- NEWS AND VIEWS
Histidine metabolism boosts cancer therapy
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 559, 484-485 (2018)
doi: https://doi.org/10.1038/d41586-018-05573-4
References
Kanarek, N. et al. Nature 559, 632–636 (2018).
Farber, S., Diamond, L. K., Mercer, R. D., Sylvester, R. F. Jr & Wolff, J. A. N. Engl. J. Med. 238, 787–793 (1948).
Assaraf, Y. G. & Schimke, R. T. Proc. Natl Acad. Sci. USA 84, 7154–7158 (1987).
Roberts, K. G. et al. N. Engl. J. Med. 371, 1005–1015 (2014).
Locasale, J. W. Nature Rev. Cancer 13, 572-583 (2013).
Institute of Medicine of the National Academies. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids Ch. 10 (Natl Acad. Press, 2005).
Brown, P. M., Pratt, A. G. & Isaacs, R. G. Nature Rev. Rheumatol. 12, 731–742 (2016).

 Read the paper: Histidine catabolism is a major determinant of methotrexate sensitivity
Read the paper: Histidine catabolism is a major determinant of methotrexate sensitivity
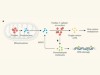 A toxin that fuels metabolism
A toxin that fuels metabolism
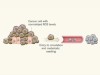 The enemy of my enemy is my friend
The enemy of my enemy is my friend