Abstract
Study design:
Clinical practice guidelines.
Objectives:
The project objectives were to develop the first Canadian recommendations on a model of care for the management of at- and below-level neuropathic pain in people with spinal cord injury (SCI).
Setting:
The guidelines are relevant for inpatient and outpatient SCI rehabilitation settings in Canada.
Methods:
On the basis of a review of the Accreditation Canada standards, the Steering Committee developed questions to guide the CanPainSCI Working Group when developing the recommendations. The Working Group agreed on recommendations through a consensus process.
Results:
The Working Group developed five recommendations for the organization of neuropathic pain rehabilitation care in people with SCI.
Conclusions:
The Working Group recommendations for a model of care for at- and below-level neuropathic pain after SCI should be used to inform clinical practice.
Similar content being viewed by others
Introduction
An international panel of experts—the CanPainSCI Working Group (WG)—was formed to develop the first Canadian Clinical Practice Guidelines to inform the management of neuropathic pain (NP) in people with spinal cord injury (SCI) in an inpatient and outpatient rehabilitation setting. Using a consensus-based, modified Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach, the CanPainSCI Working Group made recommendations for three specific areas of management: screening and diagnosis, treatment and model of care.1 This paper focuses on the area of model systems of care for managing SCI-related NP.
What is a model of care?
At its most basic, a model of care is a method of health-care delivery.2 The overall goal of developing a model of care is to ensure that patients’ needs are met throughout the course of their illness or condition. Davidson and Elliott3 have proposed several essential elements of models of care. A model of care should be evidence based, address patient and health-care provider needs, incorporate consultation with stakeholders (such as patients and clinicians) utilize a multidisciplinary approach and outcomes evaluation, consider optimal and equitable access and resource utilization, and include appropriate and culturally sensitive interventions. A comprehensive and systematic process is required to develop a model of care.4 This process needs to facilitate both quality improvement and change management, throughout the entire spectrum of planning, developing, implementing, evaluating and assessing the sustainability of the model. According to Spinal Cord Injury Rehabilitation Evidence, no internationally accepted definition or essential elements of SCI rehabilitation has yet been formulated.5 In fact, the field of SCI rehabilitation has been referred to as a ‘black box,’ whereby the lack of working definitions and/or standardized guidelines has contributed to a lack of cohesion of the field to more established domains of medicine.6
The need for a Canadian model system of care for SCI-related pain
Advances in SCI care in Canada include the development of national standards for SCI rehabilitation services by Accreditation Canada.7 Although these standards contain suggestions for developing models of care for this patient population, none is specific to the management of NP.
In Canada, the delivery of health care is not under the auspice of the federal government. Rather, the individual provinces and territories establish their own models of care following the core standards of the Canada Health Act.8 In Canada, differences in health system structures and resources for care delivery, both across and within provinces, complicate the development of a national model system to manage NP after SCI. As a result, health-care policy may require changes to meet the needs of patients with SCI-related NP, with an emphasis on providing resources to support access to care in the community.
A recent environmental scan of the status of SCI rehabilitation in Canada (N=12 rehabilitation centers) found significant regional differences, within and across provinces, in access to outpatient pain management services, wait times for service and the use of guidelines for NP treatment.9 Differences in NP identification and management and the regional availability of resources highlight the need to use standardized outcomes, implement current evidence and practice guidelines, develop interdisciplinary pain management teams and perform additional clinical research into effective pain management.
A variety of models of care exists for chronic pain in general. The specialized issues of the SCI population, however, require a delivery system specific to SCI-related NP to advance best practices and provide optimal care. One model of care proposed in a French clinical practice guideline for neuropathic pain after SCI suggests that collaborations between physical medicine and rehabilitation specialists managing SCI, and specialists managing pain, are essential.10 The appropriate extent and type of this collaboration depends on the complexity of the patient’s pain presentation.
On the basis of the need for organizing the field of SCI-related NP, the CanPainSCI WG led by a Steering Committee-initiated recommendations for the management of pain post SCI. The lack of existing models that are feasible for the Canadian SCI setting10 required a process that would identify existing resources and expertize to develop a national model system of care specific to NP after SCI rehabilitation.
Primary objective
Our aim is to develop recommendations for a national model system of care specific to the management of NP after SCI rehabilitation, which could guide the delivery of efficient and effective services to meet the needs of patients with SCI-related NP.
Materials and Methods
The Model of Care Working Group (MCWG) was formed using the methodology described in the overview paper. The Steering Committee provided the MCWG with the following questions, based on a literature search, to guide the formulation of recommendations: (1) What is the optimal model for delivery of care for individuals with NP after SCI? (2) What is the composition of the team for an inpatient or outpatient rehabilitation setting? (3) When is it appropriate to release the patient from specialized care?
The Steering Committee searched MEDLINE, PsycINFO, EMBASE and CINHAL using the following search terms: models of care; health-care delivery; spinal cord injury; and neuropathic pain. As published data on models of care for SCI-related NP were lacking, the Steering Committee examined gray literature, including Spinal Cord Injury Research Evidence11 Accreditation Canada,8 working documents from projects being conducted by group members and the Veterans Health Administration Handbook.12 The MCWG met several times to discuss the topic, draft the recommendations and reach consensus on them. The full CanPainSCI WG then discussed, revised and voted on the recommendations during the face-to-face meeting. Only those recommendations receiving at least 75% agreement were adopted and are included here. The MCWG added practical considerations to expand upon the recommendations and support their implementation.
Results
The MCWG developed five recommendations addressing the delivery of care for SCI-related NP within a rehabilitation setting. Considerations have been included with each recommendation to aid implementation.
Recommendation 3.1
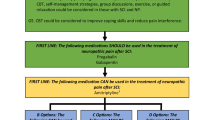
Delivery of care for neuropathic pain in people with spinal cord injury should be (1) coordinated, (2) interprofessional, (3) timely, (4) patient centered, (5) using a biopsychosocial framework and (6) evidence based.
Type of evidence: Expert opinion.
Considerations
Numerous factors affect the presentation of chronic pain, including psychosocial and environmental factors.13 Conversely, chronic pain can significantly affect function, mood and social relationships. Therefore, management of chronic pain after SCI in patients with complex presentations requires an interprofessional or interdisciplinary team approach that incorporates medical, physical, educational and cognitive-behavioral components. Communication between health-care providers, between health-care providers and administration, and between health-care providers and the patient is a central tenet of coordination of care services.
A biopsychosocial framework should guide the structure of a program and individual care plans. This model considers the interplay between physiology, psychology and social factors on the pain experience that affects NP outcomes for people with SCI.13
As proposed by Strauss et al.,14 evidence-based decisions are essential to advancing practice, with priority given to SCI-specific guidelines and studies.
Recommendation 3.2
A person with spinal cord injury and either (1) new onset or worsening spinal cord injury-related neuropathic pain, and/or (2) ongoing pain that is difficult to manage and/or (3) dissatisfaction with their current pain management protocol should be screened and assessed by a clinician with experience in managing people with spinal cord injury.
Type of evidence: Expert opinion.
Considerations
It is essential to involve clinicians with SCI experience when working with patients who have SCI-related NP, who present with any of the conditions outlined in Recommendation 3.2. A clinician with SCI experience can recommend relevant referrals, assessments, investigations and treatment steps as appropriate. If necessary, on the basis of the results of the assessment, then this individual can act as a gatekeeper to team-based care for SCI-related NP. If a diagnostic workup is required to determine the etiology or triggers of NP after SCI, it is essential to involve the rehabilitation medicine specialist to ensure that relevant conditions are considered and appropriate investigations implemented.
Recommendation 3.3
Multidisciplinary care coordinated through a spinal cord injury rehabilitation team is recommended when significant functional impacts and/or significant psychological comorbidity factors resulting from neuropathic pain need to be addressed. Further, a detailed plan of care shared among health-care providers needs to be implemented across primary, secondary and tertiary services.
Type of evidence: Expert opinion.
Considerations
It is important to recognize that pain management strategies should also address the functional and psychological impacts of pain, as current treatments may not eliminate pain or even reduce it effectively. As patients should expect to live with some degree of pain and discomfort, it is essential that they learn to minimize the impact of these symptoms on their daily life. Generally, delivery of comprehensive care through an SCI rehabilitation team has been shown to be central to improving SCI outcomes. Access to such a team is therefore essential to managing complex functional impacts and/or psychological comorbidity more effectively. Currently, implementation of specialized treatments may require access to a specialized pain clinic. Open communication and coordination between pain specialists and the SCI specialist team is required. Moving forward, we recommend that, given the unique needs of the SCI population, these treatment options be available at SCI-specific rehabilitation facilities.
As patient needs evolve, team members may change over time.15 The team approach to patient care can improve access to care, quality of care and cost effectiveness. The team approach is effective in increasing diagnostic accuracy and timeliness of treatment, which can improve health outcomes and patient satisfaction while increasing resource utilization efficiency and job satisfaction for clinicians. In addition, the team approach can streamline communication with patients and families. It is also important to consider the role of telemedicine, e-consult and other forms of distance communication to allow staff from specialized rehabilitation centers to continue to provide oversight when travel is a barrier to optimal care delivery, such as may occur for patients in rural areas.
The multidisciplinary team should develop a detailed and integrated rehabilitation care plan that includes a focus on NP in alignment with Accreditation Canada 2014 standards.7 Multidisciplinary care should take a patient-centered, goal-directed, holistic and functional approach to pain management that incorporates the caregiver and/or significant other in the care plan. Members of the multidisciplinary team should include the various rehabilitation disciplines such as physiatry, physiotherapy, occupational therapy, psychology, social work, nursing and other professionals as needed.
Recommendation 3.4
A person with neuropathic pain as a result of spinal cord injury should be discharged from specialized care when three conditions are met: (1) a stable plateau has been reached in pain severity and/or pain-related functional status; (2) an ongoing plan linked to resources and provider follow-up is in place; and (3) self-management techniques have been taught.
Type of evidence: Expert opinion.
Considerations
The goal at discharge from specialized care should be stable pain severity and optimized function relative to a person’s ongoing pain severity. Complete alleviation of pain is not usually a realistic outcome. A stable plateau may be considered to have been reached when the care providers and the patient feel maximal gains have been reached, given the available time and resources, in managing pain and its impact on everyday functioning. Periodic reassessments by specialized care providers may be appropriate after discharge to ensure stability of pain management.
The discharge plan, which is part of the ongoing care plan for NP management, must be available to the patient before discharge from rehabilitation, and the patient must be educated about its elements. The plan must also be provided to any postdischarge care providers at discharge and especially to the provider assuming primary management of the patient. Useful items to include in the discharge plan, depending on the complexity of the case and the team members involved in care, are current medication, a medication titration plan, a plan for future pain management, nonpharmacologic treatment modalities, scheduled ongoing rehabilitation visits, and suggestions for the timing of follow-up and re-referral to rehabilitation. As much as possible, a discharge plan should also remove barriers to accessing services and identify appropriate community resources for each patient. It is often possible to identify suitable resources by working with partner organizations and allied services.
It is essential to integrate the principles of self-management into the discharge plan and patient education, to support maintenance of a patient’s function and stability of pain management after discharge. Self-management interventions commonly involve psychoeducation to develop or improve self-efficacy skills in goal setting, problem solving, management of psychological consequences, medication management, symptom management, social support and communication.16, 17 Techniques should be (1) demonstrable or actionable by the patient, (2) matched to the patient’s abilities and (3) linked to further community support. The goal of self-management education is to equip the patient to manage pain as independently as possible.
Recommendation 3.5
The spinal cord injury rehabilitation team should engage in continuous quality improvement, including evaluation and feedback efforts regarding their pain management practices based on patient outcomes.
Type of evidence: Expert opinion.
Considerations
Evaluation of practice supports accountability and improvement. The subjective nature of pain and the challenging nature of successful pain management make continuous quality improvement critical to ensuring that patient needs continue to be met and that resources are used appropriately. Essential elements of a quality improvement program are process and outcome indicators to demonstrate the status of practice change. Process indicators such as monitoring measure implementation of a process by intent and by target. Outcome indicators such as reduction in intensity of a patient’s pain over time using the International Spinal Cord Injury Pain Basic Data Set element on pain intensity measure change produced by practice activities.18
Discussion
The recommendations within this section provide the essential elements and principles of a model of care for the management of at- and below-level NP after SCI. Although resources and health-care systems may differ between sites, patient flow and principles of care should be guided by these recommendations. The goal of these recommendations is to ensure that the needs of the patient are met while ensuring that resources are efficiently managed.
Although evidence for models of care for the management of SCI-related NP is lacking, an extensive literature on models for care organization for the management of chronic noncancer pain may provide some insights.19, 20 These models focus on multidisciplinary or interdisciplinary care. The biopsychosocial model, which acknowledges the impact of the interplay between physiology, psychology and social factors on the pain experience, forms the basis of this care.19 Multidisciplinary and interdisciplinary care comprises patient education, medical and behavioral therapy, and physical reconditioning, with a goal of rehabilitation, rather than cure, as cure is not often possible.
Multidisciplinary care may not be appropriate for all patients with SCI NP, but access to this type of care when needed is essential in this population. People with SCI-related NP face specific issues that differ from those with other chronic pain syndromes, which may further complicate management. An SCI rehabilitation team should assess and address the functional impact of NP on activities of daily living when necessary.
Numerous factors complicate the management of SCI-related NP, including our incomplete understanding of SCI-related NP,21 the lack of evidence for most treatments, including optimal treatment selection and sequencing and combination therapy,22 the potential for the development of treatment resistance23 and the need to consider the biological and psychological contributors to NP. In addition, because the goal of treatment is optimizing functional status despite residual pain, team-based care and self-management education have an important role in helping patients with SCI-related NP improve both pain coping skills and functional adaptation.
Conclusion
Despite the lack of evidence for specific models of care, the CanPainSCI WG felt that it was critical to develop guidelines addressing principles of care delivery to guide the development of models of care. Appropriate models of care to manage SCI-related NP should ensure that patient needs are met, care is evidence based, resources are efficiently managed, access to care is equitable, patients are referred for multidisciplinary care and/or specialized assessment as necessary and discharged from specialized care at an appropriate time, and both adequate and appropriate resources are in place at discharge.
Data archiving
There were no data to deposit.
References
Schünemann H, Brożek J, Guyatt G, Oxman A (eds). GRADE Handbook for Grading Quality of Evidence and Strength of Recommendations. Updated October 2013. The GRADE Working Group, 2013. Available at http://gdt.guidelinedevelopment.org/app/handbook (accessed on 13 July 2015).
What is a model of care? Arthritis, Bone and Joint Disease. Available at http://modelsofcare.ca/index.html (accessed on 13 August 2015).
Davidson PM, Elliott D . Managing approaches to nursing care delivery. In: Daly, J, (ed.). Preparing for professional nursing practice. Sydney, Australia: MacLennan and Petty. 2001, 123.
Davidson P, Halcomb E, Hickman L, Phillips J, Graham B . Beyond the rhetoric: what do we mean by a 'model of care'? Aust J Adv Nurs 2006; 23: 47–55.
What is SCI Rehabilitation. Available at http://www.scireproject.com/rehabilitation-evidence/rehabilitation-practices/what-sci-rehabilitation (accessed on 13 August 2015).
Whiteneck G, Gassaway J, Dijkers M, Jha A . New approach to study the contents and outcomes of spinal cord injury rehabilitation: the SCI Rehab Project. J Spinal Cord Med 2009; 32: 251–259.
Accreditation Canada. Standards: Spinal Cord Injury Rehabilitation Services 2014. Available at https://accreditation.ca/spinal-cord-injury-rehabilitation-services (accessed on 5 October 2015).
Canada Health Act. Available at http://www.hc-sc.gc.ca/hcs-sss/medi-assur/cha-lcs/index-eng.php (accessed 13 January 2016).
Craven C, Verrier M, Balioussis C, Wolfe D, Hsieh J, Noonan V et al. Rehabilitation Environmental Scan Atlas: Capturing Capacity in Canadian SCI Rehabilitation. Rick Hansen Institute: Toronto, ON, Canada. 2012.
Salle JY, Ginies P, Perrouin-Verbe B, Ventura M . Pain management: what's the more efficient model? Ann Phys Rehabil Med 2009; 52: 203–209.
Spinal Cord Injury Rehabilitation Evidence. SCIRE Project website http://www.scireproject.com/.
Department of Veterans Affairs. VHA Handbook 1176.01 Spinal Cord injury and Disorders (SCI/D) System of Care. Department of Veterans Affairs, Washington DC, USA; 2011. Available at http://www.va.gov/vhapublications/ViewPublication.asp?pub_ID=2365 (accessed on 5 October 2015).
Siddall PJ, Middleton JW . Pain following spinal cord injury In: Chhabra HS (ed.). ISCoS Textbook on Comprehensive Management of Spinal Cord Injuries. Wolters Kluwer: Gurgaon, India. 2015 pp 825–848.
Straus SE, Richardson WS, Glasziou P, Haynes RB . Evidence-Based Medicine: How to Practice and Teach EBM 3rd edn Churchill Livingstone: Edinburgh, UK. 2005.
Marshall R, Hasnan N . Team-based care In: Chhabra HS (ed.). ISCoS Textbook on Comprehensive Management of Spinal Cord Injuries. Wolters Kluwer: Gurgaon, India. 2015, 414–422.
Barlow J, Wright C, Sheasby J, Turner A, Hainsworth J . Self-management approaches for people with chronic conditions: a review. Patient Educ Couns 2002; 48: 177–187.
Lorig KR, Ritter PL, Dost A, Plant K, Laurent DD, McNeil I et al. The Expert Patients Programme online, a 1-year study of an internet-based self-management programme for people with long-term conditions. Chronic Illn 2008; 4: 247–256.
Widerström-Noga E, Biering-Sørensen F, Bryce TN, Cardenas DD, Finnerup NB, Jensen MP et al. The International Spinal Cord Injury Pain Basic Data Set (version 2.0). Spinal Cord 2014; 52: 282–286.
Jeffery MM, Butler M, Stark A, Kane RL . Multidisciplinary Pain Programs for Chronic Noncancer Pain. Technical Brief No. 8. (Prepared by Minnesota Evidence-based Practice Center under Contract No. 290-07-10064-I). Agency for Healthcare Research and Quality: Rockville, MD, USA. 2011, AHRQ Publication No. 11-EHC064-EF.
Pergolizzi J (ed). Towards a Multidisciplinary Team Approach in Chronic Pain Management. Available at http://www.pae-eu.eu/wp-content/uploads/2013/12/Multidisciplinary-approach-in-chronic-pain-management.pdf (accessed on 16 November 2015).
Siddal PJ . Management of neuropathic pain following spinal cord injury: now and in the future. Spinal Cord 2009; 47: 352–359.
Hagen EM, Rekand T . Management of neuropathic pain associated with spinal cord injury. Pain Ther 2015; 4: 51–65.
Kumar A, Pahwa D, Rinwa P . Management of neuropathic pain: challenges and opportunities. Int J Res Dev Pharm L Sci 2013; 3: 734–740.
Acknowledgements
Funding for the research and publication of this supplement is provided by the Ontario Neurotrauma Foundation and the Rick Hansen Institute in their mission to advance the care of people with spinal cord injury (#PM2 964). We thank Joanna Gorski for her help with manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
BL has received consulting fees from the Northern Regional Health Authority (2014 to 2016), founded the CHANGEpain Clinic, has received fees for lecturing from DePuy and has served as expert witness. CO’C has received consulting fees from Bonify (2015–current), Lilly (2014) and Allergan (2013–current), has received lecture fees from Allergan, Biogen, Purdue, Lilly, Tweed, Tilray, Quality Respiratory Care and Respironics, CO’C has received grant support from Cytokinetics (2013–current), Biogen (2010–current), Acorda (2005–2010; 2015–current), Allergan (2010–current) and Sensimat 2015 and has served as expert witness on disability, at request of third parties including CMPA, insurance companies and law firms. TNB has received grant support from the Craig Neilsen Foundation (2015) and Allergan (2015). CC has received consulting fees from Allergan (2013) and the Rick Hansen Institute (2013), has received grant support from the Rick Hansen Institute (2014–2016), the Ontario Neurotrauma Foundation (2011–2018), the Canadian Institutes for Health Research (2008–2016) and the Rick Hansen Institute & SCI Solutions Network (2012–2015). NF has received grant support from IMI Europain (EU/EFPIA, 2009–2015). DM has received consulting fees from Johnson and Johnson (2014), fees for lecturing from Lilly (2014), Merck-Frosst (2014) and Purdue Pharma (2013), has received grant support from Pfizer (2009–2014) and has received book royalties from Cambridge University Press. PS has received grants from the Australian & New Zealand College of Anesthetists (2015) and the New South Wales state government (2013–2015), and holds a patent for a system and method for detecting pain and its components using magnetic resonance spectroscopy, US Patent 08755862, granted 17 June 2014. RT has received grant support (2013–2016) and lecture fees (2015) from Allergan. The remaining authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Guy, S., Mehta, S., Harvey, D. et al. The CanPain SCI Clinical Practice Guideline for Rehabilitation Management of Neuropathic Pain after Spinal Cord: recommendations for model systems of care. Spinal Cord 54 (Suppl 1), S24–S27 (2016). https://doi.org/10.1038/sc.2016.91
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2016.91
This article is cited by
-
Neuropathic Pain and Spinal Cord Injury: Management, Phenotypes, and Biomarkers
Drugs (2023)
-
The CanPain SCI clinical practice guidelines for rehabilitation management of neuropathic pain after spinal cord injury: 2021 update
Spinal Cord (2022)
-
Physical activity interventions, chronic pain, and subjective well-being among persons with spinal cord injury: a systematic scoping review
Spinal Cord (2021)