Abstract
Not all patients with acute exacerbations of chronic obstructive pulmonary disease (COPD) benefit from treatment with systemic corticosteroids and antibiotics. The aim of the study was to identify criteria recommended in current COPD guidelines for treating acute exacerbations with systemic corticosteroids and antibiotics and to assess the underlying evidence. Current COPD guidelines were identified by a systematic literature search. The most recent guidelines as per country/organisation containing recommendations about treating acute exacerbations of COPD were included. Guideline development and criteria for treating acute exacerbations with systemic corticosteroids and antibiotics were appraised. Randomised controlled trials directly referred to in context with the recommendations were evaluated in terms of study design, setting, and study population. A total of 19 COPD guidelines were included. Systemic corticosteroids were often universally recommended to all patients with acute exacerbations. Criteria for treatment with antibiotics were mainly an increase in respiratory symptoms. Objective diagnostic tests or clinical examination were only rarely recommended. Only few criteria were directly linked to underlying evidence, and the trial patients represented a highly specific group of COPD patients. Current COPD guidelines are of little help in primary care to identify patients with acute exacerbations probably benefitting from treatment with systemic corticosteroids and antibiotics in primary care, and might contribute to overuse or inappropriate use of either treatment.
Similar content being viewed by others
Introduction
Acute exacerbations of chronic obstructive pulmonary disease (AECOPD) occur frequently in the course of COPD.1 They can differ in severity and many require hospitalisation, but the majority of mild to moderate AECOPD can be managed in primary care.2 Antibiotics and systemic corticosteroids are beneficial treatment options that are often used.3,4 However, the benefit of antibiotics in mild to moderate AECOPD remains controversial,5 and their overuse can contribute to the development of bacterial resistance.6 Systemic corticosteroids bear the risk of adverse side effects,3 especially in patients with co-morbidities.7 Inappropriate use of either treatment should be avoided, and targeting patient treatment requires careful patient assessment. Clinical practice guidelines are intended to assist treatment decisions, based on the best available evidence.8 A critical appraisal of 15 COPD guidelines found variations in the content and between recommendations on several management strategies for COPD, and concluded that these were rather a result of ‘selective experience’ than based on scientific evidence.9 Consequently, we designed this study to identify recommended assessment strategies for treating AECOPD patients with systemic corticosteroids and antibiotics in COPD guidelines. Furthermore, we aimed to evaluate the quality of guideline development and the applicability of underlying evidence to primary care.
Methods
A systematic literature review was conducted in Web of Science, SCOPUS, SveMed+, PubMed, Embase, Cihnal (EBsco) and Ovid MD to identify COPD guidelines. Throughout the entire search, ‘COPD’ as Mesh-term was used whenever applicable. If a database did not support Mesh-terms, ‘COPD’ was searched in keywords, abstract and title. ‘COPD’ was combined with the search phrases ‘guideline’ and ‘recommendation’. The search string used throughout the search was as follows:
-
Chronic Obstructive Pulmonary Disease AND (Guideline OR Recommendation).
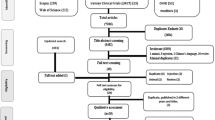
Our initial search was performed with a time limit set for publications between 2003 and 2013. It was then extended to 8 May 2014 to ensure the inclusion of any new publications during our work on this project. Eligibility assessment was conducted by the first and the last author, and the approach from the preferred reporting items for systematic reviews and meta-analyses statement was followed10 (Figure 1). To avoid overlooking documents that were published elsewhere than in the searched databases, a supplemental search was conducted in the guideline databases UpToDate, Best Practice, National Guideline Clearinghouse, Cochrane Library, Guidelines International Network and websites of the Canadian Medical Association, and American College of Physicians. Furthermore, websites of national health authorities (Germany, Denmark, Sweden, Norway, Austria, Switzerland, and Netherlands) were searched for eligible guidelines. This search was not repeated after 2013. Only guidelines and published documents with recommendations on adults with AECOPD and/or infectious diseases of the lungs when containing AECOPD were included in this study. They also had to be published in English, German, Dutch, or a Scandinavian language. The most recent guideline from each country was included. The included guidelines were analysed in terms of guideline development by applying criteria from the AGREE II tool (Appraisal of guidelines for research and evaluation II).11 The criteria applied belonged to the domains 2 (stakeholder involvement), 3 (rigor of development), and 6 (editorial independence). We extracted recommendations about patient assessment for treatment with systemic corticosteroids and antibiotics. If recommendations were given separately for inpatients and outpatients, only those for outpatients were considered. Evidence explicitly linked to the recommendations, as described in domain 3 of the AGREE II tool,11 was obtained, and randomised controlled trials published in scientific medical journals were assessed in terms of study setting, study design, and inclusion and exclusion criteria. Furthermore, we decided to add the trials included in the latest versions of the Cochrane reviews about treating AECOPD with systemic corticosteroids3 and antibiotics,4 although not directly referred to in the guidelines.
Results
The systematic database search resulted in 1,417 documents, and the supplemental search in the guideline databases in 873 documents. Further, 10 documents were retrieved from the websites of national health authorities. A total of 64 documents (47, 8, and 9 documents, respectively) remained for full-text screening after excluding duplicates and those not matching the inclusion criteria. After full-text screening, 36 documents remained, of which 17 outdated versions were excluded. Finally, 19 guidelines were included in the study (Figure 1).
Characteristics of guideline development
The guidelines were published between 2004 and 2014, and 12 of these were updates from earlier versions (Table 1). The time between previous and current editions varied from continuous updating to 15 years between two versions. Four guidelines gave a date for planned revision. A total of 14 guidelines provided information about the development committee, and in 10 committees at least one general practitioner was included. The guidelines from the Netherlands and from the International Primary Care Respiratory Group were especially targeted towards primary care physicians, and this was reflected in the high number of general practitioners in the development groups (Table 1). Furthermore, eight guidelines gave separate recommendations for inpatients and outpatients. Information about funding or conflict of interests was provided in 11 guidelines, 5 of which were sponsored by pharmaceutical companies (Table 1). A detailed description of important steps in the guideline development process, such as literature review, was only given in six guidelines (Table 1). AECOPD definitions across the guidelines were symptom based including the terms ‘dyspnoea’, ‘cough’, and ‘changes in sputum’ in the majority of cases.
Criteria for initiating treatment with systemic corticosteroids
A total of 17 of the 19 guidelines addressed the treatment option ‘systemic corticosteroids’, with 11 criteria being identified (Table 2). The guidelines from the European Respiratory Society and Germany addressed infectious diseases and did not contain recommendations about systemic corticosteroids. We found that nine guidelines recommended systemic corticosteroids universally to all AECOPD patients, and the Spanish guideline reserved such treatment to all patients with an at least moderate exacerbation (without providing information about different severity grades). One guideline reserved such treatment to patients with severe underlying COPD, and two guidelines to patients with moderate to severe COPD (Table 2). Three guidelines recommended basing treatment decisions on patients’ actual respiratory symptoms, namely a significant increase in dyspnoea and wheezing. The Dutch guideline recommended waiting for the response to increased dosage of bronchodilators, as first-line emergency treatment, and assessing the patients’ general condition before starting a course with systemic corticosteroids in all patients not requiring hospitalisation. The Swedish guideline was the only guideline to suggest objective measures by clinical examination (respiratory rate and heart rate) and to recommend the use of the diagnostic tests pulse oximetry and blood gas analysis (Table 2).
Characteristics of the primary evidence supporting recommendations for systemic corticosteroids
We found 11 randomised controlled trials directly referred to in context with a certain recommendation12–22 and two trials in the Cochrane review,3 which were not directly referred to in context with a certain recommendation in the guidelines (Table 3). Publication dates varied between 1980 and 2011, and 9 of the 11 trials were hospital based. The number of study participants ranged from 27 to 210 patients (Table 3). The majority were male, and one trial had included only male patients (Table 3). The percentage of the patients who were finally randomised among those screened for eligibility varied between 14 and 96% (Table 3). Cardiovascular co-morbidities were explicitly described as exclusion criteria in 7 trials (uncontrolled heart failure in 5 trials, diabetes mellitus in 2 trials, and uncontrolled arterial hypertension in 1 trial). The forced expiratory volume after 1 s (FEV1% predicted) or FEV1 in litre at inclusion were provided in 10 trials. Their values ranged between 24.7 and 59.6%, or between 0.5 and 1.3 litre, respectively (Table 3).
Criteria for initiating treatment with antibiotics
All guidelines contained recommendations about treatment with antibiotics, and 12 assessment criteria were identified (Table 2). Two guidelines recommended antibiotics to all patients with AECOPD. All others, apart from the Dutch guideline, recommended basing antibiotic treatment on an increase of the respiratory symptoms ‘dyspnoea’, ‘cough’, ‘sputum volume’, or ‘sputum purulence’. A total of eight of these guidelines only recommended changes in sputum (mostly purulent or changes in sputum colour). These guidelines also provided additional criteria (Table 2), which were mostly the severity of underlying COPD or systemic symptoms such as ‘fever’ and ‘impaired general condition’. Only four guidelines recommended conducting additional diagnostic tests: C-reactive protein (CRP), white blood cell count, procalcitonin, and chest radiography (Table 2). The guidelines from India23 and Saudi24 emphasised that the use of biomarkers has no role in the assessment of AECOPD. The Dutch guideline was exceptional, as they did not recommend any of the respiratory symptoms. Here, the focus was only on the patient’s general condition and fever as signs for bacterial infection, in combination with severe underlying COPD and insufficient improvement after 4 days. However, it was stated that a course of antibiotics might be initiated in all patients with a severe exacerbation, characterised by heavy dyspnoea, use of accessory muscles, respiratory rate >30/min and heart rate >120/min (Table 2).
Characteristics of the primary evidence supporting recommendations for antibiotics
We found 4 randomised controlled trials that were directly referred to in context with a certain recommendation25–28 and 11 trials in the Cochrane review4 that were not directly referred to in the guidelines28–39 (Table 4). They were published between 1960 and 2013. In four trials, patients were excluded owing to both cardiovascular diseases (left ventricular failure in one trial, severe heart disease in two trials, and stroke in one trial) and a broad range of infectious diseases. Almost all trials included significantly more men than women (Table 4). A total of 11 trials provided information about initial exclusion rates before randomisation, which ranged between 56 and 3%. The average baseline FEV1% predicted or peak expiratory flow of the included study patients was presented in 13 trials, with the FEV1% predicted ranging from 33.9 to 65% and peak expiratory flow from 63 to 295 l/min (Table 4).
Discussion
Main findings
There was a considerable lack of transparency regarding guideline development, as the literature review was often not documented comprehensively. It is also problematic that a considerable number of guidelines were financed by pharmaceutical companies, or their funding sources were not reported.40 Owing to the small number of general practitioners in the guideline development committees, primary care expertise might not be considered sufficiently during guideline development.
Treatment recommendations were mostly universal and unspecific and often recommended for all AECOPD patients or all patients with underlying moderate to severe COPD, or, in terms of antibiotics, patients with certain symptoms. The use of diagnostic tests was only recommended in a few guidelines.
The patients in the trials that the recommendations were based on were a rather selected group of COPD patients. Most trials were conducted in hospitalised patients, the exclusion rates before randomisation were high in many trials, and the patients were often characterised by severely reduced lung function and low prevalence of cardiovascular co-morbidities or diabetes.
Strengths and limitations
We conducted a rigorous and systematic literature search to get hold of the COPD guidelines. However, we might have missed guidelines published in languages other than the ones included.41 As we did not use the AGREE II tool to its full extent, we are limited in making reliable statements on the guideline quality. Further, we only considered primary studies that were explicitly linked to the recommendations in the appraisal of underlying evidence. Whether studies are cited directly linked to a recommendation or not could be owing to the technical presentation of recommendations, and it does not necessarily reflect the existence of the evidence used. However, according to the AGREE II tool, an explicit link between recommendations and evidence is important for judging the source of a recommendation.11 As we additionally appraised the trials included in the latest Cochrane reviews on treating AECOPD with systemic corticosteroids3 and antibiotics,4 we are able to make a valid statement about the evidence that the current treatment recommendations are based on.
Interpretation of findings in relation to previously published work
Relevance of the underlying evidence for primary care patients
The characteristics of the trial patients of the studies underlying the recommendations were not necessarily comparable to the ‘common’ COPD patient in primary care, who tend to have milder airflow obstruction42 and frequently suffer from co-morbidities.43 When evidence is based on patients without co-morbidities, it could be risky to follow the guidelines in primary care patients who also suffer from heart failure or diabetes. Herland et al. expressed similar concerns, questioning whether results of the trials on obstructive lung diseases really can be extrapolated to ‘real-life’ populations of patients.43 Considering that frequent co-morbidities,43 such as heart failure, can mimic the symptoms of increased cough and dyspnoea,44,45 adherence to the current guidelines might lead to over-treatment or inappropriate treatment with antibiotics and systemic corticosteroids. In addition, the authors of the latest Cochrane reviews about antibiotics4 and systemic corticosteroids3 for AECOPD underline that the effect of both treatments in outpatients and patients with mild airflow obstruction still remains unclear. They emphasise the need for diagnostic tests and biomarkers to identify patients who may benefit from the treatment.
Criteria for systemic corticosteroids
According to many guidelines, systemic corticosteroids seemed to be universally useful. Diagnostic tests or clinical examination were rarely recommended, but prescribing a corticosteroid should rather be based on the patient’s respiratory symptoms. It is striking that the recommended criteria for treating AECOPD with systemic corticosteroids resemble in most cases the (clinical) definition of an AECOPD, which is an ‘acute event characterised by a worsening of the patient’s respiratory symptoms that is beyond normal day-to-day variations and leads to change in medication’.46 Thus, once the clinical diagnosis of AECOPD is made, most patients would fit the criteria for a course of systemic corticosteroids according to the guidelines. Yet, common adverse side effects, such as hyperglycaemic episodes in patients with diabetes,7 call for a rather critical use of systemic corticosteroids. An ‘increase in dyspnoea’ might be caused by other (non-)respiratory conditions that are not necessarily responsive to systemic corticosteroids.44,45 Therefore, a more careful assessment to identify patients with a clear benefit would be of major importance. Yet, no reliable method for further investigation beyond assessment of symptoms has been established, and this is probably the reason for rather speculative recommendations such as those recommended in the Swedish guidelines (pulse oximetry and blood gas analysis). Interestingly, spirometry was explicitly advised against in, for instance, the Global initiative for chronic obstructive lung disease (GOLD) guidelines, as it is ‘difficult to perform’ and ‘measurements are not accurate enough’.47 When looking at clinical trials, we find spirometry being a common outcome measure to quantify airflow obstruction and to show the effect of, for instance, systemic corticosteroids.3 Thus, the arguments to abandon spirometry from the assessment of AECOPD do not seem to be thoroughly deliberated. Further evaluation in primary care might help identify a role for spirometry in the assessment of AECOPD.
Criteria for antibiotic treatment
Most guidelines recommend antibiotic treatment based on respiratory symptoms, and increased purulence in particular. This recommendation rests on the subgroup analyses in Anthonisens landmark study.25 The special weight laid on increased purulence is supported by the increased risk of positive bacterial culture in COPD patients with purulence48 and, recently, by Miravitlles’ study of predictors of treatment failure in AECOPD in patients with mild to moderate disease not treated with antibiotics.49 However, sputum colour alone might not be sufficient to identify patients possibly benefiting from antibiotics,50 and therefore biomarkers could be very valuable: in the study by Miravitlles,49 a CRP value >40 mg/l was found to be the strongest predictor of treatment failure. Results from another study emphasise the usefulness of the CRP test in general practice, as it was found that sputum-guided therapy alone resulted in higher prescription rates than when combined with CRP.39 However, by now, CRP is only recommended in the Norwegian guideline. ‘Procalcitonin’, which was recommended in the German and also mentioned in the Suisse guideline, has also been found to be a promising biomarker for targeting antibiotic treatment.51 It is, however, not yet available as a point-of-care test for use in primary care. The strict clinical criteria in the Dutch guideline indicating a severe AECOPD are similar to those in the systemic inflammatory response syndrome score52 and in the CRB65 score.53 Yet, they do not refer to supporting evidence. Although the CRB65 score can be helpful to identify severe AECOPD with high inpatient mortality,54 it might be problematic to apply these criteria as indicators for antibiotic treatment in AECOPD.
Future perspectives and conclusion
Our results lead to the conclusion that current COPD guidelines are of little help in identifying which AECOPD patients might benefit from treatment with systemic corticosteroids and antibiotics in a primary care setting. Increased purulence has been shown to be a useful criterion for antibiotic treatment in patients with severe disease,25 but we still do not know whether reliance on purulence leads to over-treatment in patients with mild to moderate disease. Despite little evidence supporting the usefulness of biomarkers, some guidelines have started to include tests in the diagnostic work-up. However, a better understanding of how COPD/AECOPD interferes with other conditions will probably be as important as establishing a test or biomarker to meet the current challenges, such as differentiation between AECOPD and other diseases. Future guidelines will surely be influenced by currently ongoing research on the use of biomarkers in AECOPD.55–59 Further, the new understanding of how COPD should be subclassified into phenotypes60 may also lead to a new way of understanding the exacerbations, which may vary by phenotype. Antibiotics may be more frequently needed in a phenotype associated with chronic bronchitis than in those dominated by emphysema or when the patient can be classified as COPD-asthma overlap. We recommend that future research should, to a larger extent, focus on AECOPD in patients with mild to moderate airflow obstruction (FEV1% predicted >50%), similar to the study by Llor et al.,39 and consider the concern of multimorbidity in COPD patients. Moreover, we find it necessary to reconsider the uncritical way in which the use of systemic corticosteroids is presented in current COPD guidelines, and to stress the importance of developing better methods for targeting treatment with systemic corticosteroids. Such moves will be necessary to make future guidelines more helpful in primary care and to improve care for COPD patients.
References
O'Reilly JF, Williams AE, Holt K, Rice L . Defining COPD exacerbations: impact on estimation of incidence and burden in primary care. Prim Care Respir J 2006; 15: 346–353.
Jeppesen E, Brurberg KG, Vist GE, Wedzicha JA, Wright JJ, Greenstone M et al. Hospital at home for acute exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2012; 5: CD003573.
Walters JA, Gibson PG, Wood-Baker R, Hannay M, Walters EH . Systemic corticosteroids for acute exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2009; 1: CD001288.
Vollenweider DJ, Jarrett H, Steurer-Stey CA, Garcia-Aymerich J, Puhan MA . Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2012; 12: CD010257.
Puhan M, Vollenweider D, Steurer J, Bossuyt P, ter Riet G . Where is the supporting evidence for treating mild to moderate chronic obstructive pulmonary disease exacerbations with antibiotics? A systematic review. BMC Med 2008; 6: 28.
Goossens H, Ferech M, Vander Stichele R, Elseviers M . Outpatient antibiotic use in Europe and association with resistance: a cross-national database study. Lancet 2005; 365: 579–587.
Bach PB, Brown C, Gelfand SE, McCrory DC . Management of acute exacerbations of chronic obstructive pulmonary disease: a summary and appraisal of published evidence. Ann Intern Med 2001; 134: 600–620.
Graham R, Mancher M, Wolman MD, Greenfield S, Steinberg E (eds). Clinical Practice Guidelines We Can Trust. The National Academies Press: Washington DC, USA, 2011.
Lacasse Y, Ferreira I, Brooks D, Newman T, Goldstein RS . Critical appraisal of clinical practice guidelines targeting chronic obstructive pulmonary disease. Arch Intern Med 2001; 161: 69–74.
Moher D, Liberati A, Tetzlaff J, Altman DG . Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 2009; 6: e1000097.
Brouwers MC, Kho ME, Browman GP, Burgers JS, Cluzeau F, Feder G et al. AGREE II: advancing guideline development, reporting and evaluation in health care. CMAJ 2010; 182: E839–E842.
Albert RK, Martin TR, Lewis SW . Controlled clinical trial of methylprednisolone in patients with chronic bronchitis and acute respiratory insufficiency. Ann Intern Med 1980; 92: 753–758.
Thompson WH, Nielson CP, Carvalho P, Charan NB, Crowley JJ . Controlled trial of oral prednisone in outpatients with acute COPD exacerbation. Am J Respir Crit Care Med 1996; 154: 407–412.
Niewoehner DE, Erbland ML, Deupree RH, Collins D, Gross NJ, Light RW et al. Effect of systemic glucocorticoids on exacerbations of chronic obstructive pulmonary disease. N Engl J Med 1999; 340: 1941–1947.
Davies L, Angus RM, Calverley PM . Oral corticosteroids in patients admitted to hospital with exacerbations of chronic obstructive pulmonary disease: a prospective randomised controlled trial. Lancet 1999; 354: 456–460.
Maltais F, Ostinelli J, Bourbeau J, Tonnel AB, Jacquemet B, Haddon J et al. Comparison of nebulized budesonide and oral prednisolone with placebo in the treatment of acute exacerbations of chronic obstructive pulmonary disease: a randomized controlled trial. Am J Respir Crit Care Med 2002; 165: 698–703.
Aaron SD, Vandemheen KL, Hebert P, Dales R, Stiell IG, Ahuja J et al. Outpatient oral prednisone after emergency treatment of chronic obstructive pulmonary disease. N Engl J Med 2003; 348: 2618–2625.
de Jong YP, Uil SM, Grotjohan HP, Postma DS, Kerstjens HA, van den Berg JW . Oral or IV prednisolone in the treatment of COPD exacerbations: a randomized, controlled, double-blind study. Chest 2007; 132: 1741–1747.
Gunen H, Hacievliyagil SS, Yetkin O, Gulbas G . The role of nebulised budesonide in the treatment of acute exacerbations of COPD. Eur Respir J 2007; 30: 399–400.
Ställberg B, Selroos O, Vogelmeier C, Andersson E, Ekstrom T, Larsson K . Budesonide/formoterol as effective as prednisolone plus formoterol in acute exacerbations of COPD. A double-blind, randomised, non-inferiority, parallel-group, multicentre study. Respir Res 2009; 10: 11.
Alia I, de la Cal MA, Esteban A, Abella A, Ferrer R, Molina FJ et al. Efficacy of corticosteroid therapy in patients with an acute exacerbation of chronic obstructive pulmonary disease receiving ventilatory support. Arch Intern Med 2011; 171: 1939–1946.
Leuppi JD, Schuetz P, Bingisser R, Bodmer M, Briel M, Drescher T et al. Short-term vs conventional glucocorticoid therapy in acute exacerbations of chronic obstructive pulmonary disease: the reduce randomized clinical trial. JAMA 2013; 309: 2223–2231.
Gupta D, Agarwal R, Aggarval A, Maturu VN, Dhooria S, Prasad KT et al. Guidelines for diagnosis and management of chronic obstructive pulmonary disease: Joint ICS/NCCP (I) recommendations. Lung India 2013; 30: 228–267.
Khan JH, Lababidi HM, Al-Moamary MS, Zeitouni MO, Al-Jadhali HH, Al-Amoudi OS et al. The Saudi Guidelines for the Diagnosis and Management of COPD. Ann Thorac Med 2014; 9: 55–76.
Anthonisen N, Manfreda J, Warren C . Antiobiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 1987; 106: 196–204.
Seemungal T, Harper-Owen R, Bhowmik A, Moric I, Sanderson G, Message S et al. Respiratory viruses, symptoms, and inflammatory markers in acute exacerbations and stable chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2001; 164: 1618–1623.
Patel IS, Seemungal TA, Wilks M, Lloyd-Owen SJ, Donaldson GC, Wedzicha JA . Relationship between bacterial colonisation and the frequency, character, and severity of COPD exacerbations. Thorax 2002; 57: 759–764.
Nouira S, Marghli S, Belghith M, Besbes L, Elatrous S, Abroug F . Once daily oral ofloxacin in chronic obstructive pulmonary disease exacerbation requiring mechanical ventilation: a randomised placebo-controlled trial. Lancet 2001; 358: 2020–2025.
Berry DG, Fry J, Hindley CP, Hodson JM, Horder EJ, Horder JP et al. Exacerbations of chronic bronchitis treatment with oxytetracycline. Lancet 1960; 1: 137–139.
Fear E, Edwards G . Antibiotic regimens in chronic bronchitis. Br J Dis Chest 1962; 56: 153–162.
Elmes P, King T, Langlands J . Value of ampicillin in the hospital treatment of exacerbations of chronic bronchitis. Br Med J 1965; 2: 904–908.
Pines A, Raafat H, Plucinski K, Greenfield J, Solari M . Antibiotic regimens in severe and acute purulent exacerbations of chronic bronchitis. BMJ 1968; 2: 735–738.
Pines A, Raafat H, Greenfield JS, Linsell WD, Solari ME . Antibiotic regimens in moderately ill patients with purulent exacerbations of chronic bronchitis. Br J Dis Chest 1972; 66: 107–115.
Manresa F, Blavia R, Martin R, Linares J, Rodriguez B, Verdaguer R . Antibiotics for exacerbations of chronic bronchitis. Lancet 1987; 2: 394–395.
Jørgensen AF, Coolidge J, Pedersen PA, Petersen KP, Waldorff S, Widding E . Amoxicillin in treatment of acute uncomplicated exacerbations of chronic bronchitis. A double-blind, placebo-controlled multicentre study in general practice. Scand J Prim Health Care 1992; 10: 7–11.
Sachs AP, Koëter GH, Groenier KH, van der Waaij D, Schiphuis J, Meyboom-de Jong B . Changes in symptoms, peak expiratory flow, and sputum flora during treatment with antibiotics of exacerbations in patients with chronic obstructive pulmonary disease in general practice. Thorax 1995; 50: 758–763.
Brusse-Keizer M, van der Valk P, Hendrix R, Kerstjens H, van der Pale J . Antibiotics in patients with a mild to moderate home-treated COPD exacerbation: the ABC trial. Am J Respir Crit Care Med 2009; 179: Abstract 1493.
Daniels JM, Snijders D, de Graaff CS, Vlaspolder F, Jansen HM, Boersma WG . Antibiotics in addition to systemic corticosteroids for acute exacerbations of chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2010; 181: 150–157.
Llor C, Bjerrum L, Munck A, Hansen MP, Cordoba GC, Strandberg EL et al. Predictors for antibiotic prescribing in patients with exacerbations of COPD in general practice. Ther Adv Respir Dis 2013; 7: 131–137.
Schott G, Dünnweber C, Mühlbauer B, Niebling W, Pachl H, Ludwig W . Does the pharmaceutical industry influence guidelines? Two examples from Germany. Dtsch Arztebl Int 2013; 110: 575–583.
Iqbal A, Schloss S, George D, Isonaka S . Worldwide guidelines for chronic obstructive pulmonary disease: a comparison of diagnosis and treatment recommendations. Respirology 2002; 7: 233–239.
Miravitlles M, Anzueto A, Ewig S, Legnani D, Stauch K . Characterisation of exacerbations of chronic bronchitis and COPD in Europe: the GIANT study. Ther Adv Respir Dis 2009; 3: 267–277.
Herland K, Akselsen J-P, Skjønsberg OH, Bjermer L . How representative are clinical study patients with asthma or COPD for a larger “real life” population of patients with obstructive lung disease? Respir Med 2005; 99: 11–19.
Rodriguez-Roisin R . Toward a consensus definition for COPD exacerbations. Chest 2000; 117: 398–401.
Siafakas NM, Vermeire P, Pride NB, Paoletti P, Gibson J, Howard P et al. Optimal assessment and management of chronic obstructive pulmonary disease (COPD): a consensus statement of the European Respiratory Society. Eur Respir J 1995; 8: 1398–1420.
Bullard MJ, Liaw SJ, Tsai YH, Min HP . Early corticosteroid use in acute exacerbations of chronic airflow obstruction. Am J Emerg Med 1996; 14: 139–143.
Vestbo J, Hurd SS, Agusti AG, Jones PW, Vogelmeier C, Anzueto A et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med 2013; 187: 347–365.
Allegra L, Blasi F, Diano P, Consentini R, Tarsia P, Confalonieri M et al. Sputum color as a marker of acute bacterial exacerbations of chronic obstructive pulmonary disease. Respir Med 2005; 99: 742–747.
Miravitlles M, Moragas A, Hernandez S, Bayona C, Llor C . Is it possible to identify exacerbations of mild to moderate COPD that do not require antibiotic treatment? Chest 2013; 144: 1571–1577.
Brusse-Keizer MG, Grotenhuis AJ, Kerstjens HA, Telgen MC, van der Palen J, Hendrix MG et al. Relation of sputum colour to bacterial load in acute exacerbations of COPD. Respir Med 2009; 103: 601–606.
Koutsokera A, Stolz D, Loukides S, Kostikas K . Systemic biomarkers in exacerbations of copd: the evolving clinical challenge. Chest 2012; 141: 396–405.
Nyström P . The systemic inflammatory response syndrome: definitions and aetiology. J Antimicrob Chemother 1998; 41: 1–7.
McNally M, Curtain J, O'Brien KK, Dimitrov BD, Fahey T . Validity of British Thoracic Society guidance (the CRB-65 rule) for predicting the severity of pneumonia in general practice: systematic review and meta-analysis. Br J Gen Pract 2010; 60: e423–e433.
Edwards L, Perrin K, Wijesinghe M, Weatherall M, Beasley R, Travers J . The value of the CRB65 score to predict mortality in exacerbations of COPD requiring hospital admission. Respirology 2011; 16: 625–629.
Lacoma A, Prat C, Andreo F, Lores L, Ruiz-Manzano J, Ausina V et al. Value of procalcitonin, C-reactive protein, and neopterin in exacerbations of chronic obstructive pulmonary disease. Int J Chron Obstruct Pulmon Dis 2011; 6: 157–169.
Schuetz P, Christ-Crain M, Thomann R, Falconnier C, Wolbers M, Widmer I et al. Effect of procalcitonin-based guidelines vs standard guidelines on antibiotic use in lower respiratory tract infections: the ProHOSP randomized controlled trial. JAMA 2009; 302: 1059–1066.
Bafadhel M, Clark TW, Reid C, Medina MJ, Batham S, Barer MR et al. Procalcitonin and C-reactive protein in hospitalized adult patients with community-acquired pneumonia or exacerbation of asthma or COPD. Chest 2011; 139: 1410–1418.
Daniels JMA, Schoorl M, Snijders D, Knol DL, Lutter R, Jansen HM et al. Procalcitonin vs c-reactive protein as predictive markers of response to antibiotic therapy in acute exacerbations of COPD. Chest 2010; 138: 1108–1115.
Stolz D, Christ-Crain M, Bingisser R, Leuppi J, Miedinger D, Muller C et al. Antibiotic treatment of exacerbations of COPD: a randomized, controlled trial comparing procalcitonin-guidance with standard therapy. Chest 2007; 131: 9–19.
Miravitlles M, Calle M, Soler-Cataluña JJ . Clinical Phenotypes of COPD: Identification, Definition and Implications for Guidelines. Arch Bronconeumol 2012; 48: 86–98.
Block LH, Burghuber OC, Hartl S, Zwick H . Österreichische Gesellschaft für Lungenerkrankungen und Tuberkulose: Konsensus zum Management der chronisch obstruktiven Lungenerkrankung (COPD). Wien Klin Wochenschr 2004; 116: 268–278.
Bellamy D, Bouchard J, Henrichsen S, Johansson G, Langhammer A, Reid J et al. International Primary Care Respiratory Group (IPCRG) Guidelines: management of chronic obstructive pulmonary disease (COPD). Prim Care Respir J 2006; 15: 48–57.
Sundhedsstyrelsen. KOL-Kronisk Obstruktiv Lungesygdom. Anbefalinger for Tidlig Opsporing, Opfølgning, Behandling og Rehabilitering. Sundhedsstyrelsen: København, Denmark, 2007.
Smeele I, Van Weel C, Van Schayck C, Van der Molen T, Thoonen B, Schermer T et al. De standaard en de wetenschappelijke verantwoording zijn geactualiseerd ten opzichte van de vorige versies van de NHG-Standaarden COPD en astma bij volwassenen: diagnostiek (Huisarts Wet 2001;44;107-17) en COPD: behandling (Huisarts Wet 2001;44;207-19). Huisarts Wet 2007; 50: 362–379.
Läkemedelsverket. Farmakologisk behandling av kroniskt obstruktiv lungesjukdom-KOL. Information från Läkemedelsverket 2009; 2: 13–28.
Höffken G, Lorenz J, Kern W, Welte T, Bauer T, Dalhoff K et al. [Epidemiology, diagnosis, antimicrobial therapy and management of community-acquired pneumonia and lower respiratory tract infections in adults. Guidelines of the Paul-Ehrlich-Society for Chemotherapy, the German Respiratory Society, the German Society for Infectiology and the Competence Network CAPNETZ Germany]. Pneumologie 2009; 63: e1–68.
National Clinical Guideline Centre. (2010) Chronic Obstructive Pulmonary Disease: Management of Chronic Obstructive Pulmonary Disease in Adults in Primary and Secondary Care. London: National Clinical Guideline Centre. http://guidance.nice.org.uk/CG101/Guidance/pdf/English.
Abdool-Gaffar MS, Ambaram A, Ainslie GM, Bolliger CT, Feldman C, Geffen L et al. Guideline for the management of chronic obstructive pulmonary disease-2011 update. S Afr Med J 2011; 101: 63–73.
Guidelines and Protocols Advisory Committee. Chronic Obstructive Pulmonary Disease (COPD). British Columbia Medical Association, Medical Services Commission: Victoria, BC, Canada, 2011.
Woodhead M, Blasi F, Ewig S, Garau J, Huchon G, Ieven M et al. Guidelines for the management of adult lower respiratory tract infections-Full version. Clin Microbiol Infect 2011; 17: 1–59.
McKenzie DK, Abrahamson M, Crockett AJ, Dabscheck E, Glasgow N, Jenkins S et al. The Australian Lung Foundation. The COPD X-Plan: Australian and New Q12 Zealand Guidelines for the management of Chronic Obstructive Pulmonary Disease V2.32,2011.
Helsedirektoratet. KOLS-Nasjonal Faglig Retningslinje og Veileder for Forebygging, Diagnostisering og Oppfølging av Personer med kols. Helsedirektoratet: Oslo, Norway, 2012.
Russi EW, Karrer W, Brutsche M, Eich C, Fitting JW, Frey M et al. Diagnosis and management of chronic obstructive pulmonary disease: the Swiss guidelines. Official guidelines of the Swiss Respiratory Society. Respiration 2013; 85: 160–174.
Anderson B, Conner K, Dunn C, Kerestes G, Lim K, Myers C . et al. Diagnosis and Management of Chronic Obstructive Pulmonary Disease (COPD). Bloomington, MN, USA: Institute for Clinical Systems Improvement, 2013.
Global Initiative for Chronic Obstructive Lung Disease Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. Vancouver, WA, USA: GOLD, 2013.
Stoller JK. Management of acute exacerbations of chronic obstructive pulmonary disease. UpToDate 2013.
Bartlett JG, Sethi S. Management of infection in acute exacerbations of chronic obstructive pulmonary disease. UpToDate 2013.
Miravitlles M, Soler-Cataluna JJ, Calle M, Molina J, Almagro P, Quintano JA et al. Spanish guideline for COPD (GesEPOC). Update 2014. Arch Bronconeumol 2014; 50 (Suppl 1): 1–16.
Emerman CL, Connors AF, Lukens TW, May ME, Effron D . A randomized controlled trial of methylprednisolone in the emergency treatment of acute exacerbations of COPD. Chest 1989; 95: 563–567.
Acknowledgements
We thank Nora Willie MacLaren for support with the graphical work.
Author information
Authors and Affiliations
Contributions
JL is the main author as she was primarily engaged in designing and conducting the study. ER performed the systematic literature search and contributed with guidance relevant for the method used in the study. HM supervised the whole work and assisted in the eligibility assessment of the search results.
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
Laue, J., Reierth, E. & Melbye, H. When should acute exacerbations of COPD be treated with systemic corticosteroids and antibiotics in primary care: a systematic review of current COPD guidelines. npj Prim Care Resp Med 25, 15002 (2015). https://doi.org/10.1038/npjpcrm.2015.2
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/npjpcrm.2015.2
This article is cited by
-
Drug-related problems among hospitalized patients with COPD in mainland China
International Journal of Clinical Pharmacy (2019)
-
Guideline adherence in hospital recruited and population based COPD patients
BMC Pulmonary Medicine (2018)
-
Budesonide, fluticasone propionate, and azithromycin do not modulate the membrane vesicle release by THP-1 macrophages and respiratory pathogens during macrophage infection
Inflammopharmacology (2017)