Abstract
Cancer stem cells have recently been isolated from several different solid tumors. In breast cancer, the CD44+CD24−/low population is considered to comprise stem-like cells. The identification of cancer stem cells has provided new targets for the development of therapeutics. Oncolytic herpes simplex viruses (oHSVs) are an effective strategy for killing breast cancer cells and treating breast tumors in preclinical models. Here, we examined the efficacy of the oHSV G47Δ in killing breast cancer stem cells. Human breast cancer cell line SK-BR-3 and human primary breast cancer cells were cultured in suspension under conditions conducive to the growth of stem cells. They generated mammospheres, which had cancer stem cell properties. The proportion of CD44+CD24−/low cells in these mammospheres exceeded 95%, as determined by flow cytometry. The mammospheres were found to be highly tumorigenic when implanted subcutaneously in nude BALB/c mice. G47Δ contains the LacZ gene, and X-gal staining of infected cells in vitro and in vivo showed the replication and spread of the virus. G47Δ was found to be highly cytotoxic to the CD44+CD24−/low population in vitro, even when injected at low multiplicities of infection, and G47Δ treatment in vivo significantly inhibited tumor growth compared with mock treatment. This study demonstrates that oHSV is effective against breast cancer stem cells and could be a beneficial strategy for treating breast cancer patients.
Similar content being viewed by others
Introduction
Breast cancer is the most common cancer among women, and although it can be diagnosed and treated at an early stage, it is the second leading cause of cancer-related death among women in the United States.1 The disease recurs, mostly metastasizes, in about 30% of all patients with early-stage disease.2 Conventional chemotherapies are initially effective in disease control for patients with metastatic disease but ultimately, most fail. Cancer stem cells are thought to have an important role in recurrence after treatment and contribute to the incurable nature of metastatic breast cancer.3 These cells have the potential for multilineage differentiation, therapeutic resistance, hypoxic resistance and metastasis, and have high tumorigenicity and strong ability for cell invasion. Al-Hajj et al.4 found that palpable tumors were formed when a few hundred CD44+CD24−/low cells were injected into the mammary fat pad of non-obese diabetic/severe combined immunodeficient mice. In this study, we found that mammospheres are generated when the breast cancer cell line SK-BR-3 and human primary breast cancer cells, of which a high proportion are CD44+CD24−/low cells, are cultured in suspension. An important feature of stem cell-like cells is that unlike general tumor cells, they can initiate tumors even when a very small number are present. The present study also found this result. We also confirmed the stem cell-like features of the CD44+CD24−/low cells from among the SK-BR-3 and human primary breast cancer cells, namely, the expression of the common stem cell markers oct4 and sox2. To further determine the stem cell-like characteristics of the CD44+CD24−/low population, we examined them for a key marker of breast cancer stem cells—aldehyde hydrogenase (ALDH1) activity.5, 6 Owing to their slow replication and ability to expel antitumor drugs, these cells are believed to be responsible for the failure of many conventional cancer therapies.7, 8, 9, 10
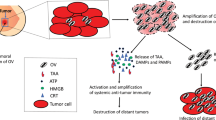
Oncolytic virotherapy is a new therapeutic strategy that is based on the inherent cytotoxicity of viruses and their ability to replicate and spread in tumors in a selective manner.11 Oncolytic herpes simplex virus (oHSV) vectors have many qualities that make them attractive cancer therapeutic agents: They have the ability to replicate in situ, disseminate within the tumor and transfer therapeutic transgenes. Further, they can induce antitumor immune responses and can be eliminated using anti-viral drugs. They are also minimally toxic to normal tissue, a feature important for clinical translation.12 The second generation oHSV vector G207 is currently under clinical trials for malignant glioma.13, 14 G207 contains deletions of both copies of the γ34.5 gene, which is the major determinant of HSV neurovirulence, and has the Escherichia coli LacZ gene in its IPC6 gene (UL39), whereby the ribonucleotide reductase needed for replication in non-dividing cells is inactivated.15 In G47Δ, which is derived from G207, the IPC47 gene and US11 promoter are also deleted, whereby growth and immunogenicity are enhanced and yet safety is maintained.16 G47Δ has been shown to be effective in several preclinical breast cancer models, including human xenografts, a model of metastatic breast cancer in the brain, and spontaneously arising breast tumors in transgenic mice.17, 18, 19 In the present study, we demonstrated the efficacy of G47Δ in suppressing cancer stem cells in a human breast cancer stem cell model.
Materials and methods
Cells and viruses
Human breast cancer tissue was obtained from six breast invasive ductal carcinoma patients who had not received chemotherapy but had undergone modified radical mastectomy (obtained from Breast Cancer Center of the Third Affiliated Hospital of Sun Yat-sen University, China). All samples were washed with phosphate-buffered saline (PBS), treated for fat removal, mechanically disaggregated, and then digested and filtered as described previously.20, 21 The tumor tissue was minced and digested for about 12–18 h at 37 °C with a solution of 100 U ml−1 collagenase I (Gibco), 150 U ml−1 hyaluronidase (Sigma), 10% calf serum (Gibco, Grand Island, NY, USA) and 5 mg l−1 bovine insulin (Sigma, St Louis, MO, USA) in Dulbecco’s modified Eagle’s medium (DMEM; Gibco). The digested tissue was strained with a 40-μm strainer, the cell suspension was washed with PBS and the red blood cells were lysed. The cells treated by the above steps and cells of the line SK-BR-3 (obtained from Dr Zeng Mu-sheng, Sun Yat-sen University Cancer Center, China) were cultured in DMEM-F12 medium (Gibco) supplemented with 10 μg l−1 basic fibroblast growth factor, 20 μg l−1 epidermal growth factor (both from Peprotech, Grand Island, NY, USA), 5 mg l−1 insulin (Gibco) and B27 (1:50; Gibco) at 37 °C in 5% CO2. Foreskin-derived fibroblasts (obtained from Dr Zhang Qi, Department of Hepatic Surgery, the Third Affiliated Hospital of Sun Yat-sen University, China) that were isolated as previously described were cultured in 1640 medium (Gibco) supplemented with 10% fetal bovine serum (Gibco) at 37 °C in 5% CO2.22 G47Δ was constructed as described previously.16 The virus was grown and titered on Vero cells (African green monkey kidney; ATCC, Manassas, VA, USA) in DMEM with glucose (4.5 g l−1) supplemented with 10% calf serum at 37 °C in 5% CO2.
Identification of breast cancer stem cells
Vimentin, fibronectin, cytokeratin activity was measured with immunofluorescent staining. Primary human breast cancer cells and foreskin-derived fibroblasts were seeded into 48-well plates at 10 000 cells per well. After overnight incubation, cells were fixed in 4% paraformaldehyde for 15 min at room temperature. Then cells were washed twice with PBS and incubated with 2% BSA and 0.2% Triton X-100 in PBS for 1 h at room temperature. Next, 200 μl of a primary antibody solution was added into each well, cells were incubated overnight at 4 °C. Then cells were washed twice with PBS and incubated with phycoerythrin-labeled secondary antibody for 1 h at room temperature. Finally, cells were stained with hoechst 33342 for 10 min. Immunofluorescence was viewed using an immunofluorescence microscope. CD45 and CD31 activity were measured by flow cytometry with allophycocyanin-conjugated antibodies and phycoerythrin–cyanine dye 7 (Cy7)-conjugated antibodies (both from eBioscience, San Diego, CA, USA), respectively.
SK-BR-3 and human primary breast cancer mammosphere cells and the adherent cells were stained with fluorescein isothiocyanate -labeled anti-CD44 and phycoerythrin-labeled anti-CD24 antibodies (both from Beckman Coulter (Brea, CA, USA) and sorted by flow cytometry (Becton Dickinson, Franklin Lakes, NJ, USA). The Aldefluor assay was performed according to the manufacturer’s suggested protocol (Stemcell Technologies, Vancouver, British Columbia, Canada). Approximately 1 × 106 cells were suspended in 1 ml of Aldefluor assay buffer containing the ALDH substrate BODIPY aminoacetaldehyde. Immediately, 0.5 ml of the mixture was transferred to another tube in the presence of the ALDH inhibitor diethylamino benzaldehyde. The cells were incubated for 30 min at 37 °C and assessed by flow cytometry. Immunofluorescent staining of paraformaldehyde-fixed mammosphere cells of both types was performed with anti-oct4 and anti-sox2 antibodies (both from Santa Cruz Biotechnology, Santa Cruz, CA, USA). ReverTra Ace-α-1 (Toyobo, Osaka, Japan) was used for semi-quantitative reverse transcriptase PCR (RT-PCR) with the following primers:
sox2 forward, 5′-TGCAGTACAACTCCATGACCA-3′;
sox2 reverse, 5′-GTGCTGGGACATGTGAAGTCT-3′;
oct4 forward, 5′-CTCCTGAAGCAGAAGAGGATCAC-3′;
oct4 reverse, 5′-CTTCTGGCGCCGGTTACAGAACCA-3′;
β-actin forward, 5′-CATGTACGTTGCTATCCAGGC-3′;
β-actin reverse, 5′-CTCCTTAATGTCACGCACGAT-3′.23
In vitro cytotoxicity assessment
SK-BR-3 and human primary breast cancer mammosphere cells were seeded in six-well plates at 1 × 105 cells per well. After 24 h incubation at 37 °C, the cells were infected with the virus at a multiplicity of infection (MOI) of 0.1 and 0.01, and controls cells were mock infected. The infected cells were incubated at 37 °C until counting, at which point they were washed twice with PBS, trypsinized and counted using a hemocytometer.
Animal studies
SK-BR-3 mammosphere cells (1 × 106) were implanted in the left flank of 6-week-old female BALB/c nude mice. When the formed tumors reached approximately 5 mm in maximal diameter, 50 μl of the G47Δ virus (1 × 107 plaque-forming units (p.f.u.)) or PBS (mock) was inoculated into the tumor (day 0), followed by repeat injections on days 3, 7 and 10. The three longest dimensions were measured twice a week using an external caliper, and the tumor volume was calculated (length × width × height).
To observe the tumor formation rate of the stem cells, 1 × 103, 1 × 104 and 1 × 105 SK-BR-3 mammosphere cells were implanted in the left flank of 6-week-old female BALB/c nude mice.
All animal procedures were approved by the Animal Care and Use Committee of Sun Yat-sen University.
Tumor tissue analysis by flow cytometry
Tumor tissue was minced and digested for about 12–18 h at 37 °C in DMEM containing 100 U ml−1 collagenase I, 150 U ml−1 hyaluronidase, 10% calf serum and 5 mg l−1 bovine insulin. The digested tissue was strained with a 40-μm strainer, the cell suspension was washed with PBS, the red blood cells were lysed, and then the proportion of CD44+CD24−/low was measured by flow cytometry.
Histological analysis
Tumor tissue was harvested and frozen at −80 °C. Cryostat sections of 5 μm thickness were then prepared and stained with an In Situ β-galactosidase Staining Kit (Beyotime Institute of Biotechnology, Shanghai, China).
Statistical analysis
Data are presented as the mean±standard deviation (s.d.). Independent samples t-test and χ2 test were used to analyze the significance of differences between the two groups. SPSS version 13.0 software (SPSS Inc., Chicago, IL, USA) was used, and a P-value of less than 0.05 was considered significant.
Results
Identification of human primary breast cancer cells
The purity of the primary mammospheres was verified by using flow cytometry and immunostaining. We found that no more than 0.5% of the primary mammospheres were positive for CD31 or CD45 by flow cytometry (Figures 1a and b). These primary mammospheres were negative for fibroblastic markers such as vimentin and fibronectin, whereas these cells strongly expressed cytokeratin (Figures 1c and d).24, 25 Taken together, these observations clarify that these primary mammospheres were prepared with minimal contamination by fibroblast populations, hematopoietic cells or endothelial cell.
Identification of human primary breast cancer cells. Flow cytometric analysis for endothelial marker CD31 (a) and hematopoietic marker CD45 (b) on human breast cancer cells. The percentage of CD31- or CD45-positive cells is indicated. Immunofluorescent staining of vimentin, fibronectin and cytokeratin in primary cancer cells (c) and foreskin-derived fibroblasts (d). Fibroblasts served as a positive control for vimentin and fibronectin. We found that foreskin-derived fibroblasts strongly expressed fibroblastic markers vimentin and fibronectin, but these cells were negative for cytokeratin. In contrast, human primary breast cancer cells strongly expressed cytokeratin, whereas these cells were negative for vimentin or fibronectin. Scale bar, 50 μm.
Identification of breast cancer stem cells
Currently, mammosphere cultures and flow cytometric sorting for the CD44+CD24−/low subpopulation are the main methods for enrichment of breast cancer stem/progenitor cells.4, 26, 27, 28 We used suspension culture of SK-BR-3 and human primary breast cancer cells to generate mammospheres (Figure 2b) in which the CD44+CD24−/low subpopulation was enriched to 99.6±0.07% and 95.3±1.2%, respectively (Figure 2a). The mammosphere cells were then allowed to form adherent cultures, thereby enabling the easy detection of oHSV G47Δ cytotoxicity. The adherent cultures (Figure 2d) of SK-BR-3 and human primary breast cancer cells retained a high proportion of CD44+CD24−/low cells (96.7±1.7%, 92.1±2.5%, respectively; Figure 2c). The difference in the proportion of CD44+CD24−/low cells between the suspended and adherent mammospheres was not found to be statistically significant (P>0.05). Further, under normal conditions, the proportion of mammospheres formed by the SK-BR-3 cells (4.1±0.3%) was significantly higher than that formed by the human primary breast cancer cells (2.7±1.1%) (P<0.05).
Mammosphere cells were analyzed by flow cytometry. (a) The proportion of CD44+CD24−/low cells among the SK-BR-3 mammosphere cells in suspension culture was 99.6±0.07%. (b) Microscopic image of mammosphere in suspension culture. (c) The proportion of CD44+CD24−/low cells among the SK-BR-3 mammosphere cells in adherent culture was 96.7±1.7%. (d) Microscopic image of mammosphere in adherent culture.
To further evaluate the stem cell characteristics of the CD44+CD24−/low population, the expression of Oct4 and Sox2 was examined. The SK-BR-3 and human primary breast cancer cell mammospheres expressed Oct4 and Sox2 protein, as detected by immunofluorescent analysis (Figures 3a and b), and Oct4 and Sox2 mRNA was detected by RT-PCR (Figure 3c).
Stem cell features of mammosphere cells. Immunofluorescent staining of Oct4 (a) and Sox2 (b) in SK-BR-3 mammosphere cells. Oct4 and Sox2 mRNA was detected by RT-PCR (c). Lanes 1–4 show mammospheres of primary breast cancer cells from different tumors, lane 5 shows non-mammosphere cells, lane 6 show mammosphere cells of SK-BR-3, M is the molecular size ladder. β-Actin served as a control for total RNA.
Flow cytometry and the ALDEFLUOR assay for detecting ALDH activity showed the percentage of ALDEFLUOR-positive SK-BR-3 and human primary breast cancer mammospheres to be 37.6±1.5% and 27.3±1.3% respectively. These values were over 10-fold higher than those of the SK-BR-3 and human primary breast cancer cells, which were 2.9±0.5% and 1.5±0.3% respectively (P<0.001; Figure 4). To observe the tumor formation rate of possible stem cells, 1 × 103, 1 × 104 and 1 × 105 SK-BR-3 mammosphere cells and parental cells were implanted in the left flank of 6-week-old female nude BALB/c mice. All mice developed tumors when injected with 1 × 104 or 1 × 105 SK-BR-3 mammosphere cells. However, one of the mice developed tumors when injected with 1 × 105 SK-BR-3 parental cells. This difference was statistically significant and strongly supports the conclusion that the tumor formation rate of mammosphere cells is much higher than that of non-mammosphere cells (Table 1).
In vitro cytotoxicity
G47Δ was found to be highly cytotoxic to both types of mammosphere cells in vitro. Over 50% of the cells were killed by days 3 and 4 when infected with the virus at an MOI of 0.1 and 0.01, respectively (Figure 5, left); similarly, over 90% of the non-mammosphere cells were killed by day 4 when infected with the virus at an MOI of 0.1 and 0.01 (Figure 5, right). The spread of the G47Δ vector in adherent cultures was visualized by X-gal histochemical analysis of the infected cells (Figure 6). Most cells were dead by day 6, because of which the number of X-gal-positive cells detected decreased.
In vitro killing of mammosphere cells and parental cells of SK-BR-3 by G47Δ. Adherent cultured mammosphere cells and parental cells of SK-BR-3 in six-well dishes were infected with G47Δ at an MOI of 0.01 or 0.1 or with PBS (mock), and the average number of cells from duplicate wells is plotted as the percent in the mock wells.
Treatment of tumors in vivo
CD44+CD24−/low cells from the mammospheres formed tumors when injected into the left flank of 6-week-old female nude BALB/c mice. Cells infected with G47Δ (MOI=0.1) before implantation did not form tumors (n=10; followed up until day 58). To evaluate the antitumor efficacy of G47Δ, the established tumors (approximately 5 mm in maximal diameter) were inoculated with the virus (1 × 107 p.f.u.) or PBS (mock) on days 0, 3, 7 and 10. G47Δ treatment significantly inhibited tumor growth, (P<0.05; Figures 7a and c). No mice had apparent tumors on days 21 and 24 after injection with G47Δ. In a separate experiment, mice were killed and X-gal histochemical analysis was performed to detect infected cells indicative of G47Δ replication. Replication was observed even 13 days after a single virus injection (Figure 7b). When tumors were removed from mice 58 days after implantation, the proportion of CD44+CD24−/low cells was reduced to between 3% and 5% in the mock- and oHSV-treated groups, respectively (Figure 8), similar to the level seen initially in non-treated SK-BR-3 cells (data not shown).
Treatment of subcutaneous SK-BR-3 mammosphere-derived tumors. (a) Example of tumors from G47Δ- (lower) or mock-treated (upper) mice at 35 days after treatment. (b) The virus spread in the tumor after intratumoral inoculation. The tumor (1.2 cm3) was injected with G47Δ (1 × 107 p.f.u.), removed 13 days later, sectioned and stained with X-gal to identify replicating G47Δ (blue). (c) SK-BR-3 mammosphere cells were implanted in the left flank of female nude BALB/c mice. when the maximal tumor diameter reached 0.5 cm (29 days after implantation), the mice were injected intratumorally with G47Δ (1 × 107 p.f.u. per 50 μl; n=9) or PBS (mock; n=8) on days 0, 3, 7 and 10 (arrows). Tumor size was measured using an external caliper twice a week, and the tumor volume was calculated. Each data point is the average tumor volume in each group, and error bars represent standard deviation. Tumors treated with G47Δ were significantly smaller than those treated with PBS from 14 days after treatment onward (P<0.05, independent samples t-test).
Single-cell suspensions from mock- and oHSV-treated tumors analyzed by flow cytometry. (a) The proportion of CD44+CD24−/low cells in tumors from mock-treated mice (n=3) was 3.9±0.79%. (b) The proportion of CD44+CD24−/low cells in tumors from oHSV-treated mice (n=2) was 4.5±0.3% (P>0.05, independent samples t-test).
Discussion
Cancer stem cells have been proposed as initiators of cancer and may be responsible for cancer recurrence, development of metastases and resistance to therapy.3, 28, 29 Breast cancer stem cells have been isolated using various techniques, including sorting for cell surface markers, serum-free suspension culture, sorting for side population cells and sorting for ALDH.6, 21, 26, 29, 30, 31 We used serum-free suspension culture to enrich stem cells, which we then detected as the CD44+CD24−/low population and ALDH activity by flow cytometry. The percentage of ALDEFLUOR-positive SK-BR-3 and human primary breast cancer mammospheres are 37.6±1.5% and 27.3±1.3%, respectively, which is significantly higher than those of the SK-BR-3 and human primary breast cancer cells, (P<0.001) and the proportion of CD44+CD24−/low cells in the non-mammosphere cells and mammosphere cells was about 4% and 99%, respectively. The purity of the primary mammospheres is also an important factor, which was verified with minimal contamination by fibroblast populations, hematopoietic cells or endothelial cell by using flow cytometry and immunostaining. The tumor formation rate after implantation of 1 × 103 mammosphere cells in 6-week-old female nude BALB/c mice was up to 50%. Although all the mice developed tumors when injected with 1 × 104 or 1 × 105 SK-BR-3 mammosphere cells, only one of the six mice developed tumors when injected 1 × 105 non-mammosphere cells. Thus, it is clear that mammosphere cells were almost 100-fold more tumorigenic than non-mammosphere cells, indicating that our serum-free suspension culture enriched cancer stem cells. Similar results for SK-BR-3 cells have been reported previously.32
In this study, we found that suspended mammosphere cells tended toward adherent growth in the course of passage, though the reason for this phenomenon is not very clear at present. However, the in vitro cytotoxicity test is easy to conduct because of the phenomenon of adherent mammosphere growth. When mammospheres were cultured in the serum medium, the frequency at which the characteristics of stem cells was observed decreased significantly, proving that the nature of stem cells changes with differentiation. The mammospheres also expressed the stem cell markers Oct4 and Sox2, which supported their stem-like phenotype.
Oncolytic virotherapy has been translated to the clinic, with numerous oncolytic viruses being tested in patients with different cancers.33 This includes studies on oHSV in patients with subcutaneous nodules of recurrent breast cancer.34, 35 Although the breast cancer stem cells were susceptible to G47Δ, it took about 6 days to reduce viability by over 90% when the virus was injected at an MOI of 0.01. Over 90% of the non-stem cells were killed by day 4 when injected at an MOI of 0.1 or 0.01. Thus, the cytotoxicity of G47Δ to CD44+CD24−/low cells was weaker than that to breast cancer cells cultured under standard conditions. Infection of mammospheres with G47Δ at a low MOI blocked their ability to form tumors in vivo. When the tumors were removed from the mice 58 days after implantation, the proportion of CD44+CD24−/low was reduced almost 20-fold, indicating that cancer stem cells differentiate during tumor growth, as has been reported previously.4 Therefore, the bulk of tumor cells are not stem cell-like, and these cells may be more susceptible to oHSV. Under in vivo conditions, G47Δ inhibited the growth of established tumors.
To our knowledge, this is the first report of the treatment of breast cancer stem cells with oHSV. The oHSV vector G47Δ was effective in killing human breast cancer stem cells in vitro and treating tumors in an animal model. The ability of oHSV to target breast cancer stem cells efficiently is an important attribute that supports the possibility of successful clinical translation.
References
Smith RA, Cokkinides V, Brawley OW . Cancer screening in the United States, 2009: a review of current American Cancer Society guidelines and issues in cancer screening. CA Cancer J Clin 2009; 59: 27–41.
Gonzalez-Angulo AM, Morales-Vasquez F, Hortobagyi GN . Overview of resistance to systemic therapy in patients with breast cancer. Adv Exp Med Biol 2007; 608: 1–22.
Lawson JC, Blatch GL, Edkins AL . Cancer stem cells in breast cancer and metastasis. Breast Cancer Res Treat 2009; 118: 241–254.
Al-Hajj M, Wicha MS, Benito-Hernandez A, Morrison SJ, Clarke MF . Prospective identification of tumorigenic breast cancer cells. Proc Natl Acad Sci USA 2003; 100: 3983–3988.
Tanei T, Morimoto K, Shimazu K, Kim SJ, Tanji Y, Taguchi T et al. Association of breast cancer stem cells identified by aldehyde dehydrogenase 1 expression with resistance to sequential paclitaxel and epirubicin-based chemotherapy for breast cancers. Clin Cancer Res 2009; 15: 4234–4241.
Ginestier C, Hur MH, Charafe-Jauffret E, Monville F, Dutcher J, Brown M et al. ALDH1 is a marker of normal and malignant human mammary stem cells and a predictor of poor clinical outcome. Cell Stem Cell 2007; 1: 555–567.
Diehn M, Cho RW, Lobo NA, Kalisky T, Dorie MJ, Kulp AN et al. Association of reactive oxygen species levels and radioresistance in cancer stem cells. Nature 2009; 458: 780–783.
Eriksson M, Guse K, Bauerschmitz G, Virkkunen P, Tarkkanen M, Tanner M et al. Oncolytic adenoviruses kill breast cancer initiating CD44+CD24-/low cells. Mol Ther 2007; 15: 2088–2093.
Fan M, Yan PS, Hartman-Frey C, Chen L, Paik H, Oyer SL et al. Diverse gene expression and DNA methylation profiles correlate with differential adaptation of breast cancer cells to the antiestrogens tamoxifen and fulvestrant. Cancer Res 2006; 66: 11954–11966.
Haraguchi N, Utsunomiya T, Inoue H, Tanaka F, Mimori K, Barnard GF et al. Characterization of a side population of cancer cells from human gastrointestinal system. Stem Cells 2006; 24: 506–511.
Russell SJ, Peng KW . Viruses as anticancer drugs. Trends Pharmacol Sci 2007; 28: 326–333.
Varghese S, Rabkin SD . Oncolytic herpes simplex virus vectors for cancer virotherapy. Cancer Gene Ther 2002; 9: 967–978.
Markert JM, Medlock MD, Rabkin SD, Gillespie GY, Todo T, Hunter WD et al. Conditionally replicating herpes simplex virus mutant, G207 for the treatment of malignant glioma: results of a phase I trial. Gene Ther 2000; 7: 867–874.
Markert JM, Liechty PG, Wang W, Gaston S, Braz E, Karrasch M et al. Phase Ib trial of mutant herpes simplex virus G207 inoculated pre-and post-tumor resection for recurrent GBM. Mol Ther 2009; 17: 199–207.
Mineta T, Rabkin SD, Yazaki T, Hunter WD, Martuza RL . Attenuated multi-mutated herpes simplex virus-1 for the treatment of malignant gliomas. Nat Med 1995; 1: 938–943.
Todo T, Martuza RL, Rabkin SD, Johnson PA . Oncolytic herpes simplex virus vector with enhanced MHC class I presentation and tumor cell killing. Proc Natl Acad Sci USA 2001; 98: 6396–6401.
Liu R, Martuza RL, Rabkin SD . Intracarotid delivery of oncolytic HSV vector G47Delta to metastatic breast cancer in the brain. Gene Ther 2005; 12: 647–654.
Liu RB, Rabkin SD . Oncolytic herpes simplex virus vectors for the treatment of human breast cancer. Chin Med J (Engl) 2005; 118: 307–312.
Liu R, Varghese S, Rabkin SD . Oncolytic herpes simplex virus vector therapy of breast cancer in C3(1)/SV40 T-antigen transgenic mice. Cancer Res 2005; 65: 1532–1540.
Huang MZ, Zhang FC, Zhang YY . Influence factors on the formation of mammospheres from breast cancer stem cells. J Peking Univ (Health Science) 2008; 40: 500–504.
Alvi AJ, Clayton H, Joshi C, Enver T, Ashworth A, Vivanco MM et al. Functional and molecular characterisation of mammary side population cells. Breast Cancer Res 2003; 5: R1–R8.
Li T, Yang Y, Hua X, Wang G, Liu W, Jia C, Tai Y et al. Hepatocellular carcinoma-associated fibroblasts trigger NK cell dysfunction via PGE2 and IDO. Cancer Lett 2012; 318: 154–161.
Huang CY, Pelaez D, Dominguez-Bendala J, Garcia-Godoy F, Cheung HS . Plasticity of stem cells derived from adult periodontal ligament. Regen Med 2009; 4: 809–821.
Akira O, Piyush BG, Dennis CS, Fernando AS, Thierry D, Rizwan N et al. Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 2005; 121: 335–348.
Kalluri R, Zeisberg M . Fibroblasts in cancer. Nature 2006; 6: 392–401.
Ponti D, Costa A, Zaffaroni N, Pratesi G, Petrangolini G, Coradini D et al. Isolation and in vitro propagation of tumorigenic breast cancer cells with stem/progenitor cell properties. Cancer Res 2005; 65: 5506–5511.
Li HZ, Yi TB, Wu ZY . Suspension culture combined with chemotherapeutic agents for sorting of breast cancer stem cells. BMC Cancer 2008; 8: 135.
Phillips TM, McBride WH, Pajonk F . The response of CD24(−/low)/CD44+ breast cancer-initiating cells to radiation. J Natl Cancer Inst 2006; 98: 1777–1785.
Frank NY, Schatton T, Frank MH . The therapeutic promise of the cancer stem cell concept. J Clin Invest 2010; 120: 41–50.
Patrawala L, Calhoun T, Schneider-Broussard R, Zhou J, Claypool K, Tang DG . Side population is enriched in tumorigenic, stem-like cancer cells, whereas ABCG2+ and ABCG2− cancer cells are similarly tumorigenic. Cancer Res 2005; 65: 6207–6219.
Liu R, Wang X, Chen GY, Dalerba P, Gurney A, Hoey T et al. The prognostic role of a gene signature from tumorigenic breast-cancer cells. N Engl J Med 2007; 356: 217–226.
Yu F, Yao H, Zhu P, Zhang X, Pan Q, Gong C et al. Let-7 regulates self renewal and tumorigenicity of breast cancer cells. Cell 2007; 131: 1109–1123.
Aghi M, Martuza RL . Oncolytic viral therapies - the clinical experience. Oncogene 2005; 24: 7802–7816.
Kimata H, Imai T, Kikumori T, Teshigahara O, Nagasaka T, Goshima F et al. Pilot study of oncolytic viral therapy using mutant herpes simplex virus (HF10) against recurrent metastatic breast cancer. Ann Surg Oncol 2006; 13: 1078–1084.
Hu JC, Coffin RS, Davis CJ, Graham NJ, Groves N, Guest PJ et al. A phase I study of OncoVEXGM-CSF, a second-generation oncolytic herpes simplex virus expressing granulocyte macrophage colony-stimulating factor. Clin Cancer Res 2006; 12: 6737–6747.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Li, J., Zeng, W., Huang, Y. et al. Treatment of breast cancer stem cells with oncolytic herpes simplex virus. Cancer Gene Ther 19, 707–714 (2012). https://doi.org/10.1038/cgt.2012.49
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cgt.2012.49
Keywords
This article is cited by
-
Triple-negative breast cancer: new perspectives for novel therapies
Medical Oncology (2013)