Abstract
Background:
Exhaled nitric oxide (eNO) is an endogenous gas involved in airway pathophysiology and is determined in orally exhaled air by various techniques. However, traditional single-breath technique (eNOSB) requires active cooperation and is not always easily practicable (especially in young children); simpler techniques including tidal breathing measurements (eNOTB) are not standardized. The aim of this study was to evaluate the possible correlation and correspondence between eNOSB and eNOTB and the impact of potential confounders in children with chronic adenotonsillar disease.
Methods:
Eighty-six children (mean age 8.7 ± 3.2 y) underwent eNO assessment by means of eNOSB and eNOTB. The correlation among eNOTB, eNOSB, and other potential confounders (i.e., gender, age, weight, height, BMI, and passive smoking exposure) were studied.
Results:
The analyses showed a poor correspondence between eNOSB and eNOTB, with the latter underestimating (P < 0.001) mean eNO values: 6.4 parts per billion (ppb) (95% confidence interval (CI): 8.4–11.4 ppb) vs. 9.8 ppb (95% CI: 5.6–7.3 ppb). A greater correlation was found between eNOSB and eNOTB in children younger than 6 y. Only eNOSB and age predicted eNOTB (R2 = 43.6%).
Conclusion:
eNOTB is not a good predictor of eNOSB in children. Constant-flow eNOSB is the technique of choice for eNO assessment in young children.
Similar content being viewed by others
Main
Nitric oxide (NO) is an endogenous gas involved in airway pathophysiology and is produced in the upper and lower airways as a result of the NO synthase (NOS) catalysis of L-arginine. It can be determined in orally exhaled and nasal air by means of various noninvasive techniques (1,2).
Orally exhaled NO (eNO) is mainly involved in important phlogistic pathways in the lower airways and can be considered a marker of inflammation in asthmatic patients (3). Increased eNO levels have been found in patients with allergic rhinitis (4) and upper respiratory tract viral infections (5) and reduced eNO levels have been found in patients with cystic fibrosis and primary ciliary dyskinesia (6). Furthermore, NO pathways are thought to be involved in the pathogenesis of chronic adenoidal disease because high nasal NO levels have been found in children with adenoidal hypertrophy (7), whereas contrasting results have been found in children with chronic tonsillar disease (8,9).
The assessment of eNO is not used in routine pediatric practice because it is not always easily practicable to follow the international guidelines (1,2). Traditional eNO measurement of oral exhalation against resistance (the single-breath technique, eNOSB) is considered the standard procedure by the American Thoracic Society (2) because it has several advantages: a constant flow is maintained, which is useful because eNO is a flow-dependent variable (10); exhalation from total lung capacity is important because the degree of lung expansion affects eNO values measured at the same flow rate (10); and contamination with nasal NO is avoided because of the induced velum closure when exhaling against resistance (10).
However, correct eNOSB performance requires the active cooperation of patients, which is not always easily achieved, especially in the case of young children (1). For this reason, simpler but less standardized techniques have been introduced in an attempt to overcome the poor compliance of children, including tidal-breath eNO measurements (eNOTB) with or without flow control, and offline reservoir sampling (1,11,12,13). Unfortunately, these do not provide accurate data because they have some methodological drawbacks, such as the use of uncontrolled expiratory flow and nasal NO contamination (1). Furthermore, previous studies (11,12,13) of eNO levels assessed by means of eNOSB and eNOTB with or without the use of sampling bags in infants or children with bronchopulmonary disease have yielded conflicting results.
The aim of this study was to evaluate the possible correlation and correspondence between eNOSB and eNOTB measurements and the impact of potential confounders in children with chronic adenotonsillar disease.
Results
As shown in Figure 1 , 184 children were considered eligible for enrollment, but the final analyses were based on the measurements of 86 children (53.5% males; mean age 8.7 ± 3.2 y) whose main characteristics are summarized in Table 1 .
Although the coefficient of variation was the same for both techniques (33.4%), the geometric mean of eNOTB was significantly less than that of eNOSB: 6.4 ppb (95% confidence interval: (CI) 8.4–11.4) vs. 9.8 ppb (95% CI: 5.6–7.3) (P < 0.001). The underestimates of the eNOTB values in comparison with the eNOSB values are shown in Figure 2 : 76% of the eNOTB values were under the bisectrix indicating perfect correspondence.
Only eNOSB and age were predictors of eNOTB; the R2 of 43.6% suggests that the model explains slightly less than half of the variability of eNOTB. The scatter plots of the values predicted by the final equations, ln(eNOTB) = f[age, ln(eNOSB)] vs. ln(eNOSB) and residuals vs. ln(eNOSB), are shown in Figure 3 and confirm the underestimated eNOTB values. They also show that the correlation between eNOSB and eNOTB values was higher in children younger than 6 y and that the discrepancy between the two techniques increased with age ( Figure 4 ).
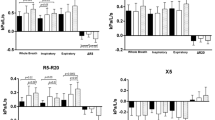
Relationship between predicted eNOTB and observed eNOSB values. (a) Scatter plots of the values predicted by the final equation ln(eNOTB) = f (age, ln(eNOSB)) vs. ln(eNOSB). (b) Scatter plots of the residuals from the final equation ln(eNOTB) = f (age, ln(eNOSB)) vs. ln(eNOSB). eNO, exhaled nitric oxide; SB, single breath; TB, tidal breath.
Scatter plots of the values predicted by the final equation ln(eNOTB) = f (age, ln(eNOSB)) vs. ln(eNOSB). (a) Triangles, children ≤ 6 y (n = 21). ln(eNOTB) = 0.93 × ln(eNOSB) (CI90% (β) = (0.86–1.00)). (b) Squares, children 7–9 y (n = 40). ln(eNOTB) = 0.79 × ln(eNOSB) (CI90% (β) = (0.75–0.83)). (c) Diamonds, children ≥10 y (n = 25). ln(eNOTB) = 0.73 × ln(eNOSB) (CI90% (β) = (0.68–0.77)). Line, bisector; dotted line, interpolating straight line. CI90%, 90% confidence interval; eNO, exhaled nitric oxide; SB, single breath; TB, tidal breath.
However, the differences between eNOSB and eNOTB led to the misclassification of normal and pathological values in every age class. When eNO was assessed using the tidal breathing technique, ~50% of the patients whose eNOSB values were in the normal range would have been considered pathological cases, and 19% of those whose eNOSB values were out of the normal range would have been considered normal. As a matter of fact, correct responses occurred in 55.8% of cases when the population was considered as a whole; when considered by age class, correct responses occurred in 52.4% of the children aged 4–7 y, in 52.5% of those aged 8–13 y, and in 64.0% of those aged 14–17 y.
Discussion
The assessment of eNO levels could be very useful in clinical practice for diagnostic purposes and for monitoring respiratory diseases such as airway inflammation (3,6,14), adenoidal disease (7), and rhino-sinusitis (15). The international guidelines recommend eNOSB as the “gold standard” technique (1) on the grounds of its accuracy and reproducibility (10). However, the active cooperation required to achieve the lasting expiratory force necessary to perform the test correctly makes it impossible in some patients, especially preschool children (16), as was found in ~45% of our enrolled patients who had a mean age of 3.6 ± 0.5 y.
Practical difficulties in assessing eNOSB in pediatric populations have been previously reported by other investigators (11,17), including Jöbsis et al. (11) who found that 29% of 101 children with a mean age of 11.7 y were unable to perform the test. These difficulties have led to the introduction of simpler but less standardized means of assessing eNO, including eNOTB measurements (11,13), but these have the disadvantages of variable expiratory flow and the impossibility of excluding nasal NO (1,18).
We therefore evaluated the correlation and correspondence between eNOTB and eNOSB values in children, also considering the other variables known to influence eNO levels, such as gender, age, height, weight, BMI, and passive smoking exposure (2), in order to assess the possibility of using eNOTB in pediatric clinical practice.
As expected (on the basis of the fact that both techniques evaluate eNO levels), our findings showed a certain correlation (good correlation occurred when eNOSB and eNOTB systematically varied together) between eNOSB and eNOTB in 86 children with chronic adenotonsillar disease (70% of whom were younger than 9 y).
However, our results showed that a good correspondence (good correspondence occurred when eNOSB and eNOTB gave the same response) between the eNO measurements was obtained neither when the population was analyzed as a whole nor when it was analyzed by age class.
In comparison with eNOSB, eNOTB systematically underestimated eNO values, as also shown by the statistically significant difference in their mean values of 9.8 and 6.4 ppb, respectively. Furthermore, the underestimated eNOTB values seem to be more pronounced at higher values (see Figure 3 ), which is in line with the findings of Franklin et al. (12). The systematic underestimation of eNO values by eNOTB is not easily interpreted and should be considered cautiously. Contamination with nasal NO, which is increased in children with adenoidal disease (7), should theoretically increase rather than decrease the eNO levels measured during tidal breathing. However, it must be remembered that eNO levels vary with flow (10), and the multiple respirations without flow control during eNOTB lead to considerable differences between the levels determined by the two techniques.
Our results add to the debate concerning the conflicting results from previous studies comparing eNO levels as measured by means of eNOSB and eNOTB in pediatric patients with lower airway diseases (11,19). Jöbsis et al. (11) and Franklin et al. (12) found that agreement between eNOSB and eNOTB was poor in asthmatic children and in infants with recurrent wheeze, recurrent cough, or no respiratory symptoms. Our findings confirm this in pediatric patients with chronic upper airway disease. To the best of our knowledge, only Daniel et al. (13) did not find any significant difference between eNOSB and eNOTB (using a facemask) in a small case series of 11 children aged 8–12 y.
Among all the variables assessed, only age significantly changed the correlation between eNOSB and eNOTB. In particular, the greatest discrepancy between the eNOSB and eNOTB values was observed in children older than 6 y, whose eNOSB values were generally higher than their eNOTB values ( Figure 4 ). It can be speculated that nasal contamination during eNOTB is more significant in younger children because they are more frequently affected by adenoidal disease (20), which is responsible for increased nasal NO levels (7). This may explain the reduced difference between eNOSB and eNOTB values in children younger than 6 y.
In conclusion, our results showed that although there was a certain correlation between eNOSB and eNOTB, eNOTB cannot be considered a good predictor of eNOSB in children with chronic adenotonsillar disease on the basis of its poor correspondence even when it was adjusted for age. On the basis of our results, and given the dependence of eNO levels on expiratory flow, constant-flow eNOSB should be considered the technique of choice for eNO assessment in young children with chronic upper airway disease, and clinicians should question the reliability of eNOTB.
Methods
Patients and Setting
The study involved 184 consecutive children aged 3–17 y, who attended the Otorhinolaryngological Unit of the University of Milan’s Department of Clinical Sciences and Community Health between January 2008 and May 2009 because of chronic adenoidal and/or tonsillar disease. Chronic adenoiditis was defined as adenoidal hypertrophy (assessed by means of flexible nasopharyngeal endoscopy) with ongoing nasopharyngeal inflammation/infection (i.e., at least three episodes of acute adenoiditis requiring antibiotic therapy in a period of 6 mo or at least four episodes in the previous year) (21), persistent mucous secretion on the adenoidal surface, and/or persistent otitis media with effusion (persistent middle ear effusion for at least 3 mo, without any sign of concomitant acute inflammation) (22), and/or recurrent acute otitis media (i.e., a history of at least three documented episodes in the previous 6 mo or at least four in the previous year) (23). Chronic tonsillitis was defined as severe recurrent tonsillar infections (at least seven episodes of acute tonsillitis in the previous year, at least five episodes per year for 2 consecutive years, or at least three episodes per year for at least 3 consecutive years) (24).
Exclusion criteria were as follows: an inability to perform eNOSB or eNOTB; allergic asthma or chronic airway diseases (25); acute respiratory infections during the previous 30 d and/or the administration of systemic antibiotics and/or steroids or other medications affecting the airways (e.g., inhaled steroids, nasal steroids, or decongestants) during the previous month; systemic diseases (e.g., cystic fibrosis, primary ciliary dyskinesia, and primary or secondary immunodeficiency) (21); and parental refusal to participate.
The protocol was approved by the University of Milan’s Ethics Committee, and written informed consent was obtained from the children’s parents or their legal guardians.
Intervention
Gender, age, weight (W), height (H), BMI (computed as W(kg)/H2(m2)), and passive smoking exposure (defined as whether parental figures such as mother, father, stepfather, or mother’s partner, and stepmother or father’s partner smoked in the home every day or sometimes) (19) were recorded for each patient, and the children underwent eNOSB and eNOTB determinations by means of a dedicated chemiluminescence analyzer (CDL 88 sp, Ecomedics, Dürnten, Suisse). At the parent’s discretion, the child was comfortably seated on a chair or on the parent’s knee. The child was encouraged to breathe only through his/her mouth and to breathe quietly for some minutes so as to acclimatize. The eNOTB measurement was made first using an online method of tidal breathing: the child was asked to perform oral tidal breathing continuously through a disposable mouthpiece connected to the CDL 88 sp by means of a two-way valve. The exercise was repeated three times separated by at least 30 s of rest. The recorded eNOTB level, expressed in parts per billion (ppb), was the geometric mean of the three values obtained.
eNOSB measurement was made using an online, constant flow method in accordance with the international guidelines (1,2). The child was encouraged to inhale NO-free air (<5 ppb) orally for 2–3 s to total lung capacity from a disposable mouthpiece connected to the analyzer by means of a two-way valve and then to exhale orally for >4 s without holding the breath at a constant flow rate (50 ml/s) through an expiratory resistance, targeting a mouth pressure of 10 cm H2O in order to close the velum and avoid nasal contamination. The test ended with another oral inhalation through the CDL 88 sp. The children were helped to maintain a constant expiratory flow rate by means of a real-time visual aid, and eNOSB was computed when an eNOSB plateau of >2 s could be identified during exhalation. The eNOSB level was recorded after three exhalations were repeated after intervals of >30 s. The analyzer was calibrated every 2 wk using certified 2,000 ppb calibration gas.
The correspondence between the eNOSB and eNOTB levels classifying patients as normal or pathological was assessed on the basis of published normal values for age classes, i.e., 5–8 ppb in children aged 4–7 y; 8–16 ppb in children aged 8–13 y; and 10–13 ppb in children aged 14–17 y (26,27,28,29,30).
Statistical Analysis
Because the eNOSB and eNOTB values were not normally distributed, log-transformed data were used for the analyses. The eNOSB and eNOTB data are given as geometric mean values with 95% CIs; the height and weight data as median values and interquartile ranges; and the other variables as frequencies (absolute numbers and percentages).
Multivariable linear regression models were used to examine the correlation among eNOTB, eNOSB, and the other potential confounders such as gender, age (continuous), height (continuous), weight (continuous), BMI, and passive smoking exposure. The goodness of fit of the models was evaluated using the coefficient of determination (R2). A P value of <0.10 was considered statistically significant. Data processing and all of the statistical analyses were performed by using the SAS software (version 9.1, SAS Institute, Cary, North Carolina).
Statement of Financial Support
No financial support from extramural sources was received for this study.
References
Baraldi E, de Jongste JC; European Respiratory Society/American Thoracic Society (ERS/ATS) Task Force. Measurement of exhaled nitric oxide in children, 2001. Eur Respir J 2002;20:223–37.
American Thoracic Society, European Respiratory Society. ATS/ERS recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide, 2005. Am J Respir Crit Care Med 2005;171:912–30.
Kharitonov SA, Yates D, Robbins RA, Logan-Sinclair R, Shinebourne EA, Barnes PJ . Increased nitric oxide in exhaled air of asthmatic patients. Lancet 1994;343:133–5.
Martin U, Bryden K, Devoy M, Howarth P . Increased levels of exhaled nitric oxide during nasal and oral breathing in subjects with seasonal rhinitis. J Allergy Clin Immunol 1996;97:768–72.
Kharitonov SA, Yates D, Barnes PJ . Increased nitric oxide in exhaled air of normal human subjects with upper respiratory tract infections. Eur Respir J 1995;8:295–7.
Hofer M, Mueller L, Rechsteiner T, Benden C, Boehler A . Extended nitric oxide measurements in exhaled air of cystic fibrosis and healthy adults. Lung 2009;187:307–13.
Torretta S, Bossi A, Capaccio P, et al. Nasal nitric oxide in children with adenoidal hypertrophy: a preliminary study. Int J Pediatr Otorhinolaryngol 2010;74:689–93.
Torretta S, Marchisio P, Esposito S, et al. Exhaled nitric oxide levels in children with chronic adenotonsillar disease. Int J Immunopathol Pharmacol 2011;24:471–80.
Kasperska-Zajac A, Brzoza Z, Czecior E, Rogala B, Polok A, Namyslowski G . Elevated levels of exhaled nitric oxide in recurrent tonsillitis. Eur Respir J 2008;31:909–10.
Silkoff PE, McClean PA, Slutsky AS, et al. Marked flow-dependence of exhaled nitric oxide using a new technique to exclude nasal nitric oxide. Am J Respir Crit Care Med 1997;155:260–7.
Jöbsis Q, Schellekens SL, Kroesbergen A, Hop WC, de Jongste JC . Sampling of exhaled nitric oxide in children: end-expiratory plateau, balloon and tidal breathing methods compared. Eur Respir J 1999;13:1406–10.
Franklin PJ, Turner SW, Mutch RC, Stick SM . Comparison of single-breath and tidal breathing exhaled nitric oxide levels in infants. Eur Respir J 2004;23:369–72.
Daniel PF, Klug B, Valerius NH . Measurement of exhaled nitric oxide in young children during tidal breathing through a facemask. Pediatr Allergy Immunol 2005;16:248–53.
Scadding G, Scadding GK . Update on the use of nitric oxide as a noninvasive measure of airways inflammation. Rhinology 2009;47:115–20.
Carraro S, Cutrone C, Cardarelli C, Zanconato S, Baraldi E . Clinical application of nasal nitric oxide measurement. Int J Immunopathol Pharmacol 2010;23:Suppl 1:50–2.
Kissoon N, Duckworth LJ, Blake KV, Murphy SP, Taylor CL, Silkoff PE . FE(NO): relationship to exhalation rates and online versus bag collection in healthy adolescents. Am J Respir Crit Care Med 2000;162(2 Pt 1):539–45.
Canady RG, Platts-Mills T, Murphy A, Johannesen R, Gaston B . Vital capacity reservoir and online measurement of childhood nitrosopnea are linearly related. Clinical implications. Am J Respir Crit Care Med 1999;159:311–4.
Franklin PJ, Turner SW, Mutch RC, Stick SM . Measuring exhaled nitric oxide in infants during tidal breathing: methodological issues. Pediatr Pulmonol 2004;37:24–30.
Holliday JC, Moore GF, Moore LA . Changes in child exposure to secondhand smoke after implementation of smoke-free legislation in Wales: a repeated cross-sectional study. BMC Public Health 2009;9:430.
Cassano P, Gelardi M, Cassano M, Fiorella ML, Fiorella R . Adenoid tissue rhinopharyngeal obstruction grading based on fiberendoscopic findings: a novel approach to therapeutic management. Int J Pediatr Otorhinolaryngol 2003;67:1303–9.
Marseglia GL, Poddighe D, Caimmi D, et al. Role of adenoids and adenoiditis in children with allergy and otitis media. Curr Allergy Asthma Rep 2009;9:460–4.
American Academy of Pediatrics. Subcommittee on management of otitis media with effusion. Otitis media with effusion. Pediatrics 2004;113:1412–29.
American Academy of Pediatrics. Subcommittee on management of acute otitis media. Diagnosis and management of acute otitis media. Pediatrics 2004;113:1451–65.
Paradise JL, Bluestone CD, Bachman RZ, et al. Efficacy of tonsillectomy for recurrent throat infection in severely affected children. Results of parallel randomized and nonrandomized clinical trials. N Engl J Med 1984;310:674–83.
Kharitonov SA, Rajakulasingam K, O’Connor B, Durham SR, Barnes PJ . Nasal nitric oxide is increased in patients with asthma and allergic rhinitis and may be modulated by nasal glucocorticoids. J Allergy Clin Immunol 1997;99(1 Pt 1):58–64.
Franklin PJ, Taplin R, Stick SM . A community study of exhaled nitric oxide in healthy children. Am J Respir Crit Care Med 1999;159:69–73.
Kharitonov SA, Gonio F, Kelly C, Meah S, Barnes PJ . Reproducibility of exhaled nitric oxide measurements in healthy and asthmatic adults and children. Eur Respir J 2003;21:433–8.
Buchvald F, Baraldi E, Carraro S, et al. Measurements of exhaled nitric oxide in healthy subjects age 4 to 17 years. J Allergy Clin Immunol 2005;115:1130–6.
Malmberg LP, Petäys T, Haahtela T, et al. Exhaled nitric oxide in healthy nonatopic school-age children: determinants and height-adjusted reference values. Pediatr Pulmonol 2006;41:635–42.
Kovesi T, Kulka R, Dales R . Exhaled nitric oxide concentration is affected by age, height, and race in healthy 9- to 12-year-old children. Chest 2008;133:169–75.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Torretta, S., Bossi, A., Brevi, A. et al. Head-to-head comparison of single-breath and tidal-breath exhaled nitric oxide measurements. Pediatr Res 73, 221–225 (2013). https://doi.org/10.1038/pr.2012.164
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2012.164