Abstract
Study design:
Monocentric Cohort Study.
Objective:
Development of a multi-dimensional outcome score of the rehabilitation of spinal cord injury (SCI) patients.
Setting:
Level 1 Trauma centre with large spinal unit.
Methods:
During the rehabilitation of 161 patients with SCI between 2005 and 2007 following outcome parameters were assessed at different time points: functional status, pain, emotion, energy, sleep, social isolation, knowledge and self-management attitude. The results for these parameters were statistically evaluated with regard to different grades of paralysis and analyzed for socio-demographic influence factors. Correlation and factor analysis were then applied to evaluate the dependencies of the parameters and the dimensional structure of the applied score.
Results:
For all factors a positive trend was found during the course of rehabilitation. Only the functional status is caused by spinal cord lesion. Age, sex and social isolation have no direct influence on the result with regard to functional status. For interactive dependencies of the parameters a three-dimensional structure was found: Success in the parameters, emotion, energy or social status, is independent of success in the parameter functional status. The result of the functional status is, next to the type of spinal injury, mainly influenced by the self-management attitude. The level of knowledge gained during rehabilitation is independent of the success in the other parameters.
Conclusion:
By the combination of functional, psychological and cognitive parameters into a result score it is possible to determine the quality of a rehabilitation process in its multiple dimensions and for different levels and grades of palsy. By this it is possible to analyze and compare the effectiveness and efficiency of rehabilitation on a national and international level. Longitudinal comparison of the long-term effects of rehabilitation after SCI is also possible, for example, in the course of follow-up examinations.
Sponsorship:
Deutsche Gesetzliche Unfallversicherung (German Statutory Occupational Accident Insurance).
Similar content being viewed by others
Introduction
Only a few studies can be found that research systematically and on a broad basis the functional, psychological and cognitive aspects, which are essential influencing factors for a successful rehabilitation and social reintegration.1 The scientific discussion in this area is molded by scales of functional performance. Next to the determination of the functional status analyses of socio-demographic data are often highlighted.2, 1, 3, 4, 5, 6, 7 Other studies focus on the importance of related symptoms such as pain, psychosocial problems and loss of energy in the rehabilitation patient or the compliance of the patient is seen as a main outcome factor.8, 9, 10, 11, 12, 13, 14, 15, 16, 17 Studies researching the social reintegration mainly focus on occupational situation, living conditions and quality of life.18, 19, 20, 21, 22, 23, 24
A multi-dimensionally measuring test device, internationally usable and applicable for inpatients as well as outpatients is thereby currently lacking. It is the main aim of this study to develop such a test device, the working name in the following paper is ‘Boberg Quality Score’ or BobScore.
Three main questions in this study are:
(1) Which parameters have to be determined for a multi-dimensional rehabilitation quality assessment? (2) Can these parameters be treated as independent dimensions? (3) Is there a need to differentiate patient-subgroups (for example, type of spinal injury, sex, age, social or occupational status)?
Materials and methods
Study sample
The study design was monocentric. A consecutive series of 161 patients with a treatment starting point from 2005 to 2007 were included. Exclusion criteria were: (1) Age below 18 years; (2) Patients with cerebral dysfunction; (3) Patients with a significantly reduced life span; patients with a foreseeable treatment period of less than 12 weeks.
For a detailed description of the study population see Table 1.
Outcome measures
The functional status of the patients was determined with the ‘Spinal Cord Independence Measure’ (SCIM II).25, 26, 27, 28 The subscale ‘FIM-Communication’ of the ‘Functional Independence Measure’ was incorporated for the study. The extent of injury regarding sensory and motor function was measured by the ASIA Impairment Scale.
For the parameter self-management-attitude a rank scaled tool called ‘RPF-Scale Uni HH’ in the form of the SCIM scale was used. It has been developed by the University Hamburg. The scale differentiates four compliance-types: passive–receptive attitude, order-accepting attitude, self-involving attitude and self-management attitude.
For measurement of pain, psychological and vital dispositions the quality of life measurement tool Nottingham Health Profile (NHP) was used. In a further questionnaire the knowledge gained by the patient about their injury, which was taught on a regular basis during the rehabilitation process, was assessed.
For a detailed description of the evaluated parameters and used scales see Table 2.
For the validation of the scales and other relevant details see Table 3.
Overall three sets of questionnaires were used: (1) Admission and discharge data sheet containing clinical findings, ASIA score and reason for palsy; (2) Documentation sheet during the course of rehabilitation containing SCIM, self-management-attitude and co-morbidities. (3) Patient sheet including NHP, disease-related knowledge, socio-demographic data and further questions. The questionnaires 2 and 3 were evaluated at the beginning of rehabilitation, after 4 weeks, after 12 weeks and at the end of rehabilitation.
Testing of data acquired during the rehabilitation process was performed using Friedman's test. Independence of data and internal consistency was tested using Cronbach's α, bivariate correlation analysis (Spearman's ρ) and factor analysis (main component analysis following the Kaiser–Guttmann criterion). The importance of external factors (socio-demographic data, form of paralysis, reason for neurological injury) was tested with bivariate analysis for the different points of data acquisition. All statistical procedures were performed by the University Hamburg using SPSS version 15.0 (SPSS Inc., Chicago, IL, USA).
Results
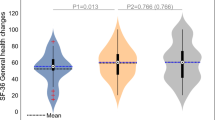
For the parameter ‘FIM-communication’ the majority of the patients (80%) showed no problems with communication already at the beginning of rehabilitation, the problem areas themselves were not of a high value. The other parameter showed beneficial effects of rehabilitation. For detailed results of the development of SCIM parameters, self-management attitude, knowledge and various NHP-dimensions see Figures 1, 2 and 3.
Results differentiated by neurological status and influence of socio-demographic features
The four subgroups of injury types can be seen as relatively homogenous regarding socio-demographic distribution. There were no significant differences found on statistical evaluation regarding the parameters age, sex, social and occupational status. The results that differentiated the four neurological subgroups are interestingly quite similar. Apart from the parameter functional status, the parameters for emotion, sleep, pain, energy, self-management-attitude and knowledge are independent of the neurological injury. There are no detectable effects of age or sex. A differentiation between traumatic and non-traumatic lesion does not show any significant differences.
Inter-correlation
The testing of the independence of the parameter showed that a high correlation was found between functional status and self-management attitude, whereas the other parameters were relatively independent of the functional status. Patients who only show a small increase in the functional status at the end of the rehabilitation also have poor self-management scores.
Regarding the NHP –parameter, average correlation results were found. The correlation between the parameter's emotion and social isolation is mainly based on a methodical effect. The parameter social isolation does not gain sufficient reliability. The parameter knowledge can be seen as a relatively independent dimension (Table 3).
Discussion
The presented results show that not only the situation regarding the functional status of spinal-injured patients can be measured during a rehabilitation process, but also the typical accompanying factors at the start and during the course of the rehabilitation. The scales of the SCIM, the NHP and the competency parameter knowledge and self-management attitude have proven to be valid and sufficiently sensitive. Only the scale for social isolation did not fulfill these criteria.
The development of the functional status during the course of the rehabilitation and the discharge-outcome shows, for the SCIM, results similar to those previously reported by other authors.27 Achievements in the functional rehabilitation of spinally injured should not be superimposed by strong pain, depression and permanent loss of energy. As our results show no such effects are measurable for the presented parameters.
The parameter pain showed an independent constant development, the development of the parameter ‘pain’ is unsatisfactory regarding the development during rehabilitation as well as regarding the result at discharge. The parameter pain has proven to be of high importance in the post-hospital stages of the rehabilitation process.15 For the parameter ‘sleep’ it can be stated that it is clearly influenced by the parameter's pain and emotion. Insofar this parameter can be abandoned from a quality scoring system.
This study has shown that with the proposed scoring system (BobScore) all relevant dimensions of the rehabilitation of spinal-injured patients can be captured. There is still an adequate scale missing to indicate relevant co-morbidities and complications. A further differentiation of the score by age groups or sex is not necessary.
Conclusions
The presented BobScore has the ability to mirror the process quality of the rehabilitation of different groups of spinal-injured patients. The measurement is multi-dimensional and can be facilitated for follow-up studies and questions of social reintegration.
Efficiency and effectivity of a rehabilitation measure can now be nationally and internationally compared by this system. For an international comparison the scales for the competency parameters knowledge and self management would have to be adapted. Regarding the sustainability of the results achieved, it has to be determined as to which significance the multi-dimensional result quality has for social re-integration. For this reason this research continues with a follow-up study.
References
Murray RF, Asghari A, Egorov DD, Rutkowski SB, Siddall PJ, Soden RJ et al. Impact of spinal cord injury on self-perceived pre- and postmorbid cognitive, emotional and physical functioning. Spinal Cord 2007; 45: 429–436.
Tooth L, McKenna K, Geraghty T . Rehabilitation outcomes in traumatic spinal cord injury in Australia: functional status, length of stay and discharge setting. Spinal Cord 2003; 41: 220–230.
McKinley W, Santos K, Meade M, Brooke K . Incidence and outcomes of spinal cord injury clinical syndromes. J Spinal Cord Med 2007; 30: 215–224.
Chan SCC, Chan APS . Rehabilitation outcomes following traumatic spinal cord injury in a tertiary spinal cord injury centre: a comparison with an international standard. Spinal Cord 2005; 43: 489–498.
Schönherr MC, Groothoff JW, Mulder GA, Eisma WH . Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the patient. Spinal Cord 2000; 38: 185–191.
New PW . The influence of age and gender on rehabilitation outcomes in nontraumatic spinal cord injury. J Spinal Cord Med 2007; 30: 225–237.
Scivoletto G, Morganti B, Ditunno P, Ditunno JF, Molinari M . Effects on age on spinal cord lesion patients’ rehabilitation. Spinal Cord 2003; 41: 457–464.
Ohry A, Weingarden H, Kiwerski J, Otom A, El-Masry WS, Kovindha A et al. Spinal injury rehabilitation complicated by psycho-social problems. Spinal Cord 1998; 36: 262–265.
Siösteen A, Kreuter M, Lampic C, Persson L-O . Patient-staff agreement in the perception of spinal cord lesioned patients’ problems, emotional well-being, and coping pattern. Spinal Cord 2005; 43: 179–186.
Norrbrink Budh C, Hultling C, Lundeberg T . Quality of sleep in individuals with spinal cord injury: a comparison between patients with and without pain. Spinal Cord 2005; 43: 85–95.
Fawkes-Kirby TM, Wheeler MA, Anton HA, Miller WC, Townson AF, Weeks CAO . Clinical correlates of fatigue in spinal cord injury. Spinal Cord 2008; 46: 21–25.
Siddall PJ, Loeser JD . Pain following spinal cord injury. Spinal Cord 2001; 39: 63–73.
Jensen MP, Hoffman AJ, Cardenas DD . Chronic pain in individuals with spinal cord injury: a survey and longitudinal study. Spinal Cord 2005; 43: 704–712.
Cardenas DD, Jensen MP . Treatments for chronic pain in persons with spinal cord injury: A Survey Study. J Spinal Cord Med 2006; 29: 109–117.
Donnelly C, Eng JJ . Pain following spinal cord injury: the impact on community reintegration. Spinal Cord 2005; 43: 278–282.
New PW, Lim TC, Brown DJ . A survey of pain during rehabilitation after acute spinal cord injury. Spinal Cord 1997; 35: 658–663.
Kennedy P, Frankel H, Gardner B, Nuseibeh I . Factors associated with acute and chronic pain following traumatic spinal cord injuries. Spinal Cord 1997; 35: 814–817.
Kreuter M, Sullivan M, Dahllöf AG, Siösteen A . Partner relationships, functioning, mood and global quality of life in persons with spinal cord injury and traumatic brain injury. Spinal Cord 1998; 36: 252–261.
Dijkers M . Quality of life after spinal cord injury: a meta analysis of the effects of disablement components. Spinal Cord 1997; 35: 829–840.
Lin K-W, Chuang C-C, Kao M-J, Lien I-N, Tsauo J-Y . Quality of life of spinal cord injured patients in Taiwan: a subgroup study. Spinal Cord 1997; 35: 841–849.
Franceschini M, Di Clemente B, Rampello A, Nora M, Spizzichino L . Longitudinal outcome 6 years after spinal cord injury. Spinal Cord 2003; 41: 280–285.
Vastenholt JM, Snoek GJ, Buschman HPJ, van der Aa HE, Alleman ERJ, Ijzerman MJ . A 7-year follow-up of sacral anterior root stimulation for bladder control in patients with a spinal cord injury: quality of life and users’ experiences. Spinal Cord 2003; 41: 397–402.
Pagliacci MC, Franceschini M, Di Clemente B, Agosti M, Spizzichino L . A multicentre follow-up of clinical aspects of traumatic spinal cord injury. Spinal Cord 2007; 45: 404–410.
Kennedy P, Lude P, Taylor N . Quality of life, social participation, appraisals and coping post spinal cord injury: a review of four community samples. Spinal Cord 2006; 44: 95–105.
Catz A, Itzkovich M, Agranov E, Ring H, Tamir A . SCIM—spinal cord independence measure: a new disability scale for patients with spinal cord lesions. Spinal Cord 1997; 35: 850–856.
Catz A, Itzkovich M, Agranov E, Ring H, Tamir A . The spinal cord independence measure (SCIM): Sensitivity to functional changes in subgroups of spinal cord lesion patients. Spinal Cord 2001; 39: 97–100.
Wirth B, van Hedel HJA, Kometer B, Dietz V, Curt A . Changes in Activity After a Complete Spinal Cord Injury as Measured by the Spinal Cord Independence Measure II (SCIM II). Neurorehab Neural Repair 2008; 22: 145–153.
Itzkovich M, Tripolski M, zeilig G, Ring H, Rosentul N, Ronen J et al. Rasch analysis of the Catz-Itzkovich spinal cord independence measure. Spinal Cord 2002; 40: 396–407.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Thietje, R., Giese, R., Kaphengst, C. et al. Parameters for positive outcome of the in-hospital rehabilitation of spinal cord lesion patients: the Boberg Quality Score. Spinal Cord 48, 537–541 (2010). https://doi.org/10.1038/sc.2009.171
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2009.171
Keywords
This article is cited by
-
Is admission to an SCI specialized rehabilitation facility associated with better functional outcomes? Analysis of data from the Thai Spinal Cord Injury Registry
Spinal Cord (2019)
-
Functional outcome of patients 12 and 48 weeks after acute traumatic tetraplegia and paraplegia: data analysis from 2004–2009
Spinal Cord (2012)
-
How does knowledge about spinal cord injury-related complications develop in subjects with spinal cord injury? A descriptive analysis in 214 patients
Spinal Cord (2011)