Abstract
The developmental stages of each foregut organ are intimately linked to the development of the other foregut organs such that the ultimate function of any one foregut organ, such as the metabolic function of the liver, depends on organizational changes associated with the maturation of multiple foregut organs. These changes include: (i) proliferation of the intrahepatic bile ducts and hepatoblasts within the liver coinciding with parenchymal expansion, (ii) elongation of extrahepatic bile ducts, which allows for proper gallbladder (GB) formation, and (iii) duodenal elongation and rotation, which coincides with all of the above to connect the intrahepatic, extrahepatic, and pancreatic ductal systems with the intestine. It is well established that cross talk between endodermal and mesenchymal components of the foregut occurs, particularly regarding the vascularization of developing organs. Furthermore, genetic mutations in mesenchymal and hepatic compartments of the developing foregut result in similar foregut pathologies: hypoplastic liver, absence of GB, biliary atresia (intrahepatic and/or extrahepatic), and failure of gut elongation and rotation. Finally, these shared pathologies can be linked to deficiencies in genes specific to the septum transversum mesenchyme (Hes1, Hlx, and Foxf1) or liver (Hhex and Hnf6), illustrating the complexity of such cross talk.
Similar content being viewed by others
Evolution and Development of the Foregut Organs: Molecular, Anatomical, and Functional Overlap
Over the past decade, much information has been revealed concerning the developmental and pathological processes involving foregut endodermal organs (liver, intestine, pancreas, etc.). The primitive gut segregates into three distinct domains: foregut, midgut, and hindgut, and specification of definitive endodermal (DE) cells in the ventral foregut endoderm occurs at around E8.5 in the mouse. These foregut DE cells eventually give rise to the endodermal components of the liver (extrahepatic and intrahepatic), pancreas, and intestine (1). For example, multipotent DE cells of the hepatic diverticulum (primitive liver bud) undergo epithelial–mesenchymal transition (EMT) and invade the adjacent septum transversum mesenchyme (STM) to form the liver bud at E9.5–10.5 (2). These DE cells contribute to the development, and potentially regeneration, of multiple foregut organs including liver and pancreas (3). In addition, it is clear that the development and pathology of multiple foregut organs is intimately linked via the extrahepatic biliary duct (EHBD) system as the maturation of multiple foregut organs depends on the proper elongation of the EHBDs ( Figure 1 ). It has been postulated that the EHBD serves as a source of progenitor DE cells and that this process is dependent on interaction with surrounding tissue types to support the temporal aspects of foregut maturation (4). For example, mesenchymal tissues such as the lesser ommentum supply the foregut organs with blood and lymph vessels and nerves. This ommenta elongates, along with the EHBD, as it moves from an anterior to a posterior position allowing for the maintenance of blood and bile conduits during duodenal gut rotation. Both the EHBD and mesenchymal tissues are continuous with the endothelium (porta hepatis—transverse fissure) at the level of the liver hilum. The intrahepatic biliary ducts (IHBDs) then develop from the porta hepatis (liver hilum) toward the periphery (E13.5–14.5) before becoming restricted to periportal areas later in gestation (E16–18) (5). Therefore, the communication between multiple cell types might underlie the regionalization, development, and potential specificity of DE organ maturation.
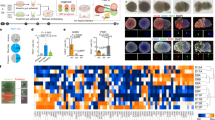
Development of the foregut organs. The development and pathology of multiple foregut organs is intimately linked via the extrahepatic biliary duct (EHBD) system. The maturation of multiple foregut organs is associated with proper elongation of the EHBDs. (a) View from left side of wild-type mouse embryo before E12.5; the midgut (duodenum), ampulla of vater, and ventral pancreas remains adjacent to the liver hilum, vascular remodeling begins with arterialization, and EHBDs/gallbladders (GBs) have not elongated. (b) View from left side of wild-type mouse embryo after E12.5, the midgut rotates and descends to align the ventral pancreas and ampulla of vater with the dorsal pancreas (gut rotation), the EHBDs/GBs elongate to maintain continuity, and the liver expands in size as vascular remodeling increases with the invading portal tract. Disturbances in the development of the liver and/or septum transversum mesenchyme can lead to abnormal EHBD elongation (atresia) and abnormal gut rotation. The failure of foregut portions of gut to expand leaving the midgut at the level of the liver hilum may be related to defects in EHBD, intrahepatic biliary duct, or both (biliary atresia). The failure of caudal portion of EHBD to proliferate cranially with the portal mesenchyme and caudally to elongate EHBD and allow duodenal rotation may be a developmental hallmark of biliary disease. These events occur around 12th wk in humans and at about E12 in mice and gives right to partitioning of the hepatic ducts and artery/veins. AT, artery/arterialization; AV, ampulla of vater; CBD, common bile duct; CD, common duct; D, duodenum; DP, dorsal pancreas; DV, ductus venosus; GB, gallbladder; HD, hepatic duct; LV, liver; OVL, left umbilical vein; OVR, right umbilical vein; PD, pancreatic duct; S, stomach; VP, ventral pancreas.
DE, Endothelial, and Mesenchymal Interactions within the Foregut
DE, mesenchyme, and endothelium interact during development and pathogenesis (has been discussed in depth elsewhere, see ref. 6,7,8). Endothelial cells (ECs) have been shown to influence IHBD development by communicating, via paracrine mechanisms, with hepatocytes in the region of the portal mesenchyme (9). ECs embedded within the portal mesenchyme attract hepatic cells to periportal areas and release oncostatin M, which is known to induce hepatic maturation. In addition, these developmental cues depend on proper angiogenesis as angiogenic inhibitors prevent the formation of primitive foregut organs (10). Furthermore, angioblasts reside between the mesenchymal component and hepatic components of the liver. In fact, it is well known that the liver is mainly a hematopoietic organ prior to E12.5 (5), replacing the yolk sac as the main site of erythropoiesis by E12 during mouse gestation (11). This shift is induced by the migration of hematopoietic stem cells (angioblasts) into the fetal liver (called definitive erythropoiesis). Erythrocytes derived from the liver have matured from primitive erythrocytes and resemble those found in the bone marrow. The functional switch of the liver to a metabolic organ after E12.5 illustrates the potential for gene expression within one resident population of cells to influence development of the other resident/transient populations within the fetal liver microenvironment. The early liver reaches its peak volume of hematopoietic output from E13 to E14, accounting for about 70% of total hematopoiesis. By E15, this output begins to decrease and by E17.5, this has been reduced to about 30% of the total hematopoietic activity. By late gestation, the erythroid cells are near the end of their peak replicative phases, and hepatoblasts are reaching their peak of replication. These events are hallmarks of proper endodermal–mesenchymal cross talk. Such interaction among the functional components of the foregut organs is not surprising given their intimate functional and pathological relationships. The cross talk between cell types that reside in adjacent populations (endodermal–mesnchymal–endothelial cross talk) often results in distinct migratory and maturational (differentiation) cues that stimulate EMT within endodermal populations. These temporal aspects of foregut development also align with distinct but overlapping gene regulatory mechanisms (signaling cascades).
Hepatic Endoderm Induction Pathway
Hlx, Lhx2, and N-myc in the STM
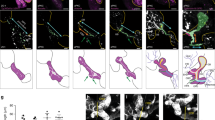
During the migration of hepatic endodermal (HE) cells into the STM, early HE cells undergo a shift in morphology from a columnar epithelium to a stellate-like appearance. It has been speculated that the STM is capable of inducing morphological changes in endodermal cell types via cell nonautonomous molecular signals (FGFs, BMPs, HGF, Hlx, and Lhx2—see Figure 2 ) that also interact with ECs within the portal mesenchyme. Furthermore, since mutations in homeobox genes expressed in the STM (Lhx2, Hlx, and Nmyc) and HE (Hhex and Prox1) produce similar hematopoietic pathologies ( Table 1 ) (12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42), they may play overlapping roles in fetal liver erythropoiesis. In fact, mutations in genes required for definitive erythropoiesis, such as Rb and C-myb, show similar hepatic defects as mutations in genes expressed in cells within the STM and HE ( Table 1 ). In summary, all of these findings support an intimate reciprocal developmental relationship (molecular and anatomical/morphological) between STM, EC, and hepatic endoderm in which paracrine signaling between these three cell compartments may regulate a complex signaling mechanism that regulate foregut development.
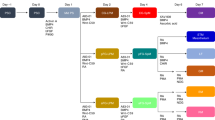
Foregut signaling cascade. The temporal aspects of foregut development can be distinguished by gene regulation within distinct cell types. In general, gene signaling from the septum transversum mesenchyme (STM) can induce the differentiation of distinct cell populations (definitive endoderm, hepatic, hepatocyte/biliary epithelial cell (BEC), and endothelial cell (EC)). In turn, these cell types provide genetic feedback to maintain hemostasis of developing organs systems throughout development. For example, genes from the STM (Hlx, Lhx2, N-myc, etc.) stimulate genes from the hepatic compartment (Hhex, Prox1, Hnf4α, Cebpa, etc.), which then regulates gene expression with the BEC (Oc1, Oc2, Hnf1b, etc.) and EC (Shh, Vegf, Epo, etc.) compartments, and suppresses pancreatic (PE) gene regulation. Such communication may define the molecular microenvironmental niche within and between developing foregut organs. Blue boxes indicate genes expressed within that tissue type and white boxes indicate which genes from those tissues positively (green) or negatively (red) influence gene regulation in other tissue types. Superscript letters a–g indicate the tissue types each gene is expressed in: amesenchyme (STM); bhepatocyte (HE); cendothelium (EC); dbiliary (BEC); epancreatic (PE); fHE/EC, and gHE/BEC. HE, hepatic endoderm.
Hhex, Prox1, and Tbx3 in HE Progenitor Cells
The homeobox gene Hhex has important developmental roles in both EC and HE cells. In the liver, Hhex is expressed in both endodermal and ECs but not in STM or definitive erythroids (43). Hhex has no effect on the development of primitive erythroids, but the absence of Hhex leads to a failure of definitive erythropoiesis both in vitro (44) and in vivo (23) (unpublished data). A role for Hhex in foregut organ development has also been observed in Zebrafish (45) and Xenopus (46). Such a role in endodermal development is quite conserved as Caenorhabditis elegans has an orthologue for Hhex (called Pha-2), which when mutated results in abnormal; pharynx development. Hhex and its orthologues likely represent a conserved mechanism for endodermal development (13,47,48). Intriguingly, other homeobox genes have been implicated at similar timepoints in HE cells and result in similar defects. Both of the homeobox genes Hhex and Prox1 have been proposed to be involved in liver specification in zebrafish and mice and mutants show similar phenotypes (13,49,50). Prox1 is not known to be expressed in ECs and the failure of the HE cells to migrate in Prox1−/− embryos may be dependent on its interaction with other HE genes (Hhex and Tbx3). Prox1 and Tbx3 may be downstream of Hhex as the emergence of the pseudostratified epithelium established at E9.0 within the STM is present in Tbx3 and Prox1 mutants but not in Hhex mutants (13). Therefore, these HE genes may interact to control EMT of HE cells at the laminin-rich membrane of the liver hilum. Furthermore, Hhex expression in endodermal cells and ECs was unchanged at E9.5 in Tbx3−/− mice, and Hlx expression in STM was also unaffected (27). These observations support the proposal for a mechanism of homeobox gene communication (between HE and STM cells) regulating early hepatic cell fate decision and indicate that hepatic differentiation from DE may be preferentially directed toward biliary epithelial cells (BEC) in the absence of homeobox signaling at E9.5 in both STM and HE cells ( Figure 2 ).
Cell Fate Choice: Biliary vs. Hepatocyte
Hepatocytes and Erythropoiesis: Cebpα and HNF4α/Erythropoietin in Hepatic Cells of the Liver
The maturation of the liver results in distinct populations of differentiated BECs and hepatocytes. The regulation of the hepatocyte/BEC cell fate decision may be in part regulated by distinct expression of Hnf4α/Cebpα and Hnf6/Hnf1β. For example, Tbx3 expression has been shown to increase Hnf4α/Cebpα, whereas expression of Hnf6 decreases Hnf4α/Cepbα. Therefore, Tbx3 and Hnf6 may work together on Hnf4α/Cebpα expression to calibrate the balance of hepatocyte vs. BEC differentiation from hepatoblasts. It has been established that Cebpα and Prox1 also represses BEC differentiation (42,50), and the regulation of Hnf4α has also been implicated in multiple aspects of liver development (though it is not required for hepatic specification). Hnf4α may be critical to reinduce a proper epithelial morphology on the endodermal cells after migration through the STM and to reduce EMT by stimulating high levels of cell adhesion genes (33). In addition to its potential role in regulating epithelial morphology in HE cells, HNF4α has also been shown to control erythropoietin (EPO)-stimulated induction of definitive erythropoiesis in the late stages of embryonic hematopoiesis (51). EPO is a protein released by hepatocytes (52) that signals via its receptor (EPOR) on primitive erythrocytes within the hematopoietic liver to induce definitive erythropoiesis. EPO directly stimulates the proliferation and survival of definitive erythrocytes in the fetal liver (51). However, it is not required for primitive erythropoiesis within the yolk sac (site for erythropoiesis before E11.5) or liver (site for erythropoiesis after E11.5). EPO activity is controlled by retinoid X receptor in the yolk sac and by both Hnf4α and retinoid X receptor in the fetal liver. Therefore, definitive erythropoiesis in the fetal liver is intimately tied to hepatocyte differentiation and may explain why defective definitive erythropoiesis is commonly observed when HE genes are mutated ( Table 1 ). Interestingly, BEC have also been shown to communicate with the endothelium at periportal areas during embryonic through adult liver development.
Biliary (Intrahepatic and Extrahepatic) Induction Pathway
Hnf6 and Hnf1β are intimately linked to the biliary developmental program in HE cells (Hes1/Notch2/Sox9) in response to mesenchymal signals (Foxf1 and Jag1—see Figure 2 ). Foxf1 is expressed in the STM around foregut organs, Hes1 is expressed within the epithelial cells of those foregut organs and Jag1 is expressed in cells within the portal mesenchyme that reside adjacent to BECs. The importance of STM vasculature has been shown in other foregut organs such as the pancreas (53), and in genetic mutations, in the endothelium (9,54,55,56). Furthermore, perturbation of the communication between Jag1 within the portal mesenchyme and Notch2 within HE cells has been implicated in diseases such as Alagille syndrome (57,58). Therefore, Jag1 within the portal STM can influence BEC differentiation and both Hnf6 and Hnf1β expression within BEC can influence the portal STM development (14,15,59,60) ( Table 1 ). Further evidence for interaction between the portal STM, endothelium, and hepatic endoderm during biliary and hepatocyte differentiation comes from the observation that deficiencies in mesenchymal (Jag1), BEC (Hnf6), and hepatocyte (Hhex) genes in the portal tract (where these three tissues types interact) all result in abnormal development. Finally, it is clear that Hhex may be upstream of many biliary and hepatocyte genes that bind Ecadherin, and therefore, Hhex may stimulate the induction of EMT in hepatic signals via communication with STM and ECs. Thus, all three cell types (STM, hepatic, and EC) share a interdependence for paracrine signaling from each other, and perturbation of genes within this signaling cascade results in functional defects within foregut organs.
Molecular Interdependence Between Foregut Endodermal Cell Types
In organs derived from foregut endoderm, three main tissue sources must interact during developmental windows in order for normal development to take place: the STM, endothelium, and the DE. It is clear that the genetic mutations specific for any one of these tissue types can result in defects within the other tissues (such as abnormal EHBD elongation and abnormal gut rotation—see Table 1 and Figure 1 ). The mesenchymal tissues adjacent to the foregut provide an overlapping microenvironment for different foregut-derived endodermal organs. As mentioned earlier, this mesenchymal component provides endothelium as well as connective tissue that act as a conduit to maintain continuity of the bile ducts during gut rotation and EHBD elongation. The failure of these tissues to properly interact can result in defective definitive erythropoiesis (hypoplastic liver, with large sinusoidal spaces, and anemia), failed gut rotation (midgut adjacent to porta hepatis, ectopic tissue, EHBD/IHBD atresia, and ductal plate malformations), and abnormal liver parenchyma (nonperiportal biliary cysts, mesenchymal and vascular disorganization) ( Table 1 ). Decreased expression of hepatocyte-related genes during liver development (Hhex, Prox1, Tbx3, Cebpα, and Hnf4α in endoderm and/or Hlx, Lhx2, and Nmyc in STM—see Table 1 and Figure 2 ) results in EHBD truncation and liver hypoplasia, defective definitive hematopoiesis (in part via defective regulation of EPO and vascular endothelial growth factor on ECs), and failed gut rotation (absence of gallbladder (GB) and ventral pancreas, and defective migration of HE cells through the STM via EMT and into the liver bud) ( Table 1 ). Decreased/absent expression of genes critical to biliary cells (Hnf6 and Hnf1β in endoderm and/or Foxf1 and Jag1 in STM—see Figure 2 ) often results in mesenchymal defects paralleled by biliary tract defects (EHBD truncation, IHBD paucity/excessive proliferation, and GB absence/paucity—see Table 1 ). Gene targeting of other genes from both mesenchymal (STM—Hlx, Foxf1, Lhx2, and Hes1/Jag1) and endodermal (Hhex, Prox1, HNF6/OC1, OC2, HNF1β, HNF4α, Cebpα, and Tbx3) compartments produce similar developmental and anatomical pathologies, further supporting the requirement for communication between and within emerging endodermal and mesenchymal (including endothelial) cell populations. Therefore, understanding the molecular interactions between the main foregut cell types (mesenchymal, endothelial, and endodermal) will aid in the diagnosis and treatment of liver diseases as well as a yield a deeper understanding of the developmental genomic profile associated with foregut maturation, for example, whether genes expressed in the STM may induce biliary vs. hepatocyte differentiation in early HE cells. From an examination of the literature, it seems that the collective anatomical and molecular data support a signaling cascade where STM (Hlx and Lhx2) communicates with early hepatic cells (Hhex, Prox1, and Tbx3) to drive hepatocyte differentiation (Hnf4α and Cebpα) and elicit definitive stages of hematopoiesis (EPO and EPOR). In addition, a similar mechanism may exist where signaling from the portal mesenchyme (Foxf1, Hes1, and Jag1) regulates the differentiation of BEC (Hnf6 and Hnf1β) during the development of the EHBD/IHBD. Interestingly, much attention has recently been given to the activity of a mesenchymal cell type called hepatic stellate cells (HSCs—also known as Ito cells). HSCs are derived from the STM (portal mesenshymal cells) of the liver and are active in the fetus and postnatally in the adult (61). HSCs reside between the parenchyme and sinusoidal epithelium and also express many of the mesenchymal genes discussed here that are associated with perturbation of the developing foregut (Hlx, Lhx2, Foxfl, Jag1, and Hes1). Surprisingly, HSCs are known to release retinoids upon their activation and RXRs are known to control erythropoiesis via EPO modulation. Therefore, it is perhaps not coincidental that EPO is regulated by Hnf4α in the liver as retinoid regulation would influence retinoid X receptor activity. Thus, HSCs may be a likely candidate for the mesenchymal component that communicates with endothelial and endodermal compartments of the liver during fetal and postnatal development. Furthermore, HSCs have also been implicated in multiple liver diseases and may represent a conserved cell type between foregut organs whose disturbance may result in pathological manifestations within distinct cell populations. Within the liver, such a relationship may exist between biliary atresia and anemia, where the paucity of EHBD/IHBD development is often observed along with anemia ( Table 1 ).
Foregut Pathology: The Overlap of Biliary Atresia and Anemia
Biliary atresia can be described as the paucity, discontinuity, or complete absence of any portion of the EHBD and IHBD trees. From the mutational models discussed here, the occurrence of biliary atresia can be associated with the following observations: failure of elongation of the EHBD (agenesis of the GB/EHBD/IHBD); small, cystic, or atresia of the ventral pancreas; absence of the extensive intestinal loop during secondary gut rotation (midgut remains adjacent to porta hepatis/liver hilum); proliferation of ducts/cysts near the liver hilum/porta hepatis (ductal plate malformation/polycystic liver disease); and defective hematopoiesis/definitive erythropoiesis (anemia/hypoplasia—large hepatic sinusoidal spaces and loose parenchyme). Biliary atresia is often associated with the continuous proliferation of primitive bile ducts at the level of the porta hepatis as the distal portions of right and left hepatic ducts and common bile duct come from EHBD (62,63). Furthermore, the continuous proliferation/dilation of primitive EHBDs around the porta hepatis may represent a failed compensatory mechanism (64) as cysts around this area are often associated with regenerative foci and influence the ability of foregut organs to produce or replace new cells (65). Most cases of biliary atresia occur at the level of the porta hepatis where defects are not isolated to the common bile duct, hilum, or IHBD alone. This type of atresia accounts for about 90% of biliary atresia cases (types 3 and 4 on the French classification scale and types 2 and 3 on the US/UK scale). Furthermore, biliary cysts at the level of the porta hepatis (portal/hilar plate) are often linked to changes in portal vein pressure, suggesting that defects in circulation at the portal vein can contribute to morphological changes within foregut development. Whether increased pressure within the portal vein is caused by crowding from excessive proliferation of BECs at the level of the porta hepatis, or vice versa, is unknown. It has been suggested that IHBD development is dependent on the presence and proper proliferation of the EHBD (66,67). Therefore, it appears that failure of caudal portion of EHBD to proliferate cranially with the portal mesenchyme and caudally to elongate EHBD ( Figure 1 ) and allow duodenal rotation may be a developmental hallmark of biliary disease. In addition, it is clear from numerous observations that the absence of the GB serves as a hallmark for developmental defects in biliary (and therefore foregut) pathology. The movement of endodermal cell populations via their expansion within the primitive midgut/foregut is critical to liver development and regeneration (EHBD/IHBD) (4,68).
In conclusion, the targeted disruption of multiple genes from each cell compartment within the developing foregut organs (mesenchyme, endothelium, and endoderm) reveals how the overlap in anatomy and function of these tissues is related to their shared interdependence on paracrine relationships. We can now begin to gain a better understanding of the molecular, anatomical, and functional manifestations of foregut endodermal pathology. Such mechanisms may initiate from within any compartment of the organs and affect surrounding cell types. The consequence of disease severity may have a temporal aspect throughout development during which distinct molecular, noncell autonomous signaling cascades regulate proper developmental events, such as hematopoiesis. Therefore, disruptions in hematopoiesis during development may occur via changes in molecular signals within different surrounding cell types.
Statement of Financial Support
This study was supported by financial assistance from National Institutes of Health (Bethesda, MD) grants DK061146-06A2 to C.W.B. and 5T32HL07272-32 to C.W.B./A.S.A.
Disclosure: Nothing to disclose.
References
Morris SA, Teo RT, Li H, Robson P, Glover DM, Zernicka-Goetz M . Origin and formation of the first two distinct cell types of the inner cell mass in the mouse embryo. Proc Natl Acad Sci USA 2010;107:6364–9.
Houssaint E . Differentiation of the mouse hepatic primordium. I. An analysis of tissue interactions in hepatocyte differentiation. Cell Differ 1980;9:269–79.
Furuyama K, Kawaguchi Y, Akiyama H, et al. Continuous cell supply from a Sox9-expressing progenitor zone in adult liver, exocrine pancreas and intestine. Nat Genet 2011;43:34–41.
Ando H . Embryology of the biliary tract. Dig Surg 2010;27:87–9.
Crawford LW, Foley JF, Elmore SA . Histology atlas of the developing mouse hepatobiliary system with emphasis on embryonic days 9.5-18.5. Toxicol Pathol 2010;38:872–906.
Apte U, Zeng G, Muller P, et al. Activation of Wnt/beta-catenin pathway during hepatocyte growth factor-induced hepatomegaly in mice. Hepatology 2006;44:992–1002.
Rossi JM, Dunn NR, Hogan BL, Zaret KS . Distinct mesodermal signals, including BMPs from the septum transversum mesenchyme, are required in combination for hepatogenesis from the endoderm. Genes Dev 2001;15:1998–2009.
Weinstein M, Monga SP, Liu Y, et al. Smad proteins and hepatocyte growth factor control parallel regulatory pathways that converge on beta1-integrin to promote normal liver development. Mol Cell Biol 2001;21:5122–31.
Sakaguchi TF, Sadler KC, Crosnier C, Stainier DY . Endothelial signals modulate hepatocyte apicobasal polarization in zebrafish. Curr Biol 2008;18:1565–71.
Tatsumi N, Miki R, Katsu K, Yokouchi Y . Neurturin-GFRalpha2 signaling controls liver bud migration along the ductus venosus in the chick embryo. Dev Biol 2007;307:14–28.
Russell ES . Hereditary anemias of the mouse: a review for geneticists. Adv Genet 1979;20:357–459.
Bhatia M, Bonnet D, Wu D, et al. Bone morphogenetic proteins regulate the developmental program of human hematopoietic stem cells. J Exp Med 1999;189:1139–48.
Bort R, Signore M, Tremblay K, Martinez Barbera JP, Zaret KS . Hex homeobox gene controls the transition of the endoderm to a pseudostratified, cell emergent epithelium for liver bud development. Dev Biol 2006;290:44–56.
Clotman F, Lannoy VJ, Reber M, et al. The onecut transcription factor HNF6 is required for normal development of the biliary tract. Development 2002;129:1819–28.
Coffinier C, Gresh L, Fiette L, et al. Bile system morphogenesis defects and liver dysfunction upon targeted deletion of HNF1beta. Development 2002;129:1829–38.
Dudas J, Papoutsi M, Hecht M, et al. The homeobox transcription factor Prox1 is highly conserved in embryonic hepatoblasts and in adult and transformed hepatocytes, but is absent from bile duct epithelium. Anat Embryol 2004;208:359–66.
Giroux S, Charron J . Defective development of the embryonic liver in N-myc-deficient mice. Dev Biol 1998;195:16–28.
Hentsch B, Lyons I, Li R, et al. Hlx homeo box gene is essential for an inductive tissue interaction that drives expansion of embryonic liver and gut. Genes Dev 1996;10:70–9.
Hilberg F, Aguzzi A, Howells N, Wagner EF . c-jun is essential for normal mouse development and hepatogenesis. Nature 1993;365:179–81.
Hofmann JJ, Zovein AC, Koh H, Radtke F, Weinmaster G, Iruela-Arispe ML . Jagged1 in the portal vein mesenchyme regulates intrahepatic bile duct development: insights into Alagille syndrome. Development 2010;137:4061–72.
Huh CG, Factor VM, Sánchez A, Uchida K, Conner EA, Thorgeirsson SS . Hepatocyte growth factor/c-met signaling pathway is required for efficient liver regeneration and repair. Proc Natl Acad Sci USA 2004;101:4477–82.
Hunter MP, Wilson CM, Jiang X, et al. The homeobox gene Hhex is essential for proper hepatoblast differentiation and bile duct morphogenesis. Dev Biol 2007;308:355–67.
Keng VW, Yagi H, Ikawa M, et al. Homeobox gene Hex is essential for onset of mouse embryonic liver development and differentiation of the monocyte lineage. Biochem Biophys Res Commun 2000;276:1155–61.
Kolterud A, Wandzioch E, Carlsson L . Lhx2 is expressed in the septum transversum mesenchyme that becomes an integral part of the liver and the formation of these cells is independent of functional Lhx2. Gene Expr Patterns 2004;4:521–8.
Lee EY, Chang CY, Hu N, et al. Mice deficient for Rb are nonviable and show defects in neurogenesis and haematopoiesis. Nature 1992;359:288–94.
Li J, Ning G, Duncan SA . Mammalian hepatocyte differentiation requires the transcription factor HNF-4alpha. Genes Dev 2000;14:464–74.
Lüdtke TH, Christoffels VM, Petry M, Kispert A . Tbx3 promotes liver bud expansion during mouse development by suppression of cholangiocyte differentiation. Hepatology 2009;49:969–78.
Mahlapuu M, Enerbäck S, Carlsson P . Haploinsufficiency of the forkhead gene Foxf1, a target for sonic hedgehog signaling, causes lung and foregut malformations. Development 2001;128:2397–406.
Margagliotti S, Clotman F, Pierreux CE, et al. The Onecut transcription factors HNF-6/OC-1 and OC-2 regulate early liver expansion by controlling hepatoblast migration. Dev Biol 2007;311:579–89.
Mucenski ML, McLain K, Kier AB, et al. A functional c-myb gene is required for normal murine fetal hepatic hematopoiesis. Cell 1991;65:677–89.
Ormestad M, Astorga J, Carlsson P . Differences in the embryonic expression patterns of mouse Foxf1 and -2 match their distinct mutant phenotypes. Dev Dyn 2004;229:328–33.
Ormestad M, Astorga J, Landgren H, et al. Foxf1 and Foxf2 control murine gut development by limiting mesenchymal Wnt signaling and promoting extracellular matrix production. Development 2006;133:833–43.
Parviz F, Matullo C, Garrison WD, et al. Hepatocyte nuclear factor 4alpha controls the development of a hepatic epithelium and liver morphogenesis. Nat Genet 2003;34:292–6.
Schmidt C, Bladt F, Goedecke S, et al. Scatter factor/hepatocyte growth factor is essential for liver development. Nature 1995;373:699–702.
Shin D, Shin CH, Tucker J, et al. Bmp and Fgf signaling are essential for liver specification in zebrafish. Development 2007;134:2041–50.
Sonnenberg E, Meyer D, Weidner KM, Birchmeier C . Scatter factor/hepatocyte growth factor and its receptor, the c-met tyrosine kinase, can mediate a signal exchange between mesenchyme and epithelia during mouse development. J Cell Biol 1993;123:223–35.
Sosa-Pineda B, Wigle JT, Oliver G . Hepatocyte migration during liver development requires Prox1. Nat Genet 2000;25:254–5.
Sumazaki R, Shiojiri N, Isoyama S, et al. Conversion of biliary system to pancreatic tissue in Hes1-deficient mice. Nat Genet 2004;36:83–7.
Tomizawa M, Garfield S, Factor V, Xanthopoulos KG . Hepatocytes deficient in CCAAT/enhancer binding protein alpha (C/EBP alpha) exhibit both hepatocyte and biliary epithelial cell character. Biochem Biophys Res Commun 1998;249:1–5.
Wu H, Liu X, Jaenisch R, Lodish HF . Generation of committed erythroid BFU-E and CFU-E progenitors does not require erythropoietin or the erythropoietin receptor. Cell 1995;83:59–67.
Xue Y, Gao X, Lindsell CE, et al. Embryonic lethality and vascular defects in mice lacking the Notch ligand Jagged1. Hum Mol Genet 1999;8:723–30.
Yamasaki H, Sada A, Iwata T, et al. Suppression of C/EBPalpha expression in periportal hepatoblasts may stimulate biliary cell differentiation through increased Hnf6 and Hnf1b expression. Development 2006;133:4233–43.
Bedford FK, Ashworth A, Enver T, Wiedemann LM . HEX: a novel homeobox gene expressed during haematopoiesis and conserved between mouse and human. Nucleic Acids Res 1993;21:1245–9.
Paz H, Lynch MR, Bogue CW, Gasson JC . The homeobox gene Hhex regulates the earliest stages of definitive hematopoiesis. Blood 2010;116:1254–62.
Wallace KN, Yusuff S, Sonntag JM, Chin AJ, Pack M . Zebrafish hhex regulates liver development and digestive organ chirality. Genesis 2001;30:141–3.
Zhao H, Han D, Dawid IB, Pieler T, Chen Y . Homeoprotein hhex-induced conversion of intestinal to ventral pancreatic precursors results in the formation of giant pancreata in Xenopus embryos. Proc Natl Acad Sci USA 2012;109:8594–9.
Dickhoff WW, Darling DS . Evolution of thyroid function and its control in lower vertebrates. Amer Zool 1983;23:697–707.
Mörck C, Rauthan M, Wågberg F, Pilon M . pha-2 encodes the C. elegans ortholog of the homeodomain protein HEX and is required for the formation of the pharyngeal isthmus. Dev Biol 2004;272:403–18.
Bort R, Martinez-Barbera JP, Beddington RS, Zaret KS . Hex homeobox gene-dependent tissue positioning is required for organogenesis of the ventral pancreas. Development 2004;131:797–806.
Ober EA, Verkade H, Field HA, Stainier DY . Mesodermal Wnt2b signalling positively regulates liver specification. Nature 2006;442:688–91.
Makita T, Hernandez-Hoyos G, Chen TH, Wu H, Rothenberg EV, Sucov HM . A developmental transition in definitive erythropoiesis: erythropoietin expression is sequentially regulated by retinoic acid receptors and HNF4. Genes Dev 2001;15:889–901.
Koury MJ, Bondurant MC . The mechanism of erythropoietin action. Am J Kidney Dis 1991;18:Suppl 1:20–3.
Lammert E, Cleaver O, Melton D . Role of endothelial cells in early pancreas and liver development. Mech Dev 2003;120:59–64.
Cleaver O, Melton DA . Endothelial signaling during development. Nat Med 2003;9:661–8.
Matsumoto K, Yoshitomi H, Rossant J, Zaret KS . Liver organogenesis promoted by endothelial cells prior to vascular function. Science 2001;294:559–63.
Coultas L, Chawengsaksophak K, Rossant J . Endothelial cells and VEGF in vascular development. Nature 2005;438:937–45.
McCright B, Lozier J, Gridley T . A mouse model of Alagille syndrome: Notch2 as a genetic modifier of Jag1 haploinsufficiency. Development 2002;129:1075–82.
Tanimizu N, Miyajima A . Notch signaling controls hepatoblast differentiation by altering the expression of liver-enriched transcription factors. J Cell Sci 2004;117(Pt 15):3165–74.
Clotman F, Libbrecht L, Gresh L, et al. Hepatic artery malformations associated with a primary defect in intrahepatic bile duct development. J Hepatol 2003;39:686–92.
Lemaigre FP . Development of the biliary tract. Mech Dev 2003;120:81–7.
Friedman SL . Hepatic stellate cells: protean, multifunctional, and enigmatic cells of the liver. Physiol Rev 2008;88:125–72.
Tan CE, Moscoso GJ . The developing human biliary system at the porta hepatis level between 11 and 25 weeks of gestation: a way to understanding biliary atresia. Part 2. Pathol Int 1994;44:600–10.
Tan CE, Moscoso GJ . The developing human biliary system at the porta hepatis level between 29 days and 8 weeks of gestation: a way to understanding biliary atresia. Part 1. Pathol Int 1994;44:587–99.
Sutton ME, op den Dries S, Koster MH, Lisman T, Gouw AS, Porte RJ . Regeneration of human extrahepatic biliary epithelium: the peribiliary glands as progenitor cell compartment. Liver Int 2012;32:554–9.
Shneider BL, Mazariegos GV . Biliary atresia: a transplant perspective. Liver Transpl 2007;13:1482–95.
Roskams T, Desmet V . Embryology of extra- and intrahepatic bile ducts, the ductal plate. Anat Rec (Hoboken) 2008;291:628–35.
Zong Y, Stanger BZ . Molecular mechanisms of bile duct development. Int J Biochem Cell Biol 2011;43:257–64.
Irie T, Asahina K, Shimizu-Saito K, Teramoto K, Arii S, Teraoka H . Hepatic progenitor cells in the mouse extrahepatic bile duct after a bile duct ligation. Stem Cells Dev 2007;16:979–87.
Author information
Authors and Affiliations
Corresponding author
PowerPoint slides
Rights and permissions
About this article
Cite this article
Arterbery, A., Bogue, C. Endodermal and mesenchymal cross talk: a crossroad for the maturation of foregut organs. Pediatr Res 75, 120–126 (2014). https://doi.org/10.1038/pr.2013.201
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2013.201
This article is cited by
-
A role for E-cadherin in ensuring cohesive migration of a heterogeneous population of non-epithelial cells
Nature Communications (2015)