Abstract
Introduction:
Cholelithiasis is increasingly encountered in childhood and adolescence due to the rise in obesity. As in adults, weight loss is presumed to be an important risk factor for cholelithiasis in children, but this has not been studied.
Methods:
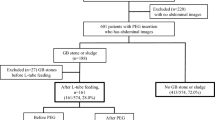
In a prospective observational cohort study we evaluated the presence of gallstones in 288 severely obese children and adolescents (mean age 14.1±2.4 years, body mass index (BMI) z-score 3.39±0.37) before and after participating in a 6-month lifestyle intervention program.
Results:
During the lifestyle intervention, 17/288 children (5.9%) developed gallstones. Gallstones were only observed in those losing >10% of initial body weight and the prevalence was highest in those losing >25% of weight. In multivariate analysis change in BMI z-score (odds ratio (OR) 3.26 (per 0.5 s.d. decrease); 95% CI:1.60–6.65) and baseline BMI z-score (OR 2.32 (per 0.5 s.d.); 95% CI: 1.16–4.70) were independently correlated with the development of gallstones. Sex, family history, OAC use, puberty and biochemistry were not predictive in this cohort. During post-treatment follow-up (range 0.4–7.8 years) cholecystectomy was performed in 22% of those with cholelithiasis. No serious complications due to gallstones occurred.
Conclusion:
The risk of developing gallstones in obese children and adolescents during a lifestyle intervention is limited and mainly related to the degree of weight loss and initial body weight.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Palasciano G, Portincasa P, Vinciguerra V, Velardi A, Tardi S, Baldassarre G et al. Gallstone prevalence and gallbladder volume in children and adolescents: an epidemiological ultrasonographic survey and relationship to body mass index. Am J Gastroenterol 1989; 84: 1378–1382.
Wesdorp I, Bosman D, de Graaff A, Aronson D, van der Blij F, Taminiau J . Clinical presentations and predisposing factors of cholelithiasis and sludge in children. J Pediatr Gastroenterol Nutr 2000; 31: 411–417.
Kaechele V, Wabitsch M, Thiere D, Kessler AL, Haenle MM, Mayer H et al. Prevalence of gallbladder stone disease in obese children and adolescents: influence of the degree of obesity, sex, and pubertal development. J Pediatr Gastroenterol Nutr 2006; 42: 66–70.
Koebnick C, Smith N, Black MH, Porter AH, Richie BA, Hudson S et al. Pediatric obesity and gallstone disease. J Pediatr Gastroenterol Nutr 2012; 55: 328–333.
Mehta S, Lopez ME, Chumpitazi BP, Mazziotti MV, Brandt ML, Fishman DS . Clinical characteristics and risk factors for symptomatic pediatric gallbladder disease. Pediatrics 2012; 129: e82–e88.
Fradin K, Racine AD, Belamarich PF . Obesity and symptomatic cholelithiasis in childhood: epidemiologic and case-control evidence for a strong relationship. J Pediatr Gastroenterol Nutr 2013; 58: 102–106.
Keskin M, Kurtoglu S, Kendirci M, Atabek ME, Yazici C . Homeostasis model assessment is more reliable than the fasting glucose/insulin ratio and quantitative insulin sensitivity check index for assessing insulin resistance among obese children and adolescents. Pediatrics 2005; 115: e500–e503.
Everhart JE . Contributions of obesity and weight loss to gallstone disease. Ann Intern Med 1993; 119: 1029–1035.
Erlinger S . Gallstones in obesity and weight loss. Eur J Gastroenterol Hepatol 2000; 12: 1347–1352.
Yang H, Petersen GM, Roth MP, Schoenfield LJ, Marks JW . Risk factors for gallstone formation during rapid loss of weight. Dig Dis Sci 1992; 37: 912–918.
Li VK, Pulido N, Fajnwaks P, Szomstein S, Rosenthal R, Martinez-Duartez P . Predictors of gallstone formation after bariatric surgery: a multivariate analysis of risk factors comparing gastric bypass, gastric banding, and sleeve gastrectomy. Surg Endosc 2009; 23: 1640–1644.
Johansson K, Sundström J, Marcus C, Hemmingsson E, Neovius M . Risk of symptomatic gallstones and cholecystectomy after a very-low-calorie diet or low-calorie diet in a commercial weight loss program: 1-year matched cohort study. Int J Obes (Lond) 2014; 38: 279–284.
Bogue CO, Murphy AJ, Gerstle JT, Moineddin R, Daneman A . Risk factors, complications, and outcomes of gallstones in children: a single-center review. J Pediatr Gastroenterol Nutr 2010; 50: 303–308.
Oude Luttikhuis H, Baur L, Jansen H, Shrewsbury VA, O’Malley C, Stolk RP et al. Interventions for treating obesity in children. Cochrane Database Syst Rev 2009; CD001872.
Acknowledgements
We gratefully acknowledge the pediatricians at Heideheuvel Childhood Obesity Centre for recruiting patients, the CBSL laboratory of the Ter Gooi Hospital for helping in collecting and storing samples. This work was supported by grants from Het Innovatiefonds Zorgverzekeraars (Zeist, The Netherlands) and Van den Broek Lohman Foundation Nunspeet (Nunspeet, The Netherlands).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Heida, A., Koot, B., vd Baan-Slootweg, O. et al. Gallstone disease in severely obese children participating in a lifestyle intervention program: incidence and risk factors. Int J Obes 38, 950–953 (2014). https://doi.org/10.1038/ijo.2014.12
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2014.12
Keywords
This article is cited by
-
Pediatric biliary calculus disease: clinical spectrum, predisposing factors, and management outcome revisited
Annals of Pediatric Surgery (2022)
-
Diagnosis, treatment and prevention of pediatric obesity: consensus position statement of the Italian Society for Pediatric Endocrinology and Diabetology and the Italian Society of Pediatrics
Italian Journal of Pediatrics (2018)