Abstract
Mice lacking the 66 kDa isoform of the adapter molecule shcA (p66shcA) display increased resistance to oxidative stress and delayed aging. In cultured cell lines, p66 promotes formation of Reactive Oxygen Species (ROS) in mitochondria, and apoptotic cell death in response to a variety of pro-oxidant noxious stimuli. As mitochondrial ROS and oxidative cell damage are clearly involved in alcohol-induced pathology, we hypothesized that p66 may also have a role in ethanol. In vivo, changes observed in p66+/+ mice after 6-week exposure to ethanol in the drinking water, including elevated serum alanine aminotransferase (ALT), liver swelling and evident liver steatosis, were significantly attenuated in p66−/− mutant mice. Biochemical analysis of liver tissues revealed induction of the p66 protein by ethanol, whereas p66-deficient livers responded to alcohol with a significant upregulation of the mitochondrial antioxidant enzyme MnSOD, nearly absent in control mice. Evidence of an inverse correlation between expression level of p66 and protection from alcohol-induced oxidative stress was also confirmed in vitro in primary hepatocytes and in HepG2-E47 cells, an ethanol-responsive hepatoma cell line. In fact, MnSOD upregulation by exposure to ethanol in vitro was much more pronounced in p66KO versus wild-type isolated liver cells, and blunted in HepG2 cells overexpressing p66shc. p66 overexpression also prevented the activation of a luciferase reporter gene controlled by the SOD2 promoter, indicating that p66 repression of MnSOD operates at a transcriptional level. Finally, p66 generated ROS in HepG2 cells and potentiated oxidative stress and mitochondrial depolarization by ethanol. Taken together, the above observations clearly indicate a role for p66 in alcohol-induced cell damage, likely via a cell-autonomous mechanism involving reduced expression of antioxidant defenses and mitochondrial dysfunction.
Similar content being viewed by others
Main
Ethanol-related pathology represents a worldwide relevant public health issue.1, 2 In the liver, pathological consequences of chronic abuse of ethanol include steatosis, steatohepatitis, fibrosis and cirrhosis. Eventually, primary hepatocarcinoma can develop as a consequence of both the direct carcinogenic effect of ethanol and alcohol-induced cell necrosis/regeneration.3
The molecular mechanisms underlying ethanol hepatotoxicity are still under debate. In a current model, hepatocyte accumulation of triglycerides and cholesterol (steatosis) is, at least in part, because of increased lipogenesis by excess NADH and acetyl-CoA derived from ethanol catabolism. Alcohol-induced modifications in the function of key regulators of lipid metabolism, such as PPAR-γ and sterol-regulated element-binding protein (SREBP), also have been convincingly shown to take a role in this process.4, 5, 6
As for ethanol-induced hepathocyte apoptosis/necrosis, inflammation, fibrosis and eventually cirrhosis, a major pathogenic role is currently imputed to the action of deleterious Reactive Oxygen Species (ROS).1, 7 These oxidant intermediates are generated both in the extra mitochondrial compartment by cytochrome p450 2E1 (CyP 2E1),8 which is part of the Microsomal Ethanol Oxidizing System, and by the mitochondrial respiratory chain9 where the reducing equivalents produced by ethanol are eventually converted into energy.
Regardless of the subcellular source of ROS, ethanol-induced oxidative stress impacts on mitochondrial function, compromising energy metabolism and promoting the cytosolic release of apoptogenic factors and, as a final consequence, cell death by both necrosis and apoptosis.10 In keeping with this general scheme, manganese-dependent mitochondrial superoxide dismutase is upregulated by ethanol treatment in rat liver,11 and modulation of antioxidant enzymes superoxide dismutases 1 (cytosolic) and 2 (mitochondrial) and catalase have been shown to affect alcohol hepatotoxicity both in vivo12, 13 and in vitro.14, 15 Moreover, we have recently reported that, in ethanol-fed mice, hepatocyte apoptosis is largely mediated by the tumor suppressor protein p53,16 which promotes cell death through the mitochondrial generation of oxidant intermediates.17 Importantly, resistance to liver apoptosis in p53-deficient mice correlates with elevated expression of the mitochondrial superoxide dismutase.16
In recent years, much attention has been drawn by the signaling adapter protein p66shcA, as a major determinant of cell resistance to oxidative stress and to oxidant-induced cell damage and death.18 This molecule is in part localized in mitochondria where it promotes, through mechanisms only partially clarified,19 the generation of ROS in response to an array of noxious stimuli.20 In fact, cell lines derived from p66-deficient mice have reduced levels of intracellular oxidant species, and are resistant to pro-oxidants such as hydrogen peroxide.21 More importantly, these animals live 30% longer than control, p66-proficient littermates,18 and are remarkably resistant to pathologies known to be mediated by oxidative tissue damage, such as atherosclerosis,22 hind limb ischemia-reperfusion23 and, most relevant to the present study, liver necrosis by carbon tetrachloride poisoning.19 p66shc has also been shown to participate in the pro-apoptotic cascade triggered by p53 and to mediate, at least in part, the effect of p53 on the mitochondrial production of radical species.20
Reproduction of the pathological effects of chronic ethanol abuse in alcohol-fed rodents, along with the increasing availability of genetically modified mouse strains has, in the last few years, significantly contributed to understanding of the molecular basis of ethanol toxicity.12, 16, 24, 25, 26, 27
Prompted by the recent emphasis on the role of p66shc in oxidant-induced cell damage and aging, and in view of the recognized role of mitochondrial oxidative stress in tissue injury by alcohol, we sought to evaluate the pathological effects of ethanol feeding in mice deficient of p66shc, in comparison to p66-proficient littermates. In parallel, we investigated in vitro the response of primary hepatocytes from wild-type and p66−/− mice, and of an ethanol-metabolizing human hepatocellular carcinoma, to physiologically relevant amounts of ethanol. The aim of this study was to evaluate p66 as a potential molecular mediator of the deleterious effects of alcohol on cell metabolism and viability, and to obtain fresh evidence on the role of mitochondrial damage in the pathogenesis of alcohol-dependent pathology.
MATERIALS AND METHODS
Animals
Sv129-p66shcA WT and p66shcA−/− (henceforth indicated as WT and p66 KO) mice have been described.18 Selective inactivation of the 66 kDa isoform of the adapter molecule Shc (Src Homology and Collagen) has been obtained by targeting part of the 5′ end of exon 2, upstream of ATG2. Mutant mice used in the present study are in the outbreed Sv129 genetic background, and appear healthy and fertile. Progeny from heterozygous p66+/− breeders was routinely genotyped by allele-specific PCR,18 and p66+/+ and p66−/− littermates were utilized for experimental procedures.
Animals were originally provided by Professor PG Pelicci (European Institute of Oncology, Milan, Italy) and were maintained in a temperature-controlled room with a 12 h light/dark cycle, in the animal facility of Universita’ Cattolica del Sacro Cuore, Rome. All experimental procedures involving animals complied with the Guidelines of the Italian National Institute of Health, and were approved by the Institutional Ethical Committee.
Plasmids and Cell Lines
The SODLUC-3340 reporter construct containing a 3340 bp fragment of the MnSOD human promoter upstream of the Firefly luciferase cDNA28 has been kindly provided by Dr MB Yim (NIH, Bethesda, MD, USA). The promoter sequence was mutagenized at position −1245(C → G) to inactivate a putative reverse binding site for the Foxo3A transcription factor, according to Kops et al.29 The retroviral construct encoding the human p66shc cDNA in the pBabe/Puro backbone, and the corresponding empty vector, have been provided by Dr Marco Giorgio (European Institute of Oncology, IEO, Milan). cDNA encoding the redox-sensitive fluorescent protein rxYFP[Cys149−Cys202] was kindly provided by Dr JR Winther (Carlsberg Laboratory, Copenhagen, Denmark). The cDNA was excised from the original plasmid and subcloned in the EcoRI site of the mammalian expression vector (Invitrogen, San Giuliano Milanese, Italy). Insert orientation and cDNA integrity were verified by automated sequencing.
HepG2 cells expressing the cytochrome P450 2E1 (CyP2E1, clone E47)35 have been provided by Dr A Cederbaum (Mount Sinai School of Medicine, NY, USA). Cells were routinely maintained in selective medium (DMEM containing 8% FCS and 400 μg/ml G418) and split 1:5 every week. Cyp2E1 expression was periodically confirmed by enzymatic assay.
HepG2 E47 cells stably overexpressing the p66 cDNA under the LTR retroviral promoter (henceforth E47-p66), or the corresponding empty vector (henceforth E47-pBabe) were generated by cell transfection with Effectene- (Qiagen, Milan, Italy) according to the manufacturer's recommendations, followed by 4 days selection in 2.5 μg/ml Puromycin (Sigma, Milan, Italy). P66 overexpression was initially verified and periodically confirmed by immunoblot analysis.
Preparation of Primary Hepatocytes
For hepatocyte preparation, pairs of male p66+/+ and p66−/− littermates were killed by cervical dislocation, and liver tissues rapidly removed, minced with scissors and incubated in Hepatocyte Complete Medium (HCM, CloneticsTM supplemented with Insulin, Transferrin, Ascorbic Acid, BSA, Hydrocortisone 21 Hemisuccinate, EGF and Antibiotics) and containing 2.5 mg/ml. Collagenase IV (Sigma cat. no. C-5138) for 1 h at 37°C with occasional shaking. Tubes were left standing for 1 min and supernatants removed and centrifuged at low speed (50 g for 5 min). Pellets containing liver cells were resuspended for 2 min at room temperature in ACK buffer (150 mM NH4Cl, 1 mM KHCO3, 0.1 mM EDTA, pH 7.2) to lyse red cells. After one wash in HCM cells were counted and seeded in 12 well clusters (5 × 104 cells per well) for further manipulation. This simple procedure yielded hepatocyte suspensions whose viability was always at least than 80% based on Trypan blue exclusion.
Ethanol Intoxication
Six- to eight-week-old, weight- (20–25 g initial body weight) matched male p66+/+ and p66−/− littermates were allowed to drink ad libitum a mixture containing increasing concentrations of ethanol (10% for 2 days; 15% for 3 days and 20% thereafter) plus 20% sucrose as the only source for drinking fluid during the 6-week period of treatment, or just water and sucrose (control groups of both genotypes).11, 16 Mice were monitored daily for clinical appearance, weight gain and drinking rate (about 5 ml per mouse per day with no differences among the four groups). As treatment consistently decreased food intake in both WT and p66−/− groups, diet in the ethanol groups was substantially enriched in vitamins and micronutrients, as previously described,11 to minimize the confounding effect of potential malnutrition on liver parameters. Decreased food intake compensated for caloric intake from ethanol-sucrose, as confirmed by the fact that weight gain curves between treated and control mice were superimposable (not shown).
Animals in the alcohol groups were kept without Et-OH for 18 h before death, but were allowed free access to drinking water. Animals from all groups were starved for food overnight before killing.
Liver Pathology
Immediately after killing the animals, livers were either fixed in paraformaldehyde or flash-frozen in liquid nitrogen and stored at −80°C. Fixed specimens were included in paraffin, sectioned and stained with Hematoxylin–Eosin for pathology. Steatosis score was assigned in a blinded manner by three of the authors (ORK, AMC and LML), as follows: 1≤25% hepatocytes containing fat droplets; 2=25–50%; 3=50–75%; 4≥75%.30
Determination of Serum ALT
Blood specimens were obtained by cardiac puncture; sera were stored at −20°C and routinely processed for enzymatic determination of alanine aminotransferase (ALT) activity.
Vitamin E Measurement
Tissue content of vitamin E in total liver homogenates was determined by HPLC as previously described.31
In Vitro Studies
For stimulation with ethanol, primary hepatocytes were seeded immediately after purification in collagen-coated 12-well tissue culture clusters (50 × 104 cells per well), in 2 ml HCM buffered with 1 mM Hepes, pH 7.4, Ethanol was added at a different concentration ranging from 50 to 200 mM and the plate was sealed with Parafilm M (SPI Supplies Inc., West Chester, PA, USA) to minimize evaporation. After 16 h, the medium was removed, and attached cells lysed directly in the well, with a standard lysis buffer [Tris-HCl 10 mM; NaCl 150 mM; EDTA 5 mM] containing 1% Triton X-100, 0.1% SDS, protease and phosphatase inhibitors. Floating cells were recovered by centrifugation, lysed separately and pooled with adherent cells.
After 15 min on ice, cell lysates were cleared by centrifugation at 14 000 rpm (18 650 g) at 4°C, and the supernatants quantified for the protein content (DC protein assay, BIORAD) and mixed with 6X Laemmli's buffer for anti-MnSOD, anti-CREB and anti-phospho Ser 133 CREB immunoblotting.
HepG2 E47 cells were seeded at 105 cells per well in 12-well clusters in DMEM containing 0.5%FCS, Hepes 1 mM, ph 7.4 and no selective drugs. Ethanol was added at 50–200 mM final concentration in 2 ml medium, and the plate sealed as described above. Cell lysis and protein analysis were performed as described for primary hepatocytes.
Luciferase Reporter Assays
The pSODLUC-3340 reporter construct, containing a 3.3 kilobase portion of the human SOD2 promoter upstream of the Firefly luciferase gene, and its derivative lacking the putative Foxo-responsive element, have been already described.28 The two constructs (pSODLUC-3340 and pSODLUC-3340mt, 0.4 μg each) were cotransfected in the HepG2 E47 cell line with the pRL-TK plasmid (0.04 μg) containing Renilla luciferase driven by the thymidine kinase promoter, as an internal control for transfection efficiency, and either the empty pBabe/Puro vector or the p66shc-Puro construct (0.6 μg), using the Effectene reagent (Qiagen) according to the manufacturer's recommendations. Forty-eight hours after transfection cells were seeded in 12-well cluster plates (105 per well) and, once attached to the plate, serum-starved and exposed to 100 mM Ethanol (0.6%) for additional 18–20 hours. The culture plate was sealed with Parafilm, to minimize ethanol evaporation. Luciferase activity was measured and normalized for transfection efficiency using the Dual Luciferase gene reporter assay (Promega s.r.l., Milan, Italy).
Analysis of Intracellular Oxidation by rxYFP
HepG2 E47 cells were seeded in 35 mm glass bottom dishes (Ibidi, Integrated Biodiagnostic, Martinsried, Germany) and transfected with 0.25 μg of the pcDNA3-rxYFP construct, mixed with 0.5 μg of p66shc-Puro or the corresponding empty vector (pBabe-Puro), using the Effectene reagent (Qiagen) according to the manufacturer's recommendations. After 72 h cells were serum starved and exposed to Ethanol for additional 18–20 h, or left untreated (PBS). Cell fluorescence was imaged and quantified by confocal microscopy (Leica, DM-IRE2 Germany).
To detect redox changes, while accounting for sample concentration, photobleaching or laser fluctuations, rxYFP emission fluorescence signals of samples excited at 488 nm (F488) and at 458 nm (F458) were measured and the ratio (F=F488/F458) calculated. Values of F for completely reduced (Fred) and completely oxidized (Fox) rxYFP were obtained from literature.36 Pseudocolor images were constructed based on I values, defined as

and ranging from 0 (complete oxidation) and 1 (complete reduction), by means of a dedicated software generated through the Labview 7.1 interface (Maulucci G et al, manuscript in preparation).
For image quantitation, average I values were determined within multiple Regions of Interest (ROIs, single cells or small cell clusters) for each sample, and their mean±s.d. (n=7–9) determined and utilized for further statistical analysis (two-way ANOVA and Bonferroni's post hoc comparison).
Evaluation of Mitochondrial Integrity
Intracellular (intramitochondrial) accumulation of the fluorescent dye Rhodamine 123 was used as an indicator of mitochondrial polarization and membrane integrity.29 Briefly, cells were exposed for 48 h to different concentrations of ethanol as described above, and labelled for the last 40 min with 10 μg/ml Rhodamine 123 (Invitrogen, Molecular Probes 1:1000 from a 10 mg/ml stock dissolved in DMSO). Cells were then washed with PBS, detached from the plate by trypsinization, resuspended in PBS and analyzed by standard flow cytometry (green fluorescence, FL-1) using a COULTER-EPICS Instrument equipped with a 488 nm Argon laser lamp.
Biochemical Studies
Liver homogenates were obtained by standard procedure. Briefly, livers were rinsed and minced in PBS, put in plastic tubes and disaggregated with a tissue homogenizer (three cycles of 15 s on ice) in PBS containing protease inhibitors. Homogenates were clarified by centrifugation at 18 500 g and assayed for protein content by a modified Lowry method, using a commercial kit according to the manufacturer's recommendations.
For western blot analysis, equal amounts of protein samples were resolved by SDS–PAGE, transferred onto nitrocellulose and immunoblotted with the sera of interest. Immunocomplexes were visualized by HRP-conjugates secondary reagents followed by ECL detection. The following antibodies were used in the present study: anti-p66shc and anti-MnSOD (Upstate Biotechnology); anti-phospho-FKHR (Thr 24)/FKHRL-1 (Thr32) (Cell Signaling Technology); anti-actin (Santa Cruz Biotechnology). Band intensities were quantified by volume densitometry, using a Gel.DOC Imaging Station equipped with a dedicated Software (QuantityOne). Densitometric values were normalized for the corresponding loading control band.
Statistics
All data from experiments in vivo are expressed as mean±s.d. Data series were compared by two-way ANOVA (http://faculty.vassar.edu/lowry/webtext.html), followed by Bonferroni's post hoc analysis (GraphPad), or by paired Student's t-test, were appropriate. The threshold of significance was set to a P-value of <0.05.
RESULTS
Attenuated Liver Damage by Alcohol in p66−/− Mice
C129sv mice harboring the homozygous deletion of the p66 kDa Shc adapter protein,18 and the corresponding p66+/+ littermates, were fed ethanol in the drinking fluid or plain water for 6 weeks, as previously described.16 Food and water/ethanol consumption, and weight gain curves did not present significant differences between the two mouse strains (not shown), ensuring that mutant and normal mice were exposed to comparable amounts of alcohol and to a similar dietary regimen.
Alcohol-fed wild-type mice presented a significant (roughly 30%) increase in the average liver weight in comparison to the corresponding control group at killing. Such an increase, indicative of organ swelling and injury, was nearly absent in p66−/− mice, providing an initial indication of a resistance to ethanol hepatotoxicity in this mouse mutant (Figure 1a). Accordingly, elevation in serum concentration of ALT, a marker of hepatocyte necrosis, was observed in p66+/+ mice following ethanol intoxication, but not (or not significantly) in p66−/− animals (Figure 1b). Although with some individual variability within groups, these data are clearly suggestive of a different response to ethanol feeding in mice lacking the longevity protein p66shc.
Effect of p66 deletion on macroscopic and hematochemical signs of chronic ethanol intoxication. (a) Exposure to ethanol increases average liver weight in p66+/+ (WT) but not in p66−/− (p66KO) mice. Experimental groups were of four mice each. Relevant P-values (two-way ANOVA followed by Bonferroni′s post-hoc comparison) are indicated. NS=not statistically significant. For each genotype data are expressed as liver weight relative to the average value of the control group, made equal to one. Average liver weight and liver- to- mouse weight ratio did not differ between WT and p66−/− animals (not shown). (b) Lack of p66 protects from ethanol hepatotoxicity. Blood was collected immediately after killing and processed by routine hematochemistry. ALT=alanine aminotransferase. The composition of the experimental groups is indicated. Statistics were calculated as in (a). NS=not statistically significant.
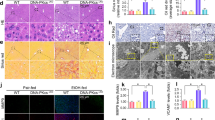
Prompted by this evidence we proceeded to histological examination of liver tissues. Hematoxylin–Eosin (H–E) staining of liver sections revealed, in agreement with several previous reports,4, 6 the presence of marked steatosis in alcohol-treated wild-type mice (Figure 2a, upper right panel). This was the predominant pathological change induced by ethanol; inflammation and fibrosis likely require a longer treatment or higher doses of alcohol to become evident, at least in our experimental setting. No or minimal steatosis was scored in mice fed the control, alcohol-free diet. Importantly, ethanol-induced lipid accumulation to a much lesser extent in the liver of p66−/− mice, in keeping with reduced organ swelling and with low serum markers of hepatocyte injury (compare upper right and lower right panels). Quantification of steatosis, based on the percentage of cells containing fat, indicated that protection from steatosis by p66shc deletion is not complete, but still highly significant (Figure 2b; P<0.05). This finding supports the idea of a role for p66shc in liver damage by alcohol, and indicates that p66 may act already at an early stage of the pathological sequence of liver lesions (steatosis → steatohepatitis → fibrosis → cirrhosis) known to entail chronical alcohol intoxication both in humans and in rodent experimental models.
Protection from liver steatosis in p66-deficient mice exposed to ethanol. (a) Examples of liver sections from control and ethanol-treated mice of the indicated genotype. Staining is Hematoxylin–Eosin (H–E). Lipid droplets, evident in treated p66+/+ (WT) mice and nearly absent in the corresponding p66−/− group, are indicated by arrows. (b) Liver steatosis quantification in the four experimental groups. Steatosis score was assigned by three of the authors, as follows: 1≤25% of hepatocytes containing fat. 2≤25–50%; 3=50–75%; 4≥75%. The number of animals per group is indicated. Statistics were calculated as in Figure 1 by factorial 2 × 2 ANOVA.
p66 is Induced by Ethanol and Modulates Antioxidant Response
p66 is transcriptionally induced and post-translationally activated (through phosphorylation on serine 36) by oxidative stress and promotes, in turn, generation of oxygen species, mitochondrial depolarization and apoptosis.18, 19 Ethanol-induced oxidative stress may trigger p66 in hepatocytes and damage cells through a p66-dependent cascade leading to mitochondrial failure and cell death. Alternatively, beneficial effects of p66 ablation on liver damage by ethanol may be indirect or non cell-autonomous.
To sort among these possibilities, p66 expression level was assessed by western blotting in liver homogenates from mice exposed to ethanol or to the alcohol-free diet. P66shc was nearly undetectable in control livers from p66+/+ mice (Figure 3a; each lane is a pool of two animals), but was clearly induced upon exposure to ethanol. As a negative control, no band was detected in homogenates from p66−/− mice. 293-T cells transfected with the p66 cDNA were used as positive control for p66 detection in the same experiment. Although the result of immunoblot analysis does not unequivocally rule out the possibility that the protein immunodetected in liver homogenates and induced by ethanol treatment derives from cells different from hepatocytes, the above observation, together with the recently reported involvement of p66 in liver injury by CCl4,19 argues in favor of a direct role for this protein in the toxic hepatocyte response to alcohol.
Attenuated oxidative stress by ethanol and upregulation of MnSOD in p66-deficient livers and isolated primary hepatocytes. (a) p66 is present in liver homogenates from p66+/+ (WT) mice and is induced by ethanol. Each lane represents a pool of two mice treated as indicated. The band corresponding to p66 shcA is indicated by an arrow. No p66 band is visualized in p66−/− (p66KO) mice. The same nitrocellulose filter was also immunoblotted with an anti-actin antiserum (lower panel) to ensure homogeneous protein loading throughout the gel. The strong actin band is indicated by an arrow. Representative of two independent experiments. (b) Vitamin E consumption by ethanol treatment in p66+/+ (WT) and p66−/− (p66KO) mice. Vitamin E content was measured in total liver homogenates, as described. Groups were of four mice each. Relevant statistics (two-way ANOVA) are indicated. Values observed in WT and p66−/− livers are expressed as are in line with the current literature. In the main histogram values for each ethanol-fed group are relative to the mean Vitamin E content in the corresponding control group. Numbers are mean±s.d. of individual mice. NS=not significant. (c) Induction of MnSOD in alcohol-treated p66−/− mice. Liver homogenates were subjected to western blot analysis with antisera against MnSOD (SOD2), and actin. Lanes are samples from individual mice treated as indicated. The marked upregulation of MnSOD in alcohol-treated mutant mice is absent in p66+/+ (WT) samples. Anti actin immunoblotting reveals comparable protein loading in all the lanes. Relevant bands are indicated by arrows. (d) Western blot analysis of MnSOD expression in primary mouse hepatocytes exposed to ethanol in vitro. Cell were isolated as described in the appropriate section and stimulated with the indicated amounts of ethanol for 16 hours. MnSOD upregulation by ethanol appears to be amplified in p66−/− cells. The actin band is displayed as loading control. Numbers are optical density values for the MnSOD band, after normalization for the corresponding actin band (NOD=Normalized Optical Density).
In support of the view that alcohol-induced oxidative stress is reduced in the absence of p66, ethanol consumption led to a significant decrease in the liver content of vitamin E, reportedly due to oxidative consumption,32 in p66+/+ mice (down to 46.8±11% of the untreated controls, Figure 3b) but not in p66−/− animals. This finding is consistent with previous reports of impaired generation of ROS in p66−/− cell lines21 and in the vasculature of p66−/− mice.22, 33 It should also be noted that liver malondialdehyde (MDA, an index of lipid peroxidation) content was not different between normal and mutant mice, and was in either case only minimally increased by alcohol (data not shown). This finding indicates that Vitamin E depletion is a more sensitive indicator of alcohol-induced oxidative stress, at least in our experimental setting, than is MDA accumulation, and that presumably, vitamin E effectively prevents lipid peroxidation and formation of MDA in p66+/+ mice.
The molecular mechanism whereby p66shc promotes oxidative stress in tissues is still under debate. Although evidence has been recently provided for an unexpected reaction in which p66 directly generates hydrogen peroxide using cytochrome c as an electron donor,19 the pro-oxidant action of this molecule is believed to be also mediated by the phosphorylation/inactivation of the FOXO family transcription factor FKHR-L1 (Foxo 3a),34 and by the downregulation of FOXO-regulated antioxidant enzymes, namely catalase and mitochondrial superoxide dismutase (SOD2).34, 29 According to the latter model, SOD2 is expected to be hyper-expressed in p66-deficient tissues; importantly, several lines of evidence indicate a protective role for MnSOD in ethanol-related liver pathology.11, 13, 14, 16
In search for a mechanism linking lack of p66shc and increased hepatocyte resistance to alcohol injury, we assessed the expression level of SOD2 in the liver of p66−/− and p66+/+ mice. As indicated by the western blot analysis shown in Figure 3c, mice from the two control groups (p66+/+ ctrl and p66−/− ctrl) expressed comparable amounts of immunoreactive SOD2; however, exposure to ethanol increased SOD2 expression in mutant mice, whereas enzyme upregulation was nearly absent in p66+/+ animals. This finding indicates that active scavenging of mitochondrial ROS may contribute, at least in part, to attenuate alcohol-induced damage in p66−/− hepatocytes.
Effects of p66 on Cell Response to Alcohol are Cell-Autonomous and can be Reproduced In Vitro
To gain a more mechanistic insight into the functional link between p66shc, MnSOD and cell response to alcohol injury, we decided to investigate the effect of cell exposure to ethanol in vitro. To this end, primary hepatocytes were freshly isolated from the liver of male p66−/− mice and their p66+/+ littermates, maintained in complete hepatocyte medium for 2–3 h and then exposed to 0.3 or 0.6% ethanol (50–100 mM roughly) for additional 16 h; culture dishes were sealed to prevent alcohol evaporation.
In keeping with evidence in vivo of MnSOD upregulation by alcohol in p66−/− liver tissue, SOD2 content was markedly increased, in a dose-dependent fashion, in p66−/− cultured liver cells; unlike in vivo, immunoreactive SOD2 was also induced, but to a lesser extent, in p66+/+ hepatocytes (Figure 3d). SOD2 content was constitutively higher in p66-deficient versus p66+/+ cells, even in the absence of ethanol challenge. Thus, in isolated liver cells, p66 inhibits MnSOD expression also in the absence of ethanol challenge, likely as part of a cellular response to purification and culture stress.
Human Hepatoma HepG2 cells (clone E47) genetically engineered to express the ethanol-metabolizing cytochrome p450 2E1 represent an established model for hepatocyte response to alcohol in vitro35 in alternative to primary hepatocytes, with the obvious advantages of an indefinitely growing cell line and the possibility to be further genetically manipulated.
HepG2 E47 cells exposed to physiologically relevant concentrations of Ethanol (0.3 or 0.6% v/v, for 24 h) recapitulated the biochemical responses observed in liver tissues and in primary hepatocytes in vitro, that is, upregulation of p66shc and induction of MnSOD (Figure 4a, left panels). More importantly, LTR-driven overexpression of p66shc cDNA in the same cell line led to a moderate accumulation of the protein and, in parallel, inhibited ethanol-induced upregulation of MnSOD (Figure 4a, right panels). These findings are consistent with the possibility, supported also by evidence from Figure 3d, that p66 inhibits a protective antioxidant response to ethanol brought about by the mitochondrial superoxide dismutase. Multiple transcriptional regulators control MnSOD expression in response to oxidative challenge. These include the cytokine-activated factors AP-1 and NF-kB, the tumor suppressor protein p53, and, as more recently reported, the FOXO-family factors FOXO-1(FKHR) and FOXO3a (FKHRL1); FOXO factors, in particular, increase the expression of MnSOD in cells deprived of exogenous growth factors,29 and have been shown, along different lines of evidence, to be phosphorylated and inactivated in a p66- and ROS-dependent fashion in NIH-3T3 cells.34 Collectively, these data qualify FOXOs as potential mediators of p66 effects on MnSOD in hepatocytes.
MnSOD induction by ethanol and modulation by p66shc in human hepatoma cells expressing CYP2E1 (HepG2-E47). (a) (left) HEPG2 E47 cells recapitulate in vitro biochemical aspects of hepatocyte response to alcohol. Induction of p66shc and upregulation of the mitochondrial superoxide in HepG2 E47 cells exposed to increasing concentrations of ethanol. (a) (right) Inhibitory effect of p66 overexpression on MnSOD response to ethanol challenge. FKHRL-1 phosphorylation on Threonine 32 is increased by Ethanol in parallel with p66 accumulation (left panels) and is constitutively high in p66 overexpressing cells (right panels). Blots representative of several (at least two) independent experiments. Relevant protein bands are indicated by arrows. Band densitometric values are reported as raw data (OD) or fold induction (FI), as indicated. (b) Gene reporter assay for MnSOD promoter activation in HEPG2 E47 cells exposed to ethanol (0.6%, about 100 mM). Values are fold induction of luciferase activity by 100 mM ethanol. The SODLUC-3334 reporter activation by ethanol is significantly repressed by coexpression of p66shc (P<0.005 by two-tailed paired t-test n=6). Response of a similar reporter lacking a Foxo3A-binding site29 (SODLUC-mut) to ethanol is reduced and largely insensitive to p66 shc. Values are mean±s.d. of multiple experiments (between two and six) performed independently.
In H47 pBabe cells cultured in serum-free medium, basal level phosphorylation of Foxo3a on Thr 32 was barely detectable, but could be increased by cell exposure to ethanol (Figure 4a). Notably, FKHRL-1 phosphorylation is associated with factor retention in the cell cytosol and decreased transcriptional activity.29 Foxo phosphorylation was found constitutively high in E47-p66 cells, and moderately increased by ethanol, consistent with the notion that this molecule represents a target for p66 in oxidant-challenged cells.34 The above finding therefore implicates Foxo3A in the inhibitory action exerted by p66 on MnSOD induction by ethanol.
To gain further insight in the modulation of MnSOD by p66, HepG2 cells were transiently transfected with a reporter construct encoding Renilla luciferase under the control of the SOD2 promoter, alone or in combination with the plasmid encoding human p66shc. In parallel cultures, a mutant form of the same reporter, lacking a putative Foxo3A target sequence (see experimental procedures) was transfected, with or without p66shc. As indicated in panel 4B, exposure to ethanol led to a significant increase of the SOD reporter activity, which was nearly completely abolished by the coexpression of p66 (1.59±0.28 fold induction versus 1.01±0.21, P<0.001). Interestingly, the mutant reporter, unresponsive to Foxo3a, was markedly less sensitive to both ethanol induction and modulation by p66 (4C). Taken together, these findings indicate that MnSOD induction by ethanol and repression by p66 operate, at least in part, at a transcriptional level, through a member of the Foxo transcription factor family.29
p66 Exacerbates Oxidative Stress and Mitochondrial Damage by Ethanol in Cultured Hepatoma Cells
Finally, to verify the functional relevance of MnSOD inhibition by p66 in the cell exposed to ethanol, HepG2E47 cells were cotransfected with the p66 cDNA or the corresponding empty control vector (pBabe), and a plasmid encoding for a redox sensitive mutant of the Yellow Fluorescent Protein (rxYFP), originally described by Ostergaard et al.36 A net decrease in fluorescent emission of this YFP derivative reveals protein oxidation through the formation of an intramolecular disulphide bond between engrafted cysteine residues 143 and 204,36 but the sensitivity of the probe can be further enhanced by ratiometric calculation, that is, by normalizing changes in emission intensity for the fluorescence values elicited at a less redox-sensitive excitation wavelength (Methods, and Maulucci G et al, manuscript in preparation). Confocal microscopy analysis of rxYFP and rxYFP/p66shc double transfectant HepG2E47 cells demonstrated that both overexpression of p66 (confirmed by immunoblot analysis of total protein lysates) and exposure to 100 mM ethanol led, separately, to a significant oxidation of HepG2E47 cells, as revealed by a yellow-to-red shift of cell pseudocolor in selected microscopic fields (Figure 5a), and by the quantification of signal ratios in multiple regions of interest (5b). Importantly, superexpression of p66 exacerbated oxidative stress by ethanol (P<0.01, two-way ANOVA). However, the combined effect was less-than-additive, suggesting that shared biochemical mechanisms, likely centered on mitochondria, underlie generation of ROS by alcohol and p66shc. In keeping with this view and with several previous reports, cell exposure to ethanol led to a decrease in mitochondrial integrity, as assessed by cell capacity to concentrate the fluorescent dye Rhodamine 1,2,3 (Figure 5d). Overexpression of p66 lowered the baseline mitochondrial potential of HepG2 E47 cells and amplified depolarization by ethanol, suggesting that, in this cell model at least, mitochondrial damage by alcohol is worsened by p66 via inhibition of MnSOD.
Effect of p66 on ethanol-induced oxidative stress and mitochondrial dysfunction in HepG2 E47 cells. (a) Representative pseudocolor images of HepG2 E47 cells 48 h after transfection of the redox-sensitive fluorescent protein rxYFP, in combination with p66shc or the corresponding empty vector (pBabe). Treatments are indicated. Cell color is function of the I parameter (see experimental procedures), whose value ranges from 0 (complete oxidation, red) to 1 (complete reduction, yellow). Yellow-to-red shift in cell color indicates cell oxidation. (b) Image quantitation based on multiple randomly chosen ROIs (Regions Of Interest, single cells or small cell clusters) for each treatment. Average I values within single ROIs were calculated. Columns are mean±s.d. of the average I values for the different treatments. N=7 for PBS, N=9 for Et-OH, N=7 for p66, N=8 for p66 + EtOH. Figure representative of two independent experiments. Relevant statistics (Two-way ANOVA followed by Bonferroni's post hoc test) are indicated. (c) Western blot analysis confirming expression of rxYFP and overexpression of p66shc in HepG2 E47 cells. (d) Mitochondrial membrane integrity monitored by the fluorescent dye Rhodamine 1,2,3. E47-p66 cells and the corresponding control line (E47-pBabe) were treated with ethanol, loaded with Rhodamine 123 and analyzed by standard flow cytometry as described in experimental procedures. Dose-dependent decrease of mean cell fluorescence in response to ethanol indicates loss of mitochondrial polarization. P66 reduces mitochondrial potential in untreated cells and exacerbates the effect of alcohol. Numbers are mean±s.d. of duplicate samples. Figure representative of two independent experiments.
DISCUSSION
In spite of extensive research in the field, the molecular mechanisms underlying damage to hepatocytes and other cell types by ethanol are still incompletely understood, and further information is critically needed to open novel preventive and therapeutic opportunities. The present work identifies the pp66kDa isoform of the adapter protein shc (p66shcA) as a molecule involved in the establishment of liver damage by alcohol, in a murine experimental model of chronic ethanol intoxication. Main findings in support of this conclusion are displayed in Figures 1 and 2, showing reduced liver swelling, serum ALT levels (a marker of hepatocyte necrosis) and attenuated fatty changes in p66−/− mice fed an alcohol-rich diet, in comparison to p66+/+ controls. Importantly, steatosis is the main pathological change observed in our model in alcohol-treated animals, with minimal signs of inflammation and fibrosis. This is probably due to the limited length of the treatment (6 weeks) and to the modality of animal exposure to ethanol (ad libitum feeding in the drinking water). This is a milder regime than other more robust models of ethanol feeding such as the liquid Lieber-DeCarli diet, or intragastric infusion.37 Therefore, although it is not possible to conclude that late stage aspects of alcohol-related pathology also would be attenuated by the absence of p66, this finding indicates an early role for p66shc in alcohol-induced hepatotoxicity.
Our data also address the mechanism underlying the role of p66 in liver damage by ethanol. In keeping with the recognized function of p66 as an inducer of oxidative stress and of mitochondrial damage in a number of ROS-related pathologies and presumably during the aging process,18, 22, 23 we provide indirect evidence, in vivo, that the establishment of oxidative stress in response to ethanol is attenuated in p66-deficient livers. In fact, vitamin E consumption, a reliable marker of tissue challenge by oxygen species, is marginal or absent in p66−/− mice exposed to ethanol, whereas significant in p66+/+ animals in parallel with the increase in the liver content of p66. Moreover, the manganese-dependent superoxide dismutase (MnSOD) is upregulated in p66-deficient livers in response to ethanol, but not in control mice, thus implying in the mutant mouse strain a better capacity of actively detoxifying mitochondrial ROS13 (Figure 3). Importantly, these data are corroborated by data provided in Figure 5, that forced expression of p66 in HepG2 E47 hepatoma cells in vitro induces ROS and potentiates oxidative stress and loss of mitochondrial membrane integrity induced by alcohol. Collectively these data provide a mechanistic link between reduced oxidative stress and protection from ethanol damage in p66−/− mice. Experiments based on antioxidant dietary supplementation during ethanol treatment, are ongoing, to further evaluate this link.
Experiments in vitro on primary hepatocytes and HepG2-E47 cells, expressing the cytochrome P450 2E1 cDNA under the transcriptional control of a viral promoter, have been designed to gain a more mechanistic insight in the molecular connection between alcohol-induced stress, p66shc and mitochondrial antioxidant response. The use of Cyp450 2E1 transfected cells, a well established in vitro model for cell response to ethanol, has been made necessary by technical limitations in genetically manipulating primary hepatocytes. This cell model has been already successfully employed to study mechanisms of ethanol toxicity at concentrations very close to those (100 mM) here utilized.38
Results displayed in Figures 3d and 4a, showing, respectively, enhanced induction of MnSOD by ethanol in p66-deficient hepatocytes and, vice versa, attenuated SOD2 increase in HepG2E47 cells overexpressing p66, are in agreement with findings in vivo and indicate that p66 effects on antioxidant response to alcohol are largely cell-autonomous, and independent from tissue factors (ie, inflammatory cytokines) presumably present in the complex microenvironment of an ethanol-metabolizing organ. Although the inhibitory action of p66shc on MnSOD expression in vitro confirms in vivo evidence, a number of differences emerge between the two experimental models. First, unlike in liver tissues, MnSOD expression in p66−/− isolated hepatocytes was found to be higher than in normal control cells. Second, in vitro, MnSOD is induced by ethanol in both p66+/+ and p66−/− cells (Figures 3d and 4a), although to a larger extent in the latter population, whereas evidence for enzyme induction in the p66+/+ livers in vivo is missing (Figure 3c). As for the first difference, it is possible that a threshold-level of cell stress is necessary to disclose p66 activity on MnSOD. With this respect, it should be acknowledged that procedure of cell enzymatic isolation and seeding in culture (at a higher oxygen concentration than is found in living tissues) represents a severe challenge for primary liver cells. It is noteworthy, on the other hand, that overexpression of p66shc in human hepatoma cells inhibits ethanol-induced SOD2 upregulation with little or no effect on the basal expression level of the enzyme (4A).
Along similar lines, culture conditions (ie, the modality of exposure to alcohol, which recapitulates more an acute intoxication than a chronic abuse) may explain MnSOD response to ethanol in p66-proficient cells (primary hepatocytes and hepatoma cells) in vitro.
Although molecular details of MnSOD regulation by p66 in response to ethanol challenge still need to be elucidated, evidence of Foxo3a hyperphosphorylation in E47-p66 cells (Figure 4a) and reporter assay data presented in Figure 4b suggest that a Foxo factor may have a role in this circuitry. As Foxo3a/FKHR-L1 appears to be phosphorylated/inactivated upon cell exposure to ethanol, this is unlikely to be the only transcriptional regulator mediating MnSOD induction by alcohol. Still, residual activity of this factor may be critical, within the MnSOD transcriptosome, to allow promoter activation by ethanol challenge, thereby justifying the inhibitory action of p66.
Unlike in HepG2 cells, ethanol-dependent phosphorylation of Foxo3a could not be detected in primary hepatocytes. Although technical limitations may underlie this result, mechanisms distinct from phosphorylation may underlie foxo regulation by ethanol and p66 in this experimental setting. For instance, NADH accumulation due to ethanol metabolism and to mitochondrial damage may interfere with Foxo deacetylation/activation by sirtuins.39 Further experimental work is required to adequately address the potential connection between p66 and Foxo factors in ethanol-induced cell damage.
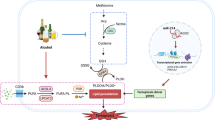
Based on the available information, a tentative pathophysiological cascade linking ethanol and p66 to alcohol-induced liver injury may be outlined as follows. Ethanol metabolism induces p66shc in liver cells (Figures 3a and 4); such induction may be mediated by the p53 tumor suppressor protein, based on our and others’ previous work.16, 21 Whatever the mechanism, increased cell content of p66 can lead to increased ROS generation in mitochondria by two distinct and parallel mechanisms: (1) direct generation of oxygen species by transfer of electrons from cytochrome c to molecular oxygen;19 and (2) inhibition of the mitochondrial scavenger MnSOD, via phosphorylation of a Forkhead transcription factor. (Figure 4a and b). Eventually, mitochondrial oxidative stress would result in organelle damage, fat accumulation in hepatocytes (Figure 2a) and, ultimately, in cell death (1B).
In keeping with the above hypothesized model, we have been able to detect, by means of a novel and sensitive fluorescent protein-based methodology, intracellular oxidation in hepatoma cells challenged with ethanol and exacerbation of oxidative burden by p66 coexpression. (Figure 5a and b). Importantly, oxidative stress in the above conditions is closely paralleled by mitochondrial functional damage (5d).
Notwithstanding these data, and although our findings and current literature suggest that modulation of ethanol toxicity by p66 is mediated by a redox mechanism, ROS-independent effects of p66 could also be operative. For instance, as in our experimental model of ethanol intoxication, a dramatic reduction of steatosis represents the most evident aspect of liver protection by p66 deficiency, a specific role for p66 in fat biosynthesis/storage cannot be excluded. Although protection from oxidative stress is per se sufficient to prevent alcohol-induced steatosis in mice,13 it is worth noting that overexpression of p66 also enhances insulin signaling and promotes adipocyte differentiation of 3T3-L1 cells (Pani et al, manuscript submitted). Therefore, purely metabolic functions of p66 related to lipid metabolism could also contribute to the establishment of liver steatosis in ethanol-fed wild-type mice. With respect to this possibility, preliminary evidence excludes major differences in the liver expression of lipogenic transcription factors PPAR-α4 and -γ between the two mouse strains (data not shown), whereas the potential role of other molecules involved in lipid metabolism and in alcoholic steatosis, such as CREB,40 the SREBP6 and the AMP-activated protein kinase AMPK41 is currently under evaluation.
In conclusion, our data invoke the longevity protein p66shc as a molecular determinant of alcohol cytotoxicity and of liver injury by chronic ethanol intoxication, already at the stage of lipid accumulation (liver steatosis); moreover, the above findings indicate a novel potential molecular mechanism of damage by p66 in the inhibition of mitochondrial antioxidant responses, and in particular of the upregulation of MnSOD. Although mechanistic interactions underlying the above phenomena still need to be clarified, these observations are potentially relevant for the understanding of how p66 regulates general cell response to oxidative challenge, and encourage intense pharmacological research aimed to block the deleterious effect of the p66 protein for the prevention and treatment of alcohol-related and other ROS-dependent diseases.
References
Mendez-Sanchez N, Almeda-Valdes P, Uribe M . Alcoholic liver disease. An update. Ann Hepatol 2005;4:32–42.
Lieber CS . Alcoholic fatty liver: its pathogenesis and mechanism of progression to inflammation and fibrosis. Alcohol 2004;34:9–19.
Mufti SI . Alcohol acts to promote incidence of tumors. Cancer Detect Prev 1992;16:157–162.
Crabb DW, Galli A, Fischer M, et al. Molecular mechanisms of alcoholic fatty liver: role of peroxisome proliferator-activated receptor alpha. Alcohol 2004;34:35–38.
You M, Crabb DW . Molecular mechanisms of alcoholic fatty liver: role of sterol regulatory element-binding proteins. Alcohol 2004;34:39–43.
You M, Fischer M, Deeg MA, et al. Ethanol induces fatty acid synthesis pathways by activation of sterol regulatory element-binding protein (SREBP). J Biol Chem 2002;277:29342–29347.
Hoek JB, Cahill A, Pastorino JG . Alcohol and mitochondria: a dysfunctional relationship. Gastroenterology 2002;122:2049–2063.
Caro AA, Cederbaum AI . Oxidative stress, toxicology, and pharmacology of CYP2E1. Annu Rev Pharmacol Toxicol 2004;44:27–42.
Bailey SM, Cunningham CC . Contribution of mitochondria to oxidative stress associated with alcoholic liver disease. Free Radic Biol Med 2002;32:11–16.
Adachi M, Ishii H . Role of mitochondria in alcoholic liver injury. Free Radic Biol Med 2002;32:487–491.
Koch OR, De Leo ME, Borrello S, et al. Ethanol treatment up-regulates the expression of mitochondrial manganese superoxide dismutase in rat liver. Biochem Biophys Res Commun 1994;201:1356–1365.
Kessova IG, Ho YS, Thung S, et al. Alcohol-induced liver injury in mice lacking Cu, Zn-superoxide dismutase. Hepatology 2003;38:1136–1145.
Wheeler MD, Nakagami M, Bradford BU, et al. Overexpression of manganese superoxide dismutase prevents alcohol-induced liver injury in the rat. J Biol Chem 2001;276:36664–36672.
Perez MJ, Cederbaum AI . Adenovirus-mediated expression of Cu/Zn- or Mn-superoxide dismutase protects against CYP2E1-dependent toxicity. Hepatology 2003;38:1146–1158.
Bai J, Cederbaum AI . Adenovirus-mediated overexpression of catalase in the cytosolic or mitochondrial compartment protects against cytochrome P450 2E1-dependent toxicity in HepG2 cells. J Biol Chem 2001;276:4315–4321.
Pani G, Fusco S, Colavitti R, et al. Abrogation of hepatocyte apoptosis and early appearance of liver dysplasia in ethanol-fed p53-deficient mice. Biochem Biophys Res Commun 2004;325:97–100.
Polyak K, Xia Y, Zweier JL, et al. A model for p53-induced apoptosis. Nature 1997;389:300–305.
Migliaccio E, Giorgio M, Mele S, et al. The p66shc adaptor protein controls oxidative stress response and life span in mammals. Nature 1999;402:309–313.
Giorgio M, Migliaccio E, Orsini F, et al. Electron transfer between cytochrome c and p66Shc generates reactive oxygen species that trigger mitochondrial apoptosis. Cell 2005;122:221–233.
Orsini F, Migliaccio E, Moroni M, et al. The life span determinant p66Shc localizes to mitochondria where it associates with mitochondrial heat shock protein 70 and regulates trans-membrane potential. J Biol Chem 2004;279:25689–25695.
Trinei M, Giorgio M, Cicalese A, et al. A p53-p66Shc signalling pathway controls intracellular redox status, levels of oxidation-damaged DNA and oxidative stress-induced apoptosis. Oncogene 2002;21:3872–3878.
Napoli C, Martin-Padura I, de Nigris F, et al. Deletion of the p66Shc longevity gene reduces systemic and tissue oxidative stress, vascular cell apoptosis, and early atherogenesis in mice fed a high-fat diet. Proc Natl Acad Sci USA 2003;100:2112–2116.
Zaccagnini G, Martelli F, Fasanaro P, et al. p66ShcA modulates tissue response to hindlimb ischemia. Circulation 2004;109:2917–2923.
Koch OR, Galeotti T, Bartoli GM, et al. Alcohol-induced oxidative stress in rat liver. Xenobiotica 1991;21:1077–1084.
Morgan K, French SW, Morgan TR . Production of a cytochrome P450 2E1 transgenic mouse and initial evaluation of alcoholic liver damage. Hepatology 2002;36:122–134.
Bradford BU, Kono H, Isayama F, et al. Cytochrome P450 CYP2E1, but not nicotinamide adenine dinucleotide phosphate oxidase, is required for ethanol-induced oxidative DNA damage in rodent liver. Hepatology 2005;41:336–344.
McKim SE, Gabele E, Isayama F, et al. Inducible nitric oxide synthase is required in alcohol-induced liver injury: studies with knockout mice. Gastroenterology 2003;125:1834–1844.
Kim HP, Roe JH, Chock PB, et al. Transcriptional activation of the human manganese superoxide dismutase gene mediated by tetradecanoylphorbol acetate. J Biol Chem 1999;274:37455–37460.
Kops GJ, Dansen TB, Polderman PE, et al. Forkhead transcription factor FOXO3a protects quiescent cells from oxidative stress. Nature 2002;419:316–321.
Nanji AA, Mendenhall CL, French SW . Beef fat prevents alcoholic liver disease in the rat. Alcohol Clin Exp Res 1989;13:15–19.
Palozza P, Calviello G, Serini S, et al. Supplementation with canthaxanthin affects plasma and tissue distribution of alpha- and gamma-tocopherols in mice. J Nutr 1998;128:1989–1994.
Koch O, Farré S, De Leo ME, et al. Regulation of manganese superoxide dismutase (MnSOD) in chronic experimental alcoholism: effects of vitamin E-supplemented and -deficient diets. Alcohol Alcohol 2000;35:159–163.
Francia P, delli Gatti C, Bachschmid M, et al. Deletion of p66shc gene protects against age-related endothelial dysfunction. Circulation 2004;110:2889–2895.
Nemoto S, Finkel T . Redox regulation of forkhead proteins through a p66shc-dependent signaling pathway. Science 2002;295:2450–2452.
Wu D, Cederbaum AI . Ethanol cytotoxicity to a transfected HepG2 cell line expressing human cytochrome P4502E1. J Biol Chem 1996;271:23914–23919.
Ostergaard H, Henriksen A, Hansen FG, et al. Shedding light on disulfide bond formation: engineering a redox switch in green fluorescent protein. EMBO J 2001;20:5853–5862.
Lieber CS, DeCarli LM, Sorrell MF . Experimental methods of ethanol administration. Hepatology 1989;10:501–510.
Chen Q, Cederbaum AI . Cytotoxicity and apoptosis produced by cytochrome P450 2E1 in Hep G2 cells. Mol Pharmacol 1998;53:638–648.
Brunet A, Sweeney LB, Sturgill JF, et al. Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science 2004;303:2011–2015.
Herzig S, Hedrick S, Morantte I, et al. CREB controls hepatic lipid metabolism through nuclear hormone receptor PPAR-gamma. Nature 2003;426:190–193.
You M, Matsumoto M, Pacold CM, et al. The role of AMP-activated protein kinase in the action of ethanol in the liver. Gastroenterology 2004;127:1798–1808.
Acknowledgements
We thank Professor Piergiuseppe Pelicci and Drs Enrica Migliaccio and Marco Giorgio for providing the p66−/− mouse strain and for critically reading the article; Dr MB Yim (NIH, Bethesda) for the gift of the SODLUC-3340 reporter constructs; Dr A Cederbaum for HepG2-E47 cells transfected with the Cytochrome P450 2E1 cDNA; Dr JR Winther for the rxYFP cDNA; Dr E Stigliano for excellent technical assistance with liver pathology; Drs Silvia Borrello, Ambra Valdannini and Emiliano Panieri for experimental contribution members of the laboratory for helpful discussions and Dr Renata Colavitti for editing the article. This work is supported by grants from Ministero Affari Esteri, Italian–Argentinian collaborative Research Program (L.401/1990) and University of Buenos Aires M042.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koch, O., Fusco, S., Ranieri, S. et al. Role of the life span determinant P66shcA in ethanol-induced liver damage. Lab Invest 88, 750–760 (2008). https://doi.org/10.1038/labinvest.2008.44
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2008.44
Keywords
This article is cited by
-
p66Shc activation promotes increased oxidative phosphorylation and renders CNS cells more vulnerable to amyloid beta toxicity
Scientific Reports (2018)
-
Activation of miR-34a-5p/Sirt1/p66shc pathway contributes to doxorubicin-induced cardiotoxicity
Scientific Reports (2017)
-
Resveratrol Pretreatment Attenuates Concanavalin A-induced Hepatitis through Reverse of Aberration in the Immune Response and Regenerative Capacity in Aged Mice
Scientific Reports (2017)
-
Recombinant adenovirus of human p66Shc inhibits MCF-7 cell proliferation
Scientific Reports (2016)
-
Activation of the SIRT1/p66shc antiapoptosis pathway via carnosic acid-induced inhibition of miR-34a protects rats against nonalcoholic fatty liver disease
Cell Death & Disease (2015)