Abstract
Regulation of allergic responses by intestinal epithelial cells (IECs) remains poorly understood. Using a model of oral allergen sensitization in the presence of cholera toxin as adjuvant and mice with cell-specific deletion of inhibitor-κB kinase (IKKβ) in IECs (IKKβΔIEC), we addressed the contribution of IECs to allergic sensitization to ingested antigens and allergic manifestations at distant mucosal site of the airways. Cholera toxin induced higher pro-inflammatory responses and altered the profile of the gut microbiota in IKKβΔIEC mice. Antigen-specific immunoglobulin E (IgE) responses were unaltered in IKKβΔIEC mice, but their IgA antibodies (Abs), T helper type 1 (Th1) and Th17 responses were enhanced. Upon nasal antigen challenge, these mice developed lower levels of allergic lung inflammation, which correlated with higher levels of IgA Abs in the airways. The IKKβΔIEC mice also recruited a higher number of gut-sensitized T cells in the airways after nasal antigen challenge and developed airway hyper-responsiveness, which were suppressed by treatment with anti-interleukin-17A. Fecal microbiota transplant during allergic sensitization reduced Th17 responses in IKKβΔIEC mice, but did not affect IgA Ab responses. In summary, we show that IKKβ in IECs shapes the gut microbiota and immune responses to ingested antigens and influences allergic responses in the airways via regulation of IgA Ab responses.
Similar content being viewed by others
Introduction
Ingestion of food antigens generally fails to promote brisk immune responses but rather results in a state of immune tolerance. However, aberrant immune responses, including food allergy, can develop in individuals with a genetic predisposition. Clinical manifestations of food allergies include gastrointestinal, systemic (anaphylaxis), cutaneous (eczema), or respiratory (asthma) symptoms1, 2 and are generally regarded as pathological responses to food antigens mediated by excessive T helper type 2 (Th2) responses and antigen-specific immunoglobulin E (IgE) antibody (Ab) responses. Past research on allergy and asthma focused on the role of cells and molecules involved in adaptive immunity. More recently, epithelial cells lining the sites of antigen entry and innate immune responses have emerged as important players in these pathologies.1, 3, 4 Studies in animal models have demonstrated that oral sensitization to allergens primes for adverse inflammatory responses at distant sites of the airways or the skin.5, 6 However, little is known about the mechanism(s) employed by intestinal epithelial cells (IECs) to shape immune responses to allergens and influence allergic manifestations in distant mucosal sites, such as the airways.
The nuclear factor-κB (NF-κB) pathway has an important role in inflammatory responses.7 Its activation is regulated by the inhibitor-κB kinase (IKKβ), the catalytic subunit of the IKK complex responsible for NF-κB translocation and transcription.7 Previous studies have shown that the IKKβ-NF-κB signaling controls a number of biological processes via tissue-specific regulation of inflammatory and anti-inflammatory responses and can mediate both pro- and anti-inflammatory effects.8, 9 These opposite effects were attributed to the nature of immune cells where the IKKβ-NF-κB signaling was affected.10 However, both attenuation of chronic and exacerbation of acute gut inflammatory diseases were reported in mice with alteration of IKKβ-dependent NF-κB activation in IECs.11 Others have shown that inhibition of IKKβ-dependent NF-κB activation limits the production of Th2-inducing cytokine by IECs and, thus, impairs the development of protective immunity against the gut-dwelling parasite, Trichuris.12
The large intestine of mammals contains a huge community of commensal bacteria, which contributes to the digestive functions,13 prevent the development of inflammatory bowel diseases,14 and support the maturation of gut immune cells.15, 16 The gut microbiota can be perturbed by endogenous or exogenous factors and it is now established that microbial dysbiosis is associated with allergy,17, 18 obesity,19 and inflammatory diseases.20, 21 IECs sense changes in gut microbiota, and transplantation of healthy infant gut microbiota could protect mice from developing allergic responses to food antigens.17
Oral administration of food antigen with cholera toxin as adjuvant in experimental animals is a well-accepted model to study allergic sensitization to food antigens.5, 6, 22 To address the role of IECs in pathogenic immune responses to ingested food antigens, mice with targeted deletion of IKKβ in IECs (IKKβΔIEC)23 were orally sensitized to a food antigen in the presence of cholera toxin. We show that a localized impairment of IKKβ in IECs alters the gut microbiota during oral allergic sensitization and regulates the profile of allergic inflammatory responses at the distant airways through IgA Abs and Th17 responses.
Results
IKKβ deletion in IECs enhances gut inflammatory responses to the adjuvant cholera toxin
Sixteen hours after oral cholera toxin treatment, phospho-nuclear factor-κB (pNF-κB) expression was enhanced in IECs of C57BL/6 mice and primarily found in the nucleus. Cholera toxin also increased pNF-κB expression in IECs of IKKβΔIEC mice, but the localization was primarily cytoplasmic (Figure 1). Except for thymic stromal lymphopoietin (TSLP) mRNA levels that were lower in the IKKβΔIEC group, we found no difference between control and IKKβΔIEC mice before treatment. Cholera toxin elevated mRNA levels of the pro-inflammatory cytokines in both IKKβΔIEC mice and control C57BL/6 mice, but tumor necrosis factor-α (TNF-α) mRNA levels were increased by∼10-fold in IKKβΔIEC mice (Figure 1b). Cholera toxin also significantly increased transforming growth factor-β (TGF-β) mRNA levels in the gut of IKKβΔIEC mice (Figure 1b). At the time point examined, cholera toxin treatment did not change TSLP mRNA levels in the gut of control mice but raised TSLP mRNA levels in IKKβΔIEC mice (Figure 1b). The enhanced level of cytokine mRNA responses in the gut of IKKβΔIEC mice was associated with higher levels of pSTAT3 (phosphorylated signal transducer and activator of transcription factor 3) responses as determined by western blotting (Figure 1c) and immunohistochemistry (Supplementary Figure S1 online).
Innate responses to cholera toxin (CT) in intestinal tissues of IKKβΔIEC (deletion of inhibitor-κB kinase (IKKβ) in intestinal epithelial cells (IECs)) mice. Mice were orally administered cholera toxin (10 μg) by gavage, and small intestines were collected 4 or 16 h later. (a) Phospho-nuclear factor (pNF)-κB expression 16 h after administration of saline (phosphate-buffered saline (PBS)) or cholera toxin. Tissue sections were labeled with anti-pNF-κB p65 Ab and counter-stained with hematoxylin and eosin. Each image ( × 400) is representative of at least three independent experiments. Higher magnifications show pNF-κB p65 expression in the nucleus (N) and cytoplasma (C) of epithelial cells (b) Real-time reverse transcriptase–PCR analysis of cytokine mRNA. Data are expressed as mean relative expression levels±1 s.d. (c) Western blot analysis of phospho-signal transducer and activator of transcription factor 3 (pSTAT3) expression and quantification of relative pSTAT3 expression as mean densitometry units. Data are from four separate experiments (*P<0.05). IL, interleukin; TGF, transforming growth factor; TNF, tumor necrosis factor; TSLP, thymic stromal lymphopoietin.
Loss of IKKβ in IECs favors dysbiosis in cholera toxin–treated mice
Unlike controls, IKKβΔIEC mice showed no signs of intestinal fluid accumulation 16 h after treatment with cholera toxin (Supplementary Figure S2 online). Analysis of bacterial 16S rRNA genes in fecal pellets showed no significant difference between the ratios of Bacteroidetes and Firmicutes phyla in controls and IKKβΔIEC mice before cholera toxin treatment (Figure 2a and Supplementary Table S1). Four days after oral administration of cholera toxin, a dysbiosis affecting phyla (Figure 2a), class (Figure 2b), and species (Figure 2b) was observed in the fecal pellets of IKKβΔIEC mice (details in Supplementary Figures S3–S5 and Supplementary Tables S1–S6 online).
Cholera toxin alters the gut microbiota in IKKβΔIEC (deletion of inhibitor-κB kinase (IKKβ) in intestinal epithelial cells (IECs)) mice. Bacterial flora was analyzed in fecal pellets collected before (day 0) and 2 and 4 days after administration of cholera toxin. (a) Ratio of main bacteria Phyla, (b) percentage of main bacteria genus, (c) pie diagrams of the 15–17 main bacteria species. The results in b are expressed as mean percentage±1 s.d. (*P<0.05; **P<0.01). All results were from 3–4 mice per groups.
Loss of IKKβ in IECs alters antigen-specific CD4+ T-cell and Ab responses to oral sensitization
Segmented filamentous bacteria (SFB) are noncultivable commensal Gram-positive anaerobic bacteria that share strong 16S rRNA similarities with the genus Clostridium24, 25, 26 and regulate Th cytokine responses.27, 28 Four days after oral administration of cholera toxin, the percentage of SFB was slightly increased in controls but was significantly elevated in IKKβΔIEC mice (Figure 3a).
Inhibitor-κB kinase (IKKβ)-deficiency in intestinal epithelial cells (IECs) alters the profile of antigen-specific CD4+ T cell and serum antibody (Ab) responses in orally sensitized mice. (a) Percentage of segmented filamentous bacteria (SFB) homolog before (day 0) and 4 days after administration of cholera toxin. (b) Cytokine secretion by ovalbumin (OVA)-specific mesenteric lymph node (MLN) and spleen T cells were analyzed by enzyme-linked immunosorbent assay (ELISA). Results are expressed as mean±s.d. of three separate experiments, with four mice per group. (*P<0.05; **P<0.01 compared with control C57BL/6 mice). (c) OVA-specific immunoglobulin G (IgG) subclass and (d) IgE and IgA isotypes. Blood was collected on day 14, and Ab titers were analyzed by ELISA. The results are expressed as the log2 titers±1 s.d. and are from three experiments and five mice/group. (*P<0.05 compared with control C57BL/6 mice). IFN, interferon; IL, interleukin.
We next examined whether innate cytokine responses and dysbiosis in the gut of IKKβΔIEC mice were associated with changes in allergen-specific Th cytokine and Ab responses. Mesenteric lymph node (MLN) and spleen T cells from control and IKKβΔIEC mice secreted the same level of interleukin (IL)-4 after in vitro restimulation with ovalbumin (OVA; data not shown). On the other hand, IL-5 and IL-10 secretion by cells from IKKβΔIEC mice were significantly decreased (Figure 3b), while IL-17 and interferon (IFN)-γ responses were both enhanced (Figure 3b). Th1-associated IgG2a (IgG2c) responses were significantly enhanced in IKKβΔIEC, whereas IgE and IgG1 Ab responses were unchanged (Figure 3c). In addition, IKKβΔIEC mice developed higher OVA-specific IgA Ab responses than control C57BL/6 mice.
To clarify whether the changes in cytokine and Ab levels were the result of a changed microbiome or were a consequence of the lack of IKKβ in epithelial cells, microbiome swap was performed by fecal microbiome transplant 4 days after each oral sensitization (Figure 4a). The fecal microbiome swap affected antigen-specific T-cell cytokine responses by MLN cells as it reduced IL-17A responses of IKKβIEC when compared with wild-type mice and eliminated the difference between the levels of IL-5 and IL-10 responses between these mice (Figure 4b). Interestingly, IKKβΔIEC mice recipient of fecal microbiome transplant from orally sensitized wild-type mice retained higher levels of serum IgA responses (Figure 4c). These results suggest that intestinal dysbiosis in IKKβΔIEC mice alters antigen-specific CD4+ T-cell responses while IKKβ in IECs primarily regulates IgA Ab levels.
Fecal microbiota transfer (FMT) modulates antigen-specific CD4+ T-cell cytokines, but not serum immunoglobulin A (IgA) responses orally sensitized IKKβΔIECmice. (a) Schedule of oral sensitization (OS) and FMT. (b) Cytokine secretion by ovalbumin (OVA)-specific mesenteric lymph node (MLN) T cells were analyzed by enzyme-linked immunosorbent assay (ELISA). (c) OVA-specific IgG subclass and IgA responses. Blood was collected on day 14, and antibody (Ab) titers were analyzed by ELISA. The results are expressed as the log2 titers±1 s.d. and are from three experiments and five mice/ group. (*P<0.05 compared with control C57BL/6 mice). IFN, interferon; IL, interleukin.
To further establish how local (gut) vs. systemic (circulating myeloid cells) alteration of IKKβ affected allergen-specific Ab responses, we analyzed these responses in mice lacking IKKβ in myeloid cells (IKKβΔMye) throughout the body.8 These mice showed higher pSTAT3 responses in the small intestine than C57BL/6 mice 16 h after oral administration of cholera toxin and developed higher levels of antigen-specific Th1-associated IgG2a (IgG2c) responses (Supplementary Figure S6 online). The OVA-specific IgE and IgG1 Ab responses were unchanged in IKKβΔMye mice, whereas IgA responses were enhanced, although not to the same extent as in IKKβΔIEC mice (Supplementary Figure S6 online). Thus, IKKβ signaling in either epithelial cells or circulating myeloid cells regulates Ab responses to ingested allergens.
Alteration of IKKβ signaling in IECs limits allergic inflammation in the airways
Allergic inflammation can develop in the airways following nasal allergen challenge of mice sensitized by the oral route.5, 6 Other reports have indicated that intestinal microbes influence susceptibility to food allergy29 and regulate immunity to respiratory influenza virus infection.30 Lung inflammation was not seen in naive (non-sensitized and not challenged), or challenged but not sensitized C57BL/6, IKKβΔMye and IKKβΔIEC mice. Orally sensitized control C57BL/6 mice developed lung inflammation with cell recruitment in the lung parenchyma and the perialveolar and perivascular space after nasal antigen challenge (Figure 5a). Interestingly, lung inflammation was significantly reduced in IKKβΔIEC mice (Figure 5a) and in IKKβΔMye mice (Figure 5a). Only minimal mucus formation was seen in the lungs of IKKβΔIEC mice after antigen challenge and none in the lungs of IKKβΔMye mice (Figure 5c). In contrast to C57B/6 mice or IKKβΔMye mice, bronchoalveolar lavage (BAL) of IKKβΔIEC mice contained higher levels of IgA (Figure 5d), and their lungs showed more IgA-secreting cells (Supplementary Figure S7 online). IgA Abs are believed to suppress allergic inflammation.31 The presence of IgA in BAL of IKKβΔIEC mice was associated with a reduction of eosinophils and macrophages, but the number of neutrophils was increased (Figure 5e). On the other hand, other mechanisms are likely involved in the protection of IKKβΔMye mice, which exhibited overall lower number of cells in the lung after allergen challenges. In this regard, the proportion of F4/80+CD11c+ alveolar macrophages after nasal challenge was reduced in IKKβΔIEC when compared with control C57BL/6 mice (20±2.2% vs. 28±2.5%) (Supplementary Figure S8A online). Nasal challenge of orally sensitized control C57BL/6 mice recruited CD11c+F4/80−CD103+ cells in the lungs, an effect significantly reduced in mice with impaired IKKβ (Supplementary Figure S8B online). We also found a higher frequency of CD3+ T cells in the lungs of IKKβΔIEC mice than in control C57BL/6 or IKKβΔMye mice after nasal challenge of orally sensitized mice (Supplementary Figure S8C online).
Inhibitor-κB kinase (IKKβ)-deficiency in intestinal epithelial cells (IECs) limits lung allergic inflammation in orally sensitized mice. (a) Hematoxylin and eosin staining of lung sections ( × 40). (b) Inflammation scores in the lungs of C57BL/6 and IKKβΔIEC mice. (c) Tissues were stained with periodic acid-Schiff and counterstained with hematoxylin and eosin to visualize mucus ( × 400). Each picture in a and c is representative of three separate experiments, with 3–4 mice per group. (d) Total and ovalbumin (OVA)-specific immunoglobulin A (IgA) antibody levels, and (e) cell subsets in bronchoalveolar lavage fluids. The results are expressed as the mean±1 s.d. and are from three experiments and five mice/group. (*P<0.05 compared with control C57BL/6 mice). OD, optical density.
Protection by IEC IKKβ requires oral sensitization
To further establish the role played by IECs in protection of IKKβΔIEC mice against allergic airway inflammation, mice were sensitized by intraperitoneal injection of OVA plus cholera toxin. Although IgG2a Abs were lower in IKKβΔIEC mice, the rest of Ig isotype and IgG subclass responses were similar to control C57BL/6 mice (Supplementary Figure S9A online). No difference was seen in lung inflammation after nasal antigen challenge, although IKKβΔIEC mice exhibited higher mucus production than control mice (Supplementary Figure S9B online). These results underline the influence of the route of antigen sensitization on Ab responses and airway responses to subsequent antigen exposure or challenge.
Gut-sensitized IL-17A-producing CD4+ T cells limit protection by IEC IKKβ
We next examined airway cytokine responses and lung functions after allergen challenges. IKKβΔIEC and IKKβΔMye mice exhibited lower levels of lung eotaxin (C-C motif chemokine ligand 11) and eosinophil peroxidase mRNA responses but enhanced IFN-γ, IL-17A, and MIP-2 (macrophage inflammatory protein-2) mRNA responses, with highest levels of response in IKKβΔIEC mice, after nasal antigen challenge (Figure 6a). Furthermore, low or no IFN-γ and IL-17 responses were measured in BAL of control mice after antigen challenge, whereas their levels were elevated in IKKβΔIEC mice (Supplementary Figure S10). No mice developed signs of airway hyper-responsiveness without previous oral sensitization (Figure 6b), and sensitized IKKβΔMye mice were completely protected against airway hyper-responsiveness. Upon challenge, IKKβΔIEC mice developed airway hyper-responsiveness responses, which were not statistically different from control C57BL/6 mice (Figure 6c). Interestingly, nasal treatment with anti-IL-17A mAbs reduced airway hyper-responsiveness in IKKβΔIEC mice (Figure 6d) and the percentage of neutrophils in BALs (Figure 6e).
Gut-sensitized interleukin (IL)-17A-producing CD4+ T cells limit the protective effect of immunoglobulin A antibodies in the airways of IKKβΔIEC (deletion of inhibitor-κB kinase (IKKβ) in intestinal epithelial cells (IECs)) mice. (a–c) Mice were orally sensitized on days 0 and 14 and nasally challenged on days 15, 16, and 19. (a) Cytokines, chemokines, and neutrophil peroxidase mRNA responses in lung tissues on day 20. Results are expressed as mean±s.d. of three separate experiments, with four mice per group. (*P<0.05 compared with control C57BL/6 mice). (b) Airway hyper-reactivity after nasal challenge of naive mice. (c) Airway hyper-reactivity after nasal challenge (day 20) of orally sensitized mice. (d–f) Responses to anti-IL-17A treatment. (d) Airway hyper-reactivity, (e) total number of cells and (f) immune cell populations in bronchoalveolar lavage (BAL). Results are expressed as mean±s.d. of 5 mice per group. (*P<0.05). (g, h) Adoptive transfers of mesenteric lymph node (MLN) cells. (g) Timeline of adoptive transfer experiments. (h) Frequency of donor (CD45.2) CD4+ T cells expressing α4β7 and CCR9 (C-C motif chemokine receptor 9). Results are expressed as the mean±one s.d. and are from four separate experiments. (*P<0.05; **P<0.01). CCL, C-C motif chemokine ligand; Epx, eosinophil peroxidase; IFN, interferon; IV, intravenous; MIP, macrophage inflammatory protein.
Finally, we adoptively transferred MLN cells of orally sensitized control C57BL/6 and IKKβΔIEC mice into naive CD45.1+ congenic recipient mice (Figure 6g). Analysis of lung cells after nasal antigen challenge showed a higher number of donor CD3+CD4+CD45.2+ cells in recipients of cells from IKKβΔIEC mice (Figure 6h). A larger number of these donor CD4+ T cells also expressed α4β7 and CCR9 (C-C motif chemokine receptor 9), suggesting that they were sensitized in the gut (Figure 6h).
Discussion
Immune homeostasis is crucial at the mucosal surface of the gastrointestinal tract, which is constantly exposed to ingested antigens and commensal flora. Alteration of this homeostasis can lead to inflammatory bowel disease or food allergy. The higher incidence of asthma in inflammatory bowel diseases patients has suggested that these pathologies could share common etiological factors.32 Furthermore, growing evidence suggests that gut commensal microbiota can affect distant mucosal sites such as those of the airways and regulate innate and adaptive immune responses to respiratory virus infection30, 33 and allergic airway inflammation.34 Using genetically modified mice with cell-specific alteration of IKKβ, we found that depletion of IKKβ-NFκB signaling in IECs alters the microbial community in the gut, reshapes immune responses to food allergens, and regulates allergic responses in the airways via its effect on IgA Ab and Th17 cell responses.
Allergic sensitization to food antigens can be modeled by oral administration of antigen with cholera toxin as adjuvant.5, 6, 22 Cholera toxin can break oral tolerance and promote adaptive immunity by binding to IECs and stimulating inflammatory cytokines.35, 36 The NF-κB pathway can mediate both pro- and anti-inflammatory effects,8, 9 and alteration of the IKKβ-NF-κB in IECs could either attenuate chronic or exacerbate acute gut inflammatory diseases.11 We clearly show that lack of IKKβ in IECs did not prevent these cells from developing pro-inflammatory and pSTAT3 responses but also increased TGF-β mRNA in IKKβΔIEC mice. The latter finding is significant, as bone marrow stromal cells were reported to suppress allergic responses via induction of TGF-β.37 Intestinal bacteria have a role in the maturation of gut immune cells,15, 27, 28 and selected commensal bacteria support allergic responses.38 The Clostridium-related bacterium SFB not only promotes Th17 responses27, 28 but is also known to support IgA Abs.39, 40 It is important to indicate that Ig class switch to the IgA isotype requires IL-6 and TGF-β,41 which also support the differentiation of Th17 cells.42 Our results clearly show that alteration of IKKβ signaling in IECs can reorganize the gut microbiota and increase the proportion of Clostridium species and SFB during allergic sensitization in our experimental model. Our findings are consistent with the reported role of SFB and suggest that this bacterium and other Clostridium sp. helped enhance Th17 and IgA Ab responses in IKKβΔIEC mice.
Nasal exposure to antigen after allergic sensitization promotes asthma-like pathology with increased airway hyper-responsiveness, airway inflammation, eosinophilia, and mucus secretion.2, 43 Despite similar levels of IgE Ab responses than control wild-type mice, IKKβΔIEC mice only developed limited lung inflammation upon antigen challenge. The fact that only IKKβΔIEC mice showed high level of IgA Abs and IgA-secreting cells in the airways support the notion that IgA Abs suppress allergic inflammation,31 possibly by neutralizing allergens in mucosal tissues.
Consistent with the reported role of alveolar macrophages in asthma-induced inflammation,44 their percentage was lower in IKKβΔIEC mice than in control mice. Airway hyper-responsiveness and eosinophilia in mice were reported to be associated with a high number of CD103+ dendritic cells.45 Our study suggests that these cells also have a role in pathologies associated with priming to food antigens in the gastrointestinal tract. IL-17A is a mucogenic cytokine,46, 47 which regulates airway inflammation,48 and double-negative T cells, producing IFN-γ and IL-17A, were reported to be the major responders in the lungs of mice during pulmonary infection with a live Francisella tularensis vaccine.49 We show that CD4+ T cells primed in mucosal tissues represent an important fraction of effector cells recruited in the lungs of IKKβΔIEC mice upon antigen challenge and that they limit the protective effect of IgA Abs on allergic airway symptoms in this model via production of IL-17A.
We have shown that IKKβ deficiency in IECs promotes a cascade of events that ultimately protects the airways against the development of allergic inflammation (Figure 7). Our results suggest that future efforts for controlling allergic responses could include strategies that promote IgA Ab responses and prevent or reduce IL-17 responses.
Regulation of pathogenic airway responses to allergens by inhibitor-κB kinase (IKKβ) in intestinal epithelial cells (IECs). Allergic sensitization in the gut promotes antigen-specific immunoglobulin E (IgE) and T helper type 2 (Th2) responses, which will later induce allergic airway inflammation and airway hyper-responsiveness in the event of airway exposure to the same antigen. Loss of IKKβ in IECs does not alter immune homeostasis in the gut at the basal level. However, during allergic sensitization, lack of IKKβ signaling in IECs could enhance gut pro-inflammatory responses and promote dysbiosis. The change in cytokine milieu could support IgA antibodies (Abs), while alteration of the gut microbiota would support Th17 responses. Subsequent exposure of the airways to allergen will result in the accumulation of IgA Abs, which will protect against allergic inflammation. CD4+ T cells expressing the gut-homing receptors α4β7 and CCR9 (C-C motif chemokine receptor 9) and producing IL-17 are also recruited in the airways of IKKβΔIEC mice upon antigen exposure. These cells more likely support hyper-responsivess of the airways to antigen exposure, and could be suppressed by treatment with anti-IL-17A Ab.IL, interleukin; SFB, segmented filamentous bacteria; STAT, signal transducer and activator of transcription factor.
Methods
Mice. Mice in which IKKβ-dependent NF-κB signaling was selectively eliminated in the IECs (IKKβΔIEC) or myeloid cells (IKKβΔmye) were generated as previously described8, 23 and bred in our facility. Control C57BL/6 mice were obtained from the NCI-Frederick and housed for 3–4 weeks with IKKβ-deficient mice. Studies were performed on mice aged 10–12 weeks, in accordance with NIH and OSU IACUC guidelines.
Quantification of mRNA by real-time reverse transcriptase–PCR. Real-time reverse transcriptase–PCR was performed as previously described,50 and mRNA responses were expressed as mRNA relative expression=(1/2ΔCt) × 100 × 1000) where ΔCt=CPunknown−CPβactin.
Histology. Five 5-μm paraffin sections were stained with hematoxylin and eosin, alone or with anti-pSTAT3 (Cell Signaling, Danvers, MA), anti-pNF-κB p65 (Santa Cruz Biotech, Dallas, TX), or subjected to periodic acid-Schiff staining.
Immunoblotting. Intestines were lysed, and proteins were separated by SDS-PAGE (sodium dodecyl sulfate-polyacrylamide gel electrophoresis). After transfer, PVDF (polyvinylidene difluoride) membranes were probed with anti-pSTAT3 (Cell Signaling) and an horseradish peroxidase–conjugated secondary Ab. The membranes were re-probed with β-actin-specific Ab (Santa Cruz Biotech) and the relative ratios of pSTAT3/β-actin were determined using Image J software (Bethesda, MD).
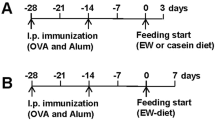
Oral treatment, oral sensitization, and nasal challenge of mice. For oral treatment, mice were deprived of food for 2 h and given 250 μl of sodium bicarbonate 30 min before intragastric gavage of 10 μg cholera toxin in 250 μl of phosphate-buffered saline (PBS). Oral sensitization was performed on days 0 and 7 by intragastric gavage of 250 μl of PBS containing 1 mg of ovalbumin (OVA) and 10 μg cholera toxin as adjuvant. Blood samples were collected on days 7 and 14. Nasal antigen challenges were performed on days 15, 16, and 19. For this purpose, mice were anesthetized by intraperitoneal injection of ketamine/xylazine and administered 200 μg of OVA in PBS. In selected experiments, mice were nasally treated (10 μg per dose) with an anti-IL-17A mAb or isotype control Ab (R&D Systems, Minneapolis, MN).
Analysis of gut microbiota. Bacterial tag-encoded FLX amplicon pyrosequencing (Roche Titanium 454 FLX pyrosequencing, Branford, CT) was used for detection and identification of the primary populations of microbes in fecal pellet samples. For identification of SFB, blast search was performed with the fasta sequences against Candidatus Arthromitus (taxid:49082) genome sequences (Candidatus Arthromitus sp. SFB-mouse-Yit and Candidatus Arthromitus sp. SFB-mouse-Japan), using Megablast (optimized for highly similar sequences; ⩾95%) and E-values below 1e-15.
Fecal microbiota transplantation. Fecal material for microbiota transfer was prepared by using a modification of a previously described method.51 Briefly, freshly emitted fecal pellets were homogenized by vortexing in sterile PBS (1 ml per 0.1 g of fecal material). After filtration of particulate matters, mice were gavage with 0.2 ml of the suspension.
Antigen-specific CD4+ T cell cytokine responses. Spleens and MLN were collected 1 week after the last immunization and mononuclear cells were restimulated in vitro with OVA (1 mg ml−1) as previously reported.52 After 5 days of culture, levels of Th1 (IFN-γ), Th2 (IL-4, IL-5, IL-10), or Th17 (IL-17A) cytokines in supernatants were determined by enzyme-linked immunosorbent assay using mAb pairs and cytokine standards (BD Biosciences, San Jose, CA or R&D Systems).
Antigen-specific Ab responses and total IgA levels. OVA-specific Ab responses were measured by enzyme-linked immunosorbent assay as previously described.52 Total IgA levels were determined by enzyme-linked immunosorbent assay and IgA standards. The frequency of IgA-secreting cells were evaluated by ELISPOT.53
Analysis of lung functions and airway responses to metacholine challenge. Mechanical properties of the mouse lung were assessed using the forced-oscillation technique54 and a flexiVent computer-controlled piston ventilator (SCIREQ, Montreal, QC, Canada). Mice were exposed to increasing doses of metacholine (0.1, 1, 10, 20, and 50 mg ml−1) in sterile normal saline,54 and total lung resistance were recorded.
Adoptive transfer. Cells (8 × 106) from control C57BL/6 (CD45.2) or IKKβΔIEC (CD45.2) were injected intravenously into congenic CD45.1 mice. Donor and recipient cells were discriminated in tissues of recipient mice by flow cytometry using CD45.1 and CD45.2 specific mAbs (BD Biosciences).
BALs. BAL fluids were obtained via cannulation of the exposed trachea, by infusion of 600 μl of sterile PBS through a 22-gauge catheter into the lungs.5
Analysis of cell populations in lung tissues. Whole-lung tissue was dissociated in 0.5 mg ml−1 collagenase type V (Sigma, St Louis, MO) for 15 min at 37 °C. Single-cell preparations were stained with one or a combination of the fluorescent anti-mouse Abs: anti-CD11b, anti-CD11c, anti-F4/80 anti-B220, anti-CD3, anti-CD4, anti-CD8, anti-CD103, anti-α4β7, and anti-CCR9 (BD Biosciences and eBiosciences, San Diego, CA) and analyzed by flow cytometry (Accuri Cytometers, San Jose, CA).
Statistics. Results are expressed as the mean±1 s.d. Statistical significance was determined by Student’s t-test or by analysis of variance followed by the Fisher Least Significant Difference Test. For analysis of mRNA responses, we used one-way analysis of variance, followed by Duncan’s Multiple Range Test.. All statistical analyses were performed with the Statistica 9.0 software package (StatSoft, Tulsa, OK).
References
Holgate, S.T. Pathophysiology of asthma: what has our current understanding taught us about new therapeutic approaches? J. Allergy Clin. Immunol. 128, 495–505 (2011).
Sicherer, S.H. & Sampson, H.A. Food allergy. J. Allergy Clin. Immunol. 125 (2 Suppl 2), S116–S125 (2010).
Broide, D.H. et al. Allergen-induced peribronchial fibrosis and mucus production mediated by IkappaB kinase beta-dependent genes in airway epithelium. Proc. Natl. Acad. Sci. USA 102, 17723–17728 (2005).
Ather, J.L., Hodgkins, S.R., Janssen-Heininger, Y.M. & Poynter, M.E. Airway epithelial NF-kappaB activation promotes allergic sensitization to an innocuous inhaled antigen. Am. J. Respir. Cell Mol. Biol. 44, 631–638 (2011).
Fischer, R. et al. Oral and nasal sensitization promote distinct immune responses and lung reactivity in a mouse model of peanut allergy. Am. J. Pathol. 167, 1621–1630 (2005).
Oyoshi, M.K. et al. Epicutaneous challenge of orally immunized mice redirects antigen-specific gut-homing T cells to the skin. J. Clin. Invest. 121, 2210–2220 (2011).
Vallabhapurapu, S. & Karin, M. Regulation and function of NF-kappaB transcription factors in the immune system. Annu. Rev. Immunol. 27, 693–733 (2009).
Greten, F.R. et al. NF-kappaB is a negative regulator of IL-1beta secretion as revealed by genetic and pharmacological inhibition of IKKbeta. Cell 130, 918–931 (2007).
Lawrence, T., Gilroy, D.W., Colville-Nash, P.R. & Willoughby, D.A. Possible new role for NF-kappaB in the resolution of inflammation. Nat. Med. 7, 1291–1297 (2001).
Fong, C.H. et al. An antiinflammatory role for IKKbeta through the inhibition of "classical" macrophage activation. J. Exp. Med. 205, 1269–1276 (2008).
Eckmann, L. et al. Opposing functions of IKKbeta during acute and chronic intestinal inflammation. Proc. Natl. Acad. Sci. USA 105, 15058–15063 (2008).
Zaph, C. et al. Epithelial-cell-intrinsic IKK-beta expression regulates intestinal immune homeostasis. Nature 446, 552–556 (2007).
Backhed, F., Ley, R.E., Sonnenburg, J.L., Peterson, D.A. & Gordon, J.I. Host-bacterial mutualism in the human intestine. Science 307, 1915–1920 (2005).
Bouma, G. & Strober, W. The immunological and genetic basis of inflammatory bowel disease. Nat. Rev. Immunol. 3, 521–533 (2003).
Chung, H. et al. Gut immune maturation depends on colonization with a host-specific microbiota. Cell 149, 1578–1593 (2012).
Macpherson, A.J. & Harris, N.L. Interactions between commensal intestinal bacteria and the immune system. Nat. Rev. Immunol. 4, 478–485 (2004).
Rodriguez, B. et al. Infant gut microbiota is protective against cow's milk allergy in mice despite immature ileal T-cell response. FEMS Microbiol. Ecol. 79, 192–202 (2012).
Bjorksten, B., Sepp, E., Julge, K., Voor, T. & Mikelsaar, M. Allergy development and the intestinal microflora during the first year of life. J. Allergy Clin. Immunol. 108, 516–520 (2001).
Turnbaugh, P.J. et al. A core gut microbiome in obese and lean twins. Nature 457, 480–484 (2009).
Greenblum, S., Turnbaugh, P.J. & Borenstein, E. Metagenomic systems biology of the human gut microbiome reveals topological shifts associated with obesity and inflammatory bowel disease. Proc. Natl. Acad. Sci. USA 109, 594–599 (2012).
Elinav, E. et al. NLRP6 inflammasome regulates colonic microbial ecology and risk for colitis. Cell 145, 745–757 (2011).
Dunkin, D., Berin, M.C. & Mayer, L. Allergic sensitization can be induced via multiple physiologic routes in an adjuvant-dependent manner. J. Allergy Clin. Immunol. 128, 1251–1258.e2 (2011).
Chen, L.W., Egan, L., Li, Z.W., Greten, F.R., Kagnoff, M.F. & Karin, M. The two faces of IKK and NF-kappaB inhibition: prevention of systemic inflammation but increased local injury following intestinal ischemia-reperfusion. Nat. Med. 9, 575–581 (2003).
Snel, J. et al. Comparison of 16S rRNA sequences of segmented filamentous bacteria isolated from mice, rats, and chickens and proposal of "Candidatus Arthromitus". Int. J. Syst. Bacteriol. 45, 780–782 (1995).
Umesaki, Y., Okada, Y., Imaoka, A., Setoyama, H. & Matsumoto, S. Interactions between epithelial cells and bacteria, normal and pathogenic. Science 276, 964–965 (1997).
Prakash, T. et al. Complete genome sequences of rat and mouse segmented filamentous bacteria, a potent inducer of th17 cell differentiation. Cell Host Microbe 10, 273–284 (2011).
Gaboriau-Routhiau, V. et al. The key role of segmented filamentous bacteria in the coordinated maturation of gut helper T cell responses. Immunity 31, 677–689 (2009).
Ivanov, I.I. et al. Induction of intestinal Th17 cells by segmented filamentous bacteria. Cell 139, 485–498 (2009).
Bashir, M.E., Louie, S., Shi, H.N. & Nagler-Anderson, C. Toll-like receptor 4 signaling by intestinal microbes influences susceptibility to food allergy. J. Immunol. 172, 6978–6987 (2004).
Ichinohe, T. et al. Microbiota regulates immune defense against respiratory tract influenza A virus infection. Proc. Natl. Acad. Sci. USA 108, 5354–5359 (2011).
Smits, H.H. et al. Cholera toxin B suppresses allergic inflammation through induction of secretory IgA. Mucosal Immunol. 2, 331–339 (2009).
Weng, X., Liu, L., Barcellos, L.F., Allison, J.E. & Herrinton, L.J. Clustering of inflammatory bowel disease with immune mediated diseases among members of a northern california-managed care organization. Am. J. Gastroenterol. 102, 1429–1435 (2007).
Abt, M.C. et al. Commensal bacteria calibrate the activation threshold of innate antiviral immunity. Immunity 37, 158–170 (2012).
Hill, D.A. et al. Commensal bacteria-derived signals regulate basophil hematopoiesis and allergic inflammation. Nat. Med. 18, 538–546 (2012).
Bromander, A.K., Kjerrulf, M., Holmgren, J. & Lycke, N. Cholera toxin enhances alloantigen presentation by cultured intestinal epithelial cells. Scand. J. Immunol. 37, 452–458 (1993).
Bandyopadhaya, A., Sarkar, M. & Chaudhuri, K. Transcriptional upregulation of inflammatory cytokines in human intestinal epithelial cells following Vibrio cholerae infection. FEBS J. 274, 4631–4642 (2007).
Nemeth, K. et al. Bone marrow stromal cells use TGF-beta to suppress allergic responses in a mouse model of ragweed-induced asthma. Proc. Natl. Acad. Sci. USA 107, 5652–5657 (2010).
Bisgaard, H. et al. Reduced diversity of the intestinal microbiota during infancy is associated with increased risk of allergic disease at school age. J. Allergy Clin. Immunol. 128, 646-52.e1–646-52.e5 (2011).
Klaasen, H.L. et al. Apathogenic, intestinal, segmented, filamentous bacteria stimulate the mucosal immune system of mice. Infect. Immun. 61, 303–306 (1993).
Talham, G.L., Jiang, H.Q., Bos, N.A. & Cebra, J.J. Segmented filamentous bacteria are potent stimuli of a physiologically normal state of the murine gut mucosal immune system. Infect. Immun. 67, 1992–2000 (1999).
Suzuki, K. & Fagarasan, S. Diverse regulatory pathways for IgA synthesis in the gut. Mucosal Immunol. 2, 468–471 (2009).
Weaver, C.T., Hatton, R.D., Mangan, P.R. & Harrington, L.E. IL-17 family cytokines and the expanding diversity of effector T cell lineages. Annu. Rev. Immunol. 25, 821–852 (2007).
Salvatori, N. et al. Asthma induced by inhalation of flour in adults with food allergy to wheat. Clin. Exp. Allergy 38, 1349–1356 (2008).
Song, C. et al. IL-17-producing alveolar macrophages mediate allergic lung inflammation related to asthma. J. Immunol. 181, 6117–6124 (2008).
Sung, S.S., Fu, S.M., Rose, C.E. Jr., Gaskin, F., Ju, S.T. & Beaty, S.R. A major lung CD103 (alphaE)-beta7 integrin-positive epithelial dendritic cell population expressing Langerin and tight junction proteins. J. Immunol. 176, 2161–2172 (2006).
Chen, Y., Thai, P., Zhao, Y.H., Ho, Y.S., DeSouza, M.M. & Wu, R. Stimulation of airway mucin gene expression by interleukin (IL)-17 through IL-6 paracrine/autocrine loop. J. Biol. Chem. 278, 17036–17043 (2003).
Lukacs, N.W., Smit, J.J., Mukherjee, S., Morris, S.B., Nunez, G. & Lindell, D.M. Respiratory virus-induced TLR7 activation controls IL-17-associated increased mucus via IL-23 regulation. J. Immunol. 185, 2231–2239 (2010).
Durrant, D.M., Gaffen, S.L., Riesenfeld, E.P., Irvin, C.G. & Metzger, D.W. Development of allergen-induced airway inflammation in the absence of T-bet regulation is dependent on IL-17. J. Immunol. 183, 5293–5300 (2009).
Cowley, S.C., Meierovics, A.I., Frelinger, J.A., Iwakura, Y. & Elkins, K.L. Lung CD4-CD8- double-negative T cells are prominent producers of IL-17A and IFN-gamma during primary respiratory murine infection with Francisella tularensis live vaccine strain. J. Immunol. 184, 5791–5801 (2010).
Duverger, A. et al. Contributions of edema factor and protective antigen to the induction of protective immunity by Bacillus anthracis edema toxin as an intranasal adjuvant. J. Immunol. 185, 5943–5952 (2010).
Turnbaugh, P.J., Ridaura, V.K., Faith, J.J., Rey, F.E., Knight, R. & Gordon, J.I. The effect of diet on the human gut microbiome: a metagenomic analysis in humanized gnotobiotic mice. Sci. Transl. Med. 1, 6ra14 (2009).
Duverger, A. et al. Bacillus anthracis edema toxin acts as an adjuvant for mucosal immune responses to nasally administered vaccine antigens. J. Immunol. 176, 1776–1783 (2006).
Boyaka, P.N. et al. Chimeras of labile toxin one and cholera toxin retain mucosal adjuvanticity and direct Th cell subsets via their B subunit. J. Immunol. 170, 454–462 (2003).
Aeffner, F., Traylor, Z.P., Yu, E.N. & Davis, I.C. Double-stranded DNA induces similar pulmonary dysfunction to respiratory syncytial virus in BALB/c mice. Am. J. Physiol. Lung Cell. Mol. Physiol. 301, L99–L109 (2011).
Acknowledgements
Supported by grants from the National Institute of Health (R01 AI043197) and the OSU Food Innovation Center (to PNB), and a fellowship from Fondation Lelous, France (to AB-B). We thank Dr Kate Hayes-Ozello for editorial assistance, Dr Jessica Grieves for assistance with scoring of histology, Tim Vojt for help with graphic design, and Dr J Delton Hanson for review of the metagenomic data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
SUPPLEMENTARY MATERIAL is linked to the online version of the paper at
Rights and permissions
About this article
Cite this article
Bonnegarde-Bernard, A., Jee, J., Fial, M. et al. IKKβ in intestinal epithelial cells regulates allergen-specific IgA and allergic inflammation at distant mucosal sites. Mucosal Immunol 7, 257–267 (2014). https://doi.org/10.1038/mi.2013.43
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2013.43