Abstract
The management of inflammatory bowel diseases has been widely investigated, especially ulcerative colitis. Thus, studies with the application of new probiotic products are needed in the prevention/treatment of these clinical conditions. The objective of this work was to evaluate the effects of probiotic orange juice containing Pediococcus acidilactici CE51 in a murine model of colitis. 45 male Swiss lineage mice were used, divided into five groups (n = 9): control, colitis, colitis + probiotic (probiotic orange juice containing CE51), colitis + placebo (orange juice) and colitis + sulfasalazine (10 mg/kg/Weight). The induction of colitis was performed with dextran sodium sulfate (3%). The treatment time was 5 and 15 days after induction. Histopathological analysis, serum measurements of TNF-α and C-reactive protein and metagenomic analysis of feces were performed after euthanasia. Probiotic treatment reduced inflammation in the small intestine, large intestine and spleen. The probiotic did not alter the serum dosages of TNF-α and C-reactive protein. Their use maintained the quantitative ratio of the phylum Firmicutes/Bacteroidetes and increased Lactobacillus helveticus with 15 days of treatment (p < 0.05). The probiotic orange juice containing P. acidilactici CE51 positively modulated the gut microbiota composition and attenuated the inflammation induced in colitis.
Similar content being viewed by others
Introduction
Inflammatory bowel diseases (IBD) are described as chronic conditions, marked by recurrent episodes of gastrointestinal tract inflammation, which can be included ulcerative colitis (UC) that takes an incidence rates that vary 2.2 to 19.2 per 100,000 inhabitants in the world1,2.
Ulcerative colitis, ulcerous colitis or ulcerative rectum colitis, is an inflammation limited to the mucosa, located most often from the rectum to the proximal colon. The main cause of ulcerative colitis is believed to be continuous inflammation in the mucosa, which is associated with significant nutritional disorders, leading to ulcerations and bleeding1,3. The current treatment of UC is mainly based on the use of anti-inflammatory drugs, immunomodulators, nutritional supplements and surgery4.
Sulfasalazine is the widely used drug for remission of ulcerative colitis. This medicine is composed by the combination of 5-aminosalicylic acid (5-ASA) with the sulphapyridine molecule, which transports the active ingredient to the colon and, in it, exerts anti-inflammatory action. In addition to, the sulphapyridine has also antibacterial action. It is possible that sulfasalazine attenuates ulcerative colitis inflammation by eliminating free radicals, and thus inhibiting the production of prostaglandins and leukotrienes and / or reducing neutrophil chemotaxis and superoxide production5.
Ulcerative colitis is also associated with a decrease in Lactobacillus spp. and Bifidobacterium spp., which suggests the need for research to assess the use of functional food substances that contains biologically active substances with clinical health benefits6,7.
Among the functional foods, there are probiotics, used mainly in dairy products, which may be associated with reducing the risk of chronic degenerative and non-communicable diseases8.
As defined by the World Health Organization (WHO)/Food and Agriculture Organization (FAO)9, probiotics are considered living microorganisms which, when administered in adequate amounts, confer benefits on the health of the host. Probiotics have the potential to maintain intestinal balance, preserve immune health and act with benefits in the treatment and prevention of inflammatory bowel diseases, especially for ulcerative colitis8,10.
The demand for probiotic non-dairy foods and drinks has grown due to the greater emergence of individuals with allergies to milk protein and lactose intolerance. Due to the scarcity of these products, the food industry has sought to innovate with probiotic products derived from vegetables. With that orange juice has become a great option due to the ease of obtaining it, as it is the most consumed juice in the world11.
In the pharmaceutical industry, there are formulations that comprise Pediococcus acidilactici as a probiotic to reduce symptoms of adverse gastrointestinal conditions12. Its effectiveness lies in the anti-inflammatory and anti-oxidative action against the stress caused in the intestinal mucosa, which makes Pediococcus spp. species as convenient methods in the prevention of intestinal disorders, such as ulcerative colitis13,14,15.
Given the current relevance of using Pediococcus spp. for treating and preventing IBD, it presents an intriguing therapeutic possibility for ulcerative colitis. It is still necessary to develop more consistent in vivo research through randomized controlled studies addressing, together, the main clinical, microbiological and immunological parameters to ensure the use of new Pediococcus acidilactici strains as useful tools in the promotion of human health16.
In this context, the preponderance of evidence suggests that marked alterations in diet can perturb the taxonomical configuration of the microbiota within a few days17. According to David et al.18, short-term changes (4 days) on the human diets was sufficient to introduce distinct community-wide alterations of the intestinal microbiota.
Although few studies have been published on the applicability of Pediococcus acidilactici as a probiotic strain related to UC, none of them evaluated the effects of probiotic orange juice containing a new isolate on the animal model of ulcerative colitis, named as Pediococcus acidilactici CE51. Thus, the objective of this study was to evaluate the anti-inflammatory response and gut modulation of probiotic orange juice treatment in a short-term consumption (5 days) and (15 days) in gut inflammation induced in murine model.
Material and methods
Elaboration of probiotic drink
The probiotic drink was prepared according to Vieira and collaborators11. Concentrated orange juice (Campo Largo, Brazil) without added preservatives and sugar was used, and inoculated P. acidilactici CE51 at 108 CFU/mL11. The juice was stored in a refrigerator at 5 °C (Gelopar, Brazil) for up to 07 days for use in animal experimentation.
Animals and experimental groups
Male Mus musculus (swiss) eight-week-old mice weighing 34.5 to 54.0 g, from the animal house of the University of Western Sao Paulo were used. The animals were kept in polypropylene boxes, on a shelf with an air filtration system and temperature and relative humidity control (23 °C; 60–70% humidity), light (12 h light/dark cycle), fed with mice feed (NUVILAB CR-1, QUIMTIA, Brazil) and filtered drinking water ad libitum19,20 and acclimated to the conditions for at least seven days before experimental manipulation. The experiments took place during the clear phase of the cycle and were carried out in accordance with the approval of the Ethics Committee on the Use of Animals of University of Western Sao Paulo (CEUA/Unoeste—nº 5897). This study was carried out in compliance with the ARRIVE guidelines. A total of 45 mice were used, randomly distributed into five groups containing nine animals, divided as shown in Table 1.
Experimental colitis induced by dextran sodium sulfate
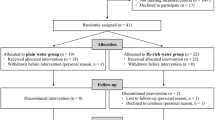
The experiment period was divided into four phases as shown in Fig. 1: (1) adaptation (7 days), (2) treatment with probiotics or placebo (9 days), (3) induction of colitis (CL) and treatment with probiotic (CLPR), placebo (CLP) or sulfasalazine (CLS) (6 days) and 4) treatment with probiotic, placebo or sulfasalazine (5 and 15 days).
Experimental design. The experiment was carried out with 45 animals divided in 5 experimental groups Control (C); Colitis (CL); Colitis + Probiotic (CLPR; Colitis + Placebo (CLP); Colitis + Sulfasalazine (CLS) for 37 days divided in the following stages: Adaptation period of 7 days (Blue line); T0/d0: Initiation of administration of probiotic orange juice containing P. acidilactici CE51 for the CLPR group, or orange juice (placebo) for the CLP group, which lasted until the last day of the experiment (Green line); T1/d09: Beginning of the period of induction of ulcerative colitis by DSS, which lasted 6 consecutive days (Yellow line); T2/d15: The arrow indicates the withdrawal of the DSS and the beginning of the treatments that lasted 5 and 15 days. In this period also started treatment with sulfasalazine (Orange line); T3/d20: Exact time when the first euthanasia occurred (Euthanasia 1) after treatment with probiotic orange juice, placebo or sulfasalazine for 5 days; T4/d30: Exact time when the second euthanasia (Euthanasia 2) occurred after treatment with probiotic orange juice, placebo or sulfasalazine for 15 days. d Day (Above the colored lines); T Time (Below the colored lines); Black arrow Induction of ulcerative colitis by DSS.
The experimental colitis was chemically induced, through the administration of dextran sodium sulfate (DSS) (Sigma-Aldrich, St. Louis, MO, USA). The DSS (3%) was dissolved (15 g) in the filtered water (500 mL) supplied daily to the animals, and administered over a period of 6 days21,22. The animals were monitored daily for weight and clinical signs.
The severity of colitis was measured every day taking into account the three parameters and their respective scores of the disease activity index (DAI). The weight of the animals was evaluated by an analytical balance (Gehaka, BT8000, Brazil), classified by the scores: body weight loss (score 0, no weight loss compared to initial weight; (1) weight loss within 1–5%; (2) weight loss within 5–10%; (3) weight loss within 10–20%; (4) greater than 20% weight loss). The stool consistency by observation of the feces in the cages (score 0, normal—solid consistency); 2, loose stool but with some solidity; 4, diarrhea). For the analysis of occult blood in the feces, the Meyer Method was used in order to identify the presence of hemoglobin in the sample23. The presence of occult/visible blood in the stools was also classified by the following score: score 0, negative; 2, fecal occult blood test positive; 4, gross bleeding24,25.
The animals in the probiotic (CLPR) and placebo (CLP) groups received 50 µL of the products under study daily, orally by means of a micropipette (Single channel Pipette, LABMATE Pro, Poland) (enough to guarantee a daily intake of 108 CFU of the probiotic microorganisms in probiotic orange juice group). The animals of the Sulfasalazine group (CLS) received the drug (Sigma-Aldrich, St. Louis, MO, USA) daily, orally through a micropipette (Single channel Pipette, LABMATE Pro, Poland) (10 mg/kg/weight). The Control (C) and Colitis (CL) groups did not receive any of the treatments, only water and food. After 5 days of treatment, four animals from each group were euthanized, and with 15 days, the remaining five animals from each group. For euthanasia, anesthetics Ketamine Hydrochloride (10%) (Rompun, Bayer HealthCare, Kansas, MO, USA and Xylazine Hydrochloride (2%) (Bayer, Leverkusen, Germany) were administered intraperitoneally (75 e 10 mg/kg). Laparotomy was performed and the organs of the gastrointestinal system (the small and large intestines, stomach, liver and spleen) were removed and opened longitudinally for later macroscopic and histological analysis.
Histological analysis
After each treatment period (5 and 15 days), the animals were euthanized. The small and large intestines were removed and then, the lengths were measured. The stomach, liver and spleen were also collected to evaluate the potential general effect of the induced inflammation in other parts of the body and possible toxic effect of probiotic juice.
All organs were cleaned (fats and tissues adhered to the wall were removed), washed in running water to remove feces, fixed by immersion in a solution of 10% buffered formalin for 48 h, processed routinely and embedded in paraffin. Histological sections of 5 μm thick were stained with Hematoxylin–eosin (HE) for analysis under light microscopy (NIKON Labophot, Japan) by one blind trained researcher to the treatment.
These general parameters were evaluated in the stomach, and small and large intestines with their respective scores were interstitial inflammatory infiltrate (0 = absent, 1 = mild, 2 = moderate, 3 = intense) and type of inflammatory cell present (polymorphonuclear and/or mononuclear); tissue congestion (0 = absent, 1 = mild, 2 = moderate, 3 = severe). The following parameters were also specifically analyzed: Intestine (small and large) the following parameters were also evaluated: lymphoid hyperplasia (0 = absent; 1 = present); epithelial ulceration (0 = absent; 1 = present and small; 2 = present and extensive); regenerative atypias of the epithelium (0 = absent; 1 = present); and intestinal wall necrosis (0 = absent; 1 = present); Spleen: white pulp hyperplasia (0 = absent; 1 = present) and red pulp hyperplasia (0 = absent; 1 = present); Liver: steatosis (0 = absent; 1 = present) and its pattern: macrovesicular; microvesicular; or mixed (macro and microvesicular)26.
Histomorphometry analysis was performed, obtaining 3 selected sections of each animal. The height (μm) of 10 villi and 10 crypts of each animal was obtained by measuring the vertical distance from the upper extremity to the lower limit of each. The villus and crypt height values for each animal were represented by the mean values of the three histological sections27.
The images of the histological sections were captured in a 100 × magnification by a digital camera connected to a light microscope (LEICA DM750, Leica Microsystems, Germany). The digital images were analyzed using appropriate software (Image J® 1.50b, National Institutes of Health, USA) by one blind trained researcher27.
Serum dosage for TNF-α and C-reactive protein
The animals' blood was collected by cardiac puncture under anesthesia, and then centrifuged (15 min at 1000×g at room temperature) (FANEM®, 206 BL, Brazil). The serum was collected and stored at – 20 °C until analysis. The concentration of TNF-α and C-reactive protein (CRP) were determined by the enzyme-linked immunosorbent assay (ELISA) with commercial kits (FineTest, Wuhan, China and Millipore, Billerica, MA, USA, respectively) with intra- and inter-assay variations (CV%) of < 8% and < 10% to TNF-α and ± 8% and ± 7% to CRP. Briefly, the serum samples were incubated with antibodies (anti-TNF or anti-PCR) and labelled with horseradish peroxidase for subsequent enzymatic reaction with tetramethylbenzidine. The reaction was stopped by the addition of acidic solution and the resulting absorbance was measured spectrophotometrically at 450 nm (SpectraMax® PLUS 384 Microplate Reader, MOLECULAR DEVICES, EUA).
Metagenomic analysis of the intestinal microbiota
A stool pool of the middle intestine of 4 (treatment = 5 days) and 5 (treatment = 15 days) mice per treatment (Control, Colitis, Probiotic, Placebo and Sulfasalazine) were sampled. The intestinal content (feces) of each animal was collected, stored individually in microtubes free of DNases and RNases and, immediately, frozen at – 20 °C (Freezer Indrel Scientific, Brazil) for subsequent metagenomic analysis. DNA extraction and DNA sequencing analysis of the samples was performed by Neoprospecta Microbiome Technologies (Florianópolis, SC, Brazil) using a molecular technique based on the sequencing of the 16S rRNA gene, amplifying the V3-V4 regions using 341F/806R primers, through the Illumina MiSeq sequencer. Sequence of primers were 341F 5′-CCTAYGGGRBGCASCAG-3′ and 806R 5′-GGACTACNNGGTATCTAAT-3′. The DNA concentration of the amplicon pool was estimated with Picogreen dsDNA assays (Invitrogen, USA), and then the pooled libraries were diluted for accurate quantification of qPCR using KAPA Library Quantification Kit for Illumina platforms (KAPA Biosystems, Woburn, MA, USA).
The library bank was adjusted to a final concentration of 11 pM and sequenced in a MiSeq system, using the Illumina primers provided in the kit. A 300 nt single-ended run was performed using a V2 × 300 sequencing kit.
Sequence data were processed and analyzed with QIIME [Quantitative Insights Into Microbial Ecology, version 2022.2.0 (https://qiime2.org/)]. On average, a total of 153,269 raw reads were sequenced. Initially, during the demultiplexing and trimming steps, low quality reads were removed, such as reads up to Q30, unsatisfactory length reads, and chimeras were removed with QIIME. After this process, the dataset contained an average of 106.918 raw reads. The clean readings were used in defining the Amplicon Sequence Variant (ASV).
To measure the rates present in the samples, a predictor model of the V3 and V4 region was used. Heatmaps and barplots of relative abundance of ASVs were generated with Python (version 3.7) through codes developed by the company ByMyCell Inova Simples Ltda.
Statistical analysis
All analyzed data were submitted to the normality test using the Kolmogorov–Smirnov test. The animal sample size calculation was performed according to Arifin and Zahiruddin28.
The comparison between two groups was performed using the Student's t test for unpaired data or the Mann–Whitney test. When three or more groups were compared, analysis of variance (ANOVA) was used, followed by the Newman-keuls post-test to verify the difference between the groups. The results were considered significant for p < 0.05. The statistical program used was GraphPad Prism 3.0.
Ethics approval
The experiments were carried out in accordance with the approval of the Ethics Committee on the Use of Animals of University of Western Sao Paulo (CEUA / Unoeste—nº 5897). This study was carried out in compliance with the ARRIVE guidelines.
Results
Beneficial effect of probiotic orange juice on DAI analysis in DSS-induced colitis
Clinical signs, symptomatologic parameters and macroscopic damage were analyzed according to the disease activity index criteria. There was a change in stool consistency and the presence of visible and occult blood was observed for up to 5 days after induction of colitis with DSS. However, the parameters were more intense in the colitis, placebo and sulfasalazine groups. Despite the loss of two mice (1 colitis group and 1 placebo group), no significant difference was observed in the survival curve between the groups after 5 and 15 days of treatment (Fig. 2A,B).
Beneficial effect of probiotic orange juice on DAI analysis in DSS-induced colitis. Survival curve (A, B) and weight variation (C, D) of mice treated with 5 days (left side) (n = 4) and 15 days (right side) (n = 5) with probiotic (orange juice containing Pediococcus acidilactici CE51), placebo (orange juice) or sulfasalazine (10 mg/kg/weight) after DSS administration (3%) for induced colitis. The control group was not submitted to the colitis protocol. Comparison was done between all groups of each treatment period. *Statistically significant difference in weight variation between control group and groups: colitis, placebo and probiotic.
After 5 days of treatment, no significant changes were observed in the weight variation of experimental groups of animals during the period before induction of colitis and after treatment with probiotic, placebo and sulfasalazine (Fig. 2C). However, the colitis, probiotic, placebo groups showed a significant decrease in weight in comparison to control group after 15 days of treatment (Fig. 2D).
Attenuation of inflammation by probiotic orange juice treatment in histopathological analysis in DSS-induced colitis with 5 days of treatment
Histopathological analyzes were performed on the stomach, small intestine, large intestine, liver and spleen (Table 2 and Fig. 3). No significant changes were found for stomach and liver (data not shown).
Attenuation of inflammation by probiotic orange juice treatment in histopathological analysis in DSS-induced colitis with 5 days of treatment. Photo microscopy of the small intestine: (A) Normal mucosa (group C animal). (B) Moderate inflammation (arrow) (animal in the CL group). (C) Normal mucosa (animal in the CLPR group). (D) Lymphoid hyperplasia (wide arrow), and moderate inflammation (thin arrow) (animal in the CLP group). (E) Mild inflammation (arrows) (animal in the CLS group). Hematoxylin–eosin, 100 × magnification. Large intestine: (F) Normal mucosa (group C animal) (Hematoxylin–eosin, 100 × magnification). (G) Ulcerated area of the mucosa (arrow) and transmural inflammation (animal in the CL group) (Hematoxylin–eosin, 100 × magnification). (H) Mild inflammation of the mucosa (arrow) (animal in the CLPR group) (Hematoxylin–eosin, 100 × magnification). Spleen: (I) Lymphoid hyperplasia (arrow) (animal in the CLP group) (Hematoxylin–eosin, 40 × magnification). (J) Mild inflammation of the mucosa (arrow) (animal in the CLS group) (Hematoxylin–eosin, 100 × magnification). (K) Normal splenic parenchyma (group C animal) (Hematoxylin–eosin, 40 × magnification). (L) Exuberant white pulp hyperplasia with a “starry sky” aspect (animal in the CL group) (Hematoxylin–eosin, 100 × magnification). (M) White pulp hyperplasia (animal in the CLPR group) (Hematoxylin–eosin, 40 × magnification). (N) White pulp hyperplasia (CLP group animal) (Hematoxylin–eosin, 40 × magnification). (O) White pulp hyperplasia (CLS group animal) (Hematoxylin–eosin, 40 × magnification).
The analysis of the small intestine evaluated parameters such as intensity of inflammation and villus measurements. With 5 days of treatment, a lower intensity of inflammation was observed in the probiotic and sulfasalazine group compared to the colitis group (p < 0.05). In the 15-day treatment, a 40% reduction in inflammation was observed in the sulfasalazine group and 20% in the probiotic group (p < 0.05). The measurements of intestinal villi showed a significant increase in the probiotic and placebo group after treatment for 5 days (p < 0.05). However, after 15 days of treatment, no significant changes were observed among the groups.
In the large intestine, the measurement of crypts, intensity of inflammation and presence of ulceration were evaluated. Crypt measurements were higher in the placebo group treated for 5 days (p < 0.05) and did not show significant differences with 15 days of treatment. There was a significant reduction of 25% in the intensity of inflammation and 25% of the presence of ulceration in the probiotic group compared to the colitis group after 5 days, however, with 15 days of treatment a more pronounced reduction was observed in the sulfasalazine group (p < 0.05).
White pulp hyperplasia was evaluated in the spleen. There was a 50% reduction in hyperplasia in the probiotic, placebo and sulfasalazine group after 5 days of treatment (p < 0.05). However, the reduction was 35, 50 and 55% respectively in the probiotic, placebo and sulfasalazine groups with treatment for 15 days compared to the untreated colitis group (p < 0.05).
Reduction of C-reactive protein levels after 15 days of treatment with P. acidilactici CE51 on DSS-induced colitis
The measurement of TNF-α demonstrated similarity between the groups during 5 and 15 days of treatment with probiotic, placebo or sulfasalazine (Fig. 4A). The treatment time impacted the levels of C-reactive protein, with a higher dosage being observed with a 5-day treatment for all groups that had colitis induction (p < 0.05). The sulfasalazine group with 15 days of treatment showed a significant reduction when compared with the other groups (p < 0.05) (Fig. 4B).
Reduction of C-reactive protein levels after 15 days of treatment with P. acidilactici CE51 on DSS-induced colitis. Serum concentrations of TNF-α (A) and C-reactive protein (B) from mice treated for 5 days (n = 4) and 15 days (n = 5) with probiotic (orange juice containing Pediococcus acidilactici CE51), placebo (orange juice) and sulfasalazine (10 mg/kg/weight) after DSS administration (3%) to induce colitis. The concentration of TNF-α and C-reactive protein (CRP) were determined by the enzyme-linked immunosorbent assay (ELISA) and, in the final of the test, the resulting absorbance was measured spectrophotometrically at 450 nm. The control group was not submitted to the colitis protocol. *Statistical difference in relation to the control group (p < 0.05). aStatistical difference in relation to the colitis, placebo and probiotic group (p < 0.05).
Probiotic orange juice positively modulates the gut microbial communities in DSS-induced colitis
Figure 5 shows the relationship between species diversity, the phylum Firmicutes/Bacteroidetes (F/B) ratio and the number of specimens in the Lactobacillaceae family. There was a significant increase in the diversity of bacterial species after 5 days of treatment for the probiotic group and colitis group (p < 0.05) (Fig. 5A). There were no significant changes after 15 days of treatment (Fig. 5B).
Probiotic orange juice positively modulates the gut microbial communities in DSS-induced colitis. Evaluation of the quantitative ratio of the phylum Firmicutes/Bacteroidetes (Y axis), number of species (x axis) and number of specimens of the Lactobacillaceae family (circle size) (A and B). Relative quantity of the most prevalent bacterial species (C and D). Results obtained from the metagenomic analysis of the pool of feces obtained from mice treated for 5 days (n = 4) and 15 days (n = 5) with probiotic (orange juice containing Pediococcus acidilactici CE51), placebo (juice orange) and sulfasalazine (10 mg/kg/weight) after DSS administration (3%) to induce colitis. The control group was not submitted to the colitis protocol.
The quantitative ratio of the phylum Firmicutes/Bacteroidetes was reduced in the colitis, placebo and sulfasalazine group after 5 days of treatment (p < 0.05). After 15 days of treatment, a significant decrease was observed in all groups (p < 0.05). The number of specimens of the Lactobacillaceae family, represented by the size of the circle, was reduced in about 50% for the probiotic group after 5 days of treatment (p < 0.05). However, such a reduction was not observed after 15 days of treatment.
The relative quantity of bacterial species after 5 days of treatment had a predominance of Lactobacillus murinus in the control group and sulfasalazine with approximately 70% each (Fig. 5C). Colitis, probiotic and placebo groups had a significant reduction in Lactobacillus murinus and an increase in the proportion of Lactobacillus hominis and Lactobacillus reuteri. However, the probiotic group also showed an increase in Enterococcus faecalis (p < 0.05).
After 15 days of treatment, a reduction in the relative amount of Lactobacillus murinus was observed in the probiotic group compared to the control group (p < 0.05) (Fig. 5D). On the other hand, there was an increase in Lactobacillus hominis for the colitis, probiotic, placebo and sulfasalazine group (p < 0.05). In the probiotic group, a significant increase in Lactobacillus helveticus was also observed (p < 0.05).
Discussion
In view of the need for studies on compounds that act in the treatment and prevention of ulcerative colitis, this study evaluated and found the positive effect of the probiotic drink containing P. acidilactici CE51 regarding the reduction of inflammatory parameters presented in histopathological analyzes and modulation of the gut microbiota composition.
Adequate concentration and administration of probiotic strains is essential to induce their positive effect, requiring an inoculum of at least 106 CFU/mL of the live probiotic strain at the time of consumption29. In the present study, a concentration of 108 CFU was used/mL and the effectiveness of this administration in reducing the effects of induced colitis has been demonstrated. Similar results were obtained by Srutkova et al.30 and Mansour et al.14, respectively for the use of 2 × 108 CFUs of B. longum ssp. Longum CCM 7952 (Bl 7952) and CCDM 372 (Bl 372) in the prevention of DSS-induced colitis, and orally daily dose containing CFU 109 Pediococcus acidilactici strains induction for colitis by acetic acid.
Histopathological analyzes showed that the group that received P. acidilactici CE51 for 5 days showed a decrease in the intensity of inflammation in the intestines, an increase in intestinal villi, absence of ulceration and a reduction in white pulp hyperplasia when compared to the untreated colitis group. After 15 days of treatment with the P. acidilactici CE51, the evidence was less pronounced.
The inflammatory process in the intestinal mucosa results in reduced villi, digestive, and absorptive activities. The probiotic strains compete with pathogenic microorganisms for binding sites, reducing the occurrence of diarrhea and favoring the absorption of nutrients, this mechanism directly influences the recovery of the intestinal mucosa, increasing the height of the villi31. This positive effect could be observed in the probiotic group treated for 5 days.
The white pulp present in the spleen is particularly lymphatic and plays a fundamental role in the immunological activity32, which justifies the hyperplasia of the white pulp, since this increase is directly related to the proliferation of leukocytes due to a severe inflammatory process induced in these animals.
Evidence suggests that UC leads to complications in gastric mucosal lesions, involving tissue inflammation and destruction, potentially causing gastritis and ulcers33. Kwon et al.34 show that DSS-induced colitis is associated with adipose tissue dysfunction and disrupted hepatic lipid metabolism leading to hepatosteatosis and dyslipidemia in mice. However, in the present study there were no histopathological differences in both organs and tissues35.
Orange juice, alone, also had the potential to reduce inflammatory parameters in murine-induced colitis. There was a reduction in the intensity of inflammation in the small intestine, an increase in the height of the villi and crypts and a reduction in spleen hyperplasia. Citrus juice, especially orange juice, is associated with improved immunity, as it is a source of vitamin C, flavonoids and bioactive compounds, which together have a potential anti-inflammatory, antioxidant effect and improved endothelial function36. This fact highlights the importance of orange as a food matrix that can reduce inflammatory biomarkers and serve as an attractive strategy to counteract these types of stresses.
Although no evidence has been found in the literature using P. acidilactici CE51 in the treatment of ulcerative colitis, the results of improvement in the histological parameters, as well as aid in the protection of the epithelial barrier is in agreement to the findings of Duary et al.37. In that work, the anti-inflammatory and immunomodulatory efficacy of probiotic strains of Lactobacillus plantarum Lp91 was observed as a prevention of ulcerative colitis when compared to the untreated colitis group and the colitis group treated with L. plantarum CSCC5276. The animals received the live cells at 109 CFU resuspended in 25 μL in PBS by mouth37.
Wang et al.38 verified the mixture (1:1, 109 CFU/mL) of Lactobacillus plantarum ZDY2013 and Bifidobacterium bifidum WBIN03 as an excellent strategy of antioxidant activity and immune stress relief in mice with DSS-induced colitis. Those animals were treated for 7 days with probiotics, with a reduction in pro-inflammatory cytokines, such as TNF-α, and an increase in antioxidant factors, such as SOD1, SOD2, GPX2. Groeger et al.39 when using 1 × 1010 CFU viable Bifidobacterium infantis 35624 in the treatment of gastrointestinal and non-gastrointestinal inflammatory disorders, concluded that this strain reduced the levels of C-reactive protein and TNF-α, but had no impact on ulcerative colitis.
The fact that the measurement of TNF-α did not give statistical difference between the groups treated for 5 and 15 days in the present study, corroborates with a systematic review where it was found that the use of probiotics does not impact the measurements of serum IL10 and TNF-α40. Regarding the C-reactive protein dosage, a significant reduction was demonstrated only in the sulfasalazine group after 15 days of treatment. The dosages of C-reactive protein and TNF-α were not influenced by the administration of P. acidilactici CE51 probable because they are considered markers of systemic inflammation and due to the short term of administration of the CE51 probiotic41. Studies evaluating its application for a longer period of time or its concomitant use with sulfasalazine are necessary to further evaluate its potential to improve the imumodulatory response of colitis induced in animals.
Studies have shown that during an IBD there is a significant reduction in potentially beneficial species such as Bifidobacterium, Lactobacilli, and Firmicutes and Bacteroidetes phyla, which make up the healthy intestinal microbiota. On the other hand, there may be a large increase in pathogenic strains under IBD conditions such as: Campylobacter jejuni, Salmonella enterica, Vibrio cholera and Escherichia coli (E. coli) and Bacteroides fragilis42.
The gut microbiota is characterized as a diverse microbial community present in the gastrointestinal tract that maintains gut symbiosis in the host. In it, the two dominant bacterial phyla, Firmicutes and Bacteroidetes, are present, which consist of more than 90% of the total community. The relationship between the two is expressed as the Firmicutes/Bacteroidetes ratio, commonly related to intestinal pathological conditions43,44. As the phyla Firmicutes and Bacteroidetes predominate in healthy intestines and help produce epithelial metabolites. In IBD, the microbiota is represented with relative absence of these phyla and with exacerbated presentation of Enterobacteriaceae and Fusobacteria45.
In intestinal biopsies and stool samples from UC, it is common to observe disproportions in the F/B ratio, in which Firmicutes are decreasing and Bacteroidetes are generally abundant46. In the present study, a significant decrease in F/B in the colitis, placebo and sulfasalazine groups treated for 5 days and maintaining the proportion in the probiotic group equivalent to the control group. This data highlights the maintenance of a healthy intestinal microbiota in the group that received P. acidilactici CE51, since the decrease in the abundance of Firmicutes and Bacteroidetes is related to the development and advancement of the disease, resulting from bacterial dysbiosis in inflamed sites compared to non-inflamed tissues47.
Strains of the Lactobacillaceae and Bifidobacteriaceae families are characterized as the most common probiotics. The family Lactobacillaceae (phylum Firmicutes) is predominant in the gut microbiota, comprising 31 genera, principally Lactobacillus species. The presence of Lactobacillaceae in the gut is important for preventing colonization by enteropathogenic bacteria through competitive adhesion and aggregation to binding sites. In addition, they demonstrate a protective effect on the intestinal tract, as they increase immunity and produce antimicrobial substances that inhibit pathogens, thus exerting antagonism against them48,49.
In the intestinal lumen, microbial genera predominate that can be identified in the feces, such as Bacteroides, Bifidobacterium, Streptococcus, Enterobacteriacae, Enterococcus, Clostridium, Lactobacillus and Ruminococcus50. The number of specimens from the Lactobacillaceae family showed a significant reduction after the 5-day period, possibly attributed to an increase in the species Enterococcus faecalis belonging to the Enterococcaceae family. Probably, this fact may be related to the condition of competition of different bacterial species for nutrients and adhesion to the mucosa in this condition51.
The results presented here did not show the presence of P. acidilactici CE51 in fecal samples, and this may be related to the application of the metagenomic technique, which has sensitivity limitations when it comes to a complex sample and which presents a microbiota with a high diversity of species with possible inhibitors; as is the case with stool analysis52. In addition, the bacteria may have been unable to colonize and compete with the murine gastrointestinal microbiota. Similar results were observed in the study by Grimm et al.53, where there was treatment for B. bifidum S17/pMGC (2 × 109 CFU in 20 μL of PBS), however, fecal levels were decreased during the pretreatment and DSS phase, making it difficult to detect them in the feces.
It was possible to observe a positive modulation of the species that make up the intestinal microbiota with the treatment of the P. acidilactici CE51. It is known that Lactobacillus murinus is the most prevalent and prevalent isolate found in this rodent species chosen for the experiment, as demonstrated in the control and sulfasalazine group with 5 days of treatment54. When analyzing the animals treated for 15 days, it was noted that all groups of animals showed an increase in Lactobacillus hominis, one of the most common species found in the intestine55. In addition, the group that received P. acidilactici CE51 also had a significant and predominant increase in Lactobacillus helveticus. These microorganisms assist in intestinal positive modulation, can improve the inflammatory response and are considered effective in the treatment of diarrhea associated with antibiotics and liver damage56.
In the literature, the use of anti-inflammatory drugs and probiotic mixtures is highlighted as the main means of combating UC. Palumbo et al.57 showed that patients treated with mesalazine and a mixture of probiotics containing Lactobacillus salivarius, Lactobacillus acidophilus and Bifidobacterium bifidus strain BGN4 (Acronelle®, Bromatech srl, Milan, Italy) showed significant improvement in relation to those treated with mesalazine alone. This demonstrates that the combination of therapies generates positive effects on the patient's health and the probiotic mixtures help in the effective improvement of the clinical condition, which can potentiate anti-inflammatory therapy. A study emphasized the potential of capsules containing 2.5–25 × 109 viable bacteria (Mutaflor 100 mg; Ardeypharm GmbH, Herdecke, Germany)of Escherichia coli Nissle 1917 (EcN) probiotic strain to maintain remission in patients with ulcerative colitis and be equivalent to the standard treatment with mesalazine58. Other researchers, applying the same strain in experiments with mice, reported the benefits in relation to pathological and/or physiological parameters, and daily 108 CFU of live bacteria and 1.5–2 × 108 CFU (Mutaflor mite, Ardeypharm, Germany) EcN twice daily by oral were applied, respectively59,60.
As a result of these data, a comparison can be established with the findings of the present study, since P. acidilactici CE51 was shown to be more effective than the treatment with the sulfasalazine drug in some parameters such as increased villi in the small intestine, reduced ulceration and intensity of inflammation in the large intestine and maintenance of the proportion of the phylum F/B when used for 5 days in the treatment.
Thus, these data suggest that the benefits obtained by the probiotic drink containing P. acidilactici CE51 are more evident in 5 days of treatment. After this period, the organism is probably able to obtain an inflammatory response for the recovery of tissue damage generated by the induction of colitis. Furthermore, it is worth mentioning that the intestine has an accelerated cell multiplication and renewal process, which may also favor its resourcefulness in recovery61.
Conclusion
In conclusion, the results showed the potential beneficial effect of the application of probiotic orange juice containing Pediococcus acidilactici CE51 as a promising therapy in the treatment and management of colitis in murine, being able to maintain the integrity of the intestinal barrier, maintain body weight, assist in the decline of DAI and positively modulated the gut microbiota.
Data availability
Derived data supporting the findings of this study are available from the corresponding author on request.
References
Flynn, S. & Eisenstein, S. Inflammatory bowel disease presentation and diagnosis. Surg. Clin. N. Am. 99, 1051–1062. https://doi.org/10.1016/j.suc.2019.08.001 (2019).
Silva, A. P. F. & Júnior, M. R. M. Fecal biomarkers useful on inflammatory bowel disease: A systematic review. Arq. Ciênc. Saúde. 23, 16–20 (2016).
Gajendran, M. et al. A comprehensive review and update on ulcerative colitis. Dis. Mon. 65, 100851. https://doi.org/10.1016/j.disamonth.2019.02.004 (2019).
Jeong, D. Y. et al. Induction and maintenance treatment of inflammatory bowel disease: A comprehensive review. Autoimmun. Rev. 18, 439–454. https://doi.org/10.1016/j.autrev.2019.03.002 (2019).
Cardozo, W. S. & Sobrado, C. W. Doença Inflamatória Intestinal (Manole, 2015).
Granato, D. et al. Functional foods: Product development, technological trends, efficacy testing, and safety. Annu. Rev. Food Sci. Technol. 11, 93–118. https://doi.org/10.1146/annurev-food-032519-051708 (2020).
Shadnoush, M. et al. Effects of probiotics on gut microbiota in patients with inflammatory bowel disease: A double-blind, placebo-controlled clinical trial. Korean J. Gastroenterol. 65, 215. https://doi.org/10.4166/kjg.2015.65.4.215 (2015).
Min, M., Bunt, C. R., Mason, S. L. & Hussain, M. A. Non-dairy probiotic food products: An emerging group of functional foods. Crit. Rev. Food Sci. Nutr. 59, 2626–2641. https://doi.org/10.1080/10408398.2018.1462760 (2019).
Food and Agriculture Organization (FAO) & World Health Organization (WHO). Report of a Joint FAO/WHO Expert Consultation on Evaluation of Health and Nutritional Properties of Probiotics in Food Including Powder Milk with Live Lactic Acid Bacteria, 1–4 (2001).
Judkins, T. C., Archer, D. L., Kramer, D. C. & Solch, R. J. Probiotics, nutrition, and the small intestine. Curr. Gastroenterol. Rep. 22, 2. https://doi.org/10.1007/s11894-019-0740-3 (2020).
Vieira, K. C. O. et al. Development and viability of probiotic orange juice supplemented by Pediococcus acidilactici CE51. LWT-Food Sci. Technol. 130, 109637. https://doi.org/10.1016/j.lwt.2020.109637 (2020).
Mazo, J. E. & Castellana, J. C. Probiotic Composition for Use in the Treatment of Bowel Inflammation. WO2011092261A1 WIPO (PCT).
Jang, H. M. et al. Enterococcus faecium and Pediococcus acidilactici deteriorate Enterobacteriaceae-induced depression and colitis in mice. Sci. Rep. 12, 9389. https://doi.org/10.1038/s41598-022-13629-9 (2022).
Mansour, N. M., Elkalla, W. S., Ragab, Y. M. & Ramadan, M. A. Inhibition of acetic acid-induced colitis in rats by new Pediococcus acidilactici strains, vitamin producers recovered from human gut microbiota. PLoS ONE 16, e0255092. https://doi.org/10.1371/journal.pone.0255092 (2021).
Bamba, S. et al. Effect of fermented vegetable beverage containing Pediococcus pentosaceus in patients with mild to moderate ulcerative colitis. Biomed. Rep. 9, 74–80. https://doi.org/10.3892/br.2018.1099 (2018).
Meghwanshi, G. K., Praveen, G., Rakesh, P. & Sinh, S. K. Probiotics and prebiotics. Int. J. Microbiol. Res. 8, 762–768 (2016).
Uhr, G. T., Dohnalová, L. & Thaiss, C. A. The dimension of time in host-microbiome interactions. MSystems. 4, e00216. https://doi.org/10.1128/mSystems.00216-18 (2019).
David, L. A. et al. Diet rapidly and reproducibly alters the human gut microbiome. Nature 505, 559–563. https://doi.org/10.1038/nature12820 (2014).
Cavallini, D. C. U., Zordão, O. P., Celiberto, L. S., Zuanon, J. A. S. & Spolidorio, L. C. Efeito da Ingestão Regular de Uma Bebida Probiótica na Fase Aguda da Colite Ulcerativa Induzida em Camundongos. [Dissertation/Master’s Thesis]. (Universidade Federal do Rio Grande do Sul, 2016).
Celiberto, L. S. Efeito de Uma Bebida Probiótica (Enterococcus faecium CRL 183 e Bifidobacterium longum ATCC 15707) à Base de Extrato Aquoso de Soja no Desenvolvimento de Colite Quimicamente Induzida em Ratos. [Dissertation/Master’s Thesis]. (Universidade Estadual Paulista, 2014).
Chassaing, B., Aitken, J. D., Malleshappa, M. & Vijay-Kumar, M. Dextran sulfate sodium (DSS)-induced colitis in mice. Curr. Protoc. Immunol. 104, 1–15. https://doi.org/10.1002/0471142735.im1525s104 (2014).
Laroui, H. et al. Dextran sodium sulfate (DSS) induces colitis in mice by forming nano-lipocomplexes with medium-chain-length fatty acids in the colon. PLoS ONE 7, e32084. https://doi.org/10.1371/journal.pone.0032084 (2012).
Silva, F. M., Silva, R. C. & Medeiros, J. S. Research of blood hidden by Meyer’s method. J. Biol. Pharm. Agric. Manag. 10, 1–5 (2014).
Cooper, H. S., Murthy, S. N., Shah, R. S. & Sedergran, D. J. Clinicopathologic study of dextran sulfate sodium experimental murine colitis. Lab. Invest. 69, 238–249 (1993).
Wang, Y. et al. IL-21/IL-21R signaling suppresses intestinal inflammation induced by DSS through regulation of Th responses in lamina propria in mice. Sci. Rep. 6, 31881. https://doi.org/10.1038/srep31881 (2016).
Pegoraro, C. M. R. et al. Protective effects of Bidens pilosa on hepatoxicity and nephrotoxicity induced by carbon tetrachloride in rats. Drug Chem. Toxicol. 44, 64–74. https://doi.org/10.1080/01480545.2018.1526182 (2021).
Gerhard, D. et al. Probiotic therapy reduces inflammation and improves intestinal morphology in rats with induced oral mucositis. Braz. Oral Res. 31, e71. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0071 (2017).
Arifin, W. N. & Zahiruddin, W. M. Sample size calculation in animal studies using resource equation approach. Malay. J. Med. Sci. 24, 101–105. https://doi.org/10.21315/mjms2017.24.5.11 (2017).
Nguyen, B. T. et al. Probiotic beverage from pineapple juice fermented with Lactobacillus and Bifidobacterium strains. Front. Nutr. 6, 54. https://doi.org/10.3389/fnut.2019.00054 (2019).
Srutkova, D. et al. Bifidobacterium longum CCM 7952 promotes epithelial barrier function and prevents acute DSS-induced colitis in strictly strain-specific manner. PLoS ONE 10, e0134050. https://doi.org/10.1371/journal.pone.0134050 (2015).
Pelicano, E. R. L. et al. Intestinal mucosa structure and ultrastructure in broilers fed with diets supplemented with different probiotics. Rev. Port. Cienc. Vet. 98, 125–134 (2003).
Suttorp, M. & Classen, C. F. Splenomegaly in children and adolescents. Front. Pediat. 9, 704635. https://doi.org/10.3389/fped.2021.704635 (2021).
Sun, Y., Zhang, Z., Zheng, C. Q. & Sang, L. X. Mucosal lesions of the upper gastrointestinal tract in patients with ulcerative colitis: A review. World J. Gastroenterol. 27, 2963–2978. https://doi.org/10.3748/wjg.v27.i22.2963 (2021).
Kwon, J. et al. DSS-induced colitis is associated with adipose tissue dysfunction and disrupted hepatic lipid metabolism leading to hepatosteatosis and dyslipidemia in mice. Sci. Rep. 11, 5283. https://doi.org/10.1038/s41598-021-84761-1 (2021).
Jeon, H. et al. TDAG51 deficiency attenuates dextran sulfate sodium-induced colitis in mice. Sci. Rep. 12, 20619. https://doi.org/10.1038/s41598-022-24873-4 (2022).
Coelho, R. C. L. A., Hermsdorff, H. H. M. & Bressan, J. Anti-inflammatory properties of orange juice: Possible favorable molecular and metabolic effects. Plant Foods Hum. Nutr. 68, 1–10. https://doi.org/10.1007/s11130-013-0343-3 (2013).
Duary, R. K., Bhausaheb, M. A., Batish, V. K. & Grover, S. Anti-inflammatory and immunomodulatory efficacy of indigenous probiotic Lactobacillus plantarum Lp91 in colitis mouse model. Mol. Biol. Rep. 39, 4765–4775. https://doi.org/10.1007/s11033-011-1269-1 (2011).
Wang, Y., Guo, Y., Chen, H., Wei, H. & Wan, C. Potential of Lactobacillus plantarum ZDY2013 and Bifidobacterium bifidum WBIN03 in relieving colitis by gut microbiota, immune, and anti-oxidative stress. Can. J. Microbiol. 64, 327–337. https://doi.org/10.1139/cjm-2017-0716 (2018).
Groeger, D. et al. Bifidobacterium infantis 35624 modulates host inflammatory processes beyond the gut. Gut Microb. 4, 325–339. https://doi.org/10.4161/gmic.25487 (2013).
Mazidi, M., Rezaie, P., Ferns, G. A. & Vatanparast, H. Impact of probiotic administration on serum C-reactive protein concentrations: Systematic review and meta-analysis of randomized control trials. Nutrients 9, 20. https://doi.org/10.3390/nu9010020 (2017).
Volp, A. C. P. et al. Inflammation biomarkers capacity in predicting the metabolic syndrome. Arq. Bras. Endocrinol. Metab. 52(537–549), 2020. https://doi.org/10.1590/s0004-27302008000300015 (2008).
Human Microbiome Project Consortium. Structure, function and diversity of the healthy human microbiome. Nature 486, 207–214. https://doi.org/10.1038/nature11234 (2012).
Magne, F. et al. The firmicutes/bacteroidetes ratio: A relevant marker of gut dysbiosis in obese patients?. Nutrients 12, 1474. https://doi.org/10.3390/nu12051474 (2020).
Houtman, T. A. et al. Gut microbiota and BMI throughout childhood: The role of firmicutes, bacteroidetes, and short-chain fatty acid producers. Sci. Rep. 12, 3140. https://doi.org/10.1038/s41598-022-07176-6 (2022).
Monteros, M. J. M. et al. Probiotic lactobacilli as a promising strategy to ameliorate disorders associated with intestinal inflammation induced by a non-steroidal anti-inflammatory drug. Sci. Rep. 11, 571. https://doi.org/10.1038/s41598-020-80482-z (2021).
Walker, A. W. et al. High-throughput clone library analysis of the mucosa-associated microbiota reveals dysbiosis and differences between inflamed and non-inflamed regions of the intestine in inflammatory bowel disease. BMC Microbiol. 11, 7. https://doi.org/10.1186/1471-2180-11-7 (2011).
LoSasso, G. et al. Inflammatory bowel disease-associated changes in the gut: Focus on Kazan patients. Inflamm. Bowel Dis. 27, 418–433. https://doi.org/10.1093/ibd/izaa188 (2021).
Zawistowska-Rojek, A., Kośmider, A., Stępień, K. & Tyski, S. Adhesion and aggregation properties of Lactobacillaceae strains as protection ways against enteropathogenic bacteria. Arch. Microbiol. 204, 285. https://doi.org/10.1007/s00203-022-02889-8 (2022).
Davray, D., Deo, D. & Kulkarni, R. Plasmids encode niche-specific traits in Lactobacillaceae. Microb. Genom. 7, 000472. https://doi.org/10.1099/mgen.0.000472 (2021).
Jandhyala, S. M. et al. Role of the normal gut microbiota. World J. Gastroenterol. 21, 8787–8803. https://doi.org/10.3748/wjg.v21.i29.8787 (2015).
Pickard, J. M., Zeng, M. Y., Caruso, R. & Núñez, G. Gut microbiota: Role in pathogen colonization, immune responses, and inflammatory disease. Immunol. Rev. 279, 70–89. https://doi.org/10.1111/imr.12567 (2017).
Sharon, I. et al. Time series community genomics analysis reveals rapid shifts in bacterial species, strains, and phage during infant gut colonization. Genome Res. 23, 111–120. https://doi.org/10.1101/gr.142315.112 (2013).
Grimm, V., Radulovic, K. & Riedel, C. U. Colonization of C57BL/6 mice by a potential probiotic Bifidobacterium bifidum strain under germ-free and specific pathogen-free conditions and during experimental colitis. PLoS ONE 10, e0139935. https://doi.org/10.1371/journal.pone.0139935 (2015).
Hemme, D. et al. Lactobacillus murinus N. sp., a new species of the autochtoneous dominant flora of the digestive tract of rat and mouse. Ann. Microbiol. 131, 297–308 (1980).
Cousin, S. et al. Draft genome sequence of Lactobacillus hominis strain CRBIP 24179T, isolated from human intestine. Genome Announc. 1, e00662. https://doi.org/10.1128/genomeA.00662-13 (2013).
Wang, Q. et al. Lactobacillus helveticus R0052 alleviates liver injury by modulating gut microbiome and metabolome in d-galactosamine-treated rats. Appl. Microbiol. Biotechnol. 103, 9673–9686. https://doi.org/10.1007/s00253-019-10211-8 (2019).
Palumbo, V. D. et al. The long-term effects of probiotics in the therapy of ulcerative colitis: A clinical study. Med. Fac. Univ. Palacky Olomouc. Czech. Repub. 160, 372–377. https://doi.org/10.5507/bp.2016.044 (2016).
Kruis, W. et al. Maintaining remission of ulcerative colitis with the probiotic Escherichia coli Nissle 1917 is as effective as with standard mesalazine. Gut 53, 1617–1623. https://doi.org/10.1136/gut.2003.037747 (2004).
Kokešová, A. et al. Oral administration of probiotic bacteria (E. coli nissle, E. coli O83, Lactobacillus casei) influences the severity of dextran sodium sulfate-induced colitis in BALB/c mice. Folia Microbiol. 51, 478–484. https://doi.org/10.1007/BF02931595 (2006).
Ukena, S. N. et al. Probiotic Escherichia coli Nissle 1917 inhibits leaky gut by enhancing mucosal integrity. PLoS ONE 2, e1308. https://doi.org/10.1371/journal.pone.0001308 (2007).
Peterson, L. W. & Artis, D. Intestinal epithelial cells: Regulators of barrier function and immune homeostasis. Nat. Rev. Immunol. 14, 141–153. https://doi.org/10.1038/nri3608 (2014).
Acknowledgements
We would like to thank all the technical assistance (Gracielle Vieira Gonçalves) from the animal house of the University of Western Sao Paulo (Unoeste) and the facilities of the Department of Physical Education at Faculty of Science and Technology at Universidade Estadual Paulista “Júlio de Mesquita Filho/Presidente Prudente Campus.
Funding
This work was supported by the São Paulo Research Foundation—FAPESP (Grant Number 2018/14658–1 and 2020/12040-0) and UNOESTE (University of Western São Paulo) (Grant # 6884).
Author information
Authors and Affiliations
Contributions
K.C.O.V. (Conceptualization, Investigation; Methodology Formal analysis Roles/Writing—original draft), A.B.B.S. (Conceptualization Investigation; Methodology Roles/Writing—original draft), S.A.F. (Conceptualization Investigation; Methodology Roles/Writing—original draft), F.S.L. (Conceptualization, Formal analysis, Resources; Writing—review & editing), C.F. (Conceptualization Investigation; Methodology Roles/Writing—original draft) E. B. (Conceptualization, Formal analysis, Writing—review & editing), V.C.P. (Conceptualization, Methodology Formal analysis Writing—review & editing), W.R.N. (Conceptualization, Methodology Formal analysis Writing—review & editing), G.A.N. (Conceptualization, Formal analysis, Resources; Writing—review & editing), L.K.W. (Conceptualization, Investigation; Methodology, Formal analysis Supervision Funding acquisition, Project administration; Writing—review & editing). All authors contributed to and have approved the final manuscript).
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
de Oliveira Vieira, K.C., da Silva, A.B.B., Felício, S.A. et al. Orange juice containing Pediococcus acidilactici CE51 modulates the intestinal microbiota and reduces induced inflammation in a murine model of colitis. Sci Rep 13, 18513 (2023). https://doi.org/10.1038/s41598-023-45819-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-45819-4
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.