Abstract
Pulse pressure (PP) has been noted as a potential independent risk factor for micro and macrovascular diabetic complications. We aimed to examine the prognostic value of home-measured PP (home PP) in patients with type 2 diabetes. This study is a 2-year prospective cohort study of 737 patients with type 2 diabetes. Home blood pressure measurements were performed for 14 consecutive days. We defined the progression of diabetic nephropathy as when the diabetic nephropathy stage advanced to a higher stage during the 2 years. Using logistic regression analyses, we investigated the relationship between home PP and home systolic blood pressure (SBP) in the morning and in the evening and the progression of diabetic nephropathy. Furthermore, we measured the area under the receiver-operating characteristic curve (AUC) to assess the predictive ability of the progression of diabetic nephropathy of home PP. During the 2-year study, progression of diabetic nephropathy was observed in 94 patients. The adjusted odds ratios (95% confidence interval (CI)) of home PP and home SBP to the progression of diabetic nephropathy were 1.23 (1.01–1.49) and 1.14 (0.98–1.33), respectively. The AUC (95% CI) of home PP to the progression of diabetic nephropathy was 0.624 (0.665–0.679). The optimal cut-off points, sensitivity and specificity for home PP that were associated with the progression of diabetic nephropathy were 57.7 mmHg, 0.649 and 0.580, respectively. Our findings suggest, for the first time, that home PP is an independent predictor of the progression of diabetic nephropathy in patients with type 2 diabetes.
Similar content being viewed by others
Introduction
Blood pressure (BP) control is essential to prevent cardiovascular events or microvascular disease in patients with type 2 diabetes [1, 2]. Home-measured BP (HBP) has been viewed as an important therapeutic parameter to predict organ damage and determine the prognosis [3,4,5]. HBP has been widely used in clinical practice for high-risk patients with cardiovascular disease.
Pulse pressure (PP), defined as the difference between systolic blood pressure (SBP) and diastolic blood pressure (DBP), is superior to both SBP and DBP in predicting cardiovascular disease mortality [6,7,8]. The risk of PP for cardiovascular disease mortality in patients with T2D was surveyed in previous studies [8, 9]. PP is also an important risk factor for incident or progression of chronic kidney disease in individuals with type 2 diabetes [10]. Thus, PP has been noted as a potential independent risk factor for micro and macrovascular disease in individuals with and without diabetes [7, 9, 11,12,13,14]. We have previously reported on a cross-sectional study of the KAMOGAWA-HBP cohort in which home-measured PP (home PP) is associated with elevated albuminuria in patients with type 2 diabetes [15].
Consequently, it can be assumed that control of home PP plays an important role in preventing the progression of diabetic nephropathy. However, there is no information about the prognostic significance of home PP for the progression of diabetic nephropathy. The aim of the current study is to examine whether home PP has prognostic significance for the progression of diabetic nephropathy in patients with type 2 diabetes.
Materials and methods
Study design
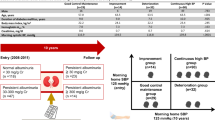
We accessed a database of our previous study, which was based on data from the HBP cohort of type 2 diabetes patients who had regularly attended the diabetes outpatient clinic at the Kyoto Prefectural University of Medicine Hospital or one of four other general hospitals (KAMOGAWA-HBP study) [16]. We evaluated the association of SBP or PP with progression of diabetic nephropathy in patients with type 2 diabetes. We defined the progression of diabetic nephropathy as when the diabetic nephropathy stage advanced to a higher stage during the 2 years. Nephropathy was graded as follows: normoalbuminuria, urinary albumin/creatinine ratio (UACR) <30 mg per gram of creatinine (mg/g Cr); microalbuminuria, 30–300 mg/g Cr; or macroalbuminuria, >300 mg/g Cr. [17] All procedures of the present study were approved by the local Research Ethics Committee and were conducted in accordance with the Declaration of Helsinki, and informed consent was obtained from all patients.
Patients
The HBP monitoring program recruited 1414 consecutive patients with type 2 diabetes, aged between 23 and 89, who visited the facilities. The details of this study have been reported elsewhere [16]. There was no BP level criterion for the study inclusion. Of the 1414 patients, 51 patients were excluded due to insufficient data on blood pressure values, and 430 patients whose UACR data were not available were also excluded. In addition, 13 patients who had advanced renal dysfunction (serum creatinine equal to or >2.0 mg/dl) [18, 19] were excluded from the analyses. Finally, 737 patients comprised the study population (437 males, 330 females). The diagnosis of type 2 diabetes was based on the American Diabetes Association criteria [20].
Data collection
Blood samples for biochemical measurements were taken in the morning. Hemoglobin A1C, serum lipid profile (low-density lipoprotein cholesterol, triglycerides, and high-density lipoprotein cholesterol), and other biochemical data were determined by standard laboratory measurements. Information including age, duration of diabetes, smoking and alcohol drinking status, and antihypertensive medication were obtained at the time of the clinic BP measurement. Diabetic nephropathy was diagnosed according to UACR because albuminuria, an early manifestation of diabetic nephropathy, is a marker of increased cardiovascular mortality and progression of cardiovascular events [21,22,23]. Neuropathy was defined by the diagnostic criteria for diabetic neuropathy proposed by Diagnostic Neuropathy Study Group [24]. Alcohol drinking status (everyday, social or never) and smoking status (current, past or never) were assessed by interview.
HBP measurements
The patients were instructed to perform triplicate morning and evening BP measurements for 14 consecutive days. The mean of the three measurements in the morning and the evening for 14 consecutive days was taken as HBP in this study. Measurements of morning BP were made within 1 h of waking, before breakfast or taking any drugs, with the patient seated and rested for at least 5 min [25]. The evening measurements of BP was obtained in a similar fashion just before going to bed. The cuff was placed around the nondominant arm and the position of the cuff was maintained at the level of the heart. HBP measurements were performed using an automatic device, HEM-70801C (Omron Healthcare Co. Ltd, Kyoto, Japan), which uses the cuff-oscillometric method to generate a digital display of heart rate and SBP/DBP values. BP was automatically recorded into integrated circuit (IC) memory of the HEM-70801C. HEM-70801C employs the identical components and BP determining algorithm to those of another device, HEM-705IT, which was previously validated and satisfied the criteria of the British Hypertension Society protocol [26]. PP was calculated as SBP minus DBP.
Statistical analysis
Baseline characteristics were summarized by median with range or numbers. Logistic regression analyses were used to investigate the relationship between the progression of diabetic nephropathy and morning PP, morning SBP, evening PP, evening SBP or other variables. To adjust the effects of various factors on the progression of diabetic nephropathy, the following factors, which were known risk factors for the progression of diabetic nephropathy, were considered covariates: sex, duration of diabetes, body mass index, total cholesterol, hemoglobin A1C, creatinine, use of antihypertensive medication, and morning PP, morning SBP, evening PP or evening SBP in multivariate logistic regression analyses. Morning PP, morning SBP, evening PP and evening SBP were not included in the same multivariate in the logistic model as continuous variables after dividing by 10. Receiver-operating characteristic (ROC) curves were constructed for PP to assess the ability to identify the progression of diabetic nephropathy and odds ratios (95% confidence interval (CI)) were calculated by using a logistic regression model. As the optimal cut-off points for PP associated with the progression of diabetic nephropathy, we chose the point on the ROC curve, which represented the largest sum of sensitivity and specificity. We next performed the subgroup analyses according to the presence or the absence of antihypertensive medication. P values<0.05 were considered statistically significant. The statistical analyses were performed using the JMP version 10.0 software (SAS Institute Inc., Cary, NC, USA)
Results
Clinical characteristics of patients (407 males and 330 females, aged 66 (60–72) years, duration of diabetes 10.0 (5–17) years, BMI 23.5 (21.6–25.6) kg/m2, hemoglobin A1C 7.0 (6.6–7.7)%) are shown in Table 1. A total of 399 patients were treated with antihypertensive drugs. During 2 years, progression of diabetic nephropathy was observed in 94 patients. The adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP, and evening SBP for the progression of diabetic nephropathy were 1.23 (1.01–1.49), 1.14 (0.98–1.33), 1.01 (0.85–1.21), and 0.92 (0.84–1.03), respectively (Table 2). The area under the curve (AUC) (95% CI) of the ROC curve of morning PP for the progression of diabetic nephropathy was 0.624 (0.665–0.679) (Fig. 1a). The optimal cut-off points, sensitivity and specificity for morning PP that were associated with progression of diabetic nephropathy were 57.7 mmHg, 0.649 and 0.580, respectively. AUC (95% CI) of the ROC curve of evening PP for the progression of diabetic nephropathy in home PP was 0.614 (0.550–0.673) (Fig. 1b). The optimal cut-off points, sensitivity and specificity for evening PP that were associated with progression of diabetic nephropathy were 54.4 mmHg, 0.733 and 0.458, respectively.
In patients without antihypertensive medications, the adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP, and evening SBP for the progression of diabetic nephropathy were 1.50 (1.05–2.15), 1.25 (0.95–1.64), 1.23 (0.89–1.70), and 1.03 (0.83–1.28), respectively (Table 3). The AUC (95% CI) of the ROC curve of morning PP for the progression of diabetic nephropathy was 0.635 (0.529–0.730) (Fig. 2a). The optimal cut-off points, sensitivity and specificity for morning PP that were associated with progression of diabetic nephropathy were 55.6 mmHg, 0.667 and 0.646, respectively. The AUC (95% CI) of the ROC curve of evening PP for the progression of diabetic nephropathy in home PP was 0.594 (0.481–0.697) (Fig. 2b). The optimal cut-off points, sensitivity and specificity for evening PP that were associated with the progression of diabetic nephropathy were 53.2 mmHg, 0.633 and 0.568, respectively.
In patients with antihypertensive medications, the adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP and evening SBP for the progression of diabetic nephropathy were 1.11 (0.87–1.39), 1.08 (0.90–1.30), 0.94 (0.77–1.02), and 0.90 (0.80–1.16), respectively (Table 4). The AUC (95% CI) of the ROC curve of morning PP for the progression of diabetic nephropathy was 0.578 (0.503–0.649) (Fig. 3a). The optimal cut-off points, sensitivity and specificity for morning PP that were associated with the progression of diabetic nephropathy were 63.9 mmHg, 0.531 and 0.639, respectively. The AUC (95% CI) of the ROC curve of evening PP for the progression of diabetic nephropathy in home PP was 0.559 (0.478–0.638) (Fig. 3b). The optimal cut-off points, sensitivity and specificity for evening PP that were associated with progression of diabetic nephropathy were 61.7 mmHg, 0.594 and 0.561, respectively.
Discussion
The present study of patients with type 2 diabetes provided novel evidence that morning PP, but not morning SBP, was an independent predictor of the progression of diabetic nephropathy in patients with type 2 diabetes. We demonstrated that morning PP was superior to morning SBP in predicting the progression of diabetic nephropathy in patients with type 2 diabetes. The results were almost the same in patients without antihypertensive medications. However, the results were not the same in patients with antihypertensive medications.
PP is a readily available hemodynamic parameter in regards to associations of office PP and progression of systemic atherosclerosis. PP is associated with multiple adverse cardiovascular outcomes and provides prognostic utility beyond that of mean arterial pressure [7]. PP was superior to both SBP and DBP in predicting coronary heart disease risk in the Framingham study [6]. We demonstrated that the ability to identify progression of diabetic nephropathy is higher in morning PP than in morning SBP. This result is consistent with previous studies suggesting that PP may provide additional prognostic information, above and beyond SBP [6, 27].
Several possible mechanisms underlying the relationship between PP and progression of diabetic nephropathy are postulated in previous studies. Knudsen et al. [28] demonstrated the strong associations between atherosclerosis and elevated plasma levels of proteins, including E-selectin and intercellular adhesion molecule 1, related to endothelial activation by an augmentation of PP in patients with type 2 diabetes. The other report also indicated that PP is inversely correlated with endothelium-dependent acetylcholine-stimulated vasodilation in hypertensive patients [29]. Elevated PP might be associated with systemic inflammation as measured by serum levels of C-reactive protein [30]. These findings indicate that endothelial dysfunction and inflammation could represent a pathophysiological link between elevated PP and progression of diabetic nephropathy. Furthermore, arterial stiffening causes elevation of SBP without elevation of DBP, which widens PP [31,32,33]. Increased arterial stiffening causes vascular damage that lowers kidney function [34,35,36]. In addition, increased aortic PP causes renal microvascular damage through altered renal hemodynamics resulting from increased peripheral resistance and flow pulsation [37]. Sustained elevation of home PP might cause the progression of diabetic nephropathy as mentioned above.
We demonstrated that morning PP had prognostic significance. Generally, increase in SBP is larger in morning because of the renin-angiotensin system, neuroendocrine and hematological factors [38,39,40]. In previous reports, morning SBP was associated with target organ damage [5, 38, 40] and was best predictor of stroke events [40]. It was also suggested that lower morning home SBP might be beneficial for patients with diabetes [41]. Increased morning SBP, resulting in increased morning PP, might be a reason why only morning PP was closely associated with the progression of diabetic nephropathy in this study.
In the present study, morning PP was an independent predictor of progression of diabetic nephropathy in patients without antihypertensive medications but not in those with antihypertensive medications. Antihypertensive therapy affects diabetic nephropathy [1, 2]. Antihypertensive medications could have an impact on PP in this study. In addition to that, angiotensin-converting-enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARB) were used in the greater part of the patients with antihypertensive medications in this study. In patients with ACE inhibitors or ARB, neither home PP nor home SBP was an independent predictor of the progression of diabetic nephropathy (Supplementary Table 1).
The patients in this study were a high-risk population. In total 6 of the 571 patients, who had no history of cardiovascular events at the time of study entry, had new incidence of cardiovascular events during the 2 years. The adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP or evening SBP for having a new incidence of cardiovascular events were 0.71 (0.34–1.47), 0.85 (0.52–1.46), 0.71 (0.36–1.39), and 0.87 (0.51–1.31), respectively.
Some antidiabetic medications might influence the progression of diabetic nephropathy. In previous studies, dipeptidyl peptidase-4 (DPP-4) inhibitors and sodium-glucose co-transporter (SGLT2) inhibitors reduced the development and progression of diabetic nephropathy in patients with type 2 diabetes [42,43,44]. DPP-4 inhibitors were prescribed in 123 patients and SGLT2 inhibitors were not used at the start of this study. We performed the logistic regression analysis also adjusting for use of DPP-4 inhibitors. The adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP or evening SBP for the progression of diabetic nephropathy were 1.23 (1.01–1.49), 1.14 (0.98–1.32), 1.01 (0.85–1.20), and 0.92 (0.83–1.03), respectively, which was consistent with the main finding of this study. DPP-4 inhibitors were newly prescribed in 118 patients and SGLT2 inhibitors were newly prescribed in 7 patients as monotherapy or add-on treatment during the 2 years. When we performed the logistic regression analysis after excluding these 125 patients, the adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP or evening SBP for the progression of diabetic nephropathy were 1.33 (1.01–1.75), 1.30 (1.05–1.61), 1.15 (0.90–1.49), and 1.06 (0.91–1.28), respectively, which was also consistent with the main finding of this study.
Clinic PP or SBP would also be one of the most important factors for the progression of diabetic nephropathy. Thus, we have evaluated the association between clinic PP or SBP and the progression of nephropathy. The adjusted odds ratios (95% CI) of clinic PP and clinic SBP for the progression of diabetic nephropathy were 1.22 (1.04–1.43) and 0.98 (0.80–1.22), respectively. ROC curves were constructed for morning PP and clinic PP to assess the ability to identify the progression of albuminuria. The AUCs were compared. AUC (95% CI) of morning PP {0.623 (0.564–0.679)} was greater than that of office PP {0.587 (0.523–0.649)}, although there was not a significant difference between them (P = 0.13) (Supplementary Figure 1). AUC (95% CI) of morning PP {0.623 (0.564–0.679)} was greater than that of clinic SBP {0.530 (0.466–0.592)} (P = 0.006) (Supplementary Figure 2).
PP gains importance as both a pathophysiologic index and prognostic factor in relatively elderly hypertensives [32]. In our study, there was no interaction between age and PP (P = 0.29). Age was closely associated with duration of diabetes in patients with diabetes. Therefore, we included only duration of diabetes, which was one of the main risks of diabetic nephropathy, as a covariate in the multivariate logistic model. Age is also a risk of diabetic nephropathy. Thus, we included age instead of duration of diabetes as a covariate. The adjusted odds ratios (95% CI) of morning PP, morning SBP, evening PP or evening SBP for the progression of diabetic nephropathy were 1.22 (0.99–1.49), 1.15 (0.99–1.33), 0.99 (0.83–1.19), and 0.93 (0.84–1.04), respectively. The adjusted odds ratios (95% CI) were almost the same, although they did not reach statistical significance.
The strengths of the present study include that we used a device that is equipped with memory to store readings rather than trusting patients’ logbooks that have poor adherence [45], that we designed a prospective study and that HBP measurements were performed over a relatively long consecutive period. On the other hand, there are some limitations in this study. First, the duration of hypertension could be a clinically significant variable in terms of the development of albuminuria [46], and physical exercise may affect urinary albumin excretion [47]. However, we did not collect the data of duration of hypertension and physical exercise. Second, the study population consisted of Japanese men and women. Therefore, it is uncertain whether these findings can be generalized to other ethnic groups. Third, our study only used a single baseline measurement of BP. This may produce potential bias. However, it has been reported that the association of target organ damage was confirmed by BP at baseline or during follow-up [48]. Further studies are needed to assess the relationship between average morning PP and progression of diabetic nephropathy. Our study might have better clinical implication if average morning PP will still be a determinant of progression of diabetic nephropathy when controlled for the average BP during follow-up of patients with type 2 diabetes. Finally, the 2-year observational data may not deserve an accurate prognostic significance of diabetic nephropathy. Longer observation is needed to confirm our findings.
In summary, home PP is an independent predictor of progression of diabetic nephropathy in patients with type 2 diabetes. We should pay more attention to increased home PP, as well as increased home SBP and should lower PP in patients whose home PP is more than a cut-off value, for example, the 57.7 mmHg determined in this study, to prevent the development and progression of diabetic nephropathy. Further prospective trials and interventional studies are needed to better assess the relationship between morning PP and progression of diabetic nephropathy. Moreover, randomized controlled trials will be needed to assess how to reduce morning PP and which antihypertensive medications or antidiabetic drugs may lower morning PP and prevent incidence and progression of diabetic nephropathy.
References
Holman RR, Paul SK, Bethel MA, Neil HA, Matthews DR. Long-term follow-up after tight control of blood pressure in type 2 diabetes. N Engl J Med. 2008;359:1565–76.
ACCORD Study Group, Cushman WC, Evans GW, Byington RP, Jr GoffDC, Jr GrimmRH, Cutler JA, Simons-Morton DG, Basile JN, Corson MA, Probstfield JL, Katz L, Peterson KA, Friedewald WT, Buse JB, Bigger JT, Gerstein HC, Ismail-Beigi F. Effects of intensive blood-pressure control in type 2 diabetes mellitus. N Engl J Med. 2010;362:1575–85.
Niiranen TJ, Johansson JK, Reunanen A, Jula AM. Optimal schedule for home blood pressure measurement based on prognostic data: The finn-home study. Hypertension. 2011;57:1081–6.
Hozawa A, Ohkubo T, Nagai K, Kikuya M, Matsubara M, Tsuji I, Ito S, Satoh H, Hisamichi S, Imai Y. Prognosis of isolated systolic and isolated diastolic hypertension as assessed by self-measurement of blood pressure at home: the Ohasama study. Arch Intern Med. 2000;160:3301–6.
Hoshide S, Kario K, Yano Y, Haimoto H, Yamagiwa K, Uchiba K, Nagasaka S, Matsui Y, Nakamura A, Fukutomi M, Eguchi K, Ishikawa J, J-HOP Study Group. Association of morning and evening blood pressure at home with Asymptomatic organ damage in the J-HOP study. Am J Hypertens. 2014;27:939–47.
Franklin SS, Khan SA, Wong ND, Larson MG, Levy D. Is pulse pressure useful in predicting risk for coronary heart Disease? The Framingham heart study. Circulation. 1999;100:354–60.
Selvaraj S, Steg PG, Elbez Y, Sorbets E, Feldman LJ, Eagle KA, Ohman EM, Blacher J, Bhatt DL, REACH Registry Investigators. Pulse pressure and risk for cardiovascular events in patients with atherothrombosis from the REACH registry. J Am Coll Cardiol. 2016;67:392–403.
McEvoy JW, Chen Y, Rawlings A, Hoogeveen RC, Ballantyne CM, Blumenthal RS, Coresh J, Selvin E. Diastolic blood pressure, subclinical myocardial damage, and cardiac events: implications for blood pressure control. J Am Coll Cardiol. 2016;68:1713–22.
Nakano S, Konishi K, Furuya K, Uehara K, Nishizawa M, Nakagawa A, Kigoshi T, Uchida K. A prognostic role of mean 24-h pulse pressure level for cardiovascular events in type 2 diabetic subjects under 60 years of age. Diabetes Care. 2005;28:95–100.
van den Hurk K, Magliano DJ, Alssema M, Schlaich MP, Atkins RC, Reutens AT, Nijpels G, Dekker JM, Shaw JE. Type 2 diabetes strengthens the association between pulse pressure and chronic kidney disease: the AusDiab study. J Hypertens. 2011;29:953–60.
Knudsen ST, Laugesen E, Hansen KW, Bek T, Mogensen CE, Poulsen PL. Ambulatory pulse pressure, decreased nocturnal blood pressure reduction and progression of nephropathy in type 2 diabetic patients. Diabetologia. 2009;52:698–704.
Schram MT, Kostense PJ, Van Dijk RA, Dekker JM, Nijpels G, Bouter LM, Heine RJ, Stehouwer CD. Diabetes, pulse pressure and cardiovascular mortality: the Hoorn Study. J Hypertens. 2002;20:1743–51.
Knudsen ST, Poulsen PL, Hansen KW, Ebbehoj E, Bek T, Mogensen CE. Pulse pressure and diurnal blood pressure variation: association with micro- and macrovascular complications in type 2 diabetes. Am J Hypertens. 2002;15:244–50.
Gu YM, Petit T, Wei FF, Thijs L, Jacobs L, Zhang ZY, Yang WY, Cauwenberghs N, Knez J, StruijkerBoudier HA, Kuznetsova T, Verhamme P, Staessen JA. Renal glomerular dysfunction in relation to retinal arteriolar narrowing and high pulse pressure in seniors. Hypertens Res. 2016;39:138–43.
Ushigome E, Fukui M, Hamaguchi M, Matsumoto S, Mineoka Y, Nakanishi N, Senmaru T, Yamazaki M, Hasegawa G, Nakamura N. Morning pulse pressure is associated more strongly with elevated albuminuria than systolic blood pressure in patients with type 2 diabetes mellitus: Post hoc analysis of a cross-sectional multicenter study. Diabetes Res Clin Pract. 2013;101:270–7.
Ushigome E, Fukui M, Sakabe K, Tanaka M, Inada S, Omoto A, Tanaka T, Fukuda W, Atsuta H, Ohnishi M, Mogami S, Kitagawa Y, Oda Y, Yamazaki M, Hasegawa G, Nakamura N. Uncontrolled home blood pressure in the morning is associated with nephropathy in Japanese type 2 diabetes. Heart Vessels. 2011;26:609–15.
Nakade Y, Toyama T, Furuichi K, Kitajima S, Miyajima Y, Fukamachi M, Sagara A, Shinozaki Y, Hara A, Shimizu M, Iwata Y, Oe H, Nagahara M, Horita H, Sakai Y, Kaneko S, Wada T. Impact of kidney function and urinary protein excretion on intima–media thickness in Japanese patients with type 2 diabetes. Clin Exp Nephrol. 2015;19:909–17.
Remuzzi G. Continuum of renoprotection with losartan at all stages of type 2 diabetic nephropathy: a post hoc analysis of the RENAAL trial results. J Am Soc Nephrol. 2004;15:3117–25.
Voyaki SM, Staessen JA, Thijs L, Wang JG, Efstratopoulos AD, Birkenhäger WH, de Leeuw PW, Leonetti G, Nachev C, Rodicio JL, Tuomilehto J, Fagard R, Systolic Hypertension in Europe (Syst-Eur) Trial Investigators. Follow-up of renal function in treated and untreated older patients with isolated systolic hypertension for the Systolic Hypertension in Europe (Syst-Eur) Trial Investigators. J Hypertens. 2001;19:511–9.
The Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Report of the expert committee on the description of diabetes categories of glucose. Diabetes Care. 2003;26:5–20. suppl 1
Gerstein HC, Mann J, Yi Q, Zinman B, Dinneen SF, Hoogwerf B, Hallé JP, Young J, Rashkow A, Joyce C, Nawaz S, Yusuf S, HOPE Study Investigators. Albuminuria and risk of cardiovascular events, death, and heart failure. J Am Med Assoc. 2001;286:421–6.
Kramer H, Jacobs DR, Bild D, Post W, Saad MF, Detrano R, Tracy R, Cooper R, Liu K. Urine albumin excretion and subclinical cardiovascular disease: The multi-ethnic study of atherosclerosis. Hypertension. 2005;46:38–43.
Krolewski AS, Niewczas MA, Skupien J, Gohda T, Smiles A, Eckfeldt JH, Doria A, Warram JH. Early progressive renal decline precedes the onset of microalbuminuria and its progression to macroalbuminuria. Diabetes Care. 2014;37:226–34.
Yasuda H, Sanada M, Kitada K, Kitajima S, Miyajima Y, Fukamachi M, Sagara A, Shinozaki Y, Hara A, Shimizu M, Iwata Y, Oe H, Nagahara M, Horita H, Sakai Y, Kaneko S, Wada T. Rationale and usefulness of newly devised abbreviated diagnostic criteria and staging for diabetic polyneuropathy. Diabetes Res Clin Pract. 2007;77:S178–S183.
Imai Y, Kario K, Shimada K, Kawano Y, Hasebe N, Matsuura H, Tsuchihashi T, Ohkubo T, Kuwajima I, Miyakawa M, Japanese Society of Hypertension Committee for Guidelines for Self-monitoring of Blood Pressure at Home. The Japanese Society of Hypertension Guidelines for self-monitoring of blood pressure at home (Second Edition). Hypertens Res. 2012;35:777–95.
Coleman A, Freeman P, Steel S, Shennan A. Validation of the Omron 705IT (HEM-759-E) oscillometric blood pressure monitoring device according to the British Hypertension Society protocol. Blood Press Monit. 2006;11:27–32.
Assmann G, Cullen P, Evers T, Petzinna D, Schulte H. Importance of arterial pulse pressure as a predictor of coronary heart disease risk in PROCAM. Eur Heart J. 2005;26:2120–6.
Knudsen ST, Jeppesen P, Frederiksen CA, Andersen NH, Bek T, Ingerslev J, Mogensen CE, Poulsen PL. Endothelial dysfunction, ambulatory pulse pressure and albuminuria are associated in Type 2 diabetic subjects. Diabet Med. 2007;24:911–5.
Ceravolo R, Maio R, Pujia A, Sciacqua A, Ventura G, Costa MC, Sesti G, Perticone F. Pulse pressure and endothelial dysfunction in never-treated hypertensive patients. J Am Coll Cardiol. 2003;41:1753–8.
Amar J, Ruidavets JB, Peyrieux JC, Mallion JM, Ferrières J, Safar ME, Chamontin B. C-reactive protein elevation predicts pulse pressure reduction in hypertensive subjects. Hypertension. 2005;46:151–5.
Stehouwer CD, Henry RM, Ferreira I. Arterial stiffness in diabetes and the metabolic syndrome: a pathway to cardiovascular disease. Diabetologia. 2008;51:527–39.
O’Rourke MF, Hashimoto J. Mechanical factors in arterial aging: a clinical perspective. J Am Coll Cardiol. 2007;50:1–13.
Dart AM, Kingwell BA. Pulse pressure—a review of mechanisms and clinical relevance. J Am Coll Cardiol. 2001;37:975–84.
Safar ME, London GM, Plante GE. Arterial stiffness and kidney function. Hypertension. 2004;43:163–8.
Knudsen ST, Andersen NH, Mogensen CE. Ambulatory pulse pressure and progression of albuminuria in type 2 diabetes: Evidence provided, new questions emerge. Hypertension. 2006;48:207–8.
Hamano K, Nitta A, Ohtake T, Kobayashi S. Associations of renal vascular resistance with albuminuria and other macroangiopathy in type 2 diabetic patients. Diabetes Care. 2008;31:1853–7.
Hashimoto J, Ito S. Central pulse pressure and aortic stiffness determine renal hemodynamics: Pathophysiological implication for microalbuminuria in hypertension. Hypertension. 2011;58:839–46.
Kario K, Saito I, Kushiro T, Teramukai S, Tomono Y, Okuda Y, Shimada K. Morning home blood pressure is a strong predictor of coronary artery disease: the HONEST study. J Am Coll Cardiol. 2016;67:1519–27.
Muller JE, Tofler GH, Stone PH. Circadian variation and triggers of onset of acute cardiovascular disease. Circulation. 1989;79:733–43.
Hoshide S, Yano Y, Haimoto H, Yamagiwa K, Uchiba K, Nagasaka S, Matsui Y, Nakamura A, Fukutomi M, Eguchi K, Ishikawa J, Kario K, J-HOP Study Group. Morning and evening home blood pressure and risks of incident stroke and coronary artery disease in the Japanese General Practice Population: the Japan morning surge-home blood pressure study. Hypertension. 2016;68:54–61.
Kushiro T, Kario K, Saito I, Teramukai S, Sato Y, Okuda Y, Shimada K. Increased cardiovascular risk of treated white coat and masked hypertension in patients with diabetes and chronic kidney disease: the HONEST Study. Hypertens Res. 2017;40:87–95.
Scirica BM, Bhatt DL, Braunwald E, Steg PG, Davidson J, Hirshberg B, Ohman P, Frederich R, Wiviott SD, Hoffman EB, Cavender MA, Udell JA, Desai NR, Mosenzon O, McGuire DK, Ray KK, Leiter LA, Raz I, M.D. for the SAVOR-TIMI 53 Streering Committee and Investigators. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus. N Engl J Med. 2013;369:1317–26.
Wanner C, Inzucchi SE, Lachin JM, Fitchett D, von Eynatten M, Mattheus M, Johansen OE, Eoerle HJ, Broedl UC, Zinman B, EMPA-REG OUTCOME investigators. Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med. 2016;375:323–34.
Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, Shaw W, Law G, Desai M, Matthews DR, CANVAS Program Collaborative Group. Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med. 2017;377:644–57. for
van der Hoeven NV, van den Born BJ, Cammenga M, van Montfrans GA. Poor adherence to home blood pressure measurement schedule. J Hypertens. 2009;27:275–9.
Molitch ME, DeFronzo RA, Franz MJ, Keane WF, Mogensen CE, Parving HH, American Diabetes Association. Diabetic nephropathy. Diabetes Care. 2003;26:S94–S98.
Climie RE, Srikanth V, Keith LJ, Davies JE, Sharman JE. Exercise excess pressure and exercise -induced albuminuria in patients with type 2 diabetes mellitus. Am J Physiol Heart Circ Physiol. 2015;308:H1136–H1142.
Zhao W, Katzmarzyk PT, Horswell R, Wang Y, Li W, Johnson J, Heymsfield SB, Cefalu WT, Ryan DH, Hu G. Aggressive blood pressure control increases coronary heart disease risk among diabetic patients. Diabetes Care. 2013;36:3287–96.
Acknowledgements
We acknowledge Dr. Atsushi Omoto and Dr. Wataru Fukuda of Kyoto First Red Cross Hospital, Dr. Shin-ichi Mogami and Dr. Yoshihiro Kitagawa of Osaka General Hospital of West Japan Railway Company and Dr. Yohei Oda of Social insurance Kyoto Hospital, for their assistance of collecting data. We thank Naoko Higo R.N., Machiko Hasegawa R.N., and Terumi Kaneko R.N. of the Kyoto Prefectural University of Medicine, for teaching patients how to measure their blood pressure and Sayoko Horibe, Hiroko Kawamura, and Aiko Aida also of the Kyoto Prefectural University of Medicine, for their secretarial assistance. EU received grant support from the Japanese Study Group for Physiology and Management of Blood Pressure and the Astellas Foundation for Research on Metabolic Disorders (Grant Number: 4024).
Author contributions
NK designed the study, performed data analyses and reviewed/edited the manuscript. EU designed the study, contributed to the collection of research data, performed data analyses, drafted the manuscript, and was the main study physician responsible for the KAMOGAWA-HBP study in Kyoto Prefectural University of Medicine, Graduate School of Medical Science. SM and CO designed the study protocol, reviewed data reports, and reviewed the study manuscript. HU designed the study protocol, reviewed data reports, contributed to the discussion, and reviewed the study manuscript. IY supervised the data analysis, contributed to the manuscript preparation, contributed to the discussion, and reviewed/edited the manuscript. MA, MT, and MY designed the study protocol, reviewed data reports, and reviewed the study manuscript. MF designed the protocol, performed data analyses, drafted the manuscript, and was the principal investigator of the Kyoto Prefectural University of Medicine, Graduate School of Medical Science and lead principal investigator for the study. All authors reviewed and provided edits and comments on manuscript drafts. NK is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
NK, EU, SM, CO, MT, MY, and MF have received grant and research support from AstraZeneca plc, Astellas Pharma Inc., Bristol-Myers Squibb K.K., Daiichi Sankyo Co., Ltd., Eli Lilly Japan K.K., Kyowa Hakko Kirin Company Ltd., Kowa Pharmaceutical Co., Ltd., Kissei Pharmaceutical Co., Ltd., MSD K.K., Mitsubishi Tanabe Pharma Corp., Novo Nordisk Pharma Ltd., Nippon Chemiphar Company Ltd., Sanwa Kagaku Kenkyusho Co., Ltd., Sanofi K.K., Taisho Toyama Pharmaceutical Co., Ltd., Takeda Pharmaceutical Co., Ltd., and TERUMO Co. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kitagawa, N., Ushigome, E., Matsumoto, S. et al. Prognostic significance of home pulse pressure for progression of diabetic nephropathy: KAMOGAWA-HBP study. Hypertens Res 41, 363–371 (2018). https://doi.org/10.1038/s41440-018-0024-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-018-0024-6
This article is cited by
-
Home blood pressure measurement: the original and the best for predicting the risk
Hypertension Research (2023)
-
Determinants of pulse pressure amplification in hypertensive and diabetic patients
Hypertension Research (2019)