The main clinical presentation of patients with oral, pharyngeal, or esophageal motility disorders is dysphagia. Dysphagia caused by oral and pharyngeal disorders can be differentiated from dysphagia due to esophageal disorders, based on the patient's localization of the site of the difficulty to the mouth and throat, or chest, respectively. Although dysphagia due to esophageal lesions may sometimes be localized to the throat, dysphagia due to oral or pharyngeal causes does not localize to the chest. The most distinguishing feature of dysphagia due to pharyngeal causes is the misdirection of food into the nose or the lungs, resulting in the complaint of nasal regurgitation of food and choking and coughing during swallowing. The oral cavity, pharynx and upper esophagus are often involved together due to the underlying neuromuscular disorders. Painful swallowing or odynophagia occurs in certain inflammatory conditions of the oral, pharyngeal, or esophageal mucosa.
Regurgitation of gastric contents into the esophagus suggests incompetence of the normal gastroesophageal antireflux barrier. Heartburn is a typical symptom of esophageal mucosal inflammation due to gastric acid-peptic reflux.
Motor Disorders of the Oral Cavity, Pharynx, and Cervical Esophagus
Muscles of the oral cavity, pharynx, and cervical esophagus are of the striated variety. These disorders may manifest as oral stasis of food, inability to initiate a swallow, premature spillage of food into the pharynx, pharyngeal stasis, nasal regurgitation, or laryngeal aspiration. A large number of neuromuscular diseases are associated with dysfunction of the oropharyngeal phase of deglutition. These can be classified by whether the disease affects the central nervous system, such as stroke, cerebral palsy, head injury, amyotrophic lateral sclerosis, multiple sclerosis, and Parkinson's disease; the peripheral nervous system, such as poliomyelitis; neuromuscular transmission, such as myasthenia gravis; and striated muscles, such as muscular dystrophy, polymyositis, and metabolic myopathies including hypo- and hyperthyroidism.
Stroke is the most common cause of oral and pharyngeal dysphagia. Patients with suspected oral and pharyngeal dysphagia should undergo a careful neurologic examination looking for signs of underlying neuromuscular disease. Further evaluation requires a barium videofluoroscopy. Otolaryngology evaluation and laryngoscopy may be helpful in ruling out structural abnormalities. Speech-language pathologists with special training in swallowing assessment and therapy are helpful in the evaluation and management of these patients. If the disease is severe enough to cause weight loss or aspiration pneumonia, the patient may require placement of a feeding gastrostomy or jejunostomy.
Motor Disorders of the Thoracic Esophagus and Lower Esophageal Sphincter (LES)
In humans, thoracic and abdominal parts of the esophagus including the LES are composed of smooth muscles and are affected by different diseases from those affecting the cervical esophagus. When used without qualification, the term esophagus implies the thoracic (smooth muscle part) esophagus. Motor disorders of the esophagus generally affect both the esophageal body and the LES; however, either the body or the sphincter may be predominantly affected.
Based on pathophysiology, motor disorders of the smooth muscle portion of the esophagus and the LES can be due to defects in the inhibitory nerves, excitatory nerves or smooth muscles. Disorders of inhibitory innervation include achalasia, diffuse esophageal spasm, and transient lower esophageal sphincter relaxation (TLESR). Increased function of excitatory innervation includes hypertensive peristalsis and hypertensive and hypercontracting LES, and decreased function of excitatory innervation of the smooth muscle includes hypotensive peristalsis, hypotensive LES, and decreased reflex LES contraction.
Achalasia
Achalasia is due to deficiency of inhibitory neural influence that involves both the esophageal body and the LES. It is characterized by nonperistaltic contractions in the smooth muscle segment of the esophagus and absent, incomplete, or abnormally timed LES relaxation in response to swallowing. These abnormalities result from loss of deglutitive inhibition that is responsible for the peristaltic sequence of esophageal contractions and relaxation of the LES, due to defective inhibitory nerves. Resting LES pressures may also be elevated due to unopposed action of the excitatory nerves. Impaired relaxation of the LES causes functional obstruction and progressive esophageal dilation, stasis of food, and secondary elevation in basal intraesophageal pressures.
Achalasia is usually caused by degeneration of the postganglionic inhibitory nitric oxide/vasoactive intestinal peptide neurons in the myenteric plexus. Postganglionic excitatory neurons may also be affected in advanced cases. The etiology of the majority of cases seen in the United States is not known; therefore, these cases are labeled as primary or idiopathic. There are many causes of secondary achalasia. In South America, the parasite Trypanosoma cruzi is endemic and it causes achalasia by destroying myenteric neurons with immunoinflammation (Chagas' disease). The term pseudoachalasia should be reserved for cases that may appear like achalasia but lack the basic pathology of achalasia, for example, extrinsic compression at the gastroesophageal junction by tumors or inflammatory masses.
The main symptom of achalasia is dysphagia that is often to both liquids and solids. Dysphagia is mainly localized to the lower chest but sometimes it may also be localized to the neck. Regurgitation of food retained in the esophagus without gastric acid is also frequent. In advanced cases nocturnal regurgitation may lead pulmonary aspiration. Weight loss also occurs in advanced cases. Many patients also complain of chest pain, and heartburn-like symptoms may occur. Chest pain may be due to esophageal distention or excessive muscle contraction. Heartburn may be due to lactic acid formed by fermentation of stagnant food in the esophagus, esophageal distention, or esophageal muscle contraction. Gastroesophageal reflux does not occur in the presence of achalasia.
Diagnosis of achalasia is often suspected by clinical symptoms. The chest x-ray may reveal a widened mediastinum and air-fluid level in the esophagus due retained food, fluid, and air. The barium swallow shows a dilated esophagus with a fluid level and characteristic bird-beak-like narrowing of the gastroesophageal junction. Administration of a smooth muscle relaxant such as sublingual nitroglycerin causes relaxation of the LES and may help distinguish achalasia from pseudoachalasia due to mechanical causes. Esophageal motility studies show nonperistaltic contractions and impaired relaxation of the LES. Basal esophageal body and LES pressure may be elevated.
Treatment of achalasia is directed at removing the functional obstruction caused by nonrelaxing LES. Drugs that relax the LES (e.g., calcium channel blockers, nitrates, phosphodiesterase inhibitors, and anticholinergics) may alleviate symptoms in a small subset of patients. Injection of botulinum toxin into the LES has also been demonstrated to be efficacious, although this needs to be repeated periodically and is generally reserved for elderly patients with comorbidities. Rupture of the LES muscle by pneumatic dilation is a commonly used treatment. It is successful in alleviated dysphagia and improving esophageal emptying in the majority of patients, although repeat dilation may be required to achieve the highest success rate. Surgical incision of the LES (Heller myotomy) performed laparoscopically has replaced that performed by open surgery. The surgical procedure is effective and is often performed when pneumatic dilation fails. Gastroesophageal reflux disease may complicate successful surgery or even pneumatic dilation.
Diffuse Esophageal Spasm
Diffuse esophageal spasm (DES) is characterized by replacement of normal peristaltic contraction by nonperistaltic contractions. Nonperistaltic contractions are not effective in causing normal esophageal transit. It is due to loss of deglutitive inhibition associated with the impairment of inhibitory nerve function that is localized to the esophageal body. The LES relaxation is normal. The impairment is usually mild, particularly in early cases. Some cases of DES may progress to achalasia. The cause of the impairment is not found in many cases (idiopathic), but it is suspected that a large number of disorders, including stress, may cause inhibitory nerve dysfunction.
Dysphagia to solids and liquids and chest pain are the usual presenting symptoms. The barium swallow may be normal or show nonpropagated contractions (also called tertiary contractions). In advanced cases the barium swallow may reveal a corkscrew esophagus and pseudodiverticula. The diagnosis is best made by an esophageal motility study. A diagnosis of DES is made when greater than 20% swallow-induced contractions are nonperistaltic. Occasional nonperistaltic contraction can occur normally. The amplitude of the nonperistaltic contractions may be increased or normal or even decreased. Sometimes contractions are multipeaked, and spontaneous contractions unassociated with swallowing may be present. Management involves reassurance and the use of smooth muscle relaxants.
Hypertensive Peristalsis, Hypercontracting LES, and Hypertensive LES
These are manometric diagnoses without clear clinical correlates. They are diagnosed when the amplitude of peristaltic contractions, after-contraction of the LES, or basal LES pressure exceeds the normal values. These disorders may result from overactivity of the excitatory nerves. Stress may cause hypertensive peristaltic contractions. Hypertensive peristalsis is the most frequent manometric finding in patients referred for evaluation of noncardiac, angina-like chest pain. Esophageal transit is normal. These patients, however, are often found to have esophageal hypersensitivity. Treatment with nitrates and calcium channel blockers has been used but with no proven benefit.
Inappropriate Transient LES Relaxation
Swallowing is associated with transient LES relaxation and esophageal peristaltic contraction. Transient LES relaxation also normally occurs during the belching reflex, but may also occur without obvious belching. Such episodes of inappropriate transient LES relaxation may be associated with gastroesophageal reflux. The reflex transient LES relaxation is mediated by inhibitory motor nerves, and its increased frequency may lead to gastroesophageal reflux disease (GERD). Diagnosis of transient LES relaxation can only be made on long-term manometric recordings that are usually employed in research but not in clinical practice.
Hypotensive Esophagus
Hypotensive esophagus is characterized by reduced basal LES pressure and reduced force of the esophageal peristaltic contractions. It may be caused by muscle atrophy and diseases or impairment of cholinergic input or both these factors. Reduced force of the peristaltic contractions results in ineffective transport of the swallowed food, resulting in dysphagia to solids. Liquids may move by gravity in the upright position but may cause difficulty in the recumbent position. Reduced LES basal tone promotes gastroesophageal reflux leading to GERD. Often LES hypotension exists without hypotensive esophageal peristaltic contractions. The precise etiology of hypotensive esophagus or hypotensive LES remains unknown in most cases. Important secondary causes are esophageal involvement in scleroderma and other connective tissue diseases, and the use of drugs with anticholinergic properties. Esophageal involvement is common in patients with scleroderma. This may occur even in the absence of obvious skin and joint involvement, although in such cases Raynaud's phenomenon is usually present. Microvessel disease and fibrosis in scleroderma and other connective tissue disorders may lead to intramural neuronal dysfunction and muscle atrophy.
Ineffective Esophageal Clearance
Ineffective esophageal clearance of food or other contents can occur with hypotensive contractions or nonperistaltic contractions (diffuse esophageal spasm) or absence of peristaltic contraction due to loss of the swallowing reflex. Ineffective esophageal clearance can be documented by proper videofluoroscopic examination of the esophagus. Recently, esophageal impedance studies have been shown to provide similar information. Peristaltic contractions of amplitude <30 mmHg are ineffective in propelling esophageal contents. Increased frequency (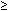 30%) of low-amplitude (<30 mmHg) peristaltic contractions or nonperistaltic contractions in the distal esophagus following wet swallows may be associated with symptoms of dysphagia. However, they are common manometric abnormalities found in patients with reflux esophagitis, and can also be found in patients without evidence of reflux disease.
30%) of low-amplitude (<30 mmHg) peristaltic contractions or nonperistaltic contractions in the distal esophagus following wet swallows may be associated with symptoms of dysphagia. However, they are common manometric abnormalities found in patients with reflux esophagitis, and can also be found in patients without evidence of reflux disease.
Gastroesophageal Reflux Disease
Gastroesophageal reflux disease occurs as a complication of ineffective antireflux barriers at the gastroesophageal junction. The ineffective antireflux barriers may be compromised because of the hypotension and increased frequency of transient LES relaxation. Dislocation of the LES in the thorax and hiatus hernia may also impair LES competence. Impaired esophageal clearance of the refluxed gastric contents due to hypotensive or nonperistaltic contractions may worsen the esophageal mucosal injury caused by acid reflux. Gastroesophageal reflux disease is associated with symptoms of heartburn and regurgitation. Some cases have symptoms due to pharyngeal and laryngeal factors, and pulmonary symptoms due to gastric acid injury. In severe cases, esophageal bleeding, peptic stricture, and intestinal metaplasia with its associated complications may occur.
Heartburn and Esophageal Chest Pain
The symptom of heartburn is characteristic of reflux esophagitis, and esophageal chest pain resembling cardiac pain (noncardiac chest pain) occurs in achalasia and diffuse esophageal spasm. Many patients with heartburn or noncardiac chest pain have no or minimal esophageal motility abnormality. In these cases the symptoms may be due to hypersensitivity of esophageal nociceptive mechanisms.


