Key Points
- Infants and children manifest congenital and developmental disorders of oral, pharyngeal, and esophageal motility, as well as many of the disorders seen in adults.
- The pediatric patient's lack of verbal abilities may challenge elicitation of symptoms from children.
- Key symptoms in young children may thus include subtle prolongation of feeds, delay in milestones of feeding abilities, impairment of normal weight gain, excessive drooling of saliva, increases of regurgitation beyond that expected physiologically, unexplained fussiness, or chronic/recurrent respiratory symptoms.
- "Silent" aspiration is a particularly insidious manifestation of these motor disorders in infants or neurologically abnormal older children.
- Diagnostic evaluation of the child often benefits from an actual observation of a feeding by a clinician trained in such observations.
- Diagnostic procedures used in children suspected of oral, pharyngeal, or esophageal motor disorders may include radiography (particularly esophagram or videofluoroscopic swallowing study), manometry, endoscopy of the esophagus or airway (including fiberoptic endoscopic evaluation of swallowing with sensory testing), scintigraphy, esophageal pH-metry or impedance, or central nervous system imaging.
- Available therapeutic interventions, often optimally choreographed by a multidisciplinary team, include a multitude of "conservative" measures, focused pharmacotherapies, and surgical interventions.
Definition and Background
This review addresses oral, pharyngeal, and esophageal motor disorders in infants (0–12 months of age) and children (1–12 years of age); during adolescence (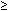 13 years of age), these motor disorders come to resemble those in adulthood, which are discussed in other articles. In contrast to the case for adults, congenital and developmental abnormalities play a prominent role in these disorders in children.
13 years of age), these motor disorders come to resemble those in adulthood, which are discussed in other articles. In contrast to the case for adults, congenital and developmental abnormalities play a prominent role in these disorders in children.
The newborn human infant requires the normal structure, function, and maturation of the oropharyngoesophageal organs in order to take in the nutrients needed for growth to adulthood. In addition, the pharyngeal intersection of the pathways for nutrient acquisition and respiration mandate that the airway protective structures and reflexes develop appropriately as the nutrient acquisition functions mature. Concurrent with the child's general neurologic development, the primitive reflexive infant suck and swallow are transformed into the mature, voluntary-reflexive, complex, integrated deglutitive functions of biting, chewing, bolus formation, and propulsion into the pharynx. Simultaneously, the airway protective reflexes also mature.1 The exquisite timing involved in the pharyngeal separation of these two functions by reflexive airway protections2, 3 is further challenged in infants by the rapidity of their respiratory rates. This physiologic tachypnea increases even further during the frequent respiratory infections children undergo in their first years of life4 or during lung disease associated with prematurity.5
The intricacies of these interactions in the proximal striated muscle and deglutitive organs are also impacted by behavior state, attention, and social learning6; by cognitive input from the developing cerebrum7; and by issues of timing and coordination modulated by sensory feedback.8 Congenital suprabulbar palsies, owing to anoxia or ischemia from congenital vascular anomalies or to abnormalities of neuronal migration, can cause dysphagia in association with dysarthria and drooling, and these disabilities may coexist with other suprabulbar abnormalities: epilepsy, learning disabilities, and delayed motor, cognitive, and language development.9
The reflexive nature of many of these deglutitive functions can be disturbed by impairments appearing anywhere in the controlling neural reflex arcs of a neonate. The anatomic source for some of these impairments may be beneath the resolution of available imaging methods but can only be surmised by clinical examination, as has been described for watershed infarcts in fetal and neonatal brainstem, clinically expressed as cranial neuropathies of nerves III to XII, producing abnormalities including dysphagia and aspiration.10
Infancy is the time during which congenital abnormalities of these organs or effects of in utero11 or neonatal exposures12 usually become evident. In addition, failure of appropriate maturation of functions and reflexes, owing to various etiologies, manifests in childhood. Finally, many disorders of these organs that occur in adulthood also occur in childhood, but may have different epidemiology, manifestations, or optimal management in these younger patients.
Disorders of the smooth muscle esophagus in children vary from those in adults to a lesser degree than the deglutitive disorders; these pediatric lower esophageal disorders are also discussed here.
This review discusses the general clinical features of pediatric disorders of these organs, the range of typical symptoms and physical findings in children, laboratory diagnostic evaluations useful in young patients with these disorders, general differential diagnostic considerations, and the variety of available therapies. This review also discusses specific pediatric oropharyngoesophageal disorders, detailing for each, where applicable, the epidemiology, pathophysiology, specific features of presenting symptoms and physical findings, optimal diagnostic evaluation, differential diagnosis, treatment approaches, clinical course, potential complications, and outcome.
Clinical Features
Dysphagia, or difficulty swallowing, is the chief manifestation of oropharyngoesophageal dysmotility in children, as in adults. The presentations are complicated in young children, as they may be in adults with severe neurologic disease, by their inability to report symptoms verbally, so that second-hand reports of signs of disease must suffice to bring attention to these disorders. Thus, pediatric dysphagia manifests as signs of feeding problems or respiratory problems, the latter due to misdirected swallowing.
It has been estimated that as many as 25% of all children may manifest some type of nonspecified feeding difficulty.13 Although only some of these feeding difficulties are because of dysphagia per se, the clinician must maintain dysphagia in the differential diagnosis of such symptoms.
The cause of dysphagia may be organic or behavioral; if organic, it may be because of disordered anatomy or function; if it is because of disordered function, the dysfunction may have roots in neurosensory, neuromotor, or central processing functions.
Although these opposing concepts are useful for considering the primary causes of disease, often etiologies are mixed or interactions occur among primary and secondary etiologies. Because these multiple etiologies interact to promote disability, all of them should be considered for optimal management.14, 15, 16 In fact, a recent study of 700 children with feeding problems found multiple etiologic contributing factors in nearly 50%.14 For example, an infant with cricopharyngeal achalasia may develop nasal regurgitation and subsequent obstructive nasal inflammation, making feeding more challenging to the parent and causing early fatigue in the child, so that nasal inflammation and parent and child behavioral aspects would play contributory roles in ongoing disability.
Another problem particular to young children is that a swallowing impairment owing to other causes (congenital anatomic anomalies of the swallowing organs, or general medical disease17) may interrupt the normal development of swallowing during critical stages, making subsequent behavioral rehabilitation of feeding aversion a critical part of the management.18, 19
This review focuses on the organic causes of dysphagia, and particularly on disordered motor function (i.e., on dysmotility rather than on structural causes of dysphagia), but it considers the alternative causes while dealing with differential diagnoses.
History and Symptoms
History
Feeding History
A complete feeding history includes information on the duration and progression of the symptoms19 and many other aspects of the feeding experience for the young child (Table 1). The temporal relationship of the symptoms to the act of swallowing may shed light on the location of the abnormality: pre-swallow gagging or choking may indicate oral disabilities; swallow-associated gagging points to location in the pharynx; and symptoms immediately post-swallow suggest disability in or below the upper esophageal sphincter. The associated nutritional history for a child, in contrast to the usual practice in adults, requires plotting of height and weight, and possibly weight-for-height and head circumference, in relationship to age.
Site of Disability
The clinician can approach the question of the site of the disability by determining whether it is localized in the striated muscles of the oropharynx and upper esophagus, or manifest by difficulties with drooling, initiation of swallow, tongue thrusting, nasopharyngeal regurgitation, or signs of aspiration. Disability limited to the smooth muscle of the mid- or lower esophagus is more likely to cause isolated sensation of food impaction, chest pain, or odynophagia, but may cause respiratory symptoms as well. The verbal limitations of young children may obscure this distinction, however.
General Medical History
A general medical history is crucial. It may disclose, for example, predispositions to secondary esophageal motor disorders (e.g., esophageal atresia, collagen vascular disorders, caustic ingestions, sclerotherapy, allergic esophageal dysmotility); suggestions of more diffuse gut motility (e.g., slowed stooling in early botulism); a travel history permitting exposure (e.g., to Chagas' disease); trauma to the head and neck (including the iatrogenic "trauma" of tracheotomy); potentially pertinent medications (e.g., benzodiazepines such as nitrazepam); and so forth.
Symptoms of Dysphagia
Symptom Clusters and Questionnaires
Questionnaires increasingly are used to gather symptom data for disorders characterized by clusters of symptoms. Ideally, such questionnaires have been tested for reliability (test-retest, interobserver, intraobserver, and accuracy) and for diagnostic and evaluative validity. Such a self-report symptom inventory has been developed and validated for use in adults with oropharyngeal dysphagia.20 A survey aimed at dysphagic children with cerebral palsy and tested in 117 such children contains several subscores.21 The Feeding Difficulty Symptom Score (FDSS) describes the severity of swallowing symptoms, and a numerical Dysphagia Complexity Index (DCI) quantifies the neurologic complexity of the swallowing difficulty; the two scores correlate closely. Lack of reported neonatal suckling problems did not predict lower severity of present problems, but term infants with cerebral palsy exhibited swallowing problems that were more complex and were more likely to be classified as athetoid than those who had been born preterm.
In addition to such simple symptom questionnaires, a recent protocol for oropharyngeal dysphagia screening not only incorporates medical history, behavioral, and gross motor variables, but also uses observations during diagnostic testing including oromotor testing and trial swallows.22 This 28-item screening protocol was able to classify patients correctly, with defined sensitivity and specificity, as having or not having aspiration 71% of the time, an oral stage disorder 69% of the time, a pharyngeal delay 72% of the time, and a pharyngeal stage swallowing problem 70% of the time. Although adolescent symptoms may be similar to those validated in adults, children are somewhat more challenging to evaluate in this way, because of all of the complexities of pediatric diagnosis discussed above.
Prolonged Feeds/Anorexia/Food Refusal
Children who refuse feedings despite not having consumed adequate calories may be suffering from oropharyngoesophageal motor disorders. In these situations, the dysmotility causes refusal to eat owing to physical incapacity to eat, to discomfort, or to the threat of respiratory compromise. In 14 children younger than 6 years of age with chronic tube-feeding–dependent food refusal, manometry diagnosed two as having diffuse esophageal spasm and one as having nonspecific esophageal motility disorder.18 One must distinguish upper digestive dysmotility from other causes of feeding refusal, including pain from psychodynamic (e.g., anorexia nervosa23) or esophageal inflammatory (e.g., reflux or eosinophilic esophagitis) sources.
Poor Weight Gain/Malnutrition/Failure to Thrive
Inadequate weight gain may accompany chronic obvious feeding refusal, or it may be the first sign of subtler instances of long-term esophageal dysmotility. In some instances, dysmotility causes inadequate energy intake simply due to extreme prolongation of feeding time rather than actual refusal of feeds. Malnutrition caused by dysmotility may negatively affect the immune system, which can worsen any associated aspiration pneumonias and cause vicious cycles of increasing debility.
Drooling
Drooling, sialorrhea, the unintentional loss of saliva and other oral contents from the mouth, is generally a sign of oral dysmotility involving striated musculature, and often occurs in the context of more general neurologic disability.24 Drooling does not itself impact nutrition or airway protection, but may be complicated clinically by maceration of the skin of face and neck, and wet and malodorous clothing.
A study examining the source for drooling compared 14 drooling children with spastic cerebral palsy (7 to 18 years old) to 14 similar children without drooling and to 14 normal controls. Both cerebral palsy groups demonstrated nonsignificant tendencies to swallow less frequently and actually to produce less saliva. There was no correlation between the amount of saliva produced and the amount drooled. Drooling did correspond to greater dysarthria severity, greater intellectual disability, and lower nonverbal intelligence, but not to gross motor function, on validated scales.25
A summary of management of 78 neurologically impaired children with drooling described interventions ranging from oral-motor skills training through palatal training appliances through surgery (diversion of salivary flow26); medication for drooling (generally anticholinergic27) was used by only 8%.28
Tongue Thrust
Tongue thrusting during swallowing is an abnormal oral motor pattern that may contribute to abnormalities of deglutition, speech, and orofacial development.29, 30, 31 Tongue thrust occurs in many children with obvious neurologic deficits, but may also occur in children who otherwise appear neurologically normal. A potential explanation for such tongue thrust has been described: watershed infarcts in brainstem vascular structures early during intrauterine development may be clinically expressed as various cranial neuropathies, which may embrace those affecting oral motor functions, including those of the tongue.10 Though clinically evident, such neuropathies are often beneath the resolution of current imaging modalities. Depending on their location and extent, such watershed infarcts have caused apnea, dysphagia, aspiration, or syndromes with orofacial abnormalities.
Dysphagia
Dysphagia (difficulty swallowing) may be a specific complaint in the older child, but in the less verbal child (either younger or developmentally delayed) it may be represented by refusal by a hungry child of offered nutrients, by regurgitation of undigested ingested food, or even by drooling in a child unable to handle oral secretions appropriately. In young or developmentally delayed nonverbal children, slow eating or repeated swallowing may be the only visible manifestation of dysphagia, whereas the teenager, like the adult, may describe the sensation, for example, of food getting stuck mid-chest. Whether dysphagia occurs with solids or liquids is important; solid dysphagia precedes liquid dysphagia in disorders that anatomically narrow the esophagus, whereas liquid dysphagia is an early manifestation of disorders of motility.
Vomiting/Regurgitation
When esophageal dysmotility prevents the appropriate caudal movement of ingested material, the material's retrograde movement may result in regurgitation. Although this is often termed "vomiting," the retrograde duodenogastric peristalsis that accompanies true vomiting is usually absent, and the esophageal contents that are ejected are undigested and nonacid.
Chest Pain, Odynophagia
Chest pain may be a sign of esophageal dysmotility, but inflammatory conditions are important in the differential diagnosis of chest pain or odynophagia. No multicenter pediatric series yet exists comparable to the adult series based on motility studies in the national Clinical Outcomes Research Initiative (CORI) database, which found that among 140 adults with isolated noncardiac chest pain who underwent esophageal motility studies, 70% had a normal motility study.32 Among those with dysmotility, hypotensive lower esophageal sphincter was the most common finding (61%), with nutcracker esophagus and nonspecific esophageal motility disorders diagnosed in 10% each. Of the 44 additional adults who had dysphagia as well as chest pain, at least 60% had dysmotility: 35% with achalasia and 25% with nonspecific esophageal motility disorder. A pediatric series of 83 children with chest pain from one center similarly found esophageal dysmotility in 25% (16% with normal endoscopy, 9% with esophagitis) and normal motility studies in 75% (57% with normal endoscopy, 18% with esophagitis). Of the chest pain patients with dysmotility, 33% had diffuse esophageal spasm, 30% had aperistalsis or hypotensive lower esophageal sphincter, 20% had hypertonic lower esophageal sphincter or nutcracker esophagus, and 19% had achalasia.33 Because of the prevalence of esophagitis in patients with chest pain or odynophagia, endoscopy generally should be performed as the primary investigation, with manometric evaluation reserved for those without esophagitis, or who do not respond adequately to therapy for any esophagitis found.
In the young or neurologically impaired nonverbal child, intractable crying may be the only sign of chest pain, but the differential diagnosis of this symptom is huge, with gastroesophageal reflux disease a prominent consideration.35, 36, 37
Impactions (Bolus Impactions)
Severe esophageal dysmotility may cause acute bolus impaction of ingested food. Esophagitis, particularly eosinophilic esophagitis, also causes impactions, although the nature of the poor esophageal propulsion in the latter disorder is not clear.38, 39
Symptoms of Misdirection of Swallows into Airway
Cardinal signs of oropharyngoesophageal dysmotility are signs of misdirection of swallowed material into the airway.
Nasopharyngeal Regurgitation
Palatal dysfunction can allow material into the nasopharynx. This is considerably more common in premature infants than in older children or adults, and tends to improve as the infant develops.40 Nasopharyngeal regurgitation sometimes results in ejection of swallowed material from the nostrils; it has also been associated with apnea in premature infants.41, 42
Laryngeal Penetration and Aspiration
Pharyngeal dysmotility can allow material into the larynx, trachea, and lower airways. Infants with lung disease related to prematurity and neurologically impaired children are particularly susceptible to such aspiration. Such misdirection can also occur during reflux, when the pharyngolaryngeal protections do not operate optimally on refluxate that reaches the pharynx; in this case, the acidic nature of the refluxate produces additional damage to the airway. In the differential diagnosis, aspiration may be due to anatomic abnormalities, such as laryngeal clefts or tracheoesophageal fistulas, which permit entry of food into the airway.
Specialized videofluoroscopic studies in 43 infants suspected of dysphagia disclosed a high frequency of laryngeal penetration and frank aspiration.40 They also demonstrated the important role of fatigue: aspiration or laryngeal penetration uncommonly occurred after the first swallows, but only later after fatigue had caused the protective functions to deteriorate. Further, they showed the frequency of silent aspiration in infants: of nine infants who aspirated during the study, only one coughed. However, the infants often were able to clear, without coughing, nonaspirated material that had penetrated the larynx.
Coughing/Choking/Gagging; Hoarseness/"Wet Voice"
Cough is a protective reflex involved in clearance of material in the airway; thus, it is a sign that the material may already have breached the primary airway protective mechanisms. Therefore, chronic cough is an important sign of disordered oropharyngoesophageal motility resulting in risk of airway disease.19 Choking and gagging on feedings are similar symptoms suggesting airway threats.43 Hoarseness and "wet voice" signify laryngeal inflammation or soiling.
Silent Aspiration
As noted, misdirected swallows may result in obvious aspiration, with immediate coughing or massive aspiration pneumonia. Often, however, the aspiration is "silent," only detectable during specialized investigations that are undertaken because of chronic or recurrent pneumonias, bronchiectasis, asthma, or other lower airway disease. This is particularly the case in young infants and in the neurologically disabled older child. The chronic lung disease produced by recurrent silent aspiration is insidious; its "silence" is evidence of failure of airway protection functions such as coughing. A study in infants found that nearly 90% of aspirating infants did so without coughing,40 in contrast to a much larger study of aspirating adults that found that fewer than 60% aspirated silently.44
Pneumonias, Bronchiectasis, Asthma, Wheezing, Stridor, Apnea
The outcome of a single episode of significant aspiration is apt to be pneumonia; when aspiration is recurrent, which is particularly likely if aspiration is silent, chronic lung disease such as bronchiectasis may result. Smaller volumes of aspiration may induce bronchospasm and hence asthmatic attacks. Similarly, microaspiration confined to the larynx may induce laryngospasm, and hence cause stridor or obstructive apnea episodes.43 Oxygen desaturation may result from many of these situations and be the only sign of disordered deglutition or abnormal esophageal motility.45
Abnormalities in Speech Development
Because the young child acquires speech as swallowing function matures, disrupted development of speech frequently accompanies oropharyngeal dysmotility in this age group. Tracheotomy in infants, for example, can impair both deglutition and speech.46
Physical Findings
Physical Examination
The physical examination of the child with suspected oropharyngoesophageal motility disorder includes a general physical examination, which may indicate abnormalities in growth or nutrition, or point to important systemic disorders, including those with neurologic, respiratory, or allergic manifestations. The focused examination includes detailed inspection and assessment of the head, neck, face, oropharynx, and chest, including search for poor head control, neck hyperextension, orofacial hypersensitivity, palate clefts, gag hyper- or hyporeflexivity, asymmetry of tongue position, disproportion of tongue-to-oral-cavity ratio, micrognathia, abnormalities of dentition, drooling, perioral rash, and hoarse voice. Abnormalities of the sounds of swallowing, detected with a stethoscope at the neck, have been described.
Feeding Observation
A specialized aspect of the physical examination in the child with suspected oropharyngoesophageal dysmotility is observation of a feeding. Participation of a speech pathologist or feeding therapist with pediatric expertise markedly improves the diagnostic utility of a feeding observation, and a diagnostic feeding is often carried out with concurrent radiographic assessment (see below). Normal movements, including jaw stabilization, chewing, and appropriate lateralization of the bolus, should be identified. Abnormal movements are also sought: jaw thrust, tongue thrust, tonic bite reflex, jaw clenching, averting the mouth, and abnormal persistence of primitive reflexes such as the phasic bite reflex and suckle feeding. After swallowing, any regurgitation or nasal reflux is identified. Choke, gag, or cough during the feeding, and hoarse or "wet" voice (or cry, in the infant) just following the feeding, are noted.
Laboratory Findings: Diagnostic Procedures
Diagnostic procedures in children must be adapted to their smaller and more variable sizes, to their immature and variable abilities to comprehend and cooperate, and to the need for surrogate informed consent procedures. The clinician, therefore, must possess technical equipment and be proficient in procedures modified for children. The procedures often take considerably longer to perform. Novel procedures must generally be thoroughly investigated in adults before they are adapted to children, so that pediatric diagnostics often lag behind those for adults. The indications for the procedures discussed below are summarized in Tables 2,3,4.
Radiographic Procedures
Chest X-ray and Routine Barium Fluoroscopy
The simple chest x-ray can disclose, for example, the widened mediastinum and air-fluid level suggesting achalasia. Radiography for most cases of upper gastrointestinal tract dysmotility, however, must utilize more focused procedures employing barium and fluoroscopy. A straightforward esophagram or upper gastrointestinal study may show, for example, the achalasia "bird's beak," and is useful to exclude anatomic abnormalities.
Videofluoroscopic Swallowing Study (Modified Swallowing Study)
A barium fluoroscopy adaptation even more specific for the evaluation of dysphagia is the "modified swallowing study," currently usually designated the videofluoroscopic swallowing study. This study is a gold-standard technique to evaluate dysphagia, particularly in instances with suspected misdirection of swallows into the airway. One approach to the videofluoroscopic swallowing study is to use a uniform, standardized protocol for all patients; another approach, used more frequently for children, is to tailor each patient's study to their typical feeding pattern in order to evaluate their function in a more individualized, patient-centered way.47 However, observer variation in these evaluations has been a problem, and the desire for more interrater reliability has prompted interest in more uniform and consistent protocols, even for children.48, 49 Such protocols should improve the validity and reliability of these studies, enabling them to function as true gold standards, while still evaluating individual children in a manner that elicits their true swallow function.
Normative data from videofluoroscopic studies have been obtained in normal adult volunteers, but less information is available from normal children. In adults, timing of events required for normal deglutition may be useful to identify specific abnormalities and quantify abnormality between and within dysphagic patients. Measures assessed include times of swallowing gesture, actual bolus transit, bolus pharyngeal transit, soft palate elevation and closure, aryepiglottic fold elevation and supraglottic closure via approximation of arytenoids and epiglottis, arrival of the bolus in the vallecula, hyoid bone displacement onset and duration, arrival of the bolus at the pharyngoesophageal sphincter, maximum pharyngeal constriction, and pharyngoesophageal sphincter opening. These parameters represent events required for normal deglutition, can be used to identify abnormalities in dysphagic patients, and enable a basis for comparison of swallowing performance both within and between patients.2 Such normative data are available for nondysphagic elderly adults as well as for young adults.50 It would be of considerable interest to have similar data from normal children of various ages, if there were a way to do so ethically; one could postulate that the normal timing parameters might either decrease with smaller size individuals or increase with more developmentally immature individuals.
Very discrete abnormalities of function are amenable to detection via videofluoroscopic swallowing studies: one study identified seven distinct, commonly repeated, abnormal epiglottic movement patterns, with each pattern associated with specific rates and amounts of aspiration.51
One of the most important findings on videofluoroscopic swallowing studies is that of material entering the airway, classified as laryngeal penetration or tracheal aspiration, and a scoring system for such penetration or aspiration has been described.52 Laryngeal penetration is infrequent in adults without swallowing problems; its incidence in normal infants and children is unknown. A study of 125 dysphagic children, from 7 days to 19 years of age, found the incidence of laryngeal penetration during videofluoroscopy to be 60%, with 31% demonstrating deep laryngeal penetration.53 Of the latter group, 85% aspirated. An important observation during this study was that children exhibiting deep laryngeal penetration often began to aspirate later during their feedings. The authors of this study emphasized the utility of extended feedings during videofluoroscopy, particularly in children who exhibit deep laryngeal penetration early in the study. Others have echoed this caveat.40
When material enters the airway without coughing, the aspiration is termed "silent." Videofluoroscopic swallowing studies can identify such silent aspiration. The authors of a huge, 2-year, retrospective adult study in two acute care hospitals analyzed the findings in 1101 patients (ages 3–98 years, median 68 years) who had such studies.44 Of them, 469 (43%) aspirated during the study, but in 276 of them (25% of the total and 59% of the aspirators) the aspiration was silent. The youngest (ages 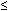 19) were the single group most likely to aspirate silently, 86% of all those who aspirated did so silently. Silent aspiration was most likely in children (86%), those over 90 years of age (72%), and those between 20 and 39 years of age (74%); p <.001. Males aspirated silently more than females did (62% vs. 46%, p = .004); those with neurologic or gastroenterologic diagnoses were more likely than those with other medical diagnoses to aspirate silently. Videofluoroscopically demonstrable silent aspiration may be even more common in aspirating infants than in aspirating adults.40
19) were the single group most likely to aspirate silently, 86% of all those who aspirated did so silently. Silent aspiration was most likely in children (86%), those over 90 years of age (72%), and those between 20 and 39 years of age (74%); p <.001. Males aspirated silently more than females did (62% vs. 46%, p = .004); those with neurologic or gastroenterologic diagnoses were more likely than those with other medical diagnoses to aspirate silently. Videofluoroscopically demonstrable silent aspiration may be even more common in aspirating infants than in aspirating adults.40
Infants with multiple medical problems, often associated with prematurity, are more likely to survive than previously, and many have respiratory and swallowing disorders. Several studies have evaluated videofluoroscopic findings in infants with suspected swallowing disorders. A study of 43 infants referred for suspected swallowing disorders found laryngeal penetration, aspiration, or nasopharyngeal backflow in more than half.40 Fatigue (after multiple swallows) was identified as an aggravating factor for penetration/aspiration, as most aspiration occurred after multiple swallows, with only three infants experiencing aspiration on the first swallow. This finding has diagnostic and therapeutic relevance: videofluoroscopic studies of infants should examine multiple swallows, and avoidance of fatigue is important for improving feeding ability in these young children. The presence of material in the pyriform sinuses before pharyngeal swallowing was also associated with penetration/aspiration. When laryngeal penetration occurred without aspiration, all infants cleared their airway during the swallow without coughing. Nine of the 43 infants aspirated, and all but one of them did not cough or clear their airway, emphasizing the high incidence of silent aspiration in infants, a very important observation that should prompt consideration of dysphagia evaluation in all instances of chronic or recurrent respiratory disease in infants. Prematurity was identified as a promoter of nasopharyngeal backflow, as that abnormality occurred significantly more often in premature than in term infants.
Another retrospective infant study reviewed the results of 77 upper gastrointestinal radiographic studies and 17 videofluoroscopic swallowing studies in 77 infants younger than 1 month of age referred for isolated feeding-related difficulties (i.e., without other medical problems) during a 5-year period. Swallowing dysfunctions with aspiration, found in 19 children, were the most frequent abnormality accounting for the infants' feeding problems. In 10 of the 19, the videofluoroscopic swallowing study was the only one of the two studies that disclosed the abnormality, highlighting the importance of considering this testing in infants with nonspecific feeding problems, that is, in infants who are well when not feeding, but develop coughing, choking, gagging, cyanosis, apnea, respiratory distress, stridor, or bradycardia during feedings.54
Patients with marked developmental delay and clinical evidence of oral-phase impairments may show specific abnormalities in the more distal, pharyngoesophageal, phases of the swallow during videofluorographic swallowing studies. This was the case in 14 patients with severe motor and intellectual disabilities, whose oral phase of swallowing was undeveloped beyond the late weaning period, manifest clinically as poor or absent lip seal, infantile swallowing, slowed or stalled bolus transit, and oral residue after swallowing.55 These studies showed severe impairment in the transitional and pharyngeal phases: pooling of liquid barium in the hypopharynx prior to swallowing, delay of cricopharyngeal relaxation, aspiration of liquids (silent in 78%), aspiration of purees, and pooling of purees in the pharynx after swallowing. These videofluorographic studies prompted specific improvements in therapy, which improved the patients' feeding abilities.
Oropharyngeal and respiratory impairments may interact in individuals with neurodisability. In a mixed group of 32 children and adults (ages 3–33 years), videofluoroscopic swallowing studies linked with respiratory recordings of inspiration, expiration, and airflow velocity examined this interaction.56 This study evaluated the pharyngeal dwell time (PDT), the duration that material remained in the pharynx before the swallow (either because of pharyngeal delay or incomplete clearance of the previous swallow). The PDTs were longer among the 12 participants who aspirated liquids (6.2 seconds) than among the 20 who did not (2.4 seconds), but the volumes of liquid in the pharynx did not differ between the two groups. The percentage of the PDT spent in inspiration was also greater among aspirators. During the PDT, aspirators showed more abnormal respiratory patterns for liquids than nonaspirators, which was not the case for purees. A score derived from the PDT and respiratory data predicted aspiration (sensitivity of 83% and specificity of 95%). The authors concluded that aspiration results from oropharyngeal impairments with inadequate respiratory integration.
Manometric Procedures
Esophageal manometry assesses motor abnormalities in the esophagus itself; catheter adaptations including sleeve ports for sphincters, particularly a radially asymmetrical "sleeve" port for the upper esophageal sphincter, also allow it to evaluate the function and coordination of this sphincter and the pharynx. When evaluating both lower and upper esophageal sphincters, the markedly variable esophageal lengths of children of different ages mandate the availability of multiple catheters with different gradations of distance between the ports, particularly between the sphincter sleeve ports. The need for cooperation from patients in order to evaluate swallowing function while tormented by an indwelling nasogastric tube makes manometry more challenging in children and mandates considerable patience from the person performing the test. Recognition of a primitive swallowing reflex has allowed the elicitation of swallowing by infants and neurologically abnormal older children during these studies.57
Manometry facilitates the classification of the various primary and secondary esophageal motor disorders, as for adults,33 and the diagnosis of various categories of impairment of bolus transfer across the upper esophageal sphincter into the esophagus. Such cricopharyngeal abnormalities include those with inadequate pharyngeal propulsive pressure, incomplete relaxation of the sphincter (cricopharyngeal achalasia), or incoordination between the pharyngeal wave and the sphincter relaxation.58
Manometry during provocation, with food, acid infusion, or drugs, elicits intermittent abnormalities undetected during routine manometry.59, 60, 61 Continuing manometry for 24 hours on an ambulatory basis and combining it with pH-metry has facilitated the detection of reflux-associated dysmotility in children who had had normal brief and stationary manometric testing.62
Combining manometry with other techniques, such as high-resolution endoluminal sonography or multichannel intraluminal impedance, facilitates examination of the coordination of muscle contraction and bolus flow, but these technical achievements have not yet been applied to evaluation of children.63, 64
Endoscopic Procedures
Fiberoptic Endoscopic Evaluation of Swallowing by Sensory Testing (FEESST)
Small nasopharyngeal endoscopes positioned to observe the pharynx and larynx in awake patients made possible the direct visualization of events during swallowing.65 Spillage, residue, penetration, and aspiration of the food material, dyed to enhance visibility, can be assessed. Subsequent supplementation of this fiberoptic endoscopic evaluation of swallowing (FEES) by sensory testing (ST) of the laryngeal adductor reflex, by pulsing air through the endoscope to the aryepiglottic location of the afferent limb of this reflex, produced the composite FEESST.66 Several reports now demonstrate the applicability of this evaluation to children.67, 68, 69, 70
A comprehensive report of 643 FEES procedures performed between 1993 and 1999 on 568 children aged 3 days to 21 years (median 2.5 years) described preprocedure diagnoses, feeding limitations, and postprocedure classification of abnormalities.69 Preprocedure, 36% had structural diagnoses; 26% had neurologic diagnoses; 12% had gastroenterologic diagnoses; and the remainder had genetic, pulmonary, prematurity-based, cardiovascular, or metabolic disorders. Feeding limitations included 40% unable to take any oral nutrition, 38% orally fed but with limitations, and 13% orally fed but requiring supplemental tube feeds. The FEES disclosed behavioral abnormalities, including sensory-based feeding disorders, in 56%; neurologic abnormalities in 16%; structural abnormalities in 15%; and normal feeding in 15%.
A smaller pediatric report of FEES in 30 patients aged 11 days to 20 years (mean, 10 years) found normal swallowing in 57%.68 Forty percent of the 10 children with dysphagia were prescribed a nonoral diet because of aspiration risk; in the other 60%, the FEES prompted specific feeding recommendations (i.e., bolus consistency modifications, positioning, and feeding strategies) to reduce risk of aspiration.
A series describing pediatric laryngopharyngeal sensory testing (the ST in FEESST) in 100 children suspected of feeding and swallowing disorders showed its feasibility in unsedated children aged 1 month to 24 years (median 2.7 years). The laryngopharyngeal sensory tests, performed by delivering a pressure-controlled (3–10 mmHg) and duration-controlled air pulse to the aryepiglottic fold through a flexible laryngoscope, were completed in 92% of patients. The test disclosed three levels of sensation: <4 mmHg, 4 to 10 mmHg, and >10 mmHg. Those children with the greatest sensitivity (<4 mmHg) rarely if ever had episodes of laryngeal penetration or aspiration. The 22 patients with the least sensitivity (>10 mmHg) demonstrated severe laryngeal penetration and/or aspiration. The intermediate group had variable amounts of aspiration and penetration. Elevated laryngopharyngeal sensory thresholds correlated positively with previous clinical diagnoses of recurrent pneumonia, neurologic disorders, and gastroesophageal reflux, and correlated positively with FEES findings of pooled secretions, laryngeal penetration, and aspiration.71
Another report, from the group that reported the large pediatric series above, examined the utility of preoperative feeding assessments in 255 children (median age 2.5 years, 53% tracheotomy dependent) undergoing laryngotracheal airway reconstruction.70 Only 13% of the patients had diagnoses limited to the airway, with 45% of patients having three or more diagnoses. Worse preoperative feeding abilities were associated with the presence of a tracheotomy, age 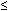 2 years, and multiple underlying diagnoses, particularly neurologic ones. Transient dysphagia was common after laryngotracheal reconstruction, but findings on the FEES that predicted poor airway protective mechanisms after reconstruction were (1) poor oral motor skills, allowing premature spillage of material into the hypopharynx; (2) pooling of secretions in the hypopharynx; and (3) residue persisting in the hypopharynx after multiple swallows. Preoperative feeding assessments directly altered the course of management of 15% of operative patients, by recommending a delay in the surgical correction, the placement of a gastrostomy tube preoperatively, or a modification in the surgical reconstruction planned for the patient. Postoperative airway protection predictions were 80% accurate.
2 years, and multiple underlying diagnoses, particularly neurologic ones. Transient dysphagia was common after laryngotracheal reconstruction, but findings on the FEES that predicted poor airway protective mechanisms after reconstruction were (1) poor oral motor skills, allowing premature spillage of material into the hypopharynx; (2) pooling of secretions in the hypopharynx; and (3) residue persisting in the hypopharynx after multiple swallows. Preoperative feeding assessments directly altered the course of management of 15% of operative patients, by recommending a delay in the surgical correction, the placement of a gastrostomy tube preoperatively, or a modification in the surgical reconstruction planned for the patient. Postoperative airway protection predictions were 80% accurate.
Quantification and scoring of various descriptive aspects of the FEESST study may improve its predictive value. Such refinements recently developed for adult studies have included the scoring of visualized secretions,72 penetration and aspiration,73 and sensory deficits,74 complemented by measurement of pharyngeal muscular tone (pharyngeal squeeze).74
Esophagoscopy with Esophageal Biopsy
Endoscopy of the upper gastrointestinal tract can provide useful information regarding inflammatory conditions contributing to nonspecific esophageal dysmotility (e.g., reflux esophagitis or eosinophilic esophagitis). Such endoscopy can also identify conditions in the differential diagnosis, such as structural causes for aspiration (e.g., laryngeal clefts or tracheoesophageal fistulae) or inflammatory causes for chest pain unassociated with dysmotility (e.g., infectious, reflux, or eosinophilic esophagitis).33, 75
In children suspected of reflux esophagitis, it is particularly important to evaluate histology even in cases in which no macroscopic abnormalities of the esophagus are evident. In the absence of macroscopic changes, morphometric changes, particularly increase in papillary length (to >53% of the total epithelial thickness) and thickening of the basal layer (to >25% of the total epithelial thickness), distinguish normal children from those with reflux disease76, 77, 78 and correlate with increasing esophageal acid exposure.79 Orientation of biopsy specimens for cutting perpendicular to the luminal surface is important in these measurements,80 but may be difficult with the size specimens obtained through the smaller pediatric endoscopes.81
Laryngotracheobronchoscopy
Endoscopy of the airway can provide information regarding sequelae of aspiration caused by dysmotility; it can also disclose abnormalities other than dysmotility that are responsible for any aspiration, such as a laryngeal cleft.
Tracheal Fluid for Lipid-Laden Macrophages or Pepsin
During airway endoscopy (or, alternatively, through an existing tracheostomy), sampling of airway fluids has been used to diagnose aspiration of fat in meals via microscopic identification of lipid-laden macrophages. Lipid-laden macrophages above a threshold number suggest aspiration of fat from meals, although the sensitivity and specificity of this test has been debated. Detection of pepsin in airway samples may be more specific for aspiration of material refluxed from the stomach.82, 83
Scintigraphic Procedures84
Scintigraphy for Aspiration During Swallows or During Reflux
Technetium-99m scintigraphy is an attractive imaging modality for children because of its limited radiation exposure and 6-hour half-life. Scintigraphy allows tracking of a physiologic meal through the upper gastrointestinal tract (and airway, if aspiration occurs), and provides data for evaluation of swallowing, reflux, gastric emptying, and aspiration. In children, such scans have been termed "milk scans," after the milk formulas fed to young children. Imaging periodically after a technetium-labeled meal provides somewhat crude information; utilizing the potential data more extensively requires specific programming, not widely exploited.85 Further, using a low dose of tracer produces a somewhat indistinct image.
Salivagram
Aspiration during swallowing of small volumes of saliva can be detected in children scintigraphically using the salivagram.86, 87
Oropharyngeal Scintigraphy
Development and rigorous validation of a scintigraphic technique for quantitative evaluation of oral-pharyneal swallowing in adults has recently been published.88 The authors established excellent scintigraphic test-retest reliability in a group of controls (>55 years old), and evaluated accuracy of transit measures by comparison with radiographic temporal measures. Diagnostic accuracy in comparison to radiographic measures were very good, showing that abnormal oral and pharyngeal residuals had a positive predictive value of 100% and 92%, respectively, for regional dysfunction disclosed radiographically. It is hoped that this test will prove similarly useful in children.
Esophageal pH-metry
Generally not considered a test of esophageal motility, distal esophageal pH-metry may identify acid reflux from the stomach into the esophagus and the duration of such episodes, suggesting aspects of the motor function of both the lower esophageal sphincter and the esophageal body. Multiple-channel pH-metry adds detail about the proximal extent of such reflux episodes.
Esophageal Multichannel Intraluminal Impedance
The ability to track the flow of nonacid material through the esophagus in ambulatory children using impedance recently had added tremendous value to some investigations. Twenty-eight children with persistent respiratory symptoms on acid-suppressive medications underwent 24-hour combined studies with pH-metry and impedance.89 The investigations were able to associate respiratory symptoms with reflux episodes, particularly in younger children and during nonacid and "full column" reflux. Suboptimal pharyngeal coordination of the airway–gastrointestinal interface may allow mishandled neutral-pH refluxate to cause respiratory symptoms in these young children, a phenomenon that would have been difficult to detect without impedance. Similar findings during swallowing, rather than during reflux, were detected in 15 infants who manifested apnea during swallowing of neutral pH material.90
Central Nervous System Imaging
Magnetic Resonance Imaging (MRI), Functional MRI, Computed Tomography (CT)
Testing for a central lesion responsible for dysphagia in the cortex or brainstem may prove useful in some children. Although CT is sometimes used, MRI may be more sensitive,91 and functional MRI of the cortex and brainstem has begun to be used in children.92 Many central lesions, however, may be beneath the resolution of current imaging techniques.10
Miscellaneous
A number of innovative techniques investigating various aspects of oropharyngoesophageal dysfunction are beginning to be used in children or may in the future become useful for clinical or research purposes in children. Some of these techniques, proposed in speech and orthodontic literature, investigate electromyographically the function of the local end organs in the mouth (e.g., the perioral, masticatory, or tongue muscles).13, 93, 94, 95, 96, 97 Others use electromyography to evaluate the pharynx or larynx,98 categorizing laryngeal disorders as normal, myopathic, or neuropathic. Yet others investigate the pressures generated by these organs (e.g., pharyngeal and nipple pressures evaluated in premature infants with various disorders).5, 11, 17 Still others use ultrasonography submentally or endoscopically to evaluate the movement of the bolus or the swallowing structures.
Some authors have proposed various "low-tech" or noninvasive techniques to evaluate swallowing function or aspiration risk, particularly in children.
In children with tracheostomies, for example, Evan's blue dye has been used to detect aspiration, manifest by the orally administered dye's appearance at the tracheostomy. The benefits of this test include simplicity, low cost, and bedside feasibility. However, a study in 20 patients at an acute rehabilitation hospital who had shown aspiration during videofluoroscopic study showed excellent reliability (100% detection) in those who had aspirated more than trace amounts at videofluoroscopy, but no detection in those who aspirated only trace amounts.99 Similarly, another adult study compared the modified Evan's blue dye test to FEES in 30 tracheotomized patients undergoing swallowing evaluation. The study found 82% sensitivity for predicting aspiration (100% in those receiving mechanical ventilation), but only 33% to 40% specificity, regardless of ventilator status, concluding that its optimal use was as a screening test, with rigorous attention to the test protocol used.100
A group of three other tests was recently proposed as a substitute for videofluorographic swallowing studies: (1) the water swallowing test (3 mL of water are placed under the tongue and the patient is asked to swallow); (2) the food test (4 g of pudding are placed on the dorsum of the tongue and the patient is asked to swallow); and (3) the x-ray test (static radiographs of the pharynx are taken before and after swallowing liquid barium). Comparing these tests with videofluorographic studies in 63 patients with dysphagia, the sensitivity of the sum of all three tests was 90% for predicting aspiration, and the specificity for predicting its absence was 71%. Eliminating the x-ray test did not reduce the sensitivity, but lowered the specificity to 56%. The tests are presented with detailed scoring algorithms.101 Again, these procedures appear most likely useful for screening.
Acoustic methods to evaluate oropharyngeal dysphagia have also been proposed as noninvasive and portable, although not "low tech," screening diagnostic techniques.3 Acoustic signals recorded with accelerometers over the trachea produced 350 signals from three bolus consistencies (semisolid, thick and thin liquids), recently allowing construction of a screening algorithm, which correctly classified 13 of 15 control subjects and 11 of 11 subjects with some degree of dysphagia and/or neurologic impairments.102
Videostroboscopic image analysis of the larynx has been integrated with laryngeal electromyography in one study of 80 patients, resulting in detailed critical interpretation of each individual's pathology.98
Differential Diagnosis
Differential diagnostic considerations for the child with symptoms of oropharyngoesophageal dysmotility are broad. General categories include mechanical obstruction of the upper gastrointestinal tract, abnormal anatomic communications between the upper gastrointestinal tract and the airway, sensory disorders, and psychobehavioral disorders.103 The history, physical examination, and laboratory tests enumerated above generally enable exclusion of these entities in the child presenting with symptoms suggesting dysmotility.
Treatments
As is true of diagnostic procedures, the development and application of therapeutic interventions for children with disorders of oropharyngoesophageal dysmotility has often lagged behind that for adults. Many of the treatments have not undergone rigorous controlled evaluation.104, 105 This section discusses therapies for these disorders: general aspects, "conservative" lifestyle measures, pharmacologic agents, and procedural or surgical techniques.
General
Because of the complexity of these disorders, and because many of them impact the child at the intersection of gastrointestinal, respiratory, and neuromuscular systems, interdisciplinary teams of personnel often must participate in designing optimal treatments. For children, optimal teams consist of personnel with in-depth pediatric experience, and may include pediatric gastroenterologists, otolaryngologists, pulmonologists, speech-language therapists, rehabilitation therapists, nutritionists, surgeons, occupational and physical therapists, orthodontists, and so on.106 The setting for such therapy may be the acute pediatric hospital, rehabilitation hospitals, outpatient clinics, the home, or the school.106, 107, 108 It is important to diagnose and begin therapy early for dysphagia in children; delay in management may interrupt normal development of swallowing during critical stages, producing feeding aversion and delaying rehabilitation.18, 19 A Japanese group found that in 51 tube-fed infants and young children, a higher rate of progression to tube extraction occurred in those with older age of onset of dysphagia, shorter duration of dysphagia prior to treatment, and younger age at starting treatment.109
Conservative Lifestyle Measures
Conservative measures to assist in management of oropharyngoesophageal dysmotility include optimizing body and head position (both during feedings and during sleep) to minimize the risk of aspiration; thickening and other adaptations of feeds and feeding equipment; performing specific maneuvers during swallowing; using the most favorable swallow intervals; "exercise" conditioning of swallowing musculature; and avoidance of fatigue. Further, optimizing the nutritional value of the meals consumed and management of associated disorders, including secondary feeding aversion, are crucial.19, 110
Body and Head Position
The position of the body and head during feeding or during sleep can influence the likelihood that swallowed material (or refluxed material) will be misdirected into the airway.111 Simply elevating the head above the stomach allows gravity to compensate for some deficits of motility, but optimal alignment and stabilization of trunk, head, and jaw (using intraoral appliances in some cases112, 113, 114) may be useful for particular disorders. Children with cerebral palsy or primary myopathies, for example, may require specialized external supports for these functions.114, 115 Specific uses for particular head positions are indicated in the paragraph on swallow maneuvers, below.
Thickening and Other Adaptations of Feedings
Thickening of feedings to alter the bolus flow and maneuverability in the oropharynx can improve airway protection. There is a need for rheologic standards, as clinicians' subjective impressions may not be completely accurate or reproducible.116, 117, 118 Various descriptive textures (e.g., pureed, minced, and soft) have proved useful for different children, although the person doing the feeding is also an important variable.119 Because thickening of feedings also decreases regurgitant reflux, thickening of feeds has added potential benefit in those children, particularly neurologically impaired children, with dysphagia as well as gastroesophageal reflux disease.120, 121
Other manipulations of foods are adding thermal or tactile stimulation to speed triggering of the pharyngeal swallow in order to prevent aspiration that would otherwise intervene during the pharyngeal delay. For this purpose, cold food, pressure from a spoon on the tongue, or a bolus that requires chewing are several useful techniques.122 Feeding equipment, including special nipples, spoons, etc., has been designed to be adapted to particular disorders and can be prescribed by speech therapists or feeding specialists.
Swallowing Maneuvers
The choice of specific head positions, maneuvers, and swallowing techniques used for individuals with oropharyngeal dysphagia depends on the disorder to be treated.122 The head is tilted back to treat inefficient oral transit due to poor propulsion of the bolus by the tongue, but this head position must be used carefully, as it may impair airway protection even in healthy individuals.95 The chin is tilted down, in contrast, to treat delayed triggering of pharyngeal swallow, reduced retraction of the tongue base leading to residue in the valleculae, or reduced laryngeal closure leading to aspiration during the swallow. Lateral head tilt toward the stronger side is used to treat unilateral oral and pharyngeal weakness leading to residue in the mouth and pharynx on that side. Head rotation toward the weak side is used to treat unilateral laryngeal dysfunction leading to aspiration during the swallow, or unilateral pharyngeal paresis leading to residue on one side of the pharynx. Head rotation is also used to pull the cricoid cartilage forward to reduce the upper esophageal sphincter tone in order to treat residue remaining in the pyriform sinuses. The empiric effect of these head and neck positions were evaluated in adults: 24 healthy controls, nine patients with unilateral lower cranial lesions, and 42 patients without laterality in their oropharyngeal muscle functioning.95 A randomized controlled trial of the efficacy of chin tilt down versus thickening of feedings for adults with Parkinson's disease has been undertaken.105
Four swallowing maneuvers to exert voluntary control over aspects of the swallow have been described: supraglottic swallow, in which inspiration before swallowing allows voluntary expiration after a swallow to clear the vocal folds of contaminating liquids; supersupraglottic swallow, with more effortful breath holding; effortful swallow, to increase the posterior tongue base movement in cases in which it is reduced; and the Mendelsohn maneuver, in which the laryngeal elevation and upper esophageal sphincter opening are increased.94, 122 The degree to which these positions and maneuvers are useful in children depends in part on their developmental stage and speech and communication skills.123, 124 However, it is notable that extremely severe swallowing disability, manifest by completely absent pharyngeal swallow, has not precluded complete dependence on oral intake in a patient as young as 18 years of age, who used a sequence of devised maneuvers to completely compensate for an absent swallowing mechanism.125
Exercises
Exercises specific to the musculature involved in swallowing, including tongue resistance and range of motion, and laryngeal adduction, may be useful. Intraoral appliances have been used to facilitate the learning of optimal oral movements. However, over the long term they may not be more beneficial than maturation alone.105, 112, 114, 122 Methods of applying electrical stimulation to the patient with pharyngeal dysphagia have been developed.107, 126
Fatigue Avoidance
It is crucial to avoid fatigue during eating in children with dysphagia.19, 40 During videofluoroscopic swallowing examinations, children with deep penetration early in the study were likely to advance to aspiration during an extended study.53 Furthermore, consistency in presentation of food seems important in oral-motor skill acquisition by children with severe neurologic impairment.123, 124
Nutritional Management
Maintaining nutrition comprises a crucial aspect of the treatment of any child with dysmotility of the upper gastrointestinal tract. If the above conservative methods, supplemented by any appropriate pharmacotherapy or surgical therapy, are insufficient to promote optimal nutrition, nasogastric feedings may be used for the very short term. If oral nutrition is not then feasible, percutaneous gastrostomies or jejunostomies may be required while other therapeutic interventions proceed. Children with oropharyngoesophageal dysmotility rarely require parenteral nutrition, unless other disabilities preclude the use of the intestinal tract.
Management of Associated Disorders
Management of associated disorders is beyond the scope of this chapter, but the fact that nearly 50% of children with dysphagia have multiple etiologic contributing factors must be kept in mind.14 Gastroesophageal reflux is a particular complicating factor to consider, because these children may be more likely to aspirate any refluxed material.121
Pharmacologic Agents
Most pharmacologic agents to treat these disorders are, like many pharmacotherapies in use today, not adequately evaluated or approved by the Food and Drug Administration for use for these indications, in children. Nonetheless, clinicians use these drugs because of the absence of adequate alternatives. Some of the newer drugs in early use in children are reviewed elsewhere.127
Motility-Modifying Agents
Agents to modify motility are the most obvious pharmacotherapies for motility disorders of the upper gastrointestinal tract.
Contractility-reducing agents treat disorders that produce elevated sphincter pressures or high peristaltic amplitudes.128 These conditions include achalasia, diffuse esophageal spasm, nutcracker esophagus, and cricopharyngeal achalasia. The agents include calcium channel blockers (e.g., nifedipine, diltiazem), nitric oxide effect promoters (e.g., sildenafil129, 130, 131) and nitrates, as well as botulinum toxin injected directly into the hypertonic lower132, 133, 134, 135, 136, 137, 138 or upper139, 140 esophageal sphincter. Effects of each of them have been imperfect and inconsistent in clinical trials.128 Botulinum toxin injections used to treat achalasia in two pediatric studies (3 and 23 patients, respectively) produced symptomatic resolution, but symptoms recurred within 7 months in at least half of the children.132, 133
Contractility-augmenting agents, on the other hand, treat the lower esophageal sphincter incompetence of gastroesophageal reflux disease.128 Agents used for this purpose include metoclopramide and several others not available in the United States, such as domperidone and cisapride. Inconsistent and imperfect results of clinical trials affect these drugs as well.
Agents to inhibit the lower esophageal sphincter relaxations responsible for gastroesophageal reflux disease include the 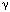 -aminobutyric acid (GABA)B agonist baclofen.141
-aminobutyric acid (GABA)B agonist baclofen.141
Gastric Acid–Suppressing Agents
Gastroesophageal reflux disease, itself the most common upper gastrointestinal motility disorder, may also play a secondary role in other upper motility disorders, such as postmyotomy achalasia patients, or patients who aspirate during reflux as well as during primary swallowing. In addition, gastroesophageal reflux disease may mimic the symptomatic presentations of many pediatric esophageal motility disorders.33 Therefore, empiric therapy for the symptoms or directed therapy for diagnosed gastroesophageal reflux disease becomes a logical early step in many algorithms for management of these disorders. The most consistently beneficial pharmacotherapy for gastroesophageal reflux disease is powerful acid suppression, which interrupts the acid damage of the esophagus and thus resulting vicious cycles of esophageal dysfunction. Proton pump inhibitors are thus currently the primary drugs in this category, with histamine-2 receptor antagonists, antacids, and topical agents such as sucralfate also playing a role.
Glucagon for Food Impaction
Because of its ability to decrease lower esophageal sphincter pressure, glucagon is sometimes used before more invasive means to treat solid food impacted in the esophagus of the patient with esophageal dysmotility. However, glucagon also may decrease lower esophageal body contraction pressures, and thus impair esophageal propulsion of the impacted bolus.142
Psychotropic Agents
Antidepressants and benzodiazepines have found some use in ameliorating the symptoms of upper gastrointestinal dysmotility disorders, but generally without affecting the motility itself. Pediatric studies of this use of these agents are even rarer than adult studies.128
Procedural or Surgical Treatments
Procedures to treat oropharyngoesophageal dysmotility include those directed at management of oral cavity disorders, provision of nutrition, improving the pharyngoesophageal motility disorder itself, or prevention of aspiration.
Orthodontia
Orthodontic procedures, which are beyond the scope of this chapter, may benefit children with abnormalities of biting and chewing; such procedures may improve their swallowing, as well as their speech and facial morphology.31, 93, 143
Gastrostomy and Enterostomy Tube Feedings
Children unable to consume adequate nutrition orally for prolonged periods because of dysphagia may require placement of a gastrostomy or enterostomy tube, either surgically or percutaneously. In a prospective 1-year study at a single institution, 20 children (mean age 6.5 years) with severe mental impairment and oropharyngeal dysphagia underwent endoscopic gastrostomy.144 Sixteen had cerebral palsy, and two each had myopathy and traumatic brain injury. During half a year of follow-up, weight gain occurred in all. However, complications consisted of three (15%) perforations, four stomal infections, seven instances of granulation tissue, three reflux pneumonias, and one pneumoperitoneum. Another pediatric report cites a 3.5% rate of gastroen teric fistulae (12 of 343 percutaneous gastrostomies during a 5-year period) presenting up to 25 months postgastrostomy, often (8/12) with acute intestinal obstruction and universally involving the posterior gastric wall.145
Late complications of percutaneous (or surgically placed) gastrostomy or jejunostomy tubes include various malfunctions that prompt emergency department visits; a report of such visits by demented patients with malfunctioning feeding tubes cited 138 visits by 33 patients during 20 months, and a total estimated national cost extrapolated at almost $11 million annually.146
Tube-fed children are more likely to be able to resume oral feeding if they have a shorter period of dysphagia before tube placement, the onset of feeding impairment after 8 months of age, younger age at initiation of treatment for eating (specifically before 36 months of age), and less severe dysphagia.109
Dilations
Dilation of the hypertensive sphincter in achalasia or in cricopharyngeal achalasia is widely used, and generally considered first-line therapy.134 It is less clear whether it should be used for nonobstructive dysphagia147 or in patients without endoscopically evident disease.148 Children, as well as adults, may be able to advance to unsedated dilation during a program of repeated dilations of strictures; the applicability of this to children with dysphagia is unknown.149 Esophageal dilation is not without risk; perforation and brain abscess150 are reported complications.
Myotomies (UES, LES)
Heller myotomy for achalasia of the lower esophageal sphincter (LES) is the most commonly used myotomy, but myotomy is performed on the upper esophageal sphincter (UES) for cricopharyngeal achalasia. Myotomy of the esophageal length and LES has been performed for intractable diffuse esophageal spasm.151
Esophageal Replacement
Dysmotility or its sequelae may affect the native esophagus so severely that esophagectomy and esophageal replacement (e.g., by gastric tube or colon interposition) is warranted.151, 152 However, a majority of 81 adults undergoing this procedure reported chronic disability in the form of heartburn, continuing dysphagia, and the necessity for smaller meal size at 10 months to 18.9 years (median 9.8 years) after the procedure.153
Surgical Approaches to Aspiration Owing to Dysmotility
When nonsurgical approaches to aspiration, including discontinuation of all oral intake and aggressive pulmonary toilet, are inadequate, surgical approaches may be required. Tracheostomy, even using a cuffed tracheostomy tube, cannot ensure the prevention of aspiration. Minor procedures, such as injection of a unilateral paralyzed vocal cord with Teflon (or Gelfoam if functional recovery is expected within 6 weeks), or implantation of a noninjectable material like Silastic (laryngeal framework surgery), to bring it to the midline for apposition by the opposite, functional cord, can be helpful.154 More aggressive procedures include laryngectomy; laryngeal closure procedures using, for example, an epiglottic flap; and tracheoesophageal diversion with laryngotracheal separation.154, 155, 156
A pediatric series of thyroplasty for the treatment of vocal fold paralysis in eight children (2 to 17 years of age), aiming to manage both aspiration and dysphonia, indicated that the lower location of the pediatric larynx must be taken into account in designing such innovative surgical procedures, highlighting the importance of specific pediatric expertise.157
Specific Pediatric Disorders
Oropharyngeal and Upper Esophageal Sphincter Motility Disorders (Striated Muscle)
Neuromuscular disorders affecting striated musculature may impair the oropharyngeal phase of swallowing. These diseases may have pathophysiology in the central nervous system, the motor neuron or neuromuscular junction, or the muscle itself. The disorder may be systemic or may produce dysfunction localized specifically in the oropharynx.
Central Nervous System Disease: Brain and Brainstem
Many varieties of diffuse central nervous system dysfunction produce congenital dysfunctions of oral or oropharyngeal function that compromise normal oral intake and the normal development of suck and swallow. Cerebral palsy—nonprogressive brain damage acquired early in life from virtually any cause—is a relatively common nonspecific pediatric disorder.114, 121, 144, 158, 159 Others include in utero drug exposures or infections affecting the central nervous system,11 congenital brain malformations,160vascular infarcts, traumatic brain injury (particularly in adolescents),161, 162seizure disorders163, 164 and so forth.11, 112, 113, 115, 165Posterior fossa tumors and their surgery in children may also produce oropharyngeal dysphagia, as well as dysarthria.166 Congenital suprabulbar palsy has a variety of causes, often unidentified in the individual child.9 The diffuse nature of many of these disorders has implications for dysphagia management: such children are often unable to participate in volitional strategies to improve their swallowing, and their lack of postural control and language in many cases further complicates treatment. Many require lifelong tube feedings because of the inability to rehabilitate their oropharyngeal function, and a considerable number risk aspiration because of inadequate airway protection functions as well as the prevalence of silent aspiration.167, 168
The central or neuromuscular source of the swallowing dysfunction may be obscure in the very young infant, particularly if the lesion is small or the disorder diffuse or mild. A description of "isolated" neonatal swallowing dysfunction in nine infants, eight of whom presented within 2 weeks of birth with choking and cyanotic spells with feeds, recurrent aspiration, apnea, stridor, and vomiting, included three who had nonspecific neurologic abnormalities and were later diagnosed to have specific disorders [myotonic dystrophy, CHARGE association (coloboma, heart anomaly, choanal atresia, retardation, and genital and ear anomalies), and velocardiofacial syndrome]. All required tube feedings, which could be discontinued in seven, but not until a mean age of more than 3 years.169
Disease of Motor Neurons and Neuromuscular Junction
Disease of the motor neurons may affect specific nerves involved in swallowing. Bell's palsy, affecting the peripheral facial (cranial VII) nerve in adolescents as in adults, may affect the oropharyngeal phase of swallowing. In a series of 44 patients with unilateral Bell's palsy, 66% of patients demonstrated disturbed oropharyngeal swallowing of varying severities, subclinical in some instances, which normalized as the palsy normalized.170Paralysis of the laryngeal nerve, similarly, may induce dysphagia.
Tetanus and poliomyelitis, uncommon infections in immunized children currently, may disturb oropharyngeal function; delayed progressive dysphagia in polio victims generally affects adults currently.171, 172, 173
Botulinum toxin, a neurotoxin affecting the release of acetylcholine from the neuromuscular junction, causes dysphagia, as does Guillain-Barré syndrome, an immune-mediated demyelinating disease of peripheral nerves. Myasthenia gravis, an autoimmune disease directed against acetylcholine receptors, may cause dysphagia,174 and may be transmitted by the mother to the neonate in a transient form or may be inherited in a rare, congenital permanent form.
Muscular Disease
Muscular diseases affecting the striated muscle of the oropharynx include muscular dystrophies (myotonic and oculopharyngeal, the former presenting more often in children, although relatively rare)175 and inflammatory myopathies (e.g., dermatomyositis, polymyositis).176 Iron deficiency causes dysphagia (sideropenic dysphagia), possibly based on decreased constricting power of the pharyngeal musculature due to impaired oxidative metabolism in the striated musculature, as well as via web formation.177, 178 (It may also affect the smooth muscle of the distal esophagus.178)
Nonneuromuscular Systemic Disease or Medications Producing Oropharyngeal Dysphagia
Diabetic neuropathy may cause oropharyngeal dysphagia, in addition to its effects on the smooth muscle esophagus.179 Some drugs produce oropharyngeal dysmotility.180, 181, 182Severe nonneurologic diseases, such as bronchopulmonary dysplasia in premature infants, may also induce developmental abnormalities in suck and swallow motor activity.5, 17
Focal Cricopharyngeal Disorders
Focal disorders also may afflict the upper esophageal sphincter. This sphincter's tone is more variable than that of the lower esophageal sphincter in children as well as in adults. It rises with stress and virtually disappears during quiet sleep; its tone increases during mild esophageal distention and completely relaxes to vent severe distending forces.183, 184 Relaxation abnormalities of the upper esophageal sphincter threaten the airway during swallowing.
Cricopharyngeal achalasia, an uncommon pediatric disorder generally reported in small series of several patients, may be caused by damage to the inhibitory oligosynaptic corticobulbar pathway to the motoneurons of the sphincter.185 It is often diagnosed on the basis of videofluoroscopic study showing partial obstruction to flow of liquids through the upper esophageal sphincter, frequently accompanied by the impression of a "bar" on the barium column. Careful manometric study, however, may distinguish groups of these children with differing pathophysiology. These include incomplete relaxation of the sphincter, corresponding to achalasia of the lower esophageal sphincter; delayed relaxation of the sphincter, whereby the pharyngeal pressure wave initially confronts a tonically contracted sphincter; and premature relaxation, with after-wave and resumption of baseline sphincter tone before the pharyngeal pressure wave is completed. One of the most common causes of these uncommon abnormalities in young children is an Arnold-Chiari malformation.58 A head MRI should be performed in children with cricopharyngeal achalasia before submitting them to invasive procedures on the sphincter, because decompression of the Arnold-Chiari malformation may itself cure the cricopharyngeal achalasia. In the absence of a malformation, infants may be treated conservatively because of the spontaneous improvement that may occur. Otherwise, the cricopharyngeal achalasia may be treated with myotomy.186, 187 As with achalasia of the LES, the use of dilations188 and injection of botulinum toxin139, 140 have also been described. In contrast to adults, Zenker's diverticulum is not generally an issue in these children.
Brain and Cervical Spine Trauma
Cervical spine injuries as well as head injuries may cause dysphagia by direct effects on the neuromusculature of swallowing (indicated above), or by secondary effects of the endotracheal intubation and tracheostomy tubes that are often required in these children and adolescents.189, 190 After spinal cord injury, predictors of dysphagia (occurring in about 17% of one series) were tracheostomy and an anterior cervical approach to reparative spinal surgery; the combination of both factors produced dysphagia in 48%.191 Another study in 51 consecutively admitted adolescents and adults who were evaluated with FEES distinguished five levels of dysphagia: levels 1 and 2 (n = 13) were severely impaired, level 3 (n = 8) manifested cough response to aspiration, level 4 (n = 20) showed mild aspiration of fluids only or laryngeal edema, and level 5 (n = 10) was normal. After treatment, patients improved: level 1 (n = 0), level 2 (n = 1), level 3 (n = 2), level 4 and 5 (n = 48).192
In a series of 54 adolescents and adults with severe brain injury that did not preclude swallowing assessments, 61% exhibited abnormal swallowing and 41% aspirated.193 Risk factors for abnormal swallowing included tracheostomy and ventilation time >2 weeks; risk factors for aspiration included worse coma scores at admission. In a separate multivariate analysis, the level of cognitive functioning at admission; CT showing midline shift or brainstem involvement, or requirement for emergent surgery; and ventilation time >2 weeks predicted abnormal swallowing, aspiration, and difficulty achieving oral feeding after severe traumatic brain injury.194 Another similar-size series in adolescents and adults illustrates an algorithm for management of such patients.195 A pediatric series of 13 children at an acute care hospital with traumatic brain injury who were investigated for oral-motor function, swallowing, and cognition had restoration of normal status in all three functions at an average of 12 weeks (range, 3–11 weeks) postinjury, suggesting milder injuries than the adolescent-adult series above.196 A large series of 1145 children consecutively admitted to an acute care setting for traumatic brain injury during a 5-year period highlights the epidemiology, characteristics, and outcomes of dysphagia among such children.197 Dysphagia incidence was 5% overall, distributed by severity level of the head injury: 68% for severe injury, 15% for moderate injury, and 1% for mild injury. Particular predictors of dysphagia were Glasgow Coma Scale score <8.5 and mechanical ventilation >1.5 days. The children with dysphagia were statistically more likely to have prolongation of inpatient stay and of mechanical ventilation, worsened coma scores and CT classification, and longer durations of speech therapy and various measures of resumption of oral feedings.
Tracheotomy
As suggested above, tracheotomy may independently produce dysphagia. A study in 36 infants undergoing tracheotomy before a year of age for indications including severe upper airway obstruction (n = 25), requirement for prolonged mechanical ventilation (n = 10), or requirement for intensive trachobroncheal suction (n = 1) detected no perioperative complications. However, swallowing ability deteriorated in nearly all infants and speech development was seriously delayed in 38%.46
Videofluoroscopy disclosed a number of abnormalities in four children (aged 14–33 months) with long-term tracheostomies compared to a similarly aged child without a tracheostomy.198 Laryngeal vestibule closure was delayed until after the onset of upper esophageal sphincter opening in the tracheotomized patients, and produced laryngeal penetration. Probably as a direct result of the fixation of the upper airway in the neck by the tracheotomy, the patients did not demonstrate the normal upward excursion of the arytenoids and epiglottis during swallowing. Delayed swallow occurred 45% of the time, and was associated with laryngeal penetration. Pharyngeal dysmotility did not occur, however.
Other Iatrogenic Trauma to the Larynx and Pharynx
The use of transesophageal echocardiography as well as long-term airway intubation during cardiovascular surgery produced swallowing abnormalities in a number of children as well as adults. Some of these children developed frank strictures, but others displayed only functional swallowing abnormalities. A series of 22 such children and adults (ages 4–89 years) referred for videoradiography during a 7-year period found abnormalities in 18 (82%), with a mean of nearly four abnormalities per patient (range, one to eight abnormalities). These abnormalities most commonly involved the hyoid and larynx (13 patients, 59%) and the pharynx (10 patients, 45%). Thirteen patients (59%) aspirated: one predeglutitive, four intradeglutitive, three postdeglutitive, and five mixed. Fourteen had undergone transesophageal echocardiography, long-term intubation, or both, and in these patients incomplete epiglottic tilting, pharyngeal weakness, and postdeglutitive aspiration were often observed.199
Differential Diagnosis
The differential diagnosis of oropharyngeal dysmotility includes structural obstructions (malformations, foreign bodies, congenital webs, extrinsic compressions) or local inflammations causing dysphagia. It may also include psychological conditions such as globus hystericus,200 but detailed investigation may be required to ensure the absence of subtle dysmotility. The clinician who considers these disorders usually can readily exclude most of them.
When the presenting symptom is an airway manifestation, the clinician must consider structural, nondysmotility causes of aspiration, such as laryngotracheal clefts and H-type tracheoesophageal fistulas. Airway manifestations also prompt consideration of cystic fibrosis, intrinsic or allergic asthma, or immunodeficiencies causing repeated infections.
Esophageal and Lower Esophageal Sphincter Motility Disorders (Smooth Muscle)
Primary Esophageal Motor Disorders
Achalasia is the most common primary esophageal motility disorder in children.13 Recent reviews and descriptions of sizable pediatric series portray the range of this disease as it manifests in the child.201, 202, 203, 204 In addition to appearing as isolated primary disease, it may present as part of various syndromes or in association with other diseases.201, 204, 205, 206, 207 Achalasia typically appears in older children with dysphagia as the predominant symptom; when it occurs in younger children, vomiting (regurgitation) is often the primary symptom. Diagnosis may be suspected on plain radiographs or barium studies, as indicated above. Manometric hallmarks include high-pressure and incompletely relaxing lower esophageal sphincter, esophageal peristaltic failure, and elevation of intraesophageal pressure. Typical peristaltic abnormalities include low-pressure simultaneous waves, but occasional patients with "vigorous achalasia" manifest high-pressure simultaneous waves early in the disease. The most definitive treatment for achalasia in children, as in adults, is myotomy201, 208, 209; myotomy may be performed using minimally invasive techniques210 and should generally be accompanied by fundoplication to prevent complications of gastroesophageal reflux through the newly incompetent sphincter.211 Esophageal dilations provide long-term relief in about half of children; dilations can be performed via pneumatic or hydrostatic techniques, and with endoscopic and/or fluoroscopic guidance, including via through-the-scope balloons.212, 213, 214 For temporary relief, or in children who are not candidates for the more invasive procedures, nifedipine may be used. Intrasphincteric injections of botulinum toxin produce 3 to 6 months of relief of symptoms in nonsurgical candidates or in the occasional child with a failed myotomy.132, 133, 201 For comparisons of these modalities and consideration of cost-effectiveness, adult reviews must be consulted.134, 135, 215 Long-term effectiveness of myotomy is generally superior to either of the other treatments, and factors responsible for treatment failure and recurrence have been identified in adult series.216, 217, 218 The issue of esophageal cancer as one long-term complication of achalasia has particular relevance to pediatric patients, as their youth provides a longer potential exposure to carcinogenic influences.219
The other primary esophageal motor disorders include diffuse esophageal spasm (simultaneous waves), nutcracker esophagus [high-pressure prolonged-duration waves (>180 mmHg and > 6 seconds) with normal progression], and nonspecific esophageal motility disorder.33 Children with chest pain but without esophagitis or cardiac disease are diagnosed using manometry, and treatments have included nitrates and calcium channel blockers, but with variable success. The pediatric presentations and management have not been thoroughly reviewed recently; for management of these disorders, adult publications provide useful information.
Secondary Esophageal Motor Disorders
The most important secondary esophageal motor disorders in children—indeed, currently among the most commonly diagnosed pediatric gastrointestinal disorders overall—are due to two inflammatory conditions that were not well distinguished until recently: gastroesophageal reflux disease and eosinophilic esophagitis.
Gastroesophageal reflux disease is the product of esophageal dysmotility: increased transient lower esophageal sphincter relaxations. In turn, it may promote motility disorders in the inflamed esophagus that further impair esophageal clearance and contribute to vicious cycles of worsening reflux.
About one third of adults with reflux disease manifest esophageal dysmotility.220 The proportion of children who do so is unknown. Of 89 adults with reflux symptoms (65% with endoscopic esophagitis) who underwent testing with manometry and pH-metry, more than half had nonspecific esophageal motility disorder (nearly all "ineffective esophageal motility"–distal esophageal peristaltic pressures <30 mmHg or <70% of contractions transmitted64).221 Although the incidence of esophagitis was similar to that in the group with normal motility, pH-metry disclosed significantly prolonged acid clearance in those with ineffective esophageal motility. This may explain the symptom of dysphagia, present in 37% of 11,945 adults with erosive esophagitis, more frequent in those with worse esophagitis endoscopically.222 This dysphagia resolved in 83% after 4 weeks of proton pump inhibitor therapy; the 17% with persisting dysphagia had a significantly decreased rate of endoscopic healing (72% vs. 90%). In a study of 147 adults with gastroesophageal reflux disease (GERD), prolonged reflux symptoms, severe esophagitis, and Barrett's esophagus were associated with dysphagia, decreased lower esophageal sphincter pressure, decreased amplitude of esophageal peristalsis throughout the esophagus, and delayed esophageal transit.223 Although other authors have disputed the association of ineffective esophageal motility with GERD,224 their analyses are likely faulty.225 A very recent study using 24-hour ambulatory motility during pH-metry in 24 children being investigated for GERD showed decreased and defective peristalsis during acid reflux even though prior routine manometry had been normal.62
In contrast to the low peristaltic pressures in ineffective esophageal motility that is frequently associated with chronic reflux esophagitis, high-amplitude peristaltic contractions ( 150 mmHg) and elevated lower esophageal sphincter pressure (
150 mmHg) and elevated lower esophageal sphincter pressure ( 45 mmHg) were found in a minority (<3%) of patients with reflux esophagitis submitted to fundoplication surgery.226 Further, in 100 adults with airway manifestations of reflux who underwent motility studies, 29% had normal motility and 48% had ineffective esophageal motility, but 10% had hypertensive lower esophageal sphincter, 9% had nutcracker esophagus, and 4% had achalasia.227 Thus, 73% had esophageal dysmotility, with high peristaltic or sphincter pressure in nearly a third of them. Others have also suggested a relationship between nutcracker esophagus and reflux disease.228, 229 Indeed, a review of 402 motility studies for chest pain showed 10% with nutcracker esophagus, at least a third of whom had reflux esophagitis, 83% of those responding to antireflux therapy with improvement of symptoms, though only a minority normalized manometry findings.230 Similarly, the manometric findings of primary diffuse esophageal spasm overlap with those secondary to reflux disease.231
45 mmHg) were found in a minority (<3%) of patients with reflux esophagitis submitted to fundoplication surgery.226 Further, in 100 adults with airway manifestations of reflux who underwent motility studies, 29% had normal motility and 48% had ineffective esophageal motility, but 10% had hypertensive lower esophageal sphincter, 9% had nutcracker esophagus, and 4% had achalasia.227 Thus, 73% had esophageal dysmotility, with high peristaltic or sphincter pressure in nearly a third of them. Others have also suggested a relationship between nutcracker esophagus and reflux disease.228, 229 Indeed, a review of 402 motility studies for chest pain showed 10% with nutcracker esophagus, at least a third of whom had reflux esophagitis, 83% of those responding to antireflux therapy with improvement of symptoms, though only a minority normalized manometry findings.230 Similarly, the manometric findings of primary diffuse esophageal spasm overlap with those secondary to reflux disease.231
Pediatric studies of dysmotility in reflux disease are few. Among 79 children with chest pain (ages 7–16 years), 31 with mild-to-moderate esophagitis did not differ in manometry findings from 48 children without esophagitis232; however, in 11 children with severe esophagitis, low-amplitude, broad-based, double-peaked, simultaneous waves were common, and normalized when the esophagitis was cleared.233 In nine children with reflux esophagitis, peristaltic and lower esophageal sphincter pressures were significantly reduced, and contraction durations increased, compared to nine controls and 15 with reflux but no esophagitis.234 In 60 children with reflux disease, LES pressure, and wave amplitude and propagation were decreased compared to controls.235 In two young infants, hypomotility, including aperistalsis and simultaneous low-amplitude waves, was associated with reflux esophagitis, but resolved with therapy.236
In three of 19 children presenting with chest pain, esophagitis, and normal unstimulated motility studies, esophageal acid perfusion induced significantly increased esophageal peristaltic amplitude and duration in conjunction with chest pain.237 Similar findings (increased wave pressure, duration, and velocity, and the occurrence of double-peaked and simultaneous waves) may occur during acid infusion in adults without erosive esophagitis.60, 238
If reflux esophagitis and distal esophageal dysmotility are associated, which is primary? Do patients have primary motility disorders, allowing reflux that subsequently produces esophagitis, or does primary reflux induce esophagitis that in turn causes the dysmotility?
Animal studies of acute experimental esophagitis have produced similar dysmotility, which resolved with recovery of the acute esophagitis, thus suggesting that the esophagitis caused the dysmotility.220
However, studies examining the relationship in humans, via aggressive therapy of reflux disease, have had difficulty showing similar improvements in dysmotility, with some reports asserting improvements239, 240, 241 and others denying them.242, 243 A pediatric study in 14 children undergoing fundoplication found failure of normalization of abnormal peristalsis several months after fundoplication.244 A later pediatric surgical study also found persistence of esophageal motor dysfunction after surgical cure of reflux.245 Investigators performed a large, prospective, randomized clinical and manometric study before and after fundoplication in 200 adult patients.246 Half of their study patients (though about a third of their referred patients) had ineffective esophageal motility: mean distal esophageal peristaltic pressures <40 mmHg and/or <40% of contractions transmitted, a fairly high threshold for this diagnosis. Of the patients with dysmotility, similar proportions worsened and improved their motility months following fundoplication (regardless of the type of fundoplication to which they had been randomized). Interestingly, a considerable minority of the patients with normal preoperative peristalsis developed decreased peristaltic transmission following surgery. The failure of such well-done human studies to show improvement in dysmotility after therapy for chronic reflux may be attributable to the induction of permanent changes in motility by fibrosing esophageal damage in chronic reflux disease.220 Once present, esophageal dysmotility, particularly that which impairs clearance, can clearly participate in worsening reflux esophagitis.
The literature thus suggests that acute acid exposure of the esophagus, perhaps primed by (nonerosive) esophagitis, may induce hypercontractile dysmotility and chest pain. It also suggests that chronic acid exposure with more severe esophagitis may induce hypocontractile dysmotility that predisposes to vicious cycles of further acid damage to the esophagus. It suggests, though does not prove, that early in the course of the induction of hypomotility, the damage may be reversible, but that in more severe or prolonged cases it is not reversible.
Diagnosis and treatment of pediatric gastroesophageal reflux disease are beyond the scope of this chapter, but are detailed elsewhere.247 Prokinetic agents have found a larger role in young children than in adolescents and adults, in whom acid suppression plays the primary role, but currently there is little rigorous evidence for marked utility of any of the available prokinetic agents.
Reflux esophagitis may also produce nondysmotility dysphagia via the induction of fibrosing strictures, important to consider in the differential diagnosis. In addition, fundoplication therapy for GERD may itself produce dysphagia, particularly in the immediate postoperative period, related to obstruction by the wrap.248
Eosinophilic esophagitis is the other important secondary esophageal motility disorder in children, although the details by which it causes esophageal dysfunction remain unclear. This disorder affects young males disproportionately, and a considerable fraction of the patients have demonstrable food allergies.249 Severe eosinophilic esophagitis may cause esophageal obstruction via actual stricture formation, and some patients manifest a Schatzki ring, or thickened esophageal wall mildly narrowing the lumen diffusely.38, 250, 251, 252 Frequently, however, no mechanical obstruction is evident, but patients often present with dysphagia or impactions out of proportion to endoscopically visible abnormalities.38 Manometric studies, infrequently performed, have not clarified the motor abnormalities that provoke the dysphagia and impactions.252 A possible explanation for the normal manometry studies despite prominent dysphagia and impactions is that they have generally not been done during food provocation. Supporting this concept, an adolescent boy who had chest pain occurring within a few minutes of eating green peppers or onions displayed a normal unprovoked manometry, but high-pressure spasmodic contractions occurred immediately following provocation with the offending food.61 This young man unfortunately did not undergo endoscopy, so that the suspicion that his chest pain was due to eosinophilic esophagitis goes unanswered. Seven adults whose subepithelial esophageal tissue was able to be examined between 1 and 12 years after diagnosis of eosinophilic esophagitis had developed impressive fibrosis of the esophageal lamina propria.253 Hypothetically, in parallel to reflux esophagitis, temporary esophageal motility abnormalities may be produced by acute exposure to the aggravating stimulus, whereas chronic exposure may induce permanent changes mediated by fibrosis.
Diagnosis and treatment of eosinophilic esophagitis are also beyond the scope of this chapter, but it should be considered in young (especially male) individuals with reflux-like symptoms, particularly chest pain and obstructive symptoms, and especially in those with a family or personal history of atopy.247, 254, 255, 256, 257
Other esophageal inflammatory or infiltrative conditions may affect motility in children and therefore may produce dysphagia independently or worsen dysphagia associated with gastroesophageal reflux. In addition to acid reflux and eosinophilic inflammation, such causes of esophageal inflammatory dysmotility are caustic ingestions, chronic indwelling nasogastric tubes, chemotherapy or radiation therapy,258 graft versus host disease, sclerotherapy,259 Crohn's disease,260 chronic granulomatous disease,261 and cystinosis.262Infectious causes of esophageal dysmotility include Chagas' disease.263
Connective tissue diseases including scleroderma, mixed connective tissue disease, and systemic lupus erythematosus may induce hypotonic LES pressure and abnormal peristalsis in the smooth muscle esophagus.264, 265, 266 In addition to effects on the oropharynx and upper esophagus, polymyositis has been reported to cause decreased amplitude peristalsis in the smooth muscle esophagus.267 A scleroderma-like esophageal dysfunction producing distal esophageal hypoperistalsis and LES hypotonia was reported in six of eight children breast-fed by mothers with silicone breast implants.12, 268 The abnormalities did not occur in bottle-fed infants from mothers with implants, nor in a control group.
Endocrine disorders including diabetes and hypothyroidism may cause esophageal dysmotility.165, 269, 270
Esophageal dysmotility may accompany the diffuse gastrointestinal dysmotility of idiopathic chronic intestinal pseudo obstruction.271
Esophageal atresia, with or without tracheoesophageal fistula, is a relatively common congenital esophageal malformation that includes intrinsic dysmotility in the distal esophageal segment; this dysmotility participates in worsening cycles of reflux disease, and may be exacerbated by anastomotic strictures.272, 273, 274, 275, 276, 277, 278, 279, 280 Clinicians must manage dysphagia and reflux aggressively to prevent the recurrent aspiration that may otherwise complicate the airway disease that these children suffer because of their primary airway malformations.
Hirschsprung disease generally affects the distal bowel, but esophageal dysmotility may accompany the intestinal dysmotility in some children.281
Pierre Robin syndrome, retrognathia with glossoptosis and cleft palate, produced esophageal manometric abnormalities in 50% of children examined. Of 35 unselected children with Pierre Robin syndrome (isolated, 27, or associated with Stickler syndrome, eight), all had feeding disorders and 86% had required nasogastric tube feeding for a mean duration of 8.6 months. The manometric abnormalities included LES hypertonia, failure of LES relaxation at deglutition, and esophageal dyskinesia. The clinical and manometric disorders tended to regress spontaneously after 12 months.282
Conclusion
Pediatric motility disorders of the mouth, pharynx, and esophagus are exceedingly important because of the potential duration of disability if they are uncorrected and because of their interactions with developmental feeding, airway, and speech functions.
As with most aspects of pediatric disease, however, rigorous study of the pathophysiology, pharmacotherapy, and other aspects of management has lagged somewhat behind studies in adults. Although there are considerable limits to our current understanding of adult motility disorders, the limits are greater in children. Few rigorous trials adequately address the management options for these diseases in children, even more so than is true for many adult motility disorders.104 The patients are fragile and vulnerable, and often limited in number; they are less cooperative and require smaller and more variable-sized equipment because of their small and variable sizes. Nonetheless, a great deal is now understood about oropharyngoesophageal motor disorders in children. Much remains to be discovered about these disorders, as well.



