. For examples, H2 protects neural cells and stimulates energy metabolism by stimulating the hormonal expression of ghrelin10 and fibroblast growth factor 21 (FGF21)11, respectively. In contrast, H2 relieves inflammation by decreasing pro-inflammatory cytokines12. However, it is difficult to explain the molecular mechanisms by which H2 exerts these functions by conventional concepts alone. To understand the molecular mechanisms by which H2 exerts these multiple functions, it is essential to identify the primary targets of H2 that modulate signal transduction and gene expression.
Therefore, in this study, we aimed to elucidate one of the molecular mechanisms by which H2 mediates signal transduction and gene expression. Our results suggested that low concentrations of H2 modulated Ca2+ signal transduction and regulated gene expression by modifying the production of oxidized phospholipid species.
Results
H2 accumulated in the lipid phases
To understand the difference between intracellular conditions and aqueous solutions, we focused on the lipid phases to determine the intracellular localization of H2 accumulation at room temperature. H2 incorporation was two- or three-fold higher in the liquid fatty acid phases than in the aqueous phase in the presence of both water and fatty acids and was retained longer in the fatty acid phases than in the aqueous phase in open vessels (Fig. 1a,b). In particular, H2 seemed to be retained significantly longer in the unsaturated fatty acid (linolenic acid) than in the saturated fatty acids (octanoic acid) (Fig. 1c), although this difference in retention time might be attributed to the difference in the number of carbons. Since unsaturated fatty acids are the primary targets for initiating a free radical chain reaction, we assumed that H2 could efficiently suppress this reaction in biomembranes, even at low concentrations.
Solubility of H2 in fatty acids in the presence of an aqueous solvent.
H2-saturated phosphate-buffered saline (PBS) was mixed with the same volume (75 mL) of saturated fatty acid (octanoic acid) (a) or unsaturated fatty acid (linolenic acid) (b) and maintained for 16 h in a closed aluminum bag as described in Methods. The same volume (3 mL) of each phase was transferred to each open tube (ϕ13 mm), followed by measurement of H2 at the indicated time (n = 4). The experiments were performed at 25 °C. ***P < 0.001 vs. PBS. (a,b) Significance was calculated using an unpaired two-tailed Student’s t-test. (c) Time courses of retention times of H2 in each phase in the open vessels. **P < 0.01, vs. octanoic acid (n = 4).
Autoxidation of unsaturated fatty acids was suppressed by low concentrations of H2 gas
Autoxidation of unsaturated fatty acids proceeds by a free radical chain reaction in air13. Thus, we measured autoxidation of a filmy di-unsaturated fatty acid (linoleic acid: R-CH = CH-CH2-CH = C-R’) at 37 °C for 20 h in the dark in the presence of various concentrations of H2 gas. A conjugated diene, which should be formed by autoxidation, was estimated by the absorption at 234 nm (Fig. 2a). The absorption at 234 nm was increased depending on the formation of the conjugated diene [R-CH = CH-CH = CH-CH(-OOH)-R’ or R-CH(-OOH)-CH = CH-CH = CH-R’] accompanied by peroxidation in a pure chemical system (H2, O2 and N2 were supplied from gas cylinders) (Fig. 2b). O2 was essential for autoxidation (Fig. 2c). As a result, even only approximately 1% H2 gas significantly suppressed autoxidation of linoleic acid at 37 °C, even in the absence of any catalysts in the dark in a pure chemical system (Fig. 2c).
Suppression of autoxidation of linoleic acid-film by H2 gas.
(a) Profile of ultraviolet absorption of 9-hydroxyoctadecadienoic acid; CH3(CH2)4-CH = CH-CH = CH-CH(-OH)-(CH2)7-COOH) (9-HODE) in cyclohexane, shown as a standard conjugated diene. (b) Linoleic acid-film was autoxidized at 37 °C for 20 h in a glass tube placed in a closed aluminum bag in the presence of various concentrations of H2 and O2 as described in Methods. Representative profiles of ultraviolet absorption of the cyclohexane solution of H2-dependent autoxidized linoleic acid are shown. (c) Linoleic acids autoxidized with various concentrations of H2 were evaluated by measuring absorption at 234 nm. *P = 0.034 (0.3% H2), #P = 0.069 (1% H2), **P < 0.01 (3% H2, 10% H2) and ***P < 0.001 (80% H2) vs. 0% H2 (n = 15).
Ca2+ signal transduction by H2-dependent chemical oxidation of phospholipids
Phospholipids are converted into oxidized mediators that modulate various signal transduction pathways by not only enzymatic reactions, but also by chemical oxidation14,15. Oxidized phospholipids, including 1-palmitoyl-2-(5-oxovaleroyl)-sn-glycero-3-phosphocholine (POVPC) and 1-palmitoyl-2-glutaroyl-sn-glycero-3-phosphocholine (PGPC), are present in oxidatively modified low-density lipoproteins (oxLDLs) and have been found in atherosclerotic lesions15. These compounds are important as inducers of different cellular responses, including inflammation, proliferation and cell death. Moreover, autoxidation of 1-palmitoyl-2-arachidonyl-sn-glycero-3-phosphocholine (PAPC) leads to the chemical production of various bioactive phospholipid species, such as POVPC, PGPC, 1-palmitoyl-2-(5-hydroxy-8-oxooct-6-enoyl)-sn-glycero-3-phosphocholine (HOOA-PC) and 5-hydroxy-8-oxo-6-octenedioic acid (HOdiA-PC)14,15.
We assumed that low concentrations of H2 would influence some chemical reactions leading to the production of putative oxidized lipid mediators for the modulation of signal transduction. Because PAPC is one of the major phospholipids in mammalian biomembranes, the role of H2 in the chemical production of oxidized phospholipid mediators was determined by conducting autoxidation of pure PAPC (resulting in OxPAPC) in the absence of any catalysts in the dark. The peroxidation of PAPC in air was confirmed by an increase in the signal for the fluorescent dye specific to lipid peroxides, Liperfluo (Fig. 3a). A previous study indicated that OxPAPC activates transcription factors involved in Ca2+ signaling16. Indeed, when THP-1 cells (a human monocytic cell line derived from a patient with acute monocytic leukemia) were exposed to OxPAPC, a transient increase in cellular Ca2+ was observed when a Ca2+-sensitive fluorescent dye, Fluo4-AM was used (Fig. 3b). This Ca2+ signaling depended on OxPAPC in an oxidation time-dependent manner (Fig. 3c).
PAPC autoxidized with H2 modulated Ca2+ signaling.
(a) Chemically pure PAPC was autoxidized in air with 100% humidity at 25 °C in a closed aluminum bag for the indicated periods and time-dependent production of peroxides in air from chemically pure PAPC was estimated using Liperfluo fluorescence, where wavelengths of excitation and emission were set at 488 and 535 nm, respectively, as described in Methods. (b) Representative responses in THP-1 by OxPAPC with the fluorescent Ca2+ indicator Fluo4-AM are shown as described in Methods. The arrow and arrowhead indicate the addition of OxPAPC and ATP, respectively. ATP (a ligand of the Ca2+ channel P2X7) was used as a positive control. (c) PAPC was autoxidized for the indicated periods at 25 °C and subjected to the Ca2+-signaling assay in THP-1 cells. The OxPAPC-induced Ca2+ response depended on autoxidizing period of OxPAPC. (d) PAPC was autoxidized in air for 3 days in the absence or presence of the indicated concentrations of H2 (H2OxPAPC) and the peroxide of OxPAPC or H2OxPAPC was estimated using Liperfluo as described in (a) (n = 3-6). *P = 0.044, **P < 0.01. (e) PAPC was autoxidized in air for 3 days with the indicated concentrations of H2 (H2OxPAPC) and then subjected to Ca2+ signaling assays as described in Methods (n = 6). *P = 0.021 (1.3%H2), *P = 0.022 (5% H2) and *P = 0.030 (80% H2) vs. no H2.
Next, the H2-dependent production of OxPAPC, which leads to the activation of Ca2+ signaling, was investigated by autoxidizing PAPC for 3 days at 25 °C in air at various concentrations of H2 (designated as H2OxPAPC and the notation of H2[x%]OxPAPC was used when autoxidized in the presence of x% H2). H2 suppressed the generation of total peroxides as revealed by Liperfluro fluorescence intensity (Fig. 3d). Ca2+ signaling was observed when PAPC was autoxidized with less than 0.3% H2, whereas more than 1.3% H2 significantly disrupted this signaling (Fig. 3e).
In order to investigate the molecule(s) influenced by H2, we analyzed H2OxPAPCs by using mass spectrometry on autoxidation day 3. In all, 209 bands were detected, with molecular masses ranging from 126.3754 to 991.6494 Da; this was consistent with the findings of a previous report15 (Supplementary Fig. 1). The differences in the production of H2OxPAPC and OxPAPC species were presented using a heat map (Supplementary Fig. 1i). The levels of many bands were increased or decreased with differences in concentrations of H2. For examples as the relatively increased species, the levels of the Ca2+ signaling inducers POVPC16, HOOA-PC, HOdiA-PC and hydroxyeicosatetraenoic acid-3-phosphocholine (HETE-PC)17 were slightly increased in response to H2 (Supplementary Fig. 1i).
Because the reduced form of POVPC was reported to function as an antagonist18, it is possible that increased levels of the reduced form(s) of some OxPAPC species, rather than the decreased levels of putative agonists (such as POVPC), might have disrupted Ca2+ signaling as a putative antagonist(s). Further studies are warranted to identify the H2-dependent bioactive mediator(s).
Comprehensive analysis of H2-dependent regulation of gene expression
Next, we investigated how H2OxPAPC influences gene expression. PAPC was autoxidized in the absence or presence of various concentrations of H2 for 3 days and then administered to cultured THP-1 cells. In a preliminary experiment, the change in the expression level of tumor necrosis factor (TNF)-α gene in response to OxPAPC from that to H2OxPAPC peaked at 4 h. Thus, by using microarray analysis, we comprehensively analyzed the change in gene expression in response to the H2-dependent mediators at 4 h in three samples under each condition. In all, 86 genes were selected according to the following criteria as described in the legend of Fig. 4a: a significant increase in OxPAPC (vs. PAPC) and a significant decrease in H2[1.3%]OxPAPC and H2[5%]OxPAPC (vs. OxPAPC) (Supplementary Table 1). The gene expression profile was presented in a heat map (Fig. 4a). The selected genes were validated by semi-quantitative real-time polymerase chain reaction (RT-PCR) and marginal changes in the expression levels of some genes were confirmed (Supplementary Fig. 2).
Changes in gene expression regulated by H2OxPAPC.
(a) Three samples of PAPC, OxPAPC and H2OxPAPC were exposed to THP-1 cells for 4 h and the gene expression was comprehensively analyzed using microarray. Eighty-six genes were selected according to the following criteria; genes up-regulated by OxPAPC (more than 2.5-fold, vs. PAPC) and those down-regulated by H2[1.3%]OxPAPC and H2[5%]OxPAPC (less than 0.75-fold and 0.5-fold, respectively, vs. OxPAPC) are shown in a heat map (red and green indicate the up-regulation vs. PAPC treatment and the down-regulation vs. OxPAPC treatment, respectively, as shown in the color gradient). Possible target genes of NFAT and CREB are marked with red on the right. Genes encoding factors involved in signal transduction and transcription are indicated by blue and black, respectively, on the right. The release of TNF-α (b) (from THP-1) and IL-8 (c) (from HAEC) was investigated using ELISA as described in Methods. (d, upper) Ratio of genes belonging to each category for a total of 7,142 genes identified by the KEGG database. (d, lower) Ratio of genes belonging to each category in the 86 selected genes listed in a. (e, upper) Ratio of genes belonging to each signaling pathway identified by the whole KEGG database. (c, lower) Ratio of genes belonging to each signaling pathway in the selected genes listed in (a). (f) The H2OxPAPC-dependent expression of genes transcribed by CREB and NFAT. Transcription factors are indicated in yellow.
In addition, the regulatory expression of TNF-α and IL-8 by H2OxPAPC was investigated using THP-1 and a different cell type (human aortic endothelial cells: HAEC), respectively (Fig. 4b,c).
According to the Kyoto Encyclopedia of Genes and Genomes (KEGG) Pathway Database (http://www.genome.jp/kegg/pathway.html), the functions of 7,143 genes were identified and classified (Fig. 4d, upper). We classified the 86 selected genes (Fig. 4e, lower). Of these 86 genes, 46.5% belonged to those involved in signaling pathways (Fig. 4d, upper), whereas 25.8% of the total number of 7,143 genes is involved in signaling pathways (Fig. 4d, lower). Genes encoding factors involved in signal transduction and transcription factors are indicated by blue and black, respectively, on the right in the heat map (Fig. 4a).
Among the genes involved in signaling pathways, the proportion of those belonging to Ca2+ signaling were lower in the selected genes than in those in the entire genome, indicating that H2 regulates fewer components of the Ca2+ signaling pathways (Fig. 4e, lower). This was consistent with the finding that H2OxPAPC decreased Ca2+ signaling. In contrast, the proportion of genes belonging to the mitogen-activate protein kinase (MAPK) signaling was higher (Fig. 4e, lower), indicating that H2 regulates more components of MAPK signal transduction pathways (Fig. 4e, lower).
The signal transduction pathways that were regulated by H2 are shown in Supplementary Table 1 according to the KEGG Pathway Database. These data suggested the possibility that low concentrations of H2 contribute to various signal transduction pathways via oxidized phospholipid species.
cAMP response element binding protein (CREB)-target genes were selected according to the CREB Target Gene Database (http://natural.salk.edu/CREB/) and nuclear factor of activated T cells (NFAT) target genes were selected by referring to Medline, as shown in Supplementary Table 1. The target genes of CREB and NFAT are marked by red on the right in the heat map panel as NFAT or CREB (Fig. 4a). A considerable number of the selected genes were targets of CREB or NFAT (Fig. 4 f). These data are consistent with the findings of previous studies showing the Ca2+-dependent regulation by these transcription factors: CREB is activated via phosphorylation by a calmodulin-dependent kinase (CaMK)19 in a Ca2+-dependent manner and NFAT is dephosphorylated by calcineurin (CN) in a Ca2+-dependent manner, translocates to the nucleus and then functions as a transcription factor with its partner proteins, e.g., activator protein 1 (AP-1), CREB, or nuclear factor-kappa B (NF-κB)20. Indeed, exposure of THP-1 to OxPAPC, but not to H2OxPAPC, stimulated the nuclear translocation of NFAT (Supplementary Fig. 3).
Thus, H2-dependent oxidized mediators or putative antagonists could be associated with transcriptional regulation via Ca2+ signaling.
Free radical inducers contributed to the NFAT pathway in cultured cells
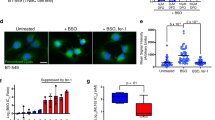
Autoxidation of unsaturated fatty acids, including PAPC, proceeds by a free radical chain reaction13, and·OH is the primary trigger for this reaction13,21,22. We previously showed that H2 reduces ·OH levels inside cultured cells by using the spin trapping method and a specific fluorescent indicator1. Thus, in this study, we investigated the effects of H2 on the lipid free radical chain reaction by using cultured cells. To initiate a free radical chain reaction inside the cells, we used 2,2′-azobis(2-methylpropionamidine)dihydrochloride (AAPH)23, which is not affected by H2 (Supplementary Fig. 4) and is suitable for the slow generation of free radicals by a spontaneous chemical reaction. The lipid free radical chain reaction results in the production of lipid peroxides (LPOs)21,24, which can be detected using the fluorescent dye Liperfluo25. Thus, we exposed cultured THP-1 cells to AAPH and estimated LPO production based on the Liperfluo signal. The Liperfluo signal significantly decreased in the presence of low levels of H2 gas (e.g., 1.3%; Fig. 5a,b). Thus, even at such low concentrations, H2 has the potential to reduce the generation of LPOs by suppressing the initiation and/or propagation of free radical chain reactions in cultured cells.
H2 suppressed free radical inducer-dependent fatty acid peroxidation and Ca2+ and NFAT signaling.
(a) THP-1 was exposed to a free radical inducer (10 mM AAPH) in the absence or presence of the indicated concentrations of H2 for 4.5 h. Representative flow cytometric profiles are shown to demonstrate lipid peroxides with Liperfluo signals. (b) The Liperfluo signals were quantified. *P = 0.015, ***P < 0.001 vs. 0% H2 (n = 6). (c) THP-1 cells were treated with 10 mM AAPH for 3 h in the presence of the indicated concentrations of H2. Intracellular Fluo-3 fluorescence intensity was observed using a laser scanning confocal microscope. Scale bar: 50 μm. (d) THP-1 cells were treated with 10 mM AAPH for the indicated periods in the absence of H2 and then time dependent increase in Ca2+-signal was monitored by intracellular Fluo-3 fluorescence intensity as described in (c). (e) Fluo3-positive cells were semi-quantified after the treatment with 10 mM AAPH for 3 h in the absence or presence of the indicated concentrations of H2. **P < 0.01 vs. no H2 (n = 3). (f) THP-1 was treated with 10 mM AAPH for 3 h in the presence of the indicated concentrations of H2. The translocation of NFAT into the nucleus was examined as described in Methods and shown by immunostaining in yellow. The nucleus was counter-stained with Hoechst 33342 as shown in blue. Scale bar: 50 μm. (g) The NFAT-expressing areas were semi-quantified and shown by the ratio of NFAT in the nucleus with that in cytosol. *P = 0.023 and **P < 0.01 vs. no H2 (n = 10). (h,i) The expressions of the NFAT-target genes (TNF-α, EGR1 and ATF3) (h) and non-NFAT target gens (NFKB2 and HMOX1) (i) were estimated using RT-PCR coupled with a TaqMan probe (the probes are listed in Supplementary Table 2). The names of the genes are described in Supplementary Table 1. *P = 0.015 (for ATF3) (+AAPH and +H2 vs. +AAPH and –H2). #P = 0.14 (for HMOX1) (+AAPH and –H2 vs. +AAPH and + H2) and **P < 0.01 (n = 3)
Next, we determined whether the responses induced by chemically produced H2OxPAPC (Figs 3 and 4) could simulate the effects induced by the free radicals in cultured cells. When THP-1 cells were exposed to AAPH, the cellular Ca2+ levels increased (Fig. 5c) in a time-dependent manner (Fig. 5d), as shown by the analysis of Fluo-3 and the Ca2+ signaling was suppressed by H2 (Fig. 5c,e). NFAT was also activated, as shown by the translocation of NFAT into the nucleus (Fig. 5f,g) and the nuclear translocation of NFAT were recovered by H2 (Fig. 5f,g). Moreover, the free radical inducer stimulated the expression of some target genes of NFAT, including TNF-α, early growth response protein 1 (EGR1) and activating transcription factor 3 (ATF3), which have been shown in Supplementary Table 1 and H2 decreased their expressions (Fig. 5h), suggesting that H2 regulates these genes via the NFAT pathway.
In contrast, AAPH-mediated activation of CREB was not observed (Supplementary Fig. 5) in this cultured cell line, regardless of the stimulation of cellular Ca2+. In particular, the expression of the CREB-target gene NFKB2 (NF-κB, subunit 2 gene) was not affected by AAPH (Fig. 5i) and the expression of HMOX1 (Heme Oxygenase 1 gene), a nuclear factor-E2-related factor 2 (Nrf2)-target, was slightly but not significantly increased by H2 (Fig. 5i). This result was consistent with those of a previous study26. Thus, the NFAT pathway could mainly contribute to the H2-dependent transcriptional response induced by free radicals at least in THP-1 cells.
Taken together, these cellular responses, at least partly, are in agreement with those obtained using the in vitro H2-dependent products of OxPAPC species (Figs 3, 4). Therefore, we proposed a model in which H2 is linked to the modulation of Ca2+ signal transduction and the NFAT pathway via oxidized phospholipid species, as illustrated in Fig. 6.
A model of the proposed pathway.
When free radical chain oxidation generates oxidized phospholipid mediators, Ca2+ signaling is induced, followed by the activation of calcineurin and subsequent induction of the NFAT pathway. On the other hand, H2 modifies the production of oxidized phospholipids by modulating free radical chain reactions. The putative oxidized phospholipids appear to function as antagonists and lead to a decline in Ca2+ signaling.
Discussion
While the biological effects of H2 have been evaluated in more than 300 animal studies and 10 clinical analyses in humans6,7, the molecular mechanisms by which H2 at low concentrations exerts its multiple effects on signal transduction remained unknown. Therefore, in this study, we aimed to examine how H2 regulates signal transduction pathways that mediate gene expression. Our results suggested that low concentrations of H2 modulated Ca2+ signal transduction and regulated gene expression by modifying the production of oxidized phospholipid species. Hence, these data provide important insights into one of the molecular mechanisms by which H2 mediates gene expression.
H2 can be ingested via several methods. Drinking of H2-infused water (H2-water) has been shown to be efficacious in the treatment of various diseases in animal models and humans6,7; however, H2 can be infused up to only 0.8 mM under atmospheric pressure and drinking saturated H2-water provides a blood concentration up to only ~10 μM, with a short dwelling time in the body11,27. Moreover, inhaling 1%–4% (v/v) H2 gas was shown to be effective, reaching concentrations of 8–32 μM H2 in the blood1,4,5. However, initiation of cellular signals by these low concentrations of H2 may be difficult to be explained because H2 should be too inert to react with most molecules. To activate H2 for reaction with the other molecules, a sufficient level of a putative catalyst must be present; however, it is unlikely that such a putative catalyst would be abundant inside cells. Moreover, H2 is very small and is unlikely to bind to a putative H2-binding receptor because its intra-molecular fluctuation would be expected to lead to instability in terms of thermodynamics, as previously discussed28. Thus, it was unknown how low concentrations of H2 regulate signal transduction and gene expression.
Since increased oxidative stress involving ·OH triggers free radical chain reactions, we assumed that the chemically produced mediators derived from phospholipids could contribute to various pathogenic conditions. In the present study, we verified that a small amount of H2 (as low as 1.3%) affected free radical-dependent lipid peroxidation, from which oxidized lipid mediators should be derived22.
Generally, H2 hydrogenates unsaturated fatty acids at higher temperatures with a palladium catalyst. To the best of our knowledge, no studies have examined autoxidation-dependent hydrogenation at approximately 1% (v/v) H2 gas at 37 °C without any catalysts. Although H2 was thought to be inert in the absence of a catalyst at body temperature, we demonstrated that approximately 1% (v/v) H2 suppressed autoxidation of an unsaturated fatty acid in a chemically pure system in this study; thus, our data provided insights into the biological activities of H2.
There are two possibilities: the effects of oxidized phospholipid species on Ca2+ signaling may be explain by decreased levels of a putative agonist that induces Ca2+ signaling or by increased levels of a putative antagonist that disturbs Ca2+ signaling. Although we could not identify these species in this study, it is likely that H2 modified the production of reduced forms of oxidized phospholipid species during free radical chain reactions by the following previous findings: POVPC is a bioactive phospholipid-mediator that is produced by chemical oxidation of PAPC and the reduced form of POPVC has been shown to function as an antagonist for signal transduction18. Thus, it is possible that during a lipid free radical chain reaction, H2 contributes to the generation of a reduced form(s) that function(s) as an antagonist(s). Therefore, we proposed a hypothetic model in which H2 is linked to the modulation of Ca2+ signal transduction and the NFAT pathway via oxidized phospholipid species as illustrated in Fig. 6.
Previous studies have shown that 1%–4% was efficacious in inhaling H2 gas in various animal experiments1,3,4,29,30,31. Since a mixed gas containing 1.3% H2, 30% O2 and 68.7% N2 is available, the effects of around 1.3% needed to be investigated in further studies, including clinical ones5. The effective concentrations of H2 gas were approximately consistent throughout this study (Figs 2, 3, 4, 5).
No receptors involved in Ca2+ signaling were identified in the present study; however, a previous study showed that some chemically oxidized phospholipid mediators, such as 9-HODE and 11-HETE, could bind a G-protein coupled receptor (G2A) to induce Ca2+ signaling17. Thus, putative oxidized phospholipid mediators or antagonists might bind to G-protein coupled receptors to modulate signal transduction.
In addition to the anti-oxidative roles of H2, it has shown to function as an immunosuppressant in allograft transplantation32. This immunosuppressant effect can be explained by the suppression of NFAT activation because an immunosuppressant such as CsA and tacrolimus (FK506) acts through the inactivation of calcineurin. Since pro-inflammatory cytokines are regulated by NFAT-dependent mechanisms20, the anti-inflammatory effects by H2 can be explained by the suppression of NFAT. Additionally, the anti-allergic effects of H2 can be explained by the decrease in Ca2+/NFAT signaling33.
A considerable number of the multiple functions of H2, as shown by previous studies, might be explained by the link between H2 and NFAT because of the numerous multiple functions of NFAT20,34. For example, decreased expression of inducible nitric oxide synthase (iNOS) by H235 can be explained by the inactivation of NFAT36. The suppression of osteoclast differentiation37 and improvement of hypertension38,39 by H2 could involve the NFAT pathway40,41. Moreover, the decreased expression of gene products through an NFAT-dependent pathway might be involved in α-synuclein-induced degeneration of midbrain dopaminergic neurons in Parkinson’s disease42. This NFAT-dependent pathway might explain the beneficial effects of H2 in these patients8. Further studies are needed to elucidate the mechanisms by which H2 exerts multiple functions in terms of the involvement of the NFAT pathway.
In summary, in this study, we investigated the link among H2, oxidized phospholipids and Ca2+ signaling. Further studies are warranted to identify the H2-dependent bioactive mediator(s). Our data provided important insights into one of the mechanisms by which H2 regulates signal transduction and gene expression; however, H2 might contribute to other types of signaling pathways as well because H2 regulates many genes belonging to various signaling pathways. A more detailed understanding of the molecular mechanisms of H2-dependent signal transduction and gene expression is expected to facilitate the application of H2 in a wide range of medical applications.
Methods
Measurement of H2
Gases containing H2 were prepared by mixing H2, O2, N2 and CO2 at various concentrations from each gas cylinder equipped with a flow meter. The H2 concentration in the mixed gas or air was tested in each experiment by using gas chromatography (Breath Gas Analyzer, Model TGA2000; TERAMECS Co. Ltd., Kyoto, Japan) as described previously1. For the measurement of H2 in the solvent, H2 was transferred to the air phase in a closed aluminum bag and the concentration of H2 measured by using gas chromatography as described previously1. The aluminum used in the bag was covered with a plastic film to avoid any influence of aluminum.
Autoxidation of linoleic acid-film
Linoleic acid and (±)9-HODE were purchased from Nacalai Tesque (Kyoto, Japan) and CAY (MI, USA), respectively. Linoleic acid was dissolved in cyclohexane to 16 mM and 2 μL was dispensed into each glass tube (ϕ10 × 50 mm) that had been filled with argon gas; it was allowed to dry up to form a linoleic acid-film at the bottom of a glass tube. The glass tubes were placed into a closed aluminum bag and the gas in the bag was completely replaced with the indicated mixed gas, where pure H2, O2 and N2 were obtained from separate cylinders. The bag was incubated at 37 °C for 20 h for the autoxidation and 0.2 mL cyclohexane was immediately added to the glass tube to obtain 0.16 mM peroxidized linoleic acid. The concentration of conjugated diene was estimated by measuring the absorption at 234 nm while scanning from 200 to 300 nm.
Autoxidation of pure PAPC in air in the absence or presence of H2
Chemically synthesized pure PAPC was purchased from Avanti Polar Lipids (Alabaster, AL, USA). PAPC was autoxidized in air as described previously43. Briefly, 0.5 mg of PAPC in 50 μL of chloroform was transferred to a ϕ10 × 50 mm glass tube and dried up under a gentle stream of nitrogen. The lipid residue was allowed to autoxidize in air with 100% humidity at 25 °C in the presence or absence of the indicated concentrations of H2 gas in a closed aluminum bag for the indicated periods and then suspended in PBS at a concentration of 0.5 mg/mL.
Estimation of OxPAPC with Liperfluo
OxPAPC was assayed in ethanol with Liperfluo as described previously25. Five min after adding OxPAPC to 1 μM Liperfluo at room temperature, the fluorescence was measured using a fluorescence spectrophotometer (RF-5300PC; Shimadzu Corporation, Kyoto, Japan), where wavelengths of excitation and emission were set at 488 and 535 nm, respectively.
Measurement of Ca2+ signaling
Intracellular Ca2+ in THP-1 cells treated with OxPAPC was measured using a Calcium Kit-Fluo 4 (CS22; Dojindo, Kumamoto, Japan) according to the manufacturer’s protocol. Briefly, THP-1 cells were washed with PBS and incubated with 4.5 μM Fluo 4-AM in recording medium (20 mM HEPES, 115 mM NaCl, 5.4 mM KCl, 0.8 mM MgCl2, 1.8 mM CaCl2, 13.8 mM glucose) containing 0.064% pluronic F-127 and 1.25 mM probenecid for 30 min at 37 °C. The cells were washed with PBS and resuspended in recording medium containing 1.25 mM probenecid. The cells were seeded on 35-mm glass-bottomed dishes and then stimulated with 100 μg/mL OxPAPC or H2OxPAPC, followed by 25 μM ATP. The changes in Fluo 4-AM fluorescence were monitored using a laser scanning confocal microscope (FV1200; Olympus Corporation, Tokyo, Japan). The strength of each fluorescent signal in 400 cells was examined and judged as positive if there was greater than 30% of the ATP signal.
Intracellular Ca2+ of THP-1 cells treated with the free radical inducer AAPH23 was measured by Fluo-3 (F-23915; Molecular Probes, Eugene, OR, USA). Briefly, THP-1 cells were pre-incubated with 2 μM Fluo 3-AM in HBSS containing 0.02% pluronic F-127 for 30 min at 37 °C, resuspended in RPMI1640 (with 10% FBS) containing 2.5 mM probenecid, seeded in 24-well plates and then treated with AAPH in the presence or absence of H2. Changes in Fluo-3 fluorescence signals were observed using a laser scanning confocal microscope (FV1200; Olympus).
Mass spectrometric analysis and presentation of data using heat maps
OxPAPC (dissolved in chloroform at 2.5 mg/mL) was analyzed using by electrospray ionization-mass spectrometry (ESI-MS) by using an LTQ ORBITRAP XL mass spectrometer (Thermo Fisher Scientific, San Jose, CA, USA) equipped with a nitrogen sheath gas flow rate of 40 AU at 300 °C. The sample was directly infused. The scanning range was from m/z 250 to 1000 in the positive ion detection mode. The ion spray voltage was set to 4 kV. OxPAPC species were identified according to their m/z values and confirmed using mass spectrometric analysis as described previously14,44,45.
Two independent experiments were performed. The average of the data was used for construction of a heat map and displayed in mass spectrometric profiles. In the heat map, bands were arranged according to molecular mass from small to large and the strength of each band obtained from H2OxPAPC was compared with those by OxPAPC. Red and green bands represented increased and decreased levels as compared with those of OxPAPC, respectively. The mass spectrometric display indicates the average band from two experiments. Only when bands were detected by all of 10 experiments (two experiments at 0%, 0.2%, 0.3%, 1.3% and 5% of H2), they were adopted.
Comprehensive analysis of gene expression
THP-1 cells were exposed for 4 h to PAPC or OxPAPC, H2[1.3%]OxPAPC and H2[5%]OxPAPC that had been autoxidized for 3 days with 0%, 1.3%, or 5% H2, respectively. Total RNA was extracted using an RNeasy Mini Kit according to the manufacturer’s protocol (Qiagen, Valencia, CA, USA) and labeled using a Low-Input QuickAmp Labeling Kit, One-Color (Agilent Technologies, Santa Clara, CA, USA). Gene expression analysis was performed on samples from three independent experiments using a microarray (SurePrint G3 Human GE 8 × 60 K v2 Microarray; Agilent Technologies). The raw microarray data were deposited in the Gene Expression Omnibus (GEO; accession number, GSE62434; http://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE62434). CREB target genes were selected according to the CREB Target Gene Database (http://natural.salk.edu/CREB/), while NFAT target genes were selected by reference to Medline, as listed in Supplementary Table 1. Signal transduction pathways associated with each gene were identified according to the KEGG Pathway Database (http://www.genome.jp/kegg/pathway.html).
Quantitative real-time PCR
To quantify mRNA levels, quantitative real-time PCR was carried out using TaqMan Probe and Premix Ex Taq (Probe qPCR; TaKaRa Bio Inc., Shiga, Japan) in a TaKaRa PCR Thermal Cycler Dice TP960 (TaKaRa Bio) according to the manufacturer’s protocols. To normalize mRNA expression levels, glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was used as an endogenous internal control. Primers and probes used for RT-PCR are described in Table 2.
ELISA (Enzyme-linked immuno-sorbent assay) HAEC and THP-1 cells were treated with PAPC, OxPAPC or H2OxPAPC for 22 h. The IL-8 (HAEC) and TNF-α (THP-1) contents in the culture media were determined using Human CXCL8/IL-8 Quantikine ELISA Kit (R&D Systems, Minneapolis, MN, USA) and Human TNF-α Quantikine ELISA Kit (R&D Systems, Minneapolis, MN, USA), respectively, according to the manufacturer’s protocol.
Detection of lipid peroxidation in cultured cells
THP-1 cells (1 × 105 cells/mL) were stained with 5 μM Liperfluo25 for 30 min and then treated with 10 mM of AAPH23 for 4.5 h in the absence or presence of the indicated concentrations of H2 gas in a closed vessel. The cells were analyzed using a Cell Lab Quanta flow cytometer (Beckman Coulter, Miami, FL, USA).
Detection of the translocation of NFAT into the nucleus by immunofluorescence
THP-1 cells (1 × 105 cells/mL) were treated with OxPAPC (0.1 mg/mL), or H2[2.5%]OxPAPC (0.1 mg/mL) for 1.5 h, which were used for the Ca2+ signaling assay and then the translocation of NFAT was determined using immunofluorescence as follows. The cells were fixed for 20 min with 10% neutral buffered formalin (3.8% formaldehyde) and then permeabilized with 0.2% Triton X-100 in Tris-buffered saline (TBS-T) for 10 min. After the cells were washed and blocked with 5% nonfat milk in TBS-T, they were incubated with anti-NFAT1 antibodies (1:100 dilution; 25A10.D6.D2; Abcam, Cambridge, MA, USA) overnight at 4 °C, followed by incubation with Alexa Fluor 488-conjugated anti-mouse antibodies (1:400 dilution; A-11029; Life Technologies, Carlsbad, CA, USA) for 1 h at 25 °C. The cells were counterstained with Hoechst 33342. Immunofluorescence was observed using a laser scanning confocal microscope (FV1200; Olympus).
THP-1 cells (1 × 105 cells/mL) were treated with 10 mM AAPH for 3 h in the absence or presence of indicated concentrations of H2 and the NFAT translocation was investigated using immunofluorescence as described above.
Cell culture
THP-1 cells (ATCC) were cultured in RPMI1640 containing 10% FBS. Human aortic endothelial cells (HAEC) were obtained from Lonza and maintained in endothelial cell growth medium [EBM medium + growth supplements+FCS (Lonza)]. Cells were cultured at 37 °C in a 5% CO2 humidified atmosphere and were used for experiments from passage 4 to 8.
Statistical analysis
Statistical differences between groups were assessed by one-way analysis of variance (ANOVA) with Tukey-Kramer post hoc analysis unless otherwise mentioned. Statistical analyses were performed with IBM SPSS21 software. Results were considered significant at P < 0.05. When 0.01 < P < 0.05, the actual P values were noted. Data are presented as means ± standard deviations.
Additional Information
How to cite this article: Iuchi, K. et al. Molecular hydrogen regulates gene expression by modifying the free radical chain reaction-dependent generation of oxidized phospholipid mediators. Sci. Rep. 6, 18971; doi: 10.1038/srep18971 (2016).
References
Ohsawa, I. et al. Hydrogen acts as a therapeutic antioxidant by selectively reducing cytotoxic oxygen radicals. Nat. Med. 13, 688–694 (2007).
Hanaoka, T., Kamimura, N., Yokota, T., Takai, S. & Ohta, S. Molecular hydrogen protects chondrocytes from oxidative stress and indirectly alters gene expressions through reducing peroxynitrite derived from nitric oxide. Med. Gas Res. 1, 18 (2011).
Fukuda, K. et al. Inhalation of hydrogen gas suppresses hepatic injury caused by ischemia/reperfusion through reducing oxidative stress. Biochem. Biophys. Res. Commun. 361, 670–674 (2007).
Hayashida, K. et al. Inhalation of hydrogen gas reduces infarct size in the rat model of myocardial ischemia-reperfusion injury. Biochem. Biophys. Res. Commun. 373, 30–35 (2008).
Hayashida, K. et al. Hydrogen Inhalation During Normoxic Resuscitation Improves Neurological Outcome in a Rat Model of Cardiac Arrest, Independent of Targeted Temperature Management. Circulation. 130, 2173–2180 (2014).
Ohta, S. Recent progress toward hydrogen medicine: potential of molecular hydrogen for preventive and therapeutic applications. Curr. Pharm. Des. 17, 2241–2252 (2011).
Ohta, S. Molecular hydrogen as a preventive and therapeutic medical gas: initiation, development and potential of hydrogen medicine. Pharmacol. Ther. 144, 1–11 (2014).
Yoritaka, A. et al. Pilot study of H(2) therapy in Parkinson’s disease: a randomized double-blind placebo-controlled trial. Mov. Disord. 28, 836–839 (2013).
Ishibashi, T. et al. Therapeutic efficacy of infused molecular hydrogen in saline on rheumatoid arthritis: a randomized, double-blind, placebo-controlled pilot study. Int. Immunopharmacol. 21, 468–473 (2014).
Matsumoto, A. et al. Oral ‘hydrogen water’ induces neuroprotective ghrelin secretion in mice. Sci. Rep. 3, 3273 (2013).
Kamimura, N., Nishimaki, K., Ohsawa, I. & Ohta, S. Molecular hydrogen improves obesity and diabetes by inducing hepatic FGF21 and stimulating energy metabolism in db/db mice. Obesity 19, 1396–1403 (2011).
Ishibashi, T. Molecular hydrogen: new antioxidant and anti-inflammatory therapy for rheumatoid arthritis and related diseases. Curr. Pharm. Des. 19, 6375–6381 (2013).
Porter, N. A., Caldwell, S. E. & Mills, K. A. Mechanisms of free radical oxidation of unsaturated lipids. Lipids 30, 277–290 (1995).
Subbanagounder, G. et al. Hydroxy alkenal phospholipids regulate inflammatory functions of endothelial cells. Vascul. Pharmacol. 38, 201–209 (2002).
Bochkov, V. N. et al. Generation and biological activities of oxidized phospholipids. Antioxid. Redox Signal. 12, 1009–1059 (2010).
Bochkov, V. N. et al. Oxidized phospholipids stimulate tissue factor expression in human endothelial cells via activation of ERK/EGR-1 and Ca(++)/NFAT. Blood 99, 199–206 (2002).
Obinata, H., Hattori, T., Nakane, S., Tatei, K. & Izumi, T. Identification of 9-hydroxyoctadecadienoic acid and other oxidized free fatty acids as ligands of the G protein-coupled receptor G2A. J. Biol. Chem. 280, 40676–40683 (2005).
Subbanagounder, G. et al. Determinants of bioactivity of oxidized phospholipids. Specific oxidized fatty acyl groups at the sn-2 position. Arterioscler. Thromb. Vasc. Biol. 20, 2248–2254 (2000).
Bading, H. Nuclear calcium signalling in the regulation of brain function. Nat. Rev. Neurosci. 14, 593–608 (2013).
Hogan, P. G., Chen, L., Nardone, J. & Rao, A. Transcriptional regulation by calcium, calcineurin and NFAT. Genes Dev. 17, 2205–2232 (2003).
Niki, E. Biomarkers of lipid peroxidation in clinical material. Biochim. Biophys. Acta 1840, 809–817 (2014).
Reis, A. & Spickett, C. M. Chemistry of phospholipid oxidation. Biochim. Biophys. Acta 1818, 2374–2387 (2012).
Werber, J., Wang, Y. J., Milligan, M., Li, X. & Ji, J. A. Analysis of 2,2′-azobis (2-amidinopropane) dihydrochloride degradation and hydrolysis in aqueous solutions. J. Pharm. Sci. 100, 3307–3315 (2011).
Fruhwirth, G. O., Loidl, A. & Hermetter, A. Oxidized phospholipids: from molecular properties to disease. Biochim. Biophys. Acta 1772, 718–736 (2007).
Yamanaka, K. et al. A novel fluorescent probe with high sensitivity and selective detection of lipid hydroperoxides in cells. RSC Advances 2, 7894 (2012).
Kawamura, T. et al. Hydrogen gas reduces hyperoxic lung injury via the Nrf2 pathway in vivo. Am. J. Physiol. Lung Cell. Mol. Physiol. 304, L646–656 (2013).
Nagata, K., Nakashima-Kamimura, N., Mikami, T., Ohsawa, I. & Ohta, S. Consumption of molecular hydrogen prevents the stress-induced impairments in hippocampus-dependent learning tasks during chronic physical restraint in mice. Neuropsychopharmacology: official publication of the American College of Neuropsychopharmacology 34, 501–508 (2009).
Ohta, S. Molecular hydrogen as a novel antioxidant: overview of the advantages of hydrogen for medical applications. Methods Enzymol. 555, 289–317 (2015).
Xie, K. et al. Hydrogen gas improves survival rate and organ damage in zymosan-induced generalized inflammation model. Shock 34, 495–501 (2010).
Buchholz, B. M. et al. Hydrogen inhalation ameliorates oxidative stress in transplantation induced intestinal graft injury. Am. J. Transplant. 8, 2015–2024 (2008).
Hayashida, K. et al. H(2) gas improves functional outcome after cardiac arrest to an extent comparable to therapeutic hypothermia in a rat model. J. Am. Heart Assoc. 1, e003459 (2012).
Cardinal, J. S. et al. Oral hydrogen water prevents chronic allograft nephropathy in rats. Kidney Int. 77, 101–109 (2010).
Motojima, H., Villareal, M. O., Iijima, R., Han, J. & Isoda, H. Acteoside inhibits type Iota allergy through the down-regulation of Ca/NFAT and JNK MAPK signaling pathways in basophilic cells. J. Nat. Med. 67, 790–798 (2013).
Musson, R. E., Cobbaert, C. M. & Smit, N. P. Molecular diagnostics of calcineurin-related pathologies. Clin. Chem. 58, 511–522 (2012).
Itoh, T. et al. Molecular hydrogen inhibits lipopolysaccharide/interferon gamma-induced nitric oxide production through modulation of signal transduction in macrophages. Biochem. Biophys. Res. Commun. 411, 143–149 (2011).
Obasanjo-Blackshire, K. et al. Calcineurin regulates NFAT-dependent iNOS expression and protection of cardiomyocytes: co-operation with Src tyrosine kinase. Cardiovasc. Res. 71, 672–683 (2006).
Li, D. Z., Zhang, Q. X., Dong, X. X., Li, H. D. & Ma, X. Treatment with hydrogen molecules prevents RANKL-induced osteoclast differentiation associated with inhibition of ROS formation and inactivation of MAPK, AKT and NF-kappa B pathways in murine RAW264.7 cells. J. Bone Miner. Metab. 32, 494–504 (2014).
He, B. et al. Protection of oral hydrogen water as an antioxidant on pulmonary hypertension. Mol. Biol. Rep. 40, 5513–5521 (2013).
Kishimoto, Y. et al. Hydrogen ameliorates pulmonary hypertension in rats by anti-inflammatory and antioxidant effects. J Thorac Cardiovasc Surg 150, 645–654 (2015).
Negishi-Koga, T. & Takayanagi, H. Ca2+-NFATc1 signaling is an essential axis of osteoclast differentiation. Immunol. Rev. 231, 241–256 (2009).
Ramiro-Diaz, J. M. et al. NFAT is required for spontaneous pulmonary hypertension in superoxide dismutase 1 knockout mice. Am. J. Physio.l Lung Cell. Mol. Physiol. 304, L613–625 (2013).
Luo, J. et al. A calcineurin- and NFAT-dependent pathway is involved in alpha-synuclein-induced degeneration of midbrain dopaminergic neurons. Hum. Mol. Genet. 23, 6567–6574 (2014).
Watson, A. D. et al. Structural identification by mass spectrometry of oxidized phospholipids in minimally oxidized low density lipoprotein that induce monocyte/endothelial interactions and evidence for their presence in vivo. J. Biol. Chem. 272, 13597–13607 (1997).
Spickett, C. M., Reis, A. & Pitt, A. R. Identification of oxidized phospholipids by electrospray ionization mass spectrometry and LC-MS using a QQLIT instrument. Free Radic. Biol. Med. 51, 2133–2149 (2011).
O’Donnell, V. B. Mass spectrometry analysis of oxidized phosphatidylcholine and phosphatidylethanolamine. Biochim. Biophys. Acta 1811, 818–826 (2011).
Acknowledgements
We thank Ms. Mayumi Takeda and Ms. Suga Kato for technical assistance and secretarial work, respectively. Financial support for this study was provided by Grants-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (23300257, 24651055 and 26282198 to S.O.; 23500971 and 26350129 to N.K.; and 25350907 to K.N.).
Author information
Authors and Affiliations
Contributions
S.O. conceived of and directed the project, analyzed data and wrote the manuscript. N.K. planned each experiment. K.I., A.I., N.K., K.N., T.Y. and H.I. performed experiments on cell culture (by K.I.), Ca2+ signaling (by A.I.), gene expression (by N.K.) and chemical reactions (by K.N.), supported by H.I. and T.Y.
Ethics declarations
Competing interests
S.O. holds the right of a patent regarding a medical use of hydrogen gas.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Iuchi, K., Imoto, A., Kamimura, N. et al. Molecular hydrogen regulates gene expression by modifying the free radical chain reaction-dependent generation of oxidized phospholipid mediators. Sci Rep 6, 18971 (2016). https://doi.org/10.1038/srep18971
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep18971
This article is cited by
-
Changes in the negative logarithm of end-tidal hydrogen partial pressure indicate the variation of electrode potential in healthy Japanese subjects
Scientific Reports (2023)
-
Hydrogen-Rich Water Alleviates the Nickel-Induced Toxic Responses (Inflammatory Responses, Oxidative Stress, DNA Damage) and Ameliorates Cocoon Production in Earthworm
Biological Trace Element Research (2022)
-
Delineation of Neuroprotective Effects and Possible Benefits of AntioxidantsTherapy for the Treatment of Alzheimer’s Diseases by Targeting Mitochondrial-Derived Reactive Oxygen Species: Bench to Bedside
Molecular Neurobiology (2022)
-
Hydrogen and therapeutic gases for neonatal hypoxic–ischemic encephalopathy: potential neuroprotective adjuncts in translational research
Pediatric Research (2021)
-
Randomized, crossover clinical efficacy trial in humans and mice on tear secretion promotion and lacrimal gland protection by molecular hydrogen
Scientific Reports (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.