Abstract
Objectives:
Currently, effective therapeutic strategy for spinal cord injury (SCI) is not clinically available. To establish a better method that may help repair the injured spinal cord, sodium hyaluronate-ciliary neurotrophic factor (CNTF) gelatinous particles were generated.
Methods:
A segment of spinal cord tissue was excised to form a 2.5-mm-long cavity at thoracic level in an adult rat, and sodium hyaluronate-CNTF gelatinous particles were implanted into the lesion cavity. The recovery of the injured spinal cord was evaluated by immunohistochemistry, nerve tracing, electrophysiological test and Basso–Beattie–Bresnahan locomotor rating scale.
Results:
Open-field locomotion of the sodium hyaluronate-CNTF rats was significantly enhanced up to 12 weeks postoperation. Together with the evidence of enhanced cortical motor evoked potentials and cortical somatosensory evoked potentials in the sodium hyaluronate-CNTF group, these findings suggested a powerful functional recovery component. Immunohistochemical analyses suggested that the functional recovery might be attributable partly to an increase in axonal regrowth as well as in replenishment of β-tubulin-III–positive neuron-like cells.
Conclusion:
Sodium hyaluronate-CNTF gelatinous particles may provide an effective method for treating SCI.
Similar content being viewed by others
Introduction
After spinal cord injury (SCI), axonal regeneration is impeded by myelin-associated inhibitors, scar barriers, loss in the intrinsic ability for adult neurons to overcome inhibitory cues and lack of neurotrophic factors.1 However, if inhibitory factors can be removed, axons may regrow in unscarred lesion area.2 Thus multiple manipulations are essential to re-establish a better microenvironment suitable for axonal regeneration after SCI.
Many methods have been tried to repair SCI, such as transplantation of stem cells, Schwann cells, olfactory ensheathing cells and peripheral nerves, knocking out of genes encoding Nogo-A/B and local supply of neurotrophic factors by transplantation of gene-modified cells.1, 3, 4 However, the above-mentioned approaches involve risks for clinical application, such as immunological rejection, causing tumor, a low survival rate of transplanted cells, damage to the donors of peripheral nerves and the potential dangers in genetic manipulation of host tissues. Application of exogenous trophic factors has been extensively studied, as they modulate axonal growth, neuronal survival, synaptic plasticity and neurotransmission.1, 4, 5, 6, 7 Ciliary neurotrophic factor (CNTF) is part of a cytokine family. Previous studies have revealed that it could prevent the degeneration or loss of axotomized motor neurons, promote the differentiation of developing sympathetic precursors and also exhibit survival effects on preganglionic sympathetic neurons, embryonic motor neurons and sensory neurons.6, 7 Dramatic changes in the level of expression of CNTF following injuries in the central nervous system and peripheral nervous system indicate that CNTF may be a key factor in the injury response in the nervous system.6 However, local injection of CNTF may result in rapid diffusion, increasing side effects and cost. Use of an osmotic pump requires a second surgery for removal. In this study, we have attempted to introduce CNTF into degradable sodium hyaluronate gelatinous particles to capture the sustained, local release of CNTF. We report here the beneficial outcomes of this approach.
Materials and methods
Fabrication of sodium hyaluronate-CNTF gelatinous particles
Under sterile conditions, 200 Da sodium hyaluronate was dissolved in 0.5% sodium hydroxide aqueous solution, and then vinylcyclohexane (5wt %) was added. After stirring for 6–8 h at 25 °C, the gelatin block was added to deionized water and allowed to swell for 6 h at 25 °C. The swollen gelatin block was washed with phosphate-buffered saline totally for 12 h. After 100-mesh sieve filtration, the sodium hyaluronate gelatinous particles were prepared either with or without (control) CNTF protein. For the type of containing CNTF, 1 mg sodium hyaluronate gelatinous particles and 15 μg CNTF were dissolved in 100 ml phosphate-buffered saline. Then the sodium hyaluronate gelatinous particles were vacuum cooled, dried and stored at 4 °C for use.
Animal surgery and care
Adult female Wistar rats, each weighing 200–250 g, were anesthetized by intraperitoneal injection of 6% chloral hydrate (0.6 ml per 100 g body weight). A dorsal laminectomy was performed at T8-T9 to expose the spinal cord. A segment of spinal cord tissue was excised to form a 2.5-mm-long cavity, and any residual fiber at the lesion site was removed by aspiration. All the rats were divided into four groups. For the sodium hyaluronate-CNTF gelatinous particles group (sodium hyaluronate-CNTF group, n=30), sodium hyaluronate gelatinous particles group (sodium hyaluronate group, n=27), CNTF group (CNTF group, n=27) and lesion-control group (lesion-control group, n=25), 3.6 μg of sodium hyaluronate-CNTF gelatinous particles, 3.6 μg of sodium hyaluronate gelatinous particles, 50 ng of CNTF (the same amount of CNTF as contained in 3.6 μg of sodium hyaluronate-CNTF gelatinous particles) and nothing were implanted into the lesion cavities, respectively. The bladder was massaged twice daily until bladder function recovered postoperation (PO).
5-Bromo-2-deoxyuridine (BrdU, 50 mg kg−1 body weight, Sigma, St Louis, MO, USA) was intraperitoneally injected once every 12 h, totaling eight injections PO.
Five rats were randomly chosen from each group 105 days PO. After anesthesia, the original surgical site was exposed, and the regenerated spinal tissue was completely re-cut under an operation microscope (M-690, Leica, Solms, Germany).
The above experimental procedures were approved by the Experimental Animal Center and Animal Care Committee, Capital University of Medical Sciences (Beijing, China).
Tissue processing, immunohistochemistry and quantitative analysis
After anesthesia, rats were transcardially perfused with 4% paraformaldehyde. Spinal cords were postfixed in 4% paraformaldehyde at 4 °C for 6–8 h and then stored in 30% sucrose. Spinal cord was sagittally sectioned at 10 μm with a Leica 1850 cryostat (CM-1850, Leica). Spinal cord sections were incubated in the following primary antibodies (Ab) at 4 °C for 48 h: mouse anti-neurofilament (Pan) monoclonal Ab (NF, 1:50, Zymed Laboratories, South San Francisco, CA, USA); rabbit anti-β-tubulin-III protein polyclonal Ab (β-tubulin-III, 1:100, Sigma); rabbit anti-glial fibrillary acidic protein polyclonal Ab (1:150, Zymed Laboratories); mouse anti-BrdU monoclonal Ab (1:70, Bioss, Woburn, MA, USA); and rabbit anti-doublecortin protein polyclonal Ab (DCX, 1:100, Abcam, Cambridge, MA, USA). After washing thrice in 0.01 M phosphate-buffered saline, the sections were incubated with Texas Red-conjugated goat anti-mouse Ab (1:100, Jackson, West Grove, PA, USA), Cy2-conjugated goat anti-rabbit Ab (1:100, Jackson), Alexa Fluor 546-conjugated donkey anti-rabbit Ab (1:100, Invitrogen, Carlsbad, CA, USA) or Alexa Fluor 488-conjugated donkey anti-mouse Ab (1:100, Invitrogen) for 8 h at room temperature. Fluorescent visualization was performed under a fluorescence microscope (BX-51, Olympus, Tokyo, Japan).
The spinal cord lesion area of the longitudinal section was divided into three regions based on locations (Figure 2c). Four rats of each group were used for quantitation, and five longitudinal sections (10-μm thick) were chosen in series (1 of 10) per rat to count the NF- and β-tubulin-III–positive fibers in the rostral, middle and caudal segments of the lesion area (Figure 2c). Only those nerve fibers longer than 40 μm were counted.
Quantitation of NF- and β-tubulin-III-positive neuronal fibers in the lesion area at 2 months PO. (a, b) Macroscopic images of the dorsal surfaces of the lesion-control (a) and sodium hyaluronate-CNTF (b) cords at 2 months PO. The lesion area of the lesion-control cord was filled with glial scar-like tissue; however, the lesion area of the sodium hyaluronate-CNTF cord was filled with smooth-surfaced and translucent tissue. The 2.5-mm-long lesion area is indicated by asterisk (*). C, caudal; R, rostral. (c) Nissl staining of the sodium hyaluronate-CNTF cord showed that the complete resection operation had made no neural residue left in the lesion area. The sodium hyaluronate-CNTF gelatinous particles are indicated by asterisk (*). The schematics above illustrate that the lesion area was divided into three regions based on locations for quantitative analysis. Rostral/caudal analysis was done within 0.9 mm extending from the rostral/caudal host–lesion interface into the lesion. Middle analysis was done within the middle 0.7 mm between the rostral and the caudal segments. C, caudal; R, rostral. (d, e) Quantitation of NF- (d) and β-tubulin-III–positive (e) neuronal fibers in the rostral, middle and caudal segments of the lesion area at 2 months PO. Asterisk (*), significant difference compared with lesion-control. It can be seen that the sodium hyaluronate-CNTF rats had more regenerating neuronal fibers compared with the lesion-control condition. Statistical analysis was done by ANOVA. Error bars represent±2 s.es. Scale bars: a and b, 2 mm; c, 200 μm.
Anterograde corticospinal tract labeling
Some animals were randomly chosen and the anterograde tracer biotinylated dextran amine conjugated with fluorescein (BDA–fluorescein, Molecular Probes, 10% w/v solution, Eugene, OR, USA) was injected into seven sites (0.4 μl per site) of the rat’s hindlimb sensorimotor cortex with a Hamilton syringe (7001KH, Hamilton, Bonaduz, Switzerland).8 Animals were transcardially perfused 2 weeks later, and serial longitudinal sections (35-μm thick) of the spinal cord were sectioned with a cryostat.
Electrophysiological assessment
Rats were anesthetized by intramuscular injection of ketamine (50 mg kg−1 body weight). Cortical motor evoked potential (cMEP) and cortical somatosensory evoked potential (cSEP) were both tested by using stimulating electrodes with a Keypoint-II bichannel evoked potential/electromyography (Dantec Company, Copenhagen, Denmark). When cMEP was tested, the positive electrode was inserted into the skull surface above the motor cortex,8 using a signal at stimulating intensity of 10 mA. cMEP was recorded from the middle of the contralateral tibialis anterior muscle. When cSEP was tested, the positive electrode was inserted into the middle of the tibialis anterior muscle, using successive signals at stimulating intensity of 3 mA, duration time of 0.2 ms, amplifier sensitivity of 10 μV D−1, filter pass band of 20 Hz–3 kHz and 200 times on average. cSEP was recorded from the skull surface above the contralateral somatosensory cortex.9 The onset latency was measured as the length of time between the presentation of the stimulus and the onset of the first wave. The amplitude was measured as the distance from the P1 wave peak to the adjacent N1 wave peak (P1–N1).
Behavioral testing
Open-field locomotion was evaluated by using the 21-point Basso–Beattie–Bresnahan (BBB) Locomotor Rating Scale.10 All tests were performed in a double-blind manner. In each testing session, the animals were observed individually for 4 min by two observers.
Statistical analyses
One-way analysis of variance (ANOVA) and least significant difference (LSD, equal variances assumed) or Dunnett’s (equal variances not assumed) post hoc test were performed for multiple group comparisons. Statistically significant difference in two parameters was determined by two-tailed Student’s t-test.
Results
Axonal growth in the lesion area
The sodium hyaluronate-CNTF gelatinous particles had significantly promoted the expression of neuron-specific intermediate filaments of neurofilament Pan (NF) and β-tubulin-III in the injured spinal cord. In the rostral segment of the lesion area, the numbers of NF- and β-tubulin-III–positive neuronal fibers in the sodium hyaluronate-CNTF groups were 2.9- and 3.2-fold greater compared with the lesion-control condition at 2 months PO, respectively (Student’s t-test, P=0.000, P=0.001, Figures 1a, d, e, h and 2d–e); in the caudal segment of the lesion area, the numbers of NF- and β-tubulin-III–positive neuronal fibers in the sodium hyaluronate-CNTF group were 2.5- and 3-fold greater compared with the lesion-control condition, respectively (Student’s t-test, P=0.005, P=0.000, Figures 2d–e). The sodium hyaluronate-CNTF group also showed greater NF-positive neuronal fiber counts compared with the sodium hyaluronate and CNTF groups in the rostral and caudal segments by 1.8, 1.9, 1.2 and 1.4, respectively (ANOVA, LSD, rostral: P=0.017, P=0.302; caudal: P=0.001, P=0.041, Figures 1b–d and 2d). NF-positive fibers represented mature neuronal fibers, and β-tubulin-III–positive fibers not only contained mature neuronal fibers but also some of the developing immature neuronal fibers. At 2 months PO, no NF-positive mature fiber was observed in the center of the lesion area for all groups (data not shown); however, β-tubulin-III–positive fibers could be observed in the middle segment of the lesion area for the sodium hyaluronate-CNTF and sodium hyaluronate groups (Figures 1j and l). Compared with lesion control, the sodium hyaluronate-CNTF and sodium hyaluronate conditions significantly increased the numbers of β-tubulin-III–positive neuronal fibers in the middle segment of the lesion area by 13.33 and 6.25, respectively (ANOVA, LSD, P=0.000, P=0.000, Figures 1i–l and 2e); there were 2.1-fold more β-tubulin-III–positive neuronal fibers for the sodium hyaluronate-CNTF compared with sodium hyaluronate group (ANOVA, LSD, P=0.000, Figures 1j, l and 2e). Even at 1 month PO, a small number of β-tubulin-III–positive neuronal fibers could be observed in the center of the lesion area in the sodium hyaluronate-CNTF group (Figures 3a and b). The sodium hyaluronate biomaterial blocked the invasion of astrocytes into the lesion area (Figure 3c), which was responsible for the formation of glial scar. This may be one of the reasons for biomaterial implantation to promote axon regrowth in the lesion area.
Images of regenerating NF-positive fibers in the rostral segment and β-tubulin-III–positive fibers in the rostral and middle segments of the lesion area at 2 months PO. These longitudinal sections showed that there were more regenerating fibers in the sodium hyaluronate-CNTF group than other groups. The symbol # indicates the position of cyst. Asterisk (*) indicates the sodium hyaluronate gelatinous particle. The dotted lines indicate the boundary between the host and lesion area. The left of dotted lines is the lesion area. Scale bars: 100 μm.
Regenerating β-tubulin-III–positive neuronal fibers in the middle segment of the lesion area and glial fibrillary acidic protein (GFAP) immunofluorescent staining. (a) At 1 month PO in the sodium hyaluronate-CNTF group, several regenerating β-tubulin-III–positive neuronal fibers could be observed in the middle of the lesion area. (b) High magnification of the boxed area in panel (a). (c) At 1 month PO in the sodium hyaluronate-CNTF group, a large number of GFAP-positive cells and fibers were blocked outside the lesion area. C, caudal; R, rostral. The dotted lines indicate the boundary between the host and the lesion area. Scale bars: (a and c), 200 μm; (b), 100 μm.
By BDA tracing of the corticospinal tract, the four groups showed positive BDA tracing in the rostral but not in the middle and caudal segments of the lesion area (data not shown), suggesting that regenerating corticospinal tract fibers have not yet traversed the injury epicenter and into the caudal segment of the lesion area until 90 days PO.
Production of β-tubulin-III–positive neuron-like cells
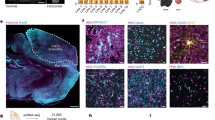
At 1 month PO in the sodium hyaluronate-CNTF group, many β-tubulin-III–positive cells were observed at the lesion edge of the host cord and in the lesion area (Figures 4a–d and 5a), which were not detectable in other groups (Figure 5b). These β-tubulin-III–positive cells varied in size from 14 to 30 μm, and typical neuronal morphological characters, for example, multiple processes and cell contacts, could be observed in these cells (Figures 4a–d and 5a). The β-tubulin-III–positive cells were also immunoreactive for NeuN (Figure 4b), thus called neuron-like cells here. On average, 37±6 β-tubulin-III–positive neuron-like cells were found in the sodium hyaluronate-CNTF group.
The β-tubulin-III–positive neuron-like cells and the differentiation of endogenous progenitors in the sodium hyaluronate-CNTF group. (a) At 1 month PO in the sodium hyaluronate-CNTF group, many small and process-extending β-tubulin-III–positive neuron-like cells (shown by white arrows) were observed at the lesion edge of the host cord. (b) The β-tubulin-III–positive neuron-like cells were immunoreactive for NeuN (shown by white arrows). (c) At 1 month PO in the sodium hyaluronate-CNTF group, the β-tubulin-III–positive neuron-like cells (shown by white arrows) were detectable in the lesion area. (d) High magnification of the boxed area in panel (c). The β-tubulin-III–positive neuronal fiber (shown by white arrowhead) extended and the β-tubulin-III–positive neuron-like cell seemed to form cell contacts (shown by white arrow). (e–h) At 4 days PO in the sodium hyaluronate-CNTF group, BrdU (red) and DCX (green) double-positive cells were observed at the lesion edge of the host cord, with neuron-like appearance. The cells directed by white arrows in panel (g) are shown in panel (h). (i–l) At 11 days PO in the sodium hyaluronate-CNTF group, BrdU (red) and β-tubulin-III (green) double-positive cells were observed in the lesion area. The cell directed by the white arrow in panel (k) is shown in panel (l). The dotted lines indicate the boundary between the host and lesion area. Scale bars: (a, e–g), 100 μm; (b, c and h), 50 μm; d, 25 μm; (i–k), 75 μm. A full color version of this figure is available at the Spinal Cord journal online.
The β-tubulin-III–positive neuron-like cells at the lesion edge of the host cord and in the lesion area. (a) Longitudinal section of the spinal cord of the sodium hyaluronate-CNTF group at 1 month PO, showing β-tubulin-III–positive neuron-like cells at the lesion edge of the host cord and in the lesion area. The β-tubulin-III–positive neuron-like cells are shown by white arrows, which were different from the normal β-tubulin-III–positive neurons (shown by white arrowheads) in the morphology and distribution. The dotted lines indicate the boundary between the host and lesion area. (b) At 1 month PO in the lesion-control group, the β-tubulin-III–positive neuron-like cell was not observed at the lesion edge of the host cord or in the lesion area. The dotted lines indicate the boundary between the host and lesion area. Scale bars: (a and b), 100 μm.
To address the question of whether β-tubulin-III–positive neuron-like cells were newly produced owing to the proliferation and differentiation of endogenous neural progenitors, BrdU was used to label the proliferating cells after operation. BrdU and DCX (a marker of migrating neural precursor) double-positive cells were observed at the lesion edge of the host cord at 4 days PO in the sodium hyaluronate-CNTF group (Figures 4e–h); BrdU and β-tubulin-III double-positive cells were also detectable at 11 days PO (Figures 4i–l), suggesting the differentiation of newborn cells toward a neuronal fate. These results implied that endogenous neurogenesis could be induced in severely injured spinal cord following implantation of the sodium hyaluronate-CNTF gelatinous particles.
Improvement of electrophysiological function
At 98 days PO, cMEPs and cSEPs were detected in most of the sodium hyaluronate-CNTF rats (5 of 6 rats) (Figures 6c–f), but none was recorded from the lesion-control, sodium hyaluronate and CNTF rats (0 of 20 rats) (Figures 6g and h). The result indicated that sodium hyaluronate-CNTF gelatinous particles had enhanced electrical signal conduction of the injured spinal cord. The onset latency and amplitude (P1–N1) of cMEPs at 98 days PO were 11.61±2.75 ms and 227.28±108.39 μV (Figure 6e), respectively, the onset latency delaying by 89% and the amplitude (P1–N1) decreasing by 99% compared with the normal values of cMEPs (6.15±0.39 ms, 20.67±8.51 mV, Figure 6a); the two groups showed significant difference (Student’s t-test, P=0.001, P=0.012). The onset latency and amplitude (P1–N1) of cSEPs recovered to 11.94±0.69 ms and 5.26±1.35 μV at 98 days PO (Figure 6f), respectively, the onset latency delaying by 69% and the amplitude (P1–N1) decreasing by 67% compared with the normal values of cSEPs (7.08±1.06 ms, 15.78±4.14 μV, Figure 6b); the two groups showed significant difference (Student’s t-test, P=0.000, P=0.000). The onset latencies of cMEPs and cSEPs at 98 days PO were significantly shorter than those at 50 days PO (15.21±1.89 ms, 18.83±4.46 ms, Figures 6c and d; Student’s t-test, P=0.009, P=0.003), and the amplitudes (P1–N1) showed no statistical difference (Student’s t-test, P=0.399, P=0.668). Electrophysiological recording was performed again at 3 days postrelesioning in the sodium hyaluronate-CNTF rats, and cMEPs and cSEPs could no longer be elicited.
CMEPs and cSEPs of the sodium hyaluronate-CNTF rats. Representative examples of cMEPs and cSEPs were shown for the normal (a, b), sodium hyaluronate-CNTF (50 and 98 days PO, c-f) and lesion-control rats (98 days PO, g, h). The sodium hyaluronate-CNTF rats recovered their typical waveform appearances 50 and 98 days PO. No signal was recorded in the lesion-control group. The waveforms of sodium hyaluronate and CNTF rats at 98 days PO were the same as those of lesion-control rats, almost a straight line (not shown).
Recovery of locomotor function
Open-field locomotion of the sodium hyaluronate-CNTF rats was significantly enhanced in the subchronic phase and the recovery proceeded relatively rapidly during this period (up to 4 weeks PO, Figure 7); this enhanced performance was maintained to the chronic phase (12 weeks PO), and the recovery continued at a slower pace (Figure 7). From week 1 PO onward, the sodium hyaluronate-CNTF rats performed significantly better than the lesion-control and sodium hyaluronate rats (ANOVA, P<0.05); From week 3 onward, the sodium hyaluronate-CNTF rats performed significantly better than the CNTF rats (ANOVA, P<0.05). At 12 weeks PO, the mean BBB score of sodium hyaluronate-CNTF rats was 7.1 (Figure 7), which corresponds to extensive movement of all three joints of the hindlimbs. The result demonstrated that sodium hyaluronate-CNTF gelatinous particles had significantly improved the recovery of hindlimb motor function, and the differences persisted to the last day of the study. At 2 weeks postrelesioning, the sodium hyaluronate-CNTF rats only achieved a mean BBB score of 2.8 (Figure 7), showing significant statistical difference compared with 7.1 before the relesioning (Student’s t-test, P=0.001).
BBB open-field locomotor scores for the four groups. The BBB scores of the sodium hyaluronate-CNTF rats were higher than those of the lesion-control rats from 1 to 12 weeks PO (*P<0.05). After the relesioning, the BBB scores of the sodium hyaluronate-CNTF rats markedly decreased. Statistical analysis was done by an ANOVA. Values are group means±s.e.
Discussion
In this study, we demonstrated that sodium hyaluronate-CNTF gelatinous particles could significantly promote axonal regrowth, neurogenesis and the recovery of locomotor and electrophysiological functions after SCI. The sodium hyaluronate-CNTF gelatinous particles were still detectable at 105 days after implantation in our experiment, which would continuously help further recovery of the function and injured tissue itself.
Biomaterials could promote axon regeneration as permissive bridges after SCI.10, 11 Several previous studies have reported axonal growth through linear scaffolds.10, 11 While the diameter of the channels of linear scaffolds was often too small to accommodate adequate axons and regenerating fibers typically could not enter the channels.10 To help alleviate this shortcoming, we implanted sodium hyaluronate-CNTF gelatinous particles into the lesion area. As gelatinous particles, they are soft and fill the lesion area by adopting the shape of the cavity, preventing mechanical stress to the surrounding host tissue. Most importantly, the sodium hyaluronate gelatinous particles could act as reservoirs to deliver CNTF directly to the injury site. CNTF is a potent trophic factor for the sprouting of the injured axon and the survival of motor neurons after SCI.6, 7 Implantation of sodium hyaluronate-CNTF gelatinous particles would make the greatest CNTF concentration in the lesion area and lower concentrations in the adjacent tissue. The gradient may facilitate axonal growth toward the lesion area. The corticospinal tract in the adult rat is not mainly involved in locomotor function.12 Thus, although there were no corticospinal fibers passing through the lesion area in this study, the locomotor recovery was still shown in the sodium hyaluronate-CNTF group. The regeneration of more relevant but less accessible tracts (for example, rubrospinal tracts) needs to be investigated in future studies.
Neural progenitors in adult rodent’s spinal cord could only differentiate into astrocytes and oligodendrocytes under normal and pathological conditions.13, 14 Neuronal differentiation was rarely found and only in some cases of minor lesions.13, 14, 15 This manuscript is the first report of the novel finding that endogenous newborn β-tubulin-III–positive neuron-like cells existed after severe SCI. The β-tubulin-III–positive neuron-like cells have assumed neuronal morphologies and expressed specific neuronal antigens, which were equally distributed in nuclei, cytoplasm and processes. These results confirmed that the β-tubulin-III–positive neuron-like cells were not inflammatory cells, which often showed positive staining of neuronal markers due to the endocytosing of neural cells or particles. We analyzed that sodium hyaluronate-CNTF gelatinous particles might create a favorable microenvironment for the differentiation of neural stem/progenitor cells to neuronal cell line. Ongoing studies need to further research the source of newborn neurons, the extent of neural progenitors’ differentiation and investigate strategies to further enhance the process.
In this study, cMEPs showed similar latencies for the sodium hyaluronate-CNTF rats at 50 or 98 days PO, which demonstrated that cMEPs were truly induced by electrical stimuli, not by spontaneous fasciculations. Each cSEP waveform was 200 responses averaged and superimposed, and repeated twice to ensure the veracity. The conduction velocities of cMEPs and cSEPs at 98 days PO were faster than those at 50 days, which we think was probably attributed to the continuous increase of myelin sheaths in the injured spinal cord and the reduction in synaptic delay along with the recovery time extension.16 After the relesioning, markedly attenuated electrophysiological function of the sodium hyaluronate-CNTF rats validated that cMEPs and cSEPs were induced by electrical stimuli, which conducted along the regenerating nerve tissue through the implant.
cMEPs and cSEPs showed a relatively wide spread of amplitudes for the sodium hyaluranate-CNTF rats at 50 or 98 days PO. The possible reasons are as follows. First, there is significant variability in amplitudes for normal rats. Second, body temperature and individual difference in sensitivity to the anesthesia could also affect evoked potentials.17, 18 Third, there may be difference in tissue impedances among rats.17
The hindlimb locomotor function of the sodium hyaluronate-CNTF rats obviously decreased postrelesioning compared with the locomotion at 12 weeks PO. This result suggested that the regenerating nerve tissue had contributed to the partial locomotor function recovery in the sodium hyaluronate-CNTF group. BBB scores of CNTF rats showed a transient increase at 1 week PO followed by a fall thereafter, reflecting that the sodium hyaluronate gelatinous particles were required for the recovery to be enduring. There was a statistically significant difference between the sodium hyaluronate-CNTF and sodium hyaluronate rats in BBB scores, indicating the potential therapeutic efficacy of the combination of sodium hyaluronate gelatinous particles with CNTF.
The transplantation of stem cells, stromal cells and engineered cells for SCI has been widely investigated in the previous studies. Many of the cell transplantation therapies have shown effectiveness in improving hindlimb locomotor function in the contusion or compression animal experiments.3 However, the transplanted cells seem to primarily differentiate towards a glial phenotype.3 The glial scar in the injury site inhibits the transplanted cells to migrate and integrate. The majority of cell-based therapies have therefore investigated the effects of transplanted cells 1–2 weeks after injury.19 It is more difficult to envisage a cell-transplantation therapy in the chronic phase. With regard to a completely transected injury, only slight functional recovery was shown in the preceding cell-based therapies. Furthermore, besides overcoming concerns about tumorigenicity, immune responses and the ethics of using human embryonic stem cells, the questions of the ideal sources of grafted cells, the optimal strategy and time for transplantation, the strategy for promoting stem cell differentiation and circuit formation still require further research before clinical trials of cell-based therapies. The sodium hyaluronate-CNTF gelatinous particles significantly improved hindlimb locomotor function, and the recovery persisted to the last day of this study. In addition, very few previous studies including neurotrophic factors, cellular bridges and gene therapies have reported a satisfactory recovery of evoked potentials, especially cMEP. There was some degree of recovery for both cMEP and cSEP in this study. These beneficial results suggest that this technique may be worth further research for the treatment of SCI.
Data Archiving
There were no data to deposit.
References
Schwab ME . Repairing the injured spinal cord. Science 2002; 295: 1029–1031.
Neumann S, Woolf CJ . Regeneration of dorsal column fibers into and beyond the lesion site following adult spinal cord injury. Neuron 1999; 23: 83–91.
Bareyre FM . Neuronal repair and replacement in spinal cord injury. J Neurol Sci 2008; 265: 63–72.
Guo JS, Zeng YS, Li HB, Huang WL, Liu RY, Li XB et al. Cotransplant of neural stem cells and NT-3 gene modified Schwann cells promote the recovery of transected spinal cord injury. Spinal Cord 2007; 45: 15–24.
Bregman BS, Coumans JV, Dai HN, Kuhn PL, Lynskey J, McAtee M et al. Transplants and neurotrophic factors increase regeneration and recovery of function after spinal cord injury. Prog Brain Res 2002; 137: 257–273.
Ip NY, Yancopoulos GD . The neurotrophins and CNTF: two families of collaborative neurotrophic factors. Annu Rev Neurosci 1996; 19: 491–515.
Ishii K, Nakamura M, Dai H, Finn TP, Okano H, Toyama Y et al. Neutralization of ciliary neurotrophic factor reduces astrocyte production from transplanted neural stem cells and promotes regeneration of corticospinal tract fibers in spinal cord injury. J Neurosci Res 2006; 84: 1669–1681.
Paxinos G, Watson C . The rat brain in stereotaxic coordinates. In: Paxinos G, Watson C (eds). Coronal Section, 2nd edn. Academic Press: California, USA, 1986, pp 91–99.
Basso DM, Beattie MS, Bresnahan JC . A sensitive and reliable locomotor rating scale for open field testing in rats. J Neurotrauma 1995; 12: 1–21.
Stokols S, Tuszynski MH . Freeze-dried agarose scaffolds with uniaxial channels stimulate and guide linear axonal growth following spinal cord injury. Biomaterials 2006; 27: 443–451.
Tysseling-Mattiace VM, Sahni V, Niece KL, Birch D, Czeisler C, Fehlings MG et al. Self-assembling nanofibers inhibit glial scar formation and promote axon elongation after spinal cord injury. J Neurosci 2008; 28: 3814–3823.
Teng YD, Lavik EB, Qu X, Park KI, Ourednik J, Zurakowski D et al. Functional recovery following traumatic spinal cord injury mediated by a unique polymer scaffold seeded with neural stem cells. Proc Natl Acad Sci USA 2002; 99: 3024–3029.
Barnabé-Heider F, Göritz C, Sabelström H, Takebayashi H, Pfrieger FW, Meletis K et al. Origin of new glial cells in intact and injured adult spinal cord. Cell Stem Cell 2010; 7: 470–482.
Ke Y, Chi L, Xu R, Luo C, Gozal D, Liu R . Early response of endogenous adult neural progenitor cells to acute spinal cord injury in mice. Stem Cells 2006; 24: 1011–1019.
Danilov AI, Covacu R, Moe MC, Langmoen IA, Johansson CB, Olsson T et al. Neurogenesis in the adult spinal cord in an experimental model of multiple sclerosis. Eur J Neurosci 2006; 23: 394–400.
Imaizumi T, Lankford KL, Kocsis JD . Transplantation of olfactory ensheathing cells or Schwann cells restores rapid and secure conduction across the transected spinal cord. Brain Res 2000; 854: 70–78.
Koyanagi I, Tator CH . The effects of cortical stimulation, anesthesia and recording site on somatosensory evoked potentials in the rat. Electroencephalogr Clin Neurophysiol 1996; 101: 534–542.
Jou IM . Effects of core body temperature on changes in spinal somatosensory-evoked potential in acute spinal cord compression injury: an experimental study in the rat. Spine 2000; 25: 1878–1885.
Barnabé-Heider F, Frisén J . Stem cells for spinal cord repair. Cell Stem Cell 2008; 3: 16–24.
Acknowledgements
This work was supported by the State Key Program of National Natural Science Foundation of China (Grants nos. 31130022, 31271037 and 31320103903), the National Science and Technology Pillar Program of China (Grant no. 2012BAI17B04), the National 863 Project (Grant no. 2012AA020506), the National Ministry of Education Special Fund for Excellent Doctoral Dissertation (Grant no. 201356), the Special Funds for Excellent Doctoral Dissertation of Beijing, China (Grant no. 20111000601) and the Key Project of Department of Science and Technology of Beijing, China (Grant no. D090800046609004).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, N., Zhang, S., Zhang, A. et al. Sodium hyaluronate-CNTF gelatinous particles promote axonal growth, neurogenesis and functional recovery after spinal cord injury. Spinal Cord 52, 517–523 (2014). https://doi.org/10.1038/sc.2014.54
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2014.54
This article is cited by
-
Application of the sodium hyaluronate-CNTF scaffolds in repairing adult rat spinal cord injury and facilitating neural network formation
Science China Life Sciences (2018)