Abstract
Mucosal interleukin (IL)-17A–producing T cells contribute to protective antimicrobial responses and to epithelial barrier integrity; their role in celiac disease (CD) is debated. We analyzed the frequency and developmental dynamics of mucosal (intraepithelial lymphocytes (IEL)) and circulating (peripheral blood (PB)) IL-17A (T17) and/or interferon (IFN)-γ–producing (T1, T1/T17) T-cell populations in 86 pediatric controls and 116 age-matched CD patients upon phorbol myristate acetate/ionomycin or CD3/CD28 stimulation. T17 and T1/17 are physiologically present among IEL and PB populations, and their frequency is selectively and significantly reduced in CD IEL. The physiological age-dependent increase of Th17 IEL is also absent in CD, while IFN-γ–producing PB-T cells significantly accumulate with patient's age. Finally, the amplitude of IL-17A+ and IFN-γ+ T-cell pools are significantly correlated in different individuals; this relationship only applies to CD4+ T cells in controls, while it involves also the CD4− counterpart in CD patients. In conclusion, both size and dynamics of mucosa-associated and circulating IL-17A+ T-cell pools are finely regulated in human pediatric subjects, and severely disturbed in CD. The impaired IL-17A+ IEL-T pool may negatively impact on epithelial barrier efficiency, and contribute to CD mucosa damage; the disturbed dynamics of circulating IL-17A+ and IFN-γ+ T-cell pools may be involved in the extraintestinal autoimmune manifestations associated with CD.
Similar content being viewed by others
Introduction
The development and functional shaping of innate and adaptive components of gut-associated lymphoid tissue is completed postnatally, and depends on the close relationship with microflora and environmental agents;1, 2, 3, 4, 5 among its components, several phenotypically and functionally distinct T lymphocyte subsets abundantly home either in the lamina propria (LP), and in close proximity with the epithelial layer (intraepithelial lymphocytes (IEL)).
Human gut intraepithelial T lymphocytes (IEL-T) are mostly α/βTCR+ (T-cell receptor), although a significant fraction of γ/δTCR+ T cells is represented; in marked contrast with LP-T cells, the vast majority of IEL-T is CD8+, a proportion of which also expresses natural killer receptors.6, 7, 8, 9 Most IEL-T cells have an effector/memory phenotype (CD45R0+), and are capable of immediately participating in immune defenses. They contribute to mucosal barrier function, to epithelial homeostasis, and to the regulation of mucosal immune responses, through cytotoxic activity and cytokine production, as well as by cell–cell communication.9, 10, 11, 12, 13, 14, 15, 16
Cytokines of the interleukin (IL)-17 family have recently emerged as important players of mucosal immune responses and in the maintenance of epithelial barrier integrity;17, 18 they orchestrate the crosstalk between immune and tissue cells, induce strengthening of tight junctions, and production of antimicrobial proteins and chemokines by both epithelium and immune cells.19 IL-17A, the best-characterized member of the family, is produced by a specialized population of CD4+ T-helper cells (Th17), and by CD8+ (Tc17) and γ/δ TCR T cells, as well as by several populations of innate cells.20, 21, 22, 23, 24, 25 The existence of IL-17A/IFN-γ (interferon-γ) double-producer T-cell populations, as well as the occurrence of Th17-to-Th1 conversion during immune responses, testify that the genetic program of IL-17–producing T cells is tightly regulated, and bears a substantial plasticity at the same time.18, 20, 26, 27
In mouse, the development of mucosal Th17-cell population depends on specific commensal flora components.2, 3, 17, 18, 19 Although IL-17A–producing T cells are physiologically present in human gut LP23, 24 and peripheral blood,25, 26 no information is available regarding either the ability of IEL-T populations to produce IL-17A, or the dynamics of IL-17A–producing mucosal and circulating T-cell pools during human development.
IL-17 dysregulation has been associated with different autoimmune and chronic inflammatory diseases.17, 18, 19, 20 Celiac disease (CD) is triggered, in genetically predisposed individuals, by an improper immune response to gluten components.28, 29 Besides specific HLA class II alleles, several genes involved in immune regulation and epithelial barrier function constitute predisposing factors for CD;29, 30 moreover, environmental agents contribute to the triggering of immune-mediated tissue damage by modulating immune response, inflammation, and epithelial permeability.
Several phenotypic and functional alterations in the IEL-T compartment, ranging from dysregulated cytokine production, aberrant expression and function of natural killer receptors on IEL CD8+ T cells, and enhanced cytotoxic activity, have all been implicated in CD tissue damage.6, 7, 8, 11, 12, 14, 28, 29, 31, 32, 33, 34, 35, 36, 37, 38, 39 In addition, the association between CD and other immune-mediated disorders supports the existence of a systemic immune dysregulation.28, 29
A possible pathogenic role for IL-17A–producing T cells in CD has been proposed by recent evidence reporting the augmentation and the aberrant phenotype of LP Th17 in CD patients;40, 41 intriguingly, gliadin-specific CD4+ T-cell lines exhibit an impaired ability to produce IL-17A,42 leaving the involvement of IL-17A in CD still open to investigation.
We evaluated duodenal IEL and peripheral blood IL-17A–producing T-cell populations in a cohort of CD children and adolescents and age-matched controls, and analyzed the dynamics of IL-17A+ T cells with respect to both subjects’ age and IFN-γ–producing T-cell populations. The results provide novel evidence that these factors regulate the pool size of IL-17A–producing T cells during human development, and disclose multiple alterations occurring in CD.
Results
Analysis of the main mucosal lymphocyte subsets in CD patients and controls
We initially performed the phenotypic characterization of the major T-cell subsets in distal duodenum bioptic specimens of newly diagnosed pediatric CD patients and age-matched control subjects. Mononuclear cell populations of control children and adolescents mostly consisted of CD3+ T cells (Figure 1a), 10–20% of which were CD4+ (Figure 1b). The preponderant CD4− T-cell population was largely composed of CD8+ (80%), and double-negative CD4−CD8− (20%) T lymphocytes, as verified in a limited number of patients (Figure 2a); moreover, a consistent population of γ/δ TCR+ T cells was present (Figure 2b), which were either CD4−CD8− double negative, or CD8+ (Figure 2c). CD103 (αEβ7 integrin) was uniformly expressed on the almost totality of cells, in CD4−, CD8+, CD4−CD8− double negative, and γ/δ TCR+ subsets, and on a large fraction of CD4+ T cells (Figure 2d).
Altered intraepithelial lymphocytes composition in mucosal biopsies of pediatric celiac disease (CD) patients. Frequency of (a, c) CD3+ and CD3− lymphocyte subsets, and (b, d) of CD4+ and CD4− T-cell subsets, in duodenal biopsies (a, b) and peripheral blood (c, d) of newly diagnosed pediatric CD patients (gray symbols) and age-matched controls (C, white symbols). Bars show median and interquartile range. *P<0.05; **P<0.005; ***P<0.001.
Characterization of T-cell subsets in mucosal intraepithelial lymphocytes of pediatric celiac disease (CD) patients and control (C) children. Mononuclear cell suspensions, obtained from duodenal biopsies of newly diagnosed pediatric CD patients (gray symbols) and age-matched controls (white symbols), were stained to evaluate the frequency of (a) CD4+, CD4−, CD8+, DN (CD4−CD8−, double-negative), and DP (CD4+CD8+, double-positive) T cells, (b) of γ/δ T-cell receptor (TCR)+ T cells, and (c) of CD8+ γ/δ or DN γ/δ TCR+ T cells. The percentage of CD103+ cells in each subset is reported in (d). Bars show median and interquartile range. *P<0.05; **P<0.01, ***P<0.001.
The percentage of T lymphocytes was significantly increased in CD patients (Figure 1a); this increase was accompanied by a skewing, with a decrease of CD4+ T cells, and an augmentation of CD4− T cells (Figure 1b), the latter mostly accounted for by the increase of CD4−CD8− and γ/δ TCR+ T cells (Figure 2a–c). Additionally, natural killer cells, identified as CD3-CD56+, were significantly lower in CD mucosal samples (data not shown). CD103 was comparably expressed on most T-cell subsets of CD patients, and slightly increased on CD4−CD8− double-negative T cells (Figure 2d).
In summary, the phenotypic analysis indicates that the lymphocyte populations obtained solely by mechanical dissociation of biopsies mostly consisted of IEL, as previously reported by various authors.6, 7, 8, 9, 36, 37, 38, 39 Moreover, the higher CD4−/CD4+ ratio, and the augmented frequency of CD4−CD8− and of γ/δ TCR+ T cells, together with the lower frequency of natural killer cells, are all recognized alterations of IEL populations in CD.7, 34, 36, 37, 38, 39
No alteration in the frequency of the main peripheral blood (PB) T-cell subsets was observed in pediatric CD patients (Figure 1c,d).
Quantitation of IL-17A- and IFN-γ–producing IEL-T lymphocytes in duodenal biopsies and in the PB of pediatric CD patients and controls
Recently, the increased presence of IL-17A–producing CD4+ T (Th17) cells has been described in the LP of CD patients.40, 41 However, no information are available on the ability of IEL-T to produce IL-17A and whether this is altered in CD.
Results in Figure 3a show that a sizeable fraction of both CD4+ and CD4− IEL-T subsets physiologically produced IL-17A, upon a short-term stimulation with phorbol myristate acetate (PMA) and ionomycin, as assessed in pediatric control subjects (Figure 3aA,aB, respectively). Strikingly, both CD4+ and CD4− IEL-T-cell populations of newly diagnosed CD patients showed a significantly lower frequency of IL-17A–producing cells (Figure 3aA,aB, respectively).
Reduced frequency of interleukin (IL)-17A–producing intraepithelial T lymphocytes (IEL-T)-cell subsets in pediatric celiac disease (CD) patients. The frequency of (a) mucosa (IEL-T) and (b) peripheral blood (PB-T) IL-17A+ (A, B) and interferon (IFN)-γ+ (C, D) cells was evaluated in CD4+ (A, C), and in CD4− (B, D) T-cell subsets of CD patients (gray symbols) and age-matched controls (C, white symbols); cells were left unstimulated (−), or stimulated (+) with phorbol myristate acetate/ionomycin (P/I). Bars show median and interquartile range. *P<0.001; ***P<0.0001. (c) Representative fluorescence-activated cell sorting analysis of IL-17A and IFN-γ staining on IEL CD3+CD4+ and CD3+CD4− gated populations, as described in the Methods section, in a CD patient (bottom panels) and an age-matched control (upper panels). Empty line: isotype control mAb; shaded line: anti-cytokine mAb. Numbers in quadrants represent the percentage of cytokine-producing cells. FSC, forward scatter; SSC, side scatter.
Under the same experimental conditions, the frequency of IFN-γ–secreting CD4+ and CD4− T cells was not significantly altered in CD patients (Figure 3aC,aD, respectively). A representative fluorescence-activated cell sorting analysis of IL-17A and IFN-γ staining on IEL-T populations of a CD patient (bottom panels) and an age-matched control (upper panels) is reported in Figure 3c.
Results depicted in Supplementary Figure S1A online show that all the major subsets (CD4+, CD4−, CD8+, CD4−CD8−, and γ/δ TCR+) contributed to IL-17A–producing IEL-T-cell pool, in a proportion that roughly paralleled their respective abundance; moreover, the different contribution of CD4+ and CD4− subsets to IL-17A+ pool in CD samples vs. controls reflected their different representativity in the IEL-T populations (compare with Figure 1b).
Interestingly, almost all IL-17A+ cells expressed CD103, across all T subsets analyzed; this held true for both CD patients and controls, with the exception of slightly increased levels in IL-17A+ CD4−CD8− double-negative T cells (see Supplementary Figure S1B online); the enrichment of IL-17A–producing cells in the CD103+ fraction was particularly significant for CD4+ T cells, owing to the lower level of CD103 positivity of this subset (Figure 2d and Selby et al.6).
The frequency of T cells spontaneously producing IL-17A+ or IFN-γ+ in ex vivo–analyzed mucosal samples was negligible in both CD patients and controls (data not shown).
Interestingly, IL-17A–producing CD4+ and CD4− T cells (Figure 3bA,bB, respectively) were also present, albeit at a lower level, in the PB of pediatric control subjects. The percentage of IL-17A+ (Figure 3bA,bB) and IFN-γ+ (Figure 3bC,bD) CD4+ and CD4− T cells was comparable in CD patients and control children. IL-17A–producing cells of both CD patients and controls markedly expressed more CD161 receptor (see Supplementary Figure S2B online), as compared with the frequency of this marker in CD4+ and CD4− PB T-cell populations (see Supplementary Figure S2A online), in accordance with previous evidence in the literature;22, 24 a representative analysis of a CD patient and a control is reported in Supplementary Figure S2C online.
Collectively taken, these results show that Th17 and IL-17A–producing CD3+CD4− T cells are physiologically present in human duodenal mucosa and, with a lower frequency, in PB; our data indicate a selectively defective abundance of IL-17A–secreting cells in intraepithelial but not circulating T populations of CD patients.
Age-dependent dynamics of IL-17A and IFN-γ–producing T cells
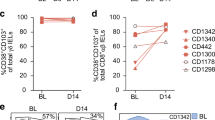
The presence and functionality of several mucosal lymphocyte populations depends on environmental signals and on commensal flora composition.1, 2, 3, 4, 5, 17, 18, 19 As shown in Figure 4, the frequency of IL-17A–producing CD4+, but not CD4−, IEL-T cells significantly augmented with age in controls, but not in CD patients (Figure 4aA,aB, respectively) of the same age distribution (Figure 4c); at variance, the frequency of IFN-γ–producing IEL-T cells was not significantly influenced by age in either group of patients (Figure 4aC,aD, respectively). A distinct pattern characterized the PB compartment: IL-17A–producing CD4+ and CD4− T cells significantly accumulated with age in both controls and CD patients (Figure 4bA,bB, respectively); moreover, an age-dependent increase of IFN-γ–producing CD4+ T cells comparably occurred in both groups of individuals (Figure 4bC), while the frequency of IFN-γ+ CD4− T cells augmented with age in CD patients but not in controls (Figure 4bD).
Dysregulated age-dependent dynamics of interleukin (IL)-17A- and interferon (IFN)-γ–producing T lymphocyte populations in pediatric celiac disease (CD) patients. (a, b) Scatter plots representing the frequency of mucosa (intraepithelial T lymphocytes (IEL-T, a), and peripheral blood (PB-T, b), IL-17A+ (A, B) or IFN-γ+ (C, D) cells with respect to age; the percentage of cytokine-producing cells was evaluated in phorbol myristate acetate/ionomycin-stimulated CD4+ (A, C) and CD4− (B, D) T subsets of CD patients (red symbols, lines, and text) and controls (black symbols, lines, and text). Lines in the plots represent the linear regression for any given pair of variables. Pearson r values are given, when P<0.05. (c) Age distribution of newly diagnosed pediatric CD patients (gray symbols) and age-matched controls (C; white symbols). Bars show median and interquartile range. *P<0.05; **P<0.005; ***P<0.0001. NS, not significant.
Collectively taken, these results first show that mucosal Th17 undergo a physiological expansion during the early life years, and suggest that this process is abrogated in CD patients; moreover, they indicate that the pool of circulating IL-17+ T cells also physiologically augments with age. Finally, although the abundance of IFN-γ–producing PB CD4− T cells was not altered in CD patients (Figure 3bD), this population pathologically accumulated with patient's age, thus underlying a deeper and systemic T-cell dysregulation in CD.
Evaluation of IL-17A/IFN-γ double-producing mucosal lymphocytes in pediatric CD patients and controls
Recent reports have described the existence of IL-17A/IFN-γ double-producer T-cell populations.17, 23, 26, 27 Here we show that IL-17A+IFN-γ+ cells were physiologically present in both CD4+ and CD4− IEL-T populations of control children, and significantly diminished in CD patients (Figure 5a,b); at variance, the frequency of IL-17A/IFN-γ T cells in PB was comparable between CD patients and age-matched controls (data not shown). A representative fluorescence-activated cell sorting analysis of IL-17A and IFN-γ staining on IEL-T populations of a CD patient and an age-matched control is reported in Figure 5c,d.
Decreased frequency of interleukin (IL)-17A/IFN-γ (interferon) double-producer intraepithelial T lymphocytes (IEL-T)-cell subsets in pediatric celiac disease (CD) patients. The percentage of IL-17A+IFN-γ+ cells was evaluated in (a) CD4+, and (b) CD4− T-cell subsets of CD patients (gray symbols) and age-matched controls (C, white symbols); cells were left unstimulated (−), or stimulated (+) with phorbol myristate acetate/ionomycin (P/I). Bars show median and interquartile range. *P<0.005; **P<0.0005; ***P<0.0001. Representative fluorescence-activated cell sorting analysis of IL-17A and IFN-γ staining on (c) CD3+CD4+ and (d) CD3+CD4− gated T-cell populations, in a CD patient (bottom panels) and an age-matched control (upper panels). Numbers in quadrants represent the percentage of double-producer cells.
Quantitative relationship between IL-17A+ and IFN-γ+ T-cell populations in mucosal and peripheral compartments in pediatric CD patients and age-matched controls
The development of IL-17A–producing T lymphocytes is controlled by signals that are partially distinct from those favouring the development of IFN-γ+ T cells.17, 18, 19, 20 We evaluated whether the amplitude of the populations producing the two cytokines were independently or coordinately regulated, either in the mucosa or in the PB of control children and pediatric CD patients.
The frequency of Th17 positively correlated with that of Th1, in both IEL and PB populations of control children and CD patients (Figure 6a,c, respectively); differently, the percentages of IL-17A+ and IFN-γ+ CD4− cells were independently regulated in controls, while showing a significantly positive correlation in CD patients, in both mucosal and PB compartments (Figure 6b,d, respectively).
Positive relationship between the frequency of interleukin (IL)-17A+ and that of interferon (IFN)-γ+ CD4− T cells in celiac disease (CD) patients. Scatter plots representing the frequency of IL-17A+ and IFN-γ+ cells in phorbol myristate acetate/ionomycin-stimulated (a, c) CD4+ and (b, d) CD4− cells of intraepithelial T lymphocytes (IEL-T; a, b) and peripheral blood T-cell (PB-T; c, d) populations, of CD patients (red symbols, lines, and text) and controls (black symbols, lines, and text). Lines in the plots represent the linear regression for any given pair of variables. Pearson r values are given, when P<0.05. *P<0.05; **P<0.01; ***P<0.0001.
These results show that the breadth of Th1 and Th17 pools are coordinately regulated in both IEL and PB compartments of different individuals. Moreover, they also suggest that a pathological correlation links the frequency of IL-17A+ cells with that of IFN-γ–producing ones, in mucosa and PB CD4− T lymphocytes of CD patients.
IL-17A and IFN-γ production by mucosal T lymphocytes, after anti-CD3/anti-CD28 stimulation
We then evaluated the presence of mucosal and circulating IL-17A–producing T cells in response to a more physiological stimulation, obtained by a combination of anti-CD3 and anti-CD28mAb. CD28 coreceptor is expressed on almost all PB and IEL CD4+ T cells; while almost half of PB CD4− T cells express CD28, only a small percentage of IEL CD4− T cells are CD28+ (i.e., <15%, our unpublished observations, and Eiras et al.34 and Russel et al.43), thus allowing the analysis of the IEL-CD4+ T subset only.
Anti-CD3/CD28mAb crosslinking induced IL-17A production in IEL-T cells (that were identified by means of CD5 pan-T surface marker,9, 34 to avoid interference with the anti-CD3mAb used in the stimulation; Figure 7a), albeit with a lower potency than PMA/ionomycin treatment (compare with Figure 3); IL-17A+ cells were enriched in the CD4+ (CD5+ CD4+) T-cell subset (Figure 7b). In these conditions, IEL from CD patients displayed a significantly reduced frequency of IL-17A+ (Figure 7a,b) and of double-producer IL-17A+IFN-γ+ T cells (data not shown), while the percentage of IFN-γ–producing T cells was comparable with controls (Figure 7c,d).
Defective frequency of interleukin (IL)-17A–producing intraepithelial T lymphocytes (IEL-T)-cell subsets in pediatric celiac disease (CD) patients, upon CD3/CD28 stimulation. The frequency of (a, b) IL-17A+ and (c, d) interferon (IFN)-γ+ cells was evaluated in (a, c) total (CD5+) T cells, and (b, d) CD4+ T-cell subset of CD patients (gray symbols) and age-matched controls (C, white symbols); cells were left unstimulated (−), or stimulated (+) with anti-CD3+anti-CD28mAb (3/28). Bars show median and interquartile range. *P<0.05; **P<0.01; ***P<0.005.
At variance, and similar to what was observed upon PMA/ionomycin stimulation, the percentages of PB IL-17A- or IFN-γ–producing CD4+ and CD4− T lymphocytes were comparable between CD patients and controls (Figure 8).
Frequency of circulating interleukin (IL)-17A–producing T-cell subsets in pediatric celiac disease (CD) patients and controls (C), upon CD3/CD28 stimulation. The frequency of peripheral blood IL-17A+ and interferon (IFN)-γ+ cells was evaluated (a, d) in total (CD5+) T cells, and (b, e) in CD4+ and (c, f) CD4− T-cell subsets of CD patients (gray symbols) and age-matched controls (white symbols); cells were left unstimulated (−), or stimulated (+) with anti-CD3+anti-CD28mAb (3/28). Bars show median and interquartile range. *P<0.05; ***P<0.0001.
Data in Figure 9 show that the frequency of Th17 positively correlated with that of Th1, in both mucosal and circulating populations of CD patients and controls (Figure 9a,b, respectively), upon anti-CD3 + anti-CD28mAb stimulation.
Positive relationship between the frequency of interleukin (IL)-17A+ and that of interferon (IFN)-γ+ CD4+ T cells in celiac disease (CD) patients and controls. Scatter plots representing the frequency of IL-17A+ and IFN-γ+ cells in anti-CD3/CD28-stimulated (a) intraepithelial lymphocytes (IEL) and (b) peripheral blood (PB) CD4+ T-cell populations of CD patients (red symbols, lines, and text) and controls (black symbols, lines, and text). Lines in the plots represent the linear regression for any given pair of variables. Pearson r values are given, when P<0.05. *P<0.05; **P<0.005; ***P=0.0005.
Taken altogether, these results show the physiological presence of IL-17A–producing T cells upon CD3/CD28 co-engagement, in both mucosa and PB; moreover, they suggest a functional defect of Th17 in CD IEL population in response to this more physiological stimulation. Finally, the coordinated regulation of Th1 and Th17 pools is also observed under these experimental conditions.
Discussion
In this study, we quantified the IL-17A–producing effector/memory T-cell (T17) pool in IEL and PB populations of pediatric subjects; we also analyzed the physiological age-dependent dynamics of T17 and T1 (IFN-γ+) cells in both compartments, and the relationship between the amplitude of the respective pools. A profound quantitative defect of mucosa, but not peripheral, T17 cells was discovered in pediatric CD patients; moreover, the equilibrium between IL-17A+ and IFN-γ+ T-cell pools, as well as their physiological age-dependent dynamics, were deeply disturbed in both IEL and circulating compartments of pediatric CD patients. Importantly, comparable results were obtained in response to stimulation either with PMA+ionomycin pharmacological agents, or by anti-CD3/CD28mAb crosslinking, under more physiological conditions.
IEL-T-cell populations participate with a decisive role to protective and pathological mucosal immune responses; these cells are primarily involved in maintaining the functionality and the homeostasis of the mucosal barrier, and, by converse, have a crucial role in the epithelial damage in CD.6, 7, 9, 10, 11, 12, 13, 14, 15, 16, 28, 29, 31, 32, 33, 34, 35
Our results show that IL-17A–producing IEL-T cells (identified by their characteristic phenotypic profile6, 7, 8, 9, 36, 37, 38, 39) are physiologically present in the duodenal mucosa of children and adolescent control subjects, thus suggesting an early development of this functional subset. IL-17A+ effector/memory lymphocytes homogeneously express CD103 marker and are found not only in the CD4+ (classical Th17), but also in the CD4− subset, where γ/δ TCR+, CD8+, and CD4−CD8− T cells all contribute to the production of IL-17A. Although the presence of Th17 in gut LP has been previously reported,23, 24, 40 our data represent novel evidence that IEL-T cells promptly produce a cytokine whose action on both epithelial and immune cells leads to recruitment of antimicrobial effector cells, production of anti-microbial peptides, and strengthening of tight junctions, thus playing a pivotal role in mucosal immune defense and homeostasis.17, 18, 19 Moreover, the physiological presence of polyfunctional (IL-17A+IFN-γ+) IEL-T cells was also evidenced, further supporting the notion of T-cell functional plasticity.17, 19, 26, 27 Finally, our results also confirm the abundant presence of antigen-experienced IFN-γ–producing CD4+ and CD4− IEL, as previously reported.10, 11, 12, 16
IL-17A+ and polyfunctional (IL-17A+IFN-γ+) effector/memory T-cell populations were also present, with an expected lower frequency, in the PB of pediatric subjects, thus suggesting that this effector/memory pool is established at an early phase during human development. In accordance with previous evidence in the literature,22, 24 PB IL-17A–producing T cells were enriched in the CD161+ fraction, comparably in CD patients and controls.
The frequency of IL-17A+, but not IFN-γ+, effector/memory mucosal and circulating T cells was found to increase according to children's age, in the control population. These data suggest that the IL-17A–producing pool of effector/memory T cells is exquisitely modulated during infancy and adolescence in humans, and are in accordance with the notion that the maturation of some components of the immune system is completed in the postnatal period.1, 2, 3, 4, 5 Our results also show that the frequency of Th17 and that of Th1 were significantly correlated, in both IEL and peripheral compartments of pediatric control subjects; at variance, the sizes of IL-17A+ and IFN-γ+ CD4− T-cell pools were independently regulated in different individuals. The coordinated regulation of distinct functional T-cell subsets may be the result of environmental stimuli and/or may underlie a positive crosstalk of immune regulatory circuits.17, 18, 19 Moreover, these observations suggest that the acquisition of the functional ability to produce IL-17A is differently regulated in CD4+ and CD4− T-cell subsets, within the same compartment.
In summary, our analysis on children and adolescent controls has elucidated some aspects of the physiological status of T1 and T17 major functional T-cell subsets during human development.
A two-tiered defect was found to selectively characterize IL-17A–producing IEL-T lymphocytes of pediatric CD patients: IL-17A+ as well as IL17A+IFN-γ+ polyfunctional T-cell pools were strongly reduced among both CD4+ and CD4− subsets, and the age-dependent accumulation of Th17 was also severely compromised. The frequency of IFN-γ–producing T cells did not significantly differ between CD patients and controls, arguing against the possibility that a generalized unresponsiveness may be at the basis of this phenomenon. The dysregulated functionality of the IEL compartment in CD patients was also underscored by the evidence that the frequency of IL-17A+ and that of IFN-γ+CD4− T cells were positively correlated in CD, but not in control, individuals.
The role of IL-17A in CD is still unclear. The presence of higher levels of IL-17A (evaluated as mRNA or protein) was reported in mucosal biopsies of CD patients;40, 44, 45 the contribution of non-T cells to IL-17A production, and the increased immune infiltrate may explain the difference with our data. This work represents a first assessment on the ability of intraepithelial T cells to produce IL-17A in CD; contrasting evidence have been reported on the ability of LP CD4+ T cells and gliadin-specific LP T-cell lines to produce IL-17A,40, 41, 42 thus leaving this issue open to further investigation. The impaired abundance of IL-17A–producing IEL-T populations may affect the homeostasis of the mucosal barrier and directly contribute to the augmented epithelial permeability, which constitutes a hallmark of CD;28, 29, 30, 31 moreover, the reduced frequency of both IL-17A+ and double-producer effector/memory T cells may negatively impact on the efficiency of antimicrobial immune responses, and indirectly concur to the worsening of inflammation in CD.17, 18, 19, 20
The mechanisms underlying the defective abundance of IL-17A+ IEL-T populations in CD are unknown. The development of T17 is controlled by microbial components, cytokines, and metabolites, and is exquisitely dependent on a network of interactions with other T-cell subsets (such as T1 and T reg), and other immune and tissue cells.1, 2, 3, 4, 5, 17, 18, 19, 20 All these factors are deeply dysregulated in the CD mucosa microenvironment;1, 11, 14, 28, 29, 30, 31, 32 moreover, alterations in the metabolic status of the gut microflora have been reported in CD.46
We could not find any significant relationship between the frequency of IL-17A+ T cells and CD clinical form (typical vs. atypical vs. silent), or histological grading (data not shown); interestingly, the frequency of IL-17A+ T cells in patients showing a positive serology and a histological grading of 0 or 1, and possibly representing an early stage of disease,28, 29, 47, 48 was not significantly different from that of those affected by the overt disease (data not shown), hinting at the possibility that the impairment of IL-17A+ T-cell pool represents an early event in CD.
The presence of circulating pathogenic T cells has been convincingly shown in CD.29 Although neither the percentage nor the age-dependent increase of PB IL-17A+ T lymphocytes were significantly affected, the pool of IFN-γ–producing CD4− T cells expanded with age (and possibly, with length of disease) in pediatric CD patients, but not in controls; moreover, in this cell population, the frequency of IL-17A–producing cells and that of IFN-γ+ ones were positively linked, thus mirroring what occurred in the mucosa compartment. Collectively taken, these observations underline that distinct and common modes of functional dysregulation characterize the IL-17A+CD4− T-cell subset in mucosal lesions and in the PB of CD patients; in fact, although this population is significantly decreased in IEL but not in PB lymphocytes, its frequency is nevertheless positively linked with that of IFN-γ+ cells in both compartments.
In summary, our work provides novel information on the amplitude and dynamics of IL-17A–producing T cells, and its relationship with IFN-γ–secreting subset, in human development. These results describe novel aspects of the alterations of immune system in CD; they may contribute to a better comprehension of the underlying pathogenetic mechanisms and be useful in the design of innovative therapeutic strategies. The multifaceted dysregulation of cytokine-producing T-cell populations at the systemic level may also be involved in the reported association between CD and other autoimmune and immune-mediated extraintestinal manifestations.28, 29, 47
Methods
Patients and controls. One hundred and sixteen newly-diagnosed children and adolescent CD subjects (age range: 0.5–18 years) and 86 age-matched controls (age range: 0.5–18 years) were consecutively enrolled in our study; all patients were referred to either the Celiac Disease and Malabsorptive Diseases Unit or the Gastroenterology and Liver Unit, Department of Pediatrics, Sapienza University, Rome, Italy.
Diagnosis of CD was assessed according to clinical, serological and histological criteria.47 Duodenal histology was graded according to Marsh classification.48 Positivity for anti-tTG IgA was assessed in all patients by enzyme-linked immunosorbent assay and/or radioimmunoassay.49
Control subjects were under investigation for upper gastrointestinal and/or systemic signs and symptoms (i.e., reflux disease, failure to thrive, dyspepsia, dysphagia, persistent vomiting, and abdominal pain) and were serologically and histologically negative. Helicobacter pylori infection was ruled out in all controls, except six, by the combined analysis of rapid urease-based method and histological examination on both antral and fundic stomach biopsies stained with Giemsa. None of the controls disclosed any inflammatory or abnormal aspect at duodenal biopsies that could be suggestive of other enteropathies (inflammatory bowel disease, autoimmune enteropathy, food allergies, non-steroidal anti-inflammatory drug-related enteropathy, and Giardia or Cryptosporidium infection).
All patients and controls were on a gluten-containing diet at diagnosis.
Demographic, clinical, serological, and histological features of CD patients and controls are reported in Table 1.
Two distal duodenum biopsies and a heparinized PB sample were taken during upper gastrointestinal endoscopy performed with a pediatric endoscope (Olympus GIF-E, or PQ20, Tokyo, Japan) and a video gastroscope (Olympus GIF180, or GIF P140), after conscious sedation with intravenous pethidine (1–2 mg kg−1) and midazolam (0.1 mg kg−1), or general anesthesia.
The study protocol was defined in accordance with the Declaration of Helsinki and approved by the institutional ethical committee. Written informed consent was obtained from children's parents; children >12 years of age signed a statement of assent.
Mononuclear cell isolation and stimulation. PB mononuclear cells were purified from heparinized blood samples by Ficoll-Hypaque (Eurobio, Les Ulis Cedex, France) density-gradient centrifugation.
Duodenal mucosa samples were put in physiological solution immediately upon biopsy; mononuclear cells were obtained by mechanical dissociation on a 70-μm cell strainer (BD Biosciences, San Jose, CA), and collected in physiological solution.
Mononuclear cells were resuspended in RPMI completed with 10% fetal calf serum and 1% glutamine (all from Euroclone, Milan, Italy), and left untreated or stimulated with 50 ng ml−1 PMA (Sigma-Aldrich, St Louis, MO) and 0.5 μg ml−1 ionomycin (Sigma-Aldrich). Alternatively, FcγR+ P815 mastocytoma cell line (3 × 105 cells) was incubated with anti-CD3 and anti-CD28 antibodies (0.5 μg each; anti-CD3 OKT3mAb clone was obtained from ATCC (Rockville, MD) and purified in our laboratory; anti-CD28mAb was from BD Biosciences) for 20 min, washed, and added to mononuclear cells in a 1:3 ratio.
All stimulations were carried out at 37 °C for 6 h, in the presence of the intracellular trafficking inhibitor brefeldin A (10 μg ml−1; Sigma-Aldrich), before intracellular staining and cytofluorimetric analysis.
Intracellular staining and multiparameter cytofluorimetric analysis. Mononuclear cells were washed with phosphate-buffered saline, fixed with 2% paraformaldehyde for 20 min, permeabilized with 0.5% saponin/1% fetal calf serum, and stained with anti-CD3 PerCP (or anti-CD5 PECy7, in samples stimulated with anti-CD3+anti-CD28 mAb), anti-CD4 FITC, IgG1 PE, and IgG1 APC isotopic controls, or anti-IFN-γ APC (all from BD Biosciences) and anti-IL-17A PE (e-Biosciences, San Diego, CA) mAb for 30 min at 4 °C.
Alternatively, mononuclear cells were stained with anti-CD3 PerCP Cy5.5, anti-CD4 PE Cy7, anti-CD8 APC H7, anti-TCR γ/δ APC, IgG1 FITC or CD103 FITC or CD161 FITC, for 30 min at 4 °C. Cells were washed with phosphate-buffered saline, fixed with 2% paraformaldehyde for 20 min and permeabilized with 0.5% saponin/1% fetal calf serum, before an additional staining with IgG1 PE or anti-IL-17A PE.
Cells were analyzed with a FACScalibur or FACSCANTO II (BD Biosciences), using CellQuest Pro (BD Biosciences) or FlowJo (Treestar, Ashland, OR) software. Lymphocyte region was defined on the basis of forward and side scatter physical parameters; T-cell subsets were identified by anti-CD3 (or anti-CD5),9, 34 and anti-CD4, anti-CD8 or anti-TCR γ/δ staining. The percentage of cytokine-producing cells in each T-cell subset was obtained by setting the lower limit on the basis of a matched isotype control mAb-stained sample, whose positivity never exceeded 0.5% of gated events. Cell viability in the populations analyzed was routinely >95% (not shown).
Statistical analysis. Differences between groups were analyzed with parametric (Student t-test) and non-parametric (Mann–Whitney and Wilcoxon) tests, as appropriate. Correlation analysis was performed using Pearson correlation test. Statistical analysis was performed with PRISM v.5 (GraphPad Software, San Diego, CA) and SPSS v.19 (Chicago, IL) softwares; P value <0.05 (two sided) was considered statistically significant.
References
Garrett, W.S., Gordon, J.I. & Glimcher, L.H. Homeostasis and inflammation in the intestine. Cell 140, 859–870 (2010).
Hooper, L.V. & Macpherson, A.J. Immune adaptations that maintain homeostasis with the intestinal microbiota. Nature Rev. Immunol. 10, 159–169 (2010).
Cerf-Bensussan, N. & Gaboriau-Routhiau, V. The immune system and the gut microbiota: friends or foes? Nat. Rev. Immunol. 10, 735–744 (2010).
Lee, Y.K. & Mazmanian, S.K. Has the microbiota played a critical role in the evolution of the adaptive immune system? Science 330, 1768–1773 (2010).
Eberl, G. & Lochner, M. The development of intestinal lymphoid tissues at the interface of self and microbiota. Mucosal Immunol. 2, 478–485 (2009).
Selby, W.S., Janossy, G., Bofill, M. & Jewell, D.P. Lymphocyte subpopulations in the human small intestine. The findings in normal mucosa and in the mucosa of patients with adult celiac disease. Clin. Exp. Immunol. 52, 219–228 (1983).
Brandtzaeg, P. et al. Immunobiology and immunopathology of human gut mucosa: humoral immunity and intraepithelial lymphocytes. Gastroenterology 97, 1562–1584 (1989).
Leon, F. Flow cytometry of intestinal intraepithelial lymphocytes in celiac disease. J. Immunol. Methods 363, 177–186 (2011).
Jarry, A., Cerf-Bensussan, N., Brousse, N., Selz, F. & Guy-Grand, D. Subsets of CD3+ (T cell receptor alpha/beta or gamma/delta) and CD3− lymphocytes isolated from normal human gut epithelium display phenotypical features different from their counterparts in peripheral blood. Eur. J. Immunol. 20, 1097–1103 (1990).
Sheridan, B.S. & Lefrançois, L. Intraepithelial lymphocytes: to serve and protect. Curr. Gastroenterol. Rep. 12, 513–521 (2010).
Jabri, B. & Ebert, E. Human CD8+ intraepithelial lymphocytes: a unique model to study the regulation of effector cytotoxic T lymphocytes in tissue. Immunol. Rev. 215, 202–214 (2007).
Meresse, B. & Cerf-Bensussan, N. Innate T cell responses in human gut. Semin. Immunol. 21, 121–129 (2009).
Shibahara, T. et al. Alteration of intestinal epithelial function by intraepithelial lymphocyte homing. J. Gastroenterol. 40, 878–886 (2005).
Bhagat, G. et al. Small intestinal CD8+TCRgammadelta+NKG2A+ intraepithelial lymphocytes have attributes of regulatory cells in patients with celiac disease. J. Clin. Invest. 118, 281–293 (2008).
León, F., Sánchez, L., Camarero, C. & Roy, G. Cytokine production by intestinal intraepithelial lymphocyte subsets in celiac disease. Dig. Dis. Sci. 50, 593–600 (2005).
Cheroutre, H., Lambolez, F. & Mucida, D. The light and dark sides of intestinal intraepithelial lymphocytes. Nat. Rev. Immunol. 11, 445–456 (2011).
Korn, T., Bettelli, E., Oukka, M. & Kuchroo, V.K. IL-17 and Th17 Cells. Annu. Rev. Immunol. 27, 485–517 (2009).
O'Connor, W. Jr, Zenewicz, L.A. & Flavell, R.A. The dual nature of T(H)17 cells: shifting the focus to function. Nat. Immunol. 11, 471–476 (2010).
Mucida, D. & Salek-Ardakani, S. Regulation of TH17 cells in the mucosal surfaces. J. Allergy Clin. Immunol. 123, 997–1003 (2009).
Cua, D.J. & Tato, C.M. Innate IL-17-producing cells: the sentinels of the immune system. Nat. Rev. Immunol. 10, 479–489 (2010).
Shrikant, P.A. et al. Regulating functional cell fates in CD8 T cells. Immunol. Res. 46, 12–22 (2010).
Maggi, L. et al. CD161 is a marker of all human IL-17-producing T-cell subsets and is induced by RORC. Eur J Immunol. 40, 2174–2181 (2010).
Annunziato, F. et al. Phenotypic and functional features of human Th17 cells. J. Exp. Med. 204, 1849–1861 (2007).
Kleinschek, M.A. et al. Circulating and gut-resident human Th17 cells express CD161 and promote intestinal inflammation. J. Exp. Med. 206, 525–534 (2009).
Kondo, T., Takata, H., Matsuki, F. & Takiguchi, M. Cutting edge: Phenotypic characterization and differentiation of human CD8+ T cells producing IL-17. J. Immunol. 182, 1794–1798 (2009).
Chen, Z. & O'Shea, J.J. Regulation of IL-17 production in human lymphocytes. Cytokine 41, 71–78 (2008).
Peck, A. & Mellins, E.D. Plasticity of T-cell phenotype and function: the T helper Type 17 example. Immunology 129, 147–153 (2010).
Di Sabatino, A. & Corazza, G.R. Coeliac disease. Lancet 373, 1480–1493 (2009).
Abadie, V., Sollid, L.M., Barreiro, L.B. & Jabri, B. Integration of genetic and immunological insights into a model of celiac disease pathogenesis. Annu. Rev. Immunol. 29, 493–525 (2011).
Fasano, A. Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer. Physiol. Rev. 91, 151–175 (2011).
Jabri, B. & Sollid, L.M. Tissue-mediated control of immunopathology in coeliac disease. Nat. Rev. Immunol. 9, 858–870 (2009).
Gianfrani, C., Auricchio, S. & Troncone, R. Adaptive and innate immune responses in celiac disease. Immunol. Lett. 99, 141–145 (2005).
Freedman, A.R., Macartney, J.C., Nelufer, J.M. & Ciclitira, P.J. Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease. J. Clin. Pathol. 40, 741–745 (1987).
Eiras, P., Roldán, E., Camarero, C., Olivares, F., Bootello, A. & Roy, G. Flow cytometry description of a novel CD3-/CD7+ intraepithelial lymphocyte subset in human duodenal biopsies: potential diagnostic value in coeliac disease. Cytometry 34, 95–102 (1998).
Meresse, B. et al. Reprogramming of CTLs into natural killer-like cells in celiac disease. J. Exp. Med. 203, 1343–1355 (2006).
Jenkins, D., Goodall, A. & Scott, B.B. T-lymphocyte populations in normal and coeliac small intestinal mucosa defined by monoclonal antibodies. Gut 27, 1330–1337 (1986).
Spencer, J., MacDonald, T.T., Diss, T.C., Walker-Smith, J.A., Ciclitira, P.J. & Isaacson, P.G. Changes in intraepithelial lymphocyte subpopulations in coeliac disease and enteropathy associated T cell lymphoma (malignant histiocytosis of the intestine). Gut 30, 339–346 (1989).
Spencer, J., Isaacson, P.G., Diss, T.C. & MacDonald, T.T. Expression of disulfide-linked and non-disulfide-linked forms of the T cell receptor gamma/delta heterodimer in human intestinal intraepithelial lymphocytes. Eur. J. Immunol. 19, 1335–1338 (1989).
Halstensen, T.S., Scott, H. & Brandtzaeg, P. Intraepithelial T cells of the TcR gamma/delta+ CD8− and V delta 1/J delta 1+ phenotypes are increased in coeliac disease. Scand. J. Immunol. 30, 665–672 (1989).
Monteleone, I. et al. Characterization of IL-17A producing cells in celiac disease mucosa. J. Immunol. 184, 2211–2218 (2010).
Fernández, S. et al. Characterization of gliadin-specific Th17 cells from the mucosa of celiac disease patients. Am. J. Gastroenterol. 106, 528–538 (2011).
Bodd, M. et al. HLA-DQ2-restricted gluten-reactive T cells produce IL-21 but not IL-17 or IL-22. Mucosal Immunol. 3, 594–601 (2010).
Russell, G.J. et al. p126 (CDw101): a costimulatory molecule preferentially expressed on mucosal T lymphocytes. J. Immunol. 157, 3366–3374 (1996).
Castellanos-Rubio, A., Santin, I., Irastorza, I., Castaño, L., Carlos Vitoria, J. & Ramon Bilbao, J. TH17 (and TH1) signatures of intestinal biopsies of CD patients in response to gliadin. Autoimmunity 42, 69–73 (2009).
Sapone, A. et al. Differential mucosal IL-17 expression in two gliadin-induced disorders: gluten sensitivity and the autoimmune enteropathy celiac disease. Int. Arch. Allergy Immunol. 152, 75–80 (2010).
Tjellström, B. et al. Gut microflora associated characteristics in children with celiac disease. Am. J. Gastroenterol. 100, 2784–2788 (2005).
Hill, ID. et al. Guideline for the diagnosis and treatment of celiac disease in children: recommendations of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. J. Pediatr. Gastroenterol. Nutr. 40, 1–19 (2005).
Marsh, M.N. Gluten, major histocompatibility complex, and the small intestine. A molecular and immunobiologic approach to the spectrum of gluten sensitivity (‘celiac sprue’). Gastroenterology 102, 330–354 (1992).
Li, M. et al. A report on the International Transglutaminase Autoantibody Workshop for Celiac Disease. Am. J. Gastroenterol. 104, 154–163 (2009).
Acknowledgements
Grant support: Sapienza University (“Progetti Coordinati di Ateneo Federato delle Scienze delle Politiche Pubbliche e Sanitarie (SPPS)”). We thank Dr Rossella Baldini for statistical advice, Dr Claudio Tiberti for anti-tTG RIA, Sofia Guida for anti-tTG ELISA, and all patients and their families who participated in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
SUPPLEMENTARY MATERIAL is linked to the online version of the paper
Rights and permissions
About this article
Cite this article
La Scaleia, R., Barba, M., Di Nardo, G. et al. Size and dynamics of mucosal and peripheral IL-17A+ T-cell pools in pediatric age, and their disturbance in celiac disease. Mucosal Immunol 5, 513–523 (2012). https://doi.org/10.1038/mi.2012.26
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2012.26