Abstract
HBV-specific cytotoxic T-lymphocyte (CTL) activity has a very important role in hepatitis B virus clearance. Present studies suggest that Tapasin, a endoplasmic reticulum (ER) chaperone, stabilizes the peptide-receptive MHC I conformation, allowing peptide exchange and increasing more peptides to be translocated into the ER. We have previously testified that cytoplasmic transduction peptide (CTP)-HBcAg18–27-Tapasin fusion protein could enter cytoplasm of dendritic cells, and enhance T cells’ response to generate specific CTLs efficiently in vitro. In the present study, we evaluated specific immune responses of CTP-HBcAg18–27-Tapasin fusion protein in HLA-A2 transgenic mice (H-2Kb) and anti-viral ability in HBV transgenic mice, and explored the mechanisms probably involved in. The studies showed that CTP-HBcAg18–27-Tapasin not only increased production of cytokine IFN-γ and interleukin-2 (IL-2), compared with CTP-HBcAg18–27, HBcAg18–27-Tapasin, and PBS, but also significantly induced the higher percentages of IFN-γ+CD8+ T cells and specific CTL responses in HLA-A2 transgenic mice. Moreover, enhancement of specific CTL activity induced by the fusion protein reduced HBV DNA and hepatitis B surface antigen (HBsAg) levels and decreased the expression of HBsAg and hepatitis B core antigen (HBcAg) in liver tissue of HBV transgenic mice. In addition, CTP-HBcAg18–27-Tapasin could upregulate the expression of JAK2, Tyk2, STAT1, and STAT4 in T lymphocytes in HLA-A2 transgenic mice splenocytes. However, there was no significant difference on the expressions of JAK1, JAK3, and STAT6 between each group. In conclusion, CTP-HBcAg18–27-Tapasin fusion protein could enhance not only the percentages of CTLs but also induce robust specific CTL activity and inhibits hepatitis B virus replication in vivo, which was associated with activation of the JAK/STAT signaling pathway.
Similar content being viewed by others
Main
Hepatitis B virus (HBV) infection remains a global problem, despite the effectiveness of the HBV vaccines in preventing infection. Although the factors that contribute to the clearance of the virus in acute self-limiting HBV infection or to the persistence of the virus in chronic HBV infection are not completely clear, increasing evidence suggests that host immune responses are an important factor in determining the outcome of HBV infection.1, 2 Acute individuals develop a strong, polyclonal, multispecific cytotoxic T-lymphocyte (CTL) response and a polyclonal T helper (Th) cell response to the virus typically, while these responses are markedly attenuated in chronically infected patients.3, 4 Persistent HBV infection is characterized by a weak adaptive immune response, thought to be due to inefficient CD4+ T-cell priming in the early stage of virus infection and subsequent development of a quantitatively and qualitatively ineffective CD8+ T-cell response. Studies of HBV infection in woodchucks and chimpanzees, as well as patients, are suggesting that multiple and frequent administration of the vaccine may be advisable in treatment of chronic hepatitis. Chronically infected individuals usually exhibit the immune tolerance to targeted antigens.5 In short, HBV-specific CTL activity has the key role in controlling the outcome of HBV infection because the magnitude of the T-cell response is a critical factor in determining viral control.6, 7, 8, 9
CD8+ T cells recognize antigenic peptides presented by MHC I molecules on the surface of APCs or target cells. Folding of MHC I molecules and loading with an appropriate peptide require the assistance of a number of chaperones present in the endoplasmic reticulum (ER), including protein disulfide isomerase, calnexin, calreticulin, ERp57, Tapasin, and the TAP, the latter four forming the peptide-loading complex (PLC).10, 11 Crystal structures of MHC I and molecular dynamic simulation studies suggest that Tapasin stabilizes the peptide-receptive MHC I conformation, allowing peptide exchange and increasing the probability of loading slow off-rate peptides. In the absence of Tapasin, MHC I molecules can be loaded with fast off-rate suboptimal peptides that can be lost before reaching the cell surface.12, 13 The low surface expression of MHC I molecules resulted in impaired positive and negative thymic T-cell selection, resulting in a reduction of CD8+ T-cell number in the thymus and periphery, and reduced antigen presentation to T cells, resulting in poor in vivo CTL response to influenza virus.14, 15
HBcAg18–27 epitope (HBcAg18–27) is a widely accepted as a CTL epitope to stimulate CTL response to hepatitis B core antigen (HBcAg).16, 17 However, HBV-specific CTL responses induced by exogenous antigens such as HBV-encoded antigens are usually weak, mainly because of the prohibition of intracellular delivery of antigens and peptides by the lipophilic nature and selective permeability of biological membranes.18 Cytoplasmic transduction peptide (CTP) was deliberately designed to ensure the efficient cytoplasmic delivery of the CTP-fused biomolecules. Thus, combining the specificity of HBcAg CTL epitope, the cell-penetrating property of CTP, and chaperone Tapasin may elicit robust specific HBV immune responses. We have previously testified that the expressed and purified recombinant CTP-HBcAg18–27-Tapasin fusion protein could enter the cytoplasm of dendritic cells, and enhance T cells’ response to generate specific CTLs efficiently in vitro.19 In the present study, we investigated whether the CTP-HBcAg18–27-Tapasin fusion protein was able to enhance HBV-specific CTL immune responses and anti-viral immunity in vivo.
MATERIALS AND METHODS
Reagents, Cells, and Fusion Proteins
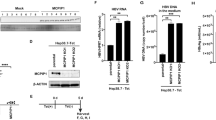
The fluorescent antibodies and isotype controls were purchased from eBioscience (USA), and ELISA kits for IFN-γ and interleukin-2 (IL-2) were purchased from R&D (USA). All antibodies were purchased from Abcam (UK). Hepatitis B surface antigen (HBsAg) was determined quantitatively using the IMX System (USA) according to the manufacturer’s instructions. The levels of HBV DNA were detected by real-time fluorescent quantitation PCR assay kits (PG Biotech, China). Phorbol 12-myristate 13-acetate (PMA), ionomycin, monensin, phytohemagglutinin (PHA), and concanavalin A (ConA) were obtained from Sigma (USA). Soluble fusion proteins CTP-HBcAg18–27-Tapasin, CTP-HBcAg18–27, and HBcAg18–27-Tapasin were purified and had undetectable endotoxin level according to our former experiments (Figures 1a and b).19 EL-4 cells (H-2Kb; from ATCC) were cultured in Dulbecco’s modified Eagle’s medium containing 10% FBS at 37 °C under a humidified condition of 5% CO2 and 100 U/ml penicillin.
Schematic diagram of fusion protein designed. (a) The schematic diagram of pREST-B-CTP-HBcAg18–27-Tapasin expression plasmid. (b) Schematic diagram of CTP-HBcAg18–27-Tapasin, HBcAg18–27-Tapasin, and CTP-HBcAg18–27 fusion proteins. The HBcAg18–27 gene and CTP and Tapasin sequences were inserted into the BamHI and EcoRI sites of pREST-B vector. The host Escherichia coli BL21 (DE3) cells were transformed with constructed vectors and the soluble fusion proteins were expressed in the supernatants. (c) The expression and purification of fusion proteins by sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE). Lane M: molecular weight standards; lanes 1, 4: expression and purification of GST-CTP-HBcAg18–27 recombinant protein, respectively; lanes 2, 5: expression and purification of His-HBcAg18–27-Tapasin recombinant protein, respectively: lanes 3, 6: expression and purification of His-CTP-HBcAg18–27-Tapasin recombinant protein, respectively. (d) Purified fusion proteins were analyzed by western blot using anti-GST or anti-Tapasin monoclonal antibody (mAb), respectively. The fusion proteins were cleaved by recombinant enterokinase to remove His-tag ultimately. Meanwhile, the control CTP-HBcAg18–27 protein was expressed and purified and separated from GST-tag using PreScission Protease. Lane 1: GST-CTP-HBcAg18–27; lane 2: HBcAg18–27-Tapasin; lane 3: CTP-HBcAg18–27-Tapasin (52.3 kDa). HBcAg, hepatitis B core antigen; CTP, cytoplasmic transduction peptide; GST, glutathione S-transferase.
HBV Transgenic Mice and Immunization
C57BL/6-HBV1.3 HBV transgenic mice, which contain 1.3 times over-length of the ayw subtype of the HBV genome, were obtained from the Key Liver Army Laboratory (The No. 458 Hospital, Guangzhou, China), were at 6–8 weeks of age, and were weighing between 20 and 23 g. The characterization of the mice has been described in detail previously,20, 21 and maintained in the experiment animal center of Shanghai No.6 Hospital under specific pathogen-free conditions. All experiments were approved by the laboratory animal ethical commission of Shanghai Jiao tong University. Mice were divided into six groups, with six mice in each group. Mice were immunized intramuscularly in the left tibialis anterior muscle three times at 1-week intervals with PBS, CTP-HBcAg18–27-Tapasin (50 μg, 100 μg), CTP-HBcAg18–27 (50 μg), HBcAg18–27-Tapasin (50 μg), and IFN-α (20 000 IU). Mice were killed, and serum samples, splenocytes, and livers were collected at day 7 after the third immunization.
HLA-A2 Transgenic Mice (H-2Kb) and Immunization
HLA-A2 transgenic mice (H-2Kb), 6–8 weeks old, which have the murine β2-microglobulin (β2m) and H-2Db genes knocked out, and are transgenic for a chimeric human HLA-A2.1 expressing the a1 and a2 domains of HLA-A2.1 and a mouse H-2Db-derived a3 domain to allow their interaction with mouse CD8,22 were purchased from Jackson Laboratory (USA) and maintained in the experiment animal center of Shanghai No. 6 Hospital under specific pathogen-free conditions. Mice were divided into four groups, with six mice in each group. Mice were immunized subcutaneously at the tail base one time at 1-week intervals with 20 μg CTP-HBcAg18–27-Tapasin, 20 μg CTP-HBcAg18–27, 20 μg HBcAg18–27-Tapasin, and PBS, respectively. Mice were killed, and splenocytes were collected at day 7 after the third immunization.
Measurement of IFN-γ Production by Intracellular Cytokine Staining to Splenocytes
To evaluate the percentages of IFN-γ-secreting cells at the individual cell level of HBV transgenic mouse splenocytes, single-cell suspensions from spleens were analyzed by flow cytometry. Splenocytes were stimulated in the presence of 10 μg/ml HBcAg for 6 h. After incubation for 3 h, 25 μg/ml of PMA, 1 μg/ml of ionomycin, and 1.7 μg/ml of monensin were added and incubation continued for another 3 h.23 After washing with PBS, cells were stained with saturating concentrations of PE-conjugated anti-CD8α McAb. After being fixed with Fix and Perm reagents A and B (BD Biosciences, USA), the cells were incubated for 20 min with FITC-labeled anti-IFN-γ McAb, followed by washing two times with PBS and analyzing by flow cytometry. Fluorescence analyses were performed on Coulter EPICS XL Flow Cytometer (Beckman) using the Expo32-ADC software.
Serological Analysis and Determination of Serum HBV DNA and HBsAg
Serum HBV DNA and HBsAg levels were determined after the second and third immunization by a quantitative polymerase chain reaction (PCR) and Abbott kits, respectively.24 Detection limit of the PCR was 1000 genomic copies per ml. The limit of detection for HBsAg was 0.28 ng/ml. We examined the inhibitory rate of HBV DNA and HBsAg induced by fusion protein. ALT and AST activities were measured by ARCHITECT Automatic Biochemistry Analyzer. The reference concentrations for serum HBV-DNA and HBsAg are copy/ml and ng/ml.
Histology and Immunohistochemistry of the Liver
Liver samples from the mice at day 7 after the third immunization were fixed in formaldehyde and embedded in paraffin. Deparaffinized 3–5-μm-thick sections were stained by hematoxylin–eosin (HE). For histological analysis, deparaffinized 3–5-μm-thick sections of the liver tissue were treated with 0.3% H2O2 in methanol for 10 min to eliminate the endogenous peroxidase activity, rinsed with distilled water, and immersed in PBS for 5 min. After the sections were blocked with normal goat serum for 30 min at room temperature, a goat anti-HBsAg polyclonal antibody and a goat anti-HBcAg polyclonal antibody (Novus Biologicals, USA) was applied overnight at 4 °C, and following three times of washing in PBS, sections were incubated for 30 min with biotinyated secondary antibody (Boster, China) at 37 °C and then for 30 min with streptavidin–biotin–peroxidase complex before being revealed by diaminobenzidine (DAB) and counterstained with hematoxylin.21
The Levels of Cytokine IFN-γ and IL-2
Splenocytes (2 × 106 cells/ml) harvested from immunized HLA-A2 transgenic mice were cultured in 24-well plates at 37 °C in the presence of 10 μg/ml HBcAg (CalBioreagents, USA). After 72 h incubation, culture supernatant concentrations of IFN-γ and IL-2 were determined using R&D.ELISA kits following the instructions provided by the manufacturer. The concentrations of cytokines in the samples were determined from the standard curves. Data are expressed as pg/ml.
Measurement of Interferon-γ Production by Intracellular Cytokine Staining
Cell staining and flow cytometry were performed with reagents according to the manufacturer’s protocols. The splenocytes from the HLA-A2 transgenic mice were stimulated in vitro for 6 h in cRPMI-1640 medium with 10 μg/ml HBcAg, PMA, ionomycin, and monensin at the concentrations described above. The cells were then harvested, and the intracellular cytokines were detected by flow cytometry as the mentioned above.
T-Lymphocyte Generation
Mixed lymphocytes were derived from splenocytes of HLA-A2 transgenic mice, which were treated using lymphocyte separation liquid (Beijing Combi Source Technology, China). T lymphocytes were derived from the above-mixed lymphocytes using nylon wool columns (Wako). Single-cell suspensions of lymphocytes (2 × 106 cells per well) were grown in six-well plates. The purity of the isolated T cells was determined by flow cytometry after staining with anti-CD3-PE-Cy5 (eBioscience, San Diego, CA, USA), and the samples purity >80% were used for this experiment.
CTL Assay and T-Lymphocyte Proliferation Activity Assay
T lymphocytes (5 × 106/ml) from HLA-A2 transgenic mice were used as effectors, and the EL-4 cells pulsed with 10 μg/ml HBcAg18–27 was used as target cells.25 EL-4 cells were seeded at a density of 5 × 104 cells per well in 96-well plates. Effector cells were incubated with EL-4 at different effector and target (E/T) ratios (5:1, 10:1 or 20:1) at 37 °C under 5% CO2 for 4 h. The specific CTL activity was measured using a CytoTox 96 Non-Radioactive Cytotoxicity Assay (Promega, Madison WI, USA) for lactate dehydrogenase (LDH) release according to the manufacturer’s instructions. The absorbance values of the supernatants were recorded at optical density 490 nm. Percent cytotoxicity was calculated as follows: ((experimental release−effector spontaneous release−target spontaneous release)/(target maximum release−target spontaneous release)) × 100%.19, 26
In this study, by using the ConA-induced T-lymphocyte proliferation, we assessed proliferation activity of T lymphocytes. Because ConA promotes cell mitogen, it mainly stimulates the effect on T lymphocytes. The above T lymphocytes (2 × 106 cells/ml) were cultured in 96-well culture plates in a final volume of 200 μl in the presence of 1 μg ConA solution at 37 °C under 5% CO2 for 48 h, and 20 μl Cell Counting Kit-8 solution (Beyotime Institute of Biotechnology, Haimen, China) was added to the plates at 37 °C under 5% CO2 for 4 h. The absorbance was finally read at 450 nm.
Enzyme-Linked Immunospot Assay
HBcAg18–27-specific CD8+ T cells were enumerated using enzyme-linked immunospot (ELISPOT).27 Splenocytes obtained from vaccinated transgenic mice (HBV transgenic mice and HLA-A2 transgenic mice), at 1 × 106 in a volume of 100 μl, were added to ImmunoSpot plates (Dakewe, China) precoated with anti-IFN-γ McAb (BD, USA). Then, the HBcAg18–27 peptide (10 μg/ml) was added to each well. A positive control (15 μg/ml, PHA) and a ‘no-peptide’ negative control were included in all assays. The plates were incubated overnight at 37 °C in a 5% humidity incubator. After incubation, the wells were washed two times with deionized water and three times with wash buffer (1 × PBS+0.05% Tween-20). The wells were then stained with saturating concentrations of biotin-conjugated anti-IFN-γ McAb (BD) at 37 °C for 1 h. After washing three times, streptavidin-alkaline phosphatase was added to each well, and the plates were incubated for 1 h at room temperature. The plates were again washed three times. Thirty microliters of activator solution (Dakewe, China) were added to develop spots. After 10 to 30 min, the plates were washed with distilled water to stop the reaction. Experiments were performed in triplicate. After being air dried, the number of spots in each well was counted using the Bioreader 4000 PRO-X (Biosys).
Analysis of Related Molecule mRNA Levels of JAK/STAT Pathway by Real-Time PCR
The above harvested T cells were collected for total RNA isolation according to the protocol for Trizol Reagent (Invitrogen, CA). cDNA was generated using PrimeScript 1st Strand cDNA Synthesis Kit (TaKaRa, Japan). Relative quantitative real-time PCR was performed using SYBR®Premix Ex TaqTM reagents (TaKaRa, Japan) on a LightCycler (Roche Diagnostic). Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as an internal reference. The PCR primers used were as follows: JAK1 forward, 5′-CAGATGCCCACCATTACC-3′ and reverse, 5′-CCCTCTTCACTCCCTTCC-3′; JAK2 forward, 5′-GGCAGCAGCAGAACCTAC-3′ and reverse, 5′-GTCTAACACCGCCATCCC-3′; JAK3 forward, 5′-CCCATCCGCTGAGTTCCT-3′ and reverse, 5′-GGCTGCTATCCGGGTCTT-3′; Tyk2 forward, 5′-TTCCGTAGCAACCGTCTC-3′ and reverse, 5′-CATCAAGCATCCTGTGGG-3′; STAT1 forward, 5′-CTATGAGCCCGACCCTAT-3′ and reverse, 5′-TTGAACTTCCGAAATCCT-3′; STAT4 forward, 5′-CCTGCTGTTGGTTGGTGT-3′ and reverse, 5′-CTTGAGGCTTTCCTGTGC-3′; STAT6 forward, 5′-TCCTGGTCACAGTTCAATAA-3′ and reverse, 5′-CGATCTCAGAGTCGCTAAA-3′; GAPDH forward, 5′-AGAAGGCTGGGGCTCATTTG-3′ and reverse, 5′-AGGGGCCATCCACAGTCTTC-3′.
Detection of Related Proteins Expression of JAK/STAT Pathway
The cells described above washed two times with 1 × PBS, gently dispersed into a single-cell suspension, and homogenized using RIPA lysis buffer (Beyotime Institute of Biotechnology, Jiangsu, China). Protein concentrations were determined using the Pierce BCA Protein Assay Reagent Kit (Rockford, IL, USA). Homogenates were diluted to the desired protein concentration with 2 × SDS-PAGE loading buffer (Invitrogen). Samples were boiled and loaded onto polyacrylamide mini gels (Invitrogen) for electrophoresis. Proteins from the gels were transferred to Immobilon-PVDF membranes (Millipore, Bedford, MA, USA) using a semidry apparatus (Bio-Rad, Hercules, CA, USA). A rabbit anti-JAK1, JAK2, JAK3, Tyk2, STAT1, STAT4, and STAT6 McAb was used as the primary antibody, and horseradish peroxidase-conjugated goat anti-rabbit immunoglobulin-G antibody was used as the secondary antibody.
Statistical Analysis
Data are expressed as the mean values±s.d. and were analyzed by the SPSS16.0 software. One-way ANOVA and post hoc least significant difference test were used to determine the statistical significance in comparison to control. P-values of ≤0.05 were considered significant.
RESULTS
Cellular Immunity Elicited by CTP-HBcAg18–27-Tapasin in HBV Transgenic Mice
We investigated whether CTP-HBcAg18–27-Tapasin fusion proteins were able to prime specific immune response in HBV transgenic mice. For this, the intracellular expression of IFN-γ in CD8+ T cells in HBV transgenic mice immunized with various fusion proteins was analyzed by flow cytometry. The results showed that 50 or 100 μg CTP-HBcAg18–27-Tapasin induced higher levels of IFN-γ+CD8+ T cells than IFN-α, CTP-HBcAg18–27, or HBcAg18–27-Tapasin vaccination, respectively (Figure 2). Thus, Tapasin fused with CTP-HBcAg18–27 could induce more efficiently T-cell immune response than CTP-HBcAg18–27 or HBcAg18–27-Tapasin in vivo.
Intracellular cytokine expression in splenocytes of hepatitis B virus (HBV) transgenic mice. The mice from each group were killed and splenocytes were isolated after last immunization, and then were restimulated in vitro. And, the whole-cell population was doubly stained with fluorescent material labeled using PE-CD8α and FITC-IFN-γ antibodies. The doubly stained cells were counted and analyzed by flow cytometry. Data are representative of at least three individual experiments per time point. The data are the means±s.d. from six mice per group (*P<0.05). FITC, fluorescein isothiocyanate; IFN, interferon; PE, phycoerythrin.
Liver sections were evaluated primarily in terms of inflammatory cell infiltration. There were few lymphocytes in the liver of mice immunized with PBS. However, the amounts of lymphocytes were increased significantly in the liver of mice treated with HBcAg18–27-Tapasin, CTP-HBcAg18–27, IFN-α, and CTP-HBcAg18–27-Tapasin. A larger number of lymphocyte infiltration appeared in the liver of mice immunized with CTP-HBcAg18–27-Tapasin (Figure 3a). Furthermore, the results suggested histological changes in the liver were related with the intracellular expression of IFN-γ in CD8+ T cells.
Histopathologic changes and immunohistological analysis of hepatitis B surface antigen (HBsAg) and hepatitis B core antigen (HBcAg) in hepatitis B virus (HBV) transgenic mice livers. (a) Liver sections were stained with hematoxylin and eosin, and examined by light microscopy. Some lymphocytes appeared in the liver of mice. Representative photographs are presented (original magnifications: × 400). (b and c) Liver sections were subjected to immunohistological analysis of HBsAg (b) and HBcAg (c). Representative photographs are presented (original magnifications: × 400).
HBsAg, HBV DNA, ALT, and AST in HBV Transgenic Mice Peripheral Blood and Histopathological Changes
Then, we evaluated the therapeutic effects of virus clreance of the above groups in HBV transgenic mice. Serum HBsAg and HBV DNA were monitored at day 7 after the second and third immunization. The inhibition rate of serum HBsAg or viral DNA in HBV transgenic mice of CTP-HBcAg18–27-Tapasin group was higher than CTP-HBcAg18–27 or HBcAg18–27-Tapasin or IFN-α (Figures 4a and b). Serum HBsAg level from the mice immunized with CTP-HBcAg18–27-Tapasin decreased markedly as compared with the mice immunized with CTP-HBcAg18–27, HBcAg18–27-Tapasin, or IFN-α (*P<0.05). The titer of HBV DNA in sera was significantly reduced from the mice immunized with CTP-HBcAg18–27-Tapasin compared with CTP-HBcAg18–27, HBcAg18–27-Tapasin, or IFN-α (*P<0.05). It was worth noting that 100 μg CTP-HBcAg18–27-Tapasin immunization decreased remarkably the level of HBsAg and HBV DNA in sera than that with 50 μg CTP-HBcAg18–27-Tapasin did (*P<0.05). Meanwhile, the AST and ALT in sera of mice treated with 100 μg CTP-HBcAg18–27-Tapasin was significantly higher than those in 50 μg CTP-HBcAg18–27-Tapasin group (*P<0.05) (Figures 4c and d).
The levels of hepatitis B surface antigen (HBsAg), hepatitis B virus (HBV) DNA, alanine aminotransferase (ALT) and aspartate aminotransferase (AST) in HBV transgenic mice. The data are the means±s.d. of six mice per group. The HBsAg (a) and HBV DNA (b) inhibitory rate in sera of mice treated with 100 μg CTP-HBcAg18–27-Tapasin was significantly higher than those in 50 μg CTP-HBcAg18–27-Tapasin group. Data represent the means±s.d. (–=6) (*P<0.05). Meanwhile, the AST (c) and ALT (d) in sera of mice treated with 100 μg CTP-HBcAg18–27-Tapasin was significantly higher than those in 50 μg CTP-HBcAg18–27-Tapasin group. Data represent the means±s.d. (n=6) (*P<0.05). CTP, cytoplasmic transduction peptide.
To further confirm the therapeutic effects of fusion proteins in transgenic mice, immunohistological analysis was performed in livers from the above various treatment groups. A large number HBsAg and HBcAg were detected (stained brownish yellow) in the cytoplasm of hepatocytes in mice treated with 1 × PBS. CTP-HBcAg18–27-Tapasin immunization reduced the HBsAg and HBcAg level in a dose-dependent manner, and HBsAg and HBcAg expression was very low with 100 μg CTP-HBcAg18–27-Tapasin treatment (Figures 3b and c).
CTP-HBcAg18–27-Tapasin Stimulates the Secretion of Cytokine IFN-γ and IL-2
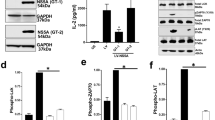
Splenocytes from immunized HLA-A2 transgenic mice were assayed for the secretion of the cytokines IFN-γ, IL-2 (Th1-like) upon restimulation with HBcAg. As shown in Figure 5, splenocytes from immunized animals with CTP-HBcAg18–27-Tapasin produced higher levels of IFN-γ (310.6±1.51 pg/ml) and IL-2 (506.42±5.79 pg/ml). However, there were no significant differences on the levels of IFN-γ and IL-2 between other groups (P>0.05).
Cytotoxic T-lymphocyte (CTL) assay and T-lymphocyte proliferation activity assay. (a) The doubly stained cells were counted and analyzed by flow cytometry. (b) Specific CTL activity was measured by lactate dehydrogenase (LDH) release assay. CTL activity is indicated as the mean percentage of specific lysis (means±s.d.) at different effector:target (E:T) ratios. (c) T-lymphocyte proliferation activity by using Cell Counting Kit-8. Data are representative of at least three independent experiments. The data are the means±s.d. from six mice per group (*P<0.05).
Strong Immune Responses Induced by CTP-HBcAg18–27-Tapasin in HLA-A2 Transgenic Mice
We measured the intracellular levels of IFN-γ in T cells by flow cytometry. The percentage of doubly stained positive cells was counted by flow cytometry after incubation. As shown in Figure 6a, significantly higher percentages of specific IFN-γ+CD8+ T cells were observed in mice immunized with CTP-HBcAg18–27-Tapasin than CTP-HBcAg18–27, HBcAg18–27-Tapasin, and 1 × PBS. Results demonstrated that delivery of Tapasin and HBcAg18–27 via CTP enhanced the generation of specific CTLs in HLA-A2 transgenic mice.
The levels of cytokine interferon-γ (IFN-γ) and interleukin-2 (IL-2). Secretion of IFN-γ and IL-2 in the HLA-A2 transgenic mice immunized with CTP-HBcAg18–27-Tapasin group is significantly higher than in the CTP-HBcAg18–27 or HBcAg18–27-Tapasin or PBS group (*P<0.05). Data are from at least three independent experiments. Data represent the means±s.d. (n=6). However, there is no statistical difference among other groups. HBcAg, hepatitis B core antigen; CTP, cytoplasmic transduction peptide.
To confirm the modulating role of CTP-HBcAg18–27-Tapasin fusion protein in cell-mediated immune responses, we further analyzed the ability of specific CTL. As shown in Figure 6b, the specific cytolysis percentages for CTP-HBcAg18–27-Tapasin immunized mice were 53.24±1.34%, 31.17±2.46%, and 18.54±3.54% for ratios of effector/target (E/T) of 20:1, 10:1, and 5:1, respectively. In contrast, specific cytolysis percentages were 23.09±2.76%, 21.06±3.77%, and 11.10 ±6.40%, respectively, in CTP-HBcAg18–27 groups for all effector/target (E/T) ratios. However, the CTL killing activity between HBcAg18–27-Tapasin and PBS had no significant difference. These results suggested that CTP-HBcAg18–27-Tapasin induced specific CTL activities, which was consistent with the high level of IFN-γ expressed in CD8+ T cells. Meanwhile, we further analyzed the ability of T-lymphocyte proliferation in different groups. CTP-HBcAg18–27-Tapasin enhanced significantly T-lymphocyte proliferation activity, which was higher than control groups (Figure 6c).
CTP-HBcAg18–27-Tapasin Boosted the Number of Specific CD8+ T Cells Elicited in vivo
HBcAg18–27-specific T cells were enumerated by measuring IFN-γ-producing cells by ELISPOT assay. As shown in Figure 7, a substantial number of T cells harvested from mice immunized with the CTP-HBcAg18–27-Tapasin responded by producing IFN-γ. The responses observed indicate that CTP-HBcAg18–27-Tapasin was found to generate stronger HBcAg18–27-specific T-cell responses by virtue of their ability to induce increased frequencies of IFN-γ-producing T cells compared with control group (**P<0.01). This result was consistent with the result of the intracellular expression of IFN-γ in CD8+ T cells analyzed by flow cytometry. Taken together, these results indicate that the CTP-HBcAg18–27-Tapasin fusion protein could induce HBcAg18–27-specific CTL responses in vivo.
Count of interferon-γ (IFN-γ) spots in cytotoxic T-lymphocyte (CTLs) detected by enzyme-linked immunospot (ELISPOT). (a) The number of IFN-γ spots from hepatitis B virus (HBV) transgenic mice. (b) The number of IFN-γ spots from HLA-A2 transgenic mice. CTP-HBcAg18–27-Tapasin was found to generate stronger HBcAg18–27-specific T-cell responses in vivo by virtue of their ability to induce increased frequencies of IFN-γ-producing T cells compared with control group. Data represent the means±s.d. (n=6) (**P<0.01). HBcAg, hepatitis B core antigen; CTP, cytoplasmic transduction peptide.
CTP-HBcAg18–27-Tapasin enhances JAK2, Tyk2, STAT1, and STAT4 Expression
To explore the involved mechanisms, we found CTP-HBcAg18–27-Tapasin had an effect on JAK/STAT signaling pathway. We further analyzed the JAK1, JAK2, JAK3, Tyk2, STAT4, STAT1, and STAT6 expression in different groups. The results revealed that expression of JAK 2, Tyk2, STAT1 and STAT4 was significantly upregulated in HLA-A2 transgenic mice immunized with CTP-HBcAg18–27-Tapasin group compared with CTP-HBcAg18–27, HBcAg18–27-Tapasin, and PBS group. However, the expressions of JAK1, JAK3, and STAT6 are no statistical difference in mice immunized with all of fusion proteins or PBS (P>0.05) (Figure 8).
Expressions of related molecules of Janus kinase/signal transducers and activators of transcription (JAK/STAT) pathway in HLA-A2 transgenic mice. (a) The expression of JAK1, JAK2, JAK3, Tyk2, STAT1, STAT4, and STAT6 mRNA. (b) The expression of the above protein. The expression of JAK2, Tyk2, STAT1 and STAT4 was significantly upregulated in HLA-A2 transgenic mice immunized with CTP-HBcAg18–27-Tapasin group compared with CTP-HBcAg18–27, HBcAg18–27-Tapasin, and phosphate-buffered saline (PBS) group. 1, CTP-HBcAg18–27-Tapasin; 2, CTP-HBcAg18–27; 3, HBcAg18–27-Tapasin; 4, PBS. Data represent the means±s.d. (n=6) (*P<0.05, **P<0.01). HBcAg, hepatitis B core antigen; CTP, cytoplasmic transduction peptide.
DISCUSSION
The development of novel immunotherapy has been highly anticipated because HBV infection is one of the leading causes of cirrhosis or hepatocellular carcinoma-related death. Several studies have demonstrated that the main cause of viral persistence during HBV infection is an inadequate anti-viral immune response to the viral antigens.28, 29 The viral-specific CD8+ T-cell response have an important role in the process of viral clearance. Patients with chronic hepatitis B (CHB) or therapeutic failure show deficient Th1 immunity associated with inefficient CD8+ T-cell cytotoxicity.30, 31 Therefore, induction of Th1 immunity and CTL responses specific to HBV represents a promising strategy to protect against HBV infection. CD8+ T cells recognize antigenic peptides presented by MHC I molecules on the surface of APCs or target cells. The presentation of mainly proteasomal degradation products on MHC I molecules at the cell surface is a way to carry information about the cellular proteome to CTLs.32, 33 Efficient antigen processing via MHC I relies on the PLC, consisting of the heterodimeric transporter associated with antigen processing (TAP) as centerpiece, which recruits the peptide-receptive MHC I heavy-chain/β2-microglobulin dimer by the adapter protein Tapasin. The type I membrane protein Tapasin fulfills various functions within the PLC. Its ER-lumenal domain binds to MHC I and its transmembrane domain to a specific interaction scaffold in TAP1 and TAP2, thereby connecting the peptide supplier TAP and the peptide acceptor MHC I.32, 34 Tapasin acts as peptide editor/facilitator, promoting the binding of immunodominant peptides.35 According to current models, peptide exchange is accelerated by Tapasin and low-affinity peptides dissociate faster.36, 37
The protein transduction domain (PTD) of HIV-1 TAT has been extensively documented with regard to its membrane transduction potential, as well as its efficient delivery of biomolecules in vivo. However, the majority of PTD and PTD-conjugated molecules translocates to the nucleus rather than to the cytoplasm after transduction, owing to the functional nuclear localization sequence (NLS).38, 39 A new approach that appears to be the safest is to produce recombinant proteins exogenously and then deliver them systemically or by localized injections into the target cells or tissues. In comparison with PTD, CTP and its fusion partners exhibited a clear preference for cytoplasmic localization, and also markedly enhanced membrane transduction potential.39, 40 By constructing recombinant protein and cell-penetrating peptide, different proteins and polypeptides were delivered into a variety of cells in vivo and in vitro.41, 42 HBcAg18–27 epitope has been shown to be able to induce HBV-specific CTL response and thus is a potential for the therapeutic design of chronic HBV infection.16, 17 In the present study, we expressed HBcAg18–27 included the complete amino-acid sequences that were fused with CTP and Tapasin. Meanwhile, our previous results showed that recombinant CTP-HBcAg18–27-Tapasin could penetrate into DCs cytoplasm.19 On the basis of this mechanism, we used CTP as a tool for the efficient delivery of Tapasin and antigen to APCs and to induce more HBV-specific CD8+ T cells.
HBV transgenic mice are immunologically tolerant to HBV-encoded antigens and represent a model of chronic HBV infection suitable to assess the anti-viral potential of immunotherapeutic strategies to break tolerance and terminate persistent HBV infection. Meanwhile, these mice do not develop chronic hepatitis because they are immunologically tolerant to viral antigens. Several studies have also illustrated that activated CTLs and secreted cytokines might effectively downregulate HBV gene expression and even control viral replication.43 At 1 week after the administration of the last treatment to HBV transgenic mice, the hepatocytes appeared swollen and there were lymphocyte infiltration and hyperemia in the liver tissue of mice from CTP-HBcAg18–27-Tapasin fusion protein group. In contrast, these histological changes were not apparent in the mice from other fusion protein groups, although there was also minimal lymphocyte infiltration in the mice from PBS and CTP-HBcAg18–27 and HBcAg18–27-Tapasin fusion protein groups. CTP-HBcAg18–27-Tapasin also enhanced the percentages of IFN-γ-producing CD8+ T cells in the spleen of HBV transgenic mice. The result indicated the inflammatory reaction in livers was consistent with specific CTL activity induced by CTP-HBcAg18–27-Tapasin. Furthermore, our results showed that the fusion peptide could decrease HBV DNA and HBsAg level in serum as well as HBsAg and HBcAg expression in liver tissue. This reduction was related closely with the dose of CTP-HBcAg18–27-Tapasin, which suggested that the parallel therapeutic effects were associated with the enhanced immune responses. To further confirm the specific CTL activity in livers, the levels of ALT and AST were measured by biochemical analysis and the results demonstrated that there was significant difference in the immunized HBV transgenic mice groups. Those levels in CTP-HBcAg18–27-Tapasin group was higher than those of others group.
We further investigated whether CTP-HBcAg18–27-Tapasin could elicit cell immune responses in HLA-A2 transgenic mice. The transgenic mice used in the experiments express heterodimeric HLA-A2.1/Kb molecules in the context of a background of H-2 class I molecules, and these transgenic mice were shown to have a relatively lower efficiency in CTL priming.20 However, our results suggested that CTP-HBcAg18–27-Tapasin increased the percentages of IFN-γ-producing CD8+ T cells in the spleen, enhanced the cytokine IFN-γ, IL-2 (Th1-like) secretion, and specific CTL activity. These indicated that the modification of Tapasin could enhance the presentation of target antigens via intracellular delivery to CD8+ T cells, and induce stronger cellular immune responses.
To further investigate CTP-HBcAg18–27-Tapasin can boost the HBcAg18-27-specific CD8+ T cells elicited in vivo, we tested it through the ELISPOT assay.27 The results showed that a substantial number of T cells harvested from mice immunized with the CTP-HBcAg18–27-Tapasin responded by producing IFN-γ. The responses observed indicate that CTP-HBcAg18–27-Tapasin was found to generate strong HBcAg18–27-specific T-cell responses by virtue of their ability to induce increased frequencies of IFN-γ-producing T cells compared with control group. This result was consistent with the result of the intracellular expression of IFN-γ in CD8+ T cells analyzed by flow cytometry. Taken together, these results indicate that the CTP-HBcAg18–27-Tapasin fusion protein could induce HBcAg18–27-specific CTL responses.
The above results indicated that HBcAg18–27 via CTP transduction could efficiently induce the cytokine IFN-γ, IL-2 (Th1-like) secretion, and our present experiments testified that CTP-HBcAg18–27-Tapasin fusion protein could enter the cytoplasm of dendritic cells and increase IL-12p70 production and then enhance cellular immune responses. Some studies have demonstrated that complete response to anti-viral treatment was correlated with predominant Th1 responses accompanied with enhanced CTL activity in CHB patients,29 implying that activation of Thl immunity might be important for the successful treatment of HBV.44, 45 Thus, activation of Thl immunity was required for CTL activity. There are several signaling that are required for Th1 cell differentiation.9 IFN-γ signaling activates STAT1 and reinforces the Th1 phenotype in a positive feedback loop.46, 47 IL-12 signaling induces STAT4, which positively regulates many aspects of the Th1 genetic program. STAT1 and STAT4 also contribute to the regulation of Tbx21 (the gene that encodes T-bet) expression.46, 47, 48, 49 Therefore, CTP-HBcAg18–27-Tapasin could increase IL-12p70 and IFN-γ production, which may mediate IL-12/STAT4 and IFN-γ/STAT1 signaling pathway. These are required for Th1 cell differentiation and mediated CTL activity indirectly. Therefore, we further analyzed the related molecules levels of JAK/STAT pathway in different groups. The expression of the related molecules mRNA levels was detected by RT-PCR and the proteins expression were detected by western blot analysis. The results revealed that the expression of JAK2, Tyk2, STAT1 and STAT4 was significantly upregulated in HLA-A2 transgenic mice immunized with CTP-HBcAg18–27-Tapasin group compared with CTP-HBcAg18–27, HBcAg18–27-Tapasin, and PBS group. However, the expressions of JAK1, JAK 3, and STAT6 are no statistical difference in mice immunized with all of fusion proteins or PBS. These results indicated that modification of Tapasin on intracellular antigen peptides via CTP transduction could mediate cytokines production and mediated CTL activity indirectly, which were associated with activation of the JAK/STAT signaling pathway.
The HBV transgenic mice we used express Kb- and Db-MHC class I molecules and HBcAg18–27 is an HLA-A0201-restricted epitope. However, studies showed that the HBcAg18–27 epitope can elicit responses and was able to be recognized by specific CTL when presented in the context of different HLA-A2 subtypes, although it is immunodominant in the context of HLA-A2.1, indicating that immunization with a peptide based on an HLA supertype epitope can lead to a CTL response in individuals expressing different HLA molecules belonging to the same HLA supertypes.21, 50, 51 In our study, our results showed that the fusion peptide CTP-HBcAg18–27-Tapasin could enhance the percentages of IFN-γ-producing CD8+ T cells, and decrease HBV DNA and HBsAg level in serum as well as HBsAg and HBcAg expression in liver tissue. These data further increase the potential coverage and efficacy of therapeutic vaccines based on the HBcAg18–27 sequence. Therefore, our results might suggest the more broad ability of HBcAg18–27 epitope, especially when fused with CTP and Tapasin, in the context of HLA restrictions.
In summary, our results demonstrate that vaccination with soluble CTP-HBcAg18–27-Tapasin fusion protein could induce robust strong immune responses in HLA-A2 transgenic mice and therapeutic effects in HBV transgenic mice, which were associated with activation of the JAK/STAT signaling pathway. Therefore, this may be a potential therapeutic strategy for eradicating virus in patients with chronic HBV infection.
References
Ganem D, Prince AM . Hepatitis B virus infection—natural history and clinical consequences. N Engl J Med 2004;350:1118–1129.
Williams R . Global challenges in liver disease. Hepatology 2006;44:521–526.
Phillips S, Chokshi S, Riva A et al. CD8+ T cell control of hepatitis B virus replication: direct comparison between cytolytic and noncytolytic functions. J Immunol 2010;184:287–295.
Chisari FV, Isogawa M, Wieland SF . Pathogenesis of hepatitis B virus infection. Pathol Biol (Paris) 2010;58:258–266.
Kosinska AD, Zhang E, Johrden L et al. Combination of DNA prime—adenovirus boost immunization with entecavir elicits sustained control of chronic hepatitis B in the woodchuck model. PLoS Pathogen 2013;9:e1003391.
Guidotti LG, Chisari FV . Immunobiology and pathogenesis of viral hepatitis. Annu Rev Pathol 2006;1:23–61.
Asabe S, Wieland SF, Chattopadhyay PK et al. The size of the viral inoculum contributes to the outcome of hepatitis B virus infection. J Virol 2009;83:9652–9662.
Brooks DG, Teyton L, Oldstone MB et al. Intrinsic functional dysregulation of CD4 T cells occurs rapidly following persistent viral infection. J Virol 2005;79:10514–10527.
Zhu J, Paul WE . Peripheral CD4+ T-cell differentiation regulated by networks of cytokines and transcription factors. Immunol Rev 2010;238:247–262.
Hammer GE, Kanaseki T, Shastri N . The final touches make perfect the peptide-MHC class I repertoire. Immunity 2007;26:397–406.
Purcell AW, Elliott T . Molecular machinations of the MHC-I peptide loading complex. Curr Opin Immunol 2008;20:75–81.
Thirdborough SM, Roddick JS, Radcliffe JN et al. Tapasin shapes immunodominance hierarchies according to the kinetic stability of peptide-MHC class I complexes. Eur J Immunol 2008;38:364–369.
Boulanger DS, Oliveira R, Ayers L et al. Absence of Tapasin alters immunodominance against a lymphocytic choriomeningitis virus polytope. J Immunol 2010;184:73–83.
Grandea AG 3rd, Golovina TN, Hamilton SE et al. Impaired assembly yet normal trafficking of MHC class I molecules in Tapasin mutant mice. Immunity 2000;13:213–222.
Garbi N, Tan P, Diehl AD et al. Impaired immune responses and altered peptide repertoire in Tapasin-deficient mice. Nat Immunol 2000;1:234–238.
Akbar SM, Chen S, Al-Mahtab M et al. Strong and multi-antigen specific immunity by hepatitis B core antigen (HBcAg)-based vaccines in a murine model of chronic hepatitis B: HBcAg is a candidate for a therapeutic vaccine against hepatitis B virus. Antiviral Res 2012;96:59–64.
Chen W, Shi M, Shi F et al. HBcAg-pulsed dendritic cell vaccine induces Th1 polarization and production of hepatitis B virus-specific cytotoxic T lymphocytes. Hepatol Res 2009;39:355–365.
Heathcote J, McHutchison J, Lee S et al. A pilot study of the CY-1899 T-cell vaccine in subjects chronically infected with hepatitis B virus. The CY1899 T Cell Vaccine Study Group. Hepatology 1999;30:531–536.
Chen X, Liu H, Tang Z et al. The modification of Tapasin enhances cytotoxic T lymphocyte activity of intracellular delivered CTL epitopes via cytoplasmic transduction peptide. ABBS 2013;45:203–212.
Guidotti LG, Matzke B, Schaller H et al. High-level hepatitis B virus replication in transgenic mice. J Virol 1995;69:6158–6169.
Wang S, Han Q, Zhang N et al. HBcAg18-27 epitope fused to HIV-Tat 49-57 adjuvanted with CpG ODN induces immunotherapeutic effects in transgenic mice. Immunol Lett 2010;127:143–149.
Pascolo S, Bervas N, Ure JM et al. HLA-A2.1-restricted education and cytolytic activity of CD8+ T lymphocytes from β2 microglobulin (β2 m) HLA-A2.1 monochain transgenic H-2Db β2 m double knockout mice. J Exp Med 1997;185:2043–2051.
Crawford TQ, Ndhlovu LC, Tan A et al. HIV-1 infection abrogates CD8+ T cell mitogen-activated protein kinase signaling responses. J Virol 2011;85:12343–12350.
Huang Y, Chen Z, Jia H et al. Induction of Tc1 response and enhanced cytotoxic T lymphocyte activity in mice by dendritic cells transduced with adenovirus expressing HBsAg. Clin Immunol 2006;119:280–290.
Tang XD, Wan Y, Chen L et al. H-2Kb-restricted CTL epitopes from mouse heparanase elicit an antitumor immune response in vivo. Cancer Res 2008;68:1529–1537.
Chen J, Yu Y, Chen X et al. Enhancement of CTLs induced by DCs loaded with ubiquitinated hepatitis B virus core antigen. World J Gastroenterology 2012;18:1319–1327.
Lycke NY, Coico R . Measurement of immunoglobulin synthesis using the ELISPOT assay. Curr Protoc Immunol 2001;17, (Chapter 7, Unit 7) 14.
Shimazaki K, Urabe M, Monahan J et al. Adeno-associated virus vector-mediated bcl-2 gene transfer into post-ischemic gerbil brain in vivo: prospects for gene therapy of ischemia-induced neuronal death. Gene Ther 2000;7:1244–1249.
Kordower JH, Emborg ME, Bloch J et al. Neurode-generation prevented by lentiviral vector delivery of GDNF in primate models of Parkinson’s disease. Science 2000;290:767–773.
Woltman AM, Op den Brouw ML, Biesta PJ et al. Hepatitis B virus lacks immune activating capacity, but hepatitis B virus lacks immune activating capacity, but actively inhibits plasmacytoid dendritic cell function. PLoS One 2011;6:e15324.
Tsai SL, Sheen IS, Chien RN et al. Activation of Th1 immunity is a common immune mechanism for the successful treatment of hepatitis B and C: tetramer assay and therapeutic implications. J Biomed Sci 2003;10:120–135.
Hulpke S, Baldauf C, Tampé R . Molecular architecture of the MHC I peptide-loading complex: one tapasin molecule is essential and sufficient for antigen processing. FASEB J 2012;26:5071–5080.
Neefjes J, Jongsma ML, Paul P et al. Towards a systems understanding of MHC class I and MHC class II antigen presentation. Nat Rev Immunol 2011;11:823–836.
Papadopoulos M, Momburg F . Multiple residues in the transmembrane helix and connecting peptide of mouse tapasin stabilize the transporter associated with the antigen-processing TAP2 subunit. J Biol Chem 2007;282:9401–9410.
Tey SK, Khanna R . Host immune system strikes back: Autophagy-mediated antigen presentation bypasses viral blockade of the classic MHC class I processing pathway. Autophagy 2012;8:1839–1841.
Chen M, Bouvier M . Analysis of interactions in a tapasin/class I complex provides a mechanism for peptide selection. EMBO J 2007;26:1681–1690.
Wearsch PA, Cresswell P . Selective loading of high-affinity peptides onto major histocompatibility complex class I molecules by the Tapasin-ERp57 heterodimer. Nat Immunol 2007;8:873–881.
Vazquez J, Sun C, Du J et al. Raizada transduction of a functional domain of the AT1 receptor in neurons by HIV-Tat PTD. Hypertension 2003;41:751–756.
Chauhan A, Tikoo A, Kapur AK et al. The taming of the cell penetrating domain of the HIV Tat: myths and realities. J Control Rel 2007;117:148–162.
Kim D, Jeon C, Kim JH et al. Cytoplasmic transduction peptide(CTP):new approach for the delivery of biomolecules into cytoplasm in vitro and in vivo. Exp Cell Res 2006;312:1277–1288.
Moron G, Dadaglio G, leclerc C . New tools for antigen delivery to the MHC class I pathway. Trends Immunol 2004;25:92–97.
Shibagaki N, Udey MC . Dendritic cells transduced with TAT protein transduction domain-containing tyrosinase-related protein 2 vaccinate against murine melanoma. Eur J Immunol 2003;33:850–860.
Roh S, Kim K . Overcoming tolerance in hepatitis B virus transgenic mice: a possible involvement of regulatory T cells. Microbiol Immunol 2003;47:453–460.
Boni C, Bertoletti A, Penna A et al. Lamivudine treatment can restore T cell responsiveness in chronic hepatitis B. J Clin Invest 1998;102:968–975.
Szkaradkiewicz A, Jopek A, Wysocki J et al. HBcAg-specific cytokine production by CD4 T lymphocytes of children with acute and chronic hepatitis B. Virus Res 2003;97:127–133.
Afkarian M, Sedy JR, Yang J et al. T-bet is a STAT1-induced regulator of IL-12R expression in naive CD4+ T cells. Nat Immunol 2002;3:549–557.
Lighvani AA, Frucht DM, Jankovic D et al. T-bet is rapidly induced by interferon-gamma in lymphoid and myeloid cells. Proc Natl Acad Sci USA 2001;98:15137–15142.
Schulz EG, Mariani L, Radbruch A et al. Sequential polarization and imprinting of type 1 T helper lymphocytes by interferon-gamma and interleukin-12. Immunity 2009;30:673–683.
Yang Y, Ochando JC, Bromberg JS et al. Identification of a distant T-bet enhancer responsive to IL-12/Stat4 and IFNgamma/Stat1 signals. Blood 2007;110:2494–2500.
Livingston BD, Crimi C, Fikes J et al. Immunization with the HBV core 18–27 epitope elicits CTL responses in humans expressing different HLA-A2 supertype molecules. Hum Immunol 1999;60:1013–1017.
Bertoletti A, Southwood S, Chesnut R et al. Molecular features of the hepatitis B virus nucleocapsid T-cell epitope 18-27: interaction with HLA and T-cell receptor. Hepatology 1997;26:1027–1034.
Acknowledgements
This study was supported by the grants from the National Natural Science Foundation of China (Nos. 31000414 and 81070335).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Hepatitis-B virus (HBV)-specific cytotoxic T lymphocyte (CTL) activity plays a key role in controlling the outcome of HBV infection. The authors proposed that combining the CTL-stimulatory ability of HBcAg18-27 with the cell-penetrating property of cytoplasmic transduction peptide (CTP) and the chaperone tapasin would elicit a robust and specific HBV immune response. The CTP-HBcAg18-27-Tapasin fusion protein induces an HBV-specific CTL immune response, causes liver inflammatory cell infiltration, and inhibits hepatitis B virus replication through activation of the JAK/STAT signaling pathway.
Rights and permissions
About this article
Cite this article
Chen, X., Tang, Y., Zhang, Y. et al. Tapasin modification on the intracellular epitope HBcAg18–27 enhances HBV-specific CTL immune response and inhibits hepatitis B virus replication in vivo. Lab Invest 94, 478–490 (2014). https://doi.org/10.1038/labinvest.2014.6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2014.6
Keywords
This article is cited by
-
The role of SOCS proteins in the development of virus- induced hepatocellular carcinoma
Virology Journal (2021)