Abstract
The purpose of the current study was to assess the frequency of overactive bladder syndrome (OBS) symptoms and their relationship to gastrointestinal symptoms in youth with abdominal pain-associated disorders of gut–brain interaction (AP-DGBI). This is a retrospective study of 226 youth diagnosed with an AP-DGBI. As part of standard care, all patients completed a symptom questionnaire regarding gastrointestinal and non-gastrointestinal symptoms including increased urinary frequency, nighttime urination, and urinary urgency. Overall, 54% of patients reported at least one OBS symptom. Increased frequency of urination was reported by 19%, urinary urgency by 34%, and nighttime urination by 36%. Increased frequency of urination and urinary urgency were associated with a change in stool form, a change in stool frequency, and in those fulfilling criteria for IBS. Increased frequency of urination was reported more frequently in those reporting predominantly loose stools (33% vs. 12%). Urinary symptoms are common in youth with AP-DGBI. Increased urinary frequency and urinary urgency are specifically associated with IBS, with increased urinary frequency being primarily associated with diarrhea predominant IBS. Further studies are needed to determine the impact of OBS on AP-DGBI severity and quality of life, and whether they impact DGBI treatment.
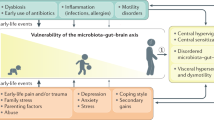
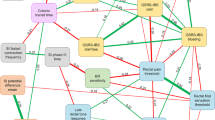
Similar content being viewed by others
Introduction
Chronic abdominal pain is quite common in children and adolescents1. The majority fulfill criteria for an abdominal pain-associated disorder of gut–brain interaction (AP-DGBI), with the most common being irritable bowel syndrome (IBS) and functional dyspepsia (FD)2,3,4. IBS is defined by the presence of abdominal pain in association with a change in stool frequency, a change in stool form, or a change (increase or decrease) in pain with a stool2. FD is defined by the presence of epigastric pain or burning, early satiety, or postprandial bloating2.
It is common for patients to fulfill criteria for both IBS and FD (i.e., FD/IBS overlap), particularly with the evolution to Rome IV criteria5,6,7. Furthermore, IBS and FD have been shown to overlap with other disorders such as gastroesophageal reflux (GERD) and overactive bladder syndrome (OBS)7,8. OBS is defined by three primary symptoms: increased urinary frequency, nighttime urination, and urinary urgency9. OBS has been associated with both IBS and FD in adults10,11,12,13. OBS has been associated with constipation in children and has been previously shown to be common in youth fulfilling FD criteria7,14,15,16,17. To our knowledge, associations of OBS symptoms with other gastrointestinal symptoms or more broadly across specific AP-DGBI diagnoses have not been previously reported for children and adolescents.
Evaluating relationships between OBS and gastrointestinal symptoms may have implication for understanding shared pathophysiology and may further delineate patient symptom heterogeneity within AP-DGBI diagnostic categories. The purpose of the current study was to assess the frequency of increased urinary frequency, nighttime urination, and urinary urgency in youth with AP-DGBI and to determine whether they are associated with specific gastrointestinal symptoms or AP-DGBI diagnosis.
Results
A total of 226 patients were evaluated. The mean age was 13.9 ± 2.7 years and 72% were female. The frequency of pain was daily in 62%, several times/week in 21%, and weekly in 17%. The frequency of individual gastrointestinal symptoms is shown in Table 1.
Rome IV criteria were fulfilled for FD by 89% and for IBS by 59% of patients; 52% fulfilled criteria for both FD and IBS. Reported stool frequency was 1–2 times daily in 62% of patients; 18% reported stooling less than daily and 21% reported having 3 or more stools daily. Predominantly hard stools were reported by 17% and predominantly loose stools were reported by 33%. No change in pain with stools was reported by 62% of patients while 24% reported decreased pain with stools and 14% reported increased pain with stools.
Overall, 54% of patients reported at least 1 overactive bladder symptom. The frequency of individual overactive bladder symptoms is shown in Fig. 1.
There were no significant differences between females and males with regards to increased urination (19% vs. 19%), nighttime urination (39% vs. 30%), or urinary urgency (36% vs. 28%). There were no significant differences between adolescents (≥ 13 years of age) and children with regards to increased urination (20% vs. 18%), nighttime urination (34% vs. 40%), or urinary urgency (34% vs. 33%).
Increased urination
Increased urination was reported more frequently in those fulfilling IBS criteria (25% vs. 10%; OR 3.14, 95%CI 1.42–6.91. Specifically, increased urination was reported more frequently in those reporting a change in stool form (32% vs. 10%; OR 4.04, 95%CI 1.99–8.20) or a change in stool frequency (38% vs. 10%; OR 5.18, 95%CI 2.56–10.46). The frequency of increased urination did not differ statistically between those fulfilling FD criteria as compared to those who did not (20% vs. 12%; OR 1.82, 95%CI 0.52–6.39). Increased urination was reported by 33% of those reporting predominantly loose stools vs. 12% of those not reporting predominantly loose stools (OR 3.82, 95%CI 1.90–7.69). Increased urination was reported by 15% of those reporting predominantly hard stools vs. 20% of those not reporting predominantly hard stools (OR 0.74, 95%CI 0.29–1.90).
Nighttime urination
There was no significant difference in the frequency of reporting nighttime urination in those reporting a change in stool form (41% vs. 40%), a change in stool frequency (37% vs. 29%), or those fulfilling criteria for IBS (37% vs. 35%) or FD (36% vs. 32%). Nighttime urination was reported by 44% of those reporting predominantly loose stools vs. 32% of those not reporting predominantly loose stools (OR 1.67, 95%CI 0.94–2.97). Increased urination was reported by 38% of those reporting predominantly hard stools vs. 36% of those not reporting predominantly hard stools (OR 1.14, 95%CI 0.56–2.31).
Urinary urgency
Urinary urgency was reported more frequently in those fulfilling IBS criteria (42% vs. 22%; OR 2.59, 95%CI 1.42–4.72) Specifically, urinary urgency was reported more frequently in those reporting a change in stool form (43% vs. 27%; OR 1.99, 95%CI 1.13–3.48) or a change in stool frequency (47% vs. 27%; OR 2.39, 95%CI 1.33–4.27). The frequency of urinary urgency did not differ statistically between those fulfilling FD criteria as compared to those who did not (35% vs. 24%; OR 1.69, 95%CI 0.65–4.43). Urinary urgency was reported by 41% of those reporting predominantly loose stools vs. 30% of those not reporting predominantly loose stools (OR 1.65, 95%CI 0.92–2.94). Increased urination was reported by 44% of those reporting predominantly hard stools vs. 32% of those not reporting predominantly hard stools (OR 1.67, 95%CI 0.82–3.37).
Discussion
OBS symptoms, particularly nighttime urination and urinary urgency, are common in youth with AP-DGBIs. The bladder may represent a potential source of pain given the frequency of patients reporting suprapubic pain, particularly in those reporting increased frequency of urination in the current study. OBS symptoms are associated with IBS, specifically diarrhea predominant IBS (IBS-D). Both increased frequency of urination and urinary urgency, but not nighttime urination, were associated with a change in stool frequency and form and increased urinary frequency was associated with predominantly loose stools. Hard stools did not increase the risk of OBS symptoms; this was somewhat surprising given the known association between constipation and OBS symptoms in children14,15,16,17. OBS symptoms have been associated with IBS in most, but not all, adult studies10,11,12,18. While OBS symptoms are also seen frequently in children with FD in the current and previous studies, they did not occur more frequently in those with FD as opposed to those without7. Additionally, we found no relationship between OBS symptoms and any specific FD symptoms. Previous adult studies have reported a relationship between OBS symptoms and FD but with a weaker association than that for IBS11,12,13.
The association of IBS and diarrhea with OBS symptoms would suggest shared pathophysiologic mechanisms or possibly visceral organ cross-sensitization. Shared pathophysiologic mechanisms may include hypersensitivity, inflammation (including allergy), an altered microbiome, altered epithelial function, and psychologic dysfunction. Visceral hypersensitivity with upregulation of TRPV1 channels is considered a key process in IBS19,20. OBS is associated with increased neural sensitivity and upregulation of TRPV1 has been reported in several studies9,21,22,23. Histologic inflammation also has been implicated in both OBS and IBS9,24,25. Both are associated with allergies and mast cells have been specifically implicated in both conditions and may be associated with increased visceral hypersensitivity9,20,24,26,27,28,29,30,31,32. Mast cell-derived histamine may be important in this process as it upregulates TRPV1 and can enhance activation of dorsal root ganglia sensory pathways shared by the bladder and colon9,20,33. Further, an altered microbiome has been demonstrated in both IBS and OBS; interestingly, OBS is associated with an altered microbiome in both the bladder and the intestinal tract9,34,35. Likewise, an altered epithelial barrier has been demonstrated in both OBS and IBS9,36. Lastly, both conditions are associated with depression and anxiety, which may be a shared cause, effect, or interactive process9,37. Alternatively, rather than only shared pathophysiology, the association of OBS and IBS could result from crosstalk or cross-sensitization as the bladder and colon share some common sensory pathways38. In an animal model, colitis results in increased bladder sensitivity, frequency of urination, and urgency without bladder inflammation9.
The main strength of the current study is the standardized symptom reporting in a relatively large group of youth with AP-DGBI. The primary limitation is that this type of study design only allows for assessment of associations and not cause-and-effect relationships. Additionally, the data did not assess the frequency of nighttime urination which may have negatively impacted sensitivity in assessing associations between nighttime urination and gastrointestinal symptoms. Lastly, urinary frequency could have been artificially inflated if patients with loose stools had more frequent stools as patients are likely to void whenever having a stool.
In conclusion, urinary symptoms are common in youth with AP-DGBI. We have demonstrated a specific association of increased urinary frequency and urgency with IBS, specifically in those with predominantly loose stools. If specific bladder and bowel symptoms do share common pathophysiology, bladder symptoms may be an indicator of underlying pathophysiologic targets for treatment of IBS. Further studies are needed to determine to what degree the bladder contributes to symptoms or quality of life, directly or indirectly, and whether the bladder represents a viable treatment target in itself in AP-DGBI patients.
Methods
This study retrospectively assessed 226 consecutive patients presenting to an abdominal pain clinic at Children’s Mercy Kansas City. All had been diagnosed with an AP-DGBI by a single board-certified pediatric gastroenterologist. Patients ranged in age from 8 to 18 years. All reported pain at least weekly for a minimum of 8 weeks. As part of standard care, all patients completed a symptom questionnaire including gastrointestinal and non-gastrointestinal symptoms. The symptoms included those regarding symptoms utilized in Rome IV criteria. The questionnaire also specifically asked about the presence of increased urinary frequency, nighttime urination, and urinary urgency. The questionnaire was completed within a REDCap database and the database was utilized for analyses. REDCap provides a secure, web-based platform for data acquisition39.
The study was approved by the Institutional Review Board (IRB) Children’s Mercy Kansas City which waived Informed consent. All methods were performed in accordance with the relevant guidelines and regulations and in accordance with the Declaration of Helsinki.
Statistical analysis
SPSS version 23 (SPSS Inc., Chicago, IL) was used to perform statistical analysis. Descriptive statistics are provided. Differences in frequencies were assessed by chi square analysis or the Fischer’s exact test as appropriate for cell sizes. Odds ratios (OR) with 95% confidence intervals (95%CI) were calculated. Differences were considered significant when the 95%CI did not contain 1.0.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Chitkara, D. K., Rawat, D. J. & Talley, N. J. The epidemiology of childhood recurrent abdominal pain in Western countries: A systematic review. Am. J. Gastroenterol. 100, 1868–1875 (2005).
Hyams, J. S. et al. Childhood gastrointestinal disorders: Child/adolescent. Gastroenterology 150, 1456–1468 (2016).
Walker, L. S. et al. Recurrent abdominal pain: Symptom subtypes based on the Rome II criteria for pediatric functional gastrointestinal disorders. J. Pediatr. Gastroenterol. Nutr. 38, 187–191 (2004).
Schurman, J. V. et al. Diagnosing functional abdominal pain with the Rome II criteria: Parent, child, and clinician agreement. J. Pediatr. Gastroenterol. Nutr. 41, 291–295 (2005).
Barberio, B. et al. Overlap of Rome IV irritable bowel syndrome and functional dyspepsia and effect on natural history: A longitudinal follow-up study. Clin. Gastroenterol. Hepatol. 20, e89–e101 (2022).
Edwards, T., Friesen, C. & Schurman, J. V. Classification of pediatric functional gastrointestinal disorders related to abdominal pain using Rome III vs. Rome IV criterions. BMC Gastroenterol. 18, 41 (2018).
Friesen, C. A., Rosen, J. M. & Schurman, J. V. Prevalence of overlap syndromes and symptoms in pediatric functional dyspepsia. BMC Gastroenterol. 16, 75 (2016).
Jones, M. P. et al. Overlap of heartburn, functional dyspepsia, and irritable bowel syndrome in a population sample: Prevalence, temporal stability, and associated comorbidities. Neurogastroenterol. Motil. 34, e14349 (2022).
Grundy, L., Caldwell, A. & Brierley, S. M. Mechanisms underlying overactive bladder and interstitial cystitis/painful bladder syndrome. Front. Neurosci. 12, 931 (2018).
Zingone, F., Iovino, P., Santonicola, A., Gallotta, S. & Ciacci, C. High risk of lower urinary tract symptoms in patients with irritable bowel syndrome. Tech. Coloproctol. 21, 433–438 (2017).
Persson, R. et al. The relationship between irritable bowel syndrome, functional dyspepsia, chronic fatigue, and overactive bladder syndrome: A controlled study 6 years after acute gastrointestinal infection. BMC Gastroenterol. 15, 66 (2015).
Wuestenberghs, F. et al. Overlaps with bladder pain syndrome and irritable bowel syndrome are associated with higher symptom burden and reduced quality of life in functional dyspepsia. Neurogastroenterol. Motil. 34, e14414 (2022).
Matsuzaki, J. et al. High frequency of overlap bladder between functional dyspepsia and overactive bladder. Neurogastroenterol. Motil. 24, 821–827 (2012).
Van Summeren, J. J. G. T. et al. Bladder symptoms in children with functional constipation: A systematic review. J. Pediatr. Gastroenterol. Nutr. 67, 552–560 (2018).
Veiga, M. L. et al. Constipation in children with isolated overactive bladders. J. Pediatr. Urol. 9, 945–949 (2013).
Sampaio, C. et al. Constipation and lower urinary tract dysfunction in children and adolescents: A population-based study. Front. Pediatr. 4, 101 (2016).
Borch, L., Hagstroem, S., Bower, W. F., Rittig, C. S. & Rittig, S. Bladder and bowel dysfunction and the resolution of urinary incontinence with successful management of bowel symptoms in children. Acta Paediatr. 102, e215–e220 (2013).
Kim, K. S., Kim, H. J., Lee, S. H., Cho, S. T. & Moon, H. S. Association between irritable bowel syndrome and overactive bladder. A research survey. Urology 109, 88–93 (2017).
Ludidi, S. et al. Rectal sensitivity as hallmark for irritable bowel syndrome: Defining the optimal cutoff. Neurogastroenterol. Motil. 24, 729-e346 (2012).
Wouters, M. M. et al. Histamine receptor H1-mediated sensitization of TRPV1 mediates visceral hypersensitivity in patients with irritable bowel syndrome. Gastroenterology 150, 875-887.e9 (2016).
Birder, L. A., Wolf-Johnston, A. S., Sun, Y. & Chai, T. C. Alteration in TRPV1 and muscarinic (M3) receptor expression and function in idiopathic overactive bladder urothelial cells. Acta Physiol. 207, 123–129 (2013).
Tykocki, N. R. et al. Development of stress-induced bladder insufficiency requires functional TRPV1 channels. Am. J. Physiol. Renal Physiol. 315, F1583–F1591 (2018).
Rosen, J. M. et al. TRPV1 and the MCP-1/CCR2 axis modulate post-UTI chronic pain. Sci. Rep. 8, 7188 (2018).
Burns, G. et al. Evidence for local and systemic immune activation in functional dyspepsia and the irritable bowel syndrome: A systematic review. Am. J. Gastroenterol. 114, 429–436 (2019).
Jiang, Y. H. et al. Urine biomarkers in ESSIC type 2 interstitial cystitis/bladder pain syndrome and overactive bladder with developing a novel diagnostic algorithm. Sci. Rep. 11, 914 (2021).
Yin, L. et al. Clinical correlation between overactive bladder and allergy in children. Front Pediatr. 9, 813161 (2022).
Zheng, Y. et al. Clinical observation of the correlation between overactive bladder and atopic constitution in children. Front. Pediatr. 9, 646118 (2021).
Friesen, C., Colombo, J. & Schurman, J. Update on the role of allergy in pediatric functional abdominal pain disorders: A clinical perspective. Nutrients 13, 2056 (2021).
Bashashati, M. et al. Colonic immune cells in irritable bowel syndrome: A systematic review and meta-analysis. Neurogastroenterol. Motil. 30, e13192 (2018).
Krammer, L., Sowa, A. S. & Lorentz, A. Mast cells in irritable bowel syndrome: A systematic review. J. Gastrointest. Liver Dis. 28, 463–472 (2019).
Friesen, H. J., Singh, M., Singh, V., Schurman, J. V. & Friesen, C. A. A survey of methodologies for assessing mast cell density and activation in patients with functional abdominal pain disorders. Gastrointest. Disorder. 3, 142–155 (2021).
Regauer, S., Gamper, M., Fehr, M. K. & Viereck, V. Sensory hyperinnervation distinguishes bladder pain syndrome/interstitial cystitis from overactive bladder syndrome. J. Urol. 197, 159–166 (2017).
Stromberga, Z., Chess-Williams, R. & Moro, C. Histamine modulation of urinary bladder urothelium, lamina propria and detrusor contractile activity via H1 and H2 receptors. Sci. Rep. 9, 3899 (2019).
Okamoto, T. et al. Altered gut microbiome associated with overactive bladder and daily urinary urgency. World J. Urol. 39, 847–853 (2021).
Liu, H. N. et al. Altered molecular signature of intestinal microbiota in irritable bowel syndrome patients compared with healthy controls: A systematic review and meta-analysis. Dig. Liver Dis. 49, 331–337 (2017).
Hanning, N. et al. Intestinal barrier dysfunction in irritable bowel syndrome: A systematic review. Ther. Adv. Gastroenterol. 14, 1756284821003585 (2021).
Zamani, M., Alizadeh-Tabari, S. & Zamani, V. Systematic review with meta-analysis: The prevalence of anxiety and depression in patients with irritable bowel syndrome. Aliment Pharmacol. Ther. 50, 132–143 (2019).
Halani, P. K., Andy, U. U., Rao, H. & Arya, L. A. Regions of the brain activated in bladder filling vs rectal distention in healthy adults: A meta-analysis of neuroimaging studies. Neurourol. Urodyn. 39, 58–65 (2020).
Harris, P. A. et al. Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 42, 377–381 (2009).
Author information
Authors and Affiliations
Contributions
H.F., P.T., J.S., J.C., and C.F. participated in study design. H.F. and C.F. completed the data analysis. H.F. and C.F. wrote the initial draft of the manuscript. H.F., P.T., J.S., J.C., and C.F. critically reviewed and revised the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Friesen, H.J., Thompson, P., Schurman, J.V. et al. Overactive bladder syndrome symptoms in youth with abdominal pain-associated disorders of gut–brain interaction. Sci Rep 13, 11042 (2023). https://doi.org/10.1038/s41598-023-37937-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-37937-w
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.