Abstract
Co-inhibitory and checkpoint molecules suppress T cell function in the tumor microenvironment, thereby rendering T cells dysfunctional. Although immune checkpoint blockade is a successful treatment option for multiple human cancers, severe autoimmune-like adverse effects can limit its application. Here, we show that the gene encoding peptidoglycan recognition protein 1 (PGLYRP1) is highly coexpressed with genes encoding co-inhibitory molecules, indicating that it might be a promising target for cancer immunotherapy. Genetic deletion of Pglyrp1 in mice led to decreased tumor growth and an increased activation/effector phenotype in CD8+ T cells, suggesting an inhibitory function of PGLYRP1 in CD8+ T cells. Surprisingly, genetic deletion of Pglyrp1 protected against the development of experimental autoimmune encephalomyelitis, a model of autoimmune disease in the central nervous system. PGLYRP1-deficient myeloid cells had a defect in antigen presentation and T cell activation, indicating that PGLYRP1 might function as a proinflammatory molecule in myeloid cells during autoimmunity. These results highlight PGLYRP1 as a promising target for immunotherapy that, when targeted, elicits a potent antitumor immune response while protecting against some forms of tissue inflammation and autoimmunity.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
Bulk and single-cell RNA-seq data (related to Fig. 2h–k) have been deposited in Gene Expression Omnibus (GEO) under the accession code GSE223896. Preexisting data accessed in Fig. 1a–c are available in GEO under accession number GSE113968 (subseries numbers are GSE113262, GSE113280, GSE113689, GSE113807 and GSE113811), and the data accessed in Extended Data Fig. 1 are available in GEO under accession number GSE120575. All other data are available in the main article and Supplementary Information or from the corresponding author upon reasonable request.
Code availability
All code is available on GitHub at https://github.com/lhuang1/Pglyrp1_Tumor_EAE.
References
Ribas, A. & Wolchok, J. D. Cancer immunotherapy using checkpoint blockade. Science 359, 1350–1355 (2018).
Pauken, K. E., Dougan, M., Rose, N. R., Lichtman, A. H. & Sharpe, A. H. Adverse events following cancer immunotherapy: obstacles and opportunities. Trends Immunol. 40, 511–523 (2019).
Schnell, A., Bod, L., Madi, A. & Kuchroo, V. K. The yin and yang of co-inhibitory receptors: toward anti-tumor immunity without autoimmunity. Cell Res. 30, 285–299 (2020).
Khan, Z. et al. Genetic variation associated with thyroid autoimmunity shapes the systemic immune response to PD-1 checkpoint blockade. Nat. Commun. 12, 3355 (2021).
Dziarski, R. & Gupta, D. The peptidoglycan recognition proteins (PGRPs). Genome Biol. 7, 232 (2006).
Dziarski, R. & Gupta, D. Mammalian peptidoglycan recognition proteins (PGRPs) in innate immunity. Innate Immun. 16, 168–174 (2010).
Royet, J., Gupta, D. & Dziarski, R. Peptidoglycan recognition proteins: modulators of the microbiome and inflammation. Nat. Rev. Immunol. 11, 837–851 (2011).
Dziarski, R., Platt, K. A., Gelius, E., Steiner, H. & Gupta, D. Defect in neutrophil killing and increased susceptibility to infection with nonpathogenic Gram-positive bacteria in peptidoglycan recognition protein-S (PGRP-S)-deficient mice. Blood 102, 689–697 (2003).
Cho, J. H. et al. Human peptidoglycan recognition protein S is an effector of neutrophil-mediated innate immunity. Blood 106, 2551–2558 (2005).
Lo, D. et al. Peptidoglycan recognition protein expression in mouse Peyer’s patch follicle associated epithelium suggests functional specialization. Cell Immunol. 224, 8–16 (2003).
Lu, X. et al. Peptidoglycan recognition proteins are a new class of human bactericidal proteins. J. Biol. Chem. 281, 5895–5907 (2006).
Wang, M. et al. Human peptidoglycan recognition proteins require zinc to kill both Gram-positive and Gram-negative bacteria and are synergistic with antibacterial peptides. J. Immunol. 178, 3116–3125 (2007).
Sashchenko, L. P. et al. Peptidoglycan recognition protein Tag7 forms a cytotoxic complex with heat shock protein 70 in solution and in lymphocytes. J. Biol. Chem. 279, 2117–2124 (2004).
Read, C. B. et al. Identification of neutrophil PGLYRP1 as a ligand for TREM-1. J. Immunol. 194, 1417–1421 (2015).
Downs-Canner, S. et al. Suppressive IL-17A+Foxp3+ and ex-TH17 IL-17A–Foxp3+ Treg cells are a source of tumour-associated Treg cells. Nat. Commun. 8, 14649 (2017).
Chihara, N. et al. Induction and transcriptional regulation of the co-inhibitory gene module in T cells. Nature 558, 454–459 (2018).
Singer, M. et al. A distinct gene module for dysfunction uncoupled from activation in tumor-infiltrating T cells. Cell 166, 1500–1511 (2016).
Ng, S. S. et al. The NK cell granule protein NKG7 regulates cytotoxic granule exocytosis and inflammation. Nat. Immunol. 21, 1205–1218 (2020).
Raskov, H., Orhan, A., Christensen, J. P. & Gogenur, I. Cytotoxic CD8+ T cells in cancer and cancer immunotherapy. Br. J. Cancer 124, 359–367 (2021).
Di Pilato, M. et al. CXCR6 positions cytotoxic T cells to receive critical survival signals in the tumor microenvironment. Cell 184, 4512–4530 (2021).
Salmon, A. J. et al. BHLHE40 regulates the T-cell effector function required for tumor microenvironment remodeling and immune checkpoint therapy efficacy. Cancer Immunol. Res. 10, 597–611 (2022).
Kurtulus, S. et al. Checkpoint blockade immunotherapy induces dynamic changes in PD-1–CD8+ tumor-infiltrating T cells. Immunity 50, 181–194 (2019).
Sade-Feldman, M. et al. Defining T cell states associated with response to checkpoint immunotherapy in melanoma. Cell 175, 998–1013 (2018).
Robinson, M. D., McCarthy, D. J. & Smyth, G. K. edgeR: a Bioconductor package for differential expression analysis of digital gene expression data. Bioinformatics 26, 139–140 (2010).
McCarthy, D. J., Chen, Y. & Smyth, G. K. Differential expression analysis of multifactor RNA-seq experiments with respect to biological variation. Nucleic Acids Res. 40, 4288–4297 (2012).
Chen, Y., Lun, A. T. & Smyth, G. K. From reads to genes to pathways: differential expression analysis of RNA-seq experiments using Rsubread and the edgeR quasi-likelihood pipeline. F1000Research 5, 1438 (2016).
Wherry, E. J. et al. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity 27, 670–684 (2007).
Doering, T. A. et al. Network analysis reveals centrally connected genes and pathways involved in CD8+ T cell exhaustion versus memory. Immunity 37, 1130–1144 (2012).
Gattinoni, L. et al. A human memory T cell subset with stem cell-like properties. Nat. Med. 17, 1290–1297 (2011).
Tirosh, I. et al. Dissecting the multicellular ecosystem of metastatic melanoma by single-cell RNA-seq. Science 352, 189–196 (2016).
Bergen, V., Lange, M., Peidli, S., Wolf, F. A. & Theis, F. J. Generalizing RNA velocity to transient cell states through dynamical modeling. Nat. Biotechnol. 38, 1408–1414 (2020).
Anz, D. et al. CD103 is a hallmark of tumor-infiltrating regulatory T cells. Int. J. Cancer 129, 2417–2426 (2011).
Karandikar, N. J., Vanderlugt, C. L., Walunas, T. L., Miller, S. D. & Bluestone, J. A. CTLA-4: a negative regulator of autoimmune disease. J. Exp. Med. 184, 783–788 (1996).
Salama, A. D. et al. Critical role of the programmed death-1 (PD-1) pathway in regulation of experimental autoimmune encephalomyelitis. J. Exp. Med. 198, 71–78 (2003).
Monney, L. et al. TH1-specific cell surface protein Tim-3 regulates macrophage activation and severity of an autoimmune disease. Nature 415, 536–541 (2002).
Joller, N. et al. TIGIT has T cell-intrinsic inhibitory functions. J. Immunol. 186, 1338–1342 (2011).
Chastain, E. M., Duncan, D. S., Rodgers, J. M. & Miller, S. D. The role of antigen presenting cells in multiple sclerosis. Biochim. Biophys. Acta 1812, 265–274 (2011).
Jordao, M. J. C. et al. Single-cell profiling identifies myeloid cell subsets with distinct fates during neuroinflammation. Science 363, eaat7554 (2019).
Shi, J., Hua, L., Harmer, D., Li, P. & Ren, G. Cre driver mice targeting macrophages. Methods Mol. Biol. 1784, 263–275 (2018).
Bettelli, E. et al. Myelin oligodendrocyte glycoprotein-specific T cell receptor transgenic mice develop spontaneous autoimmune optic neuritis. J. Exp. Med. 197, 1073–1081 (2003).
Bonacina, F. et al. Myeloid apolipoprotein E controls dendritic cell antigen presentation and T cell activation. Nat. Commun. 9, 3083 (2018).
Jia, W., Kidoya, H., Yamakawa, D., Naito, H. & Takakura, N. Galectin-3 accelerates M2 macrophage infiltration and angiogenesis in tumors. Am. J. Pathol. 182, 1821–1831 (2013).
Yao, J., Mackman, N., Edgington, T. S. & Fan, S. T. Lipopolysaccharide induction of the tumor necrosis factor-α promoter in human monocytic cells. Regulation by EGR-1, c-JUN, and NF-κB transcription factors. J. Biol. Chem. 272, 17795–17801 (1997).
Napolitani, G., Bortoletto, N., Racioppi, L., Lanzavecchia, A. & D’Oro, U. Activation of Src-family tyrosine kinases by LPS regulates cytokine production in dendritic cells by controlling AP-1 formation. Eur. J. Immunol. 33, 2832–2841 (2003).
Bashirova, A. A. et al. Diversity of the human LILRB3/A6 locus encoding a myeloid inhibitory and activating receptor pair. Immunogenetics 66, 1–8 (2014).
Artis, D. et al. The IL-27 receptor (WSX-1) is an inhibitor of innate and adaptive elements of type 2 immunity. J. Immunol. 173, 5626–5634 (2004).
Stumhofer, J. S. et al. Interleukin 27 negatively regulates the development of interleukin 17-producing T helper cells during chronic inflammation of the central nervous system. Nat. Immunol. 7, 937–945 (2006).
Awasthi, A. et al. A dominant function for interleukin 27 in generating interleukin 10-producing anti-inflammatory T cells. Nat. Immunol. 8, 1380–1389 (2007).
Fitzgerald, D. C. et al. Suppression of autoimmune inflammation of the central nervous system by interleukin 10 secreted by interleukin 27-stimulated T cells. Nat. Immunol. 8, 1372–1379 (2007).
Zhang, H. et al. An IL-27-driven transcriptional network identifies regulators of IL-10 expression across T helper cell subsets. Cell Rep. 33, 108433 (2020).
Batten, M. et al. IL-27 is a potent inducer of IL-10 but not FoxP3 in murine T cells. J. Immunol. 180, 2752–2756 (2008).
Murtagh, F. & Legendre, P. Ward’s hierarchical agglomerative clustering method: which algorithms implement Ward’s criterion? J. Classif. 31, 274–295 (2014).
Beltra, J. C. et al. Developmental relationships of four exhausted CD8+ T cell subsets reveals underlying transcriptional and epigenetic landscape control mechanisms. Immunity 52, 825–841 (2020).
Hudson, W. H. et al. Proliferating transitory T cells with an effector-like transcriptional signature emerge from PD-1+ stem-like CD8+ T cells during chronic infection. Immunity 51, 1043–1058 (2019).
Gaublomme, J. T. et al. Single-cell genomics unveils critical regulators of TH17 cell pathogenicity. Cell 163, 1400–1412 (2015).
Miller, B. C. et al. Subsets of exhausted CD8+ T cells differentially mediate tumor control and respond to checkpoint blockade. Nat. Immunol. 20, 326–336 (2019).
Best, J. A. et al. Transcriptional insights into the CD8+ T cell response to infection and memory T cell formation. Nat. Immunol. 14, 404–412 (2013).
Jager, A., Dardalhon, V., Sobel, R. A., Bettelli, E. & Kuchroo, V. K. TH1, TH17, and TH9 effector cells induce experimental autoimmune encephalomyelitis with different pathological phenotypes. J. Immunol. 183, 7169–7177 (2009).
Schnell, A. et al. Stem-like intestinal TH17 cells give rise to pathogenic effector T cells during autoimmunity. Cell 184, 6281–6298 (2021).
Satija, R., Farrell, J. A., Gennert, D., Schier, A. F. & Regev, A. Spatial reconstruction of single-cell gene expression data. Nat. Biotechnol. 33, 495–502 (2015).
Picelli, S. et al. Full-length RNA-seq from single cells using Smart-seq2. Nat. Protoc. 9, 171–181 (2014).
Li, B. et al. Cumulus provides cloud-based data analysis for large-scale single-cell and single-nucleus RNA-seq. Nat. Methods 17, 793–798 (2020).
McGinnis, C. S., Murrow, L. M. & Gartner, Z. J. DoubletFinder: doublet detection in single-cell RNA sequencing data using artificial nearest neighbors. Cell Syst. 8, 329–337 (2019).
Machado, L. et al. Tissue damage induces a conserved stress response that initiates quiescent muscle stem cell activation. Cell Stem Cell 28, 1125–1135 (2021).
Waltman, L. & Van Eck, N. J. A smart local moving algorithm for large-scale modularity-based community detection. Eur. Phys. J. B 86, 471 (2013).
McInnes, L., Healy, J. & Melville, J. UMAP: Uniform Manifold Approximation and Projection. J. Open Source Softw. 3, 861 (2018).
Zilionis, R. et al. Single-cell transcriptomics of human and mouse lung cancers reveals conserved myeloid populations across individuals and species. Immunity 50, 1317–1334 (2019).
Soneson, C. & Robinson, M. D. Bias, robustness and scalability in single-cell differential expression analysis. Nat. Methods 15, 255–261 (2018).
Melsted, P. et al. Modular, efficient and constant-memory single-cell RNA-seq preprocessing. Nat. Biotechnol. 39, 813–818 (2021).
Li, T. et al. TIMER2.0 for analysis of tumor-infiltrating immune cells. Nucleic Acids Res. 48, W509–W514 (2020).
Kim, D. et al. Graph-based genome alignment and genotyping with HISAT2 and HISAT-genotype. Nat. Biotechnol. 37, 907–915 (2019).
Li, B. & Dewey, C. N. RSEM: accurate transcript quantification from RNA-seq data with or without a reference genome. BMC Bioinformatics 12, 323 (2011).
Love, M. I., Huber, W. & Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 15, 550 (2014).
Korotkevich, G. et al. Fast gene set enrichment analysis. Preprint at bioRxiv https://doi.org/10.1101/060012 (2021).
Jiang, P. et al. Signatures of T cell dysfunction and exclusion predict cancer immunotherapy response. Nat. Med. 24, 1550–1558 (2018).
Acknowledgements
We would like to thank all members of the Kuchroo laboratory for helpful discussions and feedback. We thank J. Xia, H. Stroh, E. A. Greenfield, R. K. Krishnan and D. Kozoriz for their assistance and technical support and L. Gaffney for help with figures. Additionally, we would like to thank M. Collins for critical feedback on the manuscript.
This work was supported by National Institute of Health grants (P01AI073748, P01AI039671, P01AI056299 and R01AI144166) to V.K.K. and R01CA187975 (A.C.A.). A.S. was supported by a German Academic Scholarship Foundation (Studienstiftung des Deutschen Volkes) PhD fellowship. A.R. was supported by the Klarman Cell Observatory and Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
A.S. and V.K.K. conceived the study, designed the experiments and interpreted the results. A.S., with assistance from B.M.L.R., D.V., A.B., M.W., Y.H. and L.B., performed and analyzed the functional biological experiments. A.S., with assistance from B.M.L.R. and V.S., performed the sequencing experiments. R.A.S. helped with the histological analysis. N.C., A.M. and A.C.A. helped with the original discovery of Pglyrp1 as part of the co-inhibitory module. L.H., with assistance from A.S., A.R. and V.K.K., designed and performed the computational analysis. The manuscript was written by A.S. and L.H. and was edited by A.R., A.C.A. and V.K.K. with input from all authors.
Corresponding author
Ethics declarations
Competing interests
A.C.A. is a member of the Scientific Advisory Board for Tizona Therapeutics, Trishula Therapeutics, Compass Therapeutics, Zumutor Biologics, ImmuneOncia and Excepgen, which have interests in cancer immunotherapy. A.C.A. is also a paid consultant for iTeos Therapeutics and Larkspur Biosciences. V.K.K. is cofounder of Celsius Therapeutics, Tizona Therapeutics, Larkspur Biosciences and Bicara Therapeutics. A.C.A.’s and V.K.K.’s interests are reviewed and managed by the BWH and Partners Healthcare in accordance with their conflict of interest policies. A.R. is a cofounder of and equity holder in Celsius Therapeutics and an equity holder in Immunitas and was a Scientific Advisory Board member of Thermo Fisher Scientific, Syros Pharmaceuticals, Neogene Therapeutics and Asimov until 31 July 2020. A.R. is an employee of Genentech (member of the Roche Group) since August 2020 and has equity in Roche. The other authors declare no competing interests.
Peer review
Peer review information
Nature Immunology thanks Scott Zamvil and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Primary Handling Editor: N. Bernard, in collaboration with the Nature Immunology team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Pglyrp1 is expressed on exhausted T cells in human cancer.
Expression of Pglyrp1 and co-inhibitory receptors in single immune cells of human melanoma samples23. Plotted are the percent of cells with UMI count \(\ge\)1. Annotation as defined in publication.
Extended Data Fig. 2 Association between the expression levels of Pglyrp1 and survival rate in different human cancers.
Overall survival of patients with breast cancer (BRCA) (n = 1,100), HER2-positive BRCA (BRCA-Her2) (n = 82), colon adenocarcinoma (COAD) (n = 458), and lung squamous cell carcinoma (LUSC) (n = 501) grouped by PGLRYP1 expression through TIMER2 database70. Split expression percentage of patients: 20%. Analyses were performed with log-rank Mantel-Cox test. Hazard ratio (HR) and p-value are provided.
Extended Data Fig. 3 Immune-profiling of tumors in Pglyrp1-deficient mice.
(a) Pglyrp1−/− mouse validation. Relative expression (RE) of Pglyrp1 transcript in WT, Pglyrp1−/+, and Pglyrp1−/− CD8+ T cells from the spleen by qPCR (n = 2-3). The expression is depicted as relative to WT cells. The bar indicates the mean. (b–d) Analysis of the immune system in the colon of 7-week-old Pglyrp1−/− mice and WT littermates by flow cytometry (n = 3). General immune system composition (b), and intra-cellular cytokine staining in CD4+ T cells (c) and CD8+ T cells (d) are displayed. (e, f) B16-OVA tumors were implanted into WT and Pglyrp1−/− mice (n = 7). (e) Mean tumor growth and (f) tumor sizes on day 16 are shown. (g) MC38-OVA tumors were implanted into WT and Pglyrp1−/− mice and mice were treated with anti-PD-1 antibody on days 6, 8, and 10 post tumor-implantation. The control group included WT mice injected with control immunoglobulin (Rat IgG2a). (h) Relative expression of Pglyrp1 transcript in different immune populations isolated from MC38-OVA tumors grown in WT mice by qPCR (n = 4). (i) Frequency of different immune populations in MC38-OVA tumors grown in WT and Pglyrp1−/− mice (n = 9) by flow cytometry. In (b-i) data are presented as the mean with ±SEM. Unpaired two-tailed t-tests were performed. NS, not significant.
Extended Data Fig. 4 Immune populations in the dLN and spleen of tumor-bearing Pglyrp1-deficient mice.
(a) Frequency of Treg cells (CD45+ TCRβ+ CD4+ FOXP3+) in the spleen of naïve mice (n = 3). (b, d–g) MC38-OVA tumors were implanted into WT and Pglyrp1−/− mice and TILs were harvested for flow cytometry. (b) Summary plots of the frequency of Treg cells (CD45+ TCRβ+ CD4+ FOXP3+) in the dLN (WT n = 9, Pglyrp1−/− n = 8) (left) and spleen (WT n = 10, Pglyrp1−/− n = 8) (right). (c) Gating strategy for CD8+ T cells in the tumor. (d) Summary plots of the frequency of indicated cytokines in CD8+ T cells in the dLN (WT n = 9, Pglyrp1−/− n = 8) (top) and spleen (WT n = 10, Pglyrp1−/− n = 8) (bottom). (e) Summary plots of the frequency of indicated cytokines in CD4+ T cells in the tumor (WT n = 12, Pglyrp1−/− n = 8) (top), dLN (WT n = 10, Pglyrp1−/− n = 8) (middle) and spleen (WT n = 12, Pglyrp1−/− n = 8) (bottom). (f) Summary plots of the frequency of PD-1- and TIM-3-expressing CD8+ T cells in the dLN (n = 8) (top) and spleen (WT n = 10, Pglyrp1−/− n = 8) (bottom). (g) Summary plots of the frequency of PD-1- and TIM-3-expressing CD4+ T cells in the tumor (WT n = 10, Pglyrp1−/− n = 8). In all panels, data are presented as the mean with ±SEM. Unpaired two-tailed t-tests were performed. NS, not significant.
Extended Data Fig. 5 Characterization of tumor-infiltrating T cells in Pglyrp1-deficient mice.
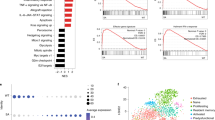
(a) Heatmap representing cluster-specific upregulated genes (FDR <0.05, log2 fold change > log2(1.5)). If a gene was upregulated in multiple clusters, it is only shown once in the cluster block where it has the biggest fold change. (b) Gene set enrichment analysis of selected Gene Ontology (GO) terms and KEGG and Reactome pathways (top) and published CD8+ T cell signatures (bottom) enriched in CD8+ T cell-1 (stem-like) cluster vs. CD8+ T cell-2 (effector/exhausted) cluster. Only WT cells were included in the analysis. Naïve CD8-1 (Supplementary Table 7); naïve CD8-2 (Supplementary Table 7); terminally exhausted-156; transitory vs. stem-like54; terminally exhausted-253; transitory vs. exhausted54; exhausted T cells75; effector-like56. P-values were computed with the empirical phenotype-based permutation tests (GSEA) and the values shown in the figures were not adjusted for multiple comparisons. (c) RNA velocity analysis was performed on the CD8+ T cell clusters (Fig. 3a) using scVelo31. The velocity vector field is displayed as streamlines (top) and at single-cell level with each arrow showing the direction and speed (thickness) of movement of an individual cell (bottom). (d) Volcano plot of differentially expressed genes comparing WT vs. Pglyrp1−/− cells in the Treg cluster (Fig. 3a). Differential genes were computed as FDR < 0.05 and |log2 fold change| > 0.25. Positive log2 fold change corresponds to upregulation in Pglyrp1−/− cells and vice versa. Log2 fold changes and -log10 p-values were capped within [−1.5, 1.5] and [0, 20] respectively for visualization purposes. P-values were computed with the empirical Bayes quasi-likelihood F-tests in edgeR, then adjusted for multiple comparisons using the Benjamini & Hochberg method (FDR).
Extended Data Fig. 6 Analysis of the tumor phenotype in Pglyrp1fl/fl mice.
(a) Relative expression (RE) of Pglyrp1 in CD8+ T cells, CD4+ T cells, CD11b+ cells, B cells and neutrophils by qPCR (n = 5). MC38-OVA tumors were implanted into WT and E8iCrePglyrp1fl/fl mice. (b) Mean tumor growth of MC38-OVA tumors implanted into WT and LysMCrePglyrp1fl/fl mice (n = 8-9). In (a,b) data are presented as the mean with ± SEM. Unpaired two-tailed t-tests were performed. NS: not significant.
Extended Data Fig. 7 Analysis of CD8+ T cell phenotype and antigen-presentation of LysMCre Pglyrp1fl/fl splenocytes.
(a) Gating strategy of CD4+ T cells in the CNS. (b) On day 18 after immunization, CNS-infiltrating lymphocytes were extracted and analyzed for the expression of intracellular cytokines in CD8+ T cells by flow cytometry (n = 5). (c) Antigen-presentation assay with splenocytes from LysMCre Pglyrp1fl/fl or WT littermate controls with 2D2 naïve CD4+ T cells with or without MOG peptide (n = 4). Cell proliferation was measured by CellTrace Violet (CTV) staining. Quantification (left) and representative plots (right). (d) Cytokine concentration in the culture medium during antigen-presentation assay as in a, measured by legendplex (n = 4). In (b-d) data are presented as the mean with + SEM. Unpaired two-tailed t-tests were performed. NS: not significant.
Extended Data Fig. 8 scRNA-seq of CNS-infiltrated myeloid cells in Pglyrp1−/− mice during EAE.
(a) UMAP of CNS-infiltrating myeloid cells (3,698 cells). EAE was induced in Pglyrp1−/− and WT littermate controls and CNS-infiltrating myeloid cells were sorted (CD45+ CD3− CD19−) for scRNA-seq at disease onset (day 10). (b) Venn diagram depicting the overlap in upregulated genes (FDR < 0.05, |log2 fold change| > 0.25) in WT cells (top) and Pglyrp1−/− cells (bottom) both in mono/MAC and neutrophil clusters as defined in (Fig. 6b). (c) Monocyte treatment with PGN, PGLYRP1, or PGN + PGLYRP1 (n = 3). Bar plot depicting the TNF concentration in the culture medium. Data are presented as the mean with ±SEM. Dotted line indicates the detection limit. Unpaired two-tailed t-tests were performed.
Supplementary information
Supplementary Tables 1–7
Supplementary Table 1. Spearman correlation of genes with co-inhibitory and stem-like genes. P values were computed with two-sided Spearman’s asymptotic t-tests and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 2. Differential expression comparing Pglyrp1–/– and WT tumor-infiltrating CD8+ T cells based on bulk RNA-seq data. P values were computed with likelihood ratio tests in edgeR and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 3. Differential expression results comparing cells in each tumor-infiltrating T cell cluster versus the rest. P values were computed with empirical Bayes quasilikelihood F-tests in edgeR and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 4. Differential expression comparing Pglyrp1–/– and WT tumor-infiltrating T cells based on scRNA-seq data. P values were computed with empirical Bayes quasilikelihood F-tests in edgeR and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 5. Differential expression results comparing cells in each CNS-infiltrating myeloid cell cluster versus the rest after EAE induction. P values were computed with empirical Bayes quasilikelihood F-tests in edgeR and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 6. Differential expression results comparing Pglyrp1–/– and WT CNS-infiltrating monocytes/macrophages and neutrophils. P values were computed with the empirical Bayes quasilikelihood F-tests in edgeR and were adjusted for multiple comparisons using the Benjamini–Hochberg method (FDR). Supplementary Table 7. Gene signatures for GSEA.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Schnell, A., Huang, L., Regan, B.M.L. et al. Targeting PGLYRP1 promotes antitumor immunity while inhibiting autoimmune neuroinflammation. Nat Immunol 24, 1908–1920 (2023). https://doi.org/10.1038/s41590-023-01645-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-023-01645-4
This article is cited by
-
Targeting PGLYRP1 in cancer and autoimmunity
Nature Immunology (2023)