Abstract
Prenatal ethanol exposure is known to cause neurodevelopmental disorders. While high prevalence of epilepsy is observed among the children whose mothers abused alcohol during pregnancy, the results from animal studies are conflicting. Here, we investigated whether embryonic exposure to ethanol can increase the susceptibility to pentylenetetrazole (PTZ)-induced seizures in larval zebrafish. Embryos at 3 hours post-fertilization (hpf) were exposed to ethanol at the concentrations ranging from 0.25% to 1% for 21 hours. Control and ethanol-exposed larvae were challenged with PTZ at 7 days post-fertilization (dpf) at the concentrations of 2.5, 5 or 15 mM. The seizure behavior of larvae was recorded and analyzed using EthoVision XT 11. We found that embryonic ethanol exposure increased the percentage of larvae exhibiting typical stage II and III seizure and resulted in a significant reduction in stage I, II and III seizure latency in an ethanol concentration-dependent manner. Embryonic exposure to ethanol also significantly increased the severity of PTZ-induced seizures in larvae, as demonstrated by increased total distance traveled and the duration of mobility. This is the first demonstration that ethanol exposure during early embryonic stage can reduce the threshold for chemically induced seizures and increase the severity of seizure behavior in larval fish.
Similar content being viewed by others
Introduction
Fetal Alcohol Spectrum Disorders (FASD) is an umbrella term to describe the disorders that can occur in a child prenatally exposed to alcohol. FASD includes Fetal alcohol syndrome (FAS), Alcohol-Related Neurodevelopment Disorders (ARND) and Alcohol-Related Birth Defects (ARBD) as well as other disorders associated with prenatal alcohol exposure1,2. Prenatal ethanol exposure results in brain damage, leading to a variety of neurological disorders and behavioral problems, including epilepsy.
Epilepsy is a prominent manifestation of neurologic dysfunction in many children prenatally exposed to alcohol3,4,5,6,7,8. In a recent prevalence analysis, Bell found that approximately 20% children with FAS have seizure disorders9. Among children who were prenatally exposed to alcohol, but without a diagnosis of FAS, the prevalence of seizure disorders range from 14.1% for partial FAS to 18.23% for the alcohol-related neurodevelopmental disorders9. It has also been estimated that the prevalence of seizure disorders range from 6% to 21% in individuals with a FAS10,11. It is clear that children whose mother drinks alcohol during pregnancy are prone to have a higher rate of epilepsy than does the general population, in which the prevalence of epilepsy is less than 1%12. These results from human studies strongly suggest that prenatal alcohol exposure can significantly increase the rate of epilepsy in children prenatally exposed to alcohol.
A number of animal studies have been conducted to determine the link between developmental ethanol exposure and the susceptibility to seizure. Results from several laboratories by using rodent models strongly suggested that ethanol exposure during early developmental stages predisposes the offspring to seizure13,14,15,16,17,18,19. However, conflicting results on whether developmental alcohol exposure predisposes the offspring to seizures were also reported by other laboratories using rodent models20,21,22,23,24. It is clear that while rodent seizure models have significantly contributed to our understanding of effects of developmental ethanol exposure on the seizure, the results from these studies are controversial. To further our understanding of the effects of fetal alcohol exposure on the vulnerability to epileptic seizures, elucidate the underlying mechanisms and develop novel treatments, additional animal models are needed. In addition, the comparison between various animal models is also critical for elucidating the mechanisms underlying neurologic dysfunctions induced by developmental alcohol exposure and for uncovering the evolutionarily conserved mechanisms of epileptogenesis. Zebrafish represent a powerful novel experimental model for this purpose.
Zebrafish (Danio rerio) are emerging as a promising animal model to study various brain dysfunctions, including epilepsy because it possesses several characteristics that are not offered by other traditional models. For example, the rapid development of zebrafish (days as opposed to weeks) makes it a great model for early developmental exposure. The tiny size of zebrafish larvae (~4 mm), and a large number of embryos (~250) produced from a single mating make it possible to test large numbers of animals at various experimental conditions simultaneously. Zebrafish larvae are also useful for pharmacological and toxicological screens, as they are permeable to small molecules25,26. In addition, a high degree of conservation of the nervous system is present between zebrafish and mammals, making comparative studies possible27,28. Furthermore, the use of larval zebrafish as a model organism in behavioral studies has been rapidly expanding due to the development and availability of advanced analytical platforms invented to measure locomotor activity in larval zebrafish29,30,31,32,33.
In this study, zebrafish was used as a model to investigate the effect of alcohol exposure during early developmental stage on the vulnerability to epileptic seizures induced by PTZ, a very well characterized chemical convulsant. To this end, zebrafish embryos at 3 hpf were exposed to ethanol at various concentrations for 21 hours. Control and ethanol-exposed seven-days-old zebrafish larvae were challenged with PTZ. The seizure behavior of larval fish was monitored and recorded using a digital camera and analyzed using EthoVision XT 11, a professional behavior tracking software. The results from this study demonstrated for the first time that ethanol exposure during early embryonic stage can decrease the threshold for chemically induced seizures and increase the severity of seizure behavior in larval fish.
Results
Embryonic ethanol exposure increased the percentage of larval zebrafish exhibiting a seizure behavioral response induced by PTZ
PTZ model is one of the most widely used animal seizure models for antiepileptic drug (AED) discovery and elucidation of the mechanisms underlying seizure34,35,36. Studies have indicated that PTZ can elicit seizures in zebrafish larvae, and a sequence of seizure-like behaviors has been well established and defined in 7 dpf zebrafish larvae by behavioral and electrographic studies, as well as by pharmacologic studies using valproate, diazepam and other antiepileptic drugs34. PTZ-induced seizures in 7 dpf zebrafish larvae, as well as in adult zebrafish have been demonstrated to be inhibited in a concentration-dependent manner by common antiepileptic drugs37,38,39. PTZ-induced seizure in zebrafish can generally be categorized into three stage patterns based on their advancement in locomotor behavior34. Using this well-established and validated 7 dpf zebrafish larvae PTZ-seizures model, we found that, at stage I, fish are characterized by a significantly general increase in locomotor activity (Fig. 1B). A stage II PTZ-induced seizure in zebrafish consists of an easily identifiable, rush, circular swimming motion, which is clearly distinguishable from the generalized increased activity observed at stage I (Fig. 1C). At stage III, zebrafish experiences a series of brief clonus-like convulsions and eventually progresses to a loss of position and remains immobile for several seconds (Fig. 1D). To determine whether embryonic exposure to ethanol increase the susceptibility to PTZ-induced seizure, zebrafish embryos were exposed to ethanol at concentrations ranging from 0.25 to 1% from 3 to 24 hpf, a period in zebrafish that encompasses both gastrulation (5.25 to 10 hpf) and neurulation (10 to 24 hpf) which falls within the first trimester of human gestation40. Control and ethanol-exposed 7 dpf zebrafish larvae, in which most of the main neuronal clusters and axon tracts have been formed41, were exposed to PTZ at the concentrations of 2.5, 5 or 15 mM. The seizure behavior of larval fish was monitored and recorded using a digital camera and analyzed using EthoVision XT11, a professional behavior tracking software. We found that seizure behavior was not observed in larvae that were not exposed to PTZ, regardless of ethanol-exposure at an embryonic stage. All larvae with or without prior embryonic ethanol exposure exhibited a stage I response when they were exposed to 2.5, 5 or 15 mM PTZ (Fig. 1E). Embryonic exposure to ethanol resulted in an increased seizure response at stage II and III in an ethanol concentration-dependent manner as compared with larvae without prior embryonic ethanol exposure and treated with the corresponding concentration of PTZ (Fig. 1E–G). When treatment with 2.5 mM PTZ, 65% larvae without prior ethanol exposure exhibited stage II seizure response but none of them exhibited stage III seizure. However, stage III seizure behavior was observed in 55%, 75% and 90% larvae with prior embryonic exposure to 0.25, 0.5 or 1% ethanol, respectively, indicating that the larvae with prior embryonic ethanol exposure can reach a stage III seizure when they were exposed to low concentration of PTZ (e.g., 2.5 mM), a concentration that cannot elicit stage III seizure at any larvae without prior ethanol exposure (Fig. 1G). When exposure to 5 mM PTZ, 90% and 28% larvae without prior embryonic ethanol exposure exhibited stage II and III seizure behavior, respectively. All larvae with prior embryonic ethanol exposure exhibited stage II seizure when exposed to 5 mM PTZ while 68%, 86% and 98% larvae with prior embryonic exposure to 0.25%, 0.5, and 1% ethanol, respectively, exhibited stage III seizure. It is noteworthy that embryonic exposure to 2.5% ethanol increased the percentage of larvae that exhibited stage III seizure to 70% in the presence of 5 mM PTZ, as compared to 30% in the larvae without prior ethanol exposure. When treatment with 15 mM PTZ, all larvae with or without prior ethanol exposure exhibited stage II seizure while 55% larvae without prior ethanol exposure, and 86% larvae with prior exposure to 0.25% ethanol exhibited stage III seizure. All larvae with prior exposure to either 0.5 or 1% ethanol exhibited stage III seizure behavior.
Percentage of fish with embryonic ethanol exposure exhibiting a seizure behavioral response induced by PTZ. (A–D) Representative trajectory plots of zebrafish larvae displaying three distinct seizure stages. (A) 0 mM PTZ, without discernable seizure behaviors; (B) 2.5 mM PTZ, typical stage I seizure behaviors; (C) 5 mM PTZ, typical stage II seizure behaviors; (D) 15 mM PTZ, typical stage III seizure behaviors. (E–G) Percentage of zebrafish with embryonic ethanol exposure reaching a defined seizure stage after exposure to PTZ for 15 min. (E) Stage I; (F) Stage II; (G) Stage III. At least 10 larvae were used for each treatment.
Embryonic ethanol exposure increased the total distance traveled in larval zebrafish exposed to PTZ
As defined above, both stage I and II seizures exhibit increased movement while stage III seizures show a decreased movement. Analysis with EthoVision after 15 min treatment with PTZ showed a significant alteration in the distance traveled in the larvae with prior ethanol exposure (Fig. 2A,B). Larvae exposed to 2.5 mM PTZ showed a significant increase in distance moved in an ethanol concentration-dependent manner. The larvae with prior exposure to 0.5% ethanol traveled at least twice the distance as the larvae without prior ethanol exposure (Fig. 2B). At a concentration of 5 mM PTZ, all larvae with prior ethanol exposure showed a general increase in distance traveled. However, the distance traveled in the group with prior exposure to a lower concentration of ethanol traveled more distance than that exposed to higher concentration of ethanol, consistent with the fact that more larvae with prior exposure to higher concentration of ethanol reach stage III seizure. In the presence of 15 mM PTZ, all ethanol-exposed groups showed a general decrease in distance moved (Fig. 2).
Effect of embryonic ethanol exposure on the total distance traveled in zebrafish exposed to PTZ. (A) Representative trajectory plots of zebrafish larvae exposed to different concentrations of ethanol and 2.5 mM PTZ. (a) Control; (b) 0.25% (v/v) EtOH; (c) 0.5% (v/v) EtOH; (d) 1% (v/v) EtOH. (B) Embryonic ethanol exposure increased the total distance traveled in zebrafish exposed to 2.5 or 5 mM PTZ. At least 10 larvae were used for each treatment. Data represent the mean ± SEM. *p < 0.05 vs. corresponding control.
Embryonic ethanol exposure increased the duration of time spent in a general active state or highly mobile state in larval zebrafish exposed to PTZ
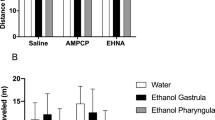
Although stage III seizure is characterized by convulsive behavior without distance movement, it exhibits stationary body movement. In addition to detecting distance moved, the latest version of EthoVision software, EthoVision XT 11, can also analyze other mobility parameters, including stationary body movement. In this study, the mobility duration, a parameter incorporates both stage II and Stage III body movement, was analyzed in the larvae exposed to PTZ. As shown in Fig. 3, at 5 mM PTZ, larvae with prior exposure to 0.25% ethanol showed a significant increase in mobility duration (Fig. 3A) as well as the duration of time spent in a strongly mobile state, which was mostly observed at stage II seizure (Fig. 3B). Larvae that were exposed to 0.5% ethanol at embryonic stage showed dramatic increases in mobility when they were exposed to all PTZ doses tested (Fig. 3A). The fish in this group also spent significantly more time in a strong mobile state at 5 mM PTZ (Fig. 3B). The larvae with prior embryonic exposure to 1% ethanol showed a significant increase in mobility duration at 2.5, 5 or 15 mM PTZ and the duration of strong mobility at 2.5 mM PTZ but not at 5 or 15 mM PTZ (Fig. 3B), indicating that these larvae were undergoing Stage III convulsive motions at higher PTZ doses. Similarly, members of two other dose groups of ethanol (0.25% and 0.5%, v/v) that have shown a significant increase in strong mobility duration at 5 mM PTZ didn’t show a significant increase in strong mobility at 15 mM PTZ doses (Fig. 3B), thereby indicating that these larvae may also undertake convulsive motions at highest PTZ dose. Although distance moved not significantly increased compared with control treatment, the members of the highest ethanol group (1%, v/v) showed a significant increase in mobility at higher PTZ doses, but its increase in duration of strong mobility is generally reduced, confirming that these larvae were undergoing relative convulsive motions.
Effect of embryonic ethanol exposure on the duration of time spent in a general active state or highly mobile state after exposure to PTZ. (A) Duration of time spent in a mobile state after exposure to PTZ. (B) Duration of time spent in a highly mobile state after exposure to PTZ. At least 10 larvae were used for each treatment. Data represent the mean ± SEM. *p < 0.05 vs. corresponding control.
Embryonic ethanol exposure resulted in a significant reduction in seizure latency in larval zebrafish exposed to PTZ
The time required for the onset of the first sign of Stage I, II and III seizures in the larvae after PTZ challenge was used to determine the seizure latency. We found that, in control fish that were not exposed to ethanol embryonically, the seizure latency in stage I, II were 425 sec and 680 sec, respectively, after they were exposed to 2.5 mM PTZ, and were 140 sec and 300 sec, respectively, after they were exposed to 15 mM PTZ (Fig. 4A and B). In control fish that were not exposed to ethanol, the seizure latency in stage III was 700 sec for 5 mM PTZ and 640 sec for 15 mM PTZ (Fig. 4C). All larvae exposed to ethanol embryonically showed a significant time reduction in stage I, II or III seizure latency after exposed to PTZ. At high PTZ concentration (15 mM), a stage I, II or III seizure was observed within 60 sec, 100 sec, and 250 sec, respectively, in the group exposed to 1% ethanol embryonically (Fig. 4). The embryonic exposure to 1% ethanol also resulted in a stage II seizure behavioral response within 100 sec following the exposure to 5 mM PTZ (Fig. 4). Significant time reductions of seizure latencies were also observed across other dose combinations of ethanol and PTZ. After exposure to 2.5, 5, or 15 mM PTZ, a significant time reduction in stage I, II or III seizure latency (p < 0.05) were observed in the larvae that were embryonically exposed to the lowest concentration of ethanol (0.25%) (Fig. 4). While no stage III seizure behavior was observed in control larvae that were exposed to 2.5 mM PTZ, exposure to this low dose of PTZ resulted in a stage III seizure in larvae that were embryonically exposed to ethanol (Fig. 4).
Effect of embryonic ethanol exposure on the latency to the first sign of PTZ-induced seizure behaviors for three different stages. (A) Stage I. (B) Stage II. (C) Stage III. aNo fish had a seizure response in the absence of PTZ. bNo fish in this group was able to reach stage III seizure. At least 10 larvae were used for each treatment. Data represent the mean ± SEM. *p < 0.05 vs. corresponding control.
Discussion
In this study, we demonstrate that embryonic exposure to ethanol at concentrations as low as 0.25–1.0% can increase the vulnerability of larval zebrafish to the PTZ-induced seizures. We found that embryonic ethanol exposure increased the percentage of larval zebrafish exhibiting typical stage II and III seizures induced by PTZ. Ethanol exposure during the early developmental stage also significantly increased the total distance traveled in larval zebrafish exposed to PTZ. In addition, embryonic ethanol exposure increased the duration of time spent in a general active state or highly mobile state in larval zebrafish exposed to PTZ. Ethanol exposure also resulted in a significant reduction in seizure latency in larval zebrafish exposed to PTZ. These results demonstrate that ethanol exposure during early embryonic stage can reduce the threshold for chemically induced seizures and increase the severity of seizure behaviors in larval fish.
Previous studies using rodent models have contributed significantly to our understanding of the effects of developmental ethanol exposure on the susceptibility to seizure. Yanai and colleagues found that the threshold for audiogenic seizures was decreased in the mice whose mothers drank alcohol during pregnancy13,14. Studies have also shown that alcohol exposure during the brain growth spurt facilitated PTZ-induced seizures, in the form of increased behavioral activity and electrographic epileptic activity16. It has also been reported that fetal alcohol exposure induced long-lasting increases in postnatal anxiety, tolerance to acute sedative/anesthetic effects of ethanol, and increases seizure susceptibility15. These studies are consistent with the results from our current studies and support the premise that exposure to ethanol during critical developmental stage predisposes the offspring to seizures later in life.
It is well known that interactions of environmental risk factors with genetic factors play an important role in the etiology of seizures42,43,44. Exposure to environmental risk factors early in life can result in profound changes in brain structure, which constitute the pathological basis of adult neurological diseases, including seizures. Early developmental exposure to nicotine45, lead46, methylazoxymethanol acetate47, hypoxia48, lamotrigine49, gamma rays50, methamphetamine51, methylmercury52, polychlorinated biphenyls53 or domoic acid29 has been shown to initiate or promote the development of seizures. In addition, improved maternal care has been shown to reduce seizure susceptibility in rodents54,55,56.
The mechanism by which early alcohol exposure increases the susceptibility to PTZ-induced seizures later in life is not well understood. However, it is well known that ethanol exposure during the early developmental stages impaired brain development and functions, including increased neuronal cell death, impaired neuronal migration, altered neurotransmitters and their receptors, and disrupted neuronal circuitry, which could predispose the developing offsprings to PTZ-induced seizures16,18,57,58. It was reported that altered hippocampal structure is one of the prominent characteristics in the offspring of an alcoholic mother59,60. Studies in animals revealed that developmental ethanol exposure produces long-term hippocampal cell loss61,62. It was well-established that hippocampus plays a critical role in seizure occurrences63,64. A direct experimental observation from Bonthius and co-works suggested that the permanent disruption of the hippocampal formation by ethanol through selected cell loss contributes heavily to the reduced seizure threshold65.
Alcohol-induced impairments in neurotransmitters and their receptors may also play a role in ethanol-induced increased vulnerability to epileptic seizures57,66. One of the neurotransmitter receptors that is targeted by ethanol is γ-aminobutyric acid (GABA) receptor67,68,69,70. It has been demonstrated that both chronic and acute ethanol administration resulted in persistent alterations in GABA receptor subunit composition, localization, and function67,68,69,70,71,72. These changes in the physiology of GABA receptors occur not only in adult animals but also in developing animals exposed to ethanol during the brain development73,74. It is well documented that animals with genetic defects of the GABA receptor are predisposed to seizures75,76. Considering the fact that PTZ is a competitive antagonist of the GABA receptor77 and that alcohol can disrupt GABA receptor, it is likely that alcohol-induced alteration of GABA receptor contributes to the reduced seizure threshold observed in this study. It is also noteworthy that the GABA systems have been shown to develop early during embryogenesis and are present in larval zebrafish78, providing a physiological basis for the possible involvement of GABA receptor in ethanol-induced vulnerability to epileptic seizures in zebrafish larvae. However, the role of GABA receptor in the ethanol-induced reduction of seizure threshold in zebrafish larvae would need to be explored further.
While multiple studies from other laboratories using rodent models and our study using zebrafish strongly suggested that ethanol exposure during the development increases the vulnerability to epileptic seizures, there were other studies that have found that developmental exposure to ethanol does not make the rats more prone to seizures later in life20,21,22,23,24,79. One of the proposed explanations for these inconsistent results is the timing of the alcohol exposure16. While those studies in rodent model that have found that developmental exposure to ethanol does not predispose the offspring to seizures later in life administered alcohol during the prenatal period20,21,22,23,24,79, other studies using rodent model that have demonstrated that early ethanol exposure increased the vulnerability to seizures administered alcohol postnatally15,16,65. It is well known that the consequences of alcohol exposure during development depend heavily on the timing of the exposure. Administration of a similar dose of alcohol at different developmental stages can have substantially different physiologic, pathologic, and behavioral effects80,81,82,83. However, our present study demonstrated that exposure of the zebrafish embryos to ethanol at 3–24 hpf, which falls within the first trimester of human gestation and prenatal stage of mouse and rat development, can increase the vulnerability to seizures in larvae, indicating that the factors other than the timing of the alcohol exposure might also contribute to the inconsistent results.
To the best of our knowledge, the rodent was the only animal model employed in all published studies examining the effect of alcohol exposure during development on the vulnerability to epileptic seizures later in life. Controversial results from previous studies using rodent models warrant further investigation using additional animal models. For this purpose, zebrafish represents a promising novel model for studying seizure behavior and epilepsy in the offspring of early ethanol exposure. That the seizure behaviors can be further analyzed using a high-speed locomotion tracking system allows rapid quantification of behavior with minimal human effort. Indeed, zebrafish has been successfully used as a behavioral model to study the effects of alcohol on locomotor activity, and these studies showed that ethanol administration produced a biphasic dose-response pattern, where lower doses increased activity, and higher doses decreased activity, in both larval84,85,86,87 or adult fish88,89. Studies have also indicated that PTZ can elicit seizures in zebrafish larvae, and a sequence of seizure-like behaviors has been well established and defined in zebrafish34. Comparing our findings in zebrafish with previously published data in rodent models may enable a better understanding of the effects of developmental ethanol exposure on the susceptibility to seizures.
In conclusion, our present study indicated that early embryonic exposure increased the percentage of larval zebrafish exhibiting typical stage II and III seizure and resulted in a significant reduction in stage I, II and III seizure latency in an ethanol concentration-dependent manner. Embryonic exposure to ethanol also significantly increased the severity of PTZ-induced seizures in larval zebrafish, as demonstrated by increased total distance traveled and the duration of mobility. This is the first demonstration that ethanol exposure during early embryonic stage can reduce the threshold to chemically induced seizures and increase the severity of seizure behavior in larval fish. These findings suggest that, in addition to causing FAS, early embryonic exposure to ethanol may enhance the biological risk for chronic diseases later in life. Future studies to analyze the alteration in the expression of genes that predispose the offspring to seizures and the potential epigenetic regulation of these genes in zebrafish embryos and larvae exposed to ethanol during early development will further elucidate the molecular mechanism underlying the embryonic ethanol exposure-induced vulnerability to seizures.
Methods
Zebrafish
Zebrafish (Danio rerio) of wild-type AB strain were obtained from Zebrafish International Resource Center (ZIRC; Eugene, OR) and maintained in a zebrafish housing system (Aquaneering; San Diego, CA). Fish were fed twice a day with commercial flake food (Tetra, Daleville, VA) and with live brine shrimp to incite optimal egg production. Females and males in a ratio of 1:2 were transferred into crossing tanks in the evening before spawning induction. Newly fertilized eggs were raised at 28 °C in embryo water (Milli-Q water with 60 mg/L Instant Ocean). All protocols used in this study were approved by the University of Louisville Institutional Animal Care and Use Committee, and all experiments were conducted in accordance with the relevant guidelines and regulations.
Ethanol treatment of embryos
Embryos were exposed to ethanol at concentrations ranging from 0.25–1% (v/v) during 3–24 hours post fertilization (hpf). Stable ethanol levels were maintained by using a screw cap for each vial. After ethanol exposure, the embryos were rinsed three times and raised to 7 days of post fertilization (dpf) in a 28 °C incubator before they were exposed to PTZ.
PTZ challenges
7-day-old larvae from control and treatment groups were transferred to individual wells of 96-well plates (VWR scientific) with 50 μL fresh Ringers solution. Any fish with growth retardation or morphology abnormalities was excluded from the study. The plate was placed on the stage of an Olympus (SZH) stereo microscope system equipped with an RGB camera which was connected to a computer running EthoVision XT 11 behavioral tracking software (Noldus Information Technology Inc., Leesburg, VA). Before they were exposed to PTZ, a 3 min baseline trial was tracked and recorded in larvae at control medium. The medium was then replaced with one of three concentrations of PTZ (2.5, 5, 15 mM). The response was recorded for a total of 18 min with an additional 3 min trial after the 15 min of exposure had lapsed.
Data analysis
Recordings of the larvae after the PTZ exposure were analyzed for behavioral changes and seizures. The distance moved and the mobility parameters were analyzed by using EthoVision XT 11 tracking program, and the baseline parameters were subtracted out before calculation. Time to reach the first definitive stage I, II or III seizure (seizure latency) was also determined. A minimum of 10 individuals per ethanol/PTZ combination was used in all calculations. Two-way analysis of variance (ANOVA) followed by Bonferroni means comparison test (Prism version 5; GraphPad Software Inc. San Diego, CA) were used to analyze the compounding effects of both ethanol and PTZ on the larval fish.
References
Sokol, R. J., Delaney-Black, V. & Nordstrom, B. Fetal alcohol spectrum disorder. Jama 290, 2996–2999, https://doi.org/10.1001/jama.290.22.2996 (2003).
O’Malley, K. D. & Rich, S. D. Clinical Implications of a Link Between Fetal Alcohol Spectrum Disorders (FASD) and Autism Or Asperger’s Disorder - A Neurodevelopmental Frame for Helping Understanding and Management. (INTECH Open Access Publisher, 2013).
Ioffe, S. & Chernick, V. Prediction of subsequent motor and mental retardation in newborn infants exposed to alcohol in utero by computerized EEG analysis. Neuropediatrics 21, 11–17 (1990).
Jones, K. L., Smith, D. W., Ulleland, C. N. & Streissguth, P. Pattern of malformation in offspring of chronic alcoholic mothers. Lancet 1, 1267–1271 (1973).
Marcus, J. C. Neurological findings in the fetal alcohol syndrome. Neuropediatrics 18, 158–160, https://doi.org/10.1055/s-2008-1052471 (1987).
Coulter, C. L., Leech, R. W., Schaefer, G. B., Scheithauer, B. W. & Brumback, R. A. Midline cerebral dysgenesis, dysfunction of the hypothalamic-pituitary axis, and fetal alcohol effects. Archives of neurology 50, 771–775 (1993).
Bhang, S. Y., Ahn, D. H., Lee, Y. J., An, H. Y. & Ahn, J. H. The first report of fetal alcohol effect in a 12 year-old child in Korea. Psychiatry investigation 6, 50–53, https://doi.org/10.4306/pi.2009.6.1.50 (2009).
Sun, Y. et al. Binge drinking during pregnancy and risk of seizures in childhood: a study based on the Danish National Birth Cohort. American journal of epidemiology 169, 313–322, https://doi.org/10.1093/aje/kwn334 (2009).
Bell, S. H. et al. The remarkably high prevalence of epilepsy and seizure history in fetal alcohol spectrum disorders. Alcoholism, clinical and experimental research 34, 1084–1089, https://doi.org/10.1111/j.1530-0277.2010.01184.x (2010).
Iosub, S., Fuchs, M., Bingol, N. & Gromisch, D. S. Fetal alcohol syndrome revisited. Pediatrics 68, 475–479 (1981).
Spohr, H. L. & Steinhausen, H. C. Follow-up studies of children with fetal alcohol syndrome. Neuropediatrics 18, 13–17, https://doi.org/10.1055/s-2008-1052428 (1987).
Tellez-Zenteno, J. F., Pondal-Sordo, M., Matijevic, S. & Wiebe, S. National and regional prevalence of self-reported epilepsy in Canada. Epilepsia 45, 1623–1629, https://doi.org/10.1111/j.0013-9580.2004.24904.x (2004).
Yanai, J., Sze, P. Y. & Ginsburg, B. E. Effects of aminergic drugs and glutamic acid on audiogenic seizures induced by early exposure to ethanol. Epilepsia 16, 67–71 (1975).
Yanai, J. & Ginsburg, B. E. Audiogenic seizures in mice whose parents drank alcohol. Journal of studies on alcohol 37, 1564–1571 (1976).
Liang, J. et al. Dihydromyricetin prevents fetal alcohol exposure-induced behavioral and physiological deficits: the roles of GABAA receptors in adolescence. Neurochemical research 39, 1147–1161, https://doi.org/10.1007/s11064-014-1291-5 (2014).
Bonthius, D. J., Woodhouse, J., Bonthius, N. E., Taggard, D. A. & Lothman, E. W. Reduced seizure threshold and hippocampal cell loss in rats exposed to alcohol during the brain growth spurt. Alcoholism, clinical and experimental research 25, 70–82 (2001).
Cho, S. J., Lovinger, D. M. & N’Gouemo, P. Prenatal alcohol exposure enhances the susceptibility to NMDA-induced generalized tonic-clonic seizures in developing rats. CNS Neurosci Ther 23, 808–817, https://doi.org/10.1111/cns.12756 (2017).
Krawczyk, M. et al. Hippocampal hyperexcitability in fetal alcohol spectrum disorder: Pathological sharp waves and excitatory/inhibitory synaptic imbalance. Experimental neurology 280, 70–79, https://doi.org/10.1016/j.expneurol.2016.03.013 (2016).
Riljak, V., Maresova, D., Jandova, K., Bortelova, J. & Pokorny, J. Impact of chronic ethanol intake of rat mothers on the seizure susceptibility of their immature male offspring. Gen Physiol Biophys 31, 173–177, https://doi.org/10.4149/gpb_2012_019 (2012).
Abel, E. L., Berman, R. F. & Church, M. W. Prenatal alcohol exposure attenuates pentylenetetrazol-induced convulsions in rats. Alcohol 10, 155–157 (1993).
Kim, C. K., Dalal, S., Pinel, J. P. & Weinberg, J. Prenatal ethanol exposure: susceptibility to convulsions and ethanol’s anticonvulsant effect in amygdala-kindled rats. Alcoholism, clinical and experimental research 18, 1506–1514 (1994).
Savage, D. D. & Reyes, E. Prenatal exposure to ethanol retards the development of kindling in adult rats. Experimental neurology 89, 583–591 (1985).
Viirre, E., Cain, D. P. & Ossenkopp, K. P. Prenatal ethanol exposure alters rat brain morphology but does not affect amygdaloid kindling. Neurobehavioral toxicology and teratology 8, 615–620 (1986).
Berman, R. F., Beare, D. J., Church, M. W. & Abel, E. L. Audiogenic seizure susceptibility and auditory brainstem responses in rats prenatally exposed to alcohol. Alcoholism, clinical and experimental research 16, 490–498 (1992).
Kokel, D. et al. Rapid behavior-based identification of neuroactive small molecules in the zebrafish. Nature chemical biology 6, 231–237, https://doi.org/10.1038/nchembio.307 (2010).
Rihel, J. et al. Zebrafish behavioral profiling links drugs to biological targets and rest/wake regulation. Science 327, 348–351, https://doi.org/10.1126/science.1183090 (2010).
Eklof-Ljunggren, E. et al. Origin of excitation underlying locomotion in the spinal circuit of zebrafish. Proceedings of the National Academy of Sciences of the United States of America 109, 5511–5516, https://doi.org/10.1073/pnas.1115377109 (2012).
Panula, P. et al. The comparative neuroanatomy and neurochemistry of zebrafish CNS systems of relevance to human neuropsychiatric diseases. Neurobiology of disease 40, 46–57, https://doi.org/10.1016/j.nbd.2010.05.010 (2010).
Tiedeken, J. A. & Ramsdell, J. S. Embryonic exposure to domoic Acid increases the susceptibility of zebrafish larvae to the chemical convulsant pentylenetetrazole. Environmental health perspectives 115, 1547–1552, https://doi.org/10.1289/ehp.10344 (2007).
Wong, K. et al. Modeling seizure-related behavioral and endocrine phenotypes in adult zebrafish. Brain research 1348, 209–215, https://doi.org/10.1016/j.brainres.2010.06.012 (2010).
Cachat, J. M. et al. In Zebrafish neurobehavioral protocols 1–14 (Springer, 2011).
Gaikwad, S. et al. Acute stress disrupts performance of zebrafish in the cued and spatial memory tests: the utility of fish models to study stress-memory interplay. Behavioural processes 87, 224–230, https://doi.org/10.1016/j.beproc.2011.04.004 (2011).
Zhou, Y., Cattley, R. T., Cario, C. L., Bai, Q. & Burton, E. A. Quantification of larval zebrafish motor function in multiwell plates using open-source MATLAB applications. Nature protocols 9, 1533–1548, https://doi.org/10.1038/nprot.2014.094 (2014).
Baraban, S. C., Taylor, M. R., Castro, P. A. & Baier, H. Pentylenetetrazole induced changes in zebrafish behavior, neural activity and c-fos expression. Neuroscience 131, 759–768, https://doi.org/10.1016/j.neuroscience.2004.11.031 (2005).
Loscher, W. Animal models of epilepsy for the development of antiepileptogenic and disease-modifying drugs. A comparison of the pharmacology of kindling and post-status epilepticus models of temporal lobe epilepsy. Epilepsy research 50, 105–123 (2002).
Mirski, M. A. & Ferrendelli, J. A. Anterior thalamic mediation of generalized pentylenetetrazol seizures. Brain research 399, 212–223 (1986).
Afrikanova, T. et al. Validation of the zebrafish pentylenetetrazol seizure model: locomotor versus electrographic responses to antiepileptic drugs. PLoS One 8, e54166, https://doi.org/10.1371/journal.pone.0054166 (2013).
Berghmans, S., Hunt, J., Roach, A. & Goldsmith, P. Zebrafish offer the potential for a primary screen to identify a wide variety of potential anticonvulsants. Epilepsy Res 75, 18–28, https://doi.org/10.1016/j.eplepsyres.2007.03.015 (2007).
Gupta, P., Khobragade, S. B. & Shingatgeri, V. M. Effect of Various Antiepileptic Drugs in Zebrafish PTZ-Seizure Model. Indian J Pharm Sci 76, 157–163 (2014).
Zhang, C., Ojiaku, P. & Cole, G. J. Forebrain and hindbrain development in zebrafish is sensitive to ethanol exposure involving agrin, Fgf, and sonic hedgehog function. Birth Defects Res A Clin Mol Teratol 97, 8–27, https://doi.org/10.1002/bdra.23099 (2013).
Tropepe, V. & Sive, H. L. Can zebrafish be used as a model to study the neurodevelopmental causes of autism? Genes Brain Behav 2, 268–281 (2003).
Ottman, R., Annegers, J. F., Risch, N., Hauser, W. A. & Susser, M. Relations of genetic and environmental factors in the etiology of epilepsy. Annals of neurology 39, 442–449, https://doi.org/10.1002/ana.410390406 (1996).
Kjeldsen, M. J., Kyvik, K. O., Friis, M. L. & Christensen, K. Genetic and environmental factors in febrile seizures: a Danish population-based twin study. Epilepsy research 51, 167–177 (2002).
Todorova, M. T., Mantis, J. G., Le, M., Kim, C. Y. & Seyfried, T. N. Genetic and environmental interactions determine seizure susceptibility in epileptic EL mice. Genes, brain, and behavior 5, 518–527, https://doi.org/10.1111/j.1601-183X.2006.00204.x (2006).
Britos, S. A. & Orsingher, O. A. Prenatal nicotine exposure increased susceptibility to electroconvulsive shock (ECS) in adult rats. Neurotoxicology and teratology 13, 271–273 (1991).
Chen, H. H. & Chan, M. H. Developmental lead exposure differentially alters the susceptibility to chemoconvulsants in rats. Toxicology 173, 249–257 (2002).
de Feo, M. R., Mecarelli, O. & Ricci, G. F. Seizure susceptibility in immature rats with micrencephaly induced by prenatal exposure to methylazoxymethanol acetate. Pharmacological research: the official journal of the Italian Pharmacological Society 31, 109–114 (1995).
De Riu, P. L., Mameli, P., Becciu, A., Simula, M. E. & Mameli, O. Effect of fetal hypoxia on seizure susceptibility in rats. Physiology & behavior 57, 315–318 (1995).
Forcelli, P. A., Gale, K. & Kondratyev, A. Early postnatal exposure of rats to lamotrigine, but not phenytoin, reduces seizure threshold in adulthood. Epilepsia 52, e20–22, https://doi.org/10.1111/j.1528-1167.2010.02971.x (2011).
Setkowicz, Z., Gzielo-Jurek, K., Uram, L., Janicka, D. & Janeczko, K. Brain dysplasia evoked by gamma irradiation at different stages of prenatal development leads to different tonic and clonic seizure reactivity. Epilepsy research 108, 66–80, https://doi.org/10.1016/j.eplepsyres.2013.10.010 (2014).
Slamberova, R. Flurothyl seizures susceptibility is increased in prenatally methamphetamine-exposed adult male and female rats. Epilepsy research 65, 121–124, https://doi.org/10.1016/j.eplepsyres.2005.04.002 (2005).
Szasz, A. et al. Chronic low-dose maternal exposure to methylmercury enhances epileptogenicity in developing rats. International journal of developmental neuroscience: the official journal of the International Society for Developmental Neuroscience 17, 733–742 (1999).
Poon, E., Bandara, S. B., Allen, J. B., Sadowski, R. N. & Schantz, S. L. Developmental PCB exposure increases susceptibility to audiogenic seizures in adulthood. Neurotoxicology 46, 117–124, https://doi.org/10.1016/j.neuro.2014.12.007 (2015).
Auvergne, R. et al. Delayed kindling epileptogenesis and increased neurogenesis in adult rats housed in an enriched environment. Brain research 954, 277–285 (2002).
Korbey, S. M., Heinrichs, S. C. & Leussis, M. P. Seizure susceptibility and locus ceruleus activation are reduced following environmental enrichment in an animal model of epilepsy. Epilepsy & behavior: E&B 12, 30–38, https://doi.org/10.1016/j.yebeh.2007.09.013 (2008).
Fares, R. P. et al. Standardized environmental enrichment supports enhanced brain plasticity in healthy rats and prevents cognitive impairment in epileptic rats. PloS one 8, e53888, https://doi.org/10.1371/journal.pone.0053888 (2013).
Phillips, T. J. & Shen, E. H. Neurochemical bases of locomotion and ethanol stimulant effects. International review of neurobiology 39, 243–282 (1996).
Luhmann, H. J. Models of cortical malformation–Chemical and physical. J Neurosci Methods 260, 62–72, https://doi.org/10.1016/j.jneumeth.2015.03.034 (2016).
Mattson, S. N., Schoenfeld, A. M. & Riley, E. P. Teratogenic effects of alcohol on brain and behavior. Alcohol research & health: the journal of the National Institute on Alcohol Abuse and Alcoholism 25, 185–191 (2001).
Riikonen, R., Salonen, I., Partanen, K. & Verho, S. Brain perfusion SPECT and MRI in foetal alcohol syndrome. Developmental medicine and child neurology 41, 652–659 (1999).
Livy, D. J., Miller, E. K., Maier, S. E. & West, J. R. Fetal alcohol exposure and temporal vulnerability: effects of binge-like alcohol exposure on the developing rat hippocampus. Neurotoxicology and teratology 25, 447–458 (2003).
Tran, T. D. & Kelly, S. J. Critical periods for ethanol-induced cell loss in the hippocampal formation. Neurotoxicology and teratology 25, 519–528 (2003).
Nishitani, N. et al. The role of the hippocampus in auditory processing studied by event-related electric potentials and magnetic fields in epilepsy patients before and after temporal lobectomy. Brain: a journal of neurology 122(Pt 4), 687–707 (1999).
Schwartzkroin, P. A. Role of the hippocampus in epilepsy. Hippocampus 4, 239–242, https://doi.org/10.1002/hipo.450040302 (1994).
Bonthius, D. J. et al. Alcohol exposure during the brain growth spurt promotes hippocampal seizures, rapid kindling, and spreading depression. Alcoholism, clinical and experimental research 25, 734–745 (2001).
Weiss, F. & Porrino, L. J. Behavioral neurobiology of alcohol addiction: recent advances and challenges. The Journal of neuroscience: the official journal of the Society for Neuroscience 22, 3332–3337, 20026359 (2002).
Kumar, S. et al. The role of GABA(A) receptors in the acute and chronic effects of ethanol: a decade of progress. Psychopharmacology 205, 529–564, https://doi.org/10.1007/s00213-009-1562-z (2009).
Grobin, A. C., Matthews, D. B., Devaud, L. L. & Morrow, A. L. The role of GABA(A) receptors in the acute and chronic effects of ethanol. Psychopharmacology 139, 2–19 (1998).
Igor Spigelman, R. W. O. et al. Chapter 23–Molecular and Functional Changes in Receptors: GABA and Chronic Alcohol Consumption. Biological research on addiction: comprehensive addictive behaviors and disorders 219–230 (2013).
Davies, M. The role of GABAA receptors in mediating the effects of alcohol in the central nervous system. Journal of psychiatry & neuroscience: JPN 28, 263–274 (2003).
Kang, M. H., Spigelman, I. & Olsen, R. W. Alteration in the sensitivity of GABA(A) receptors to allosteric modulatory drugs in rat hippocampus after chronic intermittent ethanol treatment. Alcoholism, clinical and experimental research 22, 2165–2173 (1998).
Mahmoudi, M., Kang, M. H., Tillakaratne, N., Tobin, A. J. & Olsen, R. W. Chronic intermittent ethanol treatment in rats increases GABA(A) receptor alpha4-subunit expression: possible relevance to alcohol dependence. Journal of neurochemistry 68, 2485–2492 (1997).
Hsiao, S. H., West, J. R., Mahoney, J. C. & Frye, G. D. Postnatal ethanol exposure blunts upregulation of GABAA receptor currents in Purkinje neurons. Brain research 832, 124–135 (1999).
Hsiao, S. H., Mahoney, J. C., West, J. R. & Frye, G. D. Development of GABAA receptors on medial septum/diagonal band (MS/DB) neurons after postnatal ethanol exposure. Brain research 810, 100–113 (1998).
Kralic, J. E., Korpi, E. R., O’Buckley, T. K., Homanics, G. E. & Morrow, A. L. Molecular and pharmacological characterization of GABA(A) receptor alpha1 subunit knockout mice. The Journal of pharmacology and experimental therapeutics 302, 1037–1045, https://doi.org/10.1124/jpet.102.036665 (2002).
Homanics, G. E. et al. Mice devoid of gamma-aminobutyrate type A receptor beta3 subunit have epilepsy, cleft palate, and hypersensitive behavior. Proceedings of the National Academy of Sciences of the United States of America 94, 4143–4148 (1997).
Huang, R. Q. et al. Pentylenetetrazole-induced inhibition of recombinant gamma-aminobutyric acid type A (GABA(A)) receptors: mechanism and site of action. The Journal of pharmacology and experimental therapeutics 298, 986–995 (2001).
Doldan, M. J., Prego, B. & Holmqvist, B. I. & de Miguel, E. Distribution of GABA-immunolabeling in the early zebrafish (Danio rerio) brain. European journal of morphology 37, 126–129 (1999).
Russo, E. et al. Effects of ethanol on the development of genetically determined epilepsies in rats. International journal of developmental neuroscience: the official journal of the International Society for Developmental Neuroscience 26, 739–744, https://doi.org/10.1016/j.ijdevneu.2008.07.002 (2008).
Goodlett, C. R. & Johnson, T. B. Neonatal binge ethanol exposure using intubation: timing and dose effects on place learning. Neurotoxicology and teratology 19, 435–446 (1997).
Maier, S. E., Miller, J. A., Blackwell, J. M. & West, J. R. Fetal alcohol exposure and temporal vulnerability: regional differences in cell loss as a function of the timing of binge-like alcohol exposure during brain development. Alcoholism, clinical and experimental research 23, 726–734 (1999).
Maier, S. E., Chen, W. J., Miller, J. A. & West, J. R. Fetal alcohol exposure and temporal vulnerability regional differences in alcohol-induced microencephaly as a function of the timing of binge-like alcohol exposure during rat brain development. Alcoholism, clinical and experimental research 21, 1418–1428 (1997).
Ali, S., Champagne, D. L., Alia, A. & Richardson, M. K. Large-scale analysis of acute ethanol exposure in zebrafish development: a critical time window and resilience. PloS one 6, e20037, https://doi.org/10.1371/journal.pone.0020037 (2011).
Lockwood, B., Bjerke, S., Kobayashi, K. & Guo, S. Acute effects of alcohol on larval zebrafish: a genetic system for large-scale screening. Pharmacology, biochemistry, and behavior 77, 647–654, https://doi.org/10.1016/j.pbb.2004.01.003 (2004).
Irons, T. D., MacPhail, R. C., Hunter, D. L. & Padilla, S. Acute neuroactive drug exposures alter locomotor activity in larval zebrafish. Neurotoxicology and teratology 32, 84–90, https://doi.org/10.1016/j.ntt.2009.04.066 (2010).
MacPhail, R. C. et al. Locomotion in larval zebrafish: Influence of time of day, lighting and ethanol. Neurotoxicology 30, 52–58, https://doi.org/10.1016/j.neuro.2008.09.011 (2009).
Chen, T. H., Wang, Y. H. & Wu, Y. H. Developmental exposures to ethanol or dimethylsulfoxide at low concentrations alter locomotor activity in larval zebrafish: implications for behavioral toxicity bioassays. Aquatic toxicology 102, 162–166, https://doi.org/10.1016/j.aquatox.2011.01.010 (2011).
Gerlai, R., Lahav, M., Guo, S. & Rosenthal, A. Drinks like a fish: zebra fish (Danio rerio) as a behavior genetic model to study alcohol effects. Pharmacology, biochemistry, and behavior 67, 773–782 (2000).
Gerlai, R., Lee, V. & Blaser, R. Effects of acute and chronic ethanol exposure on the behavior of adult zebrafish (Danio rerio). Pharmacology, biochemistry, and behavior 85, 752–761, https://doi.org/10.1016/j.pbb.2006.11.010 (2006).
Acknowledgements
This work was supported by the National Institute of Health Grants RO1AA020265 (S.-Y.C.), RO1AA021434 (S.-Y.C.), P50AA024337 (S.-Y.C.), and RO1AA023190 (W.F.) from the National Institute on Alcohol Abuse and Alcoholism, RO1AR063630 (X.W.) from the National Institute of Arthritis and Musculoskeletal and Skin Diseases, Excellent Young Scientist Foundation of Zhejiang Provincial People’s Hospital ZRY2016A002 (X.C.), and 81701460 (X.C.) from the National Natural Science Foundation of China.
Author information
Authors and Affiliations
Contributions
K.W., X.C. and J.L. performed experiments and participated in experimental design, data analysis and manuscript preparation. L.Z., W.F., L.C., and X.W. participated in data interpretation and discussion. S.C. conceptualized and designed the experiments, and participated in data interpretation and manuscript preparation. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, K., Chen, X., Liu, J. et al. Embryonic exposure to ethanol increases the susceptibility of larval zebrafish to chemically induced seizures. Sci Rep 8, 1845 (2018). https://doi.org/10.1038/s41598-018-20288-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-20288-2
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.