- TECHNOLOGY FEATURE
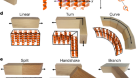
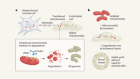
Matrix mimics shape cell studies
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 566, 563-565 (2019)
doi: https://doi.org/10.1038/d41586-019-00681-1
References
Safaee, H. et al. Cell. Mol. Bioeng. 10, 501–513 (2017).
Bissell, M. J., Hall, H. G. & Parry, G. J. Theor. Biol. 99, 31–68 (1982).
Crapo, P. M., Tottey, S., Slivka, P. F. & Badylak, S. F. Tissue Eng. A 20, 313–323 (2014).
Trappmann, B. et al. Nature Commun. 8, 371 (2017).
Davoudi, S. et al. Biomaterials 173, 34–46 (2018).
Damaraju, S. M. et al. Biomaterials 149, 51–62 (2017).
Nih, L. R., Gojgini, S., Carmichael, S. T. & Segura, T. Nature Mater. 17, 642–651 (2018).
Shin, D. S. et al. ACS Biomater. Sci. Eng. 4, 378–387 (2018).

 NatureTech
NatureTech
 Make better, safer biomaterials
Make better, safer biomaterials
 Stem-cell culture moves to the third dimension
Stem-cell culture moves to the third dimension