Abstract
Study design:
Cross-sectional validation study.
Objectives:
To develop and validate a self-report version of the Spinal Cord Independence Measure (SCIM III).
Setting:
Two SCI rehabilitation facilities in Switzerland.
Methods:
SCIM III comprises 19 questions on daily tasks with a total score between 0 and 100 and subscales for ‘self-care’, ‘respiration & sphincter management’ and ‘mobility’. A self-report version (SCIM-SR) was developed by expert discussions and pretests in individuals with spinal cord injury (SCI) using a German translation. A convenience sample of 99 inpatients with SCI was recruited. SCIM-SR data were analyzed together with SCIM III data obtained from attending health professionals.
Results:
High correlations between SCIM III and SCIM-SR were observed. Pearson’s r for the total score was 0.87 (95% confidence interval (CI) 0.82–0.91), for the subscales self-care 0.87 (0.81–0.91); respiration & sphincter management 0.81 (0.73–0.87); and mobility 0.87 (0.82–0.91). Intraclass correlations were: total score 0.90 (95% CI 0.85–0.93); self-care 0.86 (0.79–0.90); respiration & sphincter management 0.80 (0.71–0.86); and mobility 0.83 (0.76–0.89). Bland–Altman plots showed that patients rated their functioning higher than professionals, in particular for mobility. The mean difference between SCIM-SR and SCIM III for the total score was 5.14 (point estimate 95% CI 2.95–7.34), self-care 0.89 (0.19–1.59), respiration & sphincter management 1.05 (0.18–2.28 ) and mobility 3.49 (2.44–4.54). Particularly patients readmitted because of pressure sores rated their independence higher than attending professionals.
Conclusion:
Our results support the criterion validity of SCIM-SR. The self-report version may facilitate long-term evaluations of independence in persons with SCI in their home situation.
Similar content being viewed by others
Introduction
The Spinal Cord Independence Measure (SCIM), which was first published in 1997,1 has become a widely used instrument to measure functioning in activities of daily living in persons with spinal cord injury (SCI).2 Its main advantages over other instruments used for functional assessment in rehabilitation medicine are its sensitivity to changes in performance of tasks that are relevant for SCI patients, and the fact that it measures not only the burden of care, but also achievements, which have medical, psychological or social relevance for the SCI patient. The third version of the instrument, SCIM III, has been tested for validity and reliability in multicenter studies with satisfying psychometric properties.3, 4, 5
SCIM III comprises items on 19 daily tasks grouped into three subscales. Item scores are weighted according to their clinical relevance and are graded for increasing difficulty, that is, requiring higher ability of the person with SCI. Each item has between 2 and 9 grades. The total SCIM III score ranges between 0 and 100, higher scores reflecting higher levels of performance or independence of a person.3 The three subscales assess the areas of ‘self-care’ (six items, range 0–20), ‘respiration & sphincter management’ (four items, range 0–40) and ‘mobility’ (nine items, range 0–40).
SCIM III is scored in observation of persons with SCI by health professionals. Ideally, each subscale is scored by clinical staff experienced in the assessment of the activities covered by the subscale. Such observations are time consuming and mainly applicable in inpatient settings.6 In the outpatient setting, SCIM III data were collected by a single rater or in interviews previously, although with slightly decreased precision.7, 8 For research purposes, SCIM data are obtained by interview as part of the regular follow-up of large international studies, such as the European Multicenter Study about Spinal Cord Injury (EMSCI).9
Studies conducted in the SCI community usually rely on self-administered questionnaires for data collection. This method requires comparatively few resources, provides fast data collection and is applicable independent of the setting.6, 10 Using self-report questionnaires for continued monitoring of daily activities in community-dwelling persons with SCI might allow detecting special health care needs in this population.
An internal review showed that the SCIM III covers most of the relevant categories in the field of activities and participation defined in the International Classification of Functioning, Disability and Health (ICF) Core Sets for SCI.11, 12 An efficient measurement of predefined relevant ICF categories in epidemiologic studies is highly important.13 For the community survey of the Swiss Spinal Cord Injury Cohort Study,14 a self-report version of SCIM III (SCIM-SR) was thus needed. Besides the advantages for community-based research, a self-report version might also help reduce the time and effort required for administration in routine care. Therefore, SCIM-SR provides an important additional tool for assessing patients’ daily task performance.
The aim of this study was to assess the criterion validity of SCIM-SR by comparing it to the SCIM III assessment by health professionals.
Materials and methods
Subjects
Between July and December 2011, we recruited 100 persons aged over 18 years who attended the inpatient clinics of the Swiss Paraplegic Center Nottwil and REHAB Basel (Switzerland) in a convenience sample. Eligible participants needed to have traumatic or non-traumatic SCI (time since injury ⩾1 month), sufficient German language skills (assessed by clinical staff) and the ability to read and answer the self-report questions by themselves. Persons with severe health conditions or cognitive impairments as well as those who underwent surgery in the previous 7 days were excluded. Informed consent was obtained from all study participants.
Procedure
Study participants were asked to fill in a paper–pencil version of the SCIM-SR questionnaire. In case the participants had difficulties to write because of limited hand function, a researcher helped with completion but did not explain items or help choose an answer. Attending health professionals (including occupational therapists, physiotherapists and nursing staff) completed the German SCIM III by observation of the participants.3 While SCIM III is routinely used at the Swiss Paraplegic Center Nottwil by a team of staff members familiar with the care of SCI patients, this is not the case at REHAB Basel. In this center, SCIM III was completed by a physician with experience in SCIM III in collaboration with the nursing staff in charge. The German version of SCIM III has been developed by members of the EMSCI study at the University clinic of Balgrist (Switzerland) and is routinely used in German-speaking clinical settings. The maximum delay between questionnaire completion by participants and health professionals was 4 days. Both were blinded to each other’s scores. We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research.
Instrument development
On the basis of the English SCIM III,3 a preliminary English SCIM-SR version was developed. Three investigators familiar with SCIM III and experienced in questionnaire design independently drafted an adapted version for self-report. Using feedback of additional team members, the three draft versions were combined into a single harmonized draft version of SCIM-SR. Briefly, the wording of the 19 items was adapted by using personal pronouns and avoiding or explaining technical terms. For item 6 (bladder management), we omitted the criterion of residual urine volume because this information is usually not known by persons with SCI. Several complex items or response categories were decomposed to facilitate self-reporting. This included SCIM III items with several statements in one answering option (items 6 and 7) or with more than six answering options (items 5, 12–14). Scoring algorithms were developed to obtain scores from these decomposed items that are consistent with SCIM III scores.
External experts with expertise in SCIM III and the developer of SCIM III reviewed the harmonized version for face validity. On the basis of their feedback, it was revised further and translated into German by professional scientific translators.
The German draft version was then pretested in cognitive interviews with five persons with SCI. Additionally, five German-speaking experts who routinely use SCIM III in the clinical setting were asked for feedback. Overall, the pretests showed that the SCIM-SR was understandable and acceptable. However, results of the cognitive interviews indicated that participants were confused by some descriptions and definitions, and these were omitted. Also, other minor modifications were made. The final German version of the SCIM-SR was then translated into English (Appendix), French and Italian.
Furthermore, information on age, gender, years of formal education, date of injury and para-/tetraplegia was collected in the paper–pencil questionnaire. Information on completeness of lesion and reason for hospitalization was retrieved from the medical records.
Statistical analyses
Pearson’s correlation coefficients were computed to analyze associations between SCIM III and SCIM-SR. Further, intraclass correlations (ICCs) were calculated to quantify the agreement between SCIM III and SCIM-SR scores. ICC take into account systematic differences in assessments that are not reflected in ordinary correlations such as the Pearson’s correlation.15 The Bland–Altman method was used to report on differences between SCIM III and SCIM-SR scores by calculating the mean difference between the two measurements.16 Bland–Altman plots were used to depict the difference in SCIM-SR and SCIM III scores against the mean score of both measurements for each subject.
For sensitivity analyses, stratified mean differences between SCIM III and SCIM-SR scores were calculated and linear regressions were run. In regression analysis, we used the mean differences between the two scores as continuous outcome and regressed it on selected independent variables. Unadjusted and adjusted coefficients and their 95% confidence intervals (CIs) were computed. For the regression models, predictors were either introduced as categorical (age, education and reason for admission) or dichotomous variables (gender, lesion characteristics and assistance with completion of the questionnaire). Likelihood-ratio tests were performed to assess significance of associations between predictors and outcome in regression models.
One case with an incomplete SCIM III score was dropped from the database. We used multiple imputation to account for missing data in the analysis.17 For details on imputation procedures see Supplementary Electronic Appendix. Data were analyzed using STATA 12.0 (College Station, TX, USA).
Results
Characteristics of the study population are presented in Table 1.
Table 2 displays SCIM III and SCIM-SR scores. Mean and median values of the SCIM III were lower than those of the SCIM-SR. These differences were greatest in the subscale mobility. The range of the total score and the subscale respiration & sphincter management was somewhat narrower in SCIM-SR than in SCIM III. Eight SCIM-SR total scores, six scores in respiration & sphincter management, four in self-care and two in mobility were incomplete. We found most missing values in items 6 (n=5), 3A and 3B (n=2). Items 1, 2A, 2B and 9 had one missing each. The distribution of the total scores of SCIM III and SCIM-SR is shown in Figure 1.
Table 3 shows the Pearson correlations, the ICCs, the Bland–Altman and the relative differences in means of SCIM III and SCIM-SR. Pearson correlation coefficients for the total and the subscale scores ranged between 0.81 for the subscale respiration & sphincter management and 0.87 for the total score and the subscales self-care and mobility. ICC values indicated coefficients ranging from 0.80 to 0.90. The highest ICC coefficient was observed for the total score, and the lowest for the subscale respiration & sphincter management. In the Bland–Altman analysis, the largest difference between SCIM III and SCIM-SR was observed in the subscale mobility. The relative differences were highest in the subscale mobility and lowest in the subscale respiration & sphincter management (Table 3).
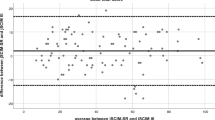
Table 4 shows results for stratified differences and uni- and multivariable sensitivity analysis. Associations of differences in total scores with age, gender, years of education and lesion characteristics were weak or inconsistent. Persons who got assistance with questionnaire completion showed less difference in scoring than those who filled in the questionnaire alone. The highest difference was found in persons hospitalized for pressure sores. The Bland-Altman plot for total scores stratified by reason for admission shown in Figure 2 confirms this finding.
Bland–Altman plot for the total scores of SCIM III and SCIM-SR stratified by reason for admission. Missing values were accounted for by multiple imputation. ○, persons in first rehabilitation; X, persons admitted because of a pressure sore and Δ, persons admitted for other reasons. s.d., standard deviation.
Discussion
The results of this study support the criterion validity of SCIM-SR as compared with SCIM III. Pearson correlation and ICC coefficients of the total and the subscale scores met the quality criterion of being above 0.7.18
Our results indicate systematically higher scores in SCIM-SR, especially in the mobility scale. This trend was not observed in similar studies that compared self-assessments by interview to observational scores of SCIM II8 or the Functional Independence Measure (FIM).19 In interviews, the interviewers might have interfered in case of uncertainties of patients, what could explain the absence of a systematic overestimation by respondents in those studies.8, 19 We found somewhat smaller differences between SCIM III and SCIM-SR in participants who got assistance in questionnaire completion. Although it was not allowed to explain or give additional information, we cannot exclude that the presence of a researcher has influenced the results.
We observed an association between reason for admission and precision of SCIM-SR. Our findings suggest that persons hospitalized because of acute health conditions (e.g. pressure sores) do not report on their current situation, but take their ‘habitual’ level of independence as reference for self-assessment. To further improve the validity of the SCIM-SR, we suggest using a clearer introductory text in the questionnaire that stresses the relation to the current situation (see Appendix A for suggestion). We assume that SCIM-SR scores of community-dwelling SCI individuals in stable health conditions will show fewer differences in scoring. Further research is needed to show whether this assumption is justified. If systematic overestimation remained, it would be possible to adjust SCIM-SR results for it. However, in absence of valid data, we do not recommend such adjustments.
This study has several limitations. Only inpatients were included in this study, and this may limit the generizability of the results. Regarding the adaption of SCIM III to SCIM-SR, the comparability of item 6 (bladder management) is limited due to the impossibility to measure residual urine volume by self-report. Nevertheless, results indicate a high correlation between item 6 of SCIM-SR and SCIM III.
SCIM III was specifically designed to provide a clinical assessment of functional performances and studies approved the responsiveness of the instrument.3, 20 In the current study, many participants were hospitalized due to health conditions such as pressure sores that reduced independence temporarily independent from the spinal cord lesion. Therefore, the design of our study did not allow assessing the sensitivity of SCIM-SR to improvement in functional level.
SCIM-SR was developed in English, based on the original English SCIM III version.3 Then, it was further refined and tested in German, and translated into French and Italian. However, only the German version has been validated and the present results might only hold true for this version. Conclusions on the validity of the English, French and Italian versions cannot be drawn and further validations of these language versions are encouraged. A Rasch analysis of the original SCIM III has been performed,3 but is not yet available for SCIM-SR.
Besides these limitations, there are also some strengths. The study size of 99 persons is large for a validation study.18 The study population included a broad spectrum of individuals in terms of sociodemographic characteristics and functional independence. Further, recruitment of inpatients had the advantage that SCIM III data were collected by trained and experienced health professionals who know the included patients well and did not rely on information from the patient. We are confident that SCIM III scorings were sufficiently accurate to fulfill the requirements of a gold standard. Finally, missing values were not systematically distributed by age or level of education. We therefore assumed that the wording of the SCIM-SR questionnaire was sufficiently clear to be used for self-administration in patients without serious cognitive deficits.
Conclusion
Our findings support the criterion validity of SCIM-SR. As SCIM III is the only comprehensive disability measurement instrument specifically developed for persons with SCI, we believe that the present self-report version will be a valuable tool for research in outpatient and community settings, as well as for resource-efficient assessment in hospitalized individuals with SCI.
Data archiving
There were no data to deposit.
References
Catz A, Itzkovich M, Agranov E, Ring H, Tamir A . SCIM--spinal cord independence measure: a new disability scale for patients with spinal cord lesions. Spinal Cord 1997; 35: 850–856.
Anderson K, Aito S, Atkins M, Biering-Sørensen F, Charlifue S, Curt A et al Functional recovery measures for spinal cord injury: an evidence-based review for clinical practice and research. J Spinal Cord Med 2008; 31: 133–144.
Catz A, Itzkovich M, Tesio L, Biering-Sorensen F, Weeks C, Laramee MT et al A multicenter international study on the Spinal Cord Independence Measure, version III: Rasch psychometric validation. Spinal Cord 2007; 45: 275–291.
Itzkovich M, Gelernter I, Biering-Sorensen F, Weeks C, Laramee MT, Craven BC et al The Spinal Cord Independence Measure (SCIM) version III: reliability and validity in a multi-center international study. Disabil Rehabil 2007; 29: 1926–1933.
Anderson KD, Acuff ME, Arp BG, Backus D, Chun S, Fisher K et al United States (US) multi-center study to assess the validity and reliability of the Spinal Cord Independence Measure (SCIM III). Spinal Cord 2011; 49: 880–885.
Hoenig H, Branch LG, McIntyre L, Hoff J, Horner RD . The validity in persons with spinal cord injury of a self-reported functional measure derived from the functional independence measure. Spine 1999; 24: 539–543.
Itzkovich M, Tamir A, Philo O, Steinberg F, Ronen J, Spasser R et al Reliability of the Catz-Itzkovich spinal cord independence measure assessment by interview and comparison with observation. Am J Phys Med Rehabil 2003; 82: 267–272.
Catz A, Itzkovich M, Steinberg F, Philo O, Ring H, Ronen J et al Disability assessment by a single rater or a team: a comparative study with the Catz-Itzkovich spinal cord independence measure. J Rehabil Med 2002; 34: 226–230.
van Hedel HJ, Dietz V . Walking during daily life can be validly and responsively assessed in subjects with a spinal cord injury. Neurorehabil Neural Repair 2009; 23: 117–124.
Dorevitch M . The ‘questionnaire’ versus the ‘direct observation’ approach to functional assessment. Br J Rheumatol 1988; 27: 326–327.
Cieza A, Kirchberger I, Biering-Sorensen F, Baumberger M, Charlifue S, Post MW et al ICF Core Sets for individuals with spinal cord injury in the long-term context. Spinal Cord 2010; 48: 305–312.
Kirchberger I, Cieza A, Biering-Sorensen F, Baumberger M, Charlifue S, Post MW et al ICF Core Sets for individuals with spinal cord injury in the early post-acute context. Spinal Cord 2010; 48: 297–304.
Fekete C, Boldt C, Post M, Eriks-Hoogland I, Cieza A, Stucki G . How to measure what matters: development and application of guiding principles to select measurement instruments in an epidemiologic study on functioning. Am J Phys Med Rehabil 2011; 90: S29–S38.
Post MW, Brinkhof MW, von Elm E, Boldt C, Brach M, Fekete C et al Design of the Swiss Spinal Cord Injury Cohort Study. Am J Phys Med Rehabil 2011; 90: S5–16.
Shrout PE, Fleiss JL . Intraclass correlations: uses in assessing rater reliability. Psychol Bull 1979; 86: 420–428.
Bland JM, Altman DG . Measuring agreement in method comparison studies. Stat Methods Med Res 1999; 8: 135–160.
Sterne JA, White IR, Carlin JB, Spratt M, Royston P, Kenward MG et al Multiple imputation for missing data in epidemiological and clinical research: potential and pitfalls. BMJ 2009; 338: b2393.
Terwee CB, Bot SD, de Boer MR, van der Windt DA, Knol DL, Dekker J et al Quality criteria were proposed for measurement properties of health status questionnaires. J Clin Epidemiol 2007; 60: 34–42.
Daving Y, Andren E, Nordholm L, Grimby G . Reliability of an interview approach to the functional independence measure. Clin Rehabil 2001; 15: 301–310.
Ackerman P, Morrison SA, McDowell S, Vazquez L . Using the Spinal Cord Independence Measure III to measure functional recovery in a post-acute spinal cord injury program. Spinal Cord 2010; 48: 380–387.
Acknowledgements
We are grateful to the clinical staff members of the Swiss Paraplegic Center (Nottwil) Cornelia Bühler, Andrea Bürgi, Astrid Eichholz, Sabine Felber, Kitty Pelt, Esther Peter, Daniel Ruckstuhl, Sylvia Seidl, Miriam van Schriek and Pascal Zehnder for their support with recruitment. We thank the research assistants Stefanie Bucher, Fabienne Michel, and Regula Sprecher for their help with recruitment. We express gratitude to Fin Biering-Sorensen, Mirjam Brach, Szilvia Geyh, Clive Glass and Gerold Stucki for their input in the development of SCIM-SR and Melissa Selb for the English check of SCIM-SR.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Spinal Cord website
Supplementary information
Appendices
Appendix A
English version of SCIM III for self-report. The validated German version is available from the authors on request. Codes in square brackets indicate the scales used for comparison with SCIM III but are not printed in the participant questionnaire

Appendix B
Scoring of item 6 (bladder management) in SCIM-SR

Appendix C
Scoring of item 7 (bowel management) in SCIM-SR SCIM-

Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Fekete, C., Eriks-Hoogland, I., Baumberger, M. et al. Development and validation of a self-report version of the Spinal Cord Independence Measure (SCIM III). Spinal Cord 51, 40–47 (2013). https://doi.org/10.1038/sc.2012.87
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2012.87
Keywords
This article is cited by
-
Correlates of physical activity in ambulatory people with spinal cord injury during the first year after inpatient rehabilitation
Spinal Cord (2024)
-
Use of professional home care in persons with spinal cord injury in Switzerland: a cross-sectional study
BMC Health Services Research (2023)
-
Australian arm of the International Spinal Cord Injury (Aus-InSCI) community survey: 1. population-based design, methodology and cohort profile
Spinal Cord (2023)
-
Standardized administration and scoring guidelines for the Spinal Cord Independence Measure Version 3.0 (SCIM-III)
Spinal Cord (2023)
-
Early and intensive motor training to enhance neurological recovery in people with spinal cord injury: trial protocol
Spinal Cord (2023)