Abstract
Congenital defects most-commonly affect the heart, with an estimated incidence of up to 10 in 1,000 live births. Over the past few decades, mortality has decreased and subsequent survival has increased; approximately 90% of all patients with congenital heart disease (CHD) reach adulthood. Echocardiography is sufficient in most cases for prenatal and postnatal diagnosis of CHD and to plan an intervention, with cardiac MRI and CT providing complementary information on vascular and extracardiac abnormalities. During follow-up, cardiovascular dysfunction is an important cause of reintervention and death. Therefore, routine evaluation of systolic, diastolic, valvular, and vascular function is essential in the care of patients with CHD. Application of echocardiography, cardiac MRI, and CT during follow-up of patients with CHD ideally identifies patients at risk of adverse outcomes, and elucidates the pathophysiological mechanisms that underlie cardiovascular dysfunction. The advent of advanced imaging strategies might further improve the detection of subclinical cardiovascular failure, although further study is required to establish the value of these techniques. Finally, imaging beyond the heart is essential for the complete understanding of the interaction between CHD and noncardiac organ systems, and to extend the success of increased survival to improvements in long-term functional outcome.
Key Points
-
Over the past few decades, survival has increased among patients with congenital heart disease
-
Advances in echocardiography, cardiac MRI, and CT limit the need for invasive studies
-
Noninvasive imaging at diagnosis assists with planning intervention
-
Monitoring of cardiovascular dysfunction is essential during follow-up
-
Imaging identifies patients who are at risk of adverse outcomes
-
Imaging beyond the heart identifies important noncardiac abnormalities
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Yang, Q., Khoury, M. J. & Mannino, D. Trends and patterns of mortality associated with birth defects and genetic diseases in the United States, 1979–1992: an analysis of multiple-cause mortality data. Genet. Epidemiol. 14, 493–505 (1997).
Hoffman, J. I. & Kaplan, S. The incidence of congenital heart disease. J. Am. Coll. Cardiol. 39, 1890–1900 (2002).
Samanek, M. Children with congenital heart disease: probability of natural survival. Pediatr. Cardiol. 13, 152–158 (1992).
Khairy, P. et al. Changing mortality in congenital heart disease. J. Am. Coll. Cardiol. 56, 1149–1157 (2010).
Gilboa, S. M., Salemi, J. L., Nembhard, W. N., Fixler, D. E. & Correa, A. Mortality resulting from congenital heart disease among children and adults in the United States, 1999 to 2006. Circulation 122, 2254–2263 (2010).
Moons, P., Bovijn, L., Budts, W., Belmans, A. & Gewillig, M. Temporal trends in survival to adulthood among patients born with congenital heart disease from 1970 to 1992 in Belgium. Circulation 122, 2264–2272 (2010).
Stark, J. Do we really correct congenital heart defects? J. Thorac. Cardiovasc. Surg. 97, 1–9 (1989).
Regitz-Zagrosek, V. et al. ESC guidelines on the management of cardiovascular diseases during pregnancy: the Task Force on the management of cardiovascular diseases during pregnancy of the European Society of Cardiology (ESC). Eur. Heart J. http://dx.doi.org/10.1093/eurheartj/ehr218.
Grotenhuis, H. B. & de Roos, A. Structure and function of the aorta in inherited and congenital heart disease and the role of MRI. Heart 97, 66–74 (2011).
Hope, M. D., Hope, T. A., Urbania, T. H. & Higgins, C. B. Four-dimensional flow magnetic resonance imaging with wall shear stress analysis before and after repair of aortopulmonary fistula. Circ. Cardiovasc. Imaging 3, 766–768 (2010).
Oosterhof, T. et al. Preoperative thresholds for pulmonary valve replacement in patients with corrected tetralogy of Fallot using cardiovascular magnetic resonance. Circulation 116, 545–551 (2007).
Geva, T., Sandweiss, B. M., Gauvreau, K., Lock, J. E. & Powell, A. J. Factors associated with impaired clinical status in long-term survivors of tetralogy of Fallot repair evaluated by magnetic resonance imaging. J. Am. Coll. Cardiol. 43, 1068–1074 (2004).
Ghai, A. et al. Left ventricular dysfunction is a risk factor for sudden cardiac death in adults late after repair of tetralogy of Fallot. J. Am. Coll. Cardiol. 40, 1675–1680 (2002).
Khairy, P. et al. Long-term survival, modes of death, and predictors of mortality in patients with Fontan surgery. Circulation 117, 85–92 (2008).
Winter, M. M. et al. Ventricular response to stress predicts outcome in adult patients with a systemic right ventricle. Am. Heart J. 160, 870–876 (2010).
Driscoll, D. et al. Guidelines for evaluation and management of common congenital cardiac problems in infants, children, and adolescents. A statement for healthcare professionals from the Committee on Congenital Cardiac Defects of the Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 90, 2180–2188 (1994).
Bonow, R. O. et al. 2008 focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to revise the 1998 guidelines for the management of patients with valvular heart disease). Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J. Am. Coll. Cardiol. 52, e1–e142 (2008).
Prakash, A., Powell, A. J. & Geva, T. Multimodality noninvasive imaging for assessment of congenital heart disease. Circ. Cardiovasc. Imaging 3, 112–125 (2010).
Randolph, G. R. et al. Intraoperative transesophageal echocardiography during surgery for congenital heart defects. J. Thorac. Cardiovasc. Surg. 124, 1176–1182 (2002).
Rigby, M. L. Transoesophageal echocardiography during interventional cardiac catheterisation in congenital heart disease. Heart 86 (Suppl. 2), II23–II29 (2001).
Wilkoff, B. L. et al. Magnetic resonance imaging in patients with a pacemaker system designed for the magnetic resonance environment. Heart Rhythm. 8, 65–73 (2011).
Kroft, L. J., Roelofs, J. J. & Geleijns, J. Scan time and patient dose for thoracic imaging in neonates and small children using axial volumetric 320-detector row CT compared to helical 64-, 32-, and 16- detector row CT acquisitions. Pediatr. Radiol. 40, 294–300 (2010).
Baumgartner, H. et al. ESC Guidelines for the management of grown-up congenital heart disease (new version 2010). Eur. Heart J. 31, 2915–2957 (2010).
Lange, L. W. et al. Qualitative real-time cross-sectional echocardiographic imaging of the human fetus during the second half of pregnancy. Circulation 62, 799–806 (1980).
Kleinman, C. S., Hobbins, J. C., Jaffe, C. C., Lynch, D. C. & Talner, N. S. Echocardiographic studies of the human fetus: prenatal diagnosis of congenital heart disease and cardiac dysrhythmias. Pediatrics 65, 1059–1067 (1980).
Hornberger, L. K. et al. Left heart obstructive lesions and left ventricular growth in the midtrimester fetus. A longitudinal study. Circulation 92, 1531–1538 (1995).
Hornberger, L. K. et al. In utero pulmonary artery and aortic growth and potential for progression of pulmonary outflow tract obstruction in tetralogy of Fallot. J. Am. Coll. Cardiol. 25, 739–745 (1995).
Bonnet, D. et al. Detection of transposition of the great arteries in fetuses reduces neonatal morbidity and mortality. Circulation 99, 916–918 (1999).
Tworetzky, W. et al. Improved surgical outcome after fetal diagnosis of hypoplastic left heart syndrome. Circulation 103, 1269–1273 (2001).
Bull, C. Current and potential impact of fetal diagnosis on prevalence and spectrum of serious congenital heart disease at term in the UK. British Paediatric Cardiac Association. Lancet 354, 1242–1247 (1999).
Daubeney, P. E. et al. Pulmonary atresia with intact ventricular septum: impact of fetal echocardiography on incidence at birth and postnatal outcome. UK and Eire Collaborative Study of Pulmonary Atresia with Intact Ventricular Septum. Circulation 98, 562–566 (1998).
Cardiac screening examination of the fetus: guidelines for performing the 'basic' and 'extended basic' cardiac scan. Ultrasound Obstet. Gynecol. 27, 107–113 (2006).
Rychik, J. et al. American Society of Echocardiography guidelines and standards for performance of the fetal echocardiogram. J. Am. Soc. Echocardiogr. 17, 803–810 (2004).
Lee, W. et al. ISUOG consensus statement: what constitutes a fetal echocardiogram? Ultrasound Obstet. Gynecol. 32, 239–242 (2008).
Levey, A. et al. The impact of prenatal diagnosis of complex congenital heart disease on neonatal outcomes. Pediatr. Cardiol. 31, 587–597 (2010).
Gorincour, G. et al. Feasibility of fetal cardiac magnetic resonance imaging: preliminary experience. Ultrasound Obstet. Gynecol. 29, 105–108 (2007).
Votino, C. et al. MR imaging in normal fetal heart and in congenital heart disease. Ultrasound Obstet. Gynecol. http://dx.doi.org/10.1002/uog.10061.
Hyett, J., Moscoso, G., Papapanagiotou, G., Perdu, M. & Nicolaides, K. H. Abnormalities of the heart and great arteries in chromosomally normal fetuses with increased nuchal translucency thickness at 11–13 weeks of gestation. Ultrasound Obstet. Gynecol. 7, 245–250 (1996).
Clur, S. A., Ottenkamp, J. & Bilardo, C. M. The nuchal translucency and the fetal heart: a literature review. Prenat. Diagn. 29, 739–748 (2009).
McElhinney, D. B., Tworetzky, W. & Lock, J. E. Current status of fetal cardiac intervention. Circulation 121, 1256–1263 (2010).
Kohl, T. Fetal echocardiography: new grounds to explore during fetal cardiac intervention. Pediatr. Cardiol. 23, 334–346 (2002).
Verheijen, P. M. et al. Prenatal diagnosis of congenital heart disease affects preoperative acidosis in the newborn patient. J. Thorac. Cardiovasc. Surg. 121, 798–803 (2001).
Tham, E. B. et al. Outcome of fetuses and infants with double inlet single left ventricle. Am. J. Cardiol. 101, 1652–1656 (2008).
Wald, R. M. et al. Outcome after prenatal diagnosis of tricuspid atresia: a multicenter experience. Am. Heart J. 153, 772–778 (2007).
Zyblewski, S. C. et al. Chromosomal anomalies influence parental treatment decisions in relation to prenatally diagnosed congenital heart disease. Pediatr. Cardiol. 30, 1105–1111 (2009).
Tworetzky, W. et al. Echocardiographic diagnosis alone for the complete repair of major congenital heart defects. J. Am. Coll. Cardiol. 33, 228–233 (1999).
Tynan, M. J. et al. Nomenclature and classification of congenital heart disease. Br. Heart J. 41, 544–553 (1979).
Geva, T., Vick, G. W. III, Wendt, R. E. & Rokey, R. Role of spin echo and cine magnetic resonance imaging in presurgical planning of heterotaxy syndrome. Comparison with echocardiography and catheterization. Circulation 90, 348–356 (1994).
Hong, Y. K. et al. Efficacy of MRI in complicated congenital heart disease with visceral heterotaxy syndrome. J. Comput. Assist. Tomogr. 24, 671–682 (2000).
Tonkin, I. L. & Tonkin, A. K. Visceroatrial situs abnormalities: sonographic and computed tomographic appearance. Am. J. Roentgenol. 138, 509–515 (1982).
Lapierre, C. et al. Segmental approach to imaging of congenital heart disease. Radiographics 30, 397–411 (2010).
Beekmana, R. P. et al. Spin echo MRI in the evaluation of hearts with a double outlet right ventricle: usefulness and limitations. Magn. Reson. Imaging 18, 245–253 (2000).
Powell, A. J., Tsai-Goodman, B., Prakash, A., Greil, G. F. & Geva, T. Comparison between phase-velocity cine magnetic resonance imaging and invasive oximetry for quantification of atrial shunts. Am. J. Cardiol. 91, 1523–1525 (2003).
Roest, A. A., Helbing, W. A., van der Wall, E. E. & de Roos, A. Postoperative evaluation of congenital heart disease by magnetic resonance imaging. J. Magn. Reson. Imaging 10, 656–666 (1999).
Grosse-Wortmann, L. et al. Borderline hypoplasia of the left ventricle in neonates: insights for decision-making from functional assessment with magnetic resonance imaging. J. Thorac. Cardiovasc. Surg. 136, 1429–1436 (2008).
Kawel, N., Valsangiacomo-Buechel, E., Hoop, R. & Kellenberger, C. J. Preoperative evaluation of pulmonary artery morphology and pulmonary circulation in neonates with pulmonary atresia—usefulness of MR angiography in clinical routine. J. Cardiovasc. Magn. Reson. 12, 52 (2010).
Yin, L. et al. Quantitative analysis of pulmonary artery and pulmonary collaterals in preoperative patients with pulmonary artery atresia using dual-source computed tomography. Eur. J. Radiol. 79, 480–485 (2010).
Tsai-Goodman, B., Geva, T., Odegard, K. C., Sena, L. M. & Powell, A. J. Clinical role, accuracy, and technical aspects of cardiovascular magnetic resonance imaging in infants. Am. J. Cardiol. 94, 69–74 (2004).
Haramati, L. B., Glickstein, J. S., Issenberg, H. J., Haramati, N. & Crooke, G. A. MR imaging and CT of vascular anomalies and connections in patients with congenital heart disease: significance in surgical planning. Radiographics 22, 337–347 (2002).
Nieminen, H. P., Jokinen, E. V. & Sairanen, H. I. Causes of late deaths after pediatric cardiac surgery: a population-based study. J. Am. Coll. Cardiol. 50, 1263–1271 (2007).
Diller, G. P. et al. Predictors of morbidity and mortality in contemporary Fontan patients: results from a multicenter study including cardiopulmonary exercise testing in 321 patients. Eur. Heart J. 31, 3073–3083 (2010).
Piran, S., Veldtman, G., Siu, S., Webb, G. D. & Liu, P. P. Heart failure and ventricular dysfunction in patients with single or systemic right ventricles. Circulation 105, 1189–1194 (2002).
Lang, R. M. et al. Recommendations for chamber quantification. Eur. J. Echocardiogr. 7, 79–108 (2006).
Lu, X. et al. How accurately, reproducibly, and efficiently can we measure left ventricular indices using M-mode, 2-dimensional, and 3-dimensional echocardiography in children? Am. Heart J. 155, 946–953 (2008).
Riehle, T. J., Mahle, W. T., Parks, W. J., Sallee, D. III & Fyfe, D. A. Real-time three-dimensional echocardiographic acquisition and quantification of left ventricular indices in children and young adults with congenital heart disease: comparison with magnetic resonance imaging. J. Am. Soc. Echocardiogr. 21, 78–83 (2008).
Helbing, W. A. et al. Comparison of echocardiographic methods with magnetic resonance imaging for assessment of right ventricular function in children. Am. J. Cardiol. 76, 589–594 (1995).
Lai, W. W. et al. Accuracy of guideline recommendations for two-dimensional quantification of the right ventricle by echocardiography. Int. J. Cardiovasc. Imaging 24, 691–698 (2008).
Friedberg, M. K. et al. Validation of 3D echocardiographic assessment of left ventricular volumes, mass, and ejection fraction in neonates and infants with congenital heart disease: a comparison study with cardiac MRI. Circ. Cardiovasc. Imaging 3, 735–742 (2010).
Shimada, Y. J., Shiota, M., Siegel, R. J. & Shiota, T. Accuracy of right ventricular volumes and function determined by three-dimensional echocardiography in comparison with magnetic resonance imaging: a meta-analysis study. J. Am. Soc. Echocardiogr. 23, 943–953 (2010).
Margossian, R. et al. Comparison of echocardiographic and cardiac magnetic resonance imaging measurements of functional single ventricular volumes, mass, and ejection fraction (from the Pediatric Heart Network Fontan Cross-Sectional Study). Am. J. Cardiol. 104, 419–428 (2009).
Soriano, B. D. et al. Matrix-array 3-dimensional echocardiographic assessment of volumes, mass, and ejection fraction in young pediatric patients with a functional single ventricle: a comparison study with cardiac magnetic resonance. Circulation 117, 1842–1848 (2008).
van der Hulst, A. E. et al. Relation of left ventricular twist and global strain with right ventricular dysfunction in patients after operative “correction” of tetralogy of Fallot. Am. J. Cardiol. 106, 723–729 (2010).
Kempny, A. et al. Right ventricular–left ventricular interaction in adults with Tetralogy of Fallot: A combined cardiac magnetic resonance and echocardiographic speckle tracking study. Int. J. Cardiol. http://dx.doi.org/10.1016/j.ijcard.2010.09.031.
Luijnenburg, S. E. et al. Intra-observer and interobserver variability of biventricular function, volumes and mass in patients with congenital heart disease measured by CMR imaging. Int. J. Cardiovasc. Imaging 26, 57–64 (2010).
Buechel, E. V., Kaiser, T., Jackson, C., Schmitz, A. & Kellenberger, C. J. Normal right- and left ventricular volumes and myocardial mass in children measured by steady state free precession cardiovascular magnetic resonance. J. Cardiovasc. Magn. Reson. 11, 19 (2009).
van der Hulst, A. E. et al. Corrected tetralogy of Fallot: Comparison of tissue Doppler imaging and velocity-encoded MR for assessment of performance and temporal activation of right ventricle. Radiology 260, 88–97 (2011).
Matsui, H., Yasukochi, S., Haseyama, K., Kaneko, S. & Satomi, G. Quantification of right and left ventricular volumes in children with congenital heart disease by multidetector-row computed tomography. Pediatr. Cardiol. 28, 267–271 (2007).
Roest, A. A., Hazekamp, M. G. & Kroft, L. J. Assessment of proximal right coronary artery and cardiac dimensions with low-dose volumetric computed tomographic angiography in a child. Cardiol. Young 21, 218–219 (2011).
Santamore, W. P., Constantinescu, M., Vinten-Johansen, J., Johnston, W. E. & Little, W. C. Alterations in left ventricular compliance due to changes in right ventricular volume, pressure and compliance. Cardiovasc. Res. 22, 768–776 (1988).
Brookes, C. et al. Acute right ventricular dilatation in response to ischemia significantly impairs left ventricular systolic performance. Circulation 100, 761–767 (1999).
Feneley, M. P. et al. Contribution of left ventricular contraction to the generation of right ventricular systolic pressure in the human heart. Circulation 71, 473–480 (1985).
Fogel, M. A., Weinberg, P. M., Fellows, K. E. & Hoffman, E. A. A study in ventricular–ventricular interaction. Single right ventricles compared with systemic right ventricles in a dual-chamber circulation. Circulation 92, 219–230 (1995).
Fogel, M. A. et al. Mechanics of the single left ventricle: a study in ventricular–ventricular interaction II. Circulation 98, 330–338 (1998).
Lurz, P. et al. Improvement in left ventricular filling properties after relief of right ventricle to pulmonary artery conduit obstruction: contribution of septal motion and interventricular mechanical delay. Eur. Heart J. 30, 2266–2274 (2009).
Garofalo, C. A. et al. Ventricular diastolic stiffness predicts perioperative morbidity and duration of pleural effusions after the Fontan operation. Circulation 114 (Suppl. 1), I56–I61 (2006).
Cullen, S., Shore, D. & Redington, A. Characterization of right ventricular diastolic performance after complete repair of tetralogy of Fallot. Restrictive physiology predicts slow postoperative recovery. Circulation 91, 1782–1789 (1995).
Norgard, G. et al. Relationship between type of outflow tract repair and postoperative right ventricular diastolic physiology in tetralogy of Fallot. Implications for long-term outcome. Circulation 94, 3276–3280 (1996).
Nagueh, S. F. et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography. Eur. J. Echocardiogr. 10, 165–193 (2009).
Frommelt, P. C. Echocardiographic measures of diastolic function in pediatric heart disease. Curr. Opin. Cardiol. 21, 194–199 (2006).
Puranik, R. et al. Abnormal right ventricular tissue velocities after repair of congenital heart disease—implications for late outcomes. Heart Lung Circ. 16, 295–299 (2007).
Vitarelli, A. et al. Quantitative assessment of systolic and diastolic ventricular function with tissue Doppler imaging after Fontan type of operation. Int. J. Cardiol. 102, 61–69 (2005).
Gatzoulis, M. A., Clark, A. L., Cullen, S., Newman, C. G. & Redington, A. N. Right ventricular diastolic function 15 to 35 years after repair of tetralogy of Fallot. Restrictive physiology predicts superior exercise performance. Circulation 91, 1775–1781 (1995).
Roes, S. D. et al. Flow assessment through four heart valves simultaneously using 3-dimensional 3-directional velocity-encoded magnetic resonance imaging with retrospective valve tracking in healthy volunteers and patients with valvular regurgitation. Invest. Radiol. 44, 669–675 (2009).
van der Hulst, A. E. et al. Tetralogy of Fallot: 3D velocity-encoded MR imaging for evaluation of right ventricular valve flow and diastolic function in patients after correction. Radiology 256, 724–734 (2010).
Westenberg, J. J. et al. Mitral valve and tricuspid valve blood flow: accurate quantification with 3D velocity-encoded MR imaging with retrospective valve tracking. Radiology 249, 792–800 (2008).
Westenberg, J. J. et al. Assessment of left ventricular dyssynchrony in patients with conduction delay and idiopathic dilated cardiomyopathy: head-to-head comparison between tissue Doppler imaging and velocity-encoded magnetic resonance imaging. J. Am. Coll. Cardiol. 47, 2042–2048 (2006).
Boogers, M. J. et al. Feasibility of diastolic function assessment With cardiac CT feasibility study in comparison with tissue Doppler imaging. JACC Cardiovasc. Imaging 4, 246–256 (2011).
Brown, D. W., Dipilato, A. E., Chong, E. C., Lock, J. E. & McElhinney, D. B. Aortic valve reinterventions after balloon aortic valvuloplasty for congenital aortic stenosis intermediate and late follow-up. J. Am. Coll. Cardiol. 56, 1740–1749 (2010).
Hoohenkerk, G. J. et al. More than 30 years' experience with surgical correction of atrioventricular septal defects. Ann. Thorac. Surg. 90, 1554–1561 (2010).
Wu, K. L. et al. Left ventricular outflow tract obstruction in complete transposition of the great arteries—-echocardiography criteria for surgical strategies. Circulation J. 74, 1214–1218 (2010).
Beroukhim, R. S. et al. An echocardiographic model predicting severity of aortic regurgitation in congenital heart disease. Circ. Cardiovasc. Imaging 3, 542–549 (2010).
Li, W. et al. Doppler-echocardiographic assessment of pulmonary regurgitation in adults with repaired tetralogy of Fallot: comparison with cardiovascular magnetic resonance imaging. Am. Heart J. 147, 165–172 (2004).
Biner, S. et al. Reproducibility of proximal isovelocity surface area, vena contracta, and regurgitant jet area for assessment of mitral regurgitation severity. JACC Cardiovasc. Imaging 3, 235–243 (2010).
Grayburn, P. A. & Bhella, P. Grading severity of mitral regurgitation by echocardiography: science or art? JACC Cardiovasc. Imaging 3, 244–246 (2010).
O'Brien, K. R. et al. MRI phase contrast velocity and flow errors in turbulent stenotic jets. J. Magn. Reson. Imaging 28, 210–218 (2008).
Higgins, C. B. & Sakuma, H. Heart disease: functional evaluation with MR imaging. Radiology 199, 307–315 (1996).
O'Brien, K. R., Myerson, S. G., Cowan, B. R., Young, A. A. & Robson, M. D. Phase contrast ultrashort TE: A more reliable technique for measurement of high-velocity turbulent stenotic jets. Magn. Reson. Med. 62, 626–636 (2009).
Caruthers, S. D. et al. Practical value of cardiac magnetic resonance imaging for clinical quantification of aortic valve stenosis: comparison with echocardiography. Circulation 108, 2236–2243 (2003).
Djavidani, B. et al. Planimetry of mitral valve stenosis by magnetic resonance imaging. J. Am. Coll. Cardiol. 45, 2048–2053 (2005).
Rebergen, S. A., Chin, J. G., Ottenkamp, J., van der Wall, E. E. & de Roos, A. Pulmonary regurgitation in the late postoperative follow-up of tetralogy of Fallot. Volumetric quantitation by nuclear magnetic resonance velocity mapping. Circulation 88, 2257–2266 (1993).
Westenberg, J. J. et al. Magnetic resonance imaging assessment of reverse left ventricular remodeling late after restrictive mitral annuloplasty in early stages of dilated cardiomyopathy. J. Thorac. Cardiovasc. Surg. 135, 1247–1252 (2008).
Udelson, J. E. & Konstam, M. A. Relation between left ventricular remodeling and clinical outcomes in heart failure patients with left ventricular systolic dysfunction. J. Card. Fail. 8 (Suppl. 6), S465–S471 (2002).
Feuchtner, G. M. et al. Quantification of aortic regurgitant fraction and volume with multi-detector computed tomography comparison with echocardiography. Acad. Radiol. 18, 334–342 (2011).
Niwa, K. et al. Structural abnormalities of great arterial walls in congenital heart disease: light and electron microscopic analyses. Circulation 103, 393–400 (2001).
Yetman, A. T. & Graham, T. The dilated aorta in patients with congenital cardiac defects. J. Am. Coll. Cardiol. 53, 461–467 (2009).
Senzaki, H. et al. Ventricular–vascular stiffening in patients with repaired coarctation of aorta: integrated pathophysiology of hypertension. Circulation 118 (Suppl. 14), S191–S198 (2008).
Senzaki, H. et al. Arterial haemodynamics in patients after repair of tetralogy of Fallot: influence on left ventricular after load and aortic dilatation. Heart 94, 70–74 (2008).
Voges, I. et al. Maladaptive aortic properties in children after palliation of hypoplastic left heart syndrome assessed by cardiovascular magnetic resonance imaging. Circulation 122, 1068–1076 (2010).
Evangelista, A. et al. Echocardiography in aortic diseases: EAE recommendations for clinical practice. Eur. J. Echocardiogr. 11, 645–658 (2010).
Niwa, K., Siu, S. C., Webb, G. D. & Gatzoulis, M. A. Progressive aortic root dilatation in adults late after repair of tetralogy of Fallot. Circulation 106, 1374–1378 (2002).
Cardis, B. M., Fyfe, D. A. & Mahle, W. T. Elastic properties of the reconstructed aorta in hypoplastic left heart syndrome. Ann. Thorac. Surg. 81, 988–991 (2006).
Grotenhuis, H. B. et al. Aortic root dysfunctioning and its effect on left ventricular function in Ross procedure patients assessed with magnetic resonance imaging. Am. Heart J. 152, 975.e1–975.e8 (2006).
Grotenhuis, H. B. et al. Aortic elasticity and left ventricular function after arterial switch operation: MR imaging—initial experience. Radiology 249, 801–809 (2008).
Grotenhuis, H. B. et al. Aortic elasticity and size are associated with aortic regurgitation and left ventricular dysfunction in tetralogy of Fallot after pulmonary valve replacement. Heart 95, 1931–1936 (2009).
Chakrabarti, S. et al. Balloon expandable stent implantation for native and recurrent coarctation of the aorta—prospective computed tomography assessment of stent integrity, aneurysm formation and stenosis relief. Heart 96, 1212–1216 (2010).
Zhang, J. et al. Large-vessel distensibility measurement with electrocardiographically gated multidetector CT: phantom study and initial experience. Radiology 245, 258–266 (2007).
Jenkins, K. J. et al. Noninherited risk factors and congenital cardiovascular defects: current knowledge: a scientific statement from the American Heart Association Council on Cardiovascular Disease in the Young: endorsed by the American Academy of Pediatrics. Circulation 115, 2995–3014 (2007).
Pierpont, M. E. et al. Genetic basis for congenital heart defects: current knowledge: a scientific statement from the American Heart Association Congenital Cardiac Defects Committee, Council on Cardiovascular Disease in the Young: endorsed by the American Academy of Pediatrics. Circulation 115, 3015–3038 (2007).
Phoon, C. K. & Neill, C. A. Asplenia syndrome: insight into embryology through an analysis of cardiac and extracardiac anomalies. Am. J. Cardiol. 73, 581–587 (1994).
Ruben, G. D., Templeton, J. M., Jr & Ziegler, M. M. Situs inversus: the complex inducing neonatal intestinal obstruction. J. Pediatr. Surg. 18, 751–756 (1983).
Phoon, C. K. & Neill, C. A. Asplenia syndrome—risk factors for early unfavorable outcome. Am. J. Cardiol. 73, 1235–1237 (1994).
Fulcher, A. S. & Turner, M. A. Abdominal manifestations of situs anomalies in adults. Radiographics 22, 1439–1456 (2002).
Ditchfield, M. R. & Hutson, J. M. Intestinal rotational abnormalities in polysplenia and asplenia syndromes. Pediatr. Radiol. 28, 303–306 (1998).
Lampl, B., Levin, T. L., Berdon, W. E. & Cowles, R. A. Malrotation and midgut volvulus: a historical review and current controversies in diagnosis and management. Pediatr. Radiol. 39, 359–366 (2009).
McElhinney, D. B. et al. Necrotizing enterocolitis in neonates with congenital heart disease: risk factors and outcomes. Pediatrics 106, 1080–1087 (2000).
Carlo, W. F., Kimball, T. R., Michelfelder, E. C. & Border, W. L. Persistent diastolic flow reversal in abdominal aortic Doppler-flow profiles is associated with an increased risk of necrotizing enterocolitis in term infants with congenital heart disease. Pediatrics 119, 330–335 (2007).
Dimopoulos, K. et al. Prevalence, predictors, and prognostic value of renal dysfunction in adults with congenital heart disease. Circulation 117, 2320–2328 (2008).
Dimopoulos, K. et al. Anemia in adults with congenital heart disease relates to adverse outcome. J. Am. Coll. Cardiol. 54, 2093–2100 (2009).
Dimopoulos, K. et al. Hyponatraemia: A strong predictor of mortality in adults with congenital heart disease. Eur. Heart J. 31, 595–601 (2010).
Gorelick, P. B. et al. Vascular contributions to cognitive impairment and dementia: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 42, 2672–2713 (2011).
Kaltman, J. R., Di, H., Tian, Z. & Rychik, J. Impact of congenital heart disease on cerebrovascular blood flow dynamics in the fetus. Ultrasound Obstet. Gynecol. 25, 32–36 (2005).
Limperopoulos, C. et al. Brain volume and metabolism in fetuses with congenital heart disease: evaluation with quantitative magnetic resonance imaging and spectroscopy. Circulation 121, 26–33 (2010).
Miller, S. P. et al. Abnormal brain development in newborns with congenital heart disease. N. Engl. J. Med. 357, 1928–1938 (2007).
Mahle, W. T. et al. An MRI study of neurological injury before and after congenital heart surgery. Circulation 106 (Suppl. 1), I109–I114 (2002).
Mahle, W. T., Clancy, R. R., McGaurn, S. P., Goin, J. E. & Clark, B. J. Impact of prenatal diagnosis on survival and early neurologic morbidity in neonates with the hypoplastic left heart syndrome. Pediatrics 107, 1277–1282 (2001).
Newburger, J. W. et al. A comparison of the perioperative neurologic effects of hypothermic circulatory arrest versus low-flow cardiopulmonary bypass in infant heart surgery. N. Engl. J. Med. 329, 1057–1064 (1993).
McQuillen, P. S. & Miller, S. P. Congenital heart disease and brain development. Ann. N. Y. Acad. Sci. 1184, 68–86 (2010).
Goldberg, D. J. et al. Impact of oral sildenafil on exercise performance in children and young adults after the Fontan operation: a randomized, double-blind, placebo-controlled, crossover trial. Circulation 123, 1185–1193 (2011).
Hsu, D. T. et al. Enalapril in infants with single ventricle: results of a multicenter randomized trial. Circulation 122, 333–340 (2010).
van der Hulst, A. E. et al. Cardiac resynchronization therapy in paediatric and congenital heart disease patients. Eur. Heart J. 32, 2236–2246 (2011).
Warnes, C. A. et al. Task force 1: the changing profile of congenital heart disease in adult life. J. Am. Coll. Cardiol. 37, 1170–1175 (2001).
Hoffman, J. I., Kaplan, S. & Liberthson, R. R. Prevalence of congenital heart disease. Am. Heart J. 147, 425–439 (2004).
Bodhey, N. K. et al. Functional analysis of the components of the right ventricle in the setting of tetralogy of Fallot. Circ. Cardiovasc. Imaging 1, 141–147 (2008).
Sheehan, F. H. et al. Three-dimensional shape analysis of right ventricular remodeling in repaired tetralogy of Fallot. Am. J. Cardiol. 101, 107–113 (2008).
Muzzarelli, S., Ordovas, K. G., Cannavale, G., Meadows, A. K. & Higgins, C. B. Tetralogy of Fallot: impact of the excursion of the interventricular septum on left ventricular systolic function and fibrosis after surgical repair. Radiology 259, 375–383 (2011).
Helbing, W. A. et al. Right ventricular diastolic function in children with pulmonary regurgitation after repair of tetralogy of Fallot: volumetric evaluation by magnetic resonance velocity mapping. J. Am. Coll. Cardiol. 28, 1827–1835 (1996).
Frigiola, A. et al. Biventricular response after pulmonary valve replacement for right ventricular outflow tract dysfunction: is age a predictor of outcome? Circulation 118 (Suppl. 14), S182–S190 (2008).
van Straten, A. et al. Time course of diastolic and systolic function improvement after pulmonary valve replacement in adult patients with tetralogy of Fallot. J. Am. Coll. Cardiol. 46, 1559–1564 (2005).
Scherptong, R. W. et al. Follow-up after pulmonary valve replacement in adults with tetralogy of Fallot: association between QRS duration and outcome. J. Am. Coll. Cardiol. 56, 1486–1492 (2010).
van Huysduynen, B. H. et al. Reduction of QRS duration after pulmonary valve replacement in adult Fallot patients is related to reduction of right ventricular volume. Eur. Heart J. 26, 928–932 (2005).
Vliegen, H. W. et al. Magnetic resonance imaging to assess the hemodynamic effects of pulmonary valve replacement in adults late after repair of tetralogy of Fallot. Circulation 106, 1703–1707 (2002).
Warner, K. G. et al. Expanding the indications for pulmonary valve replacement after repair of tetralogy of Fallot. Ann. Thorac. Surg. 76, 1066–1071 (2003).
Harrild, D. M. et al. Pulmonary valve replacement in tetralogy of Fallot: impact on survival and ventricular tachycardia. Circulation 119, 445–451 (2009).
Acknowledgements
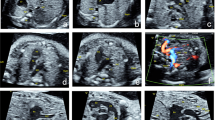
The authors thank Lucia J. M. Kroft from the Department of Radiology, Leiden University Medical Center, the Netherlands for assistance in the preparation of Figures 2f, 2g, and 3.
Author information
Authors and Affiliations
Contributions
Both authors contributed substantially to researching the article, discussion of its content, and writing, reviewing, and editing the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Roest, A., de Roos, A. Imaging of patients with congenital heart disease. Nat Rev Cardiol 9, 101–115 (2012). https://doi.org/10.1038/nrcardio.2011.162
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2011.162
This article is cited by
-
Two-Phase Contrast Injection Protocol for Pediatric Cardiac Computed Tomography in Children with Congenital Heart Disease
Pediatric Cardiology (2018)
-
Atlas-Based Computational Analysis of Heart Shape and Function in Congenital Heart Disease
Journal of Cardiovascular Translational Research (2018)
-
4D modelling for rapid assessment of biventricular function in congenital heart disease
The International Journal of Cardiovascular Imaging (2018)
-
Non-ECG-gated MDCTA of infracardiac total anomalous pulmonary venous connection in neonates and young infants
Herz (2013)