Abstract
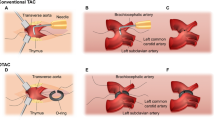
Cardiac disease is the main cause of death worldwide. Insufficient regeneration of the adult mammalian heart is a major driver of cardiac morbidity and mortality. Cardiac regeneration occurs in early postnatal mice, thus understanding mechanisms of mammalian cardiac regeneration could facilitate the development of novel therapeutic strategies. Here, we provide a detailed description of a neonatal mouse model of pressure overload by transverse aortic constriction (nTAC) that can be applied at postnatal days 1 and 7. We have previously used this model to demonstrate that mice are able to fully adapt to pressure overload following nTAC on postnatal day 1. In contrast, when nTAC is applied in the non-regenerative phase (at postnatal day 7), it is associated with a maladaptive response similar to that seen when transverse aortic constriction (TAC) is applied to adult mice. Once a user is experienced in nTAC surgery, the procedure can be completed in less than 10 min per mouse. We anticipate that this model will facilitate the discovery of therapeutic targets to treat patients or prevent pressure overload-induced cardiac failure in the future.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Hein, S. et al. Progression from compensated hypertrophy to failure in the pressure-overloaded human heart: structural deterioration and compensatory mechanisms. Circulation 107, 984–991 (2003).
Zhou, P. & Pu, W. T. Recounting cardiac cellular composition. Circ. Res. 118, 368–370 (2016).
Hesse, M., Welz, A. & Fleischmann, B. K. Heart regeneration and the cardiomyocyte cell cycle. Pflugers Arch. 470, 241–248 (2018).
Alkass, K. et al. No evidence for cardiomyocyte number expansion in preadolescent mice. Cell 163, 1026–1036 (2015).
Walsh, S., Ponten, A., Fleischmann, B. K. & Jovinge, S. Cardiomyocyte cell cycle control and growth estimation in vivo—an analysis based on cardiomyocyte nuclei. Cardiovasc. Res. 86, 365–373 (2010).
Maillet, M., van Berlo, J. H. & Molkentin, J. D. Molecular basis of physiological heart growth: fundamental concepts and new players. Nat. Rev. Mol. Cell Biol. 14, 38–48 (2013).
Heineke, J. & Molkentin, J. D. Regulation of cardiac hypertrophy by intracellular signalling pathways. Nat. Rev. Mol. Cell Biol. 7, 589–600 (2006).
Grund, A. & Heineke, J. Exercise makes the difference: deconstructing physiological hypertrophy in swine. J. Mol. Cell Cardiol. 79, 89–91 (2015).
Shimizu, I. & Minamino, T. Physiological and pathological cardiac hypertrophy. J. Mol. Cell. Cardiol. 97, 245–262 (2016).
Nakamura, M. & Sadoshima, J. Mechanisms of physiological and pathological cardiac hypertrophy. Nat. Rev. Cardiol. 15, 387–407 (2018).
Porrello, E. R. et al. Transient regenerative potential of the neonatal mouse heart. Science 331, 1078–1080 (2011).
Malek Mohammadi, M. et al. The transcription factor GATA4 promotes myocardial regeneration in neonatal mice. EMBO Mol. Med. 9, 265–279 (2017).
Zhu, W. et al. Regenerative potential of neonatal porcine hearts. Circulation 138, 2809–2816 (2018).
Ye, L. et al. Early regenerative capacity in the porcine heart. Circulation 138, 2798–2808 (2018).
Vujic, A. et al. Exercise induces new cardiomyocyte generation in the adult mammalian heart. Nat. Commun. 9, 1659 (2018).
Perrino, C. et al. Intermittent pressure overload triggers hypertrophy-independent cardiac dysfunction and vascular rarefaction. J. Clin. Invest. 116, 1547–1560 (2006).
Malek Mohammadi, M. et al. Induction of cardiomyocyte proliferation and angiogenesis protects neonatal mice from pressure overload-associated maladaptation. JCI Insight https://doi.org/10.1172/jci.insight.128336 (2019).
Rockman, H. A. et al. Segregation of atrial-specific and inducible expression of an atrial natriuretic factor transgene in an in vivo murine model of cardiac hypertrophy. Proc. Natl Acad. Sci. USA 88, 8277–8281 (1991).
Patten, R. D. & Hall-Porter, M. R. Small animal models of heart failure: development of novel therapies, past and present. Circ. Heart Fail. 2, 138–144 (2009).
Heineke, J. Screening for novel calcium-binding proteins that regulate cardiac hypertrophy: CIB1 as an example. Methods Mol. Biol. 963, 279–301 (2013).
Hartley, C. J. et al. Doppler velocity measurements from large and small arteries of mice. Am. J. Physiol. Heart Circ. Physiol. 301, H269–H278 (2011).
Tavakoli, R., Nemska, S., Jamshidi, P., Gassmann, M. & Frossard, N. Technique of minimally invasive transverse aortic constriction in mice for induction of left ventricular hypertrophy. J. Vis. Exp. https://doi.org/10.3791/56231 (2017).
Aurora, A. B. et al. Macrophages are required for neonatal heart regeneration. J. Clin. Invest. 124, 1382–1392 (2014).
Mahmoud, A. I. et al. Nerves regulate cardiomyocyte proliferation and heart regeneration. Dev. Cell 34, 387–399 (2015).
Karra, R. & Poss, K. D. Redirecting cardiac growth mechanisms for therapeutic regeneration. J. Clin. Invest. 127, 427–436 (2017).
Cui, M., Wang, Z., Bassel-Duby, R. & Olson, E. N. Genetic and epigenetic regulation of cardiomyocytes in development, regeneration and disease. Development https://doi.org/10.1242/dev.171983 (2018).
O’Tierney, P. F. et al. Reduced systolic pressure load decreases cell-cycle activity in the fetal sheep heart. Am. J. Physiol. Regul. Integ.r Comp. Physiol. 299, R573–R578 (2010).
Canseco, D. C. et al. Human ventricular unloading induces cardiomyocyte proliferation. J. Am. Coll. Cardiol. 65, 892–900 (2015).
Wohlschlaeger, J. et al. Hemodynamic support by left ventricular assist devices reduces cardiomyocyte DNA content in the failing human heart. Circulation 121, 989–996 (2010).
Mahmoud, A. I., Porrello, E. R., Kimura, W., Olson, E. N. & Sadek, H. A. Surgical models for cardiac regeneration in neonatal mice. Nat. Protoc. 9, 305–311 (2014).
Polizzotti, B. D., Ganapathy, B., Haubner, B. J., Penninger, J. M. & Kuhn, B. A cryoinjury model in neonatal mice for cardiac translational and regeneration research. Nat. Protoc. 11, 542–552 (2016).
deAlmeida, A. C., van Oort, R. J. & Wehrens, X. H. Transverse aortic constriction in mice. J. Vis. Exp. https://doi.org/10.3791/1729 (2010).
Wang, Z. et al. Mechanistic basis of neonatal heart regeneration revealed by transcriptome and histone modification profiling. Proc. Natl Acad. Sci. USA 116, 18455–18465 (2019).
Li, J. et al. Regulatory T-cells are required for neonatal heart regeneration. Preprint at bioRxiv https://doi.org/10.1101/355065 (2018).
Samak, M. et al. Cardiac hypertrophy: an introduction to molecular and cellular basis. Med. Sci. Monit. Basic Res. 22, 75–79 (2016).
Kilkenny, C., Browne, W. J., Cuthill, I. C., Emerson, M. & Altman, D. G. Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol 8, e1000412 (2010).
Appari, M. et al. C1q-TNF-related protein-9 promotes cardiac hypertrophy and failure. Circ. Res. 120, 66–77 (2017).
Grund, A. et al. TIP30 counteracts cardiac hypertrophy and failure by inhibiting translational elongation. EMBO Mol. Med. 11, e10018 (2019).
Heineke, J. et al. CIB1 is a regulator of pathological cardiac hypertrophy. Nat. Med. 16, 872–879 (2010).
Haubner, B. J., Schuetz, T. & Penninger, J. M. A reproducible protocol for neonatal ischemic injury and cardiac regeneration in neonatal mice. Basic Res. Cardiol. 111, 64 (2016).
Hesse, M. et al. Midbody positioning and distance between daughter nuclei enable unequivocal identification of cardiomyocyte cell division in mice. Circ. Res. 123, 1039–1052 (2018).
Li, Y. H. et al. Effect of age on peripheral vascular response to transverse aortic banding in mice. J. Gerontol. A 58, B895–B899 (2003).
Acknowledgements
The establishment of the nTAC model was supported by the Deutsche Forschungsgemeinschaft through the Cluster of Excellence REBIRTH (EXC62/3), the Heisenberg Program (HE3658/6-1 and HE3658/6-2), and a research grant HE 3658/11-1. The schematic images used in the figures are from Servier Medical Art (https://smart.servier.com/).
Author information
Authors and Affiliations
Contributions
M.M.M. and J.H. designed the study, planned all the experiments, and analyzed the data. M.M.M. established the methods and performed the surgeries and experiments. A.A. captured the images. M.M.M. and J.H. wrote the manuscript. J.H. supervised the study. All authors read and approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Nature Protocols thanks Robert Blanton and Yingjie Chen for their contribution to the peer review of this work.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Key reference using this protocol
Malek Mohammadi, M. et al. JCI Insight 4, e128336 (2019): https://doi.org/10.1172/jci.insight.128336
Key data used in this protocol
Malek Mohammadi, M. et al. JCI Insight 4, e128336 (2019): https://doi.org/10.1172/jci.insight.128336
Supplementary information
Supplementary Information
Supplementary Materials and Methods.
Supplementary Video 1
Video demonstrating the nTAC procedure
Source data
Source Data Fig. 6
Source data.
Rights and permissions
About this article
Cite this article
Malek Mohammadi, M., Abouissa, A. & Heineke, J. A surgical mouse model of neonatal pressure overload by transverse aortic constriction. Nat Protoc 16, 775–790 (2021). https://doi.org/10.1038/s41596-020-00434-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41596-020-00434-9
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.