Abstract
Sulfur is able to penetrate the skin, and a sulfur-rich balneotherapy has been suggested to be effective in the treatment of psoriasis. Psoriasis is now considered a genetically programmed, immune-mediated, inflammatory disease, in which intralesional T lymphocytes trigger keratinocytes to proliferate and perpetuate the disease process. Interleukin (IL)-17 and IL-22 produced by Th1/Th17 lymphocytes induce IL-8 secretion by keratinocytes, a key event in the pathogenesis of the disease. It is now clear that mitogen-activated protein kinase (MAPK) (extracellular signal-regulated kinases (ERK) 1 and 2) activity is required for IL-17-induced IL-8 synthesis by keratinocytes, and, in fact, MAPK activity is increased in lesional psoriatic skin. Here, we demonstrate both in vitro and in vivo on primary psoriatic lesions that pharmacological inhibitors of ERKs as well as hydrogen sulfide not only reduce the basal expression and secretion of IL-8, but also interfere with IL-17- and IL-22-induced IL-8 production. These observations, together with the known anti-inflammatory activity of H2S, are relevant to understanding some previously unexplained biological effects exerted by sulfur therapy.
Similar content being viewed by others
Main
Psoriasis is currently thought to be initiated by an epidermal disorder, resulting from aberrant keratinocyte activation that sustains a strong cell proliferation. However, cell- and factor-dependent interactions of keratinocytes with immune cells, rather than alterations limited to keratinocytes alone, cause psoriasis. In fact, signals derived from immune cells are able to stimulate keratinocyte proliferation, while, in turn, keratinocytes themselves may activate immune cells through surface receptors and cytokines.1 Cytokines strongly expressed by keratinocytes of psoriatic skin, like interleukin (IL)-6 and IL-8 have been shown to induce keratinocyte proliferation.2, 3 The more recently described IL-15, IL-17, IL-19, IL-20, IL-22 and IL-23, that are also expressed in psoriatic lesions and that influence keratinocyte proliferation as well, are mainly produced by cells of hematopoietic origin as dendritic (DC), macrophages, lymphocytes and granulocytes.4
Disease initiation is likely to be mediated by DCs presenting foreign antigens or self-antigens to T lymphocytes. Tissue invasion by activated T cells from the periphery seems to be essential for the development and maintenance of psoriatic plaques. Both CD4- and CD8-positive T cells are present in the psoriatic skin: whereas CD4+ T cells mainly infiltrate the dermis, CD8+ T cells preferentially accumulate in the epidermis.5 Recently, the pathophysiology of psoriasis has been revisited as a Th1-/Th17-induced inflammatory autoimmune disease:6, 7, 8 Th17 cells have been reported to produce two cytokines with a clear role in the pathogenesis of this disease, IL-179 and IL-22.10, 11 Increased IL-17 and IL-22 expression levels have been found in psoriatic skin lesions,8, 12, 13 and both IL-17 and IL-22 have been shown to induce keratinocyte gene expression of anti-microbials β-defensins S100A8 and S100A9, all upregulated in psoriatic lesions.10, 14
IL-8 release by keratinocytes has been shown to be induced by IL-17.15, 16 IL-17-mediated induction of IL-8 in keratinocytes implies, at least in part, the activation of mitogen-activated protein kinase (MAPK) pathway,16 even though other signaling axes like PI3-kinase/Akt and NF-κB have been implicated in other cell types.17, 18, 19
Abnormalities in several signaling pathways and in the expression or activation of different transcription factors in psoriatic keratinocytes have been hypothesized to have a role in the molecular pathophysiology of psoriasis.20 It has been reported that the activity of the p38 and extracellular signal-regulated kinase (ERK)1/2 MAPKs is increased in lesional psoriatic skin as compared with non-lesional skin.21, 22 Many studies have been published on the involvement of hydrogen sulfide in inflammation, and evidence has been shown for both pro- or anti-inflammatory roles of H2S.23, 24 Recently, we have demonstrated that hydrogen sulfide can impair human keratinocytes adhesion and proliferation by impairing the activation of Raf-MEK-ERK pathway.22 The specific interest to hydrogen sulfide derives from the potential applications of the results, as sulfur is able to penetrate the skin and a sulfur-rich balneotherapy, known to be effective in the treatment of psoriasis,25 might turn useful in this disease. In this context, we have also demonstrated that H2S can exert a subset-specific toxicity on peripheral blood lymphocytes, which die by a caspase-independent mechanism of necrosis after a rapid loss of mitochondrial membrane potential, and not by apoptosis. Functionally, the surviving lymphocytes show a decreased proliferative capacity and produce less IL-2 during activation.26
Here, we demonstrate both in vitro and in vivo that hydrogen sulfide not only reduces basal expression and secretion of IL-8, but also interferes with IL-17- and IL-22-induced IL-8 production by reducing ERK phosphorylation levels. These observations, together with the known anti-inflammatory activity of H2S, sound relevant to understanding some previously unexplained biological effects exerted by sulfur therapy.
MATERIALS AND METHODS
Cell Cultures
Normal skin-derived immortalized human keratinocytes, clone NCTC 2544, were obtained from the American Tissue Culture Collection and cultured in EMEM medium (Euroclone, West York, UK) containing 10% fetal calf serum, penicillin (100 U/ml), streptomycin (100 μg/ml) and L-glutamine (2 mM). Cells were passaged two or three times weekly at ratios between 1:5 and 1:10. Cell cultures were routinely assayed for mycoplasm contamination by Mycoalert mycoplasm detection kit (Lonza, Rockland, ME, USA).
Cell Treatment
NaHS (Sigma-Aldrich, St Louis, MO, USA) was dissolved in 50 ml of RPMI medium at the concentration of 400 mM. Stock solution was stored for 1 week at 4°C. Immediately before experiments, stock solution was diluted in the cell culture medium at the indicated final concentrations. In some experiments, cells were treated with U0126 (10 μM) (Calbiochem, La Jolla, CA, USA) to induce ERK1/2 irreversible inhibition. Human recombinant IL-22, IL-17A and IL-17F were dissolved as described by the manufacturer and used at 10 ng/ml (Peprotech, D.B.A. s.r.l.; Milano, Italy). IL-17A and IL-17F are reported in the text just as IL-17, since similar results were obtained with both cytokines.
Western Blot
Cells were harvested and washed with ice-cold PBS containing 1 mM sodium orthovanadate, 104 mM 4-(2-aminoethyl)-benzenesulfonyl fluoride, 0.08 mM aprotinin, 2 mM leupeptin, 4 mM bestatin, 1.5 mM pepstatin A, 1.4 mM E-64. Cells were then lysed in Triton lysis buffer. Protein concentration was determined using a BCA protein assay kit (Pierce, Rockford, IL, USA). Aliquots of total protein samples (50 μg) were blotted using antibodies specific for phosphorylated (Thr202/Tyr204) ERK1/2 (1:1000). Incubation times and washing buffers were chosen as indicated by the manufacturers’ protocols (Cell Signaling Technology, Danvers, MA, USA); anti-β-actin (Sigma) mAb was diluted 1:5000. Filters were finally washed and incubated for 1 h at room temperature with anti-rabbit (1:2000) or anti-mouse (1:2000) peroxidase-conjugated secondary antibodies, and revealed by Enhanced Chemiluminescence Western blotting detection reagent (Amersham Biosciences, Buckinghamshire, UK).22, 27, 28 The membranes were then stripped and reprobed with β-actin for protein loading control. Chemiluminescence was quantified by the KODAK Molecular Imaging Software 4.0 using the KODAK Image Station 4000 MM (Carestream Health, Rochester, NY, USA). Values were corrected for β-actin signal intensity.
Patient Treatment and Immunohistochemistry
One voluntary, 70-year-old male patient affected by psoriasis was treated with NaHS (2 mM in sterile 0.9% salt water) or saline alone as negative control. In all, 10 ml of NaHS solution were applied to a psoriatic plaque lesion on the skin of the left gluteus for 15 min/day for 7 days consecutively. As negative control, a similar lesion on the right gluteus was treated with saline solution alone. At the end of the treatment, biopsies from both skin areas were collected. As a further negative control, a biopsy was obtained from a normal skin region of the gluteus. Detailed informed consensus was obtained from the patient before the procedure.
Biopsies were fixed in 10% formalin, and embedded in paraffin.29, 30, 31 Paraffin blocks were serially cut into 5 mm sections and serial sections from each specimen were routinely stained with hematoxylin–eosin for histological examination. Sections were independently stained to detect pERK (Cell Signaling Technology) and IL-8 (BioSource, Camarillo, CA, USA). All sections were dewaxed with xylene and rehydrated by passages through decreasing concentrations of ethanol (from 100 to 80%). Endogenous peroxidase activity was blocked by a 30-min incubation at room temperature with methanol containing 3% H2O2. Sections were then microwaved in a citrate solution (pH 6.0) at 750 W for 10 min. After rinsing in Tris-buffered saline (TBS; pH 7.4), sections were preincubated for 30 min at room temperature with normal rabbit serum or normal goat serum diluted 1:5, before incubation in a humidified chamber for 90 min at room temperature with mAbs. Sections were then washed twice in TBS and incubated for 30 min with diluted biotinylated secondary antibody solution (Vector Laboratories, Burlingame, CA, USA). At the end of incubation, sections were then washed again in TBS and incubated for another 30 min at room temperature with Vectastain Elite® ABC reagent (Vector Laboratories). Peroxidase activity was detected by incubating tissue sections for 10–15 min with a solution of 3-3-diaminobenzidine (DAB) (500 μl DAB (2.5%) in 50 ml TBS; Sigma) in the presence of 50 μl 30% H2O2. Sections were finally counterstained with Mayer's hemalum (Sigma). Negative controls were treated in parallel, using isotype-matched irrelevant antibodies as first step reagents.29, 30, 31
ELISA
IL-8 release in cell culture media was quantified by human IL-8/NAP-1 enzyme-linked immunosorbent assay (Bender Medsystems Vienna, Austria).32, 33, 34 Spent medium from NCTC cell cultures was incubated in 96-well plates coated with anti-human IL-8. After washing of unbound IL-8, wells were incubated with biotin-conjugated anti-IL-8/NAP-1 antibody. Colorimetric reaction was induced by Streptavidin-HRP and tetramethyl-benzidine substrate. Color was measured (absorbance at 450 nm) by Victor3V 1420 multilabel counter (Perkin-Elmer, Waltham, MA, USA) and a set of seven standard dilutions (from 1 g/ml to 15.6 pg/ml) of human recombinant IL-8 was used to convert absorbance values to IL-8 concentrations (g/ml). Each sample was measured in triplicate, the mean of three independent experiments is reported in the text.
RT–PCR
NCTC cell cultures, treated with or without NaHS and ILs, were grown for 48 h, and 1 × 106 trypsinized cells were collected by centrifugation. Total RNA was isolated using the RNeasy mini kit (Qiagen, Hilden, Germany). Total RNA (1 μg) was reverse transcribed and progressive dilutions (1/10, 1/100, 1/1000) were then subjected to PCR amplification. cDNA of IL-8 was amplified using the primers previously described by Chiang34 and by a new set of primers developed by us that were more efficient. Thus, primers used were AGCCAGGAAGAAACCACCGGA and TCCACAACCCTCTGCACCCAGT that generated an expected PCR product of 315 bp (NM000584 Genbank locus, GI:28610153).
By the sense TGACGGGGTCACCCACACTGTGCCCATCTA and antisense CTAGAAGCATTTGCGGTGGACGATGGAGGG primers an expected 649 bp region of β-actin mRNA (E00829 Genbank locus sequence, GI:2169090) was amplified, as previously described.35, 36, 37
Temperature and time were modified from the original methodology: cDNA was amplified by 40 cycles of 30 s at 94°C, 30 s at 56°C and 30 s at 72°C. The extension time of the last 15 cycles was incremented by 3 s/cycle.
To obtain a relative quantification of gene expression, 1/10, 1/100 and 1/1000 of total cDNA was amplified, PCR products were separated in 2% agorose gel, stained with ethidium bromide and visualized under an UV transillumination by KODAK Image Station 4000 MM (Carestream Health). Band intensity of each PCR reaction was quantified by KODAK Molecular Imaging Software 4.0 and corrected for β-actin-amplified cDNA intensity.
RESULTS
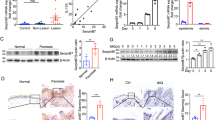
Based on what had been previously demonstrated on the signaling pathways sustaining IL-8 production in keratinocytes,15, 16 we have studied the involvement of ERKs in IL-8 production by IL-17 and IL-22-stimulated NCTC cells. NCTC cells were treated with IL-17 and IL-22 (20 ng/ml) and relative pERK levels were quantified by western blot analysis. Figure 1a shows the kinetic of MEK-ERK pathway activation by ILs treatment. After 24 h, a significant (treated vs untreated (T=0) cell cultures: P<0.05 by ANOVA) increase of pERK levels were found in both IL-17 and IL-22-treated cell cultures (Figure 1b). To test whether IL-8 production needed MEK-ERK signaling activation in NCTC cells, we quantified the released levels of IL-8 in cell culture medium after inhibition of MEK enzymatic activity by U0126. Figure 1c shows that NCTC cells spontaneously secrete detectable levels (4.0±0.4 ng/ml/106 cells) of IL-8, that are significantly reduced by the treatment with U0126 (2.6±0.2 ng/ml/106 cells; P<0.05 by ANOVA). Stimulation of NCTC cells with IL-17 and IL-22 increase significantly (treated vs untreated cell cultures: P<0.05 by ANOVA) the levels of secreted IL-8, which, in turn, is significantly reduced by the inhibition of the MEK-ERK pathway (Figure 1c, black bars vs empty bars of IL-17 and IL-22-treated cells).
IL-17 and IL-22 induce IL-8 secretion by ERK activation. (a) Kinetic analysis of IL-17 and IL-22 effects on ERKs phosphorylation levels by western blot. A representative pERK immunoblotting is shown. NCTC cells were treated with 20 ng/ml of either cytokine and at the indicated times pERKs levels were detected by western blot. (b) Densitometric histograms of pERKs expression. Means of three independent experiments±s.d.; P<0.05 ANOVA, Dunnet's test (vs unstimulated cells cultures). (c) IL-8 secretion in the culture medium of NCTC cells analyzed by ELISA. NCTC cells were treated for 24 h with IL-17 and IL-22 in the presence or absence of 10 μM U0126. Levels of IL-8 are reported as ng/ml and corrected for the number of seeded cells. Treatment with 10 μM of U0126 (filled bars) significantly impairs both basal (untreated) and IL-22- or IL-17-induced IL-8 secretion. Values are means of three independent experiments. DMSO was used as negative control. *P<0.05 vs ILs-untreated DMSO-treated cells (control); ANOVA test.
Given that hydrogen sulfide induces the dephosphorylation of the Raf-MEK-ERK signaling pathway in NCTC cells,19 we then analyzed the effects of NaHS on IL-17- and IL-22-induced MAPK signaling, and on IL-17- and IL-22-mediated secretion of IL-8. Figure 2a and b shows that 2 mM NaHS is able to significantly reduce (lane 4 vs lane 1; P<0.05 by ANOVA) basal pERKs levels as well as to impair IL-17- and IL-22-induced ERK activation (lanes 5 and 6 vs lane 1; P<0.05 by ANOVA). The analysis of IL-8 mRNA levels confirmed that hydrogen sulfide treatment was consequently able to interfere with IL-8 expression at the transcriptional level (Figure 2c). As expected, the levels of IL-8 protein secreted in cell culture media were significantly decreased in cell cultures treated with NaHS (Figure 2d). NaHS impaired both basal (#P=0.019, t-test) and IL-17- and IL-22-induced secretion of IL-8 (#P=0.012 and #P=0.005, respectively, t-test).
NaHS impairs ERK phosphorylation and IL-8 expression. (a) A representative pERKs immunoblotting is shown. NCTC cells were treated with (+) or without (−) IL-17 and IL-22 in the presence (lanes 4–6) or absence (lanes 1–3) of 2 mM NaHS for 24 h. Total proteins were immunoblotted for the detection of pERK1/2 or β-tubulin. IL-17 and IL-22 induce ERK activation while sulfurs downregulate the expression levels of pERKs. (b) Densitometric histograms of pERKs expression. Means of three independent experiments±s.d.; *P<0.05 ANOVA, Dunnet's test (vs NaHS and ILs-untreated cell cultures, lane 1). (c) A representative RT–PCR analysis of IL-17 and IL-22 NCTC cell cultures treated for 24 h with 2 mM NaHS (+). Expression of IL-8 and β-actin from a representative experiment is reported. The expression levels of IL-8-amplified cDNA was analyzed by densitometry, corrected for β-actin-amplified cDNA and reported as O.D. units. (d) IL-8 secretion in the culture medium of NCTC cells analyzed by ELISA. Levels of IL-8 are reported as ng/ml and corrected for the number of seeded cells. Treatment with 2 mM NaHS (filled bars) impairs both basal (untreated) and IL-22- or IL-17-induced IL-8 expression levels. Values are the means of three independent experiments. *P<0.05 vs ILs- and NaHS-untreated cells (control); ANOVA test. #P<0.05 vs NaHS-untreated cells; t-test.
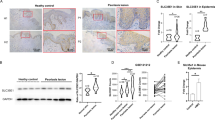
Since inhibition of ERKs represents the key event mediating the inhibition of IL-8 secretion in NaHS-treated NCTC cells, we decided to test the relevance of our findings to the pathophysiology of psoriasis by immunohistochemical detection of pERKs and IL-8 in patient biopsies. A voluntary male affected by psoriasis was locally treated with a 2-mM NaHS solution for 1 week, as described in Materials and methods. As expected, pERKs were strongly expressed in the keratinocytes of the psoriatic lesion, with both a cytoplasmic and nuclear localization (Figure 3c), while keratinocytes from normal epidermis expressed pERK with an exclusive cytoplasmic localization (Figure 3b as compared with negative control, Figure 3a). Accordingly, we observed a strong expression of IL-8 in the untreated skin of the psoriatic patient, where a diffuse immunostaining was observed in the keratinocytes present in the lesions (Figure 4c). As we previously reported,22 NaHS reduces ERK activation levels in psoriatic lesions, where total pERK expression is downregulated, with a dramatic decrease of its nuclear localization (Figure 3d). Of note, the treatment of the lesions with NaHS significantly reduced IL-8 expression as well (Figure 4d as compared with negative control, Figure 4a).
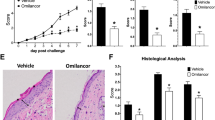
NaHS reduces ERKs activation in vivo. Immunohistochemical detection of pERK1/2 in the human skin of a patient affected by psoriasis. Biopsies of lesioned (a, c, d) and normal skin (b). Original magnification × 40. (a) PBS-treated lesion. The primary specific anti-pERKs antibody was omitted (negative control). (b) Normal, untreated skin. Staining with anti-pERK antibody. The insert shows two cells with the classic cytoplasmic localization of ERKs (original picture was 3 × zoomed). Arrows indicate the cytoplasmic localization of ERKs. (c) PBS-treated lesion. Staining with anti-pERK antibody. The insert shows three cells with nuclear localization of ERKs (original picture was 3 × zoomed). Arrows indicate the nuclear localization of ERKs. (d) NaHS-treated lesion. Staining with anti-pERK antibody.
NaHS reduces IL-8 expression in vivo. Immunohistochemical detection of IL-8 in the human skin of a patient affected by psoriasis. Biopsies of lesioned (a, c, d) and normal skin (b). Original magnification × 40. (a) PBS-treated lesion. The primary specific anti-IL-8 antibody was omitted (negative control). (b) Normal, untreated skin. Staining with anti-IL-8 antibody. (c) PBS-treated lesion. Staining with anti-IL-8 antibody. (d) NaHS-treated lesion. Staining with anti-IL-8 antibody.
DISCUSSION
IL-8 is known as a member of a large supergene family comprising a number of small (7–15 kDa) peptides with chemoattractant or mitogenic properties for a range of target cells. IL-8 is important for the recruitment of both neutrophils and T lymphocytes38 and greatly contributes to the major pathologic changes seen in psoriasis.
In line with previous data reporting that NCTC cells can secrete IL-8 under UV stimulation,39 we found that these cells spontaneously secrete detectable levels of IL-8 in culture. Knowing that IL-17 and IL-22 act as inducers of IL-8 secretion and that ERK activation is required for IL-8 production, we preliminary tested the sensitivity of NCTC cells to IL-17 and IL-22, specifically focusing on the kinetics of ERK activation, the levels of IL-8 mRNA production and IL-8 protein secretion. Like in primary keratinocytes,10, 14, 15, 16 IL-17 and IL-22 activate MAPK and induce IL-8 transcription and secretion also in NCTC cells. Although several other signaling pathways and intermediates (PKA, PKC, PI3-kinase/Akt and NF-κB) have been shown to be activated in the production of IL-8 by keratinocytes and other cells,17, 18, 19, 40 in agreement with Watanabe et al,16 we found that the role of ERK activation is critical, as IL-8 production under IL-17 and IL-22 stimulation is largely abrogated by the MEK inhibitor U0126. Here, we did not study other signaling pathways, but rather focused on the ERK signaling axis since we previously demonstrated22 that NaHS does not interfere either with the PI3K/Akt or p38 and JNK pathways.
When NCTC cells were treated with NaHS, both spontaneous and IL-17-/IL-22-induced IL-8 production was impaired via inhibition of ERK phosphorylation. However, NaHS was less efficient than U0126, probably due to lower specificity of NaHS vs U0126 in the inhibition of ERKs.
Sulfurs are able to penetrate the skin, and a sulfur-rich balneotherapy has been suggested to be effective in the treatment of psoriasis.25 According to previous studies, keratinocytes of hyperplastic epidermis express high levels of pERK and IL-8. pERKs show the classical nuclear localization, while keratinocytes of normal skin show low pERKs levels with a main cytoplasmic localization.21, 41, 42 According with the evidence that biologically active IL-8 is produced in large amounts in psoriatic skin3, 43 we have observed a strong immunoreactivity of the epidermal layer to anti-IL-8 antibody. When we treated topically a psoriatic lesion with NaHS kept in the same concentration range found in most balneotherapies, pERKs expression in the lesion was clearly reduced at both nuclear and cytoplasmic levels, paralleled by a concomitant reduction of IL-8 expression. These data must be considered as preliminary since only a single patient was treated. However, since the results obtained in vitro combined to the in vivo histological ones, the design of a clinical trial with sulfur-rich waters involving an adequate number of patients appears as reasonable. Spring water is classified as sulfurous when it contains >1 mg/l of H2S. Often sulfide concentration in such natural waters varies from 0.5 to 20 mg/l,44 which makes balneotherapy an effective option for these patients. Considering that we had previously demonstrated that sulfurs have subset-specific toxicity on CD8+ lymphocytes,26 another major player in the complex pathophysiology of psoriasis, we believe that sufficient scientific evidence is now starting to be accumulated to explain clinically relevant beneficial effects of sulfurs on psoriatic lesions.
References
Ghoreschi K, Weigert C, Röcken M . Immunopathogenesis and role of T cells in psoriasis. Clin Dermatol 2007;25:574–580.
Grossman RM, Krueger J, Yourish D, et al. Interleukin 6 is expressed in high levels in psoriatic skin and stimulates proliferation of cultured human keratinocytes. Proc Natl Acad Sci USA 1989;86:6367–6371.
Tuschil A, Lam C, Haslberger A, et al. Interleukin-8 stimulates calcium transients and promotes epidermal cell proliferation. J Invest Dermatol 1992;99:294–298.
Johnson MO, Charlebois E, Morin SF, et al. Effects of a behavioral intervention on antiretroviral medication adherence among people living with HIV: the healthy living project randomized controlled study. J Acquir Immune Defic Syndr 2007;46:574–580.
Prinz JC . Which T cells cause psoriasis? Clin Exp Dermatol 1999;24:291–295.
Ghoreschi K, Thomas P, Breit S, et al. Interleukin-4 therapy of psoriasis induces Th2 responses and improves human autoimmune disease. Nat Med 2003;9:40–46.
Lee E, Trepicchio WL, Oestreicher JL, et al. Increased expression of interleukin 23 p19 and p40 in lesional skin of patients with psoriasis vulgaris. J Exp Med 2004;199:125–130.
Zaba LC, Cardinale I, Gilleaudeau P, et al. Amelioration of epidermal hyperplasia by TNF inhibition is associated with reduced Th17 responses. J Exp Med 2007;204:3183–3194.
Annunziato F, Cosmi L, Santarlasci V, et al. Phenotypic and functional features of human Th17 cells. J Exp Med 2007;204:1849–1861.
Liang SC, Tan XY, Luxenberg DP, et al. Interleukin (IL)-22 and IL-17 are coexpressed by Th17 cells and cooperatively enhance expression of antimicrobial peptides. J Exp Med 2006;203:2271–2279.
Zheng Y, Danilenko DM, Valdez P, et al. Interleukin-22, a T(H)17 cytokine, mediates IL-23-induced dermal inflammation and acanthosis. Nature 2007;445:648–651.
Lowes MA, Kikuchi T, Fuentes-Duculan J, et al. Psoriasis vulgaris lesions contain discrete populations of Th1 and Th17 T cells. J Invest Dermatol 2008;128:1207–1211.
Boniface K, Guignouard E, Pedretti N, et al. A role for T cell-derived interleukin 22 in psoriatic skin inflammation. Clin Exp Immunol 2007;150:407–415.
Boniface K, Bernard FX, Garcia M, et al. IL-22 inhibits epidermal differentiation and induces proinflammatory gene expression and migration of human keratinocytes. J Immunol 2005;174:3695–3702.
Kawaguchi M, Kokubu F, Odaka M, et al. Induction of granulocyte-macrophage colony-stimulating factor by a new cytokine, ML-1 (IL-17F), via Raf I-MEK-ERK pathway. J Allergy Clin Immunol 2004;114:444–450.
Watanabe H, Kawaguchi M, Fujishima S, et al. Functional characterization of IL-17F as a selective neutrophil attractant in psoriasis. J Invest Dermatol 2009;129:650–656.
Kawaguchi M, Kokubu F, Kuga H, et al. Modulation of bronchial epithelial cells by IL-17. J Allergy Clin Immunol 2001;108:804–809.
Kawaguchi M, Onuchic LF, Huang SK . Activation of extracellular signal-regulated kinase (ERK)1/2, but not p38 and c-Jun N-terminal kinase, is involved in signaling of a novel cytokine, ML-1. J Biol Chem 2002;277:15229–15232.
Sebkova L, Pellicanò A, Monteleone G, et al. Extracellular signal-regulated protein kinase mediates interleukin 17 (IL-17)-induced IL-8 secretion in Helicobacter pylori-infected human gastric epithelial cells. Infect Immun 2004;72:5019–5026.
McKenzie RC, Sabin E . Aberrant signalling and transcription factor activation as an explanation for the defective growth control and differentiation of keratinocytes in psoriasis: a hypothesis. Exp Dermatol 2003;12:337–345.
Johansen C, Kragballe K, Westergaard M, et al. The mitogen-activated protein kinases p38 and ERK1/2 are increased in lesional psoriatic skin. Br J Dermatol 2005;152:37–42.
Gobbi G, Ricci F, Malinverno C, et al. Hydrogen sulfide impairs keratinocyte cell growth and adhesion inhibiting mitogen-activated protein kinase signaling. Lab Invest 2009;89:994–1006.
Wallace JL . Hydrogen sulfide-releasing anti-inflammatory drugs. Trends Pharmacol Sci 2007;28:501–505.
Caliendo G, Cirino G, Santagada V, et al. Synthesis and biological effects of hydrogen sulfide (H2S): development of H2S-releasing drugs as pharmaceuticals. J Med Chem 2010;53:6275–6286.
Matz H, Orion E, Wolf R . Balneotherapy in dermatology. Dermatol Ther 2003;16:132–140.
Mirandola P, Gobbi G, Sponzilli I, et al. Exogenous hydrogen sulfide induces functional inhibition and cell death of cytotoxic lymphocytes subsets. J Cell Physiol 2007;213:826–833.
Merighi S, Benini A, Mirandola P, et al. Hypoxia inhibits paclitaxel-induced apoptosis through adenosine-mediated phosphorylation of bad in glioblastoma cells. Mol Pharmacol 2007;72:162–172.
Merighi S, Benini A, Mirandola P, et al. A3 adenosine receptors modulate hypoxia-inducible factor-1alpha expression in human A375 melanoma cells. Neoplasia 2005;7:894–903.
Gobbi G, Mirandola P, Micheloni C, et al. Expression of HLA class I antigen and proteasome subunits LMP-2 and LMP-10 in primary vs metastatic breast carcinoma lesions. Int J Oncol 2004;25:1625–1629.
Vitale M, Pelusi G, Taroni B, et al. HLA class I antigen down-regulation in primary ovary carcinoma lesions: association with disease stage. Clin Cancer Res 2005;11:67–72.
Mirandola P, Sponzilli I, Solenghi E, et al. Down-regulation of human leukocyte antigen class I and II and beta 2-microglobulin expression in human herpesvirus-7-infected cells. J Infect Dis 2006;193:917–926.
Merighi S, Benini A, Mirandola P, et al. Caffeine inhibits adenosine-induced accumulation of hypoxia-inducible factor-1alpha, vascular endothelial growth factor, and interleukin-8 expression in hypoxic human colon cancer cells. Mol Pharmacol 2007;72:395–406.
Merighi S, Simioni C, Gessi S, et al. A(2B) and A(3) adenosine receptors modulate vascular endothelial growth factor and interleukin-8 expression in human melanoma cells treated with etoposide and doxorubicin. Neoplasia 2009;11:1064–1073.
Chiang YY . Hepatocyte growth factor induces hypoxia-related interleukin-8 expression in lung adenocarcinoma cells. Mol Carcinog 2009;48:662–670.
Mirandola P, Secchiero P, Pierpaoli S, et al. Infection of CD34(+) hematopoietic progenitor cells by human herpesvirus 7 (HHV-7). Blood 2000;96:126–131.
Mirandola P, Sponzilli I, Gobbi G, et al. Anticancer agents sensitize osteosarcoma cells to TNF-related apoptosis-inducing ligand downmodulating IAP family proteins. Int J Oncol 2006;28:127–133.
Mirandola P, Gobbi G, Ponti C, et al. PKCepsilon controls protection against TRAIL in erythroid progenitors. Blood 2006;107:508–513.
Hsu HC, Tsai WH, Chen PG, et al. In vitro effect of granulocyte-colony stimulating factor and all-trans retinoic acid on the expression of inflammatory cytokines and adhesion molecules in acute promyelocytic leukemic cells. Eur J Haematol 1999;63:11–18.
Grandjean-Laquerriere A, Gangloff SC, Le Naour R, et al. Relative contribution of NF-kappaB and AP-1 in the modulation by curcumin and pyrrolidine dithiocarbamate of the UVB-induced cytokine expression by keratinocytes. Cytokine 2002;18:168–177.
Grandjean-Laquerriere A, Le Naour R, Gangloff SC, et al. Contribution of protein kinase A and protein kinase C pathways in ultraviolet B-induced IL-8 expression by human keratinocytes. Cytokine 2005;29:197–207.
Yu XJ, Li CY, Dai HY, et al. Expression and localization of the activated mitogen-activated protein kinase in lesional psoriatic skin. Exp Mol Pathol 2007;83:413–418.
Takahashi H, Ibe M, Nakamura S, et al. Extracellular regulated kinase and c-Jun N-terminal kinase are activated in psoriatic involved epidermis. J Dermatol Sci 2002;30:94–99.
Terui T, Ozawa M, Tagami H . Role of neutrophils in induction of acute inflammation in T-cell-mediated immune dermatosis, psoriasis: a neutrophil-associated inflammation-boosting loop. Exp Dermatol 2000;9:1–10.
Stambuk-Giljanovic N . Characteristics and origin of the hydrogen sulphide spring water from the Split spa (Southern Croatia). Environ Monit Assess 2008;140:109–117.
Acknowledgements
We are grateful to Instrumentation Laboratory for scientific support, and to Enzo Palermo and Luciana Cerasuolo for technical support. This work was supported by GG grant of IT-Ministry of Health (Ricerca Finalizzata 2007–2008) Strategic Program (title: Transcriptomic and proteomic profiles for identification of novel clinical biomarkers of cardiovascular risk in women); MV grant of IT-Ministry of Heath grant (Ricerca Finalizzata 2007–2009) Ordinary Project (title: Tissue engineering in osteoarticular disease: basic and clinical evaluation); GP grant of FORST (Fondazione per la Ricerca Scientifica Termale). MV grant of IT-Ministry of Heath grant (Ricerca Finalizzata 2007–2009) Ordinary Project (title: Therapeutic applications of stem cells in the treatment of heart failure). MV grant of IT-Ministry of the University and Scientific and Technological Research/Ministry of Education, University and Research (FIRB-accordi di programma 2011–2014) (title: Pathogenesis and molecular targets in degenerative musculoskeletal diseases).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Hydrogen sulfide reduces the basal expression of IL-8, and interferes with IL-17 and IL-22-induced IL-8 production in human keratinocytes. These new observations, taken together with the known anti-inflammatory activity of H2S, are relevant to understanding previously unexplained effects of sulfur-rich balneotherapy in the treatment of psoriasis.
Rights and permissions
About this article
Cite this article
Mirandola, P., Gobbi, G., Micheloni, C. et al. Hydrogen sulfide inhibits IL-8 expression in human keratinocytes via MAP kinase signaling. Lab Invest 91, 1188–1194 (2011). https://doi.org/10.1038/labinvest.2011.76
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2011.76
Keywords
This article is cited by
-
Clinical efficacy of medical hydrology: an umbrella review
International Journal of Biometeorology (2021)
-
From in vitro research to real life studies: an extensive narrative review of the effects of balneotherapy on human immune response
Sport Sciences for Health (2021)
-
Morphological and Immunohistochemical Features of the Heart under the Effect of Hydrogen Sulfide Balneotherapy
Bulletin of Experimental Biology and Medicine (2021)
-
Digital dermatitis in cattle is associated with an excessive innate immune response triggered by the keratinocytes
BMC Veterinary Research (2013)