Abstract
We searched PubMed for primary research quantifying drug modification of light-induced circadian phase-shifting in rodents. This search, conducted for work published between 1960 and 2018, yielded a total of 146 papers reporting results from 901 studies. Relevant articles were those with any extractable data on phase resetting in wildtype (non-trait selected) rodents administered a drug, alongside a vehicle/control group, near or at the time of exposure. Most circadian pharmacology experiments were done using drugs thought to act directly on either the brain’s central pacemaker, the suprachiasmatic nucleus (SCN), the SCN’s primary relay, the retinohypothalamic tract, secondary pathways originating from the medial/dorsal raphe nuclei and intergeniculate leaflet, or the brain’s sleep-arousal centers. While the neurotransmitter systems underlying these circuits were of particular interest, including those involving glutamate, gamma-aminobutyric acid, serotonin, and acetylcholine, other signaling modalities have also been assessed, including agonists and antagonists of receptors linked to dopamine, histamine, endocannabinoids, adenosine, opioids, and second-messenger pathways downstream of glutamate receptor activation. In an effort to identify drugs that unduly influence circadian responses to light, we quantified the net effects of each drug class by ratioing the size of the phase-shift observed after administration to that observed with vehicle in a given experiment. This allowed us to organize data across the literature, compare the relative efficacy of one mechanism versus another, and clarify which drugs might best suppress or potentiate phase resetting. Aggregation of the available data in this manner suggested that several candidates might be clinically relevant as auxiliary treatments to suppress ectopic light responses during shiftwork or amplify the circadian effects of timed bright light therapy. Future empirical research will be necessary to validate these possibilities.
Similar content being viewed by others
Introduction
The suprachiasmatic nucleus (SCN), the central circadian pacemaker in mammals, integrates the stimulus information it receives from daily patterns of light exposure to align the phase-positioning of every organ and tissue collective in the body [1]. Over the past 50 years, the underlying pharmacology that shapes the magnitude and direction of these phase-shifting responses has been investigated almost exclusively in rodents and almost exclusively in piecemeal fashion, probing the isolated effects of one receptor manipulation in any one experiment. Efforts to synthesize this literature are lacking by comparison. Here, we report results from a systematic review of the complete rodent circadian-pharmacology literature up to 2017–2018. The objective was to quantify the relative contributions of different neurotransmitter systems to the circadian pacemaker’s photic resetting and identify clinically meaningful drug targets that might be tested in humans as countermeasures for situations such as shiftwork. With rotating or fixed-night schedules, shiftworkers are exposed to many competing light signals in the morning and throughout the day in their time off [2, 3]. These signals can interfere with the SCN’s interpretation of day versus night, with downstream effects that include: (1) disrupting the robustness of the sleep-wake cycle [4, 5], (2) suppressing melatonin synthesis [6], and (3) possibly seeding conditions linked to the immune-weakening effects of chronic melatonin suppression such as cancer [7, 8]. Identifying drugs that can augment light responses at night and minimize light responses during the day has the potential to strengthen the sleep-wake rhythms of night workers (e.g., nurses, public safety personnel [9]), with beneficial effects extending to many areas of mental and physical health [10,11,12].
Materials and methods
Literature search
We used a two-stage search strategy to collate published research related to the combinatory effects of light exposure and drug administration on phase shifts of the rodent circadian activity rhythm. The first stage was done by querying PubMed with the following terms connected by the Boolean operators AND/OR: “circadian,” “phase shift,” “light,” “photic,” “rodent,” “mouse,” “hamster,” and “rat.” This survey resulted in the identification of 232 unique publication hits. For the second step of the search, the “related articles” feature on PubMed was consulted to conduct secondary reviews of all papers associated with the hits. Each publication prompted 120 cross references (on average), producing a candidate pool of approximately 28,000 additional articles. All the abstracts from this pool were scanned for content related to light-induced phase shifting, with further consideration given to articles describing any pharmacology work. Records were independently screened by one of the three authors without the assistance of automation tools. From May 23rd to December 6th, 2017, a total of 146 papers were ultimately incorporated into the study database. Citations for these articles are alphabetically organized within Appendix A.
Inclusion-exclusion criteria and data extraction
Relevant articles were those with any extractable data on photic resetting enumerated within the main text or tables or those illustrated within a scatter plot or column graph. For inclusion, papers had to report: 1. Results from wildtype (non-trait selected) mice, hamsters, or rats; 2. Results from a group of vehicle-treated animals alongside a group of drug-treated animals; 3. Delivery of a single light pulse—of defined illuminance and duration—within a four-hour time window during the subjective night (CT12 to CT24); and 4. Use of activity rhythms (e.g., via running wheel or infrared monitoring) as circadian phase markers. Articles were excluded from further consideration if they did not meet all the aforementioned criteria or if phase-shifting data could not be unambiguously extracted from the manuscript’s figures. Where available, data were gathered from the Methods sections and from the tables of the Results sections. When data were presented within graphs, the XY Scan program (http://rhig.physics.yale.edu/~ullrich/software/xyscan/) was used to extract the timing of the light pulse and the magnitude of the resulting phase shift. Feedstock data that were introduced into the analysis plan were ultimately derived from studies that measured a phase-shift of the locomotor activity rhythm after light exposure sometime between CT12 and CT24; in nearly all cases, the animals used in these experiments had been housed under constant darkness. To maximize the amount of data available and best visualize trends in drug responses, data were compiled from animals exposed to light during either the first (CT12-CT18) or second-half (CT19-CT24) of the subjective night. At either time, light exposure produces a phase-shift of endogenous and observed rhythms but the directionality of the shift changes: delays are produced in the first-half of the subjective night, while advances are typically produced in the latter half [13] in accordance to the rodent phase-response curve (PRC) to light [14, 15]. Among the caveats with this all-inclusive approach is that neurotransmitter effects on “delays” versus “advances” cannot be distinguished. Another caveat in the current study was that data were drawn/aggregated from animals without regards to the characteristics of the light emission (e.g., intensity, spectrum) that was used to elicit phase resetting. Finally, it is important to note that light or glutamate stimulation can modulate phase-shifts triggered by non-photic, arousal stimuli delivered between CT0 and CT12 [16,17,18,19], the daytime window opposite the nighttime one that is considered here. Non-photic phase responses associated with novel wheel running [20], sleep deprivation [21], or NYP injections [22, 23] are all counteracted by bright light exposure during the subjective day or subsequent administration of glutamate to the SCN in vitro [24].
Analysis plan
The first part of the review consisted in developing a brief descriptive summary of the 146 papers in the study database. The following parameters were calculated:
-
(1)
percentage breakdown of studies involving drugs targeting one of the four major neurotransmitter systems operating within the SCN, including glutamate, GABA, serotonin, and acetylcholine (a dot plot of these data is available in Fig. 1A), and
Fig. 1: Drug modulation of light-induced circadian phase shifting. A Percentage of studies conducted over the past half-century targeting different receptor classes operating within the glutamate, GABA, 5-HT, or acetylcholine transmitter systems. The total number of studies canvassed is indicated to the right of each dot plot. B Number of studies in the phase-shifting literature broken down by the hour of the subjective night when combined drug and light exposure were tested. Drugs grouped by those targeting or exerting effects as: A = AMPA/kainate receptors; B = NMDA receptors; C = mGluRs; D = GABA agonists; E = GABA antagonists; F = 5-HT agonists; G = 5-HT antagonists; H = 5-HT mixed agonist/antagonists; I = nicotinic receptors; and J = muscarinic receptors.
-
(2)
breakdown in the hourly intervals across the subjective night from CT12 to CT24 that the effects of light and drug administration were measured in tandem (a heatmap of these data is available in Fig. 1B).
The second part of our investigation analyzed light-induced phase-shifting data by drug class. The average phase-shift (hours) that a cohort of animals exhibited after administration of each drug was ratioed against the average response made by a control batch of animals shown the same light stimulus but given vehicle instead (i.e., [magnitude of light-induced phase-shift after drug administration in a particular study] / [magnitude of light-induced phase-shift after vehicle administration in that same study]). These rationed values were then organized according to the drug’s purported mechanism of action (e.g., all the ratios from cohorts receiving an “NMDA receptor antagonist” in the study database were grouped together for subsequent analyses, likewise for those receiving a “GABAA agonist” or “5-HT1A antagonist”, etc). Ratios settling above a value of 1 indicated that a particular drug class potentiated circadian responses to light. Alternatively, values falling under 1 indicated that it suppressed light responses. The performance of each drug class was evaluated by a one-sample t test to determine whether the net shift it produced relative to vehicle was statistically different than one, a score which indicates no changes in phase movements beyond those attributable to light exposure alone. Significance was set at P = 0.05 (two-tailed). In the Results section, please note that these ratios are sometimes used to infer percentage changes in the size of a light-induced phase-shift produced by a particular drug class. For example if a phase-shift to light exposure was on average 1.3-fold greater in groups of mice receiving a particular type of drug compared to vehicle, then we refer to that drug as increasing the phase-shift response by 30%.
Results
Together, glutamate and γ aminobutyric acid (GABA) comprise the SCN’s most elemental neurotransmitter systems [25,26,27,28,29,30,31,32]. Their positioning atop this signaling hierarchy has motivated 274 circadian pharmacology studies combined over the past several decades (Fig. 1A), most of which were conducted at times during the subjective night when light exposure generates the largest delay (CT13-14) or advance shifts (CT18-19) of the locomotor activity rhythm in mice, rats, and hamsters (Fig. 1B). While several neural circuits regulate the phase of the SCN, the retinohypothalamic tract (RHT) provides the most direct modulation, originating from retinal ganglion cells co-expressing glutamate and pituitary adenylate cyclase-activating peptide (PACAP) [33,34,35,36,37,38,39,40,41]. The RHT forms monosynaptic connections onto terminal fields of the SCN located within the ventrolateral core region, translating photic information that the retina receives into changes in glutamatergic transmission from within the SCN [42, 43]. This target area is enriched for vasoactive intestinal peptide (VIP) positive cells expressing NMDA-type and AMPA/kainate type excitatory amino acid receptors [44,45,46,47,48,49,50,51,52,53,54,55,56], as well as L-type calcium channels [57].
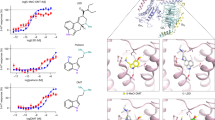
The RHT is obligatory for light-induced phase-shifting [58]. Blocking its activity with AMPA, kainate, or NMDA receptor antagonists significantly reduces the magnitude of circadian responses. On the other hand, amplifying activity with AMPA receptor positive allosteric modulators (e.g., aniracetam) enhances responses beyond those achieved with light exposure alone (Fig. 2A). Drugs that act at Type I-III metabotropic glutamate receptors also impart functional changes in the SCN [59,60,61]. Agonists and antagonists of the mGluR2/3 receptor decrease and potentiate light-induced phase-resetting, respectively. mGluR5 antagonists also seem to have potentiating effects (Fig. 2A). The literature concerning glutamate and the SCN suggests that one of the most direct ways of modulating light-induced phase-shifting is at the connection point between retinal photoreception and SCN signaling.
Data are compiled from individual experiments. Each data point reflects the average phase response made by a group of drug-treated animals rationed against the average response made by a control group of vehicle-treated animals assessed at the same time (with the same light stimulus) within the same experimental series. Asterisks indicate phase movements that were statistically lower or higher than baseline (broken dotted line) when testing the average phase-shift ratio observed across studies associated with each drug category against an expected value of 1 (no change). Number of studies for each drug category, (A): AMPA PAM, n = 8; AMPA/Kainate Antagonist, n = 8; NMDA Antagonist, n = 71; mGluR1/2 Agonist, n = 2; mGluR2/3 Agonist, n = 15; mGluR5 agonist, n = 11; mGluR2/3 Antagonist, n = 7; mGluR5 Antagonist, n = 12; (B): GABAA Agonist, n = 69; GABAB Agonist, n = 12; GABAA Antagonist, n = 20; GABAB Antagonist, n = 2; CK1epsilon Inhibitor, n = 4; mPer1/Per2 Antagonist, n = 13; (C): SSRI, n = 21; Lithium Compound, n = 6; Clorgyline, n = 5; 5HT2C Agonist, n = 2; 5HT2A Agonist, n = 2; 5HT1B Agonist, n = 22; 5HT1A/7 Agonist, n = 24; 5HT1A Agonist, n = 13; (D): 5HT1 Antagonist, n = 1; 5HT1A Antagonist, n = 21; 5HT1B Antagonist, n = 4; 5HT2/7 Antagonist, n = 13; 5HT5A Antagonist, n = 4; 5HT6 Antagonist, n = 3; 5HT1A Mixed Agonist/Antagonist, n = 36; 5HT1A Antagonist + 5HT1B Agonist, n = 3; (E): nAChRalpha7 Agonist, n = 12; nAChRalpha7 Antagonist, n = 15; M4PAM, n = 10; Muscarinic Receptor Agonist, n = 6; Muscarinic Receptor Agonist and Antagonist, n = 1; Muscarinic Agonist + Antagonist + M4PAM, n = 1; Muscarinic Receptor Antagonist, n = 6; (F): Dopamine Agonist, n = 17; Noradrenaline Agonist, n = 7; H1 Antagonist, n = 5; H2 Antagonist, n = 7; H3 Antagonist, n = 4; and Histidine Decarboxylase Inhibitor, n = 2. *P < 0.05, one sample t test.
Nearly all neurons inside the SCN proper use GABA as their predominant neurotransmitter [32, 62,63,64,65,66,67,68,69]. GABA-elicited postsynaptic currents can be hyperpolarizing (inhibitory) or depolarizing (excitatory) depending on the neuron’s baseline intracellular chloride concentration set by the relative expression level of Na-K-2Cl cotransporter 1 (NKCC1) versus K-Cl cotransporter 2 (KCC2) [70,71,72,73]. NKCC1 mediates Cl- uptake and accumulation, establishing a more negative membrane potential upon opening [71, 74]. Conversely, KCC2 opening mediates Cl- extrusion, thereby depolarizing the membrane potential [75]. The polarity of SCN GABAergic signaling is shaped by an interplay of developmental [76,77,78], physiological [79], time-of-day [80,81,82,83,84,85], and seasonal factors [86,87,88]. In combination, these factors influence the degree to which GABA synchronizes or desynchronizes pacemaker neurons and the amplitude of the SCN’s output signal [81, 89,90,91,92,93,94].
Given the highly dynamic nature of this transmitter gating, it is perhaps not surprising that both agonists and antagonists of the ionotropic GABAA receptor interfere with light-induced phase-resetting (Fig. 2B). In the case of GABAA antagonists, opposing effects are also possible based on whether the drugs are given systemically or directly infused within the SCN (Supplementary Fig. 1) [95]. Adding to the complexity still further, the phase-shifting effects of GABAA receptor activation may also depend on whether these receptors are stimulated acutely or in a sustained fashion [96].
Arguably, GABAB receptors provide a more parsimonious route for regulating circadian responses by virtue of their localization as presynaptic autoreceptors on RHT terminals [75, 97,98,99,100,101,102]. Activation of them inhibits voltage-gated Ca2+ channels [101, 103], thereby decreasing RHT glutamate release and behavioral shifts to light exposure (Fig. 2B). The scale of glutamate and GABA’s effects on SCN light responses (from near total abrogation to threefold enhancement) exceeds the effects observed when manipulating the molecular clock mechanism (Fig. 2B, right side of divided plot). Considered in full, the literature on SCN GABA suggests that GABAergic drugs are particularly effective at modulating circadian light responses. However, owing to changes in the polarity of this transmitter system along with other nuances, the effects of GABAA agonists or antagonists may not be immediately predictable. GABAB receptor agonists, by comparison, offer clearer applicability for minimizing circadian light resetting because their activation is directly tied to reductions in RHT activity.
The single largest corpus of work vis-à-vis circadian pharmacology (n = 219 studies) has examined manipulations of serotonin (5-hydroxytryptamine, 5-HT) (Fig. 1A). These assessments have been conducted at times of night consistent with when evaluations have been done on the glutamatergic and GABAergic systems (Fig. 1B). Retinal ganglion cells contributing to the circadian system send bifurcated axons to the SCN as well as other brain regions maintaining reciprocal connections with the central pacemaker, including the median and dorsal raphe nuclei [104,105,106,107,108,109,110]. Both raphe nuclei innervate the SCN with mixed serotonergic and nonserotonergic projections, although the dorsal raphe likely uses the intergeniculate leaflet (IGL) as a relay [107, 111,112,113,114]. The role of serotonin in light-induced phase-shifting has been debated since experimentation began [115]. The bulk of data suggest that 5-HT afferents convey information to the SCN about an animal’s behavioral state, particularly as it relates to sleep and arousal [116,117,118,119]. Acting through a bevy of presynaptic 5-HT autoreceptors and postsynaptic 5-HT receptors, serotonin conveys an arousal signal to the SCN that minimizes its responses to incoming light signals at the molecular [120, 121], cellular [121,122,123,124], and behavioral [125] level. An alternative corpus of work suggests that these non-photic effects might be phase dependent, or reversed, depending on the mix of 5-HT presynaptic and postsynaptic that are stimulated and/or blocked [126,127,128,129,130,131,132].
General enhancement of serotonin with serotonin selective reuptake inhibitors (SSRIs) or monoamine oxidase inhibitors (e.g., clorgyline) diminishes light-induced phase resetting (Fig. 2C). Divergent effects can be achieved, however, with drugs preferentially targeting one specific 5-HT receptor pathway or another. Depending on the subtype that is activated and where it is expressed in the SCN, 5-HT drugs either increase or decrease phase-shifting. For example, 5HT1B receptor agonists greatly impair circadian responses made to acute light exposure (by an average of 70% across studies; Fig. 2C). The effect is likely mediated by 5HT1B receptors expressed presynaptically on RHT terminals; When these autoreceptors are activated, they inhibit glutamate transmission from the RHT to the SCN [133,134,135,136,137,138].
Further nuances can be found in two separate 5HT1A pathways. One is formed by 5HT1A receptors expressed postsynaptically on SCN neurons in target areas that are innervated by the median/dorsal raphe nuclei [125, 139, 140]. The other is formed by 5HT1A receptors that are expressed somatodendritically as autoreceptors on the raphe neurons themselves [141, 142]. Depending on which 5-HT receptor population an agonist is preferential for, phase shifts to light are either reduced or potentiated (Fig. 2C, last column of data points). In the case of agonists active at raphe-neuron 5HT1A autoreceptors, potentiation occurs at a level similar to that observed with AMPA positive allosteric modulators (i.e., two or threefold enhancement; Fig. 2A).
In contrast to 5HT1A agonists targeting SCN postsynaptic receptors, 5HT1A postsynaptic antagonists amplify light responses. The amplification is similar to that achieved with 5HT1A agonists targeting raphe-neuron autoreceptors (Fig. 2C, D). 5HT1A mixed agonist/antagonists, parlaying the complex expression dichotomy for 5HT1A receptor subtypes in the SCN circuitry, also enhance light-induced phase-shifting [143,144,145,146,147,148]. The pattern of all these 5HT1A-related effects is consistent with the general notion that serotonin signaling from the raphe nuclei normally serves to impair the SCN’s light responses. Light-induced phase shifting can thus be enhanced when the serotonin signal is weakened by either: (1) stimulating raphe-neuron 5HT1A autoreceptors or (2) blocking 5HT1A postsynaptic receptors expressed by SCN neurons (Fig. 2C, D). Conversely, photic resetting can be counteracted by strategies that boost the serotonin signal, such as: (1) blocking raphe-neuron 5HT1A autoreceptors or (2) stimulating 5HT1A postsynaptic receptors on SCN neurons (Fig. 2C, D).
A smaller corpus of work (n = 51 studies) has characterized the role of acetylcholine in the central pacemaker’s responses to light across the most sensitive areas of the delay and advance zones (Fig. 1A, B). The SCN is innervated by several brain regions involved with sleep-wake regulation, among them the basal forebrain and the pedunculopontine and lateral dorsal tegmentum nuclei implicated in the maintenance of rapid eye movement (REM) sleep [149,150,151,152]. These cholinergic afferents are likely involved with arousal-driven phase shifts of the SCN’s rhythm and, as such, a point of entry for crosstalk between the sleep/wake and circadian timekeeping systems. Blockade of α7 nicotinic receptors reduces the magnitude of light-induced phase shifts by about 50%. A similar effect is observed when stimulating muscarinic receptors (including the M4 subtype; Fig. 2E), but the underlying neurophysiology mediating these responses remains ill-defined despite previous detection of both acetylcholine receptor classes within the SCN [153,154,155,156,157,158,159,160,161]. Given the unknowns in cholinergic signaling [159], drugs targeting nicotinic or muscarinic receptors may not be prime candidates for regulating circadian light responses.
Newer work has highlighted an unexpected role for dopamine (DA) in modulating adult SCN function and photoentrainment beyond a developmental window historically thought to restrict SCN sensitivity to the neurotransmitter [162,163,164,165]. DA cells from the ventral tegmental area of adult rodents connect directly to the SCN to set the pace of reentrainment following several-hour displacements of the prevailing LD cycle [166]. A few investigations have also examined the effects of dopaminergic drugs on phase-shifting. They have centered on common drugs of abuse such as cocaine and methamphetamine [167,168,169,170], which act by inhibiting the DA transporter in addition to other monoamine transporters for noradrenaline and serotonin [171, 172]. Whilst changes in DA signaling are likely to contribute to the circadian effects of cocaine and methamphetamine, extant data suggest that enhancement of serotonin signaling is likewise involved and may in fact be the primary mechanism by which monoamine transport blockers modulate the SCN [169]. In keeping with this suggestion, DA stimulants decrease the size of light-induced phase shifts (Fig. 2F). Drugs directly modifying other monoamine systems such as noradrenaline or those altering signaling pathways associated with the arousal neurotransmitter, histamine, elicit either little or no tangible effect (Fig. 2F). Interestingly, among the neurotransmitters in the brain’s wake-promoting circuitry, it appears that only serotonin, acetylcholine, and dopamine are in a position to influence the SCN’s phase-shifting responses to light exposure.
The raphe nuclei are not the only retinorecipient brain regions that send information regarding arousal and physiological state to the SCN so as to modify circadian light responses. Retinal ganglion cells also convey information to the SCN via an auxiliary route running through the IGL of the thalamus and the geniculohypothalamic tract (GHT) [173, 174]. The IGL is comprised of neurons expressing neuropeptide Y (NPY) [175,176,177,178,179,180]. Analogous to how serotonin operates through the median raphe nucleus, NPY neurons of the IGL provide a check on the resetting effects of light on SCN phase (likely by suppressing SCN responses to retinal input) [23, 181,182,183,184,185,186,187,188,189,190,191,192]. Accordingly, NPY agonists attenuate light-induced phase shifts (Fig. 3A), while antagonists raise the response ceiling about twofold. The enhancement with NPY antagonists exceeds what is observed with many of the remaining factors previously shown to modulate the SCN’s phase-shifting drive (Fig. 3A–E). IGL cells expressing enkephalin are smaller signaling elements of this circuitry [193], yet they likewise discourage light-induced responses when binding δ-opioid receptors located on RHT presynaptic terminals [179, 194, 195]. Drug agonists or antagonists of mu (μ) and kappa (κ) opioid receptors do not appear to influence circadian resetting one way or another (Fig. 3D).
A–E The impairing or enhancing effects of other drug classes on light-induced phase-shifting. Data are compiled from individual experiments. Each data point reflects the average phase response made by a group of drug-treated animals rationed against the average response made by a control group of vehicle-treated animals assessed at the same time (with the same light stimulus) within the same experimental series. Asterisks indicate phase movements that were statistically lower or higher than baseline (broken dotted line) when testing the average phase-shift ratio observed across studies associated with each drug category against an expected value of 1 (no change). *P < 0.05, one sample t test.
Another transmitter that has been studied in the context of the SCN’s light responses is adenosine. It is one of the chemical signals that mediates the homeostatic effects of prolonged wakefulness [196,197,198,199,200,201]. When energy expenditure in the brain exceeds production after daylong periods of activity, ATP released from astrocytes is degraded by ectonucleotidases, accumulating in the extracellular space as adenosine [198, 202,203,204]. At threshold concentrations, adenosine then binds to receptors within the basal forebrain and ventrolateral preoptic nucleus to facilitate sleep induction [199, 205, 206]. Within the SCN, adenosine also acts on retinorecipient areas of the ventrolateral core to suppress light-induced RHT activity. Here, stimulation of adenosine A1 receptors limits intracellular buildup of Ca2+, thereby reducing excitatory synaptic transmission [207,208,209,210,211,212]. These physiological effects are manifested at the behavioral level, where adenosine A1 receptor agonists curtail light-induced shifts of the locomotor activity rhythm by ~60%. Stimulation of other adenosine receptor subtypes A2 and A3 are without effect (Fig. 3C). The broader context for these data suggests that the adenosine pathway connects sleep homeostatic processes to circadian timekeeping. Through its encoding of sleep-wake history, such signaling is thought to coordinate with the SCN’s photic responses in order to optimize an animal’s sleep timing relative to the light transitions of the LD schedule [213].
Relative to other transmitter systems, the brain’s cannabinoid system has been understudied owing to historical roadblocks set in place by U.S. drug agencies. However, the SCN expresses receptors for endogenous cannabinoids along the axons of its resident population of GABAergic neurons. Activation of the major subtype, cannabinoid receptor 1, decreases GABA release from presynaptic terminals, thus freeing target neurons from tonic inhibition and elevating postsynaptic activity in circuits intrinsic to the SCN [214,215,216,217,218]. Cannabinoids may impart other changes to SCN excitability by coordinating astrocytic release and extracellular accumulation of adenosine [219]. In keeping with the predicted functional consequences of elevated adenosine, cannabinoid receptor agonists greatly reduce the magnitude of phase-shifts made to acute light exposure by 80% on average (Fig. 3B). No other pharmacological manipulation appears to be as effective at inhibiting circadian light responses. As such, exogenous cannabinoids and synthetic cannabinoid antagonists are worthy of further study as possible drug regulators of circadian light responses.
Transmitter systems with a more ambiguous role in SCN signaling have also been evaluated for their effects on light-induced phase-shifting. The SCN evinces a distinct margin of cells expressing neurokinin 1 (NK1) receptor just inside and extending to just outside its dorsolateral border [220]. This receptor binds Substance P. Unlike PACAP, Substance P’s incorporation within the RHT has been difficult to resolve in studies looking to generalize the peptide’s optic-tract anatomy and function across mammalian species [220,221,222]. In any circumstance, Substance P binding to NK1 receptor is likely a redundant mechanism that conveys photic input to the SCN. Commensurate with this notion, NK1 antagonists elicit small, but significant reductions in light-induced phase-shifting (Fig. 3E). The marginal effect of Substance P on SCN light responses stands in contrast to the more substantial effects that have been characterized with other neuropeptides and hormones, including corticotropin-releasing factor (CRF) and oxytocin.
The SCN maintains reciprocal connections with the paraventricular nucleus of the hypothalamus (PVH) [223, 224]. These nuclei coordinate the SCN’s output signal to maintain daily rhythms in melatonin secretion and glucocorticoid production via timed daily release of CRF [225,226,227]. Oxytocin, a hormone known for its contributions to reproduction and social bonding, also bridges each nucleus [228,229,230]. Magnocellular neurosecretory cells of the PVH are one of the principal sites of oxytocin synthesis in the brain and both the SCN and PVH express oxytocin receptors [228, 231,232,233]. Interference with either CRF or oxytocin transmission dampens the magnitude of pacemaker shifts mobilized by light (Fig. 3E). These effects may comprise part of a negative feedback mechanism related to stress and/or a zeitgeber input related to social interaction that modulates the SCN’s photic responses [234]. Without further research, however, these possibilities remain speculative.
Within the SCN, synchronization is effected by neuropeptides such as Gastrin-releasing peptide (GRP; a homolog of bombesin). GRP localizes to the SCN ventral retinorecipient zone and may operate as a photic resetting signal within and between SCN subdivisions [235,236,237,238,239,240,241,242,243]. GRP binds bombesin 2 (BB2) receptors [244,245,246], which exhibit a complex pharmacology amenable to drugs acting as antagonists as well as partial agonists [247,248,249]. Administration of BB2 drugs with partial agonist activity, a maneuver that likely facilitates GRP signaling, leads to corresponding increases in light-induced phase-shifting (Fig. 3E). The enhancement is similar to that observed after more direct manipulations of the molecular clock mechanism (Fig. 2B). In contrast to GRP, pharmacologic manipulations of other synchronization agents in the SCN, such as vasoactive intestinal peptide (VIP), show little effect (Fig. 3E). As previously suggested [249], VIP’s ability to phase-shift the central pacemaker when applied to the SCN without light administration [250] might be overshadowed when light is directly used to change the SCN’s phase. Changing circadian light responses by augmenting/reducing VIP activity alone might also be futile if there are any signaling redundancies between GRP and VIP [249].
More reductionistic work has examined molecular pathways in SCN neurons that tie glutamate receptor activation to changes in clock gene expression. Dose-dependent activation of AMPA and NMDA receptors via drug agonists, broad-spectrum light, or site-specific electrical stimulation of the RHT mobilizes intracellular Ca2+ entry [57, 251, 252]. Calcium accumulation then triggers phosphorylation of cAMP response element binding protein (CREB) [253,254,255,256,257] and induction of immediate-early genes such as c-fos and jun-B [258,259,260,261]. CREB transcriptional activity is driven through several convergent second-messenger pathways, including those anchored by protein kinase A (PKA) [262], calcium/calmodulin dependent kinase II (CaMKII) [263, 264], and mitogen-activated protein kinase (MAPK) [265,266,267]. Upstream, Ca2+ entry also triggers nitric oxide (NO) production from nitric-oxide synthase [268,269,270], stimulating cGMP production [271,272,273] and protein kinase G (PKG) activity [274, 275].
Photic stimulation couples to SCN entrainment by way of all these signaling dynamics [276, 277]. Interruption of any one step can attenuate transcriptional activation of clock genes (i.e., Per1 and Per2) and phase-shifts made in response to light exposure (Fig. 4). On the other hand, driving these signaling pathways can produce more robust circadian responses to light, as exemplified by experiments with clinically relevant phosphodiesterase 5 inhibitors preventing the degradation of cGMP (Fig. 4). Drugs regulating the accumulation of cAMP or cGMP in SCN neurons post light treatment might represent a subtle way by which to titrate the SCN’s phase-shifting response to light exposure.
Data are compiled from individual experiments. Each data point reflects the average phase response made by a group of drug-treated animals rationed against the average response made by a control group of vehicle-treated animals assessed at the same time (with the same light stimulus) within the same experimental series. Asterisks indicate phase movements that were statistically lower or higher than baseline (broken dotted line) when testing the average phase-shift ratio observed across studies associated with each drug class (e.g., Tyrosine Kinase Inhibitors, TTX, etc) against an expected value of 1 (no change). *P < 0.05, one sample t test.
A final pocket of limited work has evaluated how energy metabolism may factor into the SCN’s photic resetting [181, 278,279,280]. Outside of direct considerations of food entrainment or timing/mistiming of food intake, available data suggest that administration of agents signaling low energy status, such as agonists of the “appetite” hormone ghrelin or glycolysis inhibitors, can reduce phase-shifts made to light exposure. By contrast, those signaling high energy status, as achieved through direct infusion of glucose or the “satiety” hormone leptin, boost light-induced phase-shifting (Fig. 5). Whether such a low-versus-high metabolic dichotomy operates endogenously to calibrate the SCN’s photic responses (e.g., by way of acute dietary fasting or food overconsumption) is currently unknown and requires empirical study.
Data are compiled from a limited number of individual experiments. Each data point reflects the average phase response made by a group of drug-treated animals rationed against the average response made by a control group of vehicle-treated animals assessed at the same time (with the same light stimulus) within the same experimental series. Asterisks indicate phase movements that were statistically lower or higher than baseline (broken dotted line) when testing the average phase-shift ratio observed across studies associated with each drug class (e.g., Ghrelin agonists, Insulin, etc) against an expected value of 1 (no change). *P < 0.05, one sample t test.
Discussion
In the current systematic review, we have summarized the role of different neurotransmitter systems in the SCN’s phase-shifting responses to light. Pulling together rodent studies employing different drug classes up to 2017–2018, we found that most investigation focused on neurotransmitters expressed within the SCN proper (e.g., GABA) or those used by SCN afferents with defined points of origin in the eye or brain, including glutamate, serotonin, acetylcholine, and NPY. The remaining experiments characterized a mix of newer and older factors that may modulate SCN light responses, such as endogenous cannabinoids, the sleep-homeostatic signal adenosine, as well as signal transduction pathways that pair RHT activity to changes in clock gene expression within SCN neurons. Extant data suggest there are many avenues by which to amplify or diminish the central pacemaker’s light responses. These avenues are equally visible in traditional laboratory rodents as well as less commonly used diurnal rodents such as grass rats. In African grass rats, just as in mice or hamsters, GABAA and GABAB agonists reduce the size of phase shifts made to nighttime light exposure [84, 281], while adenosine antagonists potentiate phase-shifting [282].
For human application, the selection of one particular drug class or another may depend on the strategies that are implemented to optimize sleep-wake rhythms. For example, different strategies might be called on to optimize circadian function in workers with fixed-night schedules versus shiftworkers exposed to rapidly changing photic cycles, such as airline pilots and flight attendants. In the case of night workers, one pattern of use is conceivable. To maximize the zeitgeber strength of nighttime light exposure, individuals could use drug classes that potentiate circadian light responses during their shifts, including 5HT1A autoreceptor agonists or phosphodiesterase 5 (PDE5) inhibitors. To assure that alertness is maintained during working hours, particular emphasis might be placed on taking PDE5 inhibitors such as Sildenafil [283], which is already approved by the U.S. Food and Drug Administration (FDA) for acute treatment of erectile dysfunction [284]. Other investigational PDE5 inhibitors are being developed for the treatment of cognitive disorders [285]. Advancements in medicinal chemistry might thus lead to other structural variations of PDE5 inhibitors that are tailored to keep night workers at peak cognitive performance while potentiating the zeitgeber strength of the prevailing light environment.
Upon ending their shifts in the morning, night workers might then transition to drugs that will prevent unwanted phase shifts to light, including GABAB, 5HT1B, and cannabinoid receptor agonists. For individuals that sleep during the day, a secondary consideration might also involve whether the drug facilitates sleep. With that added criterion, GABAB and cannabinoid receptor agonists would be better candidates than 5HT1B agonists [216]. GABAB receptor agonists cause sedation and promote sleep [286]. Humans have historically used external cannabinoids like THC (tetrahydrocannabinol) from marijuana and cannabidiol oil from hemp as recreational drugs. Though research on sleep and cannabinoids is still in its infancy, preliminary data suggest that THC can reduce sleep latency, reduce nightmares, and improve sleep quality in the presence of chronic pain [287]. Future experiments might test whether different dose schedules, and prioritizing oral intake versus inhalation, can separate cannabinoids’ effects on sleep-wake rhythms versus their better-known psychogenic properties.
In the case of airline workers, travel itineraries often involve rapid transit through several time zones before returning home. Under this scenario, it may be advisable to keep the SCN of airline personnel in phase with the home time zone so that they can readjust quickly after their trip. It may also be advisable that they are as alert as possible while taking drugs that will neutralize light-induced phase shifts. With this in mind, 5HT1B agonists such as triptans (e.g., sumatriptan and zolmitriptan) might be realistic candidates [288]. Triptans are widely prescribed compounds approved by the FDA for the treatment of cluster headaches, migraines, and migraine-associated photophobia [289, 290]. Given their relatively long half-life of ~ 24 h and favorable adverse-effect profile, triptans could limit the deleterious circadian effects of jet travel when U.S. pilots are asked to fly to western Europe and back in the span of a few days.
All of the strategies conceptualized for night workers and airline personnel are borne out of the present review and the primary work preceding it. They require empirical clinical investigation to establish their efficacy. While these strategies remain speculative, they illustrate some of the secondary and tertiary considerations that factor into the use cases for taking one drug class or another to manage circadian light responses. Undoubtedly, other considerations could also be made regarding gender, age, as well as neurodevelopmental background.
While the present study is the first to tabulate the circadian pharmacology literature, it comes with a few caveats. First, data were aggregated from experiments employing different drug doses and different sites of administration. Thus, drug effects on light-induced phase-shifting may not be perfectly representative of what would be observed when dosages are optimized. Second, to achieve some semblance of statistical power and better visualize overall trends, data were aggregated from experiments conducted in the delay (first half) as well as advance zone (second half) of the subjective night. Circadian photic responses at the beginning of the night phase might be regulated differently than those occurring in the later hours before dawn. In all cases where applicable, we failed to note any general differences in drugs effects that could be attributable to the time of night when the experiments were conducted. Finally, data were aggregated from animals without regards to the characteristics of the light emission that was used to elicit phase resetting. It is possible that circadian photic responses are regulated differently based on the properties of the light exposure, including the emission’s spectrum, intensity, and duration.
The world faces unprecedented challenges to sleep and circadian health that are often met with single modality interventions rooted in either light exposure or drug treatment. The present systematic review establishes the range of neurotransmitter systems that influence the SCN’s photic responses and emphasizes that this light versus drug distinction might be a false dichotomy when thinking about potential treatments for shiftwork and the circadian disruptions associated with normative aging and chronic disease. More integrated therapies that look to synergize the effects of light exposure with FDA-approved drugs (or substances generally recognized as safe) might offer better performing treatment alternatives.
References
Morin LP. The circadian visual system. Brain Res Brain Res Rev. 1994;19:102–27.
Smith MR, Eastman CI. Shift work: health, performance and safety problems, traditional countermeasures, and innovative management strategies to reduce circadian misalignment. Nat Sci Sleep. 2012;4:111–32.
Folkard S. Do permanent night workers show circadian adjustment? A review based on the endogenous melatonin rhythm. Chronobiol Int. 2008;25:215–24.
Akerstedt T. Shift work and disturbed sleep/wakefulness. Occup Med (Lond). 2003;53:89–94.
Costa G. Sleep deprivation due to shift work. Handb Clin Neurol. 2015;131:437–46.
Razavi P, Devore EE, Bajaj A, Lockley SW, Figueiro MG, Ricchiuti V, et al. Shift Work, Chronotype, and Melatonin Rhythm in Nurses. Cancer Epidemiol Biomark Prev. 2019;28:1177–86.
Parent ME, El-Zein M, Rousseau MC, Pintos J, Siemiatycki J. Night work and the risk of cancer among men. Am J Epidemiol. 2012;176:751–9.
Hansen J, Stevens RG. Case-control study of shift-work and breast cancer risk in Danish nurses: impact of shift systems. Eur J Cancer. 2012;48:1722–9.
Fagundo-Rivera J, Allande-Cusso R, Ortega-Moreno M, Garcia-Iglesias JJ, Romero A, Ruiz-Frutos C, et al. Implications of lifestyle and occupational factors on the risk of breast cancer in shiftwork nurses. Healthcare. 2021;9:1–18.
Holst MM, Wirth MD, Allison P, Burch JB, Andrew ME, Fekedulegn D, et al. An analysis of shiftwork and self-reported depressive symptoms in a police cohort from Buffalo, New York. Chronobiol Int. 2021;38:830–38.
Holst MM, Wirth MD, Mnatsakanova A, Burch JB, Charles LE, Tinney-Zara C, et al. Shiftwork and biomarkers of subclinical cardiovascular disease: The BCOPS Study. J Occup Environ Med. 2019;61:391–96.
Samulin Erdem J, Noto HO, Skare O, Lie JS, Petersen-Overleir M, Reszka E, et al. Mechanisms of breast cancer risk in shift workers: association of telomere shortening with the duration and intensity of night work. Cancer Med. 2017;6:1988–97.
Kaladchibachi S, Fernandez F. Precision light for the treatment of psychiatric disorders. Neural Plast. 2018;2018:5868570.
Schwartz WJ, Zimmerman P. Circadian timekeeping in BALB/c and C57BL/6 inbred mouse strains. J Neurosci. 1990;10:3685–94.
Boulos Z, Terman JS, Terman M. Circadian phase-response curves for simulated dawn and dusk twilights in hamsters. Physiol Behav. 1996;60:1269–75.
Reebs SG, Mrosovsky N. Effects of induced wheel running on the circadian activity rhythms of Syrian hamsters: entrainment and phase response curve. J Biol Rhythms. 1989;4:39–48.
Mrosovsky N. Phase response curves for social entrainment. J Comp Physiol A. 1988;162:35–46.
Mead S, Ebling FJ, Maywood ES, Humby T, Herbert J, Hastings MH. A nonphotic stimulus causes instantaneous phase advances of the light-entrainable circadian oscillator of the Syrian hamster but does not induce the expression of c-fos in the suprachiasmatic nuclei. J Neurosci. 1992;12:2516–22.
Van Reeth O, Turek FW. Stimulated activity mediates phase shifts in the hamster circadian clock induced by dark pulses or benzodiazepines. Nature. 1989;339:49–51.
Yannielli PC, McKinley Brewer J, Harrington ME. Is novel wheel inhibition of per1 and per2 expression linked to phase shift occurrence? Neuroscience. 2002;112:677–85.
Grossman GH, Mistlberger RE, Antle MC, Ehlen JC, Glass JD. Sleep deprivation stimulates serotonin release in the suprachiasmatic nucleus. Neuroreport. 2000;11:1929–32.
Biello SM, Mrosovsky N. Blocking the phase-shifting effect of neuropeptide Y with light. Proc Biol Sci. 1995;259:179–87.
Maywood ES, Okamura H, Hastings MH. Opposing actions of neuropeptide Y and light on the expression of circadian clock genes in the mouse suprachiasmatic nuclei. Eur J Neurosci. 2002;15:216–20.
Biello SM, Golombek DA, Harrington ME. Neuropeptide Y and glutamate block each other’s phase shifts in the suprachiasmatic nucleus in vitro. Neuroscience. 1997;77:1049–57.
Ebling FJ. The role of glutamate in the photic regulation of the suprachiasmatic nucleus. Prog Neurobiol. 1996;50:109–32.
Albers HE, Walton JC, Gamble KL, McNeill JKT, Hummer DL. The dynamics of GABA signaling: Revelations from the circadian pacemaker in the suprachiasmatic nucleus. Front Neuroendocrinol. 2017;44:35–82.
Ding JM, Chen D, Weber ET, Faiman LE, Rea MA, Gillette MU. Resetting the biological clock: mediation of nocturnal circadian shifts by glutamate and NO. Science. 1994;266:1713–7.
Decavel C, Van den Pol AN. GABA: a dominant neurotransmitter in the hypothalamus. J Comp Neurol. 1990;302:1019–37.
Strecker GJ, Wuarin JP, Dudek FE. GABAA-mediated local synaptic pathways connect neurons in the rat suprachiasmatic nucleus. J Neurophysiol. 1997;78:2217–20.
van den Pol AN. Glutamate and GABA presence and action in the suprachiasmatic nucleus. J Biol Rhythms. 1993;8:S11–5.
Buijs RM, Hou YX, Shinn S, Renaud LP. Ultrastructural evidence for intra- and extranuclear projections of GABAergic neurons of the suprachiasmatic nucleus. J Comp Neurol. 1994;340:381–91.
Moore RY, Speh JC. GABA is the principal neurotransmitter of the circadian system. Neurosci Lett. 1993;150:112–6.
Hannibal J. Neurotransmitters of the retino-hypothalamic tract. Cell Tissue Res. 2002;309:73–88.
Chen D, Buchanan GF, Ding JM, Hannibal J, Gillette MU. Pituitary adenylyl cyclase-activating peptide: a pivotal modulator of glutamatergic regulation of the suprachiasmatic circadian clock. Proc Natl Acad Sci USA. 1999;96:13468–73.
Hannibal J, Ding JM, Chen D, Fahrenkrug J, Larsen PJ, Gillette MU, et al. Pituitary adenylate cyclase-activating peptide (PACAP) in the retinohypothalamic tract: a potential daytime regulator of the biological clock. J Neurosci. 1997;17:2637–44.
de Vries MJ, Nunes Cardozo B, van der Want J, de Wolf A, Meijer JH. Glutamate immunoreactivity in terminals of the retinohypothalamic tract of the brown Norwegian rat. Brain Res. 1993;612:231–7.
Meijer JH, van der Zee EA, Dietz M. Glutamate phase shifts circadian activity rhythms in hamsters. Neurosci Lett. 1988;86:177–83.
Meijer JH, Albus H, Weidema F, Ravesloot JH. The effects of glutamate on membrane potential and discharge rate of suprachiasmatic neurons. Brain Res. 1993;603:284–8.
Webb IC, Coolen LM, Lehman MN. NMDA and PACAP receptor signaling interact to mediate retinal-induced scn cellular rhythmicity in the absence of light. PLoS One. 2013;8:e76365.
Nielsen HS, Hannibal J, Knudsen SM, Fahrenkrug J. Pituitary adenylate cyclase-activating polypeptide induces period1 and period2 gene expression in the rat suprachiasmatic nucleus during late night. Neuroscience. 2001;103:433–41.
Gompf HS, Fuller PM, Hattar S, Saper CB, Lu J. Impaired circadian photosensitivity in mice lacking glutamate transmission from retinal melanopsin cells. J Biol Rhythms. 2015;30:35–41.
Mikkelsen JD, Larsen PJ, Mick G, Vrang N, Ebling FJ, Maywood ES, et al. Gating of retinal inputs through the suprachiasmatic nucleus: role of excitatory neurotransmission. Neurochem Int. 1995;27:263–72.
de Vries MJ, Treep JA, de Pauw ES, Meijer JH. The effects of electrical stimulation of the optic nerves and anterior optic chiasm on the circadian activity rhythm of the Syrian hamster: involvement of excitatory amino acids. Brain Res. 1994;642:206–12.
Stamp JA, Piggins HD, Rusak B, Semba K. Distribution of ionotropic glutamate receptor subunit immunoreactivity in the suprachiasmatic nucleus and intergeniculate leaflet of the hamster. Brain Res. 1997;756:215–24.
O’Hara BF, Andretic R, Heller HC, Carter DB, Kilduff TS. GABAA, GABAC, and NMDA receptor subunit expression in the suprachiasmatic nucleus and other brain regions. Brain Res Mol Brain Res. 1995;28:239–50.
Kallingal GJ, Mintz EM. An NMDA antagonist inhibits light but not GRP-induced phase shifts when administered after the phase-shifting stimulus. Brain Res. 2010;1353:106–12.
Wang LM, Schroeder A, Loh D, Smith D, Lin K, Han JH, et al. Role for the NR2B subunit of the N-methyl-D-aspartate receptor in mediating light input to the circadian system. Eur J Neurosci. 2008;27:1771–9.
Michel S, Itri J, Colwell CS. Excitatory mechanisms in the suprachiasmatic nucleus: the role of AMPA/KA glutamate receptors. J Neurophysiol. 2002;88:817–28.
Chambille I. Circadian rhythm of AMPA receptor GluR2/3 subunit-immunoreactivity in the suprachiasmatic nuclei of Syrian hamster and effect of a light-dark cycle. Brain Res. 1999;833:27–38.
Gannon RL, Rea MA. Glutamate receptor immunoreactivity in the rat suprachiasmatic nucleus. Brain Res. 1993;622:337–42.
Gannon RL, Rea MA. In situ hybridization of antisense mRNA oligonucleotides for AMPA, NMDA and metabotropic glutamate receptor subtypes in the rat suprachiasmatic nucleus at different phases of the circadian cycle. Brain Res Mol Brain Res. 1994;23:338–44.
Mikkelsen JD, Larsen PJ, Ebling FJ. Distribution of N-methyl D-aspartate (NMDA) receptor mRNAs in the rat suprachiasmatic nucleus. Brain Res. 1993;632:329–33.
Takeuchi Y, Takashima M, Katoh Y, Nishikawa T, Takahashi K. N-methyl-D-aspartate, quisqualate and kainate receptors are all involved in transmission of photic stimulation in the suprachiasmatic nucleus in rats. Brain Res. 1991;563:127–31.
Shibata S, Ono M, Tominaga K, Hamada T, Watanabe A, Watanabe S. Involvement of vasoactive intestinal polypeptide in NMDA-induced phase delay of firing activity rhythm in the suprachiasmatic nucleus in vitro. Neurosci Biobehav Rev. 1994;18:591–5.
Shibata S, Tominaga K, Hamada T, Watanabe S. Excitatory effect of N-methyl-D-aspartate and kainate receptor on the 2-deoxyglucose uptake in the rat suprachiasmatic nucleus in vitro. Neurosci Lett. 1992;139:83–6.
Paul KN, Fukuhara C, Karom M, Tosini G, Albers HE. AMPA/kainate receptor antagonist DNQX blocks the acute increase of Per2 mRNA levels in most but not all areas of the SCN. Brain Res Mol Brain Res. 2005;139:129–36.
Irwin RP, Allen CN. Calcium response to retinohypothalamic tract synaptic transmission in suprachiasmatic nucleus neurons. J Neurosci. 2007;27:11748–57.
Johnson RF, Moore RY, Morin LP. Loss of entrainment and anatomical plasticity after lesions of the hamster retinohypothalamic tract. Brain Res. 1988;460:297–313.
Scott G, Rusak B. Activation of hamster suprachiasmatic neurons in vitro via metabotropic glutamate receptors. Neuroscience. 1996;71:533–41.
Haak LL. Metabotropic glutamate receptor modulation of glutamate responses in the suprachiasmatic nucleus. J Neurophysiol. 1999;81:1308–17.
Park D, Lee S, Jun K, Hong YM, Kim DY, Kim YI, et al. Translation of clock rhythmicity into neural firing in suprachiasmatic nucleus requires mGluR-PLCbeta4 signaling. Nat Neurosci. 2003;6:337–8.
Okamura H, Berod A, Julien JF, Geffard M, Kitahama K, Mallet J, et al. Demonstration of GABAergic cell bodies in the suprachiasmatic nucleus: in situ hybridization of glutamic acid decarboxylase (GAD) mRNA and immunocytochemistry of GAD and GABA. Neurosci Lett. 1989;102:131–6.
Castel M, Morris JF. Morphological heterogeneity of the GABAergic network in the suprachiasmatic nucleus, the brain’s circadian pacemaker. J Anat. 2000;196:1–13.
Tanaka M, Matsuda T, Shigeyoshi Y, Ibata Y, Okamura H. Peptide expression in GABAergic neurons in rat suprachiasmatic nucleus in comparison with other forebrain structures: a double labeling in situ hybridization study. J Histochem Cytochem. 1997;45:1231–7.
Liou SY, Shibata S, Albers HE, Ueki S. Effects of GABA and anxiolytics on the single unit discharge of suprachiasmatic neurons in rat hypothalamic slices. Brain Res Bull. 1990;25:103–7.
Mason R, Biello SM, Harrington ME. The effects of GABA and benzodiazepines on neurones in the suprachiasmatic nucleus (SCN) of Syrian hamsters. Brain Res. 1991;552:53–7.
Gao B, Fritschy JM, Moore RY. GABAA-receptor subunit composition in the circadian timing system. Brain Res. 1995;700:142–56.
Moldavan M, Cravetchi O, Allen CN. GABA transporters regulate tonic and synaptic GABAA receptor-mediated currents in the suprachiasmatic nucleus neurons. J Neurophysiol. 2017;118:3092–106.
Moldavan M, Cravetchi O, Williams M, Irwin RP, Aicher SA, Allen CN. Localization and expression of GABA transporters in the suprachiasmatic nucleus. Eur J Neurosci. 2015;42:3018–32.
Alamilla J, Perez-Burgos A, Quinto D, Aguilar-Roblero R. Circadian modulation of the Cl(-) equilibrium potential in the rat suprachiasmatic nuclei. Biomed Res Int. 2014;2014:424982.
Belenky MA, Sollars PJ, Mount DB, Alper SL, Yarom Y, Pickard GE. Cell-type specific distribution of chloride transporters in the rat suprachiasmatic nucleus. Neuroscience. 2010;165:1519–37.
Choi HJ, Lee CJ, Schroeder A, Kim YS, Jung SH, Kim JS, et al. Excitatory actions of GABA in the suprachiasmatic nucleus. J Neurosci. 2008;28:5450–9.
Liou SY, Albers HE. Single unit response of neurons within the hamster suprachiasmatic nucleus to GABA and low chloride perfusate during the day and night. Brain Res Bull. 1990;25:93–8.
McNeill JKT, Walton JC, Albers HE. Functional significance of the excitatory effects of GABA in the suprachiasmatic nucleus. J Biol Rhythms. 2018;33:376–87.
Belenky MA, Yarom Y, Pickard GE. Heterogeneous expression of gamma-aminobutyric acid and gamma-aminobutyric acid-associated receptors and transporters in the rat suprachiasmatic nucleus. J Comp Neurol. 2008;506:708–32.
Ono D, Honma KI, Yanagawa Y, Yamanaka A, Honma S. Role of GABA in the regulation of the central circadian clock of the suprachiasmatic nucleus. J Physiol Sci. 2018;68:333–43.
Chen G, Trombley PQ, van den Pol AN. Excitatory actions of GABA in developing rat hypothalamic neurones. J Physiol. 1996;494:451–64.
Obrietan K, van den Pol AN. GABA neurotransmission in the hypothalamus: developmental reversal from Ca2+ elevating to depressing. J Neurosci. 1995;15:5065–77.
Gizowski C, Bourque CW. Sodium regulates clock time and output via an excitatory GABAergic pathway. Nature. 2020;583:421–24.
De Jeu M, Pennartz C. Circadian modulation of GABA function in the rat suprachiasmatic nucleus: excitatory effects during the night phase. J Neurophysiol. 2002;87:834–44.
Ehlen JC, Novak CM, Karom MC, Gamble KL, Paul KN, Albers HE. GABAA receptor activation suppresses Period 1 mRNA and Period 2 mRNA in the suprachiasmatic nucleus during the mid-subjective day. Eur J Neurosci. 2006;23:3328–36.
Wagner S, Sagiv N, Yarom Y. GABA-induced current and circadian regulation of chloride in neurones of the rat suprachiasmatic nucleus. J Physiol. 2001;537:853–69.
Wagner S, Castel M, Gainer H, Yarom Y. GABA in the mammalian suprachiasmatic nucleus and its role in diurnal rhythmicity. Nature. 1997;387:598–603.
Novak CM, Albers HE. Circadian phase alteration by GABA and light differs in diurnal and nocturnal rodents during the day. Behav Neurosci. 2004;118:498–504.
Gompf HS, Allen CN. GABAergic synapses of the suprachiasmatic nucleus exhibit a diurnal rhythm of short-term synaptic plasticity. Eur J Neurosci. 2004;19:2791–8.
Farajnia S, van Westering TL, Meijer JH, Michel S. Seasonal induction of GABAergic excitation in the central mammalian clock. Proc Natl Acad Sci USA. 2014;111:9627–32.
Myung J, Hong S, DeWoskin D, De Schutter E, Forger DB, Takumi T. GABA-mediated repulsive coupling between circadian clock neurons in the SCN encodes seasonal time. Proc Natl Acad Sci USA. 2015;112:E3920–9.
McNeill JKT, Walton JC, Ryu V, Albers HE. The Excitatory Effects of GABA within the Suprachiasmatic Nucleus: Regulation of Na-K-2Cl Cotransporters (NKCCs) by Environmental Lighting Conditions. J Biol Rhythms. 2020;35:275–86.
Aton SJ, Huettner JE, Straume M, Herzog ED. GABA and Gi/o differentially control circadian rhythms and synchrony in clock neurons. Proc Natl Acad Sci USA. 2006;103:19188–93.
Albus H, Vansteensel MJ, Michel S, Block GD, Meijer JH. A GABAergic mechanism is necessary for coupling dissociable ventral and dorsal regional oscillators within the circadian clock. Curr Biol. 2005;15:886–93.
DeWoskin D, Myung J, Belle MD, Piggins HD, Takumi T, Forger DB. Distinct roles for GABA across multiple timescales in mammalian circadian timekeeping. Proc Natl Acad Sci USA. 2015;112:E3911–9.
Mintz EM, Jasnow AM, Gillespie CF, Huhman KL, Albers HE. GABA interacts with photic signaling in the suprachiasmatic nucleus to regulate circadian phase shifts. Neuroscience. 2002;109:773–8.
Liu C, Reppert SM. GABA synchronizes clock cells within the suprachiasmatic circadian clock. Neuron. 2000;25:123–8.
Freeman GM Jr., Krock RM, Aton SJ, Thaben P, Herzog ED. GABA networks destabilize genetic oscillations in the circadian pacemaker. Neuron. 2013;78:799–806.
Gillespie CF, Huhman KL, Babagbemi TO, Albers HE. Bicuculline increases and muscimol reduces the phase-delaying effects of light and VIP/PHI/GRP in the suprachiasmatic region. J Biol Rhythms. 1996;11:137–44.
Hummer DL, Ehlen JC, Larkin TE 2nd, McNeill JKT, Pamplin JR 2nd, Walker CA, et al. Sustained activation of GABAA receptors in the suprachiasmatic nucleus mediates light-induced phase delays of the circadian clock: a novel function of ionotropic receptors. Eur J Neurosci. 2015;42:1830–8.
Chen G, van den Pol AN. Presynaptic GABAB autoreceptor modulation of P/Q-type calcium channels and GABA release in rat suprachiasmatic nucleus neurons. J Neurosci. 1998;18:1913–22.
Gillespie CF, Mintz EM, Marvel CL, Huhman KL, Albers HE. GABA(A) and GABA(B) agonists and antagonists alter the phase-shifting effects of light when microinjected into the suprachiasmatic region. Brain Res. 1997;759:181–9.
Gillespie CF, Van Der Beek EM, Mintz EM, Mickley NC, Jasnow AM, Huhman KL, et al. GABAergic regulation of light-induced c-Fos immunoreactivity within the suprachiasmatic nucleus. J Comp Neurol. 1999;411:683–92.
Ralph MR, Menaker M. GABA regulation of circadian responses to light. I. Involvement of GABAA-benzodiazepine and GABAB receptors. J Neurosci. 1989;9:2858–65.
Moldavan MG, Irwin RP, Allen CN. Presynaptic GABA(B) receptors regulate retinohypothalamic tract synaptic transmission by inhibiting voltage-gated Ca2+ channels. J Neurophysiol. 2006;95:3727–41.
Moldavan MG, Allen CN. GABAB receptor-mediated frequency-dependent and circadian changes in synaptic plasticity modulate retinal input to the suprachiasmatic nucleus. J Physiol. 2013;591:2475–90.
Jiang ZG, Allen CN, North RA. Presynaptic inhibition by baclofen of retinohypothalamic excitatory synaptic transmission in rat suprachiasmatic nucleus. Neuroscience. 1995;64:813–9.
Fite KV, Janusonis S, Foote W, Bengston L. Retinal afferents to the dorsal raphe nucleus in rats and Mongolian gerbils. J Comp Neurol. 1999;414:469–84.
Foote WE, Taber-Pierce E, Edwards L. Evidence for a retinal projection to the midbrain raphe of the cat. Brain Res. 1978;156:135–40.
Shen H, Semba K. A direct retinal projection to the dorsal raphe nucleus in the rat. Brain Res. 1994;635:159–68.
Meyer-Bernstein EL, Morin LP. Differential serotonergic innervation of the suprachiasmatic nucleus and the intergeniculate leaflet and its role in circadian rhythm modulation. J Neurosci. 1996;16:2097–111.
Meyer-Bernstein EL, Blanchard JH, Morin LP. The serotonergic projection from the median raphe nucleus to the suprachiasmatic nucleus modulates activity phase onset, but not other circadian rhythm parameters. Brain Res. 1997;755:112–20.
Morin LP, Shivers KY, Blanchard JH, Muscat L. Complex organization of mouse and rat suprachiasmatic nucleus. Neuroscience. 2006;137:1285–97.
Morin LP, Meyer-Bernstein EL. The ascending serotonergic system in the hamster: comparison with projections of the dorsal and median raphe nuclei. Neuroscience. 1999;91:81–105.
Moga MM, Moore RY. Organization of neural inputs to the suprachiasmatic nucleus in the rat. J Comp Neurol. 1997;389:508–34.
Hay-Schmidt A, Vrang N, Larsen PJ, Mikkelsen JD. Projections from the raphe nuclei to the suprachiasmatic nucleus of the rat. J Chem Neuroanat. 2003;25:293–310.
Blasiak T, Lewandowski MH. Dorsal raphe nucleus modulates neuronal activity in rat intergeniculate leaflet. Behav Brain Res. 2003;138:179–85.
Yamakawa GR, Antle MC. Phenotype and function of raphe projections to the suprachiasmatic nucleus. Eur J Neurosci. 2010;31:1974–83.
Antle MC, Ogilvie MD, Pickard GE, Mistlberger RE. Response of the mouse circadian system to serotonin 1A/2/7 agonists in vivo: surprisingly little. J Biol Rhythms. 2003;18:145–58.
Bradbury MJ, Dement WC, Edgar DM. Serotonin-containing fibers in the suprachiasmatic hypothalamus attenuate light-induced phase delays in mice. Brain Res. 1997;768:125–34.
Muscat L, Tischler RC, Morin LP. Functional analysis of the role of the median raphe as a regulator of hamster circadian system sensitivity to light. Brain Res. 2005;1044:59–66.
Mistlberger RE, Antle MC. Behavioral inhibition of light-induced circadian phase resetting is phase and serotonin dependent. Brain Res. 1998;786:31–8.
Marchant EG, Watson NV, Mistlberger RE. Both neuropeptide Y and serotonin are necessary for entrainment of circadian rhythms in mice by daily treadmill running schedules. J Neurosci. 1997;17:7974–87.
Meyer-Bernstein EL, Morin LP. Electrical stimulation of the median or dorsal raphe nuclei reduces light-induced FOS protein in the suprachiasmatic nucleus and causes circadian activity rhythm phase shifts. Neuroscience. 1999;92:267–79.
Rea MA, Glass JD, Colwell CS. Serotonin modulates photic responses in the hamster suprachiasmatic nuclei. J Neurosci. 1994;14:3635–42.
Ying SW, Rusak B. Effects of serotonergic agonists on firing rates of photically responsive cells in the hamster suprachiasmatic nucleus. Brain Res. 1994;651:37–46.
Liou SY, Shibata S, Ueki S. Effect of monoamines on field potentials in the suprachiasmatic nucleus of slices of hypothalamus of the rat evoked by stimulation of the optic nerve. Neuropharmacology. 1986;25:1009–14.
Ying SW, Rusak B. 5-HT7 receptors mediate serotonergic effects on light-sensitive suprachiasmatic nucleus neurons. Brain Res. 1997;755:246–54.
Weber ET, Gannon RL, Rea MA. Local administration of serotonin agonists blocks light-induced phase advances of the circadian activity rhythm in the hamster. J Biol Rhythms. 1998;13:209–18.
Ferguson SA, Kennaway DJ. The ontogeny of induction of c-fos in the rat SCN by a 5-HT(2A/2C) agonist. Brain Res Dev Brain Res. 2000;121:229–31.
Moyer RW, Kennaway DJ, Ferguson SA, Dijstelbloem YP. Quipazine and light have similar effects on c-fos induction in the rat suprachiasmatic nucleus. Brain Res. 1997;765:337–42.
Varcoe TJ, Kennaway DJ, Voultsios A. Activation of 5-HT2C receptors acutely induces Per gene expression in the rat suprachiasmatic nucleus at night. Brain Res Mol Brain Res. 2003;119:192–200.
Varcoe TJ, Kennaway DJ. Activation of 5-HT2C receptors acutely induces Per1 gene expression in the rat SCN in vitro. Brain Res. 2008;1209:19–28.
Kennaway DJ, Moyer RW. Serotonin 5-HT2c agonists mimic the effect of light pulses on circadian rhythms. Brain Res. 1998;806:257–70.
Graff C, Challet E, Pevet P, Wollnik F. 5-HT3 receptor-mediated photic-like responses of the circadian clock in the rat. Neuropharmacology 2007;52:662–71.
Gannon RL, Peglion JL, Millan MJ. Differential influence of selective 5-HT5A vs 5-HT1A, 5-HT1B, or 5-HT2C receptor blockade upon light-induced phase shifts in circadian activity rhythms: interaction studies with citalopram. Eur Neuropsychopharmacol. 2009;19:887–97.
Pickard GE, Rea MA. TFMPP, a 5HT1B receptor agonist, inhibits light-induced phase shifts of the circadian activity rhythm and c-Fos expression in the mouse suprachiasmatic nucleus. Neurosci Lett. 1997;231:95–8.
Pickard GE, Smith BN, Belenky M, Rea MA, Dudek FE, Sollars PJ. 5-HT1B receptor-mediated presynaptic inhibition of retinal input to the suprachiasmatic nucleus. J Neurosci. 1999;19:4034–45.
Pickard GE, Weber ET, Scott PA, Riberdy AF, Rea MA. 5HT1B receptor agonists inhibit light-induced phase shifts of behavioral circadian rhythms and expression of the immediate-early gene c-fos in the suprachiasmatic nucleus. J Neurosci. 1996;16:8208–20.
Smith BN, Sollars PJ, Dudek FE, Pickard GE. Serotonergic modulation of retinal input to the mouse suprachiasmatic nucleus mediated by 5-HT1B and 5-HT7 receptors. J Biol Rhythms. 2001;16:25–38.
Pickard GE, Rea MA. Serotonergic innervation of the hypothalamic suprachiasmatic nucleus and photic regulation of circadian rhythms. Biol Cell. 1997;89:513–23.
Sollars PJ, Ogilvie MD, Rea MA, Pickard GE. 5-HT1B receptor knockout mice exhibit an enhanced response to constant light. J Biol Rhythms. 2002;17:428–37.
Glass JD, Selim M, Rea MA. Modulation of light-induced C-Fos expression in the suprachiasmatic nuclei by 5-HT1A receptor agonists. Brain Res. 1994;638:235–42.
Smith VM, Iannattone S, Achal S, Jeffers RT, Antle MC. The serotonergic anxiolytic buspirone attenuates circadian responses to light. Eur J Neurosci. 2014;40:3512–25.
Moriya T, Yoshinobu Y, Ikeda M, Yokota S, Akiyama M, Shibata S. Potentiating action of MKC-242, a selective 5-HT1A receptor agonist, on the photic entrainment of the circadian activity rhythm in hamsters. Br J Pharm. 1998;125:1281–7.
Gannon RL, Millan MJ. Serotonin1A autoreceptor activation by S 15535 enhances circadian activity rhythms in hamsters: evaluation of potential interactions with serotonin2A and serotonin2C receptors. Neuroscience. 2006;137:287–99.
Rea MA, Barrera J, Glass JD, Gannon RL. Serotonergic potentiation of photic phase shifts of the circadian activity rhythm. Neuroreport. 1995;6:1417–20.
Byku M, Gannon RL. Effects of the 5HT1A agonist/antagonist BMY 7378 on light-induced phase advances in hamster circadian activity rhythms during aging. J Biol Rhythms. 2000;15:300–5.
Lall GS, Harrington ME. Potentiation of the resetting effects of light on circadian rhythms of hamsters using serotonin and neuropeptide Y receptor antagonists. Neuroscience. 2006;141:1545–52.
Sterniczuk R, Stepkowski A, Jones M, Antle MC. Enhancement of photic shifts with the 5-HT1A mixed agonist/antagonist NAN-190: intra-suprachiasmatic nucleus pathway. Neuroscience. 2008;153:571–80.
Smith VM, Hagel K, Antle MC. Serotonergic potentiation of photic phase shifts: examination of receptor contributions and early biochemical/molecular events. Neuroscience. 2010;165:16–27.
Gannon RL. Serotonergic serotonin (1A) mixed agonists/antagonists elicit large-magnitude phase shifts in hamster circadian wheel-running rhythms. Neuroscience. 2003;119:567–76.
Hut RA, Van der Zee EA. The cholinergic system, circadian rhythmicity, and time memory. Behav Brain Res. 2011;221:466–80.
Bina KG, Rusak B, Semba K. Localization of cholinergic neurons in the forebrain and brainstem that project to the suprachiasmatic nucleus of the hypothalamus in rat. J Comp Neurol. 1993;335:295–307.
Yamakawa GR, Basu P, Cortese F, MacDonnell J, Whalley D, Smith VM, et al. The cholinergic forebrain arousal system acts directly on the circadian pacemaker. Proc Natl Acad Sci USA. 2016;113:13498–503.
Madeira MD, Pereira PA, Silva SM, Cadete-Leite A, Paula-Barbosa MM. Basal forebrain neurons modulate the synthesis and expression of neuropeptides in the rat suprachiasmatic nucleus. Neuroscience. 2004;125:889–901.
Ikeda M, Sugiyama T, Suzuki K, Moriya T, Shibata S, Katsuki M, et al. PLC beta 4-independent Ca2+ rise via muscarinic receptors in the mouse suprachiasmatic nucleus. Neuroreport. 2000;11:907–12.
Ferguson SA, Kennaway DJ, Moyer RW. Nicotine phase shifts the 6-sulphatoxymelatonin rhythm and induces c-Fos in the SCN of rats. Brain Res Bull. 1999;48:527–38.
Dojo K, Yamaguchi Y, Fustin JM, Doi M, Kobayashi M, Okamura H. Carbachol induces phase-dependent phase shifts of Per1 transcription rhythms in cultured suprachiasmatic nucleus slices. J Biol Rhythms. 2017;32:101–08.
Basu P, Wensel AL, McKibbon R, Lefebvre N, Antle MC. Activation of M1/4 receptors phase advances the hamster circadian clock during the day. Neurosci Lett. 2016;621:22–27.
Bina KG, Rusak B. Muscarinic receptors mediate carbachol-induced phase shifts of circadian activity rhythms in Syrian hamsters. Brain Res. 1996;743:202–11.
Gillette MU, Buchanan GF, Artinian L, Hamilton SE, Nathanson NM, Liu C. Role of the M1 receptor in regulating circadian rhythms. Life Sci. 2001;68:2467–72.
Liu C, Ding JM, Faiman LE, Gillette MU. Coupling of muscarinic cholinergic receptors and cGMP in nocturnal regulation of the suprachiasmatic circadian clock. J Neurosci. 1997;17:659–66.
van der Zee EA, Streefland C, Strosberg AD, Schroder H, Luiten PG. Colocalization of muscarinic and nicotinic receptors in cholinoceptive neurons of the suprachiasmatic region in young and aged rats. Brain Res. 1991;542:348–52.
Liu C, Gillette MU. Cholinergic regulation of the suprachiasmatic nucleus circadian rhythm via a muscarinic mechanism at night. J Neurosci. 1996;16:744–51.
Duffield GE, McNulty S, Ebling FJ. Anatomical and functional characterisation of a dopaminergic system in the suprachiasmatic nucleus of the neonatal Siberian hamster. J Comp Neurol. 1999;408:73–96.
Duffield GE, Hastings MH, Ebling FJ. Investigation into the regulation of the circadian system by dopamine and melatonin in the adult Siberian hamster (Phodopus sungorus). J Neuroendocrinol. 1998;10:871–84.
Bender M, Drago J, Rivkees SA. D1 receptors mediate dopamine action in the fetal suprachiasmatic nuclei: studies of mice with targeted deletion of the D1 dopamine receptor gene. Brain Res Mol Brain Res. 1997;49:271–7.
Weaver DR, Rivkees SA, Reppert SM. D1-dopamine receptors activate c-fos expression in the fetal suprachiasmatic nuclei. Proc Natl Acad Sci USA. 1992;89:9201–4.
Grippo RM, Purohit AM, Zhang Q, Zweifel LS, Guler AD. Direct Midbrain Dopamine Input to the Suprachiasmatic Nucleus Accelerates Circadian Entrainment. Curr Biol. 2017;27:2465–75. e3.
Glass JD, Brager AJ, Stowie AC, Prosser RA. Cocaine modulates pathways for photic and nonphotic entrainment of the mammalian SCN circadian clock. Am J Physiol Regul Integr Comp Physiol. 2012;302:R740–50.
Brager AJ, Stowie AC, Prosser RA, Glass JD. The mPer2 clock gene modulates cocaine actions in the mouse circadian system. Behav Brain Res. 2013;243:255–60.
Prosser RA, Stowie A, Amicarelli M, Nackenoff AG, Blakely RD, Glass JD. Cocaine modulates mammalian circadian clock timing by decreasing serotonin transport in the SCN. Neuroscience. 2014;275:184–93.
Mohawk JA, Pezuk P, Menaker M. Methamphetamine and dopamine receptor D1 regulate entrainment of murine circadian oscillators. PLoS One. 2013;8:e62463.
Kotwal A, Cutrona SL. Serotonin Syndrome in the Setting of Lamotrigine, Aripiprazole, and Cocaine Use. Case Rep. Med. 2015;2015:769531.
Sofuoglu M, Sewell RA. Norepinephrine and stimulant addiction. Addict Biol. 2009;14:119–29.
Pickard GE. Bifurcating axons of retinal ganglion cells terminate in the hypothalamic suprachiasmatic nucleus and the intergeniculate leaflet of the thalamus. Neurosci Lett. 1985;55:211–7.
Morin LP, Blanchard JH, Provencio I. Retinal ganglion cell projections to the hamster suprachiasmatic nucleus, intergeniculate leaflet, and visual midbrain: bifurcation and melanopsin immunoreactivity. J Comp Neurol. 2003;465:401–16.
Harrington ME, Nance DM, Rusak B. Neuropeptide Y immunoreactivity in the hamster geniculo-suprachiasmatic tract. Brain Res Bull. 1985;15:465–72.
Hisano S, Chikamori-Aoyama M, Katoh S, Kagotani Y, Daikoku S, Chihara K. Suprachiasmatic nucleus neurons immunoreactive for vasoactive intestinal polypeptide have synaptic contacts with axons immunoreactive for neuropeptide Y: an immunoelectron microscopic study in the rat. Neurosci Lett. 1988;88:145–50.
Card JP, Moore RY. Organization of lateral geniculate-hypothalamic connections in the rat. J Comp Neurol. 1989;284:135–47.
Moore RY, Gustafson EL, Card JP. Identical immunoreactivity of afferents to the rat suprachiasmatic nucleus with antisera against avian pancreatic polypeptide, molluscan cardioexcitatory peptide and neuropeptide Y. Cell Tissue Res. 1984;236:41–6.
Morin LP, Blanchard J, Moore RY. Intergeniculate leaflet and suprachiasmatic nucleus organization and connections in the golden hamster. Vis Neurosci. 1992;8:219–30.
Morin LP, Blanchard JH. Neuromodulator content of hamster intergeniculate leaflet neurons and their projection to the suprachiasmatic nucleus or visual midbrain. J Comp Neurol. 2001;437:79–90.
Saderi N, Cazarez-Marquez F, Buijs FN, Salgado-Delgado RC, Guzman-Ruiz MA, del Carmen Basualdo M, et al. The NPY intergeniculate leaflet projections to the suprachiasmatic nucleus transmit metabolic conditions. Neuroscience 2013;246:291–300.
Yannielli PC, Harrington ME. The neuropeptide Y Y5 receptor mediates the blockade of "photic-like" NMDA-induced phase shifts in the golden hamster. J Neurosci. 2001;21:5367–73.
Yannielli PC, Harrington ME. Neuropeptide Y applied in vitro can block the phase shifts induced by light in vivo. Neuroreport. 2000;11:1587–91.
Weber ET, Rea MA. Neuropeptide Y blocks light-induced phase advances but not delays of the circadian activity rhythm in hamsters. Neurosci Lett. 1997;231:159–62.
Biello SM. Enhanced photic phase shifting after treatment with antiserum to neuropeptide Y. Brain Res. 1995;673:25–9.
Brewer JM, Yannielli PC, Harrington ME. Neuropeptide Y differentially suppresses per1 and per2 mRNA induced by light in the suprachiasmatic nuclei of the golden hamster. J Biol Rhythms. 2002;17:28–39.
Fukuhara C, Brewer JM, Dirden JC, Bittman EL, Tosini G, Harrington ME. Neuropeptide Y rapidly reduces Period 1 and Period 2 mRNA levels in the hamster suprachiasmatic nucleus. Neurosci Lett. 2001;314:119–22.
Harrington ME, Hoque S. NPY opposes PACAP phase shifts via receptors different from those involved in NPY phase shifts. Neuroreport. 1997;8:2677–80.
Lall GS, Biello SM. Attenuation of circadian light induced phase advances and delays by neuropeptide Y and a neuropeptide Y Y1/Y5 receptor agonist. Neuroscience. 2003;119:611–8.
Chen G, van den Pol AN. Multiple NPY receptors coexist in pre- and postsynaptic sites: inhibition of GABA release in isolated self-innervating SCN neurons. J Neurosci. 1996;16:7711–24.
Gamble KL, Paul KN, Karom MC, Tosini G, Albers HE. Paradoxical effects of NPY in the suprachiasmatic nucleus. Eur J Neurosci. 2006;23:2488–94.
Gamble KL, Ehlen JC, Albers HE. Circadian control during the day and night: Role of neuropeptide Y Y5 receptors in the suprachiasmatic nucleus. Brain Res Bull. 2005;65:513–9.
Morin LP, Blanchard J. Organization of the hamster intergeniculate leaflet: NPY and ENK projections to the suprachiasmatic nucleus, intergeniculate leaflet and posterior limitans nucleus. Vis Neurosci. 1995;12:57–67.
Byku M, Legutko R, Gannon RL. Distribution of delta opioid receptor immunoreactivity in the hamster suprachiasmatic nucleus and intergeniculate leaflet. Brain Res. 2000;857:1–7.
Tierno A, Fiore P, Gannon RL. Delta opioid inhibition of light-induced phase advances in hamster circadian activity rhythms. Brain Res. 2002;937:66–73.
Florian C, Vecsey CG, Halassa MM, Haydon PG, Abel T. Astrocyte-derived adenosine and A1 receptor activity contribute to sleep loss-induced deficits in hippocampal synaptic plasticity and memory in mice. J Neurosci. 2011;31:6956–62.
Nadjar A, Blutstein T, Aubert A, Laye S, Haydon PG. Astrocyte-derived adenosine modulates increased sleep pressure during inflammatory response. Glia. 2013;61:724–31.
Schmitt LI, Sims RE, Dale N, Haydon PG. Wakefulness affects synaptic and network activity by increasing extracellular astrocyte-derived adenosine. J Neurosci. 2012;32:4417–25.
Porkka-Heiskanen T, Strecker RE, Thakkar M, Bjorkum AA, Greene RW, McCarley RW. Adenosine: a mediator of the sleep-inducing effects of prolonged wakefulness. Science. 1997;276:1265–8.
Bjorness TE, Kelly CL, Gao T, Poffenberger V, Greene RW. Control and function of the homeostatic sleep response by adenosine A1 receptors. J Neurosci. 2009;29:1267–76.
Dunwiddie TV, Masino SA. The role and regulation of adenosine in the central nervous system. Annu Rev Neurosci. 2001;24:31–55.
Dunwiddie TV, Diao L, Proctor WR. Adenine nucleotides undergo rapid, quantitative conversion to adenosine in the extracellular space in rat hippocampus. J Neurosci. 1997;17:7673–82.
Guthrie PB, Knappenberger J, Segal M, Bennett MV, Charles AC, Kater SB. ATP released from astrocytes mediates glial calcium waves. J Neurosci. 1999;19:520–8.
Blutstein T, Haydon PG. The Importance of astrocyte-derived purines in the modulation of sleep. Glia. 2013;61:129–39.
Scharbarg E, Daenens M, Lemaitre F, Geoffroy H, Guille-Collignon M, Gallopin T, et al. Astrocyte-derived adenosine is central to the hypnogenic effect of glucose. Sci Rep. 2016;6:19107.
Porkka-Heiskanen T, Strecker RE, McCarley RW. Brain site-specificity of extracellular adenosine concentration changes during sleep deprivation and spontaneous sleep: an in vivo microdialysis study. Neuroscience. 2000;99:507–17.
Chen G, van den Pol AN. Adenosine modulation of calcium currents and presynaptic inhibition of GABA release in suprachiasmatic and arcuate nucleus neurons. J Neurophysiol. 1997;77:3035–47.
van Diepen HC, Lucassen EA, Yasenkov R, Groenen I, Ijzerman AP, Meijer JH, et al. Caffeine increases light responsiveness of the mouse circadian pacemaker. Eur J Neurosci. 2014;40:3504–11.
Watanabe A, Moriya T, Nisikawa Y, Araki T, Hamada T, Shibata S, et al. Adenosine A1-receptor agonist attenuates the light-induced phase shifts and fos expression in vivo and optic nerve stimulation-evoked field potentials in the suprachiasmatic nucleus in vitro. Brain Res. 1996;740:329–36.
Hallworth R, Cato M, Colbert C, Rea MA. Presynaptic adenosine A1 receptors regulate retinohypothalamic neurotransmission in the hamster suprachiasmatic nucleus. J Neurobiol. 2002;52:230–40.
Sigworth LA, Rea MA. Adenosine A1 receptors regulate the response of the mouse circadian clock to light. Brain Res. 2003;960:246–51.
Elliott KJ, Todd Weber E, Rea MA. Adenosine A1 receptors regulate the response of the hamster circadian clock to light. Eur J Pharm. 2001;414:45–53.
Jagannath A, Varga N, Dallmann R, Rando G, Gosselin P, Ebrahimjee F, et al. Adenosine integrates light and sleep signalling for the regulation of circadian timing in mice. Nat Commun. 2021;12:2113.
Acuna-Goycolea C, Obrietan K, van den Pol AN. Cannabinoids excite circadian clock neurons. J Neurosci. 2010;30:10061–6.
Wittmann G, Deli L, Kallo I, Hrabovszky E, Watanabe M, Liposits Z, et al. Distribution of type 1 cannabinoid receptor (CB1)-immunoreactive axons in the mouse hypothalamus. J Comp Neurol. 2007;503:270–9.
Sanford AE, Castillo E, Gannon RL. Cannabinoids and hamster circadian activity rhythms. Brain Res. 2008;1222:141–8.
Sladek M, Sumova A. Modulation of NMDA-mediated clock resetting in the suprachiasmatic nuclei of mPer2 (Luc) mouse by endocannabinoids. Front Physiol. 2019;10:361.
Sladek M, Liska K, Houdek P, Sumova A. Modulation of single cell circadian response to NMDA by diacylglycerol lipase inhibition reveals a role of endocannabinoids in light entrainment of the suprachiasmatic nucleus. Neuropharmacology. 2021;185:108455.
Hablitz LM, Gunesch AN, Cravetchi O, Moldavan M, Allen CN Cannabinoid signaling recruits astrocytes to modulate presynaptic function in the suprachiasmatic nucleus. eNeuro. 2020;7:1–19.
Piggins HD, Samuels RE, Coogan AN, Cutler DJ. Distribution of substance P and neurokinin-1 receptor immunoreactivity in the suprachiasmatic nuclei and intergeniculate leaflet of hamster, mouse, and rat. J Comp Neurol. 2001;438:50–65.
Takatsuji K, Miguel-Hidalgo JJ, Tohyama M. Substance P-immunoreactive innervation from the retina to the suprachiasmatic nucleus in the rat. Brain Res. 1991;568:223–9.
Mikkelsen JD, Larsen PJ. Substance P in the suprachiasmatic nucleus of the rat: an immunohistochemical and in situ hybridization study. Histochemistry. 1993;100:3–16.
Saper CB, Lu J, Chou TC, Gooley J. The hypothalamic integrator for circadian rhythms. Trends Neurosci. 2005;28:152–7.
Krout KE, Kawano J, Mettenleiter TC, Loewy AD. CNS inputs to the suprachiasmatic nucleus of the rat. Neuroscience. 2002;110:73–92.
Teclemariam-Mesbah R, Ter Horst GJ, Postema F, Wortel J, Buijs RM. Anatomical demonstration of the suprachiasmatic nucleus-pineal pathway. J Comp Neurol. 1999;406:171–82.
Vrang N, Larsen PJ, Mikkelsen JD. Direct projection from the suprachiasmatic nucleus to hypophysiotrophic corticotropin-releasing factor immunoreactive cells in the paraventricular nucleus of the hypothalamus demonstrated by means of Phaseolus vulgaris-leucoagglutinin tract tracing. Brain Res. 1995;684:61–9.
Ono D, Mukai Y, Hung CJ, Chowdhury S, Sugiyama T, Yamanaka A The mammalian circadian pacemaker regulates wakefulness via CRF neurons in the paraventricular nucleus of the hypothalamus. Sci Adv. 2020;6:1–14.
Gimpl G, Fahrenholz F. The oxytocin receptor system: structure, function, and regulation. Physiol Rev. 2001;81:629–83.
Neumann ID. Brain oxytocin: a key regulator of emotional and social behaviours in both females and males. J Neuroendocrinol. 2008;20:858–65.
Dzirbikova Z, Kiss A, Okuliarova M, Kopkan L, Cervenka L. Expressions of per1 clock gene and genes of signaling peptides vasopressin, vasoactive intestinal peptide, and oxytocin in the suprachiasmatic and paraventricular nuclei of hypertensive TGR[mREN2]27 rats. Cell Mol Neurobiol. 2011;31:225–32.
Vaccari C, Lolait SJ, Ostrowski NL. Comparative distribution of vasopressin V1b and oxytocin receptor messenger ribonucleic acids in brain. Endocrinology. 1998;139:5015–33.
Young LJ, Muns S, Wang Z, Insel TR. Changes in oxytocin receptor mRNA in rat brain during pregnancy and the effects of estrogen and interleukin-6. J Neuroendocrinol. 1997;9:859–65.
Neumann ID, Wigger A, Torner L, Holsboer F, Landgraf R. Brain oxytocin inhibits basal and stress-induced activity of the hypothalamo-pituitary-adrenal axis in male and female rats: partial action within the paraventricular nucleus. J Neuroendocrinol. 2000;12:235–43.
Resendez SL, Namboodiri VMK, Otis JM, Eckman LEH, Rodriguez-Romaguera J, Ung RL, et al. Social stimuli induce activation of oxytocin neurons within the paraventricular nucleus of the hypothalamus to promote social behavior in male mice. J Neurosci. 2020;40:2282–95.
Brown TM, Hughes AT, Piggins HD. Gastrin-releasing peptide promotes suprachiasmatic nuclei cellular rhythmicity in the absence of vasoactive intestinal polypeptide-VPAC2 receptor signaling. J Neurosci. 2005;25:11155–64.
Aida R, Moriya T, Araki M, Akiyama M, Wada K, Wada E, et al. Gastrin-releasing peptide mediates photic entrainable signals to dorsal subsets of suprachiasmatic nucleus via induction of Period gene in mice. Mol Pharm. 2002;61:26–34.
Antle MC, Kriegsfeld LJ, Silver R. Signaling within the master clock of the brain: localized activation of mitogen-activated protein kinase by gastrin-releasing peptide. J Neurosci. 2005;25:2447–54.
Earnest DJ, DiGiorgio S, Olschowka JA. Light induces expression of fos-related proteins within gastrin-releasing peptide neurons in the rat suprachiasmatic nucleus. Brain Res. 1993;627:205–9.
Gamble KL, Allen GC, Zhou T, McMahon DG. Gastrin-releasing peptide mediates light-like resetting of the suprachiasmatic nucleus circadian pacemaker through cAMP response element-binding protein and Per1 activation. J Neurosci. 2007;27:12078–87.
Piggins HD, Goguen D, Rusak B. Gastrin-releasing peptide induces c-Fos in the hamster suprachiasmatic nucleus. Neurosci Lett. 2005;384:205–10.
Tanaka M, Hayashi S, Tamada Y, Ikeda T, Hisa Y, Takamatsu T, et al. Direct retinal projections to GRP neurons in the suprachiasmatic nucleus of the rat. Neuroreport. 1997;8:2187–91.
Piggins HD, Cutler DJ, Rusak B. Effects of ionophoretically applied bombesin-like peptides on hamster suprachiasmatic nucleus neurons in vitro. Eur J Pharm. 1994;271:413–9.
Aioun J, Chambille I, Peytevin J, Martinet L. Neurons containing gastrin-releasing peptide and vasoactive intestinal polypeptide are involved in the reception of the photic signal in the suprachiasmatic nucleus of the Syrian hamster: an immunocytochemical ultrastructural study. Cell Tissue Res. 1998;291:239–53.
Ladenheim EE, Jensen RT, Mantey SA, Moran TH. Distinct distributions of two bombesin receptor subtypes in the rat central nervous system. Brain Res. 1992;593:168–78.
Piggins HD, Rusak B. Electrophysiological effects of pressure-ejected bombesin-like peptides on hamster suprachiasmatic nucleus neurons in vitro. J Neuroendocrinol. 1993;5:575–81.
McArthur AJ, Coogan AN, Ajpru S, Sugden D, Biello SM, Piggins HD. Gastrin-releasing peptide phase-shifts suprachiasmatic nuclei neuronal rhythms in vitro. J Neurosci. 2000;20:5496–502.
Akiyama T, Tominaga M, Davoodi A, Nagamine M, Blansit K, Horwitz A, et al. Roles for substance P and gastrin-releasing peptide as neurotransmitters released by primary afferent pruriceptors. J Neurophysiol. 2013;109:742–8.
Merali Z, Mountney C, Kent P, Anisman H. Activation of gastrin-releasing peptide receptors at the infralimbic cortex elicits gastrin-releasing peptide release at the basolateral amygdala: implications for conditioned fear. Neuroscience. 2013;243:97–103.
Chan RK, Sterniczuk R, Enkhbold Y, Jeffers RT, Basu P, Duong B, et al. Phase shifts to light are altered by antagonists to neuropeptide receptors. Neuroscience. 2016;327:115–24.
Piggins HD, Antle MC, Rusak B. Neuropeptides phase shift the mammalian circadian pacemaker. J Neurosci. 1995;15:5612–22.
Brancaccio M, Maywood ES, Chesham JE, Loudon AS, Hastings MH. A Gq-Ca2+ axis controls circuit-level encoding of circadian time in the suprachiasmatic nucleus. Neuron. 2013;78:714–28.
Colwell CS. NMDA-evoked calcium transients and currents in the suprachiasmatic nucleus: gating by the circadian system. Eur J Neurosci. 2001;13:1420–8.
Ginty DD, Kornhauser JM, Thompson MA, Bading H, Mayo KE, Takahashi JS, et al. Regulation of CREB phosphorylation in the suprachiasmatic nucleus by light and a circadian clock. Science. 1993;260:238–41.
Ding JM, Faiman LE, Hurst WJ, Kuriashkina LR, Gillette MU. Resetting the biological clock: mediation of nocturnal CREB phosphorylation via light, glutamate, and nitric oxide. J Neurosci. 1997;17:667–75.
von Gall C, Duffield GE, Hastings MH, Kopp MD, Dehghani F, Korf HW, et al. CREB in the mouse SCN: a molecular interface coding the phase-adjusting stimuli light, glutamate, PACAP, and melatonin for clockwork access. J Neurosci. 1998;18:10389–97.
McNulty S, Schurov IL, Sloper PJ, Hastings MH. Stimuli which entrain the circadian clock of the neonatal Syrian hamster in vivo regulate the phosphorylation of the transcription factor CREB in the suprachiasmatic nucleus in vitro. Eur J Neurosci. 1998;10:1063–72.
Wheaton KL, Hansen KF, Aten S, Sullivan KA, Yoon H, Hoyt KR, et al. The phosphorylation of CREB at serine 133 is a key event for circadian clock timing and entrainment in the suprachiasmatic nucleus. J Biol Rhythms. 2018;33:497–514.
Kornhauser JM, Nelson DE, Mayo KE, Takahashi JS. Photic and circadian regulation of c-fos gene expression in the hamster suprachiasmatic nucleus. Neuron. 1990;5:127–34.
Rea MA. Light increases Fos-related protein immunoreactivity in the rat suprachiasmatic nuclei. Brain Res Bull. 1989;23:577–81.
Abe H, Rusak B, Robertson HA. NMDA and non-NMDA receptor antagonists inhibit photic induction of Fos protein in the hamster suprachiasmatic nucleus. Brain Res Bull. 1992;28:831–5.
Rea MA, Buckley B, Lutton LM. Local administration of EAA antagonists blocks light-induced phase shifts and c-fos expression in hamster SCN. Am J Physiol. 1993;265:R1191–8.
Tischkau SA, Gallman EA, Buchanan GF, Gillette MU. Differential cAMP gating of glutamatergic signaling regulates long-term state changes in the suprachiasmatic circadian clock. J Neurosci. 2000;20:7830–7.
Fukushima T, Shimazoe T, Shibata S, Watanabe A, Ono M, Hamada T, et al. The involvement of calmodulin and Ca2+/calmodulin-dependent protein kinase II in the circadian rhythms controlled by the suprachiasmatic nucleus. Neurosci Lett. 1997;227:45–8.
Golombek DA, Ralph MR. KN-62, an inhibitor of Ca2+/calmodulin kinase II, attenuates circadian responses to light. Neuroreport. 1994;5:1638–40.
Butcher GQ, Doner J, Dziema H, Collamore M, Burgoon PW, Obrietan K. The p42/44 mitogen-activated protein kinase pathway couples photic input to circadian clock entrainment. J Biol Chem. 2002;277:29519–25.
Obrietan K, Impey S, Storm DR. Light and circadian rhythmicity regulate MAP kinase activation in the suprachiasmatic nuclei. Nat Neurosci. 1998;1:693–700.
Coogan AN, Piggins HD. Circadian and photic regulation of phosphorylation of ERK1/2 and Elk-1 in the suprachiasmatic nuclei of the Syrian hamster. J Neurosci. 2003;23:3085–93.
Agostino PV, Ferreyra GA, Murad AD, Watanabe Y, Golombek DA. Diurnal, circadian and photic regulation of calcium/calmodulin-dependent kinase II and neuronal nitric oxide synthase in the hamster suprachiasmatic nuclei. Neurochem Int. 2004;44:617–25.
Amir S. Blocking NMDA receptors or nitric oxide production disrupts light transmission to the suprachiasmatic nucleus. Brain Res. 1992;586:336–9.
Amir S, Edelstein K. A blocker of nitric oxide synthase, NG-nitro-L-arginine methyl ester, attenuates light-induced Fos protein expression in rat suprachiasmatic nucleus. Neurosci Lett. 1997;224:29–32.
Prosser RA, McArthur AJ, Gillette MU. cGMP induces phase shifts of a mammalian circadian pacemaker at night, in antiphase to cAMP effects. Proc Natl Acad Sci USA. 1989;86:6812–5.
Golombek DA, Agostino PV, Plano SA, Ferreyra GA. Signaling in the mammalian circadian clock: the NO/cGMP pathway. Neurochem Int. 2004;45:929–36.
Ferreyra GA, Golombek DA. Rhythmicity of the cGMP-related signal transduction pathway in the mammalian circadian system. Am J Physiol Regul Integr Comp Physiol. 2001;280:R1348–55.
Oster H, Werner C, Magnone MC, Mayser H, Feil R, Seeliger MW, et al. cGMP-dependent protein kinase II modulates mPer1 and mPer2 gene induction and influences phase shifts of the circadian clock. Curr Biol. 2003;13:725–33.
Weber ET, Gannon RL, Rea MA. cGMP-dependent protein kinase inhibitor blocks light-induced phase advances of circadian rhythms in vivo. Neurosci Lett. 1995;197:227–30.
Moriya T, Horikawa K, Akiyama M, Shibata S. Correlative association between N-methyl-D-aspartate receptor-mediated expression of period genes in the suprachiasmatic nucleus and phase shifts in behavior with photic entrainment of clock in hamsters. Mol Pharm. 2000;58:1554–62.
Wollnik F, Brysch W, Uhlmann E, Gillardon F, Bravo R, Zimmermann M, et al. Block of c-Fos and JunB expression by antisense oligonucleotides inhibits light-induced phase shifts of the mammalian circadian clock. Eur J Neurosci. 1995;7:388–93.
Yi CX, Challet E, Pevet P, Kalsbeek A, Escobar C, Buijs RM. A circulating ghrelin mimetic attenuates light-induced phase delay of mice and light-induced Fos expression in the suprachiasmatic nucleus of rats. Eur J Neurosci. 2008;27:1965–72.
Mendoza J, Lopez-Lopez C, Revel FG, Jeanneau K, Delerue F, Prinssen E, et al. Dimorphic effects of leptin on the circadian and hypocretinergic systems of mice. J Neuroendocrinol. 2011;23:28–38.
Challet E, Losee-Olson S, Turek FW. Reduced glucose availability attenuates circadian responses to light in mice. Am J Physiol. 1999;276:R1063–70.
Novak CM, Ehlen JC, Huhman KL, Albers HE. GABA(B) receptor activation in the suprachiasmatic nucleus of diurnal and nocturnal rodents. Brain Res Bull. 2004;63:531–5.
Jha PK, Bouaouda H, Gourmelen S, Dumont S, Fuchs F, Goumon Y, et al. Sleep deprivation and caffeine treatment potentiate photic resetting of the master circadian clock in a diurnal rodent. J Neurosci. 2017;37:4343–58.
Agostino PV, Plano SA, Golombek DA. Sildenafil accelerates reentrainment of circadian rhythms after advancing light schedules. Proc Natl Acad Sci USA. 2007;104:9834–9.
Corbin JD, Francis SH. Cyclic GMP phosphodiesterase-5: target of sildenafil. J Biol Chem. 1999;274:13729–32.
Zuccarello E, Acquarone E, Calcagno E, Argyrousi EK, Deng SX, Landry DW, et al. Development of novel phosphodiesterase 5 inhibitors for the therapy of Alzheimer’s disease. Biochem Pharm. 2020;176:113818.
Wisden W, Yu X, Franks NP. GABA receptors and the pharmacology of sleep. Handb Exp Pharm. 2019;253:279–304.
Babson KA, Sottile J, Morabito D. Cannabis, cannabinoids, and sleep: areview of the literature. Curr Psychiatry Rep.2017;19:23
Goadsby PJ, Hoskin KL. Inhibition of trigeminal neurons by intravenous administration of the serotonin (5HT)1B/D receptor agonist zolmitriptan (311C90): are brain stem sites therapeutic target in migraine? Pain 1996;67:355–9.
Charles A. Advances in the basic and clinical science of migraine. Ann Neurol. 2009;65:491–8.
Pageler L, Limmroth V. Oral triptans in the preventive management of cluster headache. Curr Pain Headache Rep. 2012;16:180–4.
Funding
We thank the Velux Stiftung for their support (Proj. No. 1360). The authors declare no competing financial interests in relation to the work described.
Author information
Authors and Affiliations
Contributions
Author contributions included conceptual and study design (FXF), data search and curation (RL, AM, FXF), and interpretation (RL, AM, FXF). All authors participated in drafting the manuscript. We thank Bowen Lu for providing comments on an earlier version of the report.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
• Highlights the 146 papers included within the meta-analysis.
Owing to its length, the appendix has been provided in a separate document.
Supplementary information
Rights and permissions
About this article
Cite this article
Lee, R., McGee, A. & Fernandez, FX. Systematic review of drugs that modify the circadian system’s phase-shifting responses to light exposure. Neuropsychopharmacol. 47, 866–879 (2022). https://doi.org/10.1038/s41386-021-01251-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-021-01251-8
This article is cited by
-
Seasonality of brain function: role in psychiatric disorders
Translational Psychiatry (2023)
-
Sex Differences in Long-term Outcome of Prenatal Exposure to Excess Glucocorticoids—Implications for Development of Psychiatric Disorders
Molecular Neurobiology (2023)
-
Patterns of activity correlate with symptom severity in major depressive disorder patients
Translational Psychiatry (2022)