Abstract
We investigated the whole blood GLUT1 mRNA expression and serum pigment epithelium-derived factor (PEDF), interleukin-6 (IL-6), fetuin-A, and pentraxin-3 (PTX3) levels in psoriatic patients and tested their correlations with the severity of psoriasis using the psoriasis area and severity index (PASI) score. Also, we tested the GLUT1 mRNA expression after an in vitro treatment of human skin fibroblast (HSF) cell lines with PEDF. The case–control part of the study recruited 74 participants (44 psoriatic patients and 30 healthy volunteers). Whole blood GLUT1 mRNA fold changes were estimated by RT-PCR, and serum PEDF, IL-6, fetuin-A, and PTX3 levels were measured by ELISA kits. In the experimental part, the HSF cell lines were treated with different concentrations of PEDF for different times to test its effect on the GLUT1 mRNA expression. The whole blood GLUT 1 expression significantly increased in psoriatic patients and correlated positively with serum IL-6, fetuin-A, PTX3 levels and with the severity of psoriasis while negatively with serum PEDF levels. The PEDF-treated HSF cell lines showed a time- and dose-dependent decline in the GLUT 1 mRNA expression. The whole blood GLUT 1 mRNA is a non-invasive biomarker that is associated with the severity of psoriasis. PEDF represses GLUT 1 expression and may be a potential therapeutic agent in psoriasis.
Trial registration: ClinicalTrials.gov Identifier: NCT04242082.
Similar content being viewed by others
Introduction
Psoriasis is a chronic non-communicable disfiguring skin disorder. It manifests as scaly plaques, pain, itching, and sometimes bleeding1. The prevalence of psoriasis is 2–4% worldwide2 while ranges from 0.19 to 3% in Egypt3.
The exact cause of psoriasis is still unknown, but immune-metabolic, inflammatory, and genetic factors are thought to play a role4. Glucose transporter-1 gene (Glut1) overexpression is an early step in the pathogenesis of psoriasis. Glut1 enhances epidermal hyperproliferation, inflammation, and angiogenesis and is associated with the psoriasis severity and its metabolic comorbidities5,6. Previous studies relied mainly on skin lesion biopsies to report data about GLUT1 and its gene expression5,6,7,8.
Pigment epithelium-derived factor (PEDF; a 50-kDa glycoprotein) is a member of the serine protease inhibitor gene family. It is encoded by Serpin Family F Member 1 (SERPINF1/EPC1) on chromosome 17p13.19. It has an antiangiogenic effect. Topical application of PEDF on a mouse model of psoriatic disease reduced the skin proliferation and angiogenesis10.
Being immune-metabolic mediated, psoriatic patients were found to have higher levels of interleukin-6 (IL-6), fetuin-A, and pentraxin-3 (PTX3) than healthy individuals11,12,13,14,15.
The current work aimed to investigate the whole blood GLUT1 mRNA expression and serum PEDF, IL-6, fetuin-A, and PTX3 levels in psoriatic patients and tested their correlations with the severity of psoriasis using the psoriasis area and severity index (PASI) score. Also, the study tested the GLUT1 mRNA expression after an in vitro treatment of HSF cell lines with different concentrations of PEDF for different times.
Materials and methods
The current study was conducted in the Medical Biochemistry Department, Faculty of Medicine, Assiut University, in collaboration with Dermatology Department, Assiut University Hospital. The study was reviewed and authorized by the local ethics committee, Faculty of Medicine, Assiut University (IRB: 17101042). It is carried out in compliance with the Declaration of Helsinki16.
Sample size calculations
We used EPI Info software version 6 to determine the sample size required for our study. We assumed that 35% of psoriatic patients and 1% of healthy controls would have increased GLUT1 expression, with 0% makes5. Based on these assumptions, we needed at least 25 people in each group.
The study included 74 participants divided into two groups: a healthy control group (G1, n = 30) and a psoriatic group (G2, n = 44). Each participant provided informed written consent. Psoriasis was diagnosed based on skin examination and assessment using the Psoriasis Area and Severity Index (PASI) score. It measures the severity and extent of psoriasis by assessing the redness, thickness, and scaling of psoriasis plaques in four body regions: the head, trunk, arms, and legs. Each region is scored on a scale of 0–4, with 0 indicating no psoriasis and 4 indicating severe psoriasis. The PASI score is then calculated by multiplying the score for each region by the area of the body region affected. The total PASI score can range from 0 to 72, with higher scores indicating more severe psoriasis17. Severity was classified as mild, moderate, severe, and very severe when 0 ≤ PASI ≤ 5, 5 < PASI ≤ 12, 12 < PASI ≤ 20, and PASI > 20, respectively17,18.
Participants were excluded if they had diabetes mellitus or any other dermatological or systemic disease that affects GLUT1 mRNA expression, such as cancer or diabetic nephropathy19. Patients taking systemic treatment were also excluded. All participants underwent a complete medical history and physical examination, including blood pressure measurements and body mass index (BMI) calculation (kg/m2)20.
Laboratory work
Under aseptic conditions about 10 ml of venous blood was collected and divided into three tubes; 2 ml was collected as whole blood on fluoride-containing tubes for glycated hemoglobin percentage (HbA1c%) and random blood glucose (RBG) analysis. Four ml was collected on EDTA containing tubes as whole blood and stored at – 80 °C. The other 4 ml was collected in a plain tube, left to clot, centrifuged at 3000 rpm for 15 min, and the sera were retrieved, aliquoted in Eppendorf tubes, and stored frozen at − 80 °C. Mid-stream freshly voided urine samples were taken from all participants to measure urinary albumin to exclude diabetic nephropathy21.
Other laboratory investigations including kidney function tests, and liver function tests lipid profiles were performed, for all patients as routine laboratory work in outpatient clinic lab, Assiut University Hospital.
Serum PEDF levels were measured by human PEDF ELISA kit (Cat# SG-11305, Sinogeneclon, China). Serum IL-6, fetuin-A, and PTX3 levels were measured by human ELISA Kit (abcam, Cambridge Biomedical Campus, Cambridge, CB2 0AX, UK); cat# ab 178013, ab269372, and ab214570, respectively.
Real-time quantitative polymerase chain reaction analysis (RT-PCR)
The frozen blood was allowed to melt on ice to increase total RNA yield22. Then as fast as possible the samples were subjected to total RNA extraction using total RNA mini extraction kit (Spin column) (Applied Biotechnology Institute, Inc, San Luis Obispo, CA United States). The blood samples were lysed using RNA lysis buffer which was followed by addition of chloroform to obtain the aqueous layer. The aqueous layer was added to 70% ethanol then the mixture was transferred to a spin column followed by centrifugation and the flow through was discarded. A washing buffer was added to each spin column with discarding the flow through then elution buffer were added to the center of the column followed by centrifugation of the centrifuge tube containing spin-column. Total RNA concentration and purity were tested using a NanoDrop spectrophotometer (BioTeck, Epoch, USA). RNA was then kept at − 80 °C till being used. Total RNA (300 ng) was used for cDNA synthesis using TOPscript TM Reverse Transcriptase (TOPscriptTM cDNA Synthesis Kit, Enzynomics, Daejeon, Korea). For each cDNA preparation, the total volume was 20 μl using a random hexamer primer. The condition used for cDNA synthesis, by thermal cycler (Applied Biosystem, USA), was at 25 °C for 10 min, 50 °C for 60 min, and the reaction was inactivated at 95 °C for 5 min.
Amplification reactions were performed in a volume of 10 μl with 5 µl of PowerUp SYBR Master Mix (Applied Biosystems, USA), 0.3 µl of each of primer forward and reverse, 3.4 µl of RNAase free water, and 1 µl of cDNA template23.
The primers used for GLUT 1, forward: 5′ GATTCCCAAGTGTGAGTCGC 3′, GLUT 1, reverse: 5′ GACATCATTGCTGGCTGGAG 3′ with accession number NM_006516.424. While housekeeping gene detection primer sets were glyceraldehyde-3-phosphate dehydrogenase (GABDH) forward: 5′ CACCACACTGAATCTCCCCT 3′, and GABDH, reverse: 5′ TGGTTGAGCACAGGGTACTT 3′ with accession number NM_001357943.225. Amplification consisted of an initial denaturation step at 95 °C for 10 min followed by 40 cycles of 15 s at 94 °C, 30 s at 58.5 °C, and 30 s at 72 °C. Performance and optimal annealing temperatures of the PCR primers were first tested with gradient PCR. Quantitative PCR was performed using a CFX Connect Real-time PCR Detection System (Bio-Rad, Hercules, CA, USA). The fold changes of GLUT 1 mRNA were calculated using the 2−ΔΔCT method26.
In vitro treatment of HSF cell lines with different concentrations of PEDF
The normal HSF (ATCC, USA, Cat # CRL-7449) was obtained from NAWAH-Cell Culture Unit, Cairo, Egypt. Cells were maintained in growth medium consisting of Dulbecco’s Modified Eagle Medium (DMEM), high glucose supplemented with 10% fetal bovine serum (FBS), and 1% penicillin/streptomycin (10,000 U/ml) (all from Gibco,USA) in an incubator controlled at 37 °C, 95% humidity, and 5% CO2 in the CO2 incubator (Contherm mitre 4000, Contherm Scientific, Hutt city, New Zealand). Human recombinant PEDF (Cat # SRP4988) was obtained from Sigma-Aldrich, Germany. The cell lines were treated with PEDF in different concentrations (20, 50, 100, 250, and 500 ng/ml) for 24, 48, and 72 h. Untreated and treated cell lines were then subjected to total RNA extraction and RT-PCR for GLUT 1 mRNA expression assessment27.
Statistical analysis
The statistical analysis was performed using SPSS version 26.0 (IBM-SPSS, Chicago, IL, USA). After testing the normality, Independent-Samples T-test and one-way analysis of variance (ANOVA) test were carried out to compare means28. Categorical variables were compared by Chi-square test29. The correlations between the variables were analyzed using the Pearson correlation coefficient test. Gene expression profile modulation was evaluated by comparing the Ct values by 2−∆∆Ct method26. The receiver operating characteristic (ROC) curve was used to detect the ability of the studied parameters to differentiate psoriatic patients from non-psoriatic healthy control30. Regression analysis in the entire sample was performed to investigate the independent associations of significant variables with the whole blood Glut 1 mRNA fold changes as dependent variable. p value ≤ 0.05 was considered significant.
Ethics approval and consent to participate
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board at the Faculty of Medicine, Assiut University [IRB: 17101042]. A written informed consent was obtained from the parents.
Results
Age, gender, BMI, and other laboratory findings of studied groups
Nonsignificant differences between the two groups were found in age and sex. The BMI values were significantly higher in G2 than in G1. Although some significant differences were found in liver function tests and serum albumin levels, the values were still within the normal ranges in both groups (Table 1).
Whole-blood GLUT1 mRNA fold changes and serum levels of IL-6, fetuin-A, and PTX3 were significantly higher, while serum PEDF levels were significantly lower, in psoriatic patients than in healthy individuals (Table 1).
Disease history and PASI score in the psoriatic patients (G2)
The duration of psoriasis in G2 was 6.9 ± 4.9 years. The PASI score values were 16.9 ± 13.5. The G2 participants were categorized according to the PASI score categories into mild [n = 5 (11.3%)], moderate [n = 20 (45.5%)], severe [n = 8 (18.2%)], and very severe [n = 11 (25%)]. Fitzpatrick skin phototypes reported in the current work were type II [n = 2 (4.5%)], III [n = 9 (20.5%)], and IV [n = 33 (75%)].
Of the patients, 37 (84.1%) received topical treatment, and 14 (31.8%) received phototherapy. A family history of psoriasis and atopy was reported in 6 (13.6%) and 10 (22.7%) patients, respectively. None of the patients had psoriatic arthritis.
Comparison of different studied parameters by the PASI score categories in psoriatic patients (G2)
Whole-blood GLUT1 mRNA fold changes and serum levels of IL-6, fetuin-A, and PTX3 were significantly higher in the very severe group than in the severe, moderate, and mild groups. Serum PEDF levels were significantly lower in the very severe group than in the severe, moderate, and mild groups (Table 2).
Corrections
In the whole study sample, whole-blood GLUT1 mRNA fold changes were negatively correlated with serum PEDF levels and positively correlated with serum levels of IL-6, fetuin-A, and PTX3. Additionally, serum PEDF levels were negatively correlated with serum levels of IL-6, fetuin-A, and PTX3. Furthermore, there were positive correlations among serum levels of IL-6, fetuin-A, and PTX3 (Table 3).
Within the psoriatic group (G2), the Psoriasis Area and Severity Index (PASI) scores correlated positively with whole-blood GLUT1 mRNA fold changes and serum levels of IL-6, fetuin-A, and PTX3, and negatively with serum PEDF levels (Fig. 1).
Regression analysis
The effect strengths of different studied parameters on the Glut 1 mRNA fold changes are displayed in Table 4. A significant impact of serum PEDF levels was found.
ROC curve analysis for the studied parameters
The AUCs, cut-off points, sensitivities, and specificities of different study parameters for distinguishing cases of psoriasis from healthy individuals are shown in Fig. 2.
Receiver operating characteristic (ROC) curve for the capability of (a) whole blood GLUT 1 mRNA fold changes (b) serum pigment epithelium-derived factor (PEDF) levels, (c) serum interleukin-6 levels, (d) serum fetuin-A levels, and (e) serum pentraxin-3 levels to discriminate psoriatic patients from normal subjects. AUC area under the curve.
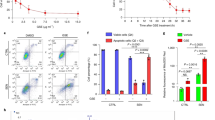
Effect of HSF treatment with PEDF on GLUT 1 mRNA expressions:
Using RT-PCR, GLUT1 mRNA fold changes were measured in HSF cell lines after treatment with different concentrations of PEDF. In our study, the treated cells showed both dose- and time-dependent decreases in GLUT1 mRNA fold changes (Fig. 3).
Discussion
To our knowledge, this is the first study to report higher levels of whole-blood Glut1 mRNA (non-invasively) in psoriatic patients. Additionally, the negative impact and reverse correlations between whole-blood Glut1 mRNA and serum PEDF levels, along with the dose- and time-dependent decreases in GLUT1 mRNA fold changes upon treatment of human fibroblast cell lines with PEDF, all suggest a possible therapeutic role for PEDF in psoriatic cases.
Glucose transporters (GLUTs) are transmembrane proteins with twelve membrane-spanning regions that facilitate glucose transport across the cell membrane31. Of these GLUTs, glucose transporter type 1 (GLUT1) is an insulin-independent glucose transporter that is present mainly in red blood cells, lymphocytes, brain, and the blood–brain barrier31,32. GLUT 1 is overexpressed in many cancers, allowing the cells to get more glucose for their energy production, growth, and proliferation33. Similar findings were reported in psoriatic keratinocytes7. Inhibition of GLUT1-mediated glucose uptake might control keratinocyte proliferation6. These findings are consistent with the results of the current study.
Also, our results are consistent with the findings of many previous studies5,6,7,8,34. GLUT1 concentration and gene expression were elevated in skin biopsies from psoriatic lesions compared to non-lesioned skin and normal control skin5. In one study, all skin biopsies from psoriatic patients expressed GLUT1 to varying degrees immunohistochemically34. Abdou et al. reported that GLUT1 was not expressed in normal control skin but was expressed in 76.6% of uninvolved and 86.7% of involved psoriatic skin8. Hodeib et al. reported that GLUT1 mRNA expression correlated positively with PASI score in skin biopsies5. Psoriatic lesions with pronounced acanthosis were more likely to express GLUT1 than lesions with mild to moderate acanthosis8. These results are consistent with the findings of the current study, but this study differs in that it used whole blood samples.
On the other hand, the significant positive correlation between duration of psoriasis and GLUT1 mRNA expression found in the current study contradicts the results of Hodeib et al., who reported no correlation between duration of psoriasis and GLUT1 expression immunohistochemically5.
The negative correlation between GLUT1 mRNA fold changes and serum PEDF levels in the current study was consistent with the findings of Calado et al.35. Additionally, we reported a positive correlation between GLUT1 mRNA fold changes and IL-6, fetuin-A, and PTX3 levels, which may indicate the multifactorial nature of psoriasis36.
Pigment epithelium-derived factor (PEDF) is a 50-kDa antiangiogenic protein, initially identified for its ability to induce differentiation in retinoblastoma cells37. Additionally, PEDF promotes a differentiated, non-proliferative state in various cell types37. It also serves as an antioxidant, protecting neurons from light-induced damage and glutamate excitotoxicity37. Normal human skin fibroblasts (HSF) express PEDF38,39. Consistent with the findings of the current study, PEDF levels were observed to be lower in psoriatic skin biopsies compared to normal skin40. The topical application of low molecular weight PEDF peptides in a mouse model of psoriatic disease led to a reduction in the thickness and angiogenesis of skin lesions10. In contrast to these findings, Nakajima et al., and Tekely et al. reported higher PEDF levels in the sera of psoriatic patients compared to controls, with no significant correlations between serum PEDF levels and the PASI score41,42.
In line with our findings, many previous studies have found high IL-6 levels and gene expression in the blood and skin lesions of psoriatic patients. These levels were associated with the severity of psoriasis and its complications13,43,44,45.
Fetuin-A is a glycoprotein produced by the liver that plays several important roles in the body, including regulating bone metabolism, inhibiting vascular calcification, protecting against inflammation, and regulating insulin activity46. Consistent with our results, serum fetuin-A levels were higher in psoriatic patients than healthy individuals and suggested to play a pivotal role in the pathogenesis of psoriasis and its accompanying inflammation and cardiometabolic complications14,46,47. On the other hand, some studies have reported lower levels of fetuin-A in psoriatic patients compared to healthy individuals48.
The PTX3 is an anti-inflammatory and anti-infection protein that activates immune cells. It has been linked to several diseases, including inflammatory diseases, cardiovascular disease, cancer49. PTX3 levels are elevated in psoriatic patients and have been reported as an indicator of psoriasis severity, as well as a useful marker for cardiovascular, metabolic, and joint involvement in these cases15,50,51,52.
The ROC curve analysis in the current study showed high diagnostic accuracies to distinguish psoriatic patients from non-psoriatic healthy people for the whole blood Glut 1 mRNA fold changes, and serum PEDF and PTX3 levels. The accuracy for the serum IL-6 and fetuin-A levels was only moderate.
The main limitation of the current study is its small sample size.
In conclusion, whole blood GLUT1 mRNA is a noninvasive parameter that is significantly increased in psoriatic patients. Its expression correlates with the severity of psoriasis, as well as with serum levels of IL-6, fetuin-A, and PTX3. Conversely, serum PEDF levels negatively correlate with whole blood GLUT1 mRNA expression. In vitro treatment of human fibroblast cell lines with PEDF significantly decreases GLUT1 mRNA expression in a dose- and time-dependent manner. Further research is necessary to investigate the potential of PEDF as a treatment for psoriasis.
Data availability
The data will be shared on reasonable request to the corresponding author.
Abbreviations
- GLUT 1:
-
Glucose transporter 1
- PEDF:
-
Pigment epithelium-derived factor,
- IL-6:
-
Interleukin-6 PTX3: pentraxin-3
- HSF:
-
Normal human skin fibroblast cell line
- Hep-G2:
-
A human hepatoma cell line
- RT-PCR:
-
Real time polymerase chain reaction
- ELISA:
-
Enzyme linked immunosorbent assay
- mRNA:
-
Messenger RNA
- T2DM:
-
Type 2 diabetes mellitus
- PASI:
-
Psoriasis Area Severity Index
- SERPINF1/EPC1:
-
Serpin Family F Member 1
- IRB:
-
Institutional Review Board
- BMI:
-
Body mass index
- EDTA:
-
Ethylenediaminetetraacetic acid
- HbA1c%:
-
Glycated hemoglobin percentage
- RNA:
-
Ribonucleic acid
- cDNA:
-
Complementary deoxyribonucleic acid
- NM:
-
Accession number links to the mRNA record in the nucleotide database
- GABDH :
-
Glyceraldehyde-3-phosphate dehydrogenase- forward
- DMEM:
-
Dulbecco’s modified eagle medium
- FBS:
-
Fetal bovine serum
- SPSS:
-
Statistical package for the social sciences
- Ct:
-
Cycle threshold
- ROC:
-
Receiver operating characteristic
- sAST:
-
Serum aspartate aminotransferase
- sALT:
-
Serum alanine aminotransferase
- salb:
-
Serum albumin
- BUN:
-
Blood urea nitrogen
- s-cr:
-
Serum creatinine
- HDL-c:
-
High density lipoprotein cholesterol
- LDL-c:
-
Low density lipoprotein cholesterol
- sTC:
-
Serum total cholesterol
- sTAG:
-
Serum triacylglycerol
- RBG:
-
Random blood glucose
- AUC:
-
Area under the curve
References
Eder, L. et al. Trends in the prevalence and incidence of psoriasis and psoriatic arthritis in Ontario, Canada: A population-based study. Arthritis Care Res. 71(8), 1084–1091 (2019).
Parisi, R., Symmons, D. P., Griffiths, C. E. & Ashcroft, D. M. Global epidemiology of psoriasis: A systematic review of incidence and prevalence. J. Investig. Dermatol. 133(2), 377–385 (2013).
Omar, S. S. & Helaly, H. A. Prevalence of ocular findings in a sample of Egyptian patients with psoriasis. Indian J. Dermatol. Venereol. Leprol. 84, 1 (2018).
Lee, E. B., Wu, K. K., Lee, M. P., Bhutani, T. & Wu, J. J. Psoriasis risk factors and triggers. Cutis 102(5S), 18–20 (2018).
Hodeib, A. A. H., Neinaa, Y. M. H., Zakaria, S. S. & Alshenawy, H. A. S. Glucose transporter-1 (GLUT-1) expression in psoriasis: Correlation with disease severity. Int. J. Dermatol. 57(8), 943–951 (2018).
Cibrian, D., de la Fuente, H. & Sánchez-Madrid, F. Metabolic pathways that control skin homeostasis and inflammation. Trends Mol. Med. 26(11), 975–986 (2020).
Huang, X. et al. Membrane-enriched solute carrier family 2 member 1 (SLC 2A1/GLUT 1) in psoriatic keratinocytes confers sensitivity to 2-deoxy-D-glucose (2-DG) treatment. Exp. Dermatol. 28(2), 198–201 (2019).
Abdou, A. G., Maraee, A. H., Eltahmoudy, M. & El-Aziz, R. A. Immunohistochemical expression of GLUT-1 and Ki-67 in chronic plaque psoriasis. Am. J. Dermatopathol. 35(7), 731–737 (2013).
Harries, R. L. et al. Impact of pigment epithelium-derived factor on colorectal cancer in vitro and in vivo. Oncotarget 9(27), 19192 (2018).
Abe, R. et al. Topical application of anti-angiogenic peptides based on pigment epithelium-derived factor can improve psoriasis. J. Dermatol. Sci. 57(3), 183–191 (2010).
Yamanaka, K., Yamamoto, O. & Honda, T. Pathophysiology of psoriasis: A review. J. Dermatol. 48(6), 722–731 (2021).
Arican, O., Aral, M., Sasmaz, S. & Ciragil, P. Serum levels of TNF-α, IFN-γ, IL-6, IL-8, IL-12, IL-17, and IL-18 in patients with active psoriasis and correlation with disease severity. Mediators Inflamm. 2005(5), 273–279 (2005).
Sobolev, V., Denisova, E., Chebysheva, S., Geppe, N. & Korsunskaya, I. IL-6 gene expression as a marker of pathological state in psoriasis and psoriatic arthritis. Bull. Exp. Biol. Med. 173(1), 77–80 (2022).
Okan, G., Baki, A. M., Yorulmaz, E., Doğru-Abbasoğlu, S. & Vural, P. Serum visfatin, fetuin-A, and pentraxin 3 levels in patients with psoriasis and their relation to disease severity. J. Clin. Lab. Anal. 30(4), 284–289 (2016).
Baran, A. et al. Potential predictive value of serum pentraxin 3 and paraoxonase 1 for cardiometabolic disorders development in patients with psoriasis—preliminary data. Metabolites 12(7), 580 (2022).
Rickham, P. P. Human experimentation. Code of ethics of the world medical association. Declaration of Helsinki. Brit. Med. J. 2(5402), 177 (1964).
Strober, B., Karki, C., Mason, M., Greenberg, J. D. & Lebwohl, M. Impact of Psoriasis Area and Severity Index (PASI) on patient reported outcomes in patients with psoriasis: Results from the Corrona Psoriasis Registry. J. Am. Acad. Dermatol. 76(6 Suppl 1), 406 (2017).
Feldman, S. A quantitative definition of severe psoriasis for use in clinical trials. J. Dermatol. Treat. 15(1), 27–29 (2004).
Avril, N. GLUT1 expression in tissue and 18F-FDG uptake. J. Nucl. Med. 45(6), 930–932 (2004).
Khanna, D., Peltzer, C., Kahar, P. & Parmar, M. S. Body mass index (BMI): A screening tool analysis. Cureus 14, 2 (2022).
Sumida, K. et al. Conversion of urine protein–creatinine ratio or urine dipstick protein to urine albumin–creatinine ratio for use in chronic kidney disease screening and prognosis: An individual participant–based meta-analysis. Ann. Internal Med. 173(6), 426–435 (2020).
Yamagata, H. et al. Optimized protocol for the extraction of RNA and DNA from frozen whole blood sample stored in a single EDTA tube. Sci. Rep. 11(1), 1–10 (2021).
Pyla, R., Poulose, N., Jun, J. Y. & Segar, L. Expression of conventional and novel glucose transporters, GLUT1,-9,-10, and-12, in vascular smooth muscle cells. Am. J. Physiol. Cell Physiol. 304(6), C574–C589 (2013).
Boscaro, C. et al. Non-genomic mechanisms in the estrogen regulation of glycolytic protein levels in endothelial cells. FASEB J. 34(9), 12768–12784 (2020).
Soraya, Z. et al. Donepezil hydrochloride as a novel inducer for osteogenic differentiation of mesenchymal stem cells on PLLA scaffolds in vitro. Biotechnol. J. 16(9), 2100112 (2021).
Schmittgen, T. D. & Livak, K. J. Analyzing real-time PCR data by the comparative CT method. Nat. Protoc. 3(6), 1101–1108 (2008).
Zhang, T., Guan, M., Xu, C., Chen, Y. & Lu, Y. Pigment epithelium-derived factor inhibits glioma cell growth in vitro and in vivo. Life Sci. 81(16), 1256–1263 (2007).
Hesamian, G. One-way ANOVA based on interval information. Int. J. Syst. Sci. 47(11), 2682–2690 (2016).
McHugh, M. L. The chi-square test of independence. Biochem. Med. 23(2), 143–149 (2013).
Hoo, Z. H., Candlish, J. & Teare, D. What is an ROC Curve? 357–359 (BMJ Publishing Group Ltd and the British Association for Accident, 2017).
Mueckler, M. & Thorens, B. The SLC2 (GLUT) family of membrane transporters. Mol. Aspects Med. 34(2–3), 121–138 (2013).
Cifuentes, M. et al. Insulin regulates GLUT1-mediated glucose transport in MG-63 human osteosarcoma cells. J. Cell. Physiol. 226(6), 1425–1432 (2011).
Zambrano, A., Molt, M., Uribe, E. & Salas, M. Glut 1 in cancer cells and the inhibitory action of resveratrol as a potential therapeutic strategy. Int. J. Mol. Sci. 20(13), 3374 (2019).
Park, J.-H. et al. Histopathological differential diagnosis of psoriasis and seborrheic dermatitis of the scalp. Ann. Dermatol. 28(4), 427–432 (2016).
Calado, S. M., Alves, L. S., Simão, S. & Silva, G. A. GLUT1 activity contributes to the impairment of PEDF secretion by the RPE. Mol. Vis. 22, 761 (2016).
Zhou, X., Chen, Y., Cui, L., Shi, Y. & Guo, C. Advances in the pathogenesis of psoriasis: From keratinocyte perspective. Cell Death Dis. 13(1), 81 (2022).
Barnstable, C. J. & Tombran-Tink, J. Neuroprotective and antiangiogenic actions of PEDF in the eye: Molecular targets and therapeutic potential. Progress Retinal Eye Res. 23(5), 561–577 (2004).
Longo, N. et al. Human fibroblasts express the insulin-responsive glucose transporter (GLUT4). Trans. Assoc. Am. Physicians 103, 202–213 (1990).
Nakashima, N. et al. Effect of dehydroepiandrosterone on glucose uptake in cultured human fibroblasts. Metabolism 44(4), 543–548 (1995).
Elbalshy, A. E. M., El-Refaie, A. M. & Akl, E. M. Expression of pigment epithelium-derived factor in psoriasis, verrucae, squamous cell carcinoma and normal skin: An immunohistochemical study. Indian J. Dermatol. Venereol. Leprol. 86, 4 (2020).
Nakajima, H., Nakajima, K., Tarutani, M. & Sano, S. The role of pigment epithelium-derived factor as an adipokine in psoriasis. Arch. Dermatol. Res. 304(1), 81–84 (2012).
Tekely, E., Szostakiewicz-Grabek, B., Krasowska, D. & Chodorowska, G. Serum levels of chemerin and pigment epithelium-derived factor in patients with psoriasis. Postępy Nauk Med. 31, 14–19 (2018).
Xu, H. et al. Soluble IL-6R-mediated IL-6 trans-signaling activation contributes to the pathological development of psoriasis. J. Mol. Med. 99, 1009–1020 (2021).
Andersen, C. S. B. et al. Blood cell biomarkers of inflammation and cytokine levels as predictors of response to biologics in patients with psoriasis. Int. J. Mol. Sci. 24(7), 6111 (2023).
Mиpaxмeдoвa, X. T., Caидpacyлoвa, Г. Б., Myxcимoвa, H. P. The role of inflammatory markers as IL 6, TNF alfa, INF gamma with psoriathic arth ritis and rates of comorbidity (2023).
Chekol Abebe, E. et al. Role of fetuin-A in the pathogenesis of psoriasis and its potential clinical applications. Clin. Cosmet. Investig. Dermatol. 20, 595–607 (2022).
Borsky, P. et al. C-reactive protein, chemerin, fetuin-A and osteopontin as predictors of cardiovascular risks in persons with psoriasis vulgaris. Physiol. Res. 70(3), 383 (2021).
Shehata, W. A., Basha, M. A., Gayed, I. M. & Elhagary, S. B. Relationship between disease severity and fetuin-A levels in patients with psoriasis. Indian J. Dermatol. Venereol. Leprol. 86, 586 (2020).
Wu, Q. et al. Pentraxin 3: A promising therapeutic target for autoimmune diseases. Autoimmunity Rev. 19(12), 102584 (2020).
Bevelacqua, V. et al. Long pentraxin 3: A marker of inflammation in untreated psoriatic patients. Int. J. Mol. Med. 18(3), 415–423 (2006).
Gündüz, Ö. S. et al. The relationship of carotid intima-media thickness with cell adhesion molecules and pentraxin-3 in patients with psoriatic arthritis. Aktuelle Rheumatol. 20, 20 (2022).
Gündüz, Ö. S. et al. The relationship of carotid intima-media thickness with cell adhesion molecules and pentraxin-3 in patients with psoriatic arthritis die relation der karotis-intima-media-Dicke zu Zelladhäsionsmolekülen und Pentraxin-3 bei Patienten mit. Akt Rheumatol. 48, 78–85 (2023).
Acknowledgements
The authors express their gratitude to the Research Grant Office, Faculty of Medicine, Assiut University for the participation in this study funding.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). This study was funded by the Research Grant Office, Faculty of Medicine, Assiut University.
Author information
Authors and Affiliations
Contributions
Conceptualization and study design: K.M.M., N.K.I., E.M.K.Y., supervision: K.M.M., N.K.I., E.M.K.Y., data curation: K.M.M., N.K.I., E.M.K.Y., S.E., and N.M.S. investigation: N.K.I., K.M.M., S.E., methodology: K.M.M., N.K.I., E.M.K.Y., S.E., software: K.M.M., and S.E., validation: N.K.I., E.M.K.Y., K.M.M., writing—initial draft, K.M.M., N.K.I., E.M.K.Y., and S.E., writing—review & editing K.M.M., N.K.I., and E.M.K.Y. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mohany, K.M., Elkady, S., Youssef, E.M.K. et al. Pigment epithelium-derived factor (PEDF) represses the glucose transporter 1 (GLUT1) mRNA expression and may be a potential therapeutic agent in psoriasis: a case–control and experimental study. Sci Rep 13, 21424 (2023). https://doi.org/10.1038/s41598-023-48565-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-48565-9
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.