Key Points
-
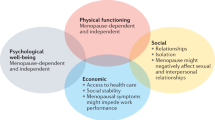
Menopausal symptoms have a substantial effect on the quality of life of women and on performance at the workplace; increased awareness of symptoms and acquisition of coping strategies might help
-
Certain menopausal symptoms might serve as markers for future health; severe vasomotor symptoms and sleep disorders might increase cardiovascular risk, whereas severe vasomotor symptoms and depression might affect cognitive function
-
The nature of menopausal symptoms is common to all women; however, geographical location and ethnicity influence the prevalence of certain symptoms
-
Individual factors such as personal history, current health status (particularly obesity) and socioeconomic status considerably worsen a woman's experience of menopause
-
Health-care providers should offer education to women on improving modifiable lifestyle factors to reduce the risk of future illness
-
Menopause seems to accelerate the ageing process; therefore, the manifestation of menopausal symptoms might be in part due to ageing
Abstract
The symptoms of menopause can be distressing, particularly as they occur at a time when women have important roles in society, within the family and at the workplace. Hormonal changes that begin during the menopausal transition affect many biological systems. Accordingly, the signs and symptoms of menopause include central nervous system-related disorders; metabolic, weight, cardiovascular and musculoskeletal changes; urogenital and skin atrophy; and sexual dysfunction. The physiological basis of these manifestations is emerging as complex and related, but not limited to, oestrogen deprivation. Findings generated mainly from longitudinal population studies have shown that ethnic, geographical and individual factors affect symptom prevalence and severity. Moreover, and of great importance to clinical practice, the latest research has highlighted how certain menopausal symptoms can be associated with the onset of other disorders and might therefore serve as predictors of future health risks in postmenopausal women. The goal of this Review is to describe in a timely manner new research findings on the global prevalence and physiology of menopausal symptoms and their impact on future health.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Harlow, S. D. et al. Executive summary of the stages of reproductive aging workshop +10: addressing the unfinished agenda of staging reproductive aging. Menopause 19, 387–395 (2012).
Woods, N. F. & Mitchell, E. S. Symptoms during the perimenopause: prevalence, severity, trajectory, and significance in women's lives. Am. J. Med. 118, 14–24 (2005).
Sutton-Tyrrell, K. et al. Reproductive hormones and obesity: 9 years of observation from the study of women's health across the nation. Am. J. Epidemiol. 171, 1203–1213 (2010).
Barbieri, R. L., Smith, S. & Ryan, K. J. The role of hyperinsulinemia in the pathogenesis of ovarian hyperandrogenism. Fertil. Steril. 50, 197–212 (1988).
Davis, S. R. et al. Menopause. Nat. Rev. Dis. Primers. 1, 15004 (2015).
Politi, M. C., Schleinitz, M. D. & Col, N. F. Revisiting the duration of vasomotor symptoms of menopause: a meta-analysis. J. Gen. Intern. Med. 23, 1507–1513 (2008).
Freeman, E. W., Sammel, M. D., Lin, H., Liu, Z. & Gracia, C. R. Duration of menopausal hot flushes and associated risk factors. Obstet. Gynecol. 117, 1095–1104 (2011).
Zeleke, B. M., Bell, R. J., Billah, B. & Davis, S. R. Vasomotor and sexual symptoms in older Australian women: a cross-sectional study. Fertil. Steril. 105, 149–155 (2016).
Avis, N. E. et al. Duration of menopausal vasomotor symptoms over the menopause transition. JAMA Intern. Med. 175, 531–539 (2015).
Kravitz, H. M. et al. An actigraphy study of sleep and pain in midlife women: the study of women's health across the nation sleep study. Menopause 22, 710–718 (2015).
Freedman, R. R. & Roehrs, T. A. Effects of REM sleep and ambient temperature on hot flash-induced sleep disturbance. Menopause 13, 576–583 (2006).
Bianchi, M. T., Kim, S., Galvan, T., White, D. P. & Joffe, H. Nocturnal hot flashes: relationship to objective awakenings and sleep stage transitions. J. Clin. Sleep Med. 12, 1003–1009 (2016).
Joffe, H., Massler, A. & Sharkey, K. M. Evaluation and management of sleep disturbance during the menopause transition. Semin. Reprod. Med. 28, 404–421 (2010).
Polo-Kantola, P. Sleep problems in midlife and beyond. Maturitas 68, 224–232 (2011).
Kravitz, H. M. et al. Sleep difficulty in women at midlife: a community survey of sleep and the menopausal transition. Menopause 10, 19–28 (2003).
Kravitz, H. M. & Joffe, H. Sleep during the perimenopause: a SWAN story. Obstet. Gynecol. Clin. North Am. 38, 567–586 (2011).
Pien, G. W., Sammel, M. D., Freeman, E. W., Lin, H. & DeBlasis, T. L. Predictors of sleep quality in women in the menopausal transition. Sleep 31, 991–999 (2008).
Baker, F. C., Willoughby, A. R., Sassoon, S. A., Colrain, I. M. & de Zambotti, M. Insomnia in women approaching menopause: beyond perception. Psychoneuroendocrinology 60, 96–104 (2015).
Campbell, I. G. et al. Evaluation of the association of menopausal status with delta and beta EEG activity during sleep. Sleep 34, 1561–1568 (2011).
Jordan, A. S., McSharry, D. G. & Malhotra, A. Adult obstructive sleep apnoea. Lancet 383, 736–747 (2014).
Kerner, N. A. & Roose, S. P. Obstructive sleep apnea is linked to depression and cognitive impairment: evidence and potential mechanisms. Am. J. Geriatr. Psychiatry 24, 496–508 (2016).
Lal, C., DiBartolo, M. M., Kumbhare, S., Strange, C. & Joseph, J. E. Impact of obstructive sleep apnea syndrome on cognition in early postmenopausal women. Sleep Breath. 20, 621–626 (2016).
Freeman, E. W. et al. Hormones and menopausal status as predictors of depression in women in transition to menopause. Arch. Gen. Psychiatry 61, 62–70 (2004).
Bromberger, J. T. et al. Depressive symptoms during the menopausal transition: the study of women's health across the nation (SWAN). J. Affect. Disord. 103, 267–272 (2007).
Woods, N. F. et al. Depressed mood during the menopausal transition and early postmenopause: observations from the Seattle midlife women's health study. Menopause 15, 223–232 (2008).
Weber, M. T., Maki, P. M. & McDermott, M. P. Cognition & mood in perimenopause: a systematic review & meta-analysis. J. Steroid Biochem. Mol. Biol. 142, 90–98 (2014).
Bromberger, J. T. et al. Longitudinal change in reproductive hormones and depressive symptoms across the menopausal transition: results from the study of women's health across the nation (SWAN). Arch. Gen. Psychiatry 67, 598–607 (2010).
Kessler, R. C. et al. The epidemiology of major depressive disorder: results from the national comorbidity survey replication (NCS-R). JAMA. 289, 3095–3105 (2003).
Bromberger, J. T., Schott, L., Kravitz, H. M. & Joffe, H. Risk factors for major depression during midlife among a community sample of women with and without prior major depression: are they the same or different? Psychol Med. 45, 1653–1664 (2014).
Bromberger, J. T. et al. Major depression during and after the menopausal transition: study of women's health across the nation (SWAN). Psychol Med. 9, 1–10 (2011).
Freeman, E. W. Depression in the menopause transition: risks in the changing hormone milieu as observed in the general population. Womens Midlife Health 1, 1 (2015).
Bromberger, J. T. et al. Does risk for anxiety increase during the menopausal transition? Study of women's health across the nation (SWAN). Menopause 20, 488–495 (2013).
Weber, M. T., Mapstone, M., Staskiewicz, J. & Maki, P. M. Reconciling subjective memory complaints with objective memory performance in the menopausal transition. Menopause 19, 735–741 (2012).
Greendale, G. A. et al. Effects of the menopause transition and hormone use on cognitive performance in midlife women. Neurology 72, 1850–1857 (2009).
Epperson, C. N., Sammel, M. D. & Freeman, E. W. Menopause effects on verbal memory: findings from a longitudinal community cohort. J. Clin. Endocrinol. Metab. 98, 3829–3838 (2013).
Fuh, J. L., Wang, S. J., Lee, S. J., Lu, S. R. & Juang, K. D. A longitudinal study of cognition change during early menopausal transition in a rural community. Maturitas 53, 447–453 (2006).
Karlamangla, A. S., Lachman, M. E., Han, W., Huang, M. & Greendale, G. A. Evidence for cognitive aging in midlife women: study of women's health across the nation. PLoS One 12, e0169008 (2017).
Rocca, W. A. et al. Increased risk of cognitive impairment or dementia in women who underwent oophorectomy before menopause. Neurology 69, 1074–1083 (2007).
Kurita, K. et al. Association of bilateral oophorectomy with cognitive function in healthy, postmenopausal women. Fertil. Steril. 106, 749–756 (2016).
Greendale, G. A., Derby, C. A. & Maki, P. M. Perimenopause and cognition. Obstet. Gynecol. Clin. North Am. 38, 519–535 (2011).
Drogos, L. L. et al. Objective cognitive performance is related to subjective memory complaints in midlife women with moderate to severe vasomotor symptoms. Menopause 20, 10 (2013).
Medic, G., Wille, M. & Hemels, M. E. Short- and long-term health consequences of sleep disruption. Nat. Sci. Sleep 9, 151–161 (2017).
Ripa, P. et al. Migraine in menopausal women: a systematic review. Int. J. Womens Health 7, 773–782 (2015).
Freeman, E. W., Sammel, M. D., Lin, H., Gracia, C. R. & Kapoor, S. Symptoms in the menopausal transition: hormone and behavioral correlates. Obstet. Gynecol. 111, 127–136 (2008).
Martin, V. T. et al. Perimenopause and menopause are associated with high frequency headache in women with migraine: results of the American migraine prevalence and prevention study. Headache 56, 292–305 (2016).
Davis, S. R. et al. Understanding weight gain at menopause. Climacteric 15, 419–429 (2012).
Sternfeld, B. et al. Physical activity and changes in weight and waist circumference in midlife women: findings from the study of women's health across the nation. Am. J. Epidemiol. 160, 912–922 (2004).
Karvonen-Gutierrez, C. & Kim, C. Association of mid-life changes in body size, body composition and obesity status with the menopausal transition. Healthcare 4, E42 (2016).
Kanaley, J. A., Giannopoulou, I., Tillapaugh-Fay, G., Nappi, J. S. & Ploutz-Snyder, L. L. Racial differences in subcutaneous and visceral fat distribution in postmenopausal black and white women. Metabolism 52, 186–191 (2003).
Tchernof, A. et al. Ovarian hormone status and abdominal visceral adipose tissue metabolism. J. Clin. Endocrinol. Metab. 89, 3425–3430 (2004).
Lovejoy, J. C., Champagne, C. M., de Jonge, L., Xie, H. & Smith, S. R. Increased visceral fat and decreased energy expenditure during the menopausal transition. Int. J. Obes. 32, 949–958 (2008).
Janssen, I., Powell, L. H., Kazlauskaite, R. & Dugan, S. A. Testosterone and visceral fat in midlife women: the study of women's health across the nation (SWAN) fat patterning study. Obesity (Silver Spring) 18, 604–610 (2010).
Gibson, C. J., Thurston, R. C., El Khoudary, S. R., Sutton-Tyrrell, K. & Matthews, K. A. Body mass index following natural menopause and hysterectomy with and without bilateral oophorectomy. Int. J. Obes. 37, 809–813 (2013).
Pou, K. M. et al. Visceral and subcutaneous adipose tissue volumes are cross-sectionally related to markers of inflammation and oxidative stress: the Framingham Heart Study. Circulation 116, 1234–1241 (2007).
Lee, C. G. et al. Adipokines, inflammation, and visceral adiposity across the menopausal transition: a prospective study. J. Clin. Endocrinol. Metab. 94, 1104–1110 (2009).
Ravussin, E. & Smith, S. R. Increased fat intake, impaired fat oxidation, and failure of fat cell proliferation result in ectopic fat storage, insulin resistance, and type 2 diabetes mellitus. Ann. NY Acad. Sci. 967, 363–378 (2002).
El Khoudary, S. R. et al. Cardiovascular fat, menopause, and sex hormones in women: the SWAN cardiovascular fat ancillary study. J. Clin. Endocrinol. Metab. 100, 3304–3312 (2015).
Matthews, K. A. et al. Are changes in cardiovascular disease risk factors in midlife women due to chronological aging or to the menopausal transition? J. Am. Coll. Cardiol. 54, 2366–2373 (2009).
El Khoudary, S. R. et al. Increase HDL-C level over the menopausal transition is associated with greater atherosclerotic progression. J. Clin. Lipidol. 10, 962–969 (2016).
Mendelsohn, M. E. Mechanisms of estrogen action in the cardiovascular system. J. Steroid Biochem. Mol. Biol. 74, 337–343 (2000).
Taddei, S. Blood pressure through aging and menopause. Climacteric 1, 36–40 (2009).
Muka, T. et al. Association of age at onset of menopause and time since onset of menopause with cardiovascular outcomes, intermediate vascular traits, and all-cause mortality. JAMA Cardiol. 1, 767–776 (2016).
Parish, S. J. et al. Impact of vulvovaginal health on postmenopausal women: a review of surveys on symptoms of vulvovaginal atrophy. Int. J. Womens Health 5, 437–447 (2013).
Robinson, D. & Cardozo, L. D. The role of estrogens in female lower urinary tract dysfunction. Urology 6, 45–51 (2003).
Freedman, M. A. Perceptions of dyspareunia in postmenopausal women with vulvar and vaginal atrophy: findings from the REVIVE survey. Womens Health 10, 445–454 (2014).
Nappi, R. E. & Kokot-Kierepa, M. Vaginal health: insights, views and attitudes (VIVA) — results from an international survey. Climacteric 15, 36–44 (2012).
Nappi, R. E., Palacios, S., Panay, N., Particco, M. & Krychman, M. L. Vulvar and vaginal atrophy in four European countries: evidence from the European REVIVE Survey. Climacteric 19, 188–197 (2016).
Portman, D. J. & Gass, M. L. Genitourinary syndrome of menopause: new terminology for vulvovaginal atrophy from the International Society for the Study of Women's Sexual Health and the North American Menopause Society. Menopause 21, 1063–1068 (2014).
Waetjen, L. E. et al. Factors associated with worsening and improving urinary incontinence across the menopausal transition. Obstet. Gynecol. 111, 667–677 (2008).
Legendre, G., Ringa, V., Panjo, H., Zins, M. & Fritel, X. Incidence and remission of urinary incontinence at midlife: a cohort study. BJOG. 122, 816–824 (2015).
Botlero, R., Davis, S. R., Urquhart, D. M., Shortreed, S. & Bell, R. J. Age-specific prevalence of, and factors associated with, different types of urinary incontinence in community-dwelling Australian women assessed with a validated questionnaire. Maturitas 62, 134–139 (2009).
Avis, N. E. et al. Longitudinal changes in sexual functioning as women transition through menopause: results from the study of women's health across the nation (SWAN). Menopause 16, 442–452 (2009).
Nappi, P. R. et al. Female sexual dysfunction (FSD): prevalence and impact on quality of life (QoL). Maturitas 94, 87–91 (2016).
Avis, N. E. et al. Change in sexual functioning over the menopausal transition: results from the study of women's health across the nation. Menopause 24, 379–390 (2017).
Dundon, C. M. & Rellini, A. H. More than sexual function: predictors of sexual satisfaction in a sample of women age 40–70. J. Sex. Med. 7, 896–904 (2010).
Manolagas, S. C., O'Brien, C. A. & Almeida, M. The role of estrogen and androgen receptors in bone health and disease. Nat. Rev. Endocrinol. 9, 699–712 (2013).
van Staa, T. P., Dennison, E. M., Leufkens, H. G. & Cooper, C. Epidemiology of fractures in England and Wales. Bone 29, 517–522 (2001).
Finkelstein, J. S. et al. Bone mineral density changes during the menopause transition in a multiethnic cohort of women. J. Clin. Endocrinol. Metab. 93, 861–868 (2008).
Douchi, T. et al. Relative contribution of aging and menopause to changes in lean and fat mass in segmental regions. Maturitas 42, 301–306 (2002).
Maltais, M. L. Desroches, J. & Dionne, I. J. Changes in muscle mass and strength after menopause. J. Musculoskelet. Neuronal Interact. 9, 186–197 (2009).
Rolland, Y. M. et al. Loss of appendicular muscle mass and loss of muscle strength in young postmenopausal women. J. Gerontol. A Biol. Sci. Med. Sci. 62, 330–335 (2007).
Asikainen, T. M., Kukkonen-Harjula, K. & Miilunpalo, S. Exercise for health for early postmenopausal women: a systematic review of randomised controlled trials. Sports Med. 34, 753–778 (2004).
Srikanth, V. K. et al. A meta-analysis of sex differences prevalence, incidence and severity of osteoarthritis. Osteoarthritis Cartilage 13, 769–781 (2005).
Felson, D. T. Developments in the clinical understanding of osteoarthritis. Arthritis Res. Ther. 11, 203 (2009).
Nadkar, M. Y., Samant, R. S., Vaidya, S. S. & Borges, N. E. Relationship between osteoarthritis of knee and menopause. J. Assoc. Physicians India 47, 1161–1163 (1999).
Calleja-Agius, J. & Brincat, M. The effect of menopause on the skin and other connective tissues. Gynecol. Endocrinol. 28, 273–277 (2012).
Archer, D. F. Postmenopausal skin and estrogen. Gynecol. Endocrinol. 28, 2–6 (2012).
Grishina, I., Fenton, A. & Sankaran-Walters, S. Gender differences, aging and hormonal status in mucosal injury and repair. Aging Dis. 5, 160–169 (2014).
Herskovitz, I. & Tosti, A. Female pattern hair loss. Int. J. Endocrinol. Metab. 11, e986 (2013).
MacPherson, K. Menopause as disease: the social construction of a metaphor. Adv. Nurs. Sci. 3, 95–114 (1981).
Nusrat, N. et al. Knowledge, attitude and experience of menopause. J. Ayub Med. Coll. Abbottabad 20, 56–59 (2008).
Opree, S. J. & Kalmijn, M. Exploring causal effects of combining work and intergenerational support on depressive symptoms among middle-aged women. Ageing Soc. 32, 130–146 (2012).
Lyons, A. C. & Griffin, C. Managing menopause: a qualitative analysis of self-help literature for women at midlife. Soc. Sci. Med. 56, 1629–1642 (2003).
Hall, L. et al. Meanings of menopause. J. Holist. Nurs. 25, 106–118 (2016).
Gartoulla, P., Bell, R. J., Worsley, R. & Davis, S. R. Moderate-severely bothersome vasomotor symptoms are associated with lowered psychological general wellbeing in women at midlife. Maturitas 81, 487–492 (2015).
Sarti, S. & Zella, S. Changes in the labour market and health inequalities during the years of the recent economic downturn in Italy. Soc. Sci. Res. 57, 116–132 (2016).
Jack, G. et al. Menopause in the workplace: what employers should be doing. Maturitas 85, 88–95 (2016).
Gartoulla, P. et al. Menopausal vasomotor symptoms are associated with poor self-assessed work ability. Maturitas 87, 33–39 (2016).
Pinkerton, J. A. Money talks: untreated hot flashes cost women, the workplace, and society. Menopause 22, 254–255 (2015).
Payne, S. & Doyal, L. Older women, work and health. Occup. Med. 60, 172–177 (2010).
Schoenaker, D. A., Jackson, C. A., Rowlands, J. V. & Mishra, G. D. Socioeconomic position, lifestyle factors and age at natural menopause: a systematic review and meta-analyses of studies across six continents. Int. J. Epidemiol. 43, 1542–1562 (2014).
Genazzani, A. R. et al. The European menopause survey 2005: women's perceptions on menopause and postmenopause hormone therapy. Gynecol. Endocrinol. 22, 369–375 (2006).
Chedraui, P., Aguirre, W., Hidalgo, L. & Fayad, L. Assessing menopausal symptoms among healthy middle-aged women with the menopause rating scale. Maturitas 57, 271–278 (2007).
Chedraui, P., San Miguel, G. & Avila, C. Quality of life impairment during the female menopausal transition is related to personal and partner factors. Gynecol. Endocrinol. 25, 130–135 (2009).
Green, R. & Santoro, N. Menopausal symptoms and ethnicity: the study of women's health across the nation. Womens Health (Lond.) 5, 127–133 (2009).
Islam, R. M., Bell, R. J., Rizvi, F. & Davis, S. R. Vasomotor symptoms in women in Asia appear comparable with women in Western countries: a systematic review. Menopause 24, 1313–1322 (2017).
Sriprasert, I. et al. An International menopause society study of vasomotor symptoms in Bangkok and Chiang Mai, Thailand. Climacteric 20, 171–177 (2017).
Al Dughaither, A., Al Mutairy, H. & Al Ateeq, M. Menopausal symptoms and quality of life among Saudi women visiting primary care clinics in Riyadh, Saudi Arabia. Int. J. Womens Health. 29, 645–653 (2015).
Stefanopoulou, E. et al. IMS study of climate, altitude, temperature and vasomotor symptoms in the United Arab Emirates. Climacteric 17, 425–432 (2014).
Stefanopoulou, E. et al. An International menopause society study of climate, altitude, temperature (IMS-CAT) and vasomotor symptoms in urban Indian regions. Climacteric 17, 417–424 (2014).
Gold, E. B. et al. Longitudinal analysis of the association between vasomotor symptoms and race/ethnicity across the menopausal transition: study of women's health across the nation. Am. J. Public Health 96, 1226–1235 (2006).
Hunter, M. S. et al. The International menopause study of climate, altitude, temperature (IMS-CAT) and vasomotor symptoms. Climacteric 16, 8–16 (2013).
Schmiegelow, M. D. et al. Race and ethnicity, obesity, metabolic health, and risk of cardiovascular disease in postmenopausal women. J. Am. Heart Assoc. 4, e001695 (2015).
Wolff, E. et al. Skin wrinkles and rigidity in early postmenopausal women vary by race/ethnicity: baseline characteristics of the skin ancillary study of the KEEPS trial. Fertil. Steril. 95, 658–662 (2011).
Chua, Y. et al. Genitourinary syndrome of menopause in five Asian countries: results from the Pan-Asian REVIVE survey. Climacteric 20, 367–373 (2017).
Cauley, J. A., Chalhoub, D., Kassem, A. M. & Fuleihan, G. E.-H. Geographic and ethnic disparities in osteoporotic fractures. Nat. Rev. Endocrinol. 10, 338–351 (2014).
Johnell, O., Gullberg, B., Allander, E. & Kanis, J. A. The apparent incidence of hip fracture in Europe: a study of national register sources. Osteoporos. Int. 2, 298–302 (1992).
Xia, W. B. et al. Rapidly increasing rates of hip fracture in Beijing, China. J. Bone Miner. Res. 27, 125–129 (2012).
Freeman, E. W. & Sammel, M. D. Anxiety as a risk factor for menopausal hot flashes: evidence from the penn ovarian aging cohort. Menopause 23, 942–949 (2016).
Vegunta, S. et al. The association between recent abuse and menopausal symptom bother: results from the data registry on experiences of aging, menopause, and sexuality (DREAMS). Menopause 23, 494–498 (2016).
Hautamäki, H. et al. Premenstrual symptoms in fertile age are associated with impaired quality of life, but not hot flashes, in recently postmenopausal women. Menopause 21, 1287–1291 (2014).
Drost, J. T., van der Schouw, Y. T., Herber-Gast, G. C. & Maas, A. H. More vasomotor symptoms in menopause among women with a history of hypertensive pregnancy diseases compared with women with normotensive pregnancies. Menopause 20, 1006–1011 (2013).
Thurston, R. C. et al. Adiposity and reporting of vasomotor symptoms among midlife women: the study of women's health across the nation. Am. J. Epidemiol. 167, 78–85 (2008).
Thurston, R. C. et al. Gains in body fat and vasomotor symptom reporting over the menopausal transition: the study of women's health across the nation. Am. J. Epidemiol. 170, 766–774 (2009).
Gold, E. B. et al. Longitudinal analysis of changes in weight and waist circumference in relation to incident vasomotor symptoms: the study of women's health across the nation (SWAN). Menopause 24, 9–26 (2017).
Thurston, R. C., Chang, Y., Mancuso, P. & Matthews, K. A. Adipokines, adiposity, and vasomotor symptoms during the menopause transition: findings from the study of women's health across the nation. Fertil. Steril. 100, 793–800 (2013).
Pastore, L. M., Carter, R. A., Hulka, B. S. & Wells, E. Self-reported urogenital symptoms in postmenopausal women: women's health initiative. Maturitas 49, 292–303 (2004).
Waetjen, L. E. et al. Association between menopausal transition stages and developing urinary incontinence. Obstet. Gynecol. 114, 989–998 (2009).
Ensrud, K. E., Cauley, J., Lipschutz, R. & Cummings, S. R. Weight change and fractures in older women. Study of osteoporotic fractures research group. Arch. Intern. Med. 157, 857–863 (1997).
Crandall, C. J. et al. Postmenopausal weight change and incidence of fracture: post hoc findings from women's health initiative observational study and clinical trials. BMJ 350, h25 (2015).
Looby, S. E. et al. Increased hot flash severity and related interference in perimenopausal human immunodeficiency virus-infected women. Menopause 21, 403–409 (2014).
Prairie, B. A. et al. Symptoms of depressed mood, disturbed sleep, and sexual problems in midlife women: cross-sectional data from the study of women's health across the nation. J. Womens Health (Larchmt) 24, 119–126 (2015).
Hale, G. E., Hughes, C. L., Burger, H. G., Robertson, D. M. & Fraser, I. S. Atypical estradiol secretion and ovulation patterns caused by luteal out-of-phase (LOOP) events underlying irregular ovulatory menstrual cycles in the menopausal transition. Menopause 16, 50–59 (2009).
Fogle, R. H. et al. Ovarian androgen production in postmenopausal women. J. Clin. Endocrinol. Metab. 92, 3040–3043 (2007).
McConnell, D. S., Stanczyk, F. Z., Sowers, M. R., Randolph, J. F. & Lasley, B. L. Menopausal transition stage-specific changes in circulating adrenal androgens. Menopause 19, 658–663 (2012).
Freedman, R. R. Hot flashes: behavioral treatments, mechanisms, and relation to sleep. Am. J. Med. 118, 124–130 (2005).
Rossmanith, W. G. & Ruebberdt, W. What causes hot flushes? The neuroendocrine origin of vasomotor symptoms in the menopause. Gynecol. Endocrinol. 25, 303–314 (2009).
Boulant, J. A. Role of the preoptic-anterior hypothalamus in thermoregulation and fever. Clin. Infect. Dis. 31, S157–S161 (2000).
Hale, G. E., Hitchcock, C. L., Williams, L. A., Vigna, Y. M. & Prior, J. C. Cyclicity of breast tenderness and night-time vasomotor symptoms in mid-life women: information collected using the Daily Perimenopause Diary. Climacteric 6, 128–139 (2003).
Rance, N. E., Dacks, P. A., Mittelman-Smith, M. A., Romanovsky. A. A. & Krajewski-Hall, S. J. Modulation of body temperature and LH secretion by hypothalamic KNDy (kisspeptin, neurokinin B and dynorphin) neurons: a novel hypothesis on the mechanism of hot flushes. Front. Neuroendocrinol. 34, 211–227 (2013).
Woods, N. F., Carr, M. C., Tao, E. Y., Taylor, H. J. & Mitchell, E. S. Increased urinary cortisol levels during the menopausal transition. Menopause 13, 212–221 (2006).
Gibson, C. J., Thurston, R. C. & Matthews, K. A. Cortisol dysregulation is associated with daily diary-reported hot flashes among midlife women. Clin. Endocrinol. 85, 645–651 (2016).
Gordon, J. L. et al. Cardiovascular, hemodynamic, neuroendocrine, and inflammatory markers in women with and without vasomotor symptoms. Menopause 23, 1189–1198 (2016).
Freeman, E. W. et al. Symptoms associated with menopausal transition and reproductive hormones in midlife women. Obstet. Gynecol. 110, 230–240 (2007).
Kravitz, H. M. et al. Relationship of day-today reproductive hormone levels to sleep in midlife women. Arch. Intern. Med. 165, 2370–2376 (2015).
Pines, A. Circadian rhythm and menopause. Climacteric 19, 551–552 (2016).
Andersen, M. L., Bittencourt, L. R., Antunes, I. B. & Tufik, S. Effects of progesterone on sleep: a possible pharmacological treatment for sleep-breathing disorders? Curr. Med. Chem. 13, 3575–3582 (2006).
Genazzani, A. R., Pluchino, N., Luisi, S. & Luisi, M. Estrogen, cognition and female ageing. Hum. Reprod. Update 13, 175–187 (2007).
Blair, J. A. et al. Luteinizing hormone downregulation but not estrogen replacement improves ovariectomy-associated cognition and spine density loss independently of treatment onset timing. Horm. Behav. 78, 60–66 (2016).
Short, R. A., Bowen, R. L., O'Brien, P. C. & Graff-Radford, N. R. Elevated gonadotropin levels in patients with Alzheimer disease. Mayo Clin. Proc. 76, 906–909 (2001).
Casadesus, G. et al. Evidence for the role of gonadotropin hormones in the development of Alzheimer disease. Cell. Mol. Life Sci. 62, 293–298 (2005).
Wöber, C. et al. Prospective analysis of factors related to migraine attacks: the PAMINA study. Cephalalgia 27, 304–314 (2007).
Karkhaneh, A., Ansari, M., Emamgholipour, S. & Rafiee, M. H. The effect of 17β-estradiol on gene expression of calcitonin gene-related peptide and some pro-inflammatory mediators in peripheral blood mononuclear cells from patients with pure menstrual migraine. Iran. J. Basic Med. Sci. 18, 894–901 (2015).
Schmidt, P. J. & Rubinow, D. R. Sex hormones and mood in the perimenopause. Ann. NY Acad. Sci. 1179, 70–85 (2010).
Avis, N. E., Brambilla, D., McKinlay, S. M. & Vass, K. A longitudinal analysis of the association between menopause and depression. Results from the Massachusetts women's health study. Ann. Epidemiol. 4, 214–220 (1994).
Freeman, E. W., Sammel, M. D., Boorman, D. W. & Zhang, R. Longitudinal pattern of depressive symptoms around natural menopause. JAMA Psychiatry. 71, 36–43 (2014).
Gordon, J. L. et al. Ovarian hormone fluctuation, neurosteroids, and HPA axis dysregulation in perimenopausal depression: a novel heuristic model. Am. J. Psychiatry. 172, 227–236 (2015).
Gordon, J. L., Eisenlohr-Moul, T. A., Rubinow, D. R., Schrubbe, L. & Girdler, S. S. Naturally occurring changes in estradiol concentrations in the menopause transition predict morning cortisol and negative mood in perimenopausal depression. Clin. Psychol. Sci. 4, 919–935 (2016).
Gordon, J. L., Rubinow, D. R., Eisenlohr-Moul, T. A., Leserman, J. & Girdler, S. S. Estradiol variability, stressful life events, and the emergence of depressive symptomatology during the menopausal transition. Menopause 23, 257–266 (2016).
Nappi, R. E. & Palacios, S. Impact of vulvovaginal atrophy on sexual health and quality of life at postmenopause. Climacteric 17, 3–9 (2014).
MacBride, M. B., Rhodes, D. J. & Shuster, L. T. Vulvo-vaginal atrophy. Mayo Clin. Proc. 85, 87–94 (2010).
Mannella, P., Palla, G., Bellini, M. & Simoncini, T. The female pelvic floor through midlife and aging. Maturitas 76, 230–234 (2013).
Randolph, J. F. Jr, Zheng, H., Avis, N. E., Greendale, G. A. & Harlow, S. D. Masturbation frequency & sexual function domains are associated with serum reproductive hormone levels across the menopausal transition. J. Endocrinol. Metab 100, 258–266 (2015).
Woods, N. F., Mitchell, E. S. & Smith-Di Julio, K. Sexual desire during the menopausal transition & early postmenopause: observations from the Seattle midlife women's health study. J. Womens Health (Larchmt) 19, 209–218 (2010).
Dennerstein, L., Lehert, P. & Burger, H. The relative effects of hormones and relationship factors on sexual function of women through the natural menopausal transition. Fertil. Steril. 84, 174–180 (2005).
Janssen, I., Powell, L. H., Jasielec, M. S. & Kazlauskaite, R. Covariation of change in bioavailable testosterone and adiposity in midlife women. Obesity (Silver Spring) 23, 488–494 (2015).
Björntorp, P. Hormonal control of regional fat distribution. Hum. Reprod. 12, 21–25 (1997).
Guthrie, J. R. et al. Central abdominal fat and endogenous hormones during the menopausal transition. Fertil. Steril. 79, 1335–1340 (2003).
Liu, X. M. et al. FSH regulates fat accumulation and redistribution in aging through the Gαi/Ca2+ pathway. Aging Cell 14, 409–420 (2015).
Kalyani, R. R. et al. The association of endogenous sex hormones, adiposity, and insulin resistance with incident diabetes in postmenopausal women. J. Clin. Endocrinol. Metab. 94, 4127–4135 (2009).
Gaspard, U. Hyperinsulinaemia, a key factor of the metabolic syndrome in postmenopausal women. Maturitas 62, 362–365 (2009).
Leeners, B., Geary, N., Tobler, P. N. & Asarian, L. Ovarian hormones and obesity. Hum. Reprod. Update. 23, 300–321 (2017).
Maric-Bilkan, C. & Manigrasso, M. B. Sex differences in hypertension: contribution of the renin-angiotensin system. Gend. Med. 9, 287–291 (2012).
Simoncini, T. et al. Interaction of oestrogen receptor with the regulatory subunit of phosphatidylinositol-3-OH kinase. Nature 407, 538–541 (2000).
Wiik, A., Ekman, M., Johansson, O., Jansson, E. & Esbjornsson, M. Expression of both oestrogen receptor alpha and beta in human skeletal muscle tissue. Histochem. Cell Biol. 131, 181–189 (2009).
Lowe, D. A., Baltgalvis, K. A. & Greising, S. M. Mechanisms behind estrogen's beneficial effect on muscle strength in females. Exerc. Sport Sci. Rev. 38, 61–67 (2010).
Fanciulli, G., Delitala, A. & Delitala, G. Growth hormone, menopause and ageing: no definite evidence for 'rejuvenation' with growth hormone. Hum. Reprod. Update 15, 341–358 (2009).
Cosma, M., Joy, B., Miles, J. M., Bowers, C. Y. & Veldhuis, J. D. Pituitary and/or peripheral estrogen-receptor regulates follicle-stimulating hormone secretion, whereas central estrogenic pathways direct growth hormone and prolactin secretion in postmenopausal women. J. Clin. Endocrinol. Metab. 93, 951–958 (2008).
Janssen, I., Heymsfield, S. B., Wang, Z. M. & Ross, R. Skeletal muscle mass & distribution in 468 men & women aged 18–88 yr. J. Appl. Physiol. 89, 81–88 (2000).
Clasey, J. L. et al. Abdominal visceral fat and fasting insulin are important predictors of 24-hour GH release independent of age, gender, and other physiological factors. J. Clin. Endocrinol. Metab. 86, 3845–3852 (2001).
Carville, S. F., Rutherford, O. M. & Newham, D. J. Power output, isometric strength and steadiness in the leg muscles of pre- and postmenopausal women; the effects of hormone replacement therapy. Eur. J. Appl. Physiol. 96, 292–298 (2006).
Cooper, R., Mishra, G., Clennell, S., Guralnik, J. & Kuh, D. Menopausal status and physical performance in midlife: findings from a British birth cohort study. Menopause 15, 1079–1085 (2008).
Kurina, L. M. et al. The effect of menopause on grip and pinch strength: results from the Chicago, Illinois, site of the study of women's health across the nation. Am. J. Epidemiol. 160, 484–491 (2004).
Yuki, A., Ando, F., Otsuka, R. & Shimokata, H. Low free testosterone is associated with loss of appendicular muscle mass in Japanese community-dwelling women. Geriatr. Gerontol. Int. 15, 326–333 (2015).
Garnero, P., Sornay-Rendu, E., Chapuy, M. C. & Delmas, P. D. Increased bone turnover in late postmenopausal women is a major determinant of osteoporosis. J. Bone Miner. Res. 11, 337–349 (1996).
Eastell, R. et al. Postmenopausal osteoporosis. Nat. Rev. Dis. Primers. 29, 16069 (2016).
Roman-Blas, J. A., Castaneda, S., Largo, R. & Herrero-Beaumont, G. Osteoarthritis associated with estrogen deficiency. Arthritis Res. Ther. 11, 241 (2009).
Hanna, F. S. et al. Women have increased rates of cartilage loss and progression of cartilage defects at the knee than men: a gender study of adults without clinical knee osteoarthritis. Menopause 16, 666–670 (2009).
Henry, F., Piérard-Franchimont, C., Cauwenbergh, G. & Piérard, G. E. Age-related changes in facial skin contours and rheology. J. Am. Geriatr. Soc. 45, 220–222 (1997).
Piérard-Franchimont, C. & Piérard, G. E. Alterations in hair follicle dynamics in women. Biomed Res. Int. 2013, 957432 (2013).
Blume-Peytavi, U., Atkin, S., Gieler, U. & Grimalt, R. Skin academy: hair, skin, hormones and menopause — current status/knowledge on the management of hair disorders in menopausal women. Eur. J. Dermatol. 22, 310–318 (2012).
Price, V. Androgenic alopecia in women. J. Investig. Dermatol. Symp. Proc. 8, 24–27 (2003).
Thurston, R. C. et al. Hot flashes and carotid intima media thickness among midlife women. Menopause 18, 352–358 (2011).
Thurston, R. C., Sutton-Tyrrell, K., Everson-Rose, S. A., Hess, R. & Matthews, K. A. Hot flashes and subclinical cardiovascular disease: findings from the study of women's health across the nation heart study. Circulation 118, 1234–1240 (2008).
Thurston, R. C. et al. Changes in heart rate variability during vasomotor symptoms among midlife women. Menopause 23, 499–505 (2016).
Silveira, J. S., Clapauch, R., Souza, M. D. & Bouskela, E. Hot flashes: emerging cardiovascular risk factors in recent and late postmenopause and their association with higher blood pressure. Menopause 23, 846–855 (2016).
Thurston, R. C. et al. Are vasomotor symptoms associated with alterations in hemostatic and inflammatory markers? Findings from the study of women's health across the nation. Menopause 18, 1044–1051 (2011).
Thurston, R. C. et al. Menopausal symptoms and cardiovascular disease mortality in the women's ischemia syndrome evaluation (WISE). Menopause 24, 126–132 (2016).
Matthews, K. A. et al. Do reports of sleep disturbance relate to coronary and aortic calcification in healthy middle-aged women? Study of women's health across the nation. Sleep Med. 14, 282–287 (2013).
Thurston, R. C. et al. Sleep characteristics and carotid atherosclerosis among midlife women. Sleep https://doi.org/10.1093/sleep/zsw052 (2016).
de Kruif, M., Spijker, A. T. & Molendijk, M. L. Depression during the perimenopause: a meta-analysis. J. Affect. Disord. 206, 174–180 (2016).
Joffe, H. et al. Independent contributions of nocturnal hot flashes and sleep disturbance to depression in estrogen-deprived women. J. Clin. Endocrinol. Metab. 101, 3847–3855 (2016).
Ownby, R. L., Crocco, E., Acevedo, A., John, V. & Loewenstein, D. Depression and risk for Alzheimer disease: systematic review, meta-analysis, and metaregression analysis. Arch. Gen. Psychiatry 63, 530–538 (2006).
Terauchi, M. et al. Prevalence and predictors of storage lower urinary tract symptoms in perimenopausal and postmenopausal women attending a menopause clinic. Menopause 22, 1084–1090 (2015).
Erekson, E. A., Li, F. Y., Martin, D. K. & Fried, T. R. Vulvovaginal symptoms prevalence in postmenopausal women and relationship to other menopausal symptoms and pelvic floor disorders. Menopause 23, 368–375 (2016).
Crandall, C. J. et al. Associations of menopausal vasomotor symptoms with fracture incidence. J. Clin. Endocrinol. Metab. 100, 524–534 (2015).
Levine, M. E. et al. Menopause accelerates biological aging. Proc. Natl Acad. Sci. USA 113, 9327–9332 (2016).
Harlow, S. D. et al. Executive summary of the stages of reproductive aging workshop +10: addressing the unfinished agenda of staging reproductive aging. Fertil. Steril. 97, 843–851 (2012).
Author information
Authors and Affiliations
Contributions
P.M., G.M. and A.G. researched data for the article. All authors made a substantial contribution to discussion of content, wrote the manuscript and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Glossary
- Hot flashes
-
A sudden wave of body heat accompanied by reddening of the face and neck and profuse sweating, sometimes followed by a feeling of cold and shivering.
- Ovarian failure
-
The definite loss of function of the ovaries.
- Postmenopause
-
The period of a woman's life that follows the final menstrual period.
- Perimenopause
-
The period of a woman's life that encompasses the menopausal transition and the first year following the final menstrual period.
- Amenorrhoea
-
The absence of menstrual periods for 3 or more consecutive months in a woman of reproductive age.
- Obstructive sleep apnoea
-
A sleeping disorder caused by repetitive upper airway collapse during sleep, leading to intermittent hypoxia and characterized by loud snoring, apnoea during sleep, insomnia, excessive daytime sleepiness, morning headache and fatigue.
- Surgical menopause
-
Menopause induced by the surgical removal of the ovaries.
- Visceral adiposity
-
Accumulation of adipose tissue in the abdomen and around internal organs.
- Premenstrual syndrome
-
A heterogeneous group of emotional symptoms, such as irritability and food cravings, and physical symptoms, such as bloating, breast tenderness and abdominal pain, that precede the menstrual period.
- Anovulation
-
The absence of ovulation.
- Urethral closure pressure
-
The fluid pressure needed to open a closed urethra.
- Valsalva leak-point pressure
-
The lowest abdominal pressure required during a stress activity that causes the urethra to open and leak.
- Free androgen index
-
An index that represents the ratio of bioactive circulating testosterone.
- Cardiac vagal control
-
An index of parasympathetic contribution to cardiac regulation.
- Cardiac index
-
The volume of blood pumped by the heart in a minute per body surface.
- Stroke volume index
-
The volume of blood pumped by the heart with each beat per body surface.
- Vascular resistance index
-
An index representing the degree to which blood vessels impede the flow of blood.
Rights and permissions
About this article
Cite this article
Monteleone, P., Mascagni, G., Giannini, A. et al. Symptoms of menopause — global prevalence, physiology and implications. Nat Rev Endocrinol 14, 199–215 (2018). https://doi.org/10.1038/nrendo.2017.180
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrendo.2017.180
This article is cited by
-
Translation and validation of menopause quick 6 (MQ6) into the Malay language
BMC Primary Care (2024)
-
Abdominal obesity as assessed by anthropometric measures associates with urinary incontinence in females: findings from the National Health and Nutrition Examination Survey 2005–2018
BMC Women's Health (2024)
-
Menopausal hormone therapy and breast cancer risk: a population-based cohort study of 1.3 million women in Norway
British Journal of Cancer (2024)
-
Effects of melatonin intake on depression and anxiety in postmenopausal women: a systematic review and meta-analysis of randomised controlled trials
Archives of Women's Mental Health (2024)
-
MicroRNAs regulate the vicious cycle of vascular calcification-osteoporosis in postmenopausal women
Molecular Biology Reports (2024)