Abstract
Asthma is a heterogeneous disorder, evidenced by distinct types of inflammation resulting in different responsiveness to therapy with glucocorticoids (GCs). Tumor necrosis factor α (TNFα) is involved in asthma pathogenesis, but anti-TNFα therapies have not proven broadly effective. The effects of anti-TNFα treatment on steroid resistance have never been assessed. We investigated the role of TNFα blockade using etanercept in the responsiveness to GCs in two ovalbumin-based mouse models of airway hyperinflammation. The first model is GC sensitive and T helper type 2 (Th2)/eosinophil driven, whereas the second reflects GC-insensitive, Th1/neutrophil-predominant asthma subphenotypes. We found that TNFα blockade restores the therapeutic effects of GCs in the GC-insensitive model. An adoptive transfer indicated that the TNFα-induced GC insensitivity occurs in the non-myeloid compartment. Early during airway hyperinflammation, mice are GC insensitive specifically at the level of thymic stromal lymphopoietin (Tslp) transcriptional repression, and this insensitivity is reverted when TNFα is neutralized. Interestingly, TSLP knockout mice displayed increased inflammation in the GC-insensitive model, suggesting a limited therapeutic application of TSLP-neutralizing antibodies in subsets of patients suffering from Th2-mediated asthma. In conclusion, we demonstrate that TNFα reduces the responsiveness to GCs in a mouse model of neutrophilic airway inflammation. Thus antagonizing TNFα may offer a new strategy for therapeutic intervention in GC-resistant asthma.
Similar content being viewed by others
INTRODUCTION
Asthma is a chronic inflammatory disorder of the airways affecting >300 million people worldwide. Asthma is characterized by variable airway obstruction caused by airway smooth muscle hyper-responsiveness, mucus hyperproduction, and airway wall inflammation. Most asthma patients have mild-to-moderate disease that can be effectively treated with inhaled glucocorticoids (GCs). These anti-inflammatory drugs are often given in combination with short- or long-acting β2-adrenergic bronchodilators. GCs exert their anti-inflammatory effects via the intracellular glucocorticoid receptor (GR). Upon binding with GCs, GR translocates to the nucleus, where it transactivates or transrepresses specific genes. Transcriptional activation by GR is mainly mediated by binding of GR dimers to GC responsive elements (GRE), followed by induction of metabolic and anti-inflammatory genes.1 In addition, GR dimers can also repress certain genes by binding to so-called negative GRE elements (nGRE).2 Furthermore, GR can repress gene transcription by DNA-independent mechanisms, such as protein–protein interactions between monomeric GR and other transcription factors. Unfortunately, approximately 10% of asthma patients respond poorly to GCs, and these patients account for more than half of the health-care costs associated with asthma.3, 4, 5 Recently, it has become evident that asthma is a heterogeneous disease and that there is a need to select and improve therapy by segregating asthma patients into subgroups based on the inflammatory environment in the lung, and consequently their response to GCs, and to treat them accordingly.6, 7, 8
The mechanisms of asthma pathogenesis are not completely understood. Many different immune cells (dendritic cells (DCs), lymphocytes, eosinophils, mast cells) and structural cells (airway smooth muscle and epithelial cells) are involved.9, 10 In mild disease, the inflammatory response is dominated by a T helper type 2 (Th2) phenotype and eosinophil influx, whereas in more severe GC-resistant forms neutrophils are also recruited and a mixed Th2/Th1 phenotype with a Th17 component is observed.11 All these cells release various cytokines that contribute to the different features of asthma. Therefore, several biological agents have been developed to target key cytokines, such as interleukin 4 (IL4), IL5, IL9, IL13, and tumor necrosis factor α (TNFα).12 TNFα cytokine is involved in the recruitment of neutrophils and eosinophils and has been implicated in the inflammatory response during asthma.13 In addition, increased TNFα levels have been observed in asthma patients who respond poorly to GC therapy.14 Although some small-scale clinical studies with the soluble blocker of TNFα, etanercept, were promising,14, 15 larger follow-up studies with golimumab and etanercept did not show a beneficial effect in patients with severe asthma.16, 17 This may be due to different design of the trials, including the differential inclusion of GC treatment in the patient population, and the response of these patients to GCs. However, the effect of TNFα neutralization on GC refractoriness was never assessed.
Because of the potential link between TNFα levels and lack of GC response observed in asthma patients, we wondered whether neutralization of TNFα could restore GC sensitivity during severe asthma. To answer this question, mouse models were applied that mimic the heterogeneity of cellular inflammation found in patients with asthma. We used two ovalbumin (OVA)-based mouse models of airway inflammation. Prior sensitization with OVA combined with complete Freund’s adjuvant (CFA), a potent Th1/Th17 skewing adjuvant, results in neutrophilic pulmonary inflammation that is poorly controlled by GCs. In contrast, mice sensitized with OVA in the presence of aluminum hydroxide (Alum) display a conventional Th2/eosinophil-driven inflammation that responds well to GCs.18 By assessing inflammatory cell infiltration, cytokine production, goblet cell metaplasia, and airway hyper-responsiveness (AHR), we showed that TNFα neutralization using etanercept restores GC sensitivity in the GC-resistant OVA/CFA model.
RESULTS
Role of TNFα in the GC-insensitivity model
Immunization of mice with OVA/CFA has been reported to cause neutrophilic pulmonary inflammation that is poorly controlled by GCs, in contrast to the Th2-dominated GC-sensitive lung inflammation provoked by OVA/Alum.18 We confirmed that immunization with OVA, followed 3 weeks later by nebulized OVA for 2 consecutive days, leads to significant cell infiltration in the broncho-alveolar lavage (BAL) fluid compared with naive mice (Figure 1a). In mice sensitized to OVA/Alum, dexamethasone (Dex) treatment significantly reduced the immune cell influx in the lungs, whereas mice sensitized with OVA/CFA were unresponsive to Dex. Thus, in contrast to the OVA/Alum-based mouse model of eosinophilic airway inflammation, the OVA/CFA-based model reflects GC-insensitive, neutrophil-predominant asthma, also seen in a subset of steroid-resistant endotypes of human asthma (Figure 1b).
Tumor necrosis factor α (TNFα) has an important role in the glucocorticoid-insensitive model of ovalbumin (OVA)/complete Freund’s adjuvant (CFA)-induced airway hyperinflammation. (a) In general, mice were systemically sensitized against OVA in the presence of either OVA/CFA or OVA/Alum, followed by exposure to OVA aerosols for 2 consecutive days. Three hours before the exposure to aerosols, mice were injected with 1 mg kg−1 Dex and/or 10 mg kg−1 etanercept. One day later, broncho-alveolar lavage (BAL) fluid was isolated to determine differential cell counts and cytokines levels. (b, c) Pulmonary immune cell populations (b) and TNFα levels (c) were measured (n=7−9). Three hours before the exposure to OVA aerosols, mice were treated with phosphate-buffered saline (PBS) or 1 mg kg−1 dexamethasone (Dex). Controls were not challenged with OVA aerosols. On the cytospin images, it is clear that there is a predominant influx of neutrophils (nucleus with 3–5 lobes) in the lungs of the OVA/CFA-treated mice, whereas the OVA/Alum model is characterized by an eosinophil (pinkish and bilobed) driven inflammation. (d) Total cell numbers were counted in the BAL fluid from mice exposed to OVA/CFA. Mice were treated with PBS or different doses of the TNFα-blocking agent (α-TNFα), etanercept (100, 200, or 400 μg per mouse; n=8−10). In all the figures, the results show one representative experiment out of at least three independent experiments. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. ND, non-detectable levels; NS, no significant differences. *P<0.05, **P<0.01, and ***P<0.001.
In severe GC-refractory asthma, neutrophils predominate19 and TNFα promotes recruitment of neutrophils into the airways.20 So we reasoned that TNFα could have a role in the pathology of severe asthma. Higher TNFα levels have already been observed in GC-resistant asthma patients.14 Likewise, in our GC-insensitive mouse model of neutrophilic airway inflammation, TNFα levels were high in the BAL fluid, in contrast to the non-detectable levels in the GC-sensitive OVA/Alum model (Figure 1c).
To investigate the role of TNFα in GC insensitivity, we neutralized TNFα with etanercept, a soluble, recombinant TNFα receptor 2, fused to a human immunoglobulin G Fc fragment. We used 200 μg of etanercept per mouse because this dose did not significantly reduce the pulmonary cell influx on its own (Figure 1d).
Neutralization of TNFα restores GC sensitivity in the OVA/CFA model
In contrast to the treatment with TNF antagonists alone, the combination of etanercept and Dex reverted the Dex insensitivity. In addition, upon genetic or pharmacological inhibition of the TNFα receptor 1 (TNFR1), BAL cellular infiltration in response to OVA/CFA sensitization could also be reduced by Dex. This suggests that TNFα signaling downstream of its TNFR1 impairs GR function in the OVA/CFA airway hypersensitivity model (Figure 2a). The total white blood cell influx in the lungs suggests that TNFα blockade restores the beneficial effects of GCs in the GC-insensitive model. Next, we determined differential cell counts in the BAL fluid in response to OVA/CFA or OVA/Alum immunization. It is known that eosinophils are the most abundant cells to infiltrate the lungs, next to infiltration of other immune cells, such as T lymphocytes, macrophages, DCs, and neutrophils. However, immunization with CFA predisposes mice to a more neutrophil-based inflammation. As expected, Dex decreased OVA/Alum-induced inflammatory cell influx in the lungs but did not reduce the recruitment of immune cells in the OVA/CFA model (Figures 1b and 2a).18 Interestingly, blocking TNFα with etanercept reverted Dex insensitivity at the level of immune cell influx (Figure 2a). Similar results were obtained for different immune cell, such as eosinophils, neutrophils, and DCs (Figure 2b). In addition to the lung airspace inflammation, tissue inflammation, determined by CD45 immunostaining, was also significantly reduced by combination treatment with etanercept and Dex. Note that Dex alone already significantly reduced the presence of immune cells residing in the lung tissue, although to a lesser extent (Figure 2c). This suggests that this model is not GC resistant but rather GC insensitive at the level of lung cellular inflammation.
Tumor necrosis factor α (TNFα) neutralization restores glucocorticoid sensitivity in the ovalbumin (OVA)/complete Freund’s adjuvant (CFA)-induced model of airway hyperinflammation. All mice were sensitized with OVA/CFA or aluminum hydroxide (OVA/Alum). After 3 weeks, they were challenged on 2 consecutive days with OVA aerosols. Twenty-four hours after the last aerosol, broncho-alveolar lavage (BAL) fluid was obtained for flow cytometry analyses and lungs for immunohistochemistry (n=6−7 per group in all experiments). (a) Total cell numbers were counted in the BAL from mice exposed to OVA/CFA or OVA/Alum. Three hours before the OVA aerosols, mice were treated with phosphate-buffered saline (PBS) or 1 mg kg−1 dexamethasone (Dex). Mice were given simultaneously 200 μg etanercept (α-TNF) or 200 μg of a TNFR1-blocking antibody (α-TNFR1). In addition to C57BL/6 mice, heterozygous (C57BL/6 × TNFR1 knockout) F1 mice (TNFR1 F1) were immunized with OVA/CFA and treated with PBS or Dex (n=5−6 per group). (b, c) Three hours before each aerosol, mice were injected intraperitoneally with 1 mg kg−1 Dex and/or 200 μg etanercept (α-TNF). (b) Differential cell counts, neutrophils and dendritic cells (DCs) in the BAL were measured by flow cytometry. (c) Lung tissue was stained with an anti-CD45 antibody to quantify the number of immune cells. All experiments were performed at least twice; data from a representative experiment are shown. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. *P<0.05, **P<0.01, and ***P<0.001.
We also measured the levels of cytokines in BAL fluid collected 24 h after the last aerosol challenge. OVA-treated mice showed high levels of pro-inflammatory cytokines, such as IL6 (Figure 3a) and IL17 (Figure 3b); these levels could not be reduced by Dex treatment in the OVA/CFA model, in contrast to the OVA/Alum model. However, when TNFα was inhibited, Dex significantly reduced the secretion of cytokines (Figure 3a, b). In addition, interferon γ levels were higher in the OVA/CFA-induced model (Figure 3c), which is typical for a Th1-mediated inflammatory environment, whereas the IL13 levels represent Th2-mediated inflammation (Figure 3d). We also measured the mRNA expression (by quantitative PCR) of other inflammatory mediators, such as the neutrophil chemoattractant keratinocytes (KC), and observed higher levels in the OVA/CFA model (Figure 3e). In addition, the expression of matrix metalloproteinase 9 (MMP9), which has a detrimental role in asthma, was increased in the OVA/CFA model (Figure 3f). These levels could only be reduced upon co-treatment with GCs and etanercept (Figure 3e, f).
Tumor necrosis factor α (TNFα) antagonism restores glucocorticoid sensitivity to several inflammatory parameters in the ovalbumin (OVA)/complete Freund’s adjuvant (CFA) model. Dexamethasone (Dex) improves lung function in the OVA/CFA model when TNF signaling is blocked. All mice were sensitized with OVA/CFA or aluminum hydroxide (OVA/Alum). After 3 weeks, they were challenged on 2 consecutive days with OVA aerosols. Twenty-four hours after the last aerosol, broncho-alveolar lavage (BAL) fluid was obtained for cytokine levels and lungs for gene expression and mucus staining (n=6−7 per group in all experiments). (a–d) BAL cytokine levels, interleukin 6 (IL6), IL17, interferon γ (IFNγ), and IL13 were measured. (e, f) mRNA expression of (e) keratinocytes (KC) and (f) matrix metalloproteinase 9 (MMP9) in the lungs was determined. (g) Mucus production was evaluated by periodic acid-Schiff staining of lung paraffin sections. Representative pictures are shown here; goblet cells are visible by the bright pink color. (h) Gene expression of the mucin genes Muc5b (left panel) and Muc5ac (right panel) was measured by quantitative PCR. All experiments were performed at least twice; data from a representative experiment are shown. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. *P<0.05, **P<0.01, and ***P<0.001. PBS, phosphate-buffered saline.
Airway mucus acts as a physical and biological barrier between the environment and the epithelium. In asthma, excessive mucus, caused by goblet cell metaplasia, is a hallmark of airway remodeling and causes severe airway obstruction, sometimes leading to death by mucus impaction. Dex reduced the number of mucus-producing goblet cells in OVA/Alum-sensitized mice, as revealed by periodic acid-Schiff staining, but not in OVA/CFA-treated mice. Goblet cell metaplasia was reduced in the OVA/CFA model only when Dex and etanercept were used together (Figure 3g). In addition, co-treatment also reduced the expression of the mucin genes, Muc5b and Muc5ac, in the lung of OVA/CFA-treated mice (Figure 3h).
OVA sensitization and subsequent challenge is known to lead to the development of AHR. Therefore, we also assessed the effect of treatment with Dex combined with the TNFα-neutralization agent, relative to treatment with Dex alone, on airway responses in the OVA/CFA model. Therefore, we measured compliance and airway tissue elasticity to aerosolized methacholine (MCh) by an invasive method 24 h after the last challenge. As expected, OVA-sensitized/challenged mice exhibited aggravation of lung function in response to MCh, which could be improved with Dex in the OVA/Alum model. Dex alone had no effect on AHR to inhaled MCh in the OVA/CFA model; it was effective only in combination with etanercept (Figure 4a, b).
Dex improves lung function in the OVA/CFA model when TNF signaling is blocked. Mice (n=6 per treatment group) were exposed to increasing doses of aerolized methacholine 24 h after the last ovalbumin (OVA) challenge, and airway flexibility was measured. Both (a) compliance and (b) airway tissue elasticity were determined. This experiment was performed twice; data are representative of both experiments. Significance levels are compared within the OVA/complete Freund’s adjuvant (CFA) or OVA/Alum model and compared with the phosphate-buffered saline (PBS)-treated group. *P<0.05. Dex, dexamethasone; TNFα, tumor necrosis factor α.
TNFα blocks GR actions in the non-myeloid compartment
Many different inflammatory cells and mediators are involved in the pathophysiology of asthma, both non-immune cells (such as epithelial cells) and immune cells. Therefore, we wondered which cellular compartment was responsible for the TNFα-induced GC insensitivity in the OVA/CFA model. We generated radiation chimeric mice by sublethally irradiating C57BL6 mice and reconstituting them with bone marrow derived from donor C57BL/6 or TNFR1 knockout (KO) mice. Note that we could not use TNFR1 KO mice as a recipient of C57BL/6 bone marrow cells as TNFR1 KO mice cannot generate an antibody response to allergens.21 These experiments showed that, in mice with defective TNFα signaling in the hematopoietic lineage, the GC insensitivity at the level of differential white blood cell influx is retained (Figure 5a). This indicates that TNFα impairs GC actions in the non-myeloid compartment.
Tumor necrosis factor α (TNFα) blocks the beneficial anti-inflammatory actions of glucocorticoid response (GR) in the non-myeloid compartment. (a) C57BL/6 mice were irradiated and reconstituted with bone marrow derived from C57BL/6 (WT) or TNFR1 knockout mice. These chimeric mice were sensitized with ovalbumin (OVA)/complete Freund’s adjuvant (CFA) and challenged with OVA 3 weeks later. In addition, control C57BL/6 mice were sensitized with OVA/Alum. All mice were treated with phosphate-buffered saline (PBS) or 1 mg kg−1 dexamethasone (Dex) and/or 200 μg etanercept (α-TNF) (n=6). Differential cell counts were determined 24 h after the last OVA aerosol. (b, c) A549 airway epithelial cells were treated for 5 h with 1 μM Dex with or without 1 h of pretreatment with 1,000 IU ml−1 TNFα (n=6). We analyzed GRE (GR element)-luciferase expression (b, left graph) and mRNA expression of Gilz, a typical GRE gene (b, right graph). In addition, the effect on the expression of a negative nGRE-luciferase reporter was checked (c). (d) A549 cells were treated with different combinations of 1 μM Dex, 1000 IU ml−1 TNFα, and 100 ng ml−1 lipopolysaccharide (LPS). TNFα or PBS was given first, 3 h later cells were washed and Dex or PBS was added, and 2 h after that the cells were washed and LPS or PBS was added. Twenty-four hours after the first treatment, interleukin 6 (IL6) in the supernatant was measured. All experiments were performed at least twice, and data from a representative experiment are shown. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. *P<0.05, **P<0.01, and ***P<0.001.
To further study how TNFα blocks GR actions in structural cells, we used A549 airway epithelial cells. Based on analysis using a GRE-luciferase reporter system and endogenous GRE gene expression, such as Tsc22d3 (Gilz), we found that TNFα pretreatment of the cells impaired the GR dimerization–dependent gene expression (Figure 5b). Moreover, TNFα pretreatment also abolished the GR dimerization–dependent repression of a nGRE luciferase reporter system (Figure 5c), but it did not affect the transrepression capacity of GR at the level of suppression of IL6 secretion (Figure 5d). These observations suggest that TNFα specifically impairs the GR dimerization–dependent actions.
Early during airway hyperinflammation, OVA/CFA-treated mice are insensitive at the level of thymic stromal lymphopoietin (Tslp) transrepression
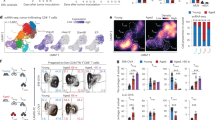
It has been suggested that reduced transcriptional activity of GR could contribute to reduced GC sensitivity in asthma patients.22 As we could not measure GRE gene induction kinetic in the lung of OVA-treated mice after 24 h of Dex treatment, we determined the induction profile of GR dimer–dependent genes first in non-immunized mice. This showed early induction by Dex of GRE-dependent genes, such as Gilz, Dusp1 and Fkbp5, in the lung tissue (Figure 6a). We examined inflammatory parameters in our GC-insensitive and GC-sensitive mouse models of airway hypersensitivity on the first day of OVA aerosol treatment after 6 h of treatment (Figure 6b). The results indicate that TNFα neutralization cannot yet revert GC insensitivity at this early time point, at the level of pulmonary white blood cell influx. Interestingly, the recruitment of neutrophils, characteristic for the OVA/CFA-induced airway hyperinflammation model, was not yet pronounced in the OVA/CFA-treated group at this early time point (Figure 6c). Next, we analyzed Dex sensitivity at this early time point at the levels of transactivation, i.e., induction of GRE genes Gilz and Fkbp5 (Figure 6d), and transrepression of IL6 levels (Figure 6e). We observed that both GR functions seemed to be functional in the GC-insensitive OVA/CFA model (Figure 6d, e). We then analyzed the transrepression actions of GR, which are mediated by direct binding of GR dimers to nGRE elements. Repression by Dex also seemed to be functional, at least at the level of the GR-mediated repression of Ccnd1 and Prkcb (Figure 6f), which are typical nGRE genes.2 However, transrepression of Tslp (involved in the communication between epithelial cells and DCs) by Dex was absent in the OVA/CFA model. Dex repressed Tslp expression only when TNFα was inhibited (Figure 6g). These data suggest that TNFα impairs GR function specifically at the level of Tslp repression.
During early stages, tumor necrosis factor α (TNFα) blocks the glucocorticoid response (GR) actions specifically at the level of thymic stromal lymphopoietin (TSLP) transrepression. (a) C57BL/6 mice were treated with 1 mg kg−1 dexamethasone (Dex), and after different intervals (0, 2, 6, and 24 h) lungs were isolated and mRNA expression of several GR element genes, Gilz, Dusp1, and Fkbp5, was determined. (b) C57BL/6 mice were sensitized with ovalbumin (OVA) combined with complete Freund’s adjuvant (OVA/CFA) or aluminum hydroxide (OVA/Alum), and after 3 weeks they were challenged with an OVA aerosol. Three hours before the aerosol, mice were injected intraperitoneally with 1 mg kg−1 Dex and/or 200 μg etanercept (α-TNF). Six hours after injection, broncho-alveolar lavage (BAL) fluid and lungs were isolated (n=6 - 7 per group in all experiments). Total cell counts and the number of neutrophils were measured in the (c) BAL fluid, and gene expression levels of (d) Gilz and Fkbp5, (e) Il6, (f) Prkcb and Ccnd1, and (g) Tslp were determined in lung tissues. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. NS, no significant differences; *P<0.05, **P<0.01, and ***P<0.001.
OVA/CFA-treated TSLP-deficient mice show increased immune responses
It is known that TSLP is involved in airway inflammation and immune cell recruitment23 and can have a pivotal role in the induction of GC resistance.24 Therefore we wanted to check whether impaired repression of Tslp by Dex in the OVA/CFA model contributes to the GC insensitivity. We subjected wild-type (WT) and TSLP KO mice to the OVA/CFA or OVA/Alum model, as described in Figure 1a. These data show that less cells were recruited in the lungs of phosphate-buffered saline (PBS)-treated TSLP KO mice in the OVA/Alum model, as expected, while more were recruited in the OVA/CFA model, compared with the PBS-treated WT mice (Figure 7a). Also at the level of neutrophil influx (Figure 7b), the levels of cytokines, TNF (Figure 7c), interferon γ (Figure 7d), and chemokine keratinocytes (Figure 7f) were higher in the OVA/CFA-treated TSLP KO mice compared with the WT mice. In contrast, the IL17A levels were similar in both the genotypes after OVA/CFA sensitization (Figure 7e), suggesting a positive role for TSLP in repressing the Th1-mediated inflammation, which occurs during OVA/CFA-induced airway immune responses. Except at the level of total immune cell recruitment (Figure 7a), TNF neutralization could restore the Dex insensitivity in the TSLP KO mice, similar to the WT mice after OVA/CFA treatment (Figure 7b–f).
Thymic stromal lymphopoietin (TSLP) deficiency aggravates immune response in ovalbumin (OVA)/complete Freund’s adjuvant (CFA)-treated mice. C57BL/6 (n=6) and TSLP knockout (n=10) mice were sensitized with OVA/CFA or aluminum hydroxide (OVA/Alum) and after 3 weeks challenged on 2 consecutive days with OVA aerosols. Three hours before each aerosol, mice were injected intraperitoneally with 1 mg kg−1 dexamethasone (Dex) and/or 200 μg etanercept (α-tumor necrosis factor (α-TNF)). Twenty-four hours after the last aerosol, broncho-alveolar lavage (BAL) fluid was obtained and (a) total cell counts, as well as (b) neutrophil counts were measured. (c - f) BAL cytokine and chemokines levels were also determined. Significance levels were calculated for differences as indicated in the figures. Error bars represent the mean±s.e. NS, no significant differences; *P<0.05, **P<0.01, and ***P<0.001. IFN, interferon; IL, interleukin; KC, keratinocytes; PBS, phosphate-buffered saline.
DISCUSSION
Asthma is a heterogeneous clinical disorder characterized by airway inflammation consisting of immune cell infiltrates, goblet cell metaplasia and mucus overproduction, remodeling of the airway wall, and AHR. Asthma is generally considered an eosinophilic/Th2 disorder that can be effectively treated by steroid therapy. However, at the severe, GC-insensitive end of the disease spectrum the inflammatory cell profile is altered and is characterized by a mixed Th2/Th1 immune response and increased influx of neutrophils, in addition to the presence of eosinophils. Several cytokines, such as TNF, interferon γ, and IL17, are specifically elevated in these subsets and may induce the influx of neutrophils.1, 18 Typically, patients with this severe asthma endotype are clinically refractory to GC treatment.7, 8, 14, 25 As these patients account for most of the health-care costs associated with asthma, and because therapeutic options are limited, more effective treatments are urgently needed. Elucidating the molecular basis of this GC insensitivity may lead to the design of more (cost-)effective GC-based therapies.
Understanding the etiology of GC-insensitive asthma endotypes requires appropriate predictive animal models. Most murine asthma models are based on Th2-biased sensitization and eosinophilic inflammation, which mimic mild-to-moderate GC-sensitive asthma. This illustrates the failure of current models to implement the neutrophil component, which is a characteristic of subsets of severe GC-insensitive asthma.26 Here we used a model in which mice were sensitized with OVA in the presence of CFA and subsequently exposed to nebulized OVA. This model reflects the Th1 and neutrophilic inflammatory environment, which is a characteristic of severe asthma and is GC insensitive, in contrast to the commonly used GC-sensitive OVA/Alum-based models.18 It had been suggested that increased TNFα is a feature of more persistent and GC refractory asthma.14 We also found increased levels of TNFα in the BAL fluid of mice exposed to OVA/CFA compared with OVA/Alum mice, which are refractory to steroid treatment. It has been postulated that TNFα has a pivotal role in the recruitment of neutrophils27, 28 and in the steroid resistance of severe asthma.14, 15, 29 Therefore, several small-scale uncontrolled studies assessed the effect of etanercept in GC insensitive asthma patients,14, 15 suggesting that anti-TNFα therapies might be beneficial in treating patients with severe asthma. However, the improvements were relatively modest and other large multicenter studies with anti-TNFα blocking agents in moderate-to-severe asthma were negative.16, 17 We also used etanercept to block the TNFα effects and could see a small reduction in inflammatory cell influx when high doses of etanercept were used in the OVA/CFA model, similarly to the recent report of Manni et al.,30 in which an anti-TNF antibody reduced Th17-mediated inflammation.31 However, smaller doses did not significantly affect immune cell influx in our study. Previous studies on TNFR1/2 KO mice immunized with OVA/Alum showed conflicting results on the contribution of TNFα to the development of allergic inflammation.32, 33 The production of other cytokines that are associated with allergic disease might compensate for the loss of TNFα bioactivity. However, these studies never analyzed the effect of TNFα antagonism on GC responsiveness. Interestingly, in the GC-insensitive OVA/CFA-induced model of airway hyperinflammation we showed that inhibition of the TNFα effect can restore GC sensitivity at different levels, including immune cell influx, cytokine and chemokine production, goblet cell metaplasia, and AHR. Note that the effects of etanercept were not caused by potential antibody-related immune suppression, because similar results were obtained with the (C57BL/6 × TNFR1 KO) F1 mice.
Several cytokines, such as IL17, which have been associated with severe asthma,34 were upregulated in our GC-insensitive OVA/CFA-based model relative to the GC-sensitive model. The increased IL17 levels in the OVA/CFA mice indicate the presence of Th17 cells in this model. As it was postulated that TNFα leads to a neutrophil-rich environment via the induction of Th17 cells,35, 36 TNFα might induce this GC-insensitive neutrophil-mediated hyperinflammation in the OVA/CFA model via IL17 induction. The contribution of IL17 to the neutrophilic inflammation might occur through upregulation of neutrophil chemoattractants, such as keratinocytes. The production of the latter chemokines was also increased in our GC-insensitive model, which correlates with their enhancement in severe GC-resistant asthmatics.29, 37, 38 Furthermore, the higher presence of IL12(p40) in OVA/CFA mice compared with OVA/Alum mice further confirmed the Th1 component in the OVA/CFA model. TNFα has also been shown to induce MMP9 synthesis.39 Interestingly, BAL neutrophils are a source of increased MMP9, which has been correlated with asthma severity.40 This is consistent with our observation of higher MMP9 levels in the OVA/CFA model compared with the OVA/Alum model. The levels of all these inflammatory mediators, which are associated with severe asthma, were reduced by treatment of mice with a combination of etanercept and Dex.
Many cell types produce TNFα, but T lymphocytes, macrophages, inflammatory DCs mast cells, neutrophils, eosinophils, and epithelial cells are especially relevant to asthma. However, more work is required to determine the main source of TNFα in the airways of patients with refractory asthma and in OVA/CFA-treated mice. Moreover, TNFR1 is expressed not only on various immune cells, such as macrophages, DCs, T lymphocytes, mast cells, and eosinophils, but also on structural cells, such as fibroblasts and epithelial cells. To identify the cell compartment in which TNFR1 is necessary for induction of TNFα-mediated GC insensitivity, bone marrow chimeric mice were subjected to OVA/CFA-induced hyperinflammation. In vitro studies have already shown that cytokines such as TNFα can induce GC insensitivity in immune cells, as well as in structural airway cells such as airway smooth muscle cells41 and airway epithelial cells.42 We found that in the OVA/CFA model TNFα blocks the GC-mediated effects in the radioresistant cells, not in the hematopoietic cells. It has become increasingly accepted that a substantial part of the efficacy of GC treatments originates from their actions in structural cell types, such as airway epithelial cells and smooth muscle cells. In addition, the epithelium has a pivotal role in the development of asthma.9 By studying the effect of TNFα on the different GR actions in vitro, we found that pretreatment with TNFα specifically impairs the GR dimer-dependent actions, i.e., induction of GRE-dependent genes such as Gilz and repression of nGRE dependent genes. It was previously suggested that reduced GR dimer-mediated transcriptional activity of GR is correlated to GC insensitivity in asthma patients.22 In addition, it was suggested that in A549 lung epithelial cells TNFα might induce GC insensitivity by impairing the transactivation actions of GR.42 Similarly, a recent report showed that respiratory syncytial virus blocks GR actions by impairing GR-mediated transcriptional induction.43 Interestingly, Gilz deficiency has been shown to lead to increased IL17/Th17 activation.44 However, this mechanism might not be involved in our GC-insensitive OVA/CFA-based model, because Dex could still induce Gilz expression in the lungs of OVA/CFA-treated mice.
The GC insensitivity in the OVA/CFA-based model seemed to occur at the level of GC-mediated repression of Tslp. It was reported that GCs repress the transcription of Tslp through direct binding of GR dimers to nGRE elements.2 TSLP is released from airway epithelial cells and has been correlated mainly withTh2 cellular immunity and allergic inflammation.45 As TSLP levels have been reported to correlate with disease severity,23 it has become a prime target for intervention in allergic diseases.46 Indeed, TSLP-deficient mice showed reduced influx of immune cells in the BAL fluids when immunized with OVA/Alum, compared with control mice. However, OVA/CFA-treated TSLP KO mice were more susceptible to OVA/CFA-induced airway inflammation than control C57BL/6 mice. This suggests that therapeutic targeting of TSLP, which is currently being studied in clinical trials,47 might not benefit all asthma patients and that patients should be stratified to ensure optimal therapy. It has been reported that TSLP can reduce IL17 during airway inflammation,48 which might explain the detrimental effects of the absence of TSLP during the OVA/CFA-induced pulmonary inflammation, in which IL17 has an important role. However, no increased IL17A levels were observed in the TSLP KO mice compared with the WT mice after OVA/CFA treatment. In addition to its Th2-promoting activity, TSLP also has a capacity to suppress Th1 immunity.49 In this way, the absence of TSLP can lead to increased immune responses in the Th1-mediated OVA/CFA model. Consistently, TNF and interferon γ levels were increased in the PBS-treated TSLP KO mice compared with the WT mice in the OVA/CFA group. This suggests that the enhanced immune responses observed in the OVA/CFA-treated TSLP KO mice might be due to reduced repression of Th1-driven immunity by TSLP. In addition, except for the total immune cell influx, inflammation could be reduced by Dex when TNF was neutralized by administration of etanercept. This implies no major role for TSLP in the TNF-induced GC insensitivity.
The heterogeneous nature of asthma requires adaptation of therapy to its different endotypes, and subtype biomarkers would be needed for that. Whereas sputum periostin is able to identify patients responsive to steroids,50 we believe that sputum TNFα levels might be a useful marker for determining refractoriness to steroid therapy. Nevertheless, TNFα is only one of the many cytokines implicated in severe asthma, and some have already been targeted in clinical studies, though often with disappointing results. Because of the great redundancy between cytokines, we believe that selective cytokine blockers might not be useful for therapeutic management of severe asthma. However, we provide data indicating that blocking TNFα might revert the GC insensitivity and thereby restore the broad attenuating effects of GCs on airway inflammation and remodeling (Figure 8). In this way, a combination therapy of TNFα antagonists and GCs might be considered for GC refractory patients. It is, however, important to note that the use of TNF blockers is often associated with adverse side effects, such as serious infections (including reactivation of tuberculosis), malignancy, congestive heart failure, and autoimmune diseases.51, 52 Moreover, the use of TNFα blockers might allow lower doses of Dex, which might reduce the adverse side effects, associated with GC therapy. Moreover, TNFα blockers and GCs might have some synergistic effects, as described in a recent report by the group of Yuksel.53 Similarly, combined therapy with TNFα antagonists and GCs has already increased therapeutic efficacy in rheumatoid arthritis54 and spinal cord trauma.55 Currently, TNFα is a major therapeutic target in a range of chronic inflammatory disorders involving neutrophils, including rheumatoid arthritis, psoriasis, and Crohn’s disease, all of which are also associated with GC resistance.56 So, it is conceivable that TNFα is also involved in the occurrence of GC resistance in other inflammatory diseases. Thus, by inhibiting the processes that interfere with the beneficial anti-inflammatory actions of GR, it might be possible to restore GC function.
Concluding scheme of the effects of tumor necrosis factor α (TNFα) on the actions of glucocorticoid (GC) receptor (GR) during severe asthma. (a) Asthma is an inflammatory disease of the airways leading to airway hyperresponsiveness, bronchial obstruction, mucus hyperproduction, and airway wall remodeling. (b) It is classically recognized as the typical Th2 disease, with an eosinophilic inflammation in the airway, and patients are effectively treated with GCs. However, this relatively simple paradigm has been doubted because a small percentage of asthma patients do not respond well to GC treatment. Patients who are refractory to the beneficial effects of GCs display a different inflammatory environment. This indicates that different phenotypes of asthma exist. To study the molecular mechanism involved in GC refractory asthma, we used two different ovalbumin (OVA)-based mouse models of airway hyperinflammation. The first is GC sensitive and eosinophil driven, whereas the second represents GC-insensitive, neutrophil-predominant asthma subphenotypes. In contrast to the Th2-dominated phenotype provoked by alum, OVA/complete Freund’s adjuvant (CFA)-based sensitization, followed by allergen challenge, elicited a pulmonary inflammation that was poorly controlled by dexamethasone. By testing different parameters, such as bronchial hyperreactivity, cytokine synthesis, immune cell recruitment, and mucus secretion, we showed that blocking TNFα with etanercept restores the beneficial effects of GCs in the GC-insensitive model. Thus, during severe neutrophil-mediated asthma, TNFα results in a state of GC insensitivity, predominantly in the non-hematopoietic cell compartment. (c) Thus neutralizing TNFα might offer a new therapeutic strategy to restore GC sensitivity in severe refractory asthma patients. GM-CSF, granulocyte-macrophages colony-stimulating factor; IL, interleukin; KC, keratinocyte; MMP, matrix metalloproteinase; TSLP, thymic stromal lymphopoietin.
METHODS
Mice. Female C57BL/6 WT mice, 6–8 weeks old were obtained from Janvier (Le Genest St-Isle, France). TSLP KO mice were provided by Dr Michael Comeau (Amgen, Thousand Oaks, CA). TNFR1 KO mice, generated by M Rothe,57 were a gift of H Bleuthmann (Hoffmann-La Roche, Basel, Switzerland). TNFR1 KO mice were crossed to C57BL/6 mice to generate F1 mice, which, in contrast to TNFR1 KO mice, can generate an antibody response to allergens.21 Mice were housed in specific pathogen-free conditions in individually ventilated cages in a controlled day–night cycle and given food and water ad libitum. All experiments were approved by the animal ethics committee of Ghent University (ethical committee number 2013-029), in accordance with European guidelines (directive 2010/63/EU; Belgian Royal Decree of 6 April 2010).
Mouse models of AHR. For the GC-sensitive OVA/Alum model, mice were sensitized to the experimental surrogate allergen ovalbumin (OVA, Sigma-Aldrich, St Louis, MO) by intraperitoneal injection of 20 μg OVA adsorbed on 1 mg of the adjuvant Alum in endotoxin-free PBS on days 0, 7, and 14. For the GC-insensitive OVA/CFA model, mice were immunized subcutaneously on day 0 with 20 μg of grade V chicken egg OVA in PBS, emulsified in 75 μl CFA (Sigma-Aldrich). On days 21 and 22, all mice were exposed to aerosols consisting of 0.1 or 1% OVA grade III. All injections were given intraperitoneally in 200 μl PBS 3 h before the aerosols (Figure 1a). Mice received 1 mg kg−1 Dex (Sigma, St. Louis, MO) and/or 200 μg (10 mg kg−1) etanercept (Pfizer, New York, NY). In some experiments, mice were treated with 200 μg of a monoclonal antibody against mouse TNFR1 (clone 55R-286, BD Pharmingen, San Diego, CA). These reagents were freshly dissolved before administration. Immunized but unchallenged mice were included in some experiments. All mice were killed for analysis 24 h after the last OVA injection. Mice were anesthetized with intraperitoneal injections of 150 μl of ketamine/xylazine solution, and then blood was collected with a glass capillary from the retro-orbital plexus and allowed to clot overnight at 4 °C. After blood collection, BAL was performed four times with 1 ml Hank’s balanced salt solution (Invitrogen, Carlsbad, CA) supplemented with 10 mM EDTA. After BAL, lungs were removed and stored in 4% paraformaldehyde (right lung) or kept in RNA later (left lung).
Measurement of total and differential cell counts in BAL fluids. Flow cytometric analyses were performed on an LSR-II flow cytometer (BD Biosciences, Erembodegem, Belgium). The BAL cell composition of individual mice was determined by analysis of surface expression of CD3, CD4, CD8, CD11c, MHCII, CD11b, and CCR3. The gating strategy was according to the publication of Bogaert et al.18 All antibodies were purchased from eBiosciences (San Diego, CA) or BD Pharmingen, except CCR3 (R&D Systems, Abingdon, UK). Cells were labeled at 4 °C in the presence of anti-CD16/CD32 to block non-specific binding. In addition, BAL cells were also loaded on a glass slide by cytospin method, after which these were dried overnight and fixed with cold methanol. Cells were subsequently stained with May-Grünwald/Giemsa staining (Sigma).
Determination of cytokine and chemokine levels. Total RNA was prepared with the RNeasy Mini Kit (Qiagen, Hilden, Germany) from the lungs or A549 cells kept in RNA later (Qiagen) or TRIzol (Invitrogen), respectively. RNA concentration was measured with the Nanodrop 1000 (Thermo Scientific, Waltham, MA), and complementary DNA was prepared with Superscript II (Invitrogen). Quantitative PCR was performed with the Roche LightCycler 480 system (Applied Biosystems, Lincoln, NE). Data were normalized for the expression levels of housekeeping genes, and amplification specificity was confirmed by evaluation of the melting curves.
Levels of secreted inflammatory mediators were measured in the first 0.5-ml fraction of the collected BAL fluid. Cytokines and chemokines were measured using the Luminex Bioplex suspension array system (Bio-Rad, Hercules, CA) according to the manufacturer’s instructions. IL6 levels in the supernatants of stimulated A549 cells were determined with a 7TD1 bioassay. TNFα was measured by a cytotoxicity assay on WEHI 164 clone 13 cells.
Histological analysis. Lung tissues were fixed and paraffin embedded. Sections of 6 μm were cut, mounted on superfrost glass slides (Fischer Scientific, Hampton, VA), and stained with periodic acid-Schiff (Sigma-Aldrich). The extent of mucus production was quantified using the five-point grading system described by Tanaka et al.58 Sections were also stained for the general hematopoietic immune cell marker CD45. Therefore sections were deparaffinized, blocked with serum, and incubated with an anti-CD45 antibody (BD Biosciences). Visualization was done with the Vectastain ABC Kit (Vector Laboratories, Burlingame, CA) and counterstaining with hematoxylin solution (Sigma-Aldrich). CD45-positive cells were counted in five random × 40 fields in a double-blinded fashion. Negative controls were made by substituting buffer for primary antibody.
Determination of airway responsiveness. Lung function was assessed using Flexivent invasive measurement of dynamic resistance as described previously.59 Briefly, airway responsiveness to increasing concentrations of MCh (Sigma Chemicals, St. Louis, MO) was recorded using Flexivent (Scireq, Montreal, Quebec, Canada). MCh is a non-specific spasmogenic stimulus that triggers enhanced responsiveness and constriction of the airways. Mice were anesthetized (intraperitoneal) with three subsequent (10’ in between) injections of 1 mg kg−1 urethane (Sigma), followed by an single injection of curare (Sigma) just before they were placed on the ventilator. Next, an 18-gauge needle was inserted into the trachea. Mice were connected to a computer-controlled small animal ventilator and quasi-sinusoidally ventilated with a tidal volume of 10 ml kg−1 at a frequency of 150 breaths min−1 and a positive end-expiratory pressure of 2 cm H2O to achieve a mean lung volume close to spontaneous breathing. After baseline measurement, mice were challenged for 10 s with saline aerosol and, at 4.5-min intervals, with MCh at increasing concentrations (6.25–200 mg ml−1). For each MCh dose, the peak response was calculated as the mean of the three maximal values and used for calculation of airway dynamic compliance, expressed as ml cm−1 H2O.
Generation of bone chimeras. Female C57BL/6 mice, 8−10-weeks old, were sublethally irradiated (8 Gy) and received intravenously 2 × 106 bone marrow cells from C57BL/6 or TNFR1 KO donors 6 h after irradiation. Afterwards, mice received 20 μg ml−1 of the antibiotic Baytril (Medini NV, Oostkamp, België) in the drinking water for 4 consecutive weeks. Mice were used in experiments not earlier than 10 weeks after bone marrow reconstitution. Success of reconstitution was controlled by PCR for TNFR1 presence in white blood cells.
Cell culture: stimulations and transfections. Airway epithelial A549 cells were cultured in Dulbecco’s modified Eagle’s medium (Invitrogen) supplemented with 10% fetal calf serum, 100 units ml−1 penicillin/streptomycin, 2 mM L-glutamine, and 1 mM sodium pyruvate. Cells were counted by trypan blue exclusion and plated on six-well plates at 1 × 106 cells per well, and 1 μm Dex (Sigma-Aldrich) and/or 1000 U ml−1 TNFα was added, for 5 and 6 h, respectively. Recombinant human TNFα was expressed in Escherichia coli and purified in our laboratory. TNFα had a specific activity of 1.0 × 109 IU mg−1. Endotoxin levels were below the detection limit. After stimulation, supernatant was collected and cells were lysed with TRIzol (Invitrogen) for RNA isolation. Plasmids GRE-Luc and nGRE-Luc were kindly provided by Professor K De Bosscher (VIB, UGent, Belgium) and Professor E Ortlund (Emory University School of Medicine, Atlanta, GA), respectively. Transfection was done using X-tremeGENE HP DNA Transfection Reagent (Roche Diagnostics) in 24-well plates. After 24 h, cells were treated with 1 μm Dex and/or 1000 U ml−1 TNFα. Note that this dose within this time frame did not lead to cytocidal effects. Luciferase activity, expressed in arbitrary light units, was measured with a Dual-Luciferase Reporter Assay Kit (Promega, Madison, WI) following the technical manual.
Statistical information. Statistical significance was inferred from Student’s t-test and one-way or two-way analysis of variance, carried out with GraphPad Prism (San Diego, CA). Data are expressed as mean±s.d. Single, double and triple asterisks (*, **, and ***) represent P<0.05, P<0.01, and P<0.001, respectively.
References
Vandevyver, S., Dejager, L., Tuckermann, J. & Libert, C. New insights into the anti-inflammatory mechanisms of glucocorticoids: an emerging role for glucocorticoid-receptor-mediated transactivation. Endocrinology 154, 993–1007 (2013).
Surjit, M. et al. Widespread negative response elements mediate direct repression by agonist-liganded glucocorticoid receptor. Cell 145, 224–241 (2011).
Dockrell, M., Partridge, M.R. & Valovirta, E. The limitations of severe asthma: the results of a European survey. Allergy 62, 134–141 (2007).
Holgate, S.T. & Polosa, R. The mechanisms, diagnosis, and management of severe asthma in adults. Lancet 368, 780–793 (2006).
Chanez, P. et al. Severe asthma in adults: what are the important questions? J. Allergy Clin. Immunol. 119, 1337–1348 (2007).
Barnes, P.J. New therapies for asthma: is there any progress? Trends Pharmacol. Sci. 31, 335–343 (2010).
Anderson, G.P. Endotyping asthma: new insights into key pathogenic mechanisms in a complex, heterogeneous disease. Lancet 372, 1107–1119 (2008).
Wenzel, S.E. Asthma phenotypes: the evolution from clinical to molecular approaches. Nat. Med. 18, 716–725 (2012).
Lambrecht, B.N. & Hammad, H. The airway epithelium in asthma. Nat. Med. 18, 684–692 (2012).
Hallstrand, T.S., Woodruff, P.G., Holgate, S.T. & Knight, D.A. Function of the airway epithelium in asthma. J. Allergy 2012, 160586 (2012).
Ordonez, C.L., Shaughnessy, T.E., Matthay, M.A. & Fahy, J.V. Increased neutrophil numbers and IL-8 levels in airway secretions in acute severe asthma: clinical and biologic significance. Am. J. Respir. Crit. Care Med. 161, 1185–1190 (2000).
Schuijs, M.J., Willart, M.A., Hammad, H. & Lambrecht, B.N. Cytokine targets in airway inflammation. Curr. Opin. Pharmacol. 13, 351–361 (2013).
Lukacs, N.W., Strieter, R.M., Chensue, S.W., Widmer, M. & Kunkel, S.L. Tnf-alpha mediates recruitment of neutrophils and eosinophils during airway inflammation. J. Immunol. 154, 5411–5417 (1995).
Howarth, P.H. et al. Tumour necrosis factor (TNF alpha) as a novel therapeutic target in symptomatic corticosteroid dependent asthma. Thorax 60, 1012–1018 (2005).
Berry, M.A. et al. Evidence of a role of tumor necrosis factor alpha in refractory asthma. N. Engl. J. Med. 354, 697–708 (2006).
Wenzel, S.E. et al. A randomized, double-blind, placebo-controlled study of tumor necrosis factor-alpha blockade in severe persistent asthma. Am. J Respir. Crit. Care Med. 179, 549–558 (2009).
Holgate, S.T. et al. Efficacy and safety of etanercept in moderate-to-severe asthma: a randomised, controlled trial. Eur. Respirat. J. 37, 1352–1359 (2011).
Bogaert, P. et al. Inflammatory signatures for eosinophilic vs. neutrophilic allergic pulmonary inflammation reveal critical regulatory checkpoints. Am. J. Physiol. Lung Cell. Mol. Physiol 300, L679–L690 (2011).
Busse, W.W., Banks-Schlegel, S. & Wenzel, S.E. Pathophysiology of severe asthma. J. Allergy Clin. Immunol. 106, 1033–1042 (2000).
Ming, W.J., Bersani, L. & Mantovani, A. Tumor necrosis factor is chemotactic for monocytes and polymorphonuclear leukocytes. J. Immunol. 138, 1469–1474 (1987).
Van Hauwermeiren, F. et al. Safe TNF-based antitumor therapy following p55TNFR reduction in intestinal epithelium. J. Clin. Invest. 123, 2590–2603 (2013).
Matthews, J.G., Ito, K., Barnes, P.J. & Adcock, I.M. Defective glucocorticoid receptor nuclear translocation and altered histone acetylation patterns in glucocorticoid-resistant patients. J. Allergy Clin. Immunol. 113, 1100–1108 (2004).
Zhou, B.H. et al. Thymic stromal lymphopoietin as a key initiator of allergic airway inflammation in mice. Nat. Immunol. 6, 1047–1053 (2005).
Kabata, H. et al. Thymic stromal lymphopoietin induces corticosteroid resistance in natural helper cells during airway inflammation. Nat. Commun. 4, 2675 (2013).
Hansbro, P.M., Kaiko, G.E. & Foster, P.S. Cytokine/anti-cytokine therapy - novel treatments for asthma? Br. J. Pharmacol. 163, 81–95 (2011).
Bogaert, P., Tournoy, K.G., Naessens, T. & Grooten, J. Where asthma and hypersensitivity pneumonitis meet and differ: noneosinophilic severe asthma. Am. J. Pathol. 174, 3–13 (2009).
Thomas, P.S., Yates, D.H. & Barnes, P.J. Tumor-necrosis-factor-alpha increases airway responsiveness and sputum neutrophilia in normal human-subjects. Am. J. Respir. Crit. Care Med. 152, 76–80 (1995).
Wershil, B.K., Wang, Z.S., Gordon, J.R. & Galli, S.J. Recruitment of neutrophils during ige-dependent cutaneous late phase reactions in the mouse is mast cell-dependent - partial inhibition of the reaction with antiserum against tumor-necrosis-factor-alpha. J. Clin. Investig. 87, 446–453 (1991).
Ito, K. et al. Steroid-resistant neutrophilic inflammation in a mouse model of an acute exacerbation of asthma. Am. J. Respir. Cell Mol. Biol. 39, 543–550 (2008).
Manni, M.L. et al. The complex relationship between inflammation and lung function in severe asthma. Mucosal immunology 7, 1186–1198 (2007).
Choi, K.J., Zhang, S.N., Choi, I.K., Kim, J.S. & Yun, C.O. Strengthening of antitumor immune memory and prevention of thymic atrophy mediated by adenovirus expressing IL-12 and GM-CSF. Gene Therapy 19, 711–723 (2012).
Rudmann, D.G. et al. Modulation of allergic inflammation in mice deficient in TNF receptors. Am. J. Physiol. Lung Cell. Mol. Physiol. 279, L1047–L1057 (2000).
Cho, J.Y., Pham, A., Rosenthal, P., Miller, M., Doherty, T. & Broide, D.H. Chronic OVA allergen challenged TNF p55/p75 receptor deficient mice have reduced airway remodeling. Int. Immunopharmacol. 11, 1038–1044 (2011).
Agache, I., Ciobanu, C., Agache, C. & Anghel, M. Increased serum IL-17 is an independent risk factor for severe asthma. Respir. Med. 104, 1131–1137 (2010).
Nakae, S., Suto, H., Berry, G.J. & Galli, S.J. Mast cell-derived TNF can promote Th17 cell-dependent neutrophil recruitment in ovalbumin-challenged OTII mice. Blood 109, 3640–3648 (2007).
McKinley, L. et al. T(H)17 cells mediate steroid-resistant airway inflammation and airway hyperresponsiveness in mice. J. Immunol. 181, 4089–4097 (2008).
Fahy, J.V., Kim, K.W., Liu, J. & Boushey, H.A. Prominent neutrophilic inflammation in sputum from subjects with asthma exacerbation. J. Allergy Clin. Immunol. 95, 843–852 (1995).
Saha, S. et al. Granulocyte-macrophage colony-stimulating factor expression in induced sputum and bronchial mucosa in asthma and COPD. Thorax 64, 671–676 (2009).
Hardyman, M.A. et al. TNF-alpha-mediated bronchial barrier disruption and regulation by src-family kinase activation. J. Allergy Clin. Immunol. 132, 665–675 (2013).
Cundall, M., Sun, Y.C., Miranda, C., Trudeau, J.B., Barnes, S. & Wenzel, S.E. Neutrophil-derived matrix metalloproteinase-9 is increased in severe asthma and poorly inhibited by glucortcoids. J. Allergy Clin. Immunol. 112, 1064–1071 (2003).
Tliba, O. et al. Cytokines induce an early steroid resistance in airway smooth muscle cells. Am. J. Respir. Cell Mol. Biol. 38, 463–472 (2008).
Rider, C.F., King, E.M., Holden, N.S., Giembycz, M.A. & Newton, R. Inflammatory stimuli inhibit glucocorticoid-dependent transactivation in human pulmonary epithelial cells: rescue by long-acting beta(2)-adrenoceptor agonists. J. Pharmacol. Exp. Ther. 338, 860–869 (2011).
Marketon, J.I.W. & Corry, J. Poly I:C and respiratory syncytial virus (RSV) inhibit glucocorticoid receptor (GR)-mediated transactivation in lung epithelial, but not monocytic; cell lines. Virus Res. 176, 303–306 (2013).
Ngo, D. et al. Glucocorticoid-induced leucine zipper (GILZ) regulates testicular FOXO1 activity and spermatogonial stem cell (SSC) function. PLoS One 8 (2013).
Ying, S. et al. Thymic stromal lymphopoietin expression is increased in asthmatic airways and correlates with expression of TH2-attracting chemokines and disease severity. J. Immunol. 174, 8183–8190 (2005).
Wang, W.L. et al. Thymic stromal lymphopoietin: a promising therapeutic target for allergic diseases. Int Arch. Allergy Immunol. 160, 18–26 (2013).
Zhang, F., Huang, G., Hu, B., Song, Y. & Shi, Y. A soluble thymic stromal lymphopoietin (TSLP) antagonist, TSLPR-immunoglobulin, reduces the severity of allergic disease by regulating pulmonary dendritic cells. Clin. Exp. Immunol. 164, 256–264 (2011).
Togbe, D. et al. Thymic stromal lymphopoietin enhances Th2/Th22 and reduces IL-17A in protease-allergen-induced airways inflammation. ISRN Allergy 2013, 971036 (2013).
Willart, M.A. et al. Interleukin-1alpha controls allergic sensitization to inhaled house dust mite via the epithelial release of GM-CSF and IL-33. J. Exp. Med. 209, 1505–1517 (2012).
Peters, M.C., Mekonnen, Z.K., Yuan, S., Bhakta, N.R., Woodruff, P.G. & Fahy, J.V. Measures of gene expression in sputum cells can identify TH2-high and TH2-low subtypes of asthma. J. Allergy Clin. Immunol. 133, e5 (2014).
Li, D.Q. et al. Short ragweed pollen triggers allergic inflammation through Toll-like receptor 4-dependent thymic stromal lymphopoietin/OX40 ligand/OX40 signaling pathways. J. Allergy Clin. Immunol. 128, e2 (2011).
Chen, L., Chen, X., Zhang, H., Feng, L. & Zhu, R. Carcinoma of the thyroid gland showing thymic-like elements: hypofunctioning nodule accumulating (99 m)Tc-MIBI and (18)F-FDG. Hellenic J. Nuclear Med. 14, 190–191 (2011).
Yilmaz, O. et al. Comparison of TNF antagonism by etanercept and dexamethasone on airway epithelium and remodeling in an experimental model of asthma. Int. Immunopharmacol. 17, 768–773 (2013).
Naumann, L., Huscher, D., Detert, J., Spengler, M., Burmester, G.R. & Buttgereit, F. Anti-tumour necrosis factor alpha therapy in patients with rheumatoid arthritis results in a significant and long-lasting decrease of concomitant glucocorticoid treatment. Ann. Rheum. Dis. 68, 1934–1936 (2009).
Genovese, T. et al. Combination of dexamethasone and etanercept reduces secondary damage in experimental spinal cord trauma. Neuroscience 150, 168–181 (2007).
Barnes, P.J. & Adcock, I.M. Glucocorticoid resistance in inflammatory diseases. Lancet 373, 1905–1917 (2009).
Rothe, J. et al. Mice lacking the tumour necrosis factor receptor 1 are resistant to TNF-mediated toxicity but highly susceptible to infection by Listeria monocytogenes. Nature 364, 798–802 (1993).
Tanaka, H. et al. The effect of allergen-induced airway inflammation on airway remodeling in a murine model of allergic asthma. Inflamm. Res. 50, 616–624 (2001).
Hammad, H. et al. Activation of the D prostanoid 1 receptor suppresses asthma by modulation of lung dendritic cell function and induction of regulatory T cells. J. Exp. Med. 204, 357–367 (2007).
Acknowledgements
We thank Joke Vanden Berghe and Wilma Burm for excellent technical assistance and Amin Bredan for editing the manuscript. The work was supported by grants from FWO (Fonds voor Wetenschappelijk Onderzoek, Belgium), IWT (Innovatie door Wetenschap en Technologie, Belgium), SBO (Strategisch Basis Onderzoek, IWT) and IUAP (Interuniversity Attraction Poles, Belgium). B.L. and H.H. are supported by a European FP7 IMI grant “EUBIOPRED”, and B.L. is supported by an ERC grant and a University of Ghent MRP grant “GROUP-ID”.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Rights and permissions
About this article
Cite this article
Dejager, L., Dendoncker, K., Eggermont, M. et al. Neutralizing TNFα restores glucocorticoid sensitivity in a mouse model of neutrophilic airway inflammation. Mucosal Immunol 8, 1212–1225 (2015). https://doi.org/10.1038/mi.2015.12
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2015.12
This article is cited by
-
Neutrophil activation and NETosis are the predominant drivers of airway inflammation in an OVA/CFA/LPS induced murine model
Respiratory Research (2022)
-
Different inhaled corticosteroid doses in triple therapy for chronic obstructive pulmonary disease: systematic review and Bayesian network meta-analysis
Scientific Reports (2022)
-
Beneficial effects of infrared light-emitting diode in corticosteroid-resistant asthma
Lasers in Medical Science (2022)
-
Blockade of protease-activated receptor 2 attenuates allergen-mediated acute lung inflammation and leukocyte recruitment in mice
Journal of Biosciences (2022)
-
New insights into the cell- and tissue-specificity of glucocorticoid actions
Cellular & Molecular Immunology (2021)