Abstract
Promoter hypermethylation occurs in various tumors and leads to silencing of tumor-relevant genes. Thus, promoter methylation analysis (MA) has been established as an important tool in cancer research and diagnostics. Here we present MethyQESD (methylation-quantification of endonuclease-resistant DNA) as a fast, easy, precise and reliable method for quantitative MA without the need of bisulfite-treatment or fluorescent probes. Though MethyQESD principally works with any gene promoter we established MethyQESD for the mismatch repair gene MLH1 and tested its utility to differentiate between sporadic microsatellite unstable (MSI-H) colorectal cancer and hereditary nonpolyposis colorectal cancer (HNPCC) by quantitative MLH1 MA. We investigated formalin-fixed and paraffin-embedded tissue samples from a previously published, well-characterized tumor collective comprising 25 HNPCC, 14 sporadic MSI-H CRC and 16 sporadic microsatellite stable (MSS) CRC. We found a high accuracy of MethyQESD by spiking experiments with dilution series of methylated (SW48 cancer cell line) and unmethylated (blood) DNA (Pearson's r=0.9997 (proximal MLH1 promoter region), r=0.9976 (distal MLH1 promoter region)). MethyQESD and conventional quantitative MA using of 96 formalin-fixed and paraffin-embedded CRC showed a high degree of concordance of both methods (Pearson's r=0.885). HNPCC tumors showed either null MLH1 methylation or a significantly lower degree of MLH1 methylation than sporadic MSI-H CRC (P<0.001). MLH1 methylation was negative in all MSS tumors. Receiver operating characteristic (ROC) curve analyses defined a cutoff value of 16.5% MLH1 methylation for specific and sensitive identification of sporadic MSI-H CRC (area under ROC curve: 1.000; asymptotic significance: P<0.001). Thus, quantitative MLH1 MA by MethyQESD provides a simple, fast and valuable tool to identify HNPCC candidates. Furthermore, MethyQESD works reliably with formalin-fixed paraffin-embedded tissue and simplifies DNA MA both for research and diagnostic purposes.
Similar content being viewed by others
Main
Aberrant CpG methylation patterns have been reported to occur frequently in cancer,1, 2 where hypermethylation of regulatory CpG islands can lead to the inactivation of a number of tumor-relevant genes.3, 4 Methylation analysis of defined marker genes is therefore a promising molecular tool with a broad range of application in diagnostics and prediction of response of chemotherapies,5, 6, 7 but none of the current quantitative techniques of DNA methylation analysis (MA) are suited for routine-diagnostic purposes because of their laborious, complicated and time-consuming procedure.
Promoter hypermethylation of the mismatch repair gene MLH1 leads to a high level of microsatellite instability (MSI-H)8, 9 and can be found in approximately 15% of sporadic CRC.10, 11, 12, 13, 14, 15 On the other hand, MSI-H is a hallmark of hereditary nonpolyposis colorectal cancers (HNPCCs)10, 11, 12, 14, 15 and caused by germline mutations rather than by promoter hypermethylation.16, 17 For diagnostic purposes, objective quantitative methods with proven cutoff methylation values are required which are validated in well-defined patient collectives.
Recently, we established a quantitative MA technique for HNPCC diagnostics7 and showed that MLH1 methylation quantification can help to identify HNPCC patients by detection of null or weak MLH1 methylation and to distinguish them from sporadic MSI-H CRC showing virtually constantly high MLH1 methylation levels. Thus, quantitative examination of MLH1 promoter hypermethylation can detect HNPCC candidates who should undergo a MLH1 germline mutation search through DNA sequencing and MLPA analysis.8, 9, 18, 19, 20
Here we present methylation-quantification of endonuclease-resistant DNA (MethyQESD) as a new, robust, fast and easy quantitative MA technique which works reliably with formalin-fixed and paraffin-embedded tissue and is best suited as a molecular tool both in routine diagnostic practice and in cancer research.
MATERIALS AND METHODS
Surgical Specimens and Cell Lines
In a multicentric study 96 formalin-fixed paraffin-embedded tumor samples were obtained from the pathology departments of the University of Regensburg (n=55), the Ludwig-Maximilians-University of Munich (n=29), and the Technical University of Munich (n=12) and analyzed for MLH1 promoter methylation, BRAF V600E mutation analysis and immunohistochemistry (IHC) of MLH1, MSH2 and MSH6 mismatch repair proteins. A reference group of 55 CRC patients were studied according to microsatellite status, BRAF V600E mutation, MLH1 germline mutation and Amsterdam-1 criteria: (1) HNPCC patients (n=25) were defined by (i) positive Amsterdam-1 criteria and/or pathogenic MLH1 germline mutations, (ii) microsatellite instability (MSI-H) and (iii) negative MLH1 IHC (median age: 37.0 years); (2) sporadic MSI-H CRC patients (n=14) were defined by (i) no evidence of fulfilled Amsterdam criteria or MLH1 germline mutations, (ii) BRAF V600E mutation, (iii) age ≥75 years and (iv) negative MLH1 IHC (median age: 80.5 years); (3) sporadic microsatellite stable (MSS) CRC patients (n=16, median age: 76.5) showing MSS and intact expression of the mismatch repair proteins were used as control group.
The human colon cancer cell line SW48 (MLH1 methylation positive) was obtained from ATCC. The cell line was maintained in DMEM with 10% fetal bovine serum at 37°C and 5% CO2.
DNA Isolation
DNA was isolated from blood, archival FFPE tissues and cell lines using the PUREGENE™ DNA Purification Kit (Gentra, Minneapolis, MN, USA) according to the supplier's recommendation. DNA was quantified photometrically.
Microsatellite Analysis
Microsatellite analysis was performed as previously described.21 Briefly, 50–100 ng genomic DNA was used for multiplex microsatellite PCR amplification of the recommended Bethesda standard panel using the HNPCC Microsatellite Instability Test kit (Roche, Mannheim, Germany) according to the manufacturer's instruction. MSI-H was defined by a MSI frequency of >30%22, 23 according to the Bethesda guidelines. Amplified PCR product (1 μl) was applied to the ABI PRISM™ 310 Genetic Analyzer using POP6 polymer. Automatic fragment analysis was performed by GeneScan™ 3.1.2 software (Applied Biosystems, Darmstadt, Germany).
BRAF Mutation Analysis
Mutation analyses of BRAF codon 600 were performed by sequencing exon 15 using an ABI PRISM 3100 Genetic Analyser. Following primers were used for BRAF V600E mutation: BRAF-600 up: 5′-TGTAAAACGACGGCCAGTTCATAATGCTTGCTCTGATAGGA-3′ und BRAF-600 down: 5′-CAGGAAACAGCTATGACCCTTTCTAGTAACTCAGCAGC-3′. Amplifications were carried out according to7, 24 using 0.02 U/μl Taq DNA polymerase (Fermentas, St. Leon-Rot, Germany) and a PCR profile consisting of a 3-min initial denaturation at 94°C followed by 35 cycles of 60 s at 94, 60 and 72°C, respectively. Final extension was performed by a 8-min incubation at 72°C.
Principle of MethyQESD
The MA is based on a combination of methylation-sensitive digestion and real-time PCR. The proportion of methylated DNA, which resists digestion by the methylation-sensitive endonuclease Hin6I is determined by real-time PCR and calibrated using a reference DNA that remains uncut.
Two restiction digestion batches are prepared for each sample, both of them containing equal amounts of DNA: (1) a methylation-quantification digestion (MQD) containing the methylation-sensitive restriction endonuclease Hin6I that cuts only unmethylated CGCG recognition sites, present within the amplicon. (2) A methylation independent calibrator digestion (CalD) with the endonucleases XbaI and DraI whose recognition sites must not be present within the amplicon. The XbaI/DraI as well as the Hin6I digests generates fragmented genomic DNA with increased PCR-accessibility and a higher PCR amplification efficiency. The XbaI/DraI leads to an equal PCR amplification efficiency but does not prevent amplification of the calibrator DNA. The proportion of methylated DNA is determined by subsequent real-time PCR using the MQD and the CalD as templates. In order to investigate methylation of archival paraffinized tissue samples, the size of the amplicon should range between 80 and 150 bp. The difference of the Ct-values give the proportion of methylated DNA according to the formula: methylation (E: PCR efficiency). The principle of MethyQESD is illustrated in Figure 1.
Principle of the MethyQESD. For each sample two digestions are prepared: a methylation-specific quantification digestion with Hin6I and a methylation independent calibrator digestion with methylation independent restriction endonucleases. (a) The restriction endonuclease Hin6I cuts DNA with unmethylated GCGC restriction sites, whereas hypermethylated DNA remain uncut and can be amplified by PCR using primers that flank the Hin6I sites of interest. The methylation independent endonucleases (ie XbaI and DraI) have no restriction sites within the amplicon of the subsequent real-time PCR. The PCR efficiencies of both digestions are equal, as both digestions contain endonuclease treated genomic DNA. (b) The real-time PCR gives the proportion of methylated and therefore uncut DNA species by comparing the amount of amplicable DNA within the quantification digestion with those of the calibrator digestion.
Methylation-Specific Digestion
Two DNA samples each containing 5 μl DNA (1–300 ng/μl) were digested overnight at 37°C in a total volume of 20 μl 1xTango™-Buffer (Fermentas) with 30 U Hin6I and XbaI/DraI (Fermentas; each 15 U), respectively. Subsequently, the endonucleases were inactivated by incubation at 70°C for 20 min and the samples were stored at 4°C.
Methylation-Specific Quantitative Real-Time PCR
The promoter methylation status was determined by relative quantitative real-time PCR using the LightCycler (Roche). Both, the methylation quantification batch and the calibrator DNA were used for PCR in duplicates.
Digested DNA of the MLH1 methylation-positive CRC cell line SW48 served as control for positive methylation, digested DNA of nonmethylated blood DNA was used as a control for 0% methylation.
Real-time PCR was carried out using the QuantiTect SYBR Green I Kit (Qiagen, Hilden, Germany) with 2 μl digested DNA in a total volume of 20 μl, containing 0.5 μM of each primer and 10 μl 1 × QuantiTect™ SYBR Green I Kit. An initial denaturation for 15 min at 95°C was followed by 45 cycles of 95°C for 10 s, 60°C for 17 s and 72°C for 10 s. Melting point analyses were performed by heating the PCR products from 50 to 95°C with an increase of 0.2°C/s while fluorescence was monitored continuously. Primer sequences were (5′ → 3′): MLH1_prox_MS_up CGGCATCTCTGCTCCTATTG; MLH1_prox_MS_down TGCCCGCTACCTAGAAGGAT; MLH1_dist_MS_up 5′-AAGTCGCCCTGAC;GCAGAC; MLH1_dist_MS_down ACTACGAGGCTGAGCACGAA.
The proportion of methylated template was calculated from the differences of the Ct-values from the CalD and MQD (=ΔCt) according to the formula: methylation (E: PCR efficiency).
RESULTS
Restriction Endonuclease Efficiency and Specificity
In order to test the minimum time needed for quantitative digestion of unmethylated DNA we treated 1.3 μg DNA from blood and 1.0 μg DNA from paraffinized normal tissue with Hin6I for different times. After 1 h 99.90% of the blood DNA was completely digested. The restriction efficiency of Hin6I was lower at the DNA from paraffinized tissue, thus complete restriction (0% undigested DNA) was achieved after an incubation time of 16 h (Figure 2). Hin6I has no intrinsic activity on methylated DNA as no degradation of methylated DNA was detectable after incubation with Hin6I for 30 h. We digested our DNA generally overnight (>16 h) to exclude false positive results from undigested, unmethylated DNA.
Quantitative Validation of MethyQESD
The linearity of the MethyQESD MA was tested by two different experiments. In a first experiment dilutions of hypermethylated DNA from the colon cancer cell line SW48 was mixed with unmethylated blood-DNA in a ratio of 1:1, 19:20, 4:5, 1:2, 1:5, 1:20 and 0:1, respectively (corresponding to 100, 95, 80, 50, 20, 5 and 0% methylated DNA). As shown in Figure 3 the methylation quantification analysis mirrored very exactly the ratios of the methylated templates in both the proximal and distal MLH1 promoter regions (Pearson's r=0.9997 (proximal), r=0.9976 (distal)) thereby demonstrating the high accuracy of the MethyQESD method.
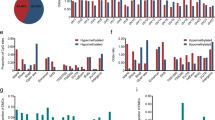
Curves of methylation values showing the methylation detected in percent of a spiking experiment with methylated DNA from SW48 cell line and unmethylated DNA from blood. The detected methylation amounts and the applied methylated DNAs were nearly identical (Pearson's r=0.9997 (proximal), r=0.9976 (distal)).
To prove the reliability of the method using formalin-fixed and paraffin-embedded (FFPE) tissue samples we compared the methylation values of the proximal MLH1 promoter region using MethyQESD and quantitative MA using conventional bisulfite-modified DNA5, 6, 7 of 96 formalin-fixed and paraffin-embedded CRC (Table 1). We found a high concordance of both methods (Pearson's r=0.885).
Technical Sensitivity of the MLH1 MethyQESD
The sensitivity was checked by real-time PCR of Hin6I digested dilutions of defined concentrations of DNA from the hypermethylated cell line SW48. The MLH1 MethyQESD was able to detect 3.2 pg of methylated DNA (Figure 4). The PCR efficiency of the MLH1 MethyQESD PCR was 2.00. For detection of 0% methylation the difference of the Ct values must be at least 7.97 (2−7.97=0.004). Thus, the MQD- and CalD real-time PCR reactions must theoretically contain at least 800 pg DNA each to detect 0% methylation.
In addition, DNA was isolated from 106, 105, 104, 103, 102 and 10 SW48 cells, dissolved in 11 μl water and proceeded according to the QESD protocol. Reproducible results with Ct values below 32 were obtained with DNA isolated from 100 SW48 cells. Thus, for accurate quantification we recommend to use only results with crossing points (Ct values) of 32 or less in the CalD real-time PCR.
Distinction of HNPCC from Sporadic Colorectal Cancers with High Level of Microsatellite Instability by MLH1 MethyQESD
In order to evaluate the MLH1 MethyQESD for HNPCC diagnostics we analyzed the methylation of the regulatory proximal MLH1 promoter region in a published tumor reference group with HNPCC (n=25) tumors, sporadic MSI-H CRC with loss of MLH1-expession (n=14) and sporadic MSS tumors expressing MLH1 (n=16). The overall methylation values ranged from 0 to 55%. None of the 16 MSS CRC showed significant MLH1 promoter methylation values (mean: 0.38%, median: 0.00%, range: 0–3%). All 14 sporadic MSI CRC showed methylation at the (proximal) MLH1 promoter region (mean methylation values: 33.36%, median: 32.50%, range: 21–55%). The MLH1 methylation-positive sporadic MSI-H CRC patients had a mean age of 80.5 years; all of them showed BRAF V600E mutations and none of them fulfilled the Amsterdam criteria or carried MLH1 germline mutations. The median values of MLH1 methylation in HNPCC was 0% (mean: 1.04%, range: 0–13%; two cases with values greater than 2%: 10, 13%). Receiver operating characteristic curve (ROC) analysis revealed an optimal cutoff value of 16.5% methylation of proximal MLH1 promoter region for sporadic MSI patients vs HNPCC cases (area under ROC curve: 1.000; asymptotic significance: P<0.001). Using this methylation cutoff value both specificity and sensitivity of classification of HNPCC and sporadic MSI-H CRC with loss of MLH1 protein expression as well as MSS CRC was 100%, respectively (sensitivity: 25 true HNPCC cases/(25 true HNPCC cases+zero false sporadic case); specificity: 30 true sporadic cases/(30 true sporadic cases+zero false HNPCC case)). The positive predictive value was 100% (25 true HNPCC/(25 true HNPCC+0 false sporadic CRC)) and the negative predictive value was 100% (30 true HNPCC/(30 true HNPCC+zero false sporadic CRC)).
Thus, in most of the HNPCC patients (92%, 23/25) no methylation (ie 0–2% methylation) was detected. However, 8% (2/25) of HNPCC tumors showed low-level methylation (10 and 13%).
The MethyQESD of proximal MLH1 methylation could discriminate between the three tumor groups. A quantile box plot of the median methylation values demonstrates that methylation is significantly different in each tumor group (PKruskal–Wallis<0.001; Figure 5). Sporadic MSI-H CRC showed strong MLH1 promoter methylation (≥21%), whereas HNPCC tumors do not show methylation at all or only low values (up to 13% at most). MSS sporadic tumors which were used as controls are consistently MLH1 methylation negative.
Comparison of MLH1 promoter methylation in tumors from HNPCC, sporadic MSI-H CRC and sporadic MSS CRC. The box for each tumor group represents the interquartile range (25–75th percentile), the line within each box shows the median value. Bottom and top bars of the whisker indicate the 10th and 90th percentiles, respectively. Outlier values are indicated (asterisks). The non-parametric Kruskal–Wallis test was used to examine differences between the three independent tumor groups (HNPCC, sporadic MSI-H tumors, sporadic MSS tumors). The Mann–Whitney –U-test was used in case of two tumor groups. P=P-value. Statistical analysis was performed using the SPSS13 software.
DISCUSSION
The aim of this study was to establish an easy, fast and robust quantitative MA as a molecular tool in research and diagnostics. Generally, several difficulties can complicate methylation analyses. Stromal and inflammatory lymphocytes within tumor tissues can have other methylation patterns than the tumor and may cause false results if nonquantitative MA techniques like simple methylation-specific PCR (MSP) are applied. Moreover, nonquantitative methylation detection techniques principally cannot distinguish between low grade, partial or monoallelic and biallelic methylation.
Beside MSP, other quantitative methylation analyses25, 26 usually require a time consuming bisulfite modification step which generates unstable modified DNA impairing the speed and reproducibility of analyses. In addition the design of primers or fluorescent probes for the degenerated sequence of bisulfite-modified DNA can be difficult or even impossible for certain promoter regions. Methylation detection by pyrosequencing is a powerful technique, but it includes also a bisulfite modification step and requires a costly technical equipment.
These drawbacks could be overcome by the MethyQESD technique which is highly reproducible, easy and sensitive as it uses stable genomic DNA and quantification based on SYBR Green real-time PCR. The high sensitivity of SYBR Green real-time PCR ensures quantification even of very small amounts of DNA, eg DNA from fine-needle biopsies. We show here that only few nanograms of DNA from as little as 100 cells are sufficient for a MA. However, for routine analysis of formalin-fixed paraffin-embedded tumor tissue we recommend to use 50–100 ng for DNA restriction and to take a 10th aliquot (ie 5–10 ng) of digested DNA for quantitative PCR. As higher Ct-values are accompanied with an increased standard deviation, we recommend the use of DNA triplicates in the real-time PCR reactions containing less than 2 ng DNA. The small size of the amplicons (80–150 bp) ensures reproducible results from fragmented DNA extracted from formalin-fixed and paraffin-embedded tissue samples. This analytical robustness makes MethyQESD best suited for retrospective studies of archival material.
A main advantage of MethyQESD is that no bisulfite modification step is required. Furthermore, the parallel use of a quantification and a calibrator batch of each DNA sample provides a self-calibrating real-time PCR with equal PCR efficiencies. This avoids the need of standard curves as well as the adjustment of DNA concentration. Furthermore, the digested DNA samples can be used for further MethyQESD MA of other genes than MLH1.
As PCR efficiency is enhanced by fragmentation of genomic DNA by endonucleases cutting outside the amplicon (data not shown) undigested DNA should not be used for creating a standard curve to avoid an overestimation of methylation. This issue is unfortunately not considered in another quantitative methylation detection methods.27
The accuracy of our technique was proven in two different ways. First, we performed spiking experiments of methylated and unmethylated template DNA from a colorectal cancer cell line and blood, respectively (Figure 3), and found a high accuracy (Pearson's r=0.9997 (proximal MLH1 promoter region), r=0.9976 (distal MLH1 promoter region)). Second, in order to evaluate MethyQESD with routine formalin-fixed and paraffin-embedded tissue samples, we compared the methylation values of the proximal MLH1 promoter region generated with MethyQESD and another quantitative MA using conventional bisulfite-modified DNA7 of 96 formalin-fixed and paraffin-embedded CRC (Table 1). Both methods showed again a high concordance (Pearson's r=0.885).
False positive signals from undigested unmethylated DNA can be excluded, as amounts of 1.5 μg DNA from blood are completely digested by Hin6I within 2 h. As Hin6I has no intrinsic activity on methylated restriction sites we digested the DNA overnight, although MethyQESD produces reliable results already within less than 5 h (3 h digestion, 1 h real-time PCR, approximately 20 min hands-on time).
We have established MethyQESD for MLH1 MA as a molecular tool in HNPCC diagnostics as it has been shown that a strong MLH1 methylation occurs in sporadic MSI CRC whereas no or only low levels of MLH1 methylation are present in HNPCC patients.7 The quantification of MLH1 methylation by MethyQESD allows the distinction between low level methylation due to, eg partial or monoallelic methylation or epigenetic germline defects in HNPCC28 and biallelic methylation. Thus, MethyQESD significantly improves the accuracy of HNPCC diagnostics as also HNPCC cases with low level of MLH1 methylation can be detected which were otherwise falsely assigned to sporadic MSI CRC.
The lowest value within the group of sporadic MSI-H tumors was 21% (Figure 5) and the highest value in HNPCC tumors was 13%. A cutoff value of 16.5% was calculated by a ROC curve analysis. False positive methylation results could be excluded as no positive methylation was detected at any MLH1 expressing MSS CRC. Interestingly, two HNPCC patients (62 and 63 years old, respectively) with pathogenic MLH1 germline mutations and loss of MLH1 expression showed weak DNA MLH1 methylation (10 and 13%, respectively). We assume that these cases carry monoallelic MLH1 promoter methylation, ie one allele is silenced by methylation, whereas the other allele carries the MLH1 germline mutation. Unfortunately, we were not able to discriminate between maternal and paternal alleles to verify monoallelic methylation by cloning and sequence analysis as there was no sequence polymorphism within the promoter regions.
Although MLH1 MA by MethyQESD is not a stand-alone test in HNPCC diagnostics, MethyQESD is a valuable tool to identify HNPCC candidates for further analysis like mutation analysis of MMR genes. In addition to MLH1 methylation, a BRAF V600E mutation has been reported to occur specifically in about 70% of sporadic MSI-H CRC.29, 30 Although the detection of a BRAF V600E mutation may exclude HNPCC, wild-type BRAF V600 can occur in both sporadic CRC and HNPCC making a BRAF V600 wild-type result meaningless. However, for best diagnostic results we recommend to perform both MLH1 MethyQESD and BRAF V600E analysis in all CRC with MSI-H and lack of MLH1 protein expression. Patients without significant MLH1 methylation and with wild-type BRAF V600 represent HNPCC candidates who should further clarified by genetic counseling and who might benefit from a tight surveillance program.
In summary, MethyQESD is a robust, fast, reliable and easy-to-handle method for quantitative MA. MethyQESD avoids a bisulfite modification step and can readily be established also for MA of other genes as we have performed it already for MGMT, P16, GSTP1, RASSF1, SFRP1, PITX2, CA4, NEUROG1, CDH3 and APC. As MethyQESD works reliably with formalin-fixed and paraffin-embedded tissue MethyQESD is ideally suited for quantitative methylation analyses both in diagnostic purposes and for research studies using archival tissues.
References
Jones PA, Baylin SB . The fundamental role of epigenetic events in cancer. Nat Rev Genet 2002;3:415–428.
Plass C . Cancer epigenomics. Hum Mol Genet 2002;11:2479–2488.
Dobrovic A, Simpfendorfer D . Methylation of the BRCA1 gene in sporadic breast cancer. Cancer Res 1997;57:3347–3350.
Greger V, Debus N, Lohmann D, et al. Frequency and parental origin of hypermethylated RB1 alleles in retinoblastoma. Hum Genet 1994;94:491–496.
Woodson K, O’Reilly KJ, Hanson JC, et al. The usefulness of the detection of GSTP1 methylation in urine as a biomarker in the diagnosis of prostate cancer. J Urol 2008;179:508–511.
Matsubara N . Diagnostic application of hMLH1 methylation in hereditary non-polyposis colorectal cancer. Dis Markers 2004;20:277–282.
Bettstetter M, Dechant S, Ruemmele P, et al. Distinction of hereditary nonpolyposis colorectal cancer and sporadic microsatellite-unstable colorectal cancer through quantification of MLH1 methylation by real-time PCR. Clin Cancer Res 2007;13:3221–3228.
Raedle J, Trojan J, Brieger A, et al. Bethesda guidelines: relation to microsatellite instability and MLH1 promoter methylation in patients with colorectal cancer. Ann Intern Med 2001;135 (8 Part 1):566–576.
Cunningham JM, Christensen ER, Tester DJ, et al. Hypermethylation of the hMLH1 promoter in colon cancer with microsatellite instability. Cancer Res 1998;58:3455–3460.
Peltomaki P, de la Chapelle A . Mutations predisposing to hereditary nonpolyposis colorectal cancer. Adv Cancer Res 1997;71:93–119.
Ionov Y, Peinado MA, Malkhosyan S, et al. Ubiquitous somatic mutations in simple repeated sequences reveal a new mechanism for colonic carcinogenesis. Nature 1993;363:558–561.
Aaltonen LA, Peltomaki P, Mecklin JP, et al. Replication errors in benign and malignant tumors from hereditary nonpolyposis colorectal cancer patients. Cancer Res 1994;54:1645–1648.
Jass JR, Do KA, Simms LA, et al. Morphology of sporadic colorectal cancer with DNA replication errors. Gut 1998;42:673–679.
Liu B, Parsons R, Papadopoulos N, et al. Analysis of mismatch repair genes in hereditary non-polyposis colorectal cancer patients. Nat Med 1996;2:169–174.
Basik M, Stoler DL, Kontzoglou KC, et al. Genomic instability in sporadic colorectal cancer quantitated by inter-simple sequence repeat PCR analysis. Genes Chromosomes Cancer 1997;18:19–29.
Liu B, Nicolaides NC, Markowitz S, et al. Mismatch repair gene defects in sporadic colorectal cancers with microsatellite instability. Nat Genet 1995;9:48–55.
Herman JG, Umar A, Polyak K, et al. Incidence and functional consequences of hMLH1 promoter hypermethylation in colorectal carcinoma. Proc Natl Acad Sci USA 1998;95:6870–6875.
Kane MF, Loda M, Gaida GM, et al. Methylation of the hMLH1 promoter correlates with lack of expression of hMLH1 in sporadic colon tumors and mismatch repair-defective human tumor cell lines. Cancer Res 1997;57:808–811.
Kuismanen SA, Holmberg MT, Salovaara R, et al. Genetic and epigenetic modification of MLH1 accounts for a major share of microsatellite-unstable colorectal cancers. Am J Pathol 2000;156:1773–1779.
Taylor CF, Charlton RS, Burn J, et al. Genomic deletions in MSH2 or MLH1 are a frequent cause of hereditary non-polyposis colorectal cancer: identification of novel and recurrent deletions by MLPA. Hum Mutat 2003;22:428–433.
Dietmaier W, Bettstetter M, Wild PJ, et al. Nuclear Maspin expression is associated with response to adjuvant 5-fluorouracil based chemotherapy in patients with stage III colon cancer. Int J Cancer 2006;118:2247–2254.
Dietmaier W, Wallinger S, Bocker T, et al. Diagnostic microsatellite instability: definition and correlation with mismatch repair protein expression. Cancer Res 1997;57:4749–4756.
Boland CR, Thibodeau SN, Hamilton SR, et al. A National Cancer Institute Workshop on Microsatellite Instability for cancer detection and familial predisposition: development of international criteria for the determination of microsatellite instability in colorectal cancer. Cancer Res 1998;58:5248–5257.
Samowitz WS, Sweeney C, Herrick J, et al. Poor survival associated with the BRAF V600E mutation in microsatellite-stable colon cancers. Cancer Res 2005;65:6063–6069.
Rand K, Qu W, Ho T, et al. Conversion-specific detection of DNA methylation using real-time polymerase chain reaction (ConLight-MSP) to avoid false positives. Methods 2002;27:114–120.
Colella S, Shen L, Baggerly KA, et al. Sensitive and quantitative universal pyrosequencing methylation analysis of CpG sites. Biotechniques 2003;35:146–150.
Bastian PJ, Palapattu GS, Lin X, et al. Preoperative serum DNA GSTP1 CpG island hypermethylation and the risk of early prostate-specific antigen recurrence following radical prostatectomy. Clin Cancer Res 2005;11:4037–4043.
Hitchins M, Williams R, Cheong K, et al. MLH1 germline epimutations as a factor in hereditary nonpolyposis colorectal cancer. Gastroenterology 2005;129:1392–1399.
Domingo E, Niessen RC, Oliveira C, et al. BRAF-V600E is not involved in the colorectal tumorigenesis of HNPCC in patients with functional MLH1 and MSH2 genes. Oncogene 2005;24:3995–3998.
Domingo E, Laiho P, Ollikainen M, et al. BRAF screening as a low-cost effective strategy for simplifying HNPCC genetic testing. J Med Genet 2004;41:664–668.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bettstetter, M., Dechant, S., Ruemmele, P. et al. MethyQESD, a robust and fast method for quantitative methylation analyses in HNPCC diagnostics using formalin-fixed and paraffin-embedded tissue samples. Lab Invest 88, 1367–1375 (2008). https://doi.org/10.1038/labinvest.2008.100
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2008.100
Keywords
This article is cited by
-
Differentially methylation of IFI44L gene promoter in Iranian patients with systemic lupus erythematosus and rheumatoid arthritis
Molecular Biology Reports (2022)
-
Modern day screening for Lynch syndrome in endometrial cancer: the KEM experience
Archives of Gynecology and Obstetrics (2021)
-
Enhanced Tumoral MLH1-Expression in MLH1-/PMS2-Deficient Colon Cancer Is Indicative of Sporadic Colon Cancer and Not HNPCC
Pathology & Oncology Research (2020)
-
Erblicher Darmkrebs bei Lynch‑/HNPCC-Syndrom in Deutschland
Der Pathologe (2019)
-
Colorectal mixed adenoneuroendocrine carcinomas and neuroendocrine carcinomas are genetically closely related to colorectal adenocarcinomas
Modern Pathology (2017)