Abstract
The accumulation of senescent cells is associated with aging, inflammation and cellular dysfunction. Senolytic drugs can alleviate age-related comorbidities by selectively killing senescent cells. Here we screened 2,352 compounds for senolytic activity in a model of etoposide-induced senescence and trained graph neural networks to predict the senolytic activities of >800,000 molecules. Our approach enriched for structurally diverse compounds with senolytic activity; of these, three drug-like compounds selectively target senescent cells across different senescence models, with more favorable medicinal chemistry properties than, and selectivity comparable to, those of a known senolytic, ABT-737. Molecular docking simulations of compound binding to several senolytic protein targets, combined with time-resolved fluorescence energy transfer experiments, indicate that these compounds act in part by inhibiting Bcl-2, a regulator of cellular apoptosis. We tested one compound, BRD-K56819078, in aged mice and found that it significantly decreased senescent cell burden and mRNA expression of senescence-associated genes in the kidneys. Our findings underscore the promise of leveraging deep learning to discover senotherapeutics.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
Data generated from chemical screens, machine learning models and computational analyses are available as Supplementary Data 1–4. For molecular docking studies, protein structures from accession codes 6qgh (Bcl-2), 3wiz (Bcl-XL), 1osf (Hsp90), 4hg7 (MDM2) and 4f1s (PI3K) were obtained from the PDB at https://www.rcsb.org/. All other data are available from the corresponding author upon request. Source Data are provided with this paper.
Code availability
Chemprop is publicly available at https://github.com/chemprop/chemprop. A detailed code platform, including a Jupyter notebook and the Chemprop checkpoints for the different models developed in this work, is publicly available at https://github.com/felixjwong/senolyticsai.
References
Niedernhofer, L. J. & Robbins, P. D. Senotherapeutics for healthy aging. Nat. Rev. Drug Disc. 17, 377 (2018).
Childs, B. G. et al. Senescent cells: an emerging target for diseases of ageing. Nat. Rev. Drug Disc. 16, 718–735 (2017).
Baker, D. J. et al. Clearance of p16Ink4a-positive senescent cells delays ageing-associated disorders. Nature 479, 232–236 (2011).
Johmura, Y. et al. Senolysis by glutaminolysis inhibition ameliorates various age-associated disorders. Science 371, 265–270 (2021).
Xu, M. et al. Senolytics improve physical function and increase lifespan in old age. Nat. Med. 24, 1246–1256 (2018).
Fuhrmann-Stroissnigg, H. et al. Identification of HSP90 inhibitors as a novel class of senolytics. Nat. Commun. 8, 422 (2017).
Guerrero, A. et al. Cardiac glycosides are broad-spectrum senolytics. Nat. Metab. 1, 1074–1088 (2019).
Wakita, M. et al. A BET family protein degrader provokes senolysis by targeting NHEJ and autophagy in senescent cells. Nat. Commun. 11, 1935 (2020).
Xu, Q. et al. The flavonoid procyanidin C1 has senotherapeutic activity and increases lifespan in mice. Nat. Metab. 3, 1706–1726 (2021).
Robbins, P. D. Senolytic drugs: reducing senescent cell viability to extend health span. Annu. Rev. Pharmacol. Toxicol. 61, 779–803 (2021).
Demaria, M. et al. An essential role for senescent cells in optimal wound healing through secretion of PDGF-AA. Dev. Cell 31, 722–733 (2014).
Grosse, L. et al. Defined p16High senescent cell types are indispensable for mouse healthspan. Cell Metab. 32, 87–99 (2020).
Zhu, Y. et al. The Achilles’ heel of senescent cells: from transcriptome to senolytic drugs. Aging Cell 14, 644–658 (2015).
Zhu, Y. et al. Identification of a novel senolytic agent, navitoclax, targeting the Bcl-2 family of anti-apoptotic factors. Aging Cell 15, 428–435 (2016).
Yosef, R. et al. Directed elimination of senescent cells by inhibition of BCL-W and BCL-XL. Nat. Commun. 7, 11190 (2016).
Kirkland, J. K. & Tchkonia, T. Senolytic drugs: from discovery to translation. J. Intern. Med. 288, 518–536 (2020).
Triana-Martínez, F. et al. Identification and characterization of cardiac glycosides as senolytic compounds. Nat. Commun. 10, 4731 (2019).
Rudin, C. M. et al. Phase II study of single-agent navitoclax (ABT-263) and biomarker correlates in patients with relapsed small cell lung cancer. Clin. Cancer Res. 18, 3163–3169 (2012).
Vamathevan, J. et al. Applications of machine learning in drug discovery and development. Nat. Rev. Drug Disc. 18, 463–477 (2019).
Mamoshina, P., Vieira, A., Putin, E. & Zhavoronkov, A. Applications of deep learning in biomedicine. Mol. Pharm. 13, 1445–1454 (2016).
Zhavoronkov, A. et al. Artificial intelligence for aging and longevity research: recent advances and perspectives. Ageing Res. Rev. 49, 49–66 (2019).
Moskalev, A., Chernyagina, E., Kudryavtseva, A. & Shaposhnikov, M. Geroprotectors: a unified concept and screening approaches. Aging Dis. 8, 354–363 (2017).
Stokes, J. M. et al. A deep learning approach to antibiotic discovery. Cell 180, 688–702 (2020).
Ma, Y. et al. Identification of antimicrobial peptides from the human gut microbiome using deep learning. Nat. Biotech. 40, 921–931 (2022).
Aliper, A. et al. Deep learning applications for predicting pharmacological properties of drugs and drug repurposing using transcriptomic data. Mol. Pharm. 13, 2524–2530 (2016).
Mayr, A. et al. Large-scale comparison of machine learning methods for drug target prediction on ChEMBL. Chem. Sci. 24, 5441–5451 (2018).
Bagherian, M. et al. Machine learning approaches and databases for prediction of drug–target interaction: a survey paper. Brief Bioinform. 22, 247–269 (2021).
Putin, E. et al. Deep biomarkers of human aging: application of deep neural networks to biomarker development. Aging 8, 1021–1030 (2016).
Zhavoronkov, A., Li, R., Ma, C. & Mamoshina, P. Deep biomarkers of aging and longevity: from research to applications. Aging 11, 10771–10780 (2019).
Mamoshina, P. et al. Machine learning on human muscle transcriptomic data for biomarker discovery and tissue-specific drug target identification. Front. Genet. 9, 242 (2018).
Zhavoronkov, A. et al. Deep learning enables rapid identification of potent DDR1 kinase inhibitors. Nat. Biotech. 37, 1038–1040 (2019).
Popa, M., Isayev, O. & Tropsha, A. Deep reinforcement learning for de novo drug design. Sci. Adv. 4, eaap7885 (2018).
Olivecrona, M., Blaschke, T., Engkvist, O. & Chen, H. Molecular de-novo design through deep reinforcement learning. J. Cheminform. 9, 48 (2017).
Yang, K. et al. Analyzing learned molecular representations for property prediction. J. Chem. Inf. Model. 59, 3370–3388 (2019).
Lal, A. et al. p16INK4a translation suppressed by miR-24. PLoS ONE 3, e1864 (2008).
Omori, S. et al. Generation of a p16 reporter mouse and its use to characterize and target p16high cells in vivo. Cell Metab. 3, 814–828 (2020).
Liu, J.-Y. et al. Cells exhibiting strong p16INK4a promoter activation in vivo display features of senescence. Proc. Natl Acad. Sci. USA 116, 2603–2611 (2019).
Kirschner, K. et al. Phenotype specific analyses reveal distinct regulatory mechanism for chronically activated p53. PLoS Genet. 19, e1005053 (2015).
Gerdes, J. et al. Cell cycle analysis of a cell proliferation-associated human nuclear antigen defined by the monoclonal antibody Ki-67. J. Immunol. 133, 1710–1715 (1984).
Uxa, S. et al. Ki-67 gene expression. Cell Death Diff. 28, 3357–3370 (2021).
Corsello, S. M. et al. The Drug Repurposing Hub: a next-generation drug library and information resource. Nat. Med. 23, 405–408 (2017).
Van der Maaten, L. & Hinton, G. Visualizing data using t-SNE. J. Mach. Learn. Res. 9, 2579–2605 (2008).
Baell, J. B. & Holloway, G. A. New substructure filters for removal of pan assay interference compounds (PAINS) from screening libraries and for their exclusion in bioassays. J. Med. Chem. 53, 2719–2740 (2010).
Brenk, R. et al. Lessons learnt from assembling screening libraries for drug discovery for neglected diseases. ChemMedChem 3, 435–444 (2008).
Lipinski, C. A., Lombardo, F., Dominy, B. W. & Feeney, P. J. Experimental and computational approaches to estimate solubility and permeability in drug discovery and development settings. Adv. Drug Disc. Rev. 23, 3–25 (1997).
Karpinich, N. O., Tafani, M., Rothman, R. J., Russo, M. A. & Farber, J. L. The course of etoposide-induced apoptosis from damage to DNA and p53 activation to mitochondrial release of cytochrome c. J. Biol. Chem. 277, 16547–16552 (2002).
Jamil, S., Lam, I., Majd, M., Tsai, S.-H. & Duronio, V. Etoposide induces cell death via mitochondrial-dependent actions of p53. Cancer Cell Int. 15, 79 (2015).
Veber, D. F. et al. Molecular properties that influence the oral bioavailability of drug candidates. J. Med. Chem. 45, 2615–2623 (2002).
Wu, Y. et al. Senolytics: eliminating senescent cells and alleviating intervertebral disc degeneration. Front. Bioeng. Biotechnol. 10, 823945 (2022).
Wang, L. et al. Discovery of A-1331852, a first-in-class, potent, and orally-bioavailable BCL-XL inhibitor. ACS Med. Chem. Lett. 11, 1829–1836 (2020).
Youle, R. J. & Strasser, A. The BCL-2 protein family: opposing activities that mediate cell death. Nat. Rev. Mol. Cell Biol. 9, 47–59 (2008).
Schopf, F. H., Biebl, M. M. & Buchner, J. The HSP90 chaperone machinery. Nat. Rev. Mol. Cell Biol. 18, 345–360 (2017).
Fuhrmann-Stroissnigg, H., Niedernhofer, L. J. & Robbins, P. D. Hsp90 inhibitors as senolytic drugs to extend healthy aging. Cell Cycle 17, 1048–1055 (2018).
Shangary, S. & Wang, S. Targeting the MDM2–p53 interaction for cancer therapy. Clin. Cancer Res. 14, 5318–5324 (2008).
Chène, P. Inhibiting the p53–MDM2 interaction: an important target for cancer therapy. Nat. Rev. Cancer 3, 102–109 (2003).
Wang, L., Lankhorst, L. & Bernards, R. Exploiting senescence for the treatment of cancer. Nat. Rev. Cancer 22, 340–355 (2022).
Pawge, G. & Khatik, G. L. p53 regulated senescence mechanism and role of its modulators in age-related disorders. Biochem. Pharmacol. 190, 114651 (2021).
Porta, C., Paglino, C. & Mosca, A. Targeting PI3K/Akt/mTOR signaling in cancer. Front. Oncol. 4, 64 (2014).
Kirkland, J. L., Tchkonia, T., Zhu, Y., Niedernhofer, L. J. & Robbins, P. D. The clinical potential of senolytic drugs. J. Am. Geriatr. Soc. 65, 2297–2301 (2017).
Lozano-Torres, B. et al. The chemistry of senescence. Nat. Rev. Chem. 3, 426–441 (2019).
Lim, J. Y., Lee, J. Y., Byun, B. J. & Kim, S. W. Fisetin targets phosphatidylinositol-3-kinase and induces apoptosis of human B lymphoma Raji cells. Toxicol. Rep. 2, 984–989 (2015).
Eberhardt, J., Santos-Martins, D., Tillack, A. F. & Forli, S. AutoDock Vina 1.2.0: new docking methods, expanded force field, and Python bindings. J. Chem. Inf. Model. 61, 3891–3898 (2021).
Murray, J. B. et al. Establishing drug discovery and identification of hit series for the anti-apoptotic proteins, Bcl-2 and Mcl-1. ACS Omega 4, 8892–8906 (2019).
Tanaka, Y. et al. Discovery of potent Mcl-1/Bcl-xL dual inhibitors by using a hybridization strategy based on structural analysis of target proteins. J. Med. Chem. 56, 9635–9645 (2013).
Jez, J. M., Chen, J. C., Rastelli, G., Stroud, R. M. & Santi, D. V. Crystal structure and molecular modeling of 17-DMAG in complex with human Hsp90. Chem. Biol. 10, 361–368 (2003).
Anil, B., Riedinger, C., Endicott, J. A. & Noble, M. E. The structure of an MDM2-nutlin-3a complex solved by the use of a validated MDM2 surface-entropy reduction mutant. Acta Crystallogr. D 69, 1358–1366 (2013).
Wurz, R. P. et al. Synthesis and structure–activity relationships of dual PI3K/mTOR inhibitors based on a 4-amino-6-methyl-1,3,5-triazine sulfonamide scaffold. Bioorg. Med. Chem. Lett. 22, 5714–5720 (2012).
Ha, J.-Y. Molecular mimicry-based repositioning of nutlin-3 to anti-apoptotic Bcl-2 family proteins. J. Am. Chem. Soc. 133, 1244–1247 (2011).
Novais, E. J. et al. Long-term treatment with senolytic drugs dasatinib and quercetin ameliorates age-dependent intervertebral disc degeneration in mice. Nat. Commun. 12, 5213 (2021).
He, Y. et al. Using proteolysis-targeting chimera technology to reduce navitoclax platelet toxicity and improve its senolytic activity. Nat. Commun. 11, 1996 (2020).
Chang, J. et al. Clearance of senescent cells by ABT263 rejuvenates aged hematopoietic stem cells in mice. Nat. Med. 22, 78–83 (2016).
Mylonas, K. J. et al. Cellular senescence inhibits renal regeneration after injury in mice, with senolytic treatment promoting repair. Sci. Trans. Med. 13, abb0203 (2021).
Idda, M. L. et al. Survey of senescent cell markers with age in human tissues. Aging 12, 4052–4066 (2020).
Öztürk, H., Özgür, A. & Ozkirimli, E. DeepDTA: deep drug–target binding affinity prediction. Bioinformatics 34, i821–i829 (2018).
Thafar, M. A. et al. Affinity2Vec: drug–target binding affinity prediction through representation learning, graph mining, and machine learning. Sci Rep. 12, 4751 (2022).
He, T., Heidemeyer, M., Ban, F., Cherkasov, A. & Ester, M. SimBoost: a read-across approach for predicting drug–target binding affinities using gradient boosting machines. J. Cheminform. 9, 24 (2017).
Adeshina, Y. O., Deeds, E. J. & Karanicolas, J. Machine learning classification can reduce false positives in structure-based virtual screening. Proc. Natl Acad. Sci. USA 117, 18477–18488 (2020).
Bender, B. J. et al. A practical guide to large-scale docking. Nat. Protoc. 16, 4799–4832 (2021).
Wong, F. et al. Benchmarking AlphaFold-enabled molecular docking predictions for antibiotic discovery. Mol. Syst. Biol. 18, e11081 (2022).
Jiménez-Luna, J., Grisoni, F. & Schneider, G. Drug discovery with explainable artificial intelligence. Nat. Mach. Intell. 2, 573–584 (2020).
Karin, O., Agrawal, A., Porat, Z., Krizhanovsky, V. & Alon, U. Senescent cell turnover slows with age providing an explanation for the Gompertz law. Nat. Commun. 10, 5495 (2019).
Daina, A., Michielin, O. & Zoete, V. SwissADME: a free web tool to evaluate pharmacokinetics, drug-likeness and medicinal chemistry friendliness of small molecules. Sci. Rep. 7, 42717 (2017).
Morris, G. M. et al. AutoDock4 and AutoDockTools4: automated docking with selective receptor flexibility. J. Comput. Chem. 30, 2785–2791 (2009).
Greco, I. et al. Correlation between hemolytic activity, cytotoxicity and systemic in vivo toxicity of synthetic antimicrobial peptides. Sci. Rep. 6, 13206 (2020).
Dimri, G. P. et al. A biomarker that identifies senescent human cells in culture and in aging skin in vivo. Proc. Natl Acad. Sci. USA 92, 9363–9367 (1995).
Valentijn, F. A., Falke, L. L., Nguyen, T. Q. & Goldschmeding, R. Cellular senescence in the aging and diseased kidney. J. Cell Commun. Signal. 12, 69–82 (2018).
Krol, L. R. Permutation test. GitHub https://github.com/lrkrol/permutationTest (2022).
Acknowledgements
F.W. was supported by the James S. McDonnell Foundation. J.J.C. was supported by the Broad Institute of MIT and Harvard. The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript. We apologize to those colleagues whose relevant works we have been unable to mention, in attempting to survey such a broad area within a limited amount of space.
Author information
Authors and Affiliations
Contributions
F.W. conceived research, designed models and experiments, performed experiments and analysis, wrote the paper and supervised research. S.O. and N.M.D. designed and performed experiments and analysis. E.J.Z. assisted with experiments. J.J.C. supervised research. All authors assisted with manuscript editing.
Corresponding author
Ethics declarations
Competing interests
J.J.C. is an academic co-founder and board member of Cellarity, and the founding Scientific Advisory Board chair of Integrated Biosciences. F.W. is a co-founder of Integrated Biosciences. The remaining authors declare no competing interests.
Peer review
Peer review information
Nature Aging thanks Dyrba Martin and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Timeline of etoposide-induced senescence.
Control (DMSO-treated) and senescent (etoposide-treated) cells were treated with test compounds and assayed for cellular viability at the indicated times for compound screening and dose-response experiments.
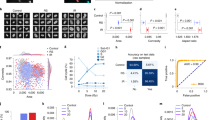
Extended Data Fig. 2 Screening of 2,352 compounds for senolytic activity and validation of four active compounds.
a, Cellular viability of vehicle- and etoposide-treated cells after a 3-day course of test compound treatment (10 μM). Values are from two biological replicates, and viability measurements are normalized by the interquartile mean of each cell plate. Active compounds (red points) are those for which the relative control cell viability is >0.5, the relative Snc viability is <0.7, and the ratio of Snc to control cell viability is <0.7. All other compounds are inactive (blue points). The Pearson’s correlation coefficient, R, and two-sided p-value are shown. b, Dose-response curves of control and etoposide-treated IMR-90 cells, treated with each compound shown. Zero μM (1% DMSO vehicle) treatment was included. Values are normalized by the average of two untreated samples from the same phenotype: here, a cellular viability of 1 indicates that of either untreated control cells or Sncs. Black curves indicate control (vehicle-treated) cells, and blue curves indicate (etoposide-treated) Sncs. Measurements are shown for two biological replicates in each treatment group (open points), and mean viability values (closed points) were fitted to calculate IC50 values. The therapeutic index (TI) is the ratio of IC50 values for vehicle- and etoposide-treated cells. The chemical structure of each compound is shown at the bottom of each plot. Note that, with our criteria for activity, ABT-263 has borderline activity at 1 µM and was inactive in our screen at 1 µM (panel (c)), due to marginal decreases in Snc viability. c, Senolytic screening results for 2,352 compounds at a final concentration of 1 µM. Values indicate the mean of two biological replicates, and viability measurements are normalized by the interquartile mean of each cell plate. Active and inactive compounds (red and blue points, respectively) are designated as in (a). Two known senolytics, ABT-737 and A-1331852, are inactive and highlighted with large blue points, and two active compounds, sulfisoxazole and imipramine hydrochloride, are highlighted with large red points. Sncs were induced with etoposide, and control cells were treated with vehicle (0.5% DMSO). d, Similar to (a), but for the screen shown in (c).
Extended Data Fig. 3 Comparison of machine learning models.
Shown are precision-recall curves for the two-best random forest models, trained and tested on the data shown in Fig. 1d. The black dashed curves represent the baseline fraction of active compounds in the training set (1.9%). Blue curves and the 95% confidence interval (CI) indicate the variation generated by bootstrapping. AUC, area under the precision-recall curve. The model hyperparameters used were: a, max depth, 5; number of estimators, 80; max features, 20; b, max depth, 5; number of estimators, 40; max features, 40.
Extended Data Fig. 4 Chemical filters for favorable medicinal chemistry properties and structural novelty.
The numbers of compounds after each chemical filtering step are shown, for both the Broad Institute Drug Repurposing Hub and the extended Broad Institute library. Numbers of curated compounds are indicated at bottom.
Extended Data Fig. 5 Screening of 216 compounds with high predicted senolytic activity, 50 compounds with low predicted senolytic activity, and validation of six additional active compounds.
a, Relative viability of vehicle- and etoposide-treated cells after a 3-day course of test compound treatment (10 μM). Values are from two biological replicates, and viability measurements are normalized by the interquartile mean of each cell plate. Active compounds (red points) are those for which relative control cell viability is >0.5, relative Snc viability is <0.7, and the ratio of Snc to control cell viability is <0.7. All other compounds are inactive (blue points). The Pearson’s correlation coefficient, R, and two-sided p-value are shown. b, Dose-response curves of control and etoposide-treated IMR-90 cells, treated with each compound shown. Compounds were serially diluted twofold starting from a final concentration of 50 μM, and 0 μM (1% DMSO vehicle) treatment was included. Cells were treated for 3 days. Cellular viability was determined by the metabolic reduction of resazurin into fluorescent resorufin, and values are normalized by the fluorescence intensities of the average of two untreated samples from the same phenotype: here, a cellular viability of 1 indicates that of either untreated control cells or Sncs. Vehicle treatment may result in cellular viability values <1 due to minor effects of DMSO on cellular viability. Black curves indicate control (vehicle-treated) cells, and blue curves indicate (etoposide-treated) Sncs. Measurements are shown for two biological replicates in each treatment group (open points), and mean viability values (closed points) were fitted to calculate IC50 values. The therapeutic index (TI) is the ratio of IC50 values for vehicle- and etoposide-treated cells. The chemical structure of each compound is shown at the bottom of each plot.
Extended Data Fig. 6 Structural comparisons of identified compounds.
Shown are the compounds in the training dataset with highest structural similarity to each of BRD-K20733377, BRD-K56819078, and BRD-K44839765, as measured by the Tanimoto similarity.
Extended Data Fig. 7 BRD-K20733377, BRD-K56819078, and BRD-K44839765 exhibit senolytic activity in a model of doxorubicin-induced senescence.
a, SA-β-gal staining of vehicle- (0.5% DMSO) and doxorubicin-treated IMR-90 cells plated at times on corresponding to the day before and day of compound addition (see also Fig. 1b and Extended Data Fig. 1). Each image is representative of two biological replicates. Scale bar, 100 μm. b, Relative mRNA expression of p16, p21, and KI67 in vehicle- (0.5% DMSO), doxorubicin-, and etoposide-treated IMR-90 cells harvested on the day of compound addition. Data for vehicle-and etoposide-treated cells are identical to those shown in Fig. 1c of the main text, and are shown here for comparison. Data from three biological replicates are shown. Error bars indicate one standard deviation. One-way, two-sided ANOVA with Tukey’s multiple comparisons: *p≤0.05,**p<0.01,***p<0.001. c, Dose-response curves of control and doxorubicin-treated IMR-90 cells, treated with each compound shown. Compounds were serially diluted twofold starting from a final concentration of 50 μM, and 0 μM (1% DMSO vehicle) treatment was included. Cells were treated for 3 days. Cellular viability was determined by the metabolic reduction of resazurin into fluorescent resorufin, and values are normalized by the fluorescence intensities of the average of two untreated samples from the same phenotype: here, a cellular viability of 1 indicates that of either untreated control cells or Sncs. Vehicle treatment may result in cellular viability values <1 due to minor effects of DMSO on cellular viability. Black curves indicate control (vehicle-treated) cells, and blue curves indicate (doxorubicin-treated) Sncs. Measurements are shown for two biological replicates in each treatment group (open points), and mean viability values (closed points) were fitted to calculate IC50 values. The therapeutic index (TI) is the ratio of IC50 values for vehicle- and doxorubicin-treated cells. The chemical structure of each compound is displayed in each inset. Data for control cells are identical to those shown in Fig. 3a–d of the main text.
Extended Data Fig. 8 Preliminary assessments of compound toxicological properties.
a, Fractional hemolysis measurements of human red blood cells treated with BRD-K20733377, BRD-K56819078, BRD-K44839765, and ABT-737 at the indicated final concentrations. Vehicle (1% DMSO) was used as a negative control, and Triton X-100 was used as a positive control. Black points indicate values from individual biological replicates, and red bars indicate average values. b, Ames test mutagenesis measurements of the fractions of revertant S. typhimurium TA100 cultures treated with BRD-K20733377, BRD-K56819078, BRD-K44839765, and ABT-737 at a final concentration of 100 µM. Vehicle (1% DMSO) was used as a negative control, and 0.25 µg/mL (~1 µM) 4-nitroquinoline 1-oxide was used as a positive control. Black points indicate values from individual biological replicates, and purple bars indicate average values. Higher fractions of revertant cultures indicate higher mutagenic potential.
Supplementary information
Supplementary Information
Supplementary Note 1, Tables 1–11, references and legends for Supplementary Data 1–4.
Supplementary Data 1
Senolytic screens of 2,352 compounds and 200 RDKit features used to augment the model. Compounds were screened at final concentrations of 10 μM and 1 μM in biological duplicate.
Supplementary Data 2
Model predictions for 804,959 compounds. Values indicate the mean of 20 Chemprop models. Compounds are from either the Broad Institute’s Drug Repurposing Hub or an extended Broad Institute library.
Supplementary Data 3
Compound filtering, curation and testing for senolytic activity. Compounds were filtered as described in Methods. Curated compounds were screened at a final concentration of 10 μM in biological duplicate.
Supplementary Data 4
Additional calculations of physicochemical properties. For comparison, values for ABT-737, ABT-263 and A-1331852 are shown. As in Table 1, Lipinski-conforming indicates that a compound violates no more than one of Lipinski’s rule of five: (a) ≤5 hydrogen bond donors, (b) ≤10 hydrogen-bond acceptors, (c) molecular weight <500 Da and (d) log P partition coefficient <5. Veber-conforming indicates that a compound violates none of Veber’s rules for oral bioavailability: (a) ≤10 rotatable bonds and (b) TPSA ≤140 Å2.
Source data
Source Data
Statistical source data.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wong, F., Omori, S., Donghia, N.M. et al. Discovering small-molecule senolytics with deep neural networks. Nat Aging 3, 734–750 (2023). https://doi.org/10.1038/s43587-023-00415-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s43587-023-00415-z
This article is cited by
-
Rejuvenation of diabetic macular edema with senolytic therapy
Nature Medicine (2024)
-
Machine learning for antimicrobial peptide identification and design
Nature Reviews Bioengineering (2024)
-
Transfer learning with graph neural networks for improved molecular property prediction in the multi-fidelity setting
Nature Communications (2024)
-
Discovery of a structural class of antibiotics with explainable deep learning
Nature (2024)