Abstract
Epithelial-to-mesenchymal transition (EMT) and apoptosis of peritoneal mesothelial cells are known to be the earliest mechanisms of peritoneal fibrosis in peritoneal dialysis (PD). Endoplasmic reticulum (ER) stress with an unfolded protein response is regarded to have a role in the development of organ fibrosis. To investigate the potential role of ER stress as a target to prevent and/or delay the development of peritoneal fibrosis, we examined the effect of ER stress on EMT or apoptosis of human peritoneal mesothelial cells (HPMCs) and elucidated the mechanisms underlying the protective effect of ER stress preconditioning on TGF-β1-induced EMT. ER stress inducers, tunicamycin (TM) and thapsigargin (TG), induced EMT with Smad2/3 phosphorylation, an increased nuclear translocation of β-catenin and Snail expression. Low concentrations of TM and TG did not induce apoptosis within 48 h; however, high concentrations of TM- (>1 ng/ml) and TG- (>1 nM) induced apoptosis at 12 h with a persistent increase in C/EBP homologous protein. TGF-β1 induced EMT and apoptosis in HPMCs, which was ameliorated by taurine-conjugated ursodeoxycholic acid, an ER stress blocker. Interestingly, pre-treatment with TM or TG for 4 h also protected the cells from TGF-β1-induced EMT and apoptosis, demonstrating the role of ER stress as an adaptive response to protect HPMCs from EMT and apoptosis. Peritoneal mesothelial cells isolated from PD patients displayed an increase in GRP78/94, which was correlated with the degree of EMT. These findings suggest that the modulation of ER stress in HPMCs could serve as a novel approach to ameliorate peritoneal damage in PD patients.
Similar content being viewed by others
Main
Peritoneal dialysis (PD) is one of the modalities for the treatment of end-stage renal disease (ESRD), which is based on the use of the peritoneum as a living dialysis membrane.1, 2, 3 Continuous exposure to nonphysiologic PD solutions and episodes of peritonitis cause damage to the peritoneum, which results in functional and structural deterioration of the peritoneal membrane.4, 5, 6 Previous studies suggested that peritoneal mesothelial cells underwent phenotype transition, epithelial-to-mesenchymal transition (EMT), during the process of PD.7, 8, 9, 10, 11 Because EMT is known to be a reversible process, it can be a therapeutic target for preserving peritoneal membrane function.8, 9, 11, 12, 13 In addition to EMT, apoptosis of the peritoneal mesothelial cells is also believed to be one of the early mechanisms of peritoneal damage. The accumulation of misfolded proteins and the induction of endoplasmic reticulum (ER) stress have been implicated in the development of phenotypic transition and apoptosis of epithelial cells.14, 15, 16, 17 ER stress is reported to induce EMT of epithelial cells in the kidney and lung, which may result in fibroblast accumulation.15, 18, 19, 20, 21, 22 The ER has a key role in the maintenance of protein homeostasis through its control of the content, structure, folding and trafficking of proteins.23, 24, 25 The accumulation of unfolded proteins in the ER lumen results in a release of glucose-regulated protein (GRP)78/94, a central regulator of ER stress, from the ER membrane, which allows GRP78/94 to either dimerize or move to other locations within cells.26, 27 This process initiates unfolded protein response (UPR) signaling to reestablish homeostasis and normal ER function through the activation of pathways involving inositol-requiring enzyme 1,28 double-stranded RNA-activated protein kinase-like ER kinase (PERK),29 and activating transcription factor 6 (ATF6).30, 31
Peritoneal dialysate has been reported to induce ER stress in mesothelial cells;32 however, no studies have addressed the role of ER stress in peritoneal EMT and fibrosis. This study was undertaken to investigate whether ER stress per se induced EMT and apoptosis of peritoneal mesothelial cells and whether ER stress modulation protected the peritoneum from EMT and apoptosis induced by TGF-β1.
MATERIALS AND METHODS
Reagents
All of the chemicals and tissue culture plates were obtained from Sigma-Aldrich (St Louis, MO, USA) and Nunc Labware (Waltham, MA, USA), unless otherwise stated.
Isolation and Maintenance of HPMCs
Human peritoneal mesothelial cells (HPMCs) were isolated and maintained using a previously published method.33 All of the experiments were performed using cells between the second and fourth passages. Tissue collection was approved by the ethics committee of the institution (ECT 1647-35), and informed consent was obtained from each patient.
Cell Morphology and Immunofluorescence Analysis of HPMCs
Cell morphology was analyzed under an inverted phase-contrast microscope (Axiovert 200; Carl Zeiss, Oberkochen, Germany), and the images were obtained using a digital camera (AxioCam HRC; Carl Zeiss). For immunofluorescence staining, the cells were washed and fixed in 4% phosphate-buffered paraformaldehyde (25 min at 20 °C) and permeabilized with 1% Triton X-100 in PBS (15 min at 4 °C). After washing with PBS, the cells were treated with 5% BSA in PBS for 1 h before incubation with primary antibodies specific for ZO-1 (Invitrogen, CA, USA), α-SMA (Abcam, Cambridge, MA, USA), or β-catenin (Santa Cruz Biotechnology, Santa Cruz, CA, USA) in 5% BSA overnight at 4 °C. The cells were then washed with 0.2% Tween 20 in PBS before incubation with a goat anti-mouse IgG-FITC-conjugated secondary antibody (Santa Cruz Biotechnology) for 1 h at room temperature in the dark. The nucleus was counterstained with DAPI, and the cells were visualized under the Axiovert 200 fluorescence microscope with 10 × 10 and 20 × 10 NA objectives equipped with an AxioCam HRC digital camera.
Western Blotting
Protein samples were isolated from the cell lysate (30 μg) and mixed in reducing buffer, boiled, resolved on 10% SDS-PAGE gels, and transferred to a polyvinylidene difluoride membrane by electroblotting. The blot was incubated overnight at 4 °C in a blocking solution with primary antibodies directed to the following antigens: GRP78/94 (Enzo Life Sciences, Plymouth, PA, USA); p-PERK, p-eIF2α, ATF4, ATF6, CHOP (Cell signaling Technology, Danvers, MA, USA); E-cadherin (BD Bioscience, Bedford, MA, USA); α-SMA (Abcam), β-catenin, Lamin B1, p-Smad2, p-Smad3 Smad2, Smad3, Snail, cleaved Caspase-3 and β-actin (Santa Cruz Biotechnology). After washing the blots with PBS/Tween 20, they were incubated with horseradish peroxidase-conjugated secondary antibodies corresponding to each primary antibody, followed by enhanced chemiluminescence detection (Santa Cruz Biotechnology). The positive immunoreactive bands were quantified by densitometry and compared with the expression of human β-actin.
Extraction of Nuclear and Cytoplasmic Fraction
HPMCs were collected and washed with PBS before addition of the cytoplasmic lysis buffer. Cells were lysed for 10 min on ice and then quick-spun for 15 s to collect cytosolic lysate. Pellets were washed two times with cytoplasmic lysis buffer (10 mM Hepes at pH 8.0, 1.5 mM MgCl2, 10 mM KCl, 0.5 mM DTT, 300 mM sucrose, 0.1% NP-40, 10 mM NaF, 20 mM β-glycerophosphate, 10 mM Na3VO4, 1 × protease inhibitors, and 0.5 mM PMSF) and then lysed with nuclear lysis buffer (50 mM Hepes at pH 7.9, 250 mM KCl, 0.1 mM EDTA, 0.1 mM EGTA, 0.1% NP-40, 0.1% glycerol, 10 mM NaF, 10 mM Na3VO4, 1 mM DTT, 1 × protease inhibitors, and 0.5 mM PMSF) for 30 min on ice. The lysates were spun for 20 min at 14 000 r.p.m. at 4 °C to collect nuclear lysates. Lysates were run in SDS-PAGE for Western blot analysis.
Reverse Transcriptase-PCR Analysis for X-Box-Binding Protein 1 (XBP-1) Splicing
The splicing of XBP-1 mRNA was detected by semiquantitative real-time PCR (RT-PCR) using primers specific for XBP-1, which detected both the unspliced (424 bp) and spliced (398 bp) isoforms: (forward primer: 5'-CTGGAAAGCAAGTGGTAGA-3', reverse primer: 5'-CTGGGTCCTTCTGGGTAGAC-3') or β-actin: (forward primer: 5'-TTCTGACCCATGCCCACCAT-3', reverse primer: 5'-ATGGATGATATCGCCGCGCTC-3').
Quantitative RT-PCR Analysis
The levels of transcripts were determined by RT-PCR on the ABI PRISM 7000 sequence detection system using SYBR Green I as a double-stranded DNA-specific dye according to the manufacturer’s instructions (Applied Biosystems, Foster City, CA, USA). The PCR reaction was carried out using 5 μM of cDNA, 10 μM of SYBR Green PCR master mix, and 5 pM of sense and antisense primers of E-cadherin: (forward primer: 5'-ACCCCTGTTGGTGTCTTT-3', reverse primer: 5'-TTCGGGCTTGTTGTCATTCT-3') or α-SMA: (forward primer: 5'-GGGAATGGGACAAAAAGACA-3', reverse primer: 5'-CTTCAGGGGCAACACGAA-3') in a final volume of 20 μl/reaction. The relative mRNA expression levels of the target genes in each sample were calculated using the comparative CT method. The CT value is the cycle number at which the fluorescence signal is greater than a defined threshold. At least three independent PCR procedures were performed to allow statistical analysis. The amount of PCR products was normalized with the house-keeping gene, β-actin.
Transfection of siRNA
To determine the effect of Smad2/3 gene silencing on ER stress-induced EMT of HPMCs, we treated HPMCs with human Smad2 and Smad3 siRNA (Thermo Fisher Scientific, San Diego, CA, USA). The following siRNAs were used: Smad2, ON-TARGETplus SMARTpool human Smad2 (4087); and Smad3 siRNA, ON-TARGETplus SMARTpool human Smad3 (4088). The scrambled siRNA from a non-targeting siRNA pool from Thermo Fisher Scientific was used as a control. Lipofectamine 2000 (Invitrogen) was used for the siRNA transfection.
Flow Cytometric Analysis for Annexin V-FITC Binding
After exposure of HPMCs to TM or TG for 12 and 48 h, cell suspensions were prepared by treating the cells with a trypsin/EDTA mixture in DMEM. The cells were resuspended in 1 × Annexin V binding buffer at a concentration of 1 × 106 cells/ml. After incubation of 100 μl of cell suspension with 5 μl of FITC-Annexin V at room temperature in the dark for 15 minutes, 400 μl of 1 × binding buffer was added to each tube. The samples were then analyzed on a FACS Calibur flow cytometer (Beckton Dickinson, San Jose, CA, USA) and CellQuest software (Beckton Dickinson). The 10 000 events per sample were collected with an exclusion of cell debris by scatter gating (forward vs side). The data were displayed as two-color dot plot with FITC-Annexin V (green fluorescence, x-axis) vs PI (red fluorescence, y-axis). Apoptosis was assessed by measuring the fraction of Annexin V-positive cells.
TdT-Mediated dUTP Nick-End Labeling (TUNEL) Staining
HPMCs were washed and fixed in 4% phosphate-buffered paraformaldehyde for 25 minutes at 20 °C. After washing three times with PBS, HPMCs were stained using the In Situ Cell Death Detection Kit (Roche Diagnostics, Laval, Quebec, Canada) according to the manufacturer’s protocol. The nucleus was counterstained with DAPI, and the cells were visualized under the Axiovert 200 fluorescence microscope with 10 × 10 and 20 × 10 NA objectives equipped with AxioCam HRC digital camera.
Effect of ER Stress Modulation on TGF-β1-Induced EMT in HPMCs
The effects of the ER stress blocker, taurine-conjugated ursodeoxycholic acid (TUDCA, 300 μM, Tokyo Kasei, Tokyo, Japan), on TGF-β1-induced changes in HPMCs were investigated. After repeated experiments to determine the condition of ER stress preconditioning in HPMCs, the cells were pre-incubated with TM at 0.01 ng/ml or TG at 0.01 nM for 4 h before treatment with TGF-β1 (1 ng/ml).
Isolation of Mesothelial Cells from Peritoneal Effluent in Patients on PD: Ex Vivo Analysis of ER Stress
Peritoneal mesothelial cells were obtained from nine clinically stable PD patients using a previously described method.34 After centrifugation of the whole-dialysate effluent collected after a standard peritoneal equilibration test (PET), the cell pellets were suspended in medium 199 containing 10% FBS, 100 U/ml penicillin, 100 μg/ml streptomycin, and 26 mmol/l NaHCO3. Half of the medium was exchanged at 48 h after seeding, and the entire medium was replaced once every 4 days. After reaching confluence, the cells were detached by trypsinization and seeded into culture plates. Western blotting for GRP78/94, E-cadherin, α-SMA and cleaved Caspase-3 was performed by the methods described in in vitro experiments.
PET and Urea Kinetic Modeling
Standardized PET was performed by using a 2.27% glucose concentration 2- L dialysate.35 The dialysate-to-instilled ratio of glucose (D/D0Glucose) and the dialysate-to-plasma ratio of creatinine (D/PCr) were calculated from the data of PET. The total daily exposure to glucose in each patient was calculated by the product of volume and the glucose concentration for each exchange. The dialysis dose was assessed by calculating the weekly Kt/Vurea from the 24-h urinary and dialysate clearance of urea. The nPNA was calculated by the formula of Bergström et al.36 and normalized to standard body weight.
Statistical Analysis
All of the data are presented as the mean±SD. Differences in the various parameters between the groups were evaluated by Student’s t-test or one-way analysis of variance followed by correction for multiple comparisons. Pearson’s correlation was applied for correlation analyses. The results were considered significant if the P-value was ≤0.05.
RESULTS
ER Stress Induces EMT of HPMCs
Tunicamycin (TM) and thapsigargin (TG) elicited ER stress as indicated by an induction of ER chaperone GRP78/94 at concentrations of 0.01 ng/ml and 0.01 nM, respectively, from 4 h (Supplementary Figure S1). TM and TG increased the phosphorylation of PERK and eIF2α from 4 and 6 h, followed by an upregulation of ATF4 after 12 h. An increase in ATF6 after 6 h and XBP-1 mRNA splicing after 12 or 24 h were also noted in HPMCs exposed to TM or TG (Supplementary Figure S2).
TM (0.01 ng/ml) and TG (0.01 nM) induced the morphological changes of HPMCs from 12 h from a cuboidal, cobble-stone appearance to an elongated, fibroblastoid morphology (Figure 1a). Expression of the markers for epithelial and mesenchymal cells was also altered by treatment with TM or TG, including a decreased expression of ZO-1 and E-cadherin with an acquisition of α-SMA expression in HPMCs (Figure 1b). Interestingly, EMT induced by a 12-h exposure to TM or TG was reversible upon the removal of TM or TG (Figure 1c); however, EMT induced by a prolonged stimulation of cells with TM or TG for 48 h was not reversed upon the removal of the ER stress inducer (Figure 2), suggesting that ER stress-induced EMT is reversible in a time-dependent manner.
ER stress-induced EMT and its reversibility. TM (0.01 ng/ml) or TG (0.01 nM) induces the morphologic changes of HPMCs from a cuboidal, cobble-stone appearance to elongated, fibroblastoid morphology (a) with decreased expression of ZO-1 and E-cadherin and the acquisition of α-SMA expression in HPMCs (a and b). Removal of TM or TG after 12 h of stimulation results in a reversal of TM- or TG-induced EMT (a and c). Representative cell morphology and fluorescein immunocytochemistry for ZO-1 (green) and α-SMA (green) with nuclear DAPI staining (blue) at 12 h and 48 h after a 12-h treatment with TM (0.01 ng/ml) or TG (0.01 nM) are shown (a). Quantitation bars for real-time PCR (n=5) and representative western blots with quantitation bars (n=6) are shown (b and c). M denotes control media without TM or TG. *P<0.05 vs control, #P<0.05 vs others.
Time-dependent reversal of ER stress-induced EMT. EMT induced by a prolonged stimulation of cells with TM (0.01 ng/ml) or TG (0.01 nM) for 48 h is not reversed by the removal of TM or TG. Representative phase-contrast microscopy and fluorescein immunocytochemistry for ZO-1 (green) and α-SMA (green) with nuclear DAPI staining (blue) at 48 h, and 48 h after a 48-h treatment with TM or TG are shown (a). Representative real-time PCR (b) and western blotting with quantitation bars (c) are shown (n=5). M denotes control media without TM or TG. *P<0.05 vs control.
ER Stress Induces Snail Expression and Nuclear Translocation of β-Catenin via Smad2/3 Activation
To understand the mechanism of ER stress-induced EMT in HPMCs, we examined the activation of the Smad2/3 pathway and the expression of β-catenin and snail. TM or TG enhanced the phosphorylation of Smad2/3 and increased the nuclear translocation of β-catenin and Snail expression (Figure 3). Blocking the activation of Smad2/3 by siRNA alleviated the ER stress-induced alterations in E-cadherin and α-SMA levels in HPMCs. Smad2 and Smad3 gene silencing also reduced the nuclear translocation of β-catenin and Snail expression (Figure 4).
Activation of Smad2/3, nuclear translocation of β-catenin and expression of Snail in TM or TG-treated HPMCs. TM (0.01 ng/ml) or TG (0.01 nM) enhances the phosphorylation of Smad2/3 (a), the nuclear translocation of β-catenin (b and c) and Snail expression (b). Representative western blots with quantitative analyses are shown (a and b). Fluorescein immunocytochemistry reveals the translocation of β-catenin (green) from the cytoplasmic membrane into the nucleus (cyan) upon TM or TG stimulation at 12 h (c); n=6. *P<0.05 vs others.
Effect of Smad2/3 siRNA transfection on ER stress-induced EMT. Blocking the activation of Smad2/3 by siRNA alleviates TM (0.01 ng/ml) or TG (0.01 nM)-induced alterations in E-cadherin and α-SMA in HPMCs after 12 h (a). siRNA of Smad2 and Smad3 also reduces the expression of β-catenin in the nuclear extracts and snail after 12 h (b). Representative western blots with quantitative analyses are shown; n=6. *P<0.05 vs 0.
ER Stress Induces Apoptosis in a Dose- and Time-Dependent Manner
TM and TG at the concentration that induced EMT of HPMCs (0.01 ng/ml and 0.01 nM, respectively) did not lead to apoptosis in HPMCs within 48 h assessed by FACScan analysis (Figure 5a) or TUNEL staining (Figure 5b); however, higher concentrations of TM (1 and 5 ng/ml) and TG (1 and 5 nM) increased the number of apoptotic cells within 12 h (Figures 5c and d), suggesting a dose-dependency of ER stress-induced apoptosis of HPMCs.
A dose-dependency of ER stress-induced apoptosis in HPMCs. TM (0.01 ng/ml) or TG (0.01 nM) does not induce apoptosis in HPMCs within 48 h (a and b). At higher concentrations of TM (≥1 ng/ml) or TG (≥1 nM) induce apoptosis of HPMCs within 12 h (c and d). Representative histogram and dot blots depict shifts in the fluorescence intensity of annexin V binding (numbers in parenthesis) at 12 and 48 h; n=5. Representative TUNEL staining with quantitation of TUNEL (+) cell (cyan) is shown (n=3). *P<0.05 vs 0.
Apoptosis of HPMCs using a higher concentration of ER stress inducers was associated with a persistent increase in the expression of C/EBP homologous protein (CHOP; Figure 6a), a UPR marker has been implicated in apoptosis.19,37, 38 A mild and transient upregulation of CHOP was observed with a lower concentration of TM or TG (Figure 6b).
Effect of ER stress-induced CHOP expression. A higher concentration of ER stress inducers (TM 5 ng/ml, TG 5 nM) induces a persistent increase in the expression of CHOP within 30 min (a). A mild and transient upregulation of CHOP is observed using a lower concentration of TM (0.01 ng/ml) or TG (0.01 nM); n=5 (b). Representative western blotting with quantitative analyses is shown. *P<0.05 vs others.
On the basis of this observation, we investigated the effect of using an intermediate dose of ER stress inducers on EMT and apoptosis of HPMCs. Interestingly, an exposure of HPMCs to 0.1 ng/ml of TM or 0.1 nM of TG resulted in EMT at earlier time points (3–4 h; Supplementary Figure S3a) but induced apoptosis with CHOP expression by prolonged ER stress (48 h; Supplementary Figure S3b and c).
ER Stress-Induced Apoptosis Is Not Mediated by Smad2/3 Activation
siRNA of Smad2/3 did not ameliorate TM- or TG-induced apoptosis. CHOP expression in TM- or TG-treated cells was not altered by Smad2/3 gene silencing (Supplementary Figure S4).
TGF-β1 Induces Persistent ER Stress That Results in EMT and Apoptosis of HPMCs
TGF-β1, a representative pro-fibrotic cytokine, induced ER stress in HPMCs, as indicated by an increase in the expression of GRP78/94 and ATF6 with XBP-1 splicing (Figure 7a). TUDCA, an endogenous bile acid known to attenuate ER stress,39, 40 blocked the TGF-β1-induced expression of GRP78/94 and ATF6 (Figure 7b). TUDCA also inhibited XBP-1 splicing induced by TM or TG. Interestingly, TGF-β1 did not induce the phosphorylation of PERK, eIF2α, or ATF4.
Effect of TGF-β1 on ER stress in HPMCs. TGF-β1 (1 ng/ml) induces an increase in the expression of GRP78/94 and ATF6 with XBP-1 splicing in HPMCs, but does not induce the phosphorylation of PERK, eIF2α, or ATF4 (a). TUDCA (300 μM) blocks the ER stress-induced increase in GRP78/94 and ATF6 with XBP-1 splicing at 12 h; n=5 (b). Representative western blots and RT-PCR bands with quantitative analyses are shown. *P<0.05 vs others.
TGF-β1 induced EMT of HPMCs within 24 and 48 h, as confirmed by a transition of the cell morphology and altered expression of epithelial and mesenchymal cell markers (Figure 8). TGF-β1 also induced apoptosis of HPMCs (Figures 8b and c). TUDCA blocked TGF-β1-induced EMT and apoptosis in HPMCs (Figure 8).
Effect of TUDCA on TGF-β1-induced EMT and apoptosis. TGF-β1 (1 ng/ml) induces EMT of HPMCs assessed by cell morphology (48 h) and altered expression of E-cadherin and α-SMA at 24 and 48 h (a). TGF-β1 also induces apoptosis of HPMCs assessed by FACScan analysis (b) and TUNEL staining (c) at 48h. TUDCA (300 μM) blocks TGF-β1-induced EMT and apoptosis in HPMCs at 48 h (n=6). Representative cell morphology, western blotting, histogram, and TUNEL staining are shown. The numbers in parentheses in the histogram denote the shifts in fluorescence intensity of annexin V binding. *P<0.05 vs others.
ER Stress Preconditioning Protects HPMCs from TGF-β1-Induced EMT and Apoptosis with an Amelioration of Smad2/3 Activation and Snail Expression
Pre-treatment with TM (0.01 ng/ml) or TG (0.01 nM) for 4 h protected the cells from TGF-β1-induced EMT in HPMCs. Figure 9a shows the effect of ER stress preconditioning on the alteration in cell morphology and the expression of E-cadherin and α-SMA. ER stress preconditioning blocked the phosphorylation of Smad2/3, the translocation of β-catenin, and the increase in Snail expression in HPMCs exposed to TGF-β1 (Supplementary Figure S5). ER stress preconditioning also protected the cells from TGF-β1-induced apoptosis as assessed by Annexin V (+) cells upon FACScan analysis (Figure 9b) and TUNEL positivity (Figure 9c).
Effect of ER stress preconditioning on TGF-β1-induced EMT and apoptosis. Pre-treatment with TM (0.01 ng/ml) or TG (0.01 nM) for 4 h protects the cells from TGF-β1-induced EMT in HPMCs at 48 h (a), as well as TGF-β1-induced apoptosis n=5 (b, c). The representative histogram depicts shifts in the fluorescence intensity of annexin V binding at 48 h (b). Representative TUNEL staining with quantitation of TUNEL (+) cell (cyan) is shown (c) (n=3). pTM or pTG denotes preconditioning with TM or TG. *P<0.05 vs others.
Increased GRP Expression in Mesothelial Cells Isolated from Peritoneal Effluent Is Correlated with EMT in PD Patients
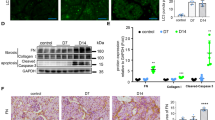
GRP94/78 expression was increased in mesothelial cells from 14 peritoneal effluents of 9 PD patients (Table 1) compared with mesothelial cells isolated from the omentum in subjects with normal renal function who had never been exposed to PD (Figure 10). E-cadherin expression was decreased with an increase in α-SMA in mesothelial cells from PD effluent (Figure 10b). There was a tendency of an enhanced expression of cleaved Caspase-3 in cells from PD patients, however it was not statistically significant. There was no significant correlation of GRP94/78 expression in mesothelial cells from PD patients with age, duration of dialysis, the incidence of peritonitis, and parameters of peritoneal function such as D/PCr or D/D0glucose. The expression of GRP94/78 in mesothelial cells from PD patients was correlated with the expression of E-cadherin (r=−0.35, P<0.05) or α-SMA (r=0.47, P<0.05; Figure 10c).
ER stress and EMT of HPMCs from peritoneal effluent in PD patients. Expression of GRP78/94 is increased in HPMCs isolated from nine clinically stable PD patients compared with HPMCs from the omentum of nine subjects never exposed to the peritoneal dialysate (a). E-cadherin expression was decreased in HPMCs from PD patients with increased α-SMA (b). Cleaved Caspase-3 expression is comparable. The quantitation bar shows the mean expression of each protein in mesothelial cells from the PD effluent and omentum. GRP expression in HPMCs from 14 peritoneal effluents was correlated with the expression of E-cadherin and α-SMA (c). *P<0.05 vs HPMCs isolated from the omentum.
DISCUSSION
In this study, we demonstrate that a chemical induction of ER stress by TM or TG leads to EMT and apoptosis of HPMCs in a dose- and time-dependent manner. ER stress-induced apoptosis was associated with a persistent upregulation of CHOP, whereas mild ER stress induced transient CHOP expression with the development of reversible EMT of HPMCs. Intermediate doses of ER stress inducers promote EMT at early time points but result in cell apoptosis upon prolonged exposure to ER stress (Figure 11). Despite the causative role of ER stress in EMT and apoptosis, ER stress preconditioning by a transient exposure to low concentrations of TM or TG protects HPMCs from TGF-β1-induced EMT and apoptosis (Figure 12). Our data provide evidence for the role of ER stress as a modifiable target to protect the peritoneal membrane via ER stress preconditioning or blocking of excessive ER stress.
One of the most interesting findings of this study is that ER stress per se induces EMT in HPMCs. The phenotypic transition of a peritoneal mesothelial cell to mesenchymal cell, the so-called EMT, has been recognized as an important mechanism of peritoneal fibrosis.8, 9 EMT in PD patients was associated with ultrafiltration failure, which highlighted the clinical significance of peritoneal EMT as a cause of peritoneal dysfunction.5, 6, 41 ER stress has been implicated in EMT and fibroblast accumulation in organ fibrosis.42 One of the chemical inducers of ER stress, TM, was reported to induce EMT of renal proximal tubular cells via the release of calcium from the ER and the activation of Wnt signaling.18 ER stress also induced EMT in cultured alveolar epithelial cells by activating MAPKinase, Smad and Src.20 The role of the UPR and ER stress has been demonstrated in idiopathic pulmonary fibrosis, as well as glomerulonephritis, diabetic nephropathy and drug-induced renal damage.17, 19,43,44 Despite ample evidence regarding the role of ER stress in organ fibrosis, the about ER stress and peritoneal fibrosis remain very limited. Previous studies revealed ultrastructural alterations of rough ER in the parietal peritoneum of patients on PD.45 An expansion of ER in mesothelial cells in an animal model of PD and an induction of ER stress by acidic dialysate in cultured mesothelial cells suggested the potential role of ER stress in peritoneal damage;32 however, there have been no studies investigating whether ER stress induces EMT in peritoneal mesothelial cells. We used two chemical inducers of ER stress, TM and TG, and assessed the expression of ER stress markers. Low concentrations of TM or TG induced an approximately twofold increase in GRP78/94 expression in HMPCs, followed by the activation of downstream markers of ER activation. Our data clearly demonstrated that both TM and TG induced EMT of peritoneal mesothelial cells. Importantly, ER stress-induced EMT was reversible at early time points; however, prolonged ER stress resulted in irreversible EMT. We have already demonstrated a reversal of high-glucose-induced EMT upon the removal of high-glucose stimuli in HPMCs with an improvement of peritoneal thickening and fibrosis in an animal model of PD by peritoneal rest.8
ER stress was not only a direct inducer of EMT of HPMCs but was also a mediator of TGF-β1-induced EMT in HPMCs. TGF-β1 is a representative pro-fibrotic cytokine that is known to induce peritoneal fibrosis through a phenotypic transition of peritoneal mesothelial cells.9 TGF-β1 increased the expression of GRP78/94 and ATF6 with XBP-1 splicing in HPMCs. We also demonstrated that a known inhibitor of ER stress, TUDCA, ameliorated TGF-β1-induced EMT, suggesting the role of ER stress as a mediator of EMT of HPMCs. TUDCA is an endogenous bile acid derivative that is likely to increase the stability of unfolded proteins upon the activation of the adaptive UPR.46
ER stress is reported to be associated with the upregulation of multiple signaling pathways. In this study, ER stress induced the activation of Smad2/3 in HPMCs, and siRNA transfection for silencing Smad2 or Smad3 resulted in a partial inhibition of ER stress-induced EMT. This finding suggests that the Smad2/3 pathway activated by ER stress has a role in the development of EMT of mesothelial cells. The nuclear localization of β-catenin was also noted in TM- or TG-treated cells, whereas cell membrane staining was observed in control cells. The nuclear translocation of β-catenin is accompanied by an increase in snail, a key transcription factor that suppresses E-cadherin expression, as was also observed in TM- or TG-treated cells. There has been limited data regarding the association of ER stress and β-catenin mobilization. Raab et al.47 showed that a rapid accumulation of β-catenin in nucleus by an inhibition of proteasomal degradation of β-catenin resulted in ER stress in multiple myeloma cells whereas TG induced nuclear translocation of β-catenin in renal tubular cells.18 Snail is known as a transcriptional repressor of E-cadherin which stimulates EMT. Although cross-talk between β-catenin and snail has been speculated, there is no consensus on the interaction of these two molecules. Previous studies failed to prove β-catenin-induced upregulation of Snail, rather snail may upregulate β-catenin degradation and nuclear translocation. In this study, we have not addressed the mechanism for interaction of β-catenin and Snail in peritoneal mesothelial cells, which needs to be further investigated. Importantly, siRNA for Smad2/3 reduced both the nuclear localization of β-catenin and Snail expression. Considering the serial activation of Smad2/3, β-catenin and snail with the effect of Smad2/3 silencing on the expression of β-catenin and Snail, the Smad2/3 pathway appears to be an upstream signal to activate β-catenin and Snail expression in HPMCs exposed to ER stress. The Smad2/3 pathway is known to be an important mediator of EMT induced by TGF-β1.48, 49 In our study, a protective effect of TUDCA on TGF-β1-induced EMT was associated with an amelioration of Smad2/3 activation, suggesting that the Smad2/3 pathway is a key mediator of EMT. Tanjore et al.20 also demonstrated an activation of Smad2/3 in TM-treated alveolar epithelial cells and reported that either a Smad2/3 inhibitor or siRNA targeting Smad2/3 attenuated EMT of pulmonary alveolar cells.
Another important finding of this study was the enhanced apoptosis of HPMCs upon ER stress induction. ER stress is known to trigger cell apoptosis when cells fail to resolve homeostasis in the ER upon excessive or prolonged ER stress.50, 51 In this study, mild ER stress induced by a low concentration of TM or TG did not induce apoptosis within 48 h; however, intermediate and high concentrations of TM or TG increased apoptosis of HPMCs within 12 h. Importantly, TM- or TG-induced apoptosis was associated with a persistent activation of CHOP, whereas a low concentration of TM or TG induced a transient upregulation of CHOP. As noted, a transient increase in CHOP is not sufficient to induce significant apoptosis, despite the sustained activation of UPR under conditions of mild ER stress.19 Apoptosis of HPMCs may also be induced by a CHOP-independent pathway via the activation of JNK, caspase, or mitochondrial cytochrome C. Interestingly, in contrast to the role of smad2/3 in EMT, smad2/3 activation was mediated by neither ER stress- nor TGF-β1-induced apoptosis in HPMCs in our study (Supplementary Figures S4 and S6).
Beneficial effect of preconditioning with ER stress was demonstrated in an animal model of mesangioproliferative glomerulonephritis.52 ER stress resulting from the application of a subnephritogenic dose of an ER stress inducer (TM or TG) induced the adaptive UPR.26, 52 Cytoprotection by ER stress preconditioning was also confirmed in cultured renal tubular cells exposed to nephrotoxic drugs via the induction of GRP78 and an enhancement of ER folding capacity.53, 54, 55 In this study, preconditioning targeting ER stress ameliorated TGF-β1-induced EMT and apoptosis in HPMCs, suggesting the role of ER as a potential target for protecting the peritoneal membrane. ER stress preconditioning in HPMCs may enhance the maturation of protein by enhancing GRP expression, which resulted in the preservation of peritoneal membrane integrity. Interestingly, ER stress preconditioning ameliorated Smad2/3 activation, nuclear translocation of β-catenin and Snail expression in TGF-β1-treated HPMCs.
We also measured GRP78/94 expression in mesothelial cells isolated from peritoneal effluents of PD patients. GRP78/94 expression was significantly increased in the mesothelial cells of PD patients, suggesting the presence of ER stress in these patients. Expression of proapoptic cleaved Caspase-3 was comparable in mesothelial cells isolated from PD patients and healthy controls. A degree of ER stress was significantly correlated with EMT (Figure 10), but EMT was not linked to parameters of peritoneal membrane transport. Considering the small number of subjects in our study and the fact that many other clinical parameters, including peritoneal blood flow, determine the membrane transport rate, drawing a conclusion about the role of ER stress as one of the determinants of peritoneal characteristics is difficult. Nonetheless, the clinical implications of ER stress modulation, including the effect of ER stress blockers on peritoneal function, need to be determined in PD patients and animal models of PD. Because our data clearly demonstrated enhanced ER stress in peritoneum exposed to peritoneal dialysate, we may speculate on the benefit of ER stress preconditioning in peritoneal preservation. A temporary transfer to daytime ambulatory PD with a nocturnal ‘empty belly’ resulted in an improved peritoneal function, which was observed as a decrease in D/PCr and the peritoneal fluid absorption rate.56 The beneficial effect of peritoneal rest on ultrafiltration capacity in PD patients, as well as an animal model of PD can be explained by the effect of ER stress preconditioning.57, 58
In conclusion, this study provides the first evidence of ER stress-induced EMT and apoptosis in HPMCs in a time- and dose-dependent manner. Both the blocking and preconditioning of ER stress ameliorated TGF-β1-induced EMT and apoptosis, demonstrating the role of ER stress as an adaptive response that serves to protect HPMCs against ER stress-induced apoptosis. Therefore, the modulation of ER stress in peritoneal mesothelial cells could represent a novel approach to ameliorate EMT and apoptosis in the pathogenesis of peritoneal fibrosis.
References
Blake PG . Integrated end-stage renal disease care: the role of peritoneal dialysis. Nephrol Dial Transplant 2001;16:61–66.
Krediet RT . The peritoneal membrane in chronic peritoneal dialysis. Kidney Int 1999;55:341–356.
Krediet RT, Lindholm B, Rippe B . Pathophysiology of peritoneal membrane failure. Perit Dial Int 2000;20:S22–S42.
Davies SJ, Phillips L, Griffiths AM et al. What really happens to people on long-term peritoneal dialysis? Kidney Int 1998;54:2207–2217.
Selgas R, Fernandez-Reyes MJ, Bosque E et al. Functional longevity of the human peritoneum: how long is continuous peritoneal dialysis possible? Results of a prospective medium long-term study. Am J Kidney Dis 1994;23:64–73.
Williams JD, Craig KJ, Topley N et al. Morphologic changes in the peritoneal membrane of patients with renal disease. J Am Soc Nephrol 2002;13:470–479.
Yang AH, Chen JY, Lin YP et al. Peritoneal dialysis solution induces apoptosis of mesothelial cells. Kidney Int 1997;51:1280–1288.
Yu MA, Shin KS, Kim JH et al. HGF and BMP-7 ameliorate high glucose-induced epithelial-to-mesenchymal transition of peritoneal mesothelium. J Am Soc Nephrol 2009;20:567–581.
Jang YH, Shin HS, Sun Choi H et al. Effects of dexamethasone on the TGF-beta1-induced epithelial-to-mesenchymal transition in human peritoneal mesothelial cells. Lab Invest 2013;93:194–206.
Yanez-Mo M, Lara-Pezzi E, Selgas R et al. Peritoneal dialysis and epithelial-to-mesenchymal transition of mesothelial cells. N Engl J Med 2003;348:403–413.
Loureiro J, Aguilera A, Selgas R et al. Blocking TGF-beta1 protects the peritoneal membrane from dialysate-induced damage. J Am Soc Nephrol 2011;22:1682–1695.
Guo H, Leung JC, Lam MF et al. Smad7 transgene attenuates peritoneal fibrosis in uremic rats treated with peritoneal dialysis. J Am Soc Nephrol 2007;18:2689–2703.
Loureiro J, Schilte M, Aguilera A et al. BMP-7 blocks mesenchymal conversion of mesothelial cells and prevents peritoneal damage induced by dialysis fluid exposure. Nephrol Dial Transplant 2010;25:1098–1108.
Ulianich L, Garbi C, Treglia AS et al. ER stress is associated with dedifferentiation and an epithelial-to-mesenchymal transition-like phenotype in PC Cl3 thyroid cells. J Cell Sci 2008;121:477–486.
Pallet N, Bouvier N, Bendjallabah A et al. Cyclosporine-induced endoplasmic reticulum stress triggers tubular phenotypic changes and death. Am J Transplant 2008;8:2283–2296.
Szegezdi E, Logue SE, Gorman AM et al. Mediators of endoplasmic reticulum stress-induced apoptosis. EMBO Rep 2006;7:880–885.
Liu G, Sun Y, Li Z et al. Apoptosis induced by endoplasmic reticulum stress involved in diabetic kidney disease. Biochem Biophys Res Commun 2008;370:651–656.
Carlisle RE, Heffernan A, Brimble E et al. TDAG51 mediates epithelial-to-mesenchymal transition in human proximal tubular epithelium. Am J Physiol Renal Physiol 2012;303:F467–F481.
Zhong Q, Zhou B, Ann DK et al. Role of endoplasmic reticulum stress in epithelial-mesenchymal transition of alveolar epithelial cells: effects of misfolded surfactant protein. Am J Respir Cell Mol Biol 2011;45:498–509.
Tanjore H, Cheng DS, Degryse AL et al. Alveolar epithelial cells undergo epithelial-to-mesenchymal transition in response to endoplasmic reticulum stress. J Biol Chem 2011;286:30972–30980.
Malhi H, Kaufman RJ . Endoplasmic reticulum stress in liver disease. J Hepatol 2011;54:795–809.
Ayala P, Montenegro J, Vivar R et al. Attenuation of endoplasmic reticulum stress using the chemical chaperone 4-phenylbutyric acid prevents cardiac fibrosis induced by isoproterenol. Exp Mol Pathol 2012;92:97–104.
Kaufman RJ . Stress signaling from the lumen of the endoplasmic reticulum: coordination of gene transcriptional and translational controls. Genes Dev 1999;13:1211–1233.
Yoshida H . ER stress and diseases. FEBS J 2007;274:630–658.
Inagi R . Endoplasmic reticulum stress as a progression factor for kidney injury. Curr Opin Pharmacol 2010;10:156–165.
Ni M, Lee AS . ER chaperones in mammalian development and human diseases. FEBS Lett 2007;581:3641–3651.
Inagi R . Endoplasmic reticulum stress in the kidney as a novel mediator of kidney injury. Nephron Exp Nephrol 2009;112:e1–e9.
Chen Y, Brandizzi F . IRE1: ER stress sensor and cell fate executor. Trends Cell Biol 2013;23:547–555.
Malhotra JD, Kaufman RJ . Endoplasmic reticulum stress and oxidative stress: a vicious cycle or a double-edged sword? Antioxid Redox Signal 2007;9:2277–2293.
Adachi Y, Yamamoto K, Okada T et al. ATF6 is a transcription factor specializing in the regulation of quality control proteins in the endoplasmic reticulum. Cell Struct Funct 2008;33:75–89.
Yamamoto K, Sato T, Matsui T et al. Transcriptional induction of mammalian ER quality control proteins is mediated by single or combined action of ATF6alpha and XBP1. Dev Cell 2007;13:365–376.
Johno H, Ogata R, Nakajima S et al. Acidic stress-ER stress axis for blunted activation of NF-kappaB in mesothelial cells exposed to peritoneal dialysis fluid. Nephrol Dial Transplant 2012;27:4053–4060.
Kang DH, Hong YS, Lim HJ et al. High glucose solution and spent dialysate stimulate the synthesis of transforming growth factor-beta1 of human peritoneal mesothelial cells: effect of cytokine costimulation. Perit Dial Int 1999;19:221–230.
Diaz C, Selgas R, Castro MA et al. Ex vivo proliferation of mesothelial cells directly obtained from peritoneal effluent: its relationship with peritoneal antecedents and functional parameters. Adv Perit Dial 1998;14:19–24.
Twardowski ZJ . PET–a simpler approach for determining prescriptions for adequate dialysis therapy. Adv Perit Dial 1990;6:186–191.
Bergstrom J, Heimburger O, Lindholm B . Calculation of the protein equivalent of total nitrogen appearance from urea appearance. Which formulas should be used? Perit Dial Int 1998;18:467–473.
Park SH, Choi HJ, Yang H et al. Endoplasmic reticulum stress-activated C/EBP homologous protein enhances nuclear factor-kappaB signals via repression of peroxisome proliferator-activated receptor gamma. J Biol Chem 2010;285:35330–35339.
Hayakawa K, Nakajima S, Hiramatsu N et al. ER stress depresses NF-kappaB activation in mesangial cells through preferential induction of C/EBP beta. J Am Soc Nephrol 2010;21:73–81.
Malo A, Kruger B, Seyhun E et al. Tauroursodeoxycholic acid reduces endoplasmic reticulum stress, trypsin activation, and acinar cell apoptosis while increasing secretion in rat pancreatic acini. Am J Physiol Gastrointest Liver Physiol 2010;299:G877–G886.
Ozcan U, Yilmaz E, Ozcan L et al. Chemical chaperones reduce ER stress and restore glucose homeostasis in a mouse model of type 2 diabetes. Science 2006;313:1137–1140.
Aroeira LS, Aguilera A, Sanchez-Tomero JA et al. Epithelial to mesenchymal transition and peritoneal membrane failure in peritoneal dialysis patients: pathologic significance and potential therapeutic interventions. J Am Soc Nephrol 2007;18:2004–2013.
Tanjore H, Lawson WE, Blackwell TS . Endoplasmic reticulum stress as a pro-fibrotic stimulus. Biochim Biophys Acta 2013;1832:940–947.
Tanjore H, Blackwell TS, Lawson WE . Emerging evidence for endoplasmic reticulum stress in the pathogenesis of idiopathic pulmonary fibrosis. Am J Physiol Lung Cell Mol Physiol 2012;302:L721–L729.
Kitamura M . Endoplasmic reticulum stress and unfolded protein response in renal pathophysiology: Janus faces. Am J Physiol Renal Physiol 2008;295:F323–F334.
Dobbie JW . Morphology of the peritoneum in CAPD. Blood Purif 1989;7:74–85.
Lee YY, Hong SH, Lee YJ et al. Tauroursodeoxycholate (TUDCA), chemical chaperone, enhances function of islets by reducing ER stress. Biochem Biophys Res Commun 2010;397:735–739.
Raab MS, Breitkreutz I, Tonon G et al. Targeting PKC: a novel role for beta-catenin in ER stress and apoptotic signaling. Blood 2009;113:1513–1521.
Bottinger EP . Bitzer M. TGF-beta signaling in renal disease. J Am Soc Nephrol 2002;13:2600–2610.
Willis BC, Borok Z . TGF-beta-induced EMT: mechanisms and implications for fibrotic lung disease. Am J Physiol Lung Cell Mol Physiol 2007;293:L525–L534.
Tabas I, Ron D . Integrating the mechanisms of apoptosis induced by endoplasmic reticulum stress. Nat Cell Biol 2011;13:184–190.
Xu C, Bailly-Maitre B, Reed JC . Endoplasmic reticulum stress: cell life and death decisions. J Clin Invest 2005;115:2656–2664.
Inagi R, Kumagai T, Nishi H et al. Preconditioning with endoplasmic reticulum stress ameliorates mesangioproliferative glomerulonephritis. J Am Soc Nephrol 2008;19:915–922.
Lorz C, Justo P, Sanz A et al. Paracetamol-induced renal tubular injury: a role for ER stress. J Am Soc Nephrol 2004;15:380–389.
Liu H, Baliga R . Endoplasmic reticulum stress-associated caspase 12 mediates cisplatin-induced LLC-PK1 cell apoptosis. J Am Soc Nephrol 2005;16:1985–1992.
Peyrou M, Hanna PE, Cribb AE . Cisplatin, gentamicin, and p-aminophenol induce markers of endoplasmic reticulum stress in the rat kidneys. Toxicol Sci 2007;99:346–353.
Zhe XW, Tian XK, Cheng L et al. Effects of peritoneal resting on peritoneal fluid transport kinetics. Perit Dial Int 2007;27:575–579.
de Alvaro F, Castro MJ, Dapena F et al. Peritoneal resting is beneficial in peritoneal hyperpermeability and ultrafiltration failure. Adv Perit Dial 1993;9:56–61.
Kim YL, Kim SH, Kim JH et al. Effects of peritoneal rest on peritoneal transport and peritoneal membrane thickening in continuous ambulatory peritoneal dialysis rats. Perit Dial Int 1999;19:S384–S387.
Acknowledgements
This work was supported by the Bio and Medical Technology Development Program of the National Research Foundation (NRF) funded by the Ministry of Science, ICT and Future Planning (2010-0019866), and a National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIP; 2012R1A2A2A01013541) and Hi Seoul Science (Humanities) Fellowship funded by Seoul Scholarship Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
Endoplasmic reticulum (ER) stress induces epithelial-to-mesenchymal transition (EMT) and apoptosis in peritoneal mesothelial cells in a time- and dose-dependent manner. Blocking ER stress ameliorates transforming growth factor-β1-induced EMT and apoptosis, demonstrating the role of ER stress as an adaptive response to peritoneal damage. Therefore, the modulation of ER stress is a novel approach to ameliorate peritoneal fibrosis.
Supplementary information
Rights and permissions
About this article
Cite this article
Shin, HS., Ryu, ES., Oh, ES. et al. Endoplasmic reticulum stress as a novel target to ameliorate epithelial-to-mesenchymal transition and apoptosis of human peritoneal mesothelial cells. Lab Invest 95, 1157–1173 (2015). https://doi.org/10.1038/labinvest.2015.91
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2015.91
This article is cited by
-
Role of IGF-1R in epithelial–mesenchymal transdifferentiation of human peritoneal mesothelial cells
Clinical and Experimental Nephrology (2022)
-
Relationship of endoplasmic reticulum stress with the etiopathogenesis of chronic tonsillitis and tonsillar hypertrophy in pediatric patients: a prospective, parallel-group study
Molecular Biology Reports (2021)
-
Ursolic acid alleviates airway-vessel remodeling and muscle consumption in cigarette smoke-induced emphysema rats
BMC Pulmonary Medicine (2019)
-
Metformin ameliorates the Phenotype Transition of Peritoneal Mesothelial Cells and Peritoneal Fibrosis via a modulation of Oxidative Stress
Scientific Reports (2017)
-
Active compounds extracted from extra virgin olive oil counteract mesothelial-to-mesenchymal transition of peritoneal mesothelium cells exposed to conventional peritoneal dialysate: in vitro and in vivo evidences
Journal of Nephrology (2017)