Abstract
Objectives:
Lithium has recently been found to enhance neuronal regeneration and differentiation. This arouses its potential use to treat spinal cord injury patients. The safety and pharmacokinetics of lithium are not verified for this group of patients as their internal organ functions may change. This is a phase 1 clinical trial to evaluate the safety and pharmacokinetics of lithium in spinal cord injury patients.
Methods:
A total of 20 chronic spinal cord injury subjects were recruited. Oral lithium carbonate was given in divided dose to maintain the serum lithium level 0.6–1.2 mmol l−1 for 6 weeks. Safety parameters, adverse events and pharmacokinetic data were carefully collected and monitored.
Results:
No severe adverse event was documented. All blood parameters remained stable. Nausea and vomiting were the most common complaints but tolerance was improved in 2 weeks for most subjects. A wide range of oral doses was required to maintain serum lithium level at the targeted range. However, the dose for individual subject was relatively constant.
Conclusion:
This phase 1 clinical trial is the first report indicating the safety of lithium in chronic spinal cord injury patients. It is well tolerated after the first 2 weeks. Individual titration of lithium is essential to maintain an optimal serum lithium level but once the desirable level is achieved, the oral dose remains relatively unchanged for maintenance.
Similar content being viewed by others
Introduction
Lithium attracted much attention as a potential neuroregenerative agent in 2004 when Yick et al.1 reported that lithium reinforces regeneration-promoting effect of the enzyme, chondroitinase ABC, on rat rubrospinal neurons. A recent study by Su et al.2 revealed the enhancing effect of lithium on proliferation and neuronal differentiation of neural progenitor cells in the adult rat spinal cord. At the same time, it reduces microglia and macrophage activation and thus immune response of host. Fornai and co-workers3, 4 reported that daily doses of oral lithium carbonate achieving 0.4–0.8 mmol l−1 plasma levels, not only remarkably prevented death of 22 patients with amyotrophic lateral sclerosis but also resulted in minimal motor deterioration over 15 months, compared to 29% mortality and significant motor deterioration in 22 patients who did not receive lithium. If confirmed, this would be the first therapy that prevents mortality rate and neurological deteriorations in patients with amyotrophic lateral sclerosis.
The safety and pharmacokinetics of lithium in the spinal cord injury patients remain unknown. The renal, endocrinal and metabolic functions of the spinal cord injury patients may differ from the normal population. Lithium may increase neuropathic pain, spasticity and other symptoms of spinal cord injury. The current phase 1 clinical trial was designed to determine the feasibility and safety of oral lithium carbonate treatment associated with the therapeutic level of lithium (0.6–1.2 mmol l−1). The goal is to obtain sufficient safety and pharmocokinetic information to permit the design of phase 2 spinal cord regeneration studies that combine lithium with other treatment regimens.
Materials and methods
A total of 20 eligible patients were recruited from MacLehose Medical Rehabilitation Centre, Hong Kong in 2007. The study was sponsored by the China Spinal Cord Injury Network Company, Ltd and approved by the local research ethics committee. The investigation was conducted in accordance with the Declaration of Helsinki Principles and International Conference on Harmonization Guidelines for Good Clinical Practice. All patients gave written informed consent before their enrollment.
Patient recruitment
Patients, 18- to 60-years old, classified as American Spinal Injury Association Impairment Scale (2000 standards) A–C due to spinal cord injury more than 12 months ago were eligible. Exclusion criteria included hypersensitivity to lithium; significant renal, cardiovascular, hepatic or psychiatric diseases; associated severe brain injury; concomitant intake of drugs interacting with lithium; history of alcohol or drug abuse; pregnant or lactating women and women reluctant for effective contraception.
Study design and drug administration
Each eligible subject received lithium carbonate in a daily dosage of 500 mg initially. Dosage was titrated upward by an additional tablet of 250 mg in steps to achieve and maintain a plasma lithium concentration within the range 0.6–1.2 mmol l−1. The subjects visited the clinic at screening (week −4), baseline (day 0), day 3 and at week 1, 6 and 12 for assessments and serum lithium examination.
Dose modification
Dosing of lithium was determined and adjusted according to plasma lithium level concentrations. At 72 h (day 3) after the initial oral intake of lithium, blood was sampled for lithium levels. If the plasma lithium concentration had reached the minimum level of 0.6 mmol l−1, no adjustment of dosage was required.
If the initial plasma lithium at day 3 did not reach the minimum level, an additional 250 mg tablet was added. Blood was sampled for lithium levels at week 1. If the minimum level 0.6 mmol l−1 was still not achieved, a further additional tablet was added and blood was sampled again at 72 h. This was repeated until the criterion of 0.6–1.2 mmol l−1 was reached. All serum lithium samples were drawn 12±1 h after the last dose. Thus, the steady-state trough level was being used for the adjustment of the oral lithium dosage.
If the lithium levels exceeded the maximum level 1.2 mmol l−1 but below 1.5 mmol l−1 without any presenting symptoms of intoxication at day 3, the dosage was reduced by one unit, that is, 250 mg. Blood was sampled for lithium level at week 1. If the therapeutic range 0.6–1.2 mmol l−1 was reached, no further readjustment of drug dosage was required and the subject was maintained at that dosage level for the rest of the 6-week treatment period.
Outcome measures
All patients were monitored for adverse events (AEs). Clinical assessment included side effects of lithium, body weight, vital signs (temperature, pulses, respiratory rates, blood pressures in the sitting position), visual analog scale for any pain all over the body, Ashworth scale of limbs and American Spinal Injury Association scoring. Scheduled blood tests were carried out to monitor the renal, liver, thyroid and parathyroid functions. In addition, full blood count, clotting profile, serum glucose level and urinalysis were performed to document any other possible AEs. Electrocardiography was used to monitor cardiac status.
Pharmacokinetic sampling and assay
Lithium levels were assessed at visit 1 (screening), visit 2a (before the administration of lithium), visit 2b (72 h after initial dosage), visit 3 (1 week after the initial dosage or after the dose increment), visit 3b, 3c… (72 h after adjustment of each lithium dose), visit 4 (12 h after the last dose) and visit 5 (6 weeks after stopping lithium). Drug compliance was estimated by comparing the expected and observed consumption of lithium carbonate. The algorithm was as follows:

Observed consumption was equal to the total number of tablets dispensed minus the total number of tablets returned. Expected consumption referred to the expected daily dosage times the corresponding number of treatment days.
Statistical methods
All statistical tests were two-tailed, at the 0.05 significance level; and all P-values were rounded up to three decimal places. The analyses were conducted using the Statistical Analysis System (SAS version 9.1; SAS Institute Inc., Cary, NC, USA). The full analysis set was carried out based on the intention-to-treat principle. Therefore, all subjects with protocol violations or those withdrawing from the study prematurely were included. Any subject who received at least one dose of lithium carbonate was included in the data analysis.
Results
Safety
We recorded 95 AEs during the treatment period, and only 2 of them (2.1%) were preexisting conditions. A total of 58 AEs (61.1%) were known side effects of lithium carbonate and 37 AEs (38.9%) were unexpected. Most of the reported AEs (95.8%) were recovered before the end of study period. Four AEs (4.2%) that persisted after the end of the study were laxer muscle tone, easier bowel motion, abnormal T-wave inversion of the electrocardiography and sacral pressure sore. The first two AEs were considered to be beneficial by the patients. The patient with T-wave inversion did not have any symptom and the cardiac enzymes were normal. The patient with sacral bedsore had history of recurrent bedsores.
A quarter of AEs occurred during the first 3 days of medication and 90% of the AEs occurred while oral lithium was being adjusted to reach the therapeutic levels 0.6–1.2 mmol l−1. A total of seven subjects stopped treatment prematurely. With an exception of subject 11 who quit at day 23, all other subjects quit the study during the initial 2 weeks because of the AEs. Three subjects withdrew because of gastrointestinal symptoms such as nausea and vomiting. Other reasons included increase in bowel movement, headache and hand tremor, shortness of breath and increasing ‘dullness’.
Vital signs of all patients were stable throughout the study period. Physical examination did not reveal any remarkable change although two subjects (nos. 003 and 004) complained of puffiness of face. Their body weight remained the same compared to the baseline levels. No significant change was found for pain visual analogue scale, modified Ashworth Scale and American Spinal Injury Association Impairment Scale. Pressure ulcers were found in four subjects, but three of them had the ulcers before the study. One subject (no. 016) developed a grade 4 sacral pressure ulcer at the final visit. He had history of recurrent pressure sores.
None of the subjects showed significant changes of hematological and biochemical parameters (Table 1). Subject 005 was found to have hyperglycemia at screening but because this was not an exclusion criterion, the subject was recruited into the study. No thyroid or parathyroid dysfunction was reported. One subject had prolonged PR interval of electrocardiography at visit 4 and 5. Another subject developed a T-inversion. Both of them were asymptomatic and cardiac enzymes were normal. Therefore, these electrocardiographic changes were considered to be clinically insignificant.
Pharmacokinetics
Eighteen subjects reached blood lithium levels of at least 0.6 mmol l−1 (Figure 1) during the treatment period. A daily dose of 500 mg was not sufficient to achieve the therapeutic level in any of the subjects. Individual daily requirement of oral lithium varied widely from 750 to 1750 mg. Two subjects quit the study before serum level of 0.6 mmol l−1 due to AEs. At the final follow-up, lithium level of all subjects was below 0.2 mmol l−1.
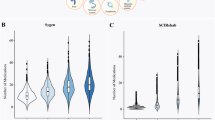
The mean serum lithium associated with the administration of various doses of lithium carbonate is shown in Figure 2. The serum lithium level rose steadily and smoothly with every tablet increment. No abrupt variation of drug level was noted. The range of serum lithium did not increase with higher oral doses. In fact, the range of serum level is wider at 750 and 1000 mg compared with 1250 and 1500 mg (Figure 3). The box plot did not show significant up or down skewing and the means were close to the medians. This implied that the serum lithium level distribution was a nearly normal distribution at a particular dose. There were few exceptionally high or low levels. These make adjustment of the individual dose relatively easier.
Compliance
Eighteen subjects had drug compliance over 90% whereas the compliance of the remaining two subjects was 80.8 and 88%, respectively. Fatigue and gastrointestinal upset were the most common reasons given for noncompliance. Compliance improved with time and the side effects were finally well tolerated once a steady oral dose was being taken. Although 7 of the 20 subjects discontinued treatment due to perceived side effects, none of these subjects even reached the therapeutic range of 0.6–1.2 mmol l−1 when they began experiencing their symptoms. Finally, once optimal plasma level was reached at a particular dose and the dose was maintained, the plasma levels remained quite consistently close to what they were at the beginning of the maintenance phase. There was no significant statistical difference between the serum lithium levels at visits 3 and 4.
Discussion
Although 95 AEs were recorded, a vast majority of these were mild and did not manifest in any signs of organic abnormalities. None required therapeutic or corrective actions other than stopping the lithium treatment when requested by the subject. Most (59%) of the AEs were intermittent, moderate or mild intensity (78%), temporarily related to the lithium treatment (86%), required no action (81%) and disappeared when lithium was discontinued.
Lithium appears to be well tolerated by a majority of cases. Some subjects reported mild side effects such as gastrointestinal tract upset, sleepiness or dizziness at the initial phase of oral lithium intake even though the serum level was at or below the therapeutic level. Most complaints disappeared after a short while. More severe side effects causing organ dysfunction were not seen. Most of the AEs occurred during the titration phase and before plasma lithium levels reached therapeutic levels. Nausea and gastrointestinal upset appear to be the most common AEs associated with initial lithium use.5 The symptoms of upset stomach and nausea decreased with time and no cumulative or additional symptoms occurred during the treatment period. Transitory subjective complaints do not require termination of treatment.6
Seven subjects dropped out during the study. Most were during the initial phase of lithium titration. Because the side effects usually appeared at the beginning before serum lithium levels were therapeutic and almost all of the subjects had less symptoms with time, it is likely that the dropout rate would have been less if the patients were better reassured. Of the 13 patients who completed the 6-week course, most of them reported similar side effects but in general they tolerated lithium carbonate better with time.
Lithium is mainly excreted by the kidneys and spinal cord injury patients are prone to have coexisting renal impairment. Therefore renal function monitoring is important. In addition, long-term lithium treatment itself can cause nephropathy.7 Careful monitoring of the renal function throughout the study period did not reveal any renal toxic effect. No patient complained of or found to have polyuria, electrode disturbance, albuminuria or impaired renal function test.
We were concerned that lithium may increase neuropathic pain or spasticity. Our data indicate that lithium does not increase either. We were also concerned with the effect of lithium on thyroid, parathyroid and other hormonal functions. Lithium suppresses thyroid function and is associated with goiter. The incidence was reported to be 7.4/1000.8 Another study by Carle et al.9 reported 1.6% of hypothyroidism in the Danes due to lithium use. Lithium-induced hyperparathyroidism is relatively rare10 and may be associated with hypercalcemia and delirium. Our data indicate that lithium has no effect on T3 or T4 levels, parathyroid hormone levels or blood chemistry in chronic spinal cord injury subjects. Thus, subsequent clinical trials require less frequent monitoring of these parameters. However, close scrutiny remains essential in acute cases due to the potential pharmacokinetic difference of lithium.
None of the patients in this study reached therapeutic plasma levels with 250 mg twice per day. Several reached therapeutic levels >0.6 mm with 250 mg three times per day. However, several patients needed daily dose of as high as 1750 mg to reach and stay in therapeutic range. We therefore recommend starting the titration with 750 mg per day in three divided dose, that is, 250 mg three times per day and going up from there in 250 mg increment.
Transient overdosing defined as plasma levels exceeding 1.2 mmol l−1 was found in five subjects. The serum lithium level returned promptly to therapeutic level after reducing the oral lithium intake. No patient had clinical signs or symptoms of lithium overdose. Only about half of the plasma lithium reaches the central nervous system.11, 12, 13 Oral route causes gastrointestinal side effects. Intrathecal administration may minimize the side effects and improve the efficacy of lithium treatment in spinal cord injury patients. Conversely, our study indicates that people with chronic spinal cord injury tolerated the drug well and there was no objective evidence of organ dysfunction associated with the serum lithium levels, 0.6–1.2 mmol l−1.
In conclusion, much evidence suggests neuroprotective and neuroregenerative properties of lithium. It increases neuronal markers and gray matter in brain and at least one preclinical study suggests that lithium can enhance axonal growth in spinal cord in combination with other chondroitinase. This phase 1 clinical trial indicates the safety of lithium in chronic spinal cord injury subjects, although its safety in acute cases needs further study. Although there were an unexpected number of voluntary dropouts from the study during the first 2 weeks of initiating lithium treatment, the results indicate that the drug is well tolerated after the first 2 weeks. This study is preliminary to a double-blind placebo-controlled trial of lithium versus placebo treatment of spinal cord injury.
References
Yick LW, So KF, Cheung PT, Wu WT . Lithium chloride reinforces the regeneration-promoting effect of chondroitinase ABC on rubrospinal neurons after spinal cord injury. J Neurotrauma 2004; 21: 932–943.
Su H, Chu TH, Wu W . Lithium enhances proliferation and neuronal differentiation of neural progenitor cells in vitro and after transplantation into the adult rat spinal cord. Exp Neurol 2007; 206: 296–307.
Fornai F, Longone P, Ferrucci M, Lenzi P, Isidoro C, Ruggieri S et al. Autophagy and amyotrophic lateral sclerosis: the multiple roles of lithium. Autophagy 2008; 4: 527–530.
Watase K, Gatchel JR, Sun Y, Emamian E, Atkinson R, Richman R et al. Lithium therapy improves neurological function and hippocampal dendritic arborization in a spinocerebellar ataxia type 1 mouse model. PLoS Med 2007; 4: e182.
Li H, Ma C, Wang G, Zhu X, Peng M, Gu N . Response and remission rates in Chinese patients with bipolar mania treated for 4 weeks with either quetiapine or lithium: a randomized and double-blind study. Curr Med Res Opin 2008; 24: 1–10.
Muller D, Kruger E . Side-effects of lithium therapy. Psychiatr Neurol Med Psychol (Leipz) 1975; 27: 172–180.
Presne C, Fakhouri F, Noel LH, Stengel B, Even C, Kreis H et al. Lithium-induced nephropathy: rate of progression and prognostic factors. Kidney Int 2003; 64: 585–592.
Kirov G, Tredget J, John R, Owen MJ, Lazarus JH . A cross-sectional and a prospective study of thyroid disorders in lithium-treated patients. J Affect Disord 2005; 87: 313–317.
Carle A, Laurberg P, Pedersen IB, Knudsen N, Perrild H, Ovesen L et al. Epidemiology of subtypes of hypothyroidism in Denmark. Eur J Endocrinol 2006; 154: 21–28.
Carchman E, Ogilvie J, Holst J, Yim J, Carty S . Appropriate surgical treatment of lithium-associated hyperparathyroidism. World J Surg 2008; 32: 2195–2199.
Terhaag B, Scherber A, Schaps P, Winkler H . The distribution of lithium into cerebrospinal fluid, brain tissue and bile in man. Int J Clin Pharmacol Biopharm 1978; 16: 333–335.
Kato T, Shioiri T, Inubushi T, Takahashi S . Brain lithium concentrations measured with lithium-7 magnetic resonance spectroscopy in patients with affective disorders: relationship to erythrocyte and serum concentrations. Biol Psychiatry 1993; 33: 147–152.
Plenge P, Stensgaard A, Jensen HV, Thomsen C, Mellerup ET, Henriksen O . 24-hour lithium concentration in human brain studied by Li-7 magnetic resonance spectroscopy. Biol Psychiatry 1994; 36: 511–516.
Acknowledgements
We thank Ms Fanny SH Ip (coordinator of the study), Professor Johan PE Karlberg, Mr Vincent HK Ng (occupational therapist), Ms Anita Wong and Mr Admond FY Wong (physiotherapist) for significant contributions to this phase 1 clinical study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wong, Y., Tam, S., So, K. et al. A three-month, open-label, single-arm trial evaluating the safety and pharmacokinetics of oral lithium in patients with chronic spinal cord injury. Spinal Cord 49, 94–98 (2011). https://doi.org/10.1038/sc.2010.69
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2010.69
Keywords
This article is cited by
-
Research Progress of Antioxidants in Oxidative Stress Therapy after Spinal Cord Injury
Neurochemical Research (2023)
-
Lithium Chloride Facilitates Autophagy Following Spinal Cord Injury via ERK-dependent Pathway
Neurotoxicity Research (2017)
-
New strategies for the repair of spinal cord injury
Chinese Science Bulletin (2014)
-
Efficacy and safety of lithium carbonate treatment of chronic spinal cord injuries: a double-blind, randomized, placebo-controlled clinical trial
Spinal Cord (2012)