Abstract
Being a frequent malignant tumor of the genitourinary system, Bladder Urothelial Carcinoma (BLCA) has a poor prognosis. This study focused on identifying and validating prognostic biomarkers utilizing methylation, transcriptomics, and clinical data from The Cancer Genome Atlas Bladder Urothelial Carcinoma (TCGA BLCA) cohort. The impact of altered differentially methylated hallmark pathway genes was subjected to clustering analysis to observe changes in the transcriptional landscape on BLCA patients and identify two subtypes of patients from the TCGA BLCA population where Subtype 2 was associated with the worst prognosis with a p-value of 0.00032. Differential expression and enrichment analysis showed that subtype 2 was enriched in immune-responsive and cancer-progressive pathways, whereas subtype 1 was enriched in biosynthetic pathways. Following, regression and network analyses revealed Epidermal Growth Factor Receptor (EGFR), Fos-related antigen 1 (FOSL1), Nuclear Factor Erythroid 2 (NFE2), ADP-ribosylation factor-like protein 4D (ARL4D), SH3 domain containing ring finger 2 (SH3RF2), and Cadherin 3 (CDH3) genes to be the most significant prognostic gene markers. These genes were used to construct a risk model that separated the BLCA patients into high and low-risk groups. The risk model was also validated in an external dataset by performing survival analysis between high and low-risk groups with a p-value < 0.001 and the result showed the high group was significantly associated with poor prognosis compared to the low group. Single-cell analyses revealed the elevated level of these genes in the tumor microenvironment and associated with immune response. High-grade patients also tend to have a high expression of these genes compared to low-grade patients. In conclusion, this research developed a six-gene signature that is pertinent to the prediction of overall survival (OS) and might contribute to the advancement of precision medicine in the management of bladder cancer.
Similar content being viewed by others
Introduction
With a tenfold higher risk of occurrence compared to women, bladder cancer (BLCA) is the tenth most prevalent cancer worldwide and the sixth most prevalent in men1. Early in the prognosis, muscle-invasive or metastatic cancer is identified in around 25% of BLCA patients2. Patients with non-muscle-invasive BLCA are nevertheless experiencing significant rates of progression. Generally, the 5-year survival rate for bladder cancer is less than 20% at all stages. Even though there are multiple drugs, the lack of clinically potential biomarkers hinders the development of optimal treatment3. Tumor recurrence and metastasis are two key risk factors that have a significant impact on patients with BLCA prognosis. Thus, research concentrating on early identification and the prevention of the growth and spread of BLCA must be carried out with the help of efficient diagnostic procedures including optical techniques, imaging systems, and tumor biomarkers, to enhance the survival and reduce recurrence and progression of BLCA patients4,5.
Cystoscopy is a routine operation almost everywhere due to its high sensitivity and is still the gold standard for BLCA, but because of its invasiveness, it has adverse effects6. Nevertheless, urine cytology has poorer sensitivity for low-grade cancers even if it is a wonderful method for high-grade malignancies7. In this case, biomarkers are crucial and many biomarkers have been investigated during the past few years in a variety of clinical scenarios, including screening, monitoring, and follow-up8.
Urine cytology is currently the recommended urine marker for bladder cancer detection, but its sensitivity for detecting low-grade tumors is limited9. Single protein-based markers like NMP22 and BTA may be influenced by benign conditions, leading to false-positive results10. In recent years, commercially available markers have focused on multiplex protein, mRNA, and DNA assays. Non-coding RNA forms and extracellular vesicles are emerging areas of research for novel urinary biomarkers11. Genomic markers provide molecular insights into tumor biology and have potential applications beyond diagnosis and surveillance. Although non-invasive assays for bladder cancer (BC) diagnosis and follow-up currently exhibit high sensitivities and specificities, they still entail inconvenient rates of false positive results. Therefore, the development of more advanced and specific prognostic biomarkers holds promise for improving bladder cancer detection and management12.
The investigation of prognostic biomarkers in BLCA patients is still quite novel. Often, while constructing gene sets, cells or immunological pathways are the targets. Hallmark pathway-related gene sets and particular molecular pathway-selected gene sets have recently gained a lot of popularity in this area of research13,14. Typically, the research designs of these studies revolve around investigating immune cells and their impact on prognosis. Differential expression and route enrichment analyses are used in several studies15,16. Predictive modeling has become increasingly prevalent as a result of the creation of a prognostic gene set to validate them17.
With the development of molecular biology and bioinformatics over the past few decades, a number of unique bladder cancer tumor biomarkers have been found. Despite this advancement, key BLCA risk profiles have been developed using genes associated with a variety of symptoms. Potential machine learning algorithms are now being developed to group patients based on their clinical, molecular markers and prognostic factors18. To yet, little research has been done on the precise characterization of prognostic biomarkers associated with hallmark pathways19.
DNA methylation is a significant epigenetic alteration that has a significant impact on the transcriptional regulation of gene expression. In studies on tumors, it has been discovered that altering DNA methylation results in abnormalities in gene structure and function, which can serve as an early indicator of the development of tumors20. Additionally, many studies have been undertaken to understand the epigenetic mechanism behind cancer progression and resistance21,22. Hence, this novel study concentrated on the utilization of methylation data to study the impact of altered methylation pattern in bladder cancer patients by exploiting transcriptome analysis, and clinical traits.
Initially, methylation and survival analysis revealed prognostic hallmark genes and subjected them to clustering of the BLCA patients. Following transcriptomic analysis between two clusters identified novel biomarkers that may be involved in the survivability of bladder cancer patients and validated using the TCGA database and external dataset. The study proposed prognostic signature genes that can predict a patient’s prognosis and also validated using an external dataset. The signature genes were found to be associated with immune cells which may help in immune therapy. Collectively, the study followed a unique approach by integrating methylation, transcriptomic, and clinical data analysis to identify such prognostic biomarkers and was therefore provided with a novel insight to investigate bladder cancer.
Method
Data acquisition
This study utilized RNASeq, methylation, and clinical data of bladder carcinoma (BLCA) from The Cancer Genome Atlas (TCGA) to uncover prognostic biomarkers (https://www.cancer.gov/ccg/research/genome-sequencing/tcga). Gene sets of cancer hallmark pathways were collected from the Molecular Signatures Database v7.x (MSigDB; https://www.gsea-msigdb.org/gsea/msigdb), which were about 2322 genes. The study included 406 bladder cancer patients and 19 normal samples as training data and the GSE13507 dataset was used as test data. UCSC Xena the University of California, Santa Cruz (UCSC), Xena Browser (https://xenabrowser.net/) was used to download transcriptomic data of the TCGA which were already preprocessed23.
Differential methylation analysis
Methylation data were downloaded from the TCGA of patients as well as normal samples. Filtering was performed by removing CpG probes corresponding to chromosome X and chromosome Y. Overlapping probes were also filtered out to uniquely identify the differentially methylated genes. The data were downloaded as beta values which were then converted to M-value by executing log2 (beta/1-beta) transformation as M-value is easier to interpret, where positive M-value indicates hypermethylated and negative value indicates down methylation24,25. The limma package was used for differential methylation analysis between normal and bladder cancer patients using R programming language26. Cut-off criteria for adjusted value and |log fold change| were < 0.05 and > 1.5 respectively.
Clustering, identification, and characterization of molecular subtypes
Significantly methylated genes were then subjected to Cox regression survival analysis to identify the prognostic genes involved in the survivability of the cancer patient by considering p-value < 0.05. Hallmark pathway genes were then extracted from the significant prognostic genes, which were then considered to cluster the TCGA bladder cancer patients by unsupervised non-negative matrix factorization (NMF) clustering method using R package NMF27. The operation was performed by setting the method to “Brunet” and nrun to 50. This test was performed for ranks 2–6 in order to find the best cluster rank. The clustering performance was assessed by the principal components analysis (PCA) of the transcriptome data of TCGA BLCA. PCA plot was drawn considering K-means clustering using the Fviz_cluster method in R28,29. Overall survival (OS) and disease-free survival (DFS) analysis was performed using the survival package in R and cancer tumor stage, neoplasm histologic grade, neoplasm disease stage and metastasis stage were also observed between these subtypes using cBioPortal30.
Assessing amplification and deletion of chromosome between subtypes
To assess the genomic instability between subtypes Genomic Identification of Significant Targets in Cancer (GISTIC) v2.0 was used to observe the amplification and deletion in different chromosomes between subtypes31. Amplification and deletion data were downloaded from cBioPortal database based on the subtype of TCGA BLCA population and subjected to GISTIC server for CNV analysis.
Immunological assessment between subtypes
The number of stromal and immune cells infiltrating BLCA tissues was compared between subtypes by utilizing the ESTIMATE technique developed by the National Institute of Health. Estimate score was calculated for each sample considering both stromal and immune scores which indicate the tumor purity within each sample32. Subsequently, the CIBERSORT method was exploited to determine the strength of 22 immune cell types in each TCGA BLCA sample. CIBERSORT employs a deconvolution criterion via linear support vector regression (SVR) to deconvolute the gene expression profile33. The Wilcoxon rank-sum significance test was performed between subtypes to understand the difference in immune filtration levels34. The data for CIBERSORT analysis was extracted from the CIBERSORT website and the UCSC Xena browser.
Differential expression and enrichment analysis between subtypes
Differential expression data between molecular subtypes was collected from the cBioPortal website and a set of cutoff values (False Discovery Rate: FDR < 0.05 and |log2fold|> 1) was employed to determine the differentially expressed genes (DEGs). The upregulated genes of molecular subtypes were then utilized for enrichment analysis including biological process and KEGG: Kyoto Encyclopedia of Genes and Genomes, analysis via Enrichr webserver35,36,37. R programming was used to perform the analysis.
Identification of signature gene set
DEGs were subjected to a univariate Cox proportional hazards regression analysis considering the survival data of the BLCA cancer patients. For this, “coxph” and “survival” packages were utilized in R with an adjusted p-value < 0.05 as the cut-off value38,39. In addition, the least absolute shrinkage and selection operator (Lasso) method was employed on the resultant data from univariate analysis to create a predictive model with a high degree of accuracy. Lasso regression narrows the coefficients of the remaining variables toward zero and only chooses a subset of the important predictor variables. The penalty term employed by Lasso encourages the coefficients of the less important variables to be shrunk toward zero, effectively removing them from the model40,41. The resulting model is simpler and more interpretable, with a reduced risk of overfitting and multicollinearity problems. For the analysis, survival time and survival status were considered as independent variable, where the genes were dependent variable. The result reveal significant genes that influence patients survival.
Risk score and risk model construction
Following lasso regression analysis, multivariate analysis was performed on the significant genes from the lasso model with a cut-off p-value of < 0.05 in order to identify the most significant prognostic markers. The resultant genes were then subjected to network analysis and enrichment analysis to observe the involvement in cancer progression by NetworkAnalyst42. Network analysis involves constructing and visualizing biological networks to understand gene interactions. From the network analysis, best hub genes were considered for final prognostic gene markers, and a risk formula was constructed utilizing regression coefficient and RNAseq expression data of the final gene set43. The formula goes by,
\(\begin{aligned} {\mathbf{Risk}} \, {\mathbf{Score}} = & {\text{Coefficient1}}*{\text{expGene1}} + {\text{Coefficient2}}*{\text{expGene2}} + {\text{Coefficient3}}*{\text{expGene3}} \\ & + {\text{Coefficient4}}*{\text{expGene4}} + {\text{Coefficient5}}*{\text{expGene5}} + {\text{Coefficient6}}*{\text{expGene6}} \\ \end{aligned}\) where expGene1 to expGene6 represented the gene expression levels which were continuous values of the identified genes for a particular patient and coefficient 1 to coefficient 6 are the corresponding regression coefficients representing the impact of each gene's expression on the overall risk score.
Using the risk scores the BLCA patients were separated into two groups including high-risk and low-risk groups based on the median value. The survival analysis was performed between these two groups using the survival package in R and observed the Kaplan–Meir curves for overall survival44. Receiving operating characteristic curves (ROCs) were generated for 1 year, 3 years, and 5 years OS and AUC values were calculated to examine the prediction potential of the risk model using the timeROC package in R. The AUC value measures the overall performance of a binary classification model and provides an intuitive way to compare different models45,46. The timeROC package provides resources for studying time-dependent ROC curves in survival analysis. It provides a simple interface for computing, analyzing, and comparing the prediction accuracy of numerous biomarkers or tests across time. The expression of the final gene set was also observed in a heatmap and the independence of the risk score for OS was examined using multivariate Cox regression analysis using clinical factors. The survminer package was then used to create a forest plot that included the hazard ratio (HR) and 95% confidence interval (CI) for each variable47.
Nomogram model generation
Using the rms package in R, a nomogram for predicting overall survival (OS) and disease-free survival (DFS) was created by combining clinical data and the risk score of the TCGA BLCA patients. Based on the regression coefficients of the individual variables, scores were assigned. The matching individual scores of all factors were added up to provide a total score for each patient. Following that, the likelihood of each patient's outcome was determined using the conversion function. Calibration plots were used to examine the nomogram's prediction capability with a default penalty factor = adapen and boot. times = 10 which indicates an internal sampling for the test. As for model selection, “lasso” was used with an nfold of 5 which specifies the number of folds or subsets into which the dataset will be divided during the cross-validation process48.
Validation of the signature gene set in an independent dataset
To further assess the robustness of the signature gene set, an external dataset was used to validate the result. GEO dataset GSE1350749 was used with 165 primary cancer patients and the data was split into high and low-risk groups based on the threshold value of the risk scores calculated by the risk formula. Kaplan–Meir curves were observed for overall survival and AUC values were calculated using the timeROC package in R, where the time unit was considered in the year.
Correlation analysis between signature gene set and interleukins as well as immune cell filtration
The correlation between gene set expression with interleukin-6 (IL-6) and interleukin-20 (IL-20) was examined using the GEPIA2 web server50. Both IL-6 and IL-20 have a significant association with bladder cancer progression and metastasis51,52,53. With the help of the TCGA BLCA cohort, the UALCAN server was utilized to monitor the expression of genes at different phases of BLCA cancer patients54. The relationship between gene expressions and tumor-infiltrating immune cells (TIICs), including B-cells, T-cells, macrophages, neutrophils, and others, was observed using the TIMER server55. In order to calculate the frequency of TIICs from gene expression patterns, the server considered available TCGA cohort data. The expression pattern of the signature gene set was also observed in different stages and grades of bladder cancer.
Mutational assessment between subtypes
cBioPortal server was used to observe the mutational status of the 6 signature genes in subtype 1 and subtype 2. Missense mutations, inframe mutations, truncating mutations, and others were compared between subtypes to comprehend the impact of mutation in regulating the expressions of these genes.
Single-cell RNA-seq and grade expression analyses
The analysis of single-cell RNA sequencing data was conducted using the Tumor Immune Single-cell Hub 2 web service56, accessible at http://tisch.comp-genomics.org/home/. The study employed the uniform manifold approximation and projection (UMAP) method to reduce data dimensionality and visualize the clustering outcomes. Additionally, mRNA expression patterns of distinct cells were illustrated using UMAP distribution Figures. GSE13000157 and GSE14965258 bladder cancer datasets were utilized to observe the expression of pattern of the signature genes in different cell types within tumor microenvironment and intrtumor immune cells, respectively. Expression pattern was also observed between high and low grade patients for the signature genes using TCGA BLCA FPKM count data.
Result
The workflow of the study is summarized in Fig. 1. All the tools and algorithms used in this study were represented in Supplementary Table 1.
Workflow of the experiment. The workflow was structured into four sequential Sects. (1, 2, 3, and 4), each denoted by the (-o) sign to signify the analysis direction. The outcomes generated from each section were subsequently utilized, following a sequential flow from section "Introduction" to section "Method", then from section "Method" to section "Result", and finally from section "Result" to section "Discussion".
Identification of differentially methylated hallmark genes
Methylation analysis between normal and bladder cancer patients revealed 3606 differentially methylated genes (Fig. 2A), which were then subjected to Cox regression analysis to identify prognostic genes and the analysis uncovered 793 genes associated with the survival of the bladder patients. Following this analysis, 71 genes of hallmark pathways were identified from these prognostic genes and subjected to the clustering of the bladder cancer patients (Fig. 2B). These genes were than utilized to observe the impact of altered methylation pattern in TCGA BLCA population in terms of transcriptional landscape.
Creation of molecular subtypes
NMF clustering algorithm was employed on the expression profile of the selected hallmark genes of the cancer patients (n = 406) via NMF package in R. As for method parameter “Brunet” was used with a rank of 2:6 and nrun was 50. Based on the cophenetic correlation coefficient, the best rank was selected for clustering which was k = 2 as the cophenetic began to fall from 2 (Fig. 3A). When k = 2, the heatmap naturally displayed the consensus matrix (Fig. 3B). A consensus map for all 2 to 6 ranks was visualized and rank 2 showed the best clustering (Supplementary Fig. 1). The PCA analysis also supported the clustering into two subtypes (Fig. 3C) and therefore, the BLCA samples were divided into subtype 1 (n = 250) and subtype 2 (n = 156) molecular subtypes.
Clustering of TCGA BLCA patients. (A) Ranking of factors for k = 2–6. Less than two cophenetic and rss values indicate that two clusters are the most equally dispersed throughout the samples. (B) Heat diagram of the consensus matrix at k = 2. The values are between 0 and 1. Using hierarchical clustering, the columns and rows are arranged according to the average link's Euclidean distance. The samples are organized equally when k = 2, or two clusters, which denotes an ideal clustering number. (C) Visualization of the cluster using PCA plot.
Validation and characterization of molecular subtypes
Clinical evaluation was conducted for two subtypes among patients diagnosed with BLCA (Bladder Cancer). Overall survival and disease-specific survival analyses revealed that subtype 2 significantly displayed the worst prognosis than subtype 1 (Fig. 4A,B). Clinical assessment was done between two subtypes by observing tumor stage, neoplasm histologic grade, neoplasm disease stage, and metastasis stage. In each case, subtype 2 involved patients with higher percentage of T4 invasive, high grade, and stage 4 indicating the worst clinical outcome compared to subtype 1 (Fig. 4C–F).
Kaplan–Meier (A) overall survival plot and (B) Disease-free survival plot observation between two subtypes and p-value was calculated to measyre the significance of the analyses. Comparison of (C) tumor stage, (D) neoplasm grade, (E) neoplasm disease stage, and (F) metastasis stage between two clusters. The colors indicated distinct characteristic group of patients.
Chromosomal amplification and deletion analysis between two subtypes
The mutation frequencies of CNV were observed for two subtypes of bladder cancer patients. The most frequently amplified chromosome for both subtypes was observed in chromosomes 8 and 20. On the other hand, chromosomes 9 were found to be the most frequently deleted chromosome in subtype 1 and chromosome 22 were most frequently deleted in subtype 2. Overall, the mean frequency of amplification of subtype 2 (0.2689120) was lower than subtype 1 (0.2736826) and the mean deletion for subtype 2 (0.2864311) was higher than subtype 1 (0.2729289) (Supplementary Fig. 2).
Stromal and immune cells estimation in bladder tumors
Focusing on the stromal and immune cells that make up the bulk of the non-tumor components in tumor samples, the stromal and immunological assessment was performed by looking for distinctive signatures connected to stromal and immune cell infiltration in tumor tissues. The ESTIMATE score is based on these to infer tumor purity in tumor tissues. The poor prognosis subtype 2 was indicated by high levels of the stromal score, immunological score, and ESTIMATE score (Supplementary Fig. 3A), which validated the survival analysis. The P-value was calculated using the Wilcoxon rank test and was found to be significant for each scoring analysis (p-value < 0.05).
Tumor purity comparison using multiple methods
Five different methods—ESTIMATE, ABSOLUTE, LUMP, IHC, and CPE—were used to assess tumor purity. All of the data demonstrated a strong distinction between the subtypes in the tumor purity score, with subtype 2 exhibiting lower tumor purity and a worse prognosis (Supplementary Fig. 3B). Based on the Wilcoxon rank test, the p-value was calculated, which were all statistically significant (p-value < 0.05).
Immune checkpoint gene assessment
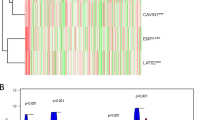
LAG3 (Lymphocyte-activation gene 3), PDCD1LG2 (Programmed cell death 1 ligand 2), CD274 (cluster of differentiation 274), IDO1 (indoleamine 2,3-dioxygenase 1), PDCD1 (Programmed Cell Death 1), CTLA4 (Cytotoxic T-lymphocyte-associated protein 4), and TIGIT (T cell immunoreceptor with Ig and ITIM domains) were considered important immune checkpoint genes because these genes are activated when T lymphocytes recognize and connect to related proteins on other cells, such as certain tumor cells. The T cells are informed that the checkpoint and partner proteins are "off" whenever they interact. This can make it more difficult for the immune system to get rid of cancer. All of these genes were elevated in subtype 2, and the Wilcoxon rank test revealed statistical significance for each of them (Fig. 5A). These findings demonstrate conclusively the potential importance of subtyping.
Immunological analysis of (A) immune checkpoint genes, (B) chemokines, and tumor-infiltrating cells between two clusters and p-value < 0.05 was considered to be significant. Differentially expressed genes between two clusters observation through (D) volcano plot by employing |logFC|> 1 and FDR < 0.05 parameters.
Chemokines expression observation
Across the two subtypes, CXC chemokine expression levels were compared. Analysis was done on the chemokines connected to bladder cancer using their expression profile from TCGA data. CXCL1, CXCL2, CXCL5, CXCL10, CXCL11, and CXCL13 all exhibited greater expression of Subtype 2, whereas CXCL14 had a higher expression of the subtype 1 (Fig. 5B). In bladder cancer, CXCL14 naturally plays a protective effect, supporting earlier findings 59. Other chemokines are often associated with a poorer prognosis for BLCA, supporting earlier research.
Infiltration level analysis between two subtypes
Analysis of 22 TICs was done to find out more about the connections between the subtypes and the immunological milieu since the differences between the two groups were connected to immunity. The 22 TIC profiles required for the ensuing experiments were first created using the CIBERSORT technique. Following that, the outcomes for the two subtypes were compared. The quantity of each cell component differed noticeably between the two subtypes (Fig. 5C). All the details are provided in Supplementary Table 2.
Expressional and ontology analysis between subtypes
Expression analysis between subtypes revealed 1430 significantly differentially expressed genes (DEGs), where 730 and 700 genes were found to be upregulated in Subtype 1 and Subtype 2, respectively (Fig. 5D). These upregulated genes were further assessed by enrichment analysis. This analysis was done for KEGG and the biological process. Whereas the immune system-related pathways were concentrated in the upregulated genes of subtype 2, those of subtype 1 were mostly involved in steroid hormone production and metabolic pathways (Supplementary Fig. 4A–B). The pathways for the Cytokine-Cytokine Receptor, Toll-Like Receptor Signaling, and cancer-related pathways exhibited high enrichment scores and significance for the subtype 2 elevated genes (Supplementary Fig. 4D). Major enriched pathways associated with cytochrome P450, hormone, lipid synthesis, etc. were associated with the Subtype 1 upregulated genes (Supplementary Fig. 4C). For this analysis, FDR had a cutoff threshold value of 0.05.
Univariate and Lasso regression analysis of DEGs
The DEGs of Subtype 1 versus Subtype 2 were subjected to univariate cox regression analysis to uncover prognostic genes. A total of 405 genes were found to be significant from the analysis with an FDR < 0.05. Following univariate analysis, lasso regression analysis was performed on these genes to identified genes with significant prognostic potential and the analysis revealed 50 genes after applying minimum lambda value. These genes were further analyzed for survivability of the patients by considering survival status and survival time which lead to the determination of 16 most significant genes (Supplementary Fig. 5A,B).
Cox regression analysis of 50 prognostic genes and network analysis
16 genes had significant findings from cox regression survival analysis (Supplementary Table 3). Among 16 genes 8 genes including SERPINB7 (Serpin family B member 7), FOSL1, ARL4D, NFE2, MBOAT2 (Membrane bound O-acyltransferase domain containing 2), ALDH1L2 (Aldehyde dehydrogenase 1 family member L2), TCHHL1 (Trichohyalin like 1), and EGFR, had a hazard ratio (HR) value greater than 1 which indicated that they can act as a hazardous gene in bladder cancer, while the rest had HR value less than 1 predicting their role in the survival of the cancer patients60. Following the analysis, 16 genes were then subjected to the network (Fig. 6A) and pathway analyses, which revealed that these genes are involved in several cancer-related pathways including Jak-stat signaling, MAPK cascade, epidermal growth factor signaling, TNF signaling pathways, and many others (Fig. 6B). The network analysis revealed 6 hub genes including EGFR, ARL4D, CDH3, SH3RF2, NFE2, and FOSL1. These 6 hub genes were found in the center of large networks and therefore, may serve as significant prognostic genes (Fig. 6A). The risk scores for each sample were calculated based on the expression of these 6 genes, and the risk score cutoff values were used to categorize all BLCA patients into high- and low-risk groups. The expression profile of the genes was visualized in a heatmap (Fig. 6C).
(A) Network analysis of the prognostic gene and hub gene identification. Orange color in the network indicated the hub genes. (B) Enrichment analysis of the prognostic genes where the color gradient was set based on the -log10(p-value). (C) Expression observation of 6 signature genes. (D) Multivariate analysis using clinical factors.
Multivariate analysis for the final prognostic genes using clinical parameters
Multivariate analysis was performed to confirm the prognostic capability of the six-signature gene set and the independence of other clinical characteristics. For this, several co-variables include age, gender, tumor grade, metastasis grade, tumor stage, and risk score. A risk score of the signature gene set was found to be a potent and independent factor in the TCGA bladder cancer populations after incorporating additional clinical factors to modify the multivariate analyses (HR = 1.67, 95% CI 1.29–2.1, P < 0.001) (Fig. 6D).
Survival analysis of risk groups
The percentage of patients who died increased as the risk score increased (Fig. 7A,B). The chi-square test value between survival status and risk status was 13.663 with a p-value of 0.0002187 indicating a significant association between the two variables. Significant disparities between the High and Low-risk categories were observed through survival analysis and the ROC curve also validated the significance of survival analysis (Fig. 7C). The AUC value displayed satisfactory results indicating the risk model had high discriminatory power and it can accurately distinguish between patients who will survive and those who will not survive for 1 year, 3 years, and 5 years (Fig. 7D).
(A) Rank score and (B) survival status observation between high and low-risk groups. Based on the risk ratings of a set of six gene signatures, Kaplan–Meier OS curves were created for high and low-risk groups. (C) Overall survival plot demonstrates the difference between the two groups. The Log-rank test was used for the statistical analysis. The ROC analysis was carried out using the R program TIMEROC, as shown in (D). The analysis's False Positive Rate (AUC) was negligible, which is a strong indication of how well the risk score performed in terms of predicting OS for 1 year, 3 years, and 5 years.
Nomogram model generation
To predict the overall survival of BLCA patients, a nomogram was created by integrating the six-gene signature risk score with clinical variables such as age, gender, metastatic grade, tumor grade, and cancer stage. Nomogram results were consistent across all clinical variables. A declining survival probability was visible with the points at 1 year, 3 years, and 5 years (Supplementary Fig. 6A). Moreover, the calibration plot showed the best predictive accuracy, with the anticipated survival rate being about equal to the actual survival rate (Supplementary Fig. 6B–D). The nomogram combining the five-gene signature, grade, age, and gender may improve the prognosis prediction accuracy for BLCA patients.
Performance evaluation and validation of the signature model
An independent dataset GSE13507 was used for validating the risk model and survival analysis. Around 165 primary bladder cancer patients were selected with their survival data and divided into high and low-risk groups based on the mean value of the risk scores. The survival analysis was performed between two groups and the result showed higher risk group had lower survivability than the low-risk group which validates the findings of this study (Fig. 8A). The ROC curves were generated for 2 years, 3 years, and 5 years of overall survival and all the AUC values were above the baseline (AUC > 50%) (Fig. 8B). Also, the AUC curves were nearly parallel with identical shapes, indicating that the model's predictive performance remains consistent and stable over the period of measurement.
Correlation analysis of the signature genes with interleukins and immune cell infiltration
To further evaluate the impact of hub genes, a correlation study between the expression of signature genes and IL-6 and IL-20 was carried out. The analysis showed that all genes were significantly positively associated with IL-6 except ARL4D (P-value > 0.05) and CDH3 (P-value > 0.05) and also significantly positively correlated with IL-20 (Supplementary Fig. 7A–L). Correlation between signature genes and immune filtration revealed that signature genes were shown to be favorably regulated with at least four levels of immune cell infiltration (Supplementary Fig. 8A–F), indicating the involvement of these genes in tolerating immune response. It was also observed that expression of the signature gene set was higher in high grade and also gradually increased in tumor stages (Supplementary Fig. 9) indicating the impact of the signature gene set in the development of high tumor grade and stage.
Impact of mutations on signature genes
The mutational status between the two subtypes revealed that there are no driver missense mutations in the subtypes. Only NFE2 had a driver truncating mutation in subtype 1 (Supplementary Fig. 10A–F). These results indicated that there may be no association of mutations with expression patterns of these signature genes in both subtypes. This indeed signified the presence of crucial factors other than mutation including epigenetic, post-trasncriptional modificaitons, and environmental influence. This observation makes it more crucial to study the genetics behind the characteristics of these genes in cancer progression.
Single-cell observation and grade comparison of signature genes
The analysis revealed most cells in tumor microenvironment including stromal cell expressed EGFR, NFE2, and FSL1 genes while a lower number of cells expressed CDH3, ARL4D, and SH3RF2 (Fig. 9). The expression of these genes in tumor microenvironment by cells that promote cancer progression indicated the the potential involvement of these genes in bladder cnacer development. In addition, ARL4D, SH3RF2, and FOSL1 were found to be expressed in tumor immune cells (TICs) (Fig. 10). Expression comparison between high and low grade patients for the signature genes showed that the signature genes tends to have a higher expression in high grade patients depicting the significance of these genes in the development of more advance form of cancer (Supplementary Fig. 11). EGFR, ARL4D, and NFE2 were significantly upregulated (p-value < 0.05) in high grade patients whereas the other were not significant but trend was higher in high grade patients.
The single-cell RNA-seq analysis focuses on prognostic signature genes. (A) Utilizing the UMAP method, the distribution of cells in tumor microenvironment was visualized, and (B) the visualization of malignant stromal cells tumor microenvironment. The mRNA expression levels of (C) EGFR, (D) NFE2, (E) ARL4D, (F) CDH3, (G) FOSL1 and (H) SH3RF2, were examined across distinct cellular populations in tumor microenvironment.
Discussion
Patients with BLCA have a high risk of metastasis and recurrence. Before immune checkpoint therapy, platinum chemotherapy has not been successful in treating metastatic BLCA throughout the last few decades61,62,63. With the rising acceptance of immunotherapy, emphasis has shifted to the creation of new biomarkers associated with tumor immune milieus that may be used to predict treatment efficacy and survival outcomes. Mechanistic investigations of cancer development now have a theoretical foundation thanks to the use of RNA-Seq and bioinformatic analysis of databases and allow researchers to simultaneously analyze the expression of thousands of genes across multiple samples64. This makes it possible to identify changes in gene expression that are associated with different experimental conditions or disease states. The purpose of this research was to identify a signature gene set that might be used as a biomarker for BLCA patients by utilizing bulk methylation and RNA-Seq data from TCGA BLCA data.
There are currently few biomarkers that can forecast both clinical outcomes and the effectiveness of immunotherapy. Previously performed studies only considered a particular criteria for instance expression data, gene-specific approach, etc. to propose biomarkers65,66. Some research work proposed signature models with good performance but they all followed a different approach to create such gene sets and did not consider hallmark pathways along with other gentic fators67,68. The study aimed to refine the prognostic accuracy and therapeutic strategies for BLCA patients through the integration of multi-omics data and the application of advanced bioinformatics methodologies. The novelty of the research lies in its comprehensive integration of RNASeq, methylation, and clinical data from TCGA, offering a holistic perspective on BLCA that considers the intricate interplay between genetic alterations and clinical outcomes. Using integrated methylation and transcriptomic data, along with clinical features a prediction model with six signature genes was created in this work which was also validated using an external dataset. Various analyses were performed to support the identification of the signature gene set including, multivariate analysis, survival analysis, correlation analysis, expression observation in tumor grade and stage, etc. This model can predict a patient's survivability and prognosis.
Initially, methylation data were extracted from TCGA and differential analysis was performed between normal and cancer patients performed. Following the analysis, prognostic genes were identified by using univariate cox regression analysis which revealed 793 genes. Hallmark pathways including the KRAS signaling pathway69, epithelial-mesenchymal transition70, DNA repair71, glycolysis72, signaling73, and a few other pathways-related genes were then screened through the prognostic genes and 71 hallmark pathway genes were found to be differentially methylated from the process which was involved in the survival of the cancer patients and used for NMF clustering of the BLCA patients by exploiting the expression data of these 71 genes.
To determine the ideal number of subtypes for the samples, numerous test runs with a rank of 2:6 were performed in this case. The cophenetic coefficient began to decrease after 2, indicating that 2 would be the ideal number of subtypes and the consensus matrix supported the clustering into 2 subtypes (Fig. 3A,B). To further validate the clustering, PCA analysis was performed and the plot was clearly divided into two portions. Immune checkpoint genes are important in regulating the immune system and preventing excessive immune responses that can lead to tissue damage therefore, immune checkpoint gene expression was observed between two subtypes (Fig. 5A). The higher expression of immune checkpoint genes in subtype 2 suggested that this subtype may have a stronger immune response and a greater ability to recognize and attack tumor cells. This could potentially make subtype 2 more responsive to immune-based therapies that target these checkpoint proteins. On the other hand, the lower expression of these genes in subtype 1 suggested that this subtype may be less responsive to immune-based therapies, and may require different treatment approaches. The expression pattern of chemokines was also observed between two subtypes and was highly expressed in subtype 2 indicating a poor prognosis of subtype 2 (Fig. 5B). Furthermore, CXCL14 was found to be highly expressed in subtype 1 and studies suggested that this chemokine is responsible for better prognosis in prostate cancer which opens up a possibility for this chemokine to become an effective marker for bladder cancer. The link between CD4 and CD8 cells is still unclear, despite changes in the numbers of neutrophils, NK cells, macrophages, dendritic cells, and mast cells in BLCA74. Several studies showed that CD8 is responsible for a better prognosis of bladder cancer. Throughout the work, it was found that individuals with subtype 1 who had a better prognosis had a higher CD8 cell count75. On the other hand, a worse prognosis has been associated with higher CD4 cell counts and CD3/CD4 ratios, which was corroborated in this study for subtype 276.
Differential expression and gene ontology analysis revealed that genes upregulated in subtype 1 were involved in biosynthesis-related pathways whereas genes in subtype 2 were involved in immune response-related pathways. It was also observed that individuals from subtype 2 were enriched in various cancer-related pathways including the JAK-Stat signaling pathway, TNF signaling pathway, and NF-kB signaling pathway indicating the worst survivability of subtype 2 compared to subtype 1. Subtype 1 showed a high enrichment score for cytochrome P450-related pathways, which might be explained by the fact that these patients' improved prognoses led to better drug metabolism responses to anticancer therapy. Univariate analysis and subsequent lasso regression and network analysis discovered 6 hub genes and considered as the most significant prognostic gene set which were EGFR, FOSL1, NFE2, ARL4D, SH3RF2, and CDH3 (Fig. 6A).
EGFR is positively associated with poor outcomes in bladder cancer. It also promotes cancer growth, progression, and metastasis of various cancers77. FOSL1 or FOS Like 1, AP-1 Transcription Factor Subunit is a leucine zipper protein that regulates tumor cell proliferation and survival in cancer. This protein was found to be involved in controlling the motility of bladder cancer cells through upregulating receptor tyrosine kinase AXL78. NFE2 is mostly involved in the regulation of maturation and biogenesis of platelets, cellular detoxification, and drug influx/efflux and was found to be involved in bone metastasis by promoting the WNT signaling pathway. This was found to be associated with poor prognosis and chemotherapy resistance in bladder cancer79. ARL family proteins including ARL4D, are involved in cancer cell migration, invasion, and proliferation80. Cancer cells are successfully kept from undergoing apoptosis when SH3RF2 is expressed ectopically because it promotes cell motility, colony formation, and tumor development in vivo81. The ability of cells to adhere to the extracellular matrix and other cells is mediated by the cell adhesion protein CDH3. It also regulates tissue morphology and is found to be highly expressed in different malignancies including bladder cancer82.
Based on the expression pattern and survival coefficients of these 6 prognostic genes, the risk score model was generated and risk scores were calculated for each TCGA BLCA patient. Multivariate analysis disclosed that risk score can independently predict the survivability of bladder cancer patients which strengthens the potential of the risk model. A Kaplan–Meier survival analysis between the high-risk and low-risk groups was performed to corroborate these findings, and the results showed that the high-risk groups had a poorer prognosis rate with significant log-rank test values.
Based on the clinical data and risk score, a nomogram model was developed. It depicts a mathematical likelihood of a clinical event from a statistical prediction model. It can be used to combine various prognostic factors, such as tumor stage, age, tumor markers, and treatment modalities, to estimate the likelihood of certain outcomes. This clinical prediction nomogram may help create personalized treatment strategies for BLCA patients by offering each patient a predicted result.
Using the independent dataset GSE13507, the risk score for six genes was assessed. High-risk groups had significantly lower values in the survival plot. Nonetheless, the independent dataset's AUC curve produced values above the baseline, validating the survival analysis's findings (Fig. 8). However, the results need to be further verified because of the data variation and differences in data distribution in the independent dataset GSE13507 since it was generated from the Korean population, whereas the data used in this study came from the American population. In addition, the TCGA BLCA data considered a wide variety of data types such as geographical locations, gender, age, biopsy location, age, race, smoking, tumor grade, metastasis, etc. whereas the independent dataset considered only a few factors.
To further strengthen prediction for 6 signature genes, the association between interleukins and immune cell filtration was observed. IL-6 promotes bladder cancer progression through AKT and STAT3 activations which ultimately lead to epithelial-mesenchymal transition and angiogenesis. Interleukin-20 induces the up-regulation of p21(WAF1) protein expression, which in turn causes nuclear factor (NF-B) to activate by promoting the migration of bladder cancer cells via ERK-mediated MMP-9 protein production. The correlation analysis revealed that the six signature genes were positively correlated with IL-6 and IL-20 indicating the dysregulation of these genes may hamper the regulation of IL-6 and IL-20 and may cause cancer progression. It was also found to be positively correlated with immune filtration cells including CD8 + , CD4 + , macrophage, and others. This implied that the expression of signature genes may react significantly in response to immune therapy. The signiature genes were also found to be expressed in tumor microenvironment by cells that promote cancer progression and expressed in immune-related genes which may provide valuable insights about immune therapy. The elevated expression levels of these genes in high-grade patients indicate their importance in the development of aggressive cancer forms and their relevance to prognosis.
It is essential to conduct proteomic investigations and analyze miRNAs that regulate mRNA translation83. By combining proteomic techniques with miRNA analysis, it is possible to gain valuable insights into the complex regulatory mechanisms controlling protein expression in cells. This integrated approach can provide a comprehensive understanding of how miRNAs influence the translation of specific mRNAs, leading to a more comprehensive understanding of cellular processes and potential therapeutic targets84. Integration of miRNA-lncRNA interactions using extensive machine learning model85 relating the signature genes may refine the molecular landscape, contributing to a more comprehensive and clinically relevant characterization of bladder cancer. Utilizing predictive models such as, DMFGAM which considers both molecular fingerprint and molecular graph features, can aid in prioritizing candidate biomarkers for further validation and experimental exploration86. Moreover, consideration of metabolite-disease associations through utilizing deep learning model, such as GCNAT87, will enhance the clinical relevance of the identified gene signature and underscores the multifaceted nature of molecular interactions in bladder carcinoma. Establishing intricate relationship networks in the context of signature genes with diseases may provide novel strategy to study the disease mechanisms and many deep learning approaches including, NSCGRN and MPCLCDA, are being developed that consider the biological data sources to understand the association with disease progression88,89. However, due to data availability, scope limitations, and resource constraints, these analyses weren’t included in the study but rather provided necessary insights based on which a comprehensive study can be designed to improve the robustness of the biomarkers proposed in this study in bladder cancer management.
The six-gene signature showed promising results as a robust prognostic biomarker, facilitating effective risk stratification and personalized treatment decisions in the context of bladder carcinoma. Its potential applications extend to informing clinical trial design, monitoring treatment efficacy, and identifying therapeutic targets. However, several challenges such as practical implementation, ethical considerations, disease heterogeneity, and predicting treatment responses need careful consideration before establishing the signature geneset as a viable biomarker. Ordinary Differential Equations (ODE)-based theoretical modeling studies on signature gene signaling networks could provide a more comprehensive understanding of regulatory mechanisms and potential therapeutic targets in bladder cancer90. In addition, Applying the insights from phase separation mechanisms and knowledge of intracellular organization to the intricate molecular landscapes of cancer cells can enhance the interpretation of biomolecular interactions, spatial patterns, and regulatory mechanisms, thereby contributing to the depth and applicability of your prognostic signature study in the context of bladder carcinoma91. As this study unveils the promising six-gene signature as a prognostic biomarker in bladder carcinoma, the integration of theoretical modeling studies further emphasizes the translational implications. While further validation and collaborative efforts are essential, successful implementation holds the potential to significantly enhance bladder cancer management, ultimately improving patient outcomes. Addressing these challenges will be pivotal in advancing more precise diagnostics and tailored interventions for bladder carcinoma.
In this study, a distinct signature gene collection based on methylation and transcriptomic data was discovered. Six genes were shown to be significantly associated with a patient's survival from bladder cancer. Some limits still need to be looked upon despite the unique insights that this study has provided. With a bigger sample size, the findings of this retrospective investigation would be more credible.
Conclusion
In summary, the six signature genes EGFR, FOSL1, NFE2, ARL4D, SH3RF2, and CDH3 may serve as possible biomarkers for BLCA patients' prognoses. This signature collection showed strong prediction performance in both the training and validation cohorts and might be used to more precisely identify prognostic risk in bladder cancer patients. This work may offer insights for additional research into the biological processes, clinical diagnosis, and treatment approaches of BLCA related to these genes. It may also lead to the development of targeted therapies, exploration of epigenetic treatments, and integration of other omics data for a more comprehensive understanding of bladder cancer.
Data availability
The datasets utilized in this study are available in TCGA (https://portal.gdc.cancer.gov/) and GEO repository (https://www.ncbi.nlm.nih.gov/geo/).
References
Antoni, S. et al. Bladder cancer incidence and mortality: A global overview and recent trends. Eur. Urol. 71, 96–108 (2017).
Robertson, A. G. et al. Comprehensive molecular characterization of muscle-invasive bladder cancer. Cell 171, 540-556.e25 (2017).
Aggen, D. H. & Drake, C. G. Biomarkers for immunotherapy in bladder cancer: a moving target. J. Immunother. cancer 5, 1–13 (2017).
Hu, X., Li, G. & Wu, S. Advances in diagnosis and therapy for bladder cancer. Cancers. 14, 3181 (2022).
Li, Y. et al. A qualitative transcriptional signature for predicting recurrence risk of stage I-III bladder cancer patients after surgical resection. Front. Oncol. 9, 436843 (2019).
Zhu, C. Z., Ting, H. N., Ng, K. H. & Ong, T. A. A review on the accuracy of bladder cancer detection methods. J. Cancer 10, 4038 (2019).
Planz, B. et al. The role of urinary cytology for detection of bladder cancer. Eur. J. Surg. Oncol. 31, 304–308 (2005).
Giordano, A. & Soria, F. Role and efficacy of current biomarkers in bladder cancer. AME Med. J. 5, 6–6 (2020).
Shariat, S. F., Karam, J. A., Lotan, Y. & Karakiewizc, P. I. Critical evaluation of urinary markers for bladder cancer detection and monitoring. Rev. Urol. 10, 120 (2008).
Sharma, S., Zippe, C. D., Pandrangi, L., Nelson, D. & Agarwal, A. Exclusion criteria enhance the specificity and positive predictive value of NMP22 and BTA stat. J. Urol. 162, 53–57 (1999).
Bian, B. et al. Urinary exosomal long non-coding RNAs as noninvasive biomarkers for diagnosis of bladder cancer by RNA sequencing. Front. Oncol. 12, 976329 (2022).
Batista, R. et al. Biomarkers for bladder cancer diagnosis and surveillance: a comprehensive review. Diagnostics 10, 39 (2020).
Xu, C. et al. Identification of immune subtypes to guide immunotherapy and targeted therapy in clear cell renal cell carcinoma. Aging 14, 6917 (2022).
Zhong, W. et al. Characterization of hypoxia-related molecular subtypes in clear cell renal cell carcinoma to aid immunotherapy and targeted therapy via multi-omics analysis. Front. Mol. Biosci. 8, 615 (2021).
Qiu, H. et al. Identification and validation of an individualized prognostic signature of bladder cancer based on seven immune related genes. Front. Genet. 11, 507802 (2020).
Liang, Y., Su, Q. & Wu, X. Identification and validation of a novel six-gene prognostic signature of stem cell characteristic in colon cancer. Front. Oncol. 10, 571655 (2021).
Kourou, K., Exarchos, T. P., Exarchos, K. P., Karamouzis, M. V. & Fotiadis, D. I. Machine learning applications in cancer prognosis and prediction. Comput. Struct. Biotechnol. J. 13, 8–17 (2015).
Redondo-Gonzalez, E. et al. Bladder carcinoma data with clinical risk factors and molecular markers: A cluster analysis. Biomed Res. Int. 2015, 168682 (2015).
Sugeeta, S. S., Sharma, A., Ng, K., Nayak, A. & Vasdev, N. Biomarkers in bladder cancer surveillance. Front. Surg. 8, 735868 (2021).
Zhang, S. et al. Identification of prognostic biomarkers for bladder cancer based on DNA methylation profile. Front. Cell Dev. Biol. 9, 31 (2022).
KaramiFath, M. et al. Current understanding of epigenetics role in melanoma treatment and resistance. Cancer Cell Int. 22, 1–23 (2022).
KaramiFath, M. et al. The role of epigenetic modifications in drug resistance and treatment of breast cancer. Cell. Mol. Biol. Lett. 27, 1–25 (2022).
Goldman, M. J. et al. Visualizing and interpreting cancer genomics data via the Xena platform. Nat. Biotechnol. 38, 675–678 (2020).
Xie, C. et al. Differential methylation values in differential methylation analysis. Bioinformatics 35, 1094–1097 (2019).
Du, P. et al. Comparison of Beta-value and M-value methods for quantifying methylation levels by microarray analysis. BMC Bioinform. 11, 1–9 (2010).
Ritchie, M. E. et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 43, e47–e47 (2015).
Gaujoux, R. & Seoighe, C. A flexible R package for nonnegative matrix factorization. BMC Bioinform. 11, 1–9 (2010).
Sehgal, S., Singh, H., Agarwal, M., Bhasker, V. & Shantanu. Data analysis using principal component analysis. 2014 Int. Conf. Med. Imaging, m-Health Emerg. Commun. Syst. MedCom 2014 45–48 (2014) doi:https://doi.org/10.1109/MEDCOM.2014.7005973.
Shi, N., Liu, X. & Guan, Y. Research on k-means clustering algorithm: An improved k-means clustering algorithm, in 3rd Int. Symp. Intell. Inf. Technol. Secur. Informatics, IITSI 2010 63–67 (2010) https://doi.org/10.1109/IITSI.2010.74.
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cbioportal. Sci. Signal. 6, l1 (2013).
Mermel, C. H. et al. GISTIC2.0 facilitates sensitive and confident localization of the targets of focal somatic copy-number alteration in human cancers. Genome Biol. 12, 1–14 (2011).
Yoshihara, K. et al. Inferring tumour purity and stromal and immune cell admixture from expression data. Nat. Commun. 4, 1–11 (2013).
Chen, B., Khodadoust, M. S., Liu, C. L., Newman, A. M. & Alizadeh, A. A. Profiling tumor infiltrating immune cells with CIBERSORT. Methods Mol. Biol. 1711, 243 (2018).
Venkatesh, K. V., Darunte, L. & Jayadeva Bhat, P. Wilcoxon rank sum test. Encycl. Syst. Biol. https://doi.org/10.1007/978-1-4419-9863-7_1185 (2013).
Ashburner, M. et al. Gene ontology: tool for the unification of biology. The gene ontology consortium. Nat. Genet. 25, 25–29 (2000).
Kanehisa, M. & Goto, S. KEGG: Kyoto encyclopedia of genes and genomes. Nucleic Acids Res. 28, 27–30 (2000).
Chen, E. Y. et al. Enrichr: interactive and collaborative HTML5 gene list enrichment analysis tool. BMC Bioinform. 14, 1–14 (2013).
Borgan, Ø. Modeling Survival Data: Extending the Cox Model, in Therneau, TM & Grambsch P.M., , 2000. No. of pages: xiii + 350. Stat. Med. 20, 2053–2054 (Springer-Verlag, New York, 2001).
Harrell, F. E. Cox Proportional Hazards Regression Model. 465–507 (2001) https://doi.org/10.1007/978-1-4757-3462-1_19.
Hastie, T., Qian, J., Repositary, K. T.-C. R. & 2021, undefined. An Introduction to glmnet. cloud.r-project.org (2023).
Vasquez, M. M. et al. Least absolute shrinkage and selection operator type methods for the identification of serum biomarkers of overweight and obesity: simulation and application. BMC Med. Res. Methodol. 16, 1–19 (2016).
Zhou, G. et al. NetworkAnalyst 3.0: A visual analytics platform for comprehensive gene expression profiling and meta-analysis. Nucleic Acids Res. 47, W234–W241 (2019).
Davies, M. J. et al. Developing the risk score. (2017).
Stalpers, L. J. A., Kaplan, E. L. & Edward, L. Kaplan and the Kaplan–Meier survival curve. BSHM Bull. 33, 109–135 (2018).
Blanche, P., Dartigues, J. F. & Jacqmin-Gadda, H. Estimating and comparing time-dependent areas under receiver operating characteristic curves for censored event times with competing risks. Stat. Med. 32, 5381–5397 (2013).
Hajian-Tilaki, K. Receiver operating characteristic (ROC) curve analysis for medical diagnostic test evaluation. Casp. J. Intern. Med. 4, 627 (2013).
Floer, M. et al. Higher adenoma detection rates with endocuff-assisted colonoscopy—A randomized controlled multicenter trial. PLoS One 9, e114267 (2014).
Xiao, N., Xu, Q.-S. & Li, M.-Z. hdnom: Building Nomograms for Penalized Cox Models with High-Dimensional Survival Data. (2016). https://doi.org/10.1101/065524.
Lee, J. S. et al. Expression signature of E2F1 and its associated genes predict superficial to invasive progression of bladder tumors. J. Clin. Oncol. 28, 2660–2667 (2010).
Tang, Z., Kang, B., Li, C., Chen, T. & Zhang, Z. GEPIA2: an enhanced web server for large-scale expression profiling and interactive analysis. Nucleic Acids Res. 47, W556–W560 (2019).
Lee, S. J. et al. Interleukin-20 promotes migration of bladder cancer cells through extracellular signal-regulated kinase (ERK)-mediated MMP-9 protein expression leading to nuclear factor (NF-κB) activation by inducing the up-regulation of p21(WAF1) protein expression. J. Biol. Chem. 288, 5539–5552 (2013).
Goulet, C. R. et al. Cancer-associated fibroblasts induce epithelial-mesenchymal transition of bladder cancer cells through paracrine IL-6 signalling. BMC Cancer 19, 1–13 (2019).
Chen, M. F., Lin, P. Y., Wu, C. F., Chen, W. C. & Wu, C. Te. IL-6 expression regulates tumorigenicity and correlates with prognosis in bladder cancer. PLoS One 8, e61901 (2013).
Chandrashekar, D. S. et al. UALCAN: An update to the integrated cancer data analysis platform. Neoplasia 25, 18–27 (2022).
Li, T. et al. TIMER: A web server for comprehensive analysis of tumor-infiltrating immune cells. Cancer Res. 77, e108 (2017).
Sun, D. et al. TISCH: A comprehensive web resource enabling interactive single-cell transcriptome visualization of tumor microenvironment. Nucleic Acids Res. 49, D1420–D1430 (2021).
Wang, L. et al. A reference profile-free deconvolution method to infer cancer cell-intrinsic subtypes and tumor-type-specific stromal profiles. Genome Med. 12, 1–12 (2020).
Oh, D. Y. et al. Intratumoral CD4+ T cells mediate anti-tumor cytotoxicity in human bladder cancer. Cell 181, 1612-1625.e13 (2020).
Westrich, J. A., Vermeer, D. W., Colbert, P. L., Spanos, W. C. & Pyeon, D. The multifarious roles of the chemokine CXCL14 in cancer progression and immune responses. Mol. Carcinog. 59, 794 (2020).
Spruance, S. L., Reid, J. E., Grace, M. & Samore, M. Hazard ratio in clinical trials. Antimicrob. Agents Chemother. 48, 2787 (2004).
Ghasemzadeh, A., Bivalacqua, T. J., Hahn, N. M. & Drake, C. G. New strategies in bladder cancer: A second coming for immunotherapy. Clin. Cancer Res. 22, 793–801 (2016).
Milowsky, M. I. et al. Guideline on muscle-invasive and metastatic bladder cancer (European Association of Urology Guideline): American society of clinical oncology clinical practice guideline endorsement. J. Clin. Oncol. 34, 1945–1952 (2016).
Bellmunt, J. et al. Bladder cancer: ESMO practice guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 25, iii40–iii48 (2014).
Zhu, J. et al. Identification of immune-related genes as prognostic factors in bladder cancer. Sci. Rep. 10, 1–13 (2020).
Li, X. et al. Identification of the prognostic biomarkers CBX6 and CBX7 in bladder cancer. Diagnostics 13, 1393 (2023).
Tang, F. et al. A 7-gene signature predicts the prognosis of patients with bladder cancer. BMC Urol. 22, 1–12 (2022).
Tang, F. et al. A 7-gene signature predicts the prognosis of patients with bladder cancer. BMC Urol. 22, 1–12 (2022).
Xing, P., Jiang, Z. & Liu, Y. Construction and validation of a gene signature related to bladder urothelial carcinoma based on immune gene analysis. BMC Cancer 22, 1–18 (2022).
Kim, H. J., Lee, H. N., Jeong, M. S. & Jang, S. B. Oncogenic KRAS: Signaling and Drug Resistance. Cancers 13, 5599 (2021).
Ribatti, D., Tamma, R. & Annese, T. Epithelial-mesenchymal transition in cancer: a historical overview. Transl. Oncol. 13, 100773 (2020).
Li, L. Y., Guan, Y. Di., Chen, X. S., Yang, J. M. & Cheng, Y. DNA repair pathways in cancer therapy and resistance. Front. Pharmacol. 11, 629266 (2021).
Ganapathy-Kanniappan, S. & Geschwind, J. F. H. Tumor glycolysis as a target for cancer therapy: progress and prospects. Mol. Cancer 12, 1–11 (2013).
Alzahrani, A. S. PI3K/Akt/mTOR inhibitors in cancer: At the bench and bedside. Semin. Cancer Biol. 59, 125–132 (2019).
Joseph, M. & Enting, D. Immune responses in bladder cancer-role of immune cell populations, prognostic factors and therapeutic implications. Front. Oncol. 9, 1270 (2019).
Baras, A. S. et al. The ratio of CD8 to Treg tumor-infiltrating lymphocytes is associated with response to cisplatin-based neoadjuvant chemotherapy in patients with muscle invasive urothelial carcinoma of the bladder. Oncoimmunology 5, e1134412 (2016).
Shi, M. J., Meng, X. Y., Wu, Q. J. & Zhou, X. H. High CD3D/CD4 ratio predicts better survival in muscle-invasive bladder cancer. Cancer Manag. Res. 11, 2987 (2019).
Colquhoun, A. J. & Mellon, J. K. Epidermal growth factor receptor and bladder cancer. Postgrad. Med. J. 78, 584–589 (2002).
Sayan, A. E. et al. Fra-1 controls motility of bladder cancer cells via transcriptional upregulation of the receptor tyrosine kinase AXL. Oncogene 31, 1493–1503 (2012).
Hayden, A. et al. The Nrf2 transcription factor contributes to resistance to cisplatin in bladder cancer. Urol. Oncol. 32, 806–814 (2014).
Casalou, C., Ferreira, A. & Barral, D. C. The role of ARF family proteins and their regulators and effectors in cancer progression: A therapeutic perspective. Front. Cell Dev. Biol. 8, 217 (2020).
Kim, T. W. et al. SH3RF2 functions as an oncogene by mediating PAK4 protein stability. Carcinogenesis 35, 624–634 (2014).
Bryan, R. T. Cell adhesion and urothelial bladder cancer: the role of cadherin switching and related phenomena. Philos. Trans. R. Soc. B Biol. Sci. 370, 20140042 (2015).
Ofer, D. & Linial, M. Inferring microRNA regulation: A proteome perspective. Front. Mol. Biosci. 9, 916639 (2022).
Liu, Q. et al. Integrative omics analysis reveals the importance and scope of translational repression in microRNA-mediated regulation. Mol. Cell. Proteomics 12, 1900–1911 (2013).
Wang, W., Zhang, L., Sun, J., Zhao, Q. & Shuai, J. Predicting the potential human lncRNA–miRNA interactions based on graph convolution network with conditional random field. Brief. Bioinform. 23, bbac463 (2022).
Wang, T., Sun, J. & Zhao, Q. Investigating cardiotoxicity related with hERG channel blockers using molecular fingerprints and graph attention mechanism. Comput. Biol. Med. 153, 106464 (2023).
Sun, F., Sun, J. & Zhao, Q. A deep learning method for predicting metabolite–disease associations via graph neural network. Brief. Bioinform. 23, bbad226 (2022).
Liu, W. et al. MPCLCDA: predicting circRNA–disease associations by using automatically selected meta-path and contrastive learning. Brief. Bioinform. 24, bbad227 (2023).
Liu, W. et al. NSCGRN: A network structure control method for gene regulatory network inference. Brief. Bioinform. 23, bbac156 (2022).
Li, X. et al. Caspase-1 and Gasdermin D afford the optimal targets with distinct switching strategies in nlrp1b inflammasome-induced cell death. Research 2022, 9838341–9838341 (2022).
Xu, F. et al. Specificity and competition of mRNAs dominate droplet pattern in protein phase separation. Phys. Rev. Res. 5, 023159 (2023).
Acknowledgements
The authors express their gratitude to the University of Dhaka, Bangladesh, for extending an International Publication Grant to cover the APC payment.
Funding
The funding for this research was provided by the University Grant Commission for Dhaka University (UGC-DU) and awarded to Dr. Md. Omar Faruk under the reference number Reg/Admin-3/29875 for the year 2023–24. Additionally, the article processing charge (APC) was covered by the University of Dhaka administration.
Author information
Authors and Affiliations
Contributions
D.C.: Investigation, Data curation, Methodology, Formal analysis, Writing—Original draft. S.I.M.: Data curation, Writing—Original draft preparation, Visualization. T.S.: Visualization, Investigation, Validation. M.I.H.: Writing—Reviewing, Editing, Conceptualization. M.O.F.: Writing—Reviewing, Conceptualization, Supervision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chatterjee, D., Mou, S.I., Sultana, T. et al. Identification and validation of prognostic signature genes of bladder cancer by integrating methylation and transcriptomic analysis. Sci Rep 14, 368 (2024). https://doi.org/10.1038/s41598-023-50740-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-50740-x
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.