Abstract
Objective:
To determine whether further cervical length shortening by transvaginal ultrasonography in asymptomatic high-risk women with a short cervical length adds additional predictive value for spontaneous preterm birth and perinatal morbidity.
Study Design:
Women with a history of spontaneous preterm birth, loop electrosurgical excision procedure, cone biopsy or uterine anomaly, who were pregnant with singleton gestations and were found by transvaginal ultrasonography to have a cervical length <3.0 cm at 20 to 28 weeks’ gestation, and who underwent a follow-up cervical length within 3 weeks were evaluated, comparing those with further cervical length shortening (>10%) to those without further shortening. Primary outcomes were spontaneous preterm birth <35 weeks’ gestation and perinatal morbidity. Secondary outcomes included spontaneous preterm birth <37 weeks, <34 weeks, <32 weeks, birth weight <2500 g, maternal and other neonatal outcomes.
Result:
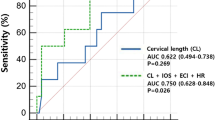
Compared with women without further cervical shortening, those with further shortening were found by univariate analyses to have higher rates of spontaneous preterm birth <35 weeks (34.8 versus 8.5%, P=0.014), <37 weeks (56.5 versus 21.3%, P=0.003), <34 weeks (30.4 versus 2.1%, P=0.001), <32 weeks (21.7 versus 0%, P=0.003), birth weight <2500 g (60.9 versus 17.0%, P<0.0001), neonatal intensive care unit admission (47.8 versus 17.0%, P=0.006) and composite perinatal morbidity (43.5 versus 14.9%, P=0.009). Logistic regression revealed the only independent predictors of spontaneous preterm birth <35 weeks were further cervical length shortening (adjusted odds ratio (aOR) 5.73; 95% confidence interval (CI) 1.31 to 24.43) and gestational age at short cervical length (aOR 0.95; 95% CI 0.91 to 0.99).
Conclusion:
Further cervical length shortening in asymptomatic high-risk women with a short cervical length is an important independent predictor of spontaneous preterm birth <35 weeks and perinatal morbidity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Committee on understanding premature birth and assuring healthy outcomes. Board on Health Sciences Policy, Institute of Medicine of the National Academies. Behrman RE, Butler AS, editors. Preterm birth: causes, consequences and prevention. Washington: National Academies Press, 2007.
Hack M, Taylor HG, Klein N, Eiben R, Schatschneider C, Mercuri-Minich N . School-age outcomes in children with birth weights under 750 g. New Engl J Med 1994; 331: 753–759.
McCormick MC . The contribution of low birth weight to infant mortality and childhood morbidity. New Engl J Med 1985; 312: 82–90.
Alexander GR, Kogan M, Bader D, Carlo W, Allen M, Mor J . US birth weight/gestational age-specific neonatal mortality: 1995–1997 rates for whites, hispanics, and blacks. Pediatrics 2003; 111: e61–e66.
Lawn JE, Cousens S, Zupan J . 4 million neonatal deaths: when? Where? Why? Lancet 2005; 365 (9462): 891–900.
Mercer BM, Goldenberg RL, Moawad AH, Meis PJ, Iams JD, Das AF et al. The Preterm Prediction Study: effect of gestational age and cause of preterm birth on subsequent obstetric outcome. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Am J Obstet Gynecol 1999; 181: 1216–1221.
Iams JD, Goldenberg RL, Mercer BM, Moawad A, Thom E, Meis PJ et al. The Preterm Prediction Study: recurrence risk of spontaneous preterm birth. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Am J Obstet Gynecol 1998; 178: 1035–1040.
Creasy RK, Gummer BA, Liggins GC . System for predicting spontaneous preterm birth. Obstet Gynecol 1980; 55: 692–695.
Mercer BM, Goldenberg RL, Das A, Moawad AH, Iams JD, Meis PJ et al. The preterm prediction study: a clinical risk assessment system. Am J Obstet Gynecol 1996; 174: 1885–1893; 93–95.
Bloom SL, Yost NP, McIntire DD, Leveno KJ . Recurrence of preterm birth in singleton and twin pregnancies. Obstet Gynecol 2001; 98: 379–385.
Adams MM, Elam-Evans LD, Wilson HG, Gilbertz DA . Rates of and factors associated with recurrence of preterm delivery. JAMA 2000; 283: 1591–1596.
Mazaki-Tovi S, Romero R, Kusanovic JP, Erez O, Pineles BL, Gotsch F et al. Recurrent preterm birth. Semin Perinatol 2007; 31: 142–158.
Crane JM, Delaney T, Hutchens D . Transvaginal ultrasonography in the prediction of preterm birth after treatment for cervical intraepithelial neoplasia. Obstet Gynecol 2006; 107: 37–44.
Arbyn M, Kyrgiou M, Simoens C, Raifu AO, Koliopoulos G, Martin-Hirsch P et al. Perinatal mortality and other severe adverse pregnancy outcomes associated with treatment of cervical intraepithelial neoplasia: meta-analysis. BMJ (Clinical Research Ed) 2008; 337: a1284.
Jolley JA, Wing DA . Pregnancy management after cervical surgery. Curr Opin Obstet Gynecol 2008; 20: 528–533.
Grimbizis GF, Camus M, Tarlatzis BC, Bontis JN, Devroey P . Clinical implications of uterine malformations and hysteroscopic treatment results. Hum Reprod Update 2001; 7: 161–174.
Acien P . Incidence of Mullerian defects in fertile and infertile women. Hum Reprod (Oxford, England) 1997; 12: 1372–1376.
Raga F, Bauset C, Remohi J, Bonilla-Musoles F, Simon C, Pellicer A . Reproductive impact of congenital Mullerian anomalies. Hum Reprod (Oxford, England) 1997; 12: 2277–2281.
Ludmir J, Samuels P, Brooks S, Mennuti MT . Pregnancy outcome of patients with uncorrected uterine anomalies managed in a high-risk obstetric setting. Obstet Gynecol 1990; 75: 906–910.
Crane JM, Hutchens D . Transvaginal sonographic measurement of cervical length to predict preterm birth in asymptomatic women at increased risk: a systematic review. Ultrasound Obstet Gynecol 2008; 31: 579–587.
Crane JM, Hutchens D . Use of transvaginal ultrasonography to predict preterm birth in women with a history of preterm birth. Ultrasound Obstet Gynecol 2008; 32: 640–645.
Andrews WW, Copper R, Hauth JC, Goldenberg RL, Neely C, Dubard M . Second-trimester cervical ultrasound: associations with increased risk for recurrent early spontaneous delivery. Obstet Gynecol 2000; 95: 222–226.
Durnwald CP, Walker H, Lundy JC, Iams JD . Rates of recurrent preterm birth by obstetrical history and cervical length. Am J Obstet Gynecol 2005; 193: 1170–1174.
de Carvalho MH, Bittar RE, Brizot Mde L, Bicudo C, Zugaib M . Prediction of preterm delivery in the second trimester. Obstet Gynecol 2005; 105: 532–536.
To MS, Palaniappan V, Skentou C, Gibb D, Nicolaides KH . Elective cerclage vs ultrasound-indicated cerclage in high-risk pregnancies. Ultrasound Obstet Gynecol 2002; 19: 475–477.
Owen J, Yost N, Berghella V, Thom E, Swain M, Dildy III GA et al. Mid-trimester endovaginal sonography in women at high risk for spontaneous preterm birth. JAMA 2001; 286: 1340–1348.
Berghella V, Pereira L, Gariepy A, Simonazzi G . Prior cone biopsy: prediction of preterm birth by cervical ultrasound. Am J Obstet Gynecol 2004; 191: 1393–1397.
Airoldi J, Berghella V, Sehdev H, Ludmir J . Transvaginal ultrasonography of the cervix to predict preterm birth in women with uterine anomalies. Obstet Gynecol 2005; 106: 553–556.
Fox NS, Jean-Pierre C, Predanic M, Chasen ST . Short cervix: is a follow-up measurement useful? Ultrasound Obstet Gynecol 2007; 29: 44–46.
Naim A, Haberman S, Burgess T, Navizedeh N, Minkoff H . Changes in cervical length and the risk of preterm labor. Am J Obstet Gynecol 2002; 186: 887–889.
Szychowski JM, Owen J, Hankins G, Iams J, Sheffield J, Perez-Delboy A et al. Timing of mid-trimester cervical length shortening in high-risk women. Ultrasound Obstet Gynecol 2009; 33: 70–75.
Carvalho MH, Bittar RE, Brizot ML, Maganha PP, Borges da Fonseca ES, Zugaib M . Cervical length at 11–14 weeks’ and 22–24 weeks’ gestation evaluated by transvaginal sonography, and gestational age at delivery. Ultrasound Obstet Gynecol 2003; 21: 135–139.
Guzman ER, Mellon C, Vintzileos AM, Ananth CV, Walters C, Gipson K . Longitudinal assessment of endocervical canal length between 15 and 24 weeks’ gestation in women at risk for pregnancy loss or preterm birth. Obstet Gynecol 1998; 92: 31–37.
Yoshizato T, Obama H, Nojiri T, Miyake Y, Miyamoto S, Kawarabayashi T . Clinical significance of cervical length shortening before 31 weeks’ gestation assessed by longitudinal observation using transvaginal ultrasonography. J Obstet Gynaecol Res 2008; 34: 805–811.
Watson WJ, Stevens D, Welter S, Day D . Observations on the sonographic measurement of cervical length and the risk of premature birth. J Matern Fetal Med 1999; 8: 17–19.
Dilek TU, Yazici G, Gurbuz A, Tasdelen B, Gulhan S, Dilek B et al. Progressive cervical length changes versus single cervical length measurement by transvaginal ultrasound for prediction of preterm delivery. Gynecol Obstet Invest 2007; 64: 175–179.
Sotiriadis A, Kavvadias A, Papatheodorou S, Paraskevaidis E, Makrydimas G . The value of serial cervical length measurements for the prediction of threatened preterm labour. Eur J Obstet Gynecol Reprod Biol 2009; 148: 17–20.
Valentin L, Bergelin I . Intra- and interobserver reproducibility of ultrasound measurements of cervical length and width in the second and third trimesters of pregnancy. Ultrasound Obstet Gynecol 2002; 20: 256–262.
Sackett DL, Richardson WS, Rosenberg W, Haynes RB . Evidence-Based Medicine: How to Practice and Teach EBM. Churchill Livingstone: New York, NY, 1997, p 135, 79–81.
Berghella V, Roman A, Daskalakis C, Ness A, Baxter JK . Gestational age at cervical length measurement and incidence of preterm birth. Obstet Gynecol 2007; 110 (2 Part 1): 311–317.
Berghella V, Odibo AO, To MS, Rust OA, Althuisius SM . Cerclage for short cervix on ultrasonography: meta-analysis of trials using individual patient-level data. Obstet Gynecol 2005; 106: 181–189.
Owen J, Hankins G, Iams JD, Berghella V, Sheffield JS, Perez-Delboy A et al. Multicenter randomized trial of cerclage for preterm birth prevention in high-risk women with shortened midtrimester cervical length. Am J Obstet Gynecol 2009; 201: 375.e1–375.e8.
Meis PJ, Klebanoff M, Thom E, Dombrowski MP, Sibai B, Moawad AH et al. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. New Engl J Med 2003; 348: 2379–2385.
Fonseca EB, Celik E, Parra M, Singh M, Nicolaides KH . Progesterone and the risk of preterm birth among women with a short cervix. New Engl J Med 2007; 357: 462–469.
DeFranco EA, O’Brien JM, Adair CD, Lewis DF, Hall DR, Fusey S et al. Vaginal progesterone is associated with a decrease in risk for early preterm birth and improved neonatal outcome in women with a short cervix: a secondary analysis from a randomized, double-blind, placebo-controlled trial. Ultrasound Obstet Gynecol 2007; 30: 697–705.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Crane, J., Hutchens, D. Follow-up cervical length in asymptomatic high-risk women and the risk of spontaneous preterm birth. J Perinatol 31, 318–323 (2011). https://doi.org/10.1038/jp.2010.149
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2010.149
Keywords
This article is cited by
-
First-trimester vaginal microbiome diversity: A potential indicator of preterm delivery risk
Scientific Reports (2017)