Abstract
Transient molecules in the gastrointestinal tract such as nitric oxide and hydrogen sulfide are key signals and mediators of inflammation. Owing to their highly reactive nature and extremely short lifetime in the body, these molecules are difficult to detect. Here we develop a miniaturized device that integrates genetically engineered probiotic biosensors with a custom-designed photodetector and readout chip to track these molecules in the gastrointestinal tract. Leveraging the molecular specificity of living sensors1, we genetically encoded bacteria to respond to inflammation-associated molecules by producing luminescence. Low-power electronic readout circuits2 integrated into the device convert the light emitted by the encapsulated bacteria to a wireless signal. We demonstrate in vivo biosensor monitoring in the gastrointestinal tract of small and large animal models and the integration of all components into a sub-1.4 cm3 form factor that is compatible with ingestion and capable of supporting wireless communication. With this device, diseases such as inflammatory bowel disease could be diagnosed earlier than is currently possible, and disease progression could be more accurately tracked. The wireless detection of short-lived, disease-associated molecules with our device could also support timely communication between patients and caregivers, as well as remote personalized care.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All data are provided in the paper and in the supplementary information. Genetic sequences and plasmids have been deposited into the Addgene repository under Addgene identifiers 199782–199792.
References
Inda, M. E. & Lu, T. K. Microbes as biosensors. Annu. Rev. Microbiol. 74, 337–359 (2020).
Liu, Q. et al. A threshold-based bioluminescence detector with a CMOS-integrated photodiode array in 65 nm for a multi-diagnostic ingestible capsule. IEEE J. Solid State Circuits 58, 838–851 (2023).
Bourgonje, A. R. et al. Oxidative stress and redox-modulating therapeutics in inflammatory bowel disease. Trends Mol. Med. 26, 1034–1046 (2020).
Lee, J.-Y., Tsolis, R. M. & Bäumler, A. J. The microbiome and gut homeostasis. Science 377, eabp9960 (2022).
Million, M. et al. Increased gut redox and depletion of anaerobic and methanogenic prokaryotes in severe acute malnutrition. Sci. Rep. 6, 26051 (2016).
Pribis, J. P. et al. Gamblers: an antibiotic-induced evolvable cell subpopulation differentiated by reactive-oxygen-induced general stress response. Mol. Cell 74, 785–800.e7 (2019).
Reese, A. T. et al. Antibiotic-induced changes in the microbiota disrupt redox dynamics in the gut. eLife 7, e35987 (2018).
Rivera-Chávez, F. et al. Depletion of butyrate-producing clostridia from the gut microbiota drives an aerobic luminal expansion of Salmonella. Cell Host Microbe 19, 443–454 (2016).
Dumitrescu, L. et al. Oxidative stress and the microbiota–gut–brain axis. Oxid. Med. Cell. Longev. 2018, 2406594 (2018).
Yardeni, T. et al. Host mitochondria influence gut microbiome diversity: A role for ROS. Sci. Signal. 12, eaaw3159 (2019).
Jose, S., Bhalla, P. & Suraishkumar, G. K. Oxidative stress decreases the redox ratio and folate content in the gut microbe, Enterococcus durans (MTCC 3031). Sci. Rep. 8, 12138 (2018).
Hagan, T. et al. Antibiotics-driven gut microbiome perturbation alters immunity to vaccines in humans. Cell 178, 1313–1328.e13 (2019).
Million, M. & Raoult, D. Linking gut redox to human microbiome. Hum. Microbiome J. 10, 27–32 (2018).
Rivera-Chávez, F. & Bäumler, A. J. The pyromaniac inside you: Salmonella metabolism in the host gut. Annu. Rev. Microbiol. 69, 31–48 (2015).
Kalantar-Zadeh, K. et al. A human pilot trial of ingestible electronic capsules capable of sensing different gases in the gut. Nat. Electron. 1, 79–87 (2018).
Steiger, C. et al. Dynamic monitoring of systemic biomarkers with gastric sensors. Adv. Sci. 8, 2102861 (2021).
Archer, E. J., Robinson, A. B. & Süel, G. M. Engineered E. coli that detect and respond to gut inflammation through nitric oxide sensing. ACS Synth. Biol. 1, 451–457 (2012).
Rubens, J. R., Selvaggio, G. & Lu, T. K. Synthetic mixed-signal computation in living cells. Nat. Commun. 7, 11658 (2016).
Daeffler, K. N. et al. Engineering bacterial thiosulfate and tetrathionate sensors for detecting gut inflammation. Mol. Syst. Biol. 13, 923 (2017).
Annese, V. et al. European evidence-based consensus: inflammatory bowel disease and malignancies. J. Crohns. Colitis 9, 945–965 (2015).
Amir, A. et al. Room-temperature, correcting for microbial blooms in fecal samples during shipping. mSystems 2, e00199–16 (2017).
Raymond, F. et al. Culture-enriched human gut microbiomes reveal core and accessory resistance genes. Microbiome 7, 56 (2019).
Zmora, N. et al. Personalized gut mucosal colonization resistance to empiric probiotics is associated with unique host and microbiome features. Cell 174, 1388–1405.e21 (2018).
Jain, U. et al. Debaryomyces is enriched in Crohn’s disease intestinal tissue and impairs healing in mice. Science 371, 1154–1159 (2021).
Courbet, A., Endy, D., Renard, E., Molina, F. & Bonnet, J. Detection of pathological biomarkers in human clinical samples via amplifying genetic switches and logic gates. Sci. Transl. Med. 7, 289ra83 (2015).
Kotula, J. W. et al. Programmable bacteria detect and record an environmental signal in the mammalian gut. Proc. Natl Acad. Sci. USA 111, 4838–4843 (2014).
Lim, B., Zimmermann, M., Barry, N. A. & Goodman, A. L. Engineered regulatory systems modulate gene expression of human commensals in the gut. Cell 169, 547–558.e15 (2017).
Mimee, M., Tucker, A. C., Voigt, C. A. & Lu, T. K. Programming a human commensal bacterium, Bacteroides thetaiotaomicron, to sense and respond to stimuli in the murine gut microbiota. Cell Syst. 1, 62–71 (2015).
Riglar, D. T. et al. Engineered bacteria can function in the mammalian gut long-term as live diagnostics of inflammation. Nat. Biotechnol. 35, 653–658 (2017).
Pickard, J. M. et al. Rapid fucosylation of intestinal epithelium sustains host–commensal symbiosis in sickness. Nature 514, 638–641 (2014).
Swain, P. Wireless capsule endoscopy. Gut 52 (suppl. 4), 48–50 (2003).
van der Schaar, P. J. et al. A novel ingestible electronic drug delivery and monitoring device. Gastrointest. Endosc. 78, 520–528 (2013).
Din, M. O. et al. Interfacing gene circuits with microelectronics through engineered population dynamics. Sci. Adv. 6, eaaz8344 (2020).
Mimee, M. et al. An ingestible bacterial-electronic system to monitor gastrointestinal health. Science 360, 915–918 (2018).
Bass, D. M., Prevo, M. & Waxman, D. S. Gastrointestinal safety of an extended-release, nondeformable, oral dosage form (OROS). Drug Saf. 25, 1021–1033 (2002).
Isabella, V. M. et al. Development of a synthetic live bacterial therapeutic for the human metabolic disease phenylketonuria. Nat. Biotechnol. 36, 857–864 (2018).
Bush, M., Ghosh, T., Tucker, N., Zhang, X. & Dixon, R. Transcriptional regulation by the dedicated nitric oxide sensor, NorR: a route towards NO detoxification. Biochem. Soc. Trans. 39, 289–293 (2011).
Chen, X. J., Wang, B., Thompson, I. P. & Huang, W. E. Rational design and characterization of nitric oxide biosensors in E. coli Nissle 1917 and mini SimCells. ACS Synth. Biol. 10, 2566–2578 (2021).
Ceze, L., Nivala, J. & Strauss, K. Molecular digital data storage using DNA. Nat. Rev. Genet. 20, 456–466 (2019).
Beck, P. L. et al. Paradoxical roles of different nitric oxide synthase isoforms in colonic injury. Am. J. Physiol. 286, 137–147 (2004).
Jiminez, J. A., Uwiera, T. C., Douglas Inglis, G. & Uwiera, R. R. E. Animal models to study acute and chronic intestinal inflammation in mammals. Gut Pathog. 7, 29 (2015).
Strand-Amundsen, R. J. et al. Ischemia/reperfusion injury in porcine intestine—viability assessment. World J. Gastroenterol. 24, 2009–2023 (2018).
Lundberg, J. O. N., Lundberg, J. M., Alving, K. & Hellström, P. M. Greatly increased luminal nitric oxide in ulcerative colitis. Lancet 344, 1673–1674 (1994).
Liu, X. et al. Magnetic living hydrogels for intestinal localization, retention, and diagnosis. Adv. Funct. Mater. 31, 2010918 (2021).
Song, M. et al. In 2020 IEEE International Solid- State Circuits Conference 474–476 https://doi.org/10.1109/ISSCC19947.2020.9063083 (IEEE, 2020).
Krawczyk, K. et al. Electrogenetic cellular insulin release for real-time glycemic control in type 1 diabetic mice. Science. 368, 993–1001 (2020).
Zhao, H. et al. Autonomous push button-controlled rapid insulin release from a piezoelectrically activated subcutaneous cell implant. Sci. Adv. 8, 24 (2022).
Harimoto, T. et al. A programmable encapsulation system improves delivery of therapeutic bacteria in mice. Nat. Biotechnol. 40, 1259–1269 (2022).
Li, Z. et al. Biofilm-inspired encapsulation of probiotics for the treatment of complex infections. Adv. Mater. 30, e1803925 (2018).
Chen, W. et al. Bacteria-driven hypoxia targeting for combined biotherapy and photothermal therapy. ACS Nano 12, 5995–6005 (2018).
Cao, Z., Wang, X., Pang, Y., Cheng, S. & Liu, J. Biointerfacial self-assembly generates lipid membrane coated bacteria for enhanced oral delivery and treatment. Nat. Commun. 10, 5783 (2019).
Hu, Q. et al. Engineering nanoparticle-coated bacteria as oral DNA vaccines for cancer immunotherapy. Nano Lett. 15, 2732–2739 (2015).
Vujkovic-cvijin, I. et al. Host variables confound gut microbiota studies of human disease. Nature 587, 448–454 (2020).
Chiu, C. Y. & Miller, S. A. Clinical metagenomics. Nat. Rev. Genet. 20, 341–355 (2019).
Steiger, C. et al. Ingestible electronics for diagnostics and therapy. Nat. Rev. Mater. 4, 83–98 (2019).
Ma, Y., Selby, N. & Adib, F. Minding the billions: ultra-wideband localization for deployed RFID tags. In Proc. MobiCom ’17 https://doi.org/10.1145/3117811.3117833 (Association for Computing Machinery, 2017).
Siuti, P., Yazbek, J. & Lu, T. K. Synthetic circuits integrating logic and memory in living cells. Nat. Biotechnol. 31, 448–452 (2013).
Lloyd-Price, J., Abu-Ali, G. & Huttenhower, C. The healthy human microbiome. Genome Med. 8, 51 (2016).
Inda, M. E., Mimee, M. & Lu, T. K. Cell-based biosensors for immunology, inflammation, and allergy. J. Allerg. Clin. Immunol. 144, 645–647 (2019).
Gibson, D. G. et al. Enzymatic assembly of DNA molecules up to several hundred kilobases. Nat. Methods 6, 343–345 (2009).
Reinders, C. I. et al. Rectal mucosal nitric oxide in differentiation of inflammatory bowel disease and irritable bowel syndrome. Clin. Gastroenterol. Hepatol. 3, 777–783 (2005).
Acknowledgements
This work was supported by Leona M. and Harry B. Helmsley Charitable Trust (3239), Pew Charitable Trusts (to M.E.I.-W.; 00030623) and Catalyst Foundation (to R.T.Y., Q.L. and M.E.I.-W.; Secure Bio-Engineered Sensors for Disease Management, SAP grant no. 55208844). M.J. was supported by the Translational Research Institute of Space Health through Cooperative Agreement NNX16AO69A. G.T. was supported in part by the Department of Mechanical Engineering, MIT and the Karl van Tassel (1925) Career Development Professorship, MIT. Part of this material is based on research sponsored by 711 Human Performance Wing (HPW) and Defense Advanced Research Projects Agency (DARPA) under agreement number FA8650-21-2-7120. The US Government is authorized to reproduce and distribute reprints for governmental purposes notwithstanding any copyright notation thereon. The views and conclusions contained herein are those of the authors and should not be interpreted as necessarily representing the official policies or endorsements, either expressed or implied, of 711 Human Performance Wing (HPW) and Defense Advanced Research Projects Agency (DARPA) or the US Government.
Author information
Authors and Affiliations
Contributions
M.E.I.-W., M.J., Q.L., N.V.P., C.S., M.M., P.N., G.T., R.T.Y. and T.K.L. conceived and designed the research. M.E.I.-W., M.J., Q.L., C.S., A.W., M.M., P.N., A.P.C., G.T., R.T.Y. and T.K.L. conceptualized the miniaturized pill form factor, including integration of the bacteria, electronics and pill casings. M.E.I.-W. designed and performed in vitro biological experiments. Q.L., A.R. and T.Z. designed and built the integrated electronic circuits. M.E.I.-W. designed and performed in vivo mouse experiments. M.J., J.A., A.W. and K.W. developed the pill casing manufacturing process and validated the pill casing robustness in vitro, including membrane attachment. M.J., A.W., K.W. and R.M. generated 3D-printed device components. M.J. developed and validated the free-standing enteric films. M.E.I.-W., M.J., Q.L., N.V.P., C.S., A.H. and GT validated early prototypes. M.J., N.V.P., C.S., K.I., J.J., J.K., A.H. and G.T. conceptualized and validated the intestinal compartment animal model. K.I., N.F., J.J., J.K., A.H. and W.M. carried out animal husbandry and anaesthesia of pigs. M.E.I.-W., M.J. and Q.L. experimentally tested the function of the integrated devices in vitro and in vivo. M.E.I.-W., M.J. and Q.L. performed formal analysis of the data. M.E.I.-W., M.J., Q.L., J.A., P.N. and R.T.Y. contributed to data analysis of in vitro and in vivo experiments of the integrated devices. M.E.I.-W., M.J., Q.L., N.V.P., J.A., A.W., P.N. and R.T.Y. contributed to visualization. M.E.I.-W., M.J., Q.L., M.M., P.N., A.P.C., G.T., R.T.Y. and T.K.L. wrote the manuscript. M.E.I.-W., M.J., Q.L., P.N., C.S., A.W., A.H., G.T. and R.T.Y. managed daily project progress and personnel. M.E.I.-W. and T.K.L. supervised and managed general project administration. R.T.Y., G.T. supervised and managed funding of the project related to the integrated electronics and integrated pill casings and swine husbandry, respectively. M.E.I.-W., M.J., N.V.P., C.S., Y.L., M.M., P.N., A.P.C., R.T.Y., G.T. and T.K.L. contributed with funding acquisition.
Corresponding authors
Ethics declarations
Competing interests
MIT and Boston University have filed a Patent Cooperation Treaty (PCT) patent application (WO/2022/232188) regarding ingestible biosensors and methods of their use. T.K.L. is a co-founder of Senti Biosciences, Synlogic, Engine Biosciences, Tango Therapeutics, Corvium, BiomX, Eligo Biosciences and Bota.Bio. T.K.L. also holds financial interests in nest.bio, Ampliphi, IndieBio, MedicusTek, Quark Biosciences, Personal Genomics, Thryve, Lexent Bio, MitoLab, Vulcan and Serotiny. A.P.C. is on the board of Analog Devices. M.J. consults for VitaKey. C.S. is currently employed by Bayer AG (Germany). Complete details of all relationships for profit and not for profit for G.T. can found at https://www.dropbox.com/sh/szi7vnr4a2ajb56/AABs5N5i0q9AfT1IqIJAE-T5a?dl=0.
Peer review
Peer review information
Nature thanks Jeff Hasty and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer review reports are available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Inflammatory bowel disease (IBD) is mediated by labile molecules that are not detectable with current technologies.
Following an inflammatory insult, disproportionate mucosal immune responses via cytokine signaling lead to the release of redox-active molecules such as reactive oxygen species (ROS) and nitric oxide (NO). The resulting oxidative stress inhibits microbial growth in the gut lumen. However, chronic intestinal inflammation damages the epithelium and destroys the epithelial barrier, allowing intestinal microbes to invade the mucosa. The sources of thiosulfate (TS) in the GI tract are mucin-derived cysteine and sulfate, which are metabolized to hydrogen sulfide (H2S)19. During ulceration, epithelial cells and red blood cells enter the colon; these cells produce enzymes that convert H2S to TS. In the presence of ROS, TS is oxidized to tetrathionate (TT). Consumption of TT and sulfate allows certain pathogens to establish a foot-hold for infection19,29, evoking further immune responses. These mediators of disease are labile and cannot be measured with existing technology. With only the limited information current approaches provide, breaking this positive feedback loop is challenging.
Extended Data Fig. 2 Genetic circuit optimization and characterization of incorporated recombinase-based switch.
a, Dose-response curves of NO-sensing genetic circuits in E. coli Nissle 1917. The translational initiation strength of the recombinase Bxb1 was varied by using different computationally designed ribosome binding sites (RBS). Predicted RBS strengths are listed in the inset. Lower RBS strength led to a higher SNR. b, The memory circuit in the three NO sensors was stable over multiple rounds of re-growth. Engineered bacteria collected in stool were cultured in a selective media to measure NO detection, and the memory system was validated to ascertain that it accurately reflected, over multiple rounds of culturing, the initial input. c, GFP expression did not affect growth of bacteria when ON vs. OFF states were compared. d, NO detection in anaerobiosis. e, Time course of switch activation. The recombinase system triggered GFP expression within minutes (5 min for sensor NO Sensor 1 and NO Sensor 2, 10 min for NO Sensor 3, and less than 1 min for the ROS sensor) of exposure to the target molecule. f, Correlation of number of cells, time and concentration to show the performance of the system, (n = 3 per group). Lines represent the mean. Data are represented as mean ± SEM of three independent biological replicates derived from flow cytometry experiments (a–b, d–e), each of which involved n = 10,000 events.
Extended Data Fig. 3 Multiple specific disease biomarkers detected in vitro and in vivo.
a–c, The bacterial sensors were validated for the ROS H2O2, TS, and TT in vitro (a,d) and in vivo (b–c), following the protocol shown in Fig. 2. In the presence of H2O2, the transcription factor OxyR is oxidized and activated in E. coli. To construct a ROS biosensor that detected H2O2, the recombinase gene bxb1 was placed under the control of the OxyR-regulated oxyS promoter, oxySp, on the same genetic circuit18 (panel a). To construct the TT and TS sensors, we sought to overcome the oxygen repression that can affect Fumarate and Nitrate Reductase Regulator (FNR)-dependent sensors such as the previously reported two-component system TtrSR29. Oxygen levels fluctuate in the gut, depending on the level of disruption of the mucosal epithelium. To avoid this cross-repression, we used two newly identified sensors to express the recombinase system for detecting TS and TT: a TT sensor from Shewanella baltica, which does not depend on the FNR system, and the ThsRS sensor from Shewanella halifaxensis, the only genetically encoded TS sensor characterized so far19. Both sensors distinguished their target molecules from other terminal electron acceptors in vitro19. d, The cross-reactivity of the NorR-engineered bacteria was tested against ROS (H2O2), TT and TS in a series of dose-response curves (series of two-fold dilutions of the inducer with an initial concentration of 0.1 mM, 1 mM and 10mM respectively and 1mM for the positive control with DETA-NO). In (a and d) lines represent the mean, the errors (SEM) are derived from flow cytometry experiments of three representative biological replicates, each of which involved n = 10,000 events. In (b-c) individual points represent independent biological replicates, n = 5 animals per group, and the bars (b), **p = 0.0091 (ROS, day 14), *p = 0.0243 (TT, day 10), ***p = 0.0006 (TS, day 6), and lines (c) show the mean with SEM, **p = 0.0011 (TS, day 6), **p = 0.0029 (ROS, day 10), *p = 0.0126 (ROS, day 14), **p = 0.0053 (TT, day 10), two-way ANOVA for multiple comparisons. e, The NO biosensor was evaluated for its use as an NO disease stage detector. NorR, constitutively expressed from a library of ribosome-binding sites (RBS), exhibited different NO activation thresholds. Selected NO sensors (Sensor 1, 2, and 3) detected three concentrations (15, 30, and 80uM), which could correspond respectively to mild, moderate, and severe states of inflammation61. Based on the recombinase system described in Fig. 2a, flow cytometry was used to measure the percentage of GFP-positive cells at different concentrations of NO. For each point, the mean of three biological replicates, each with n = 10,000 flow cytometry events, is plotted. Error bars are the standard error of the mean (SEM).
Extended Data Fig. 4 In vivo validation of inflammatory biosensors.
a, Detection of NO by the NO biosensor as a marker of GI inflammation in vivo over time, n = 10 animals per group. Data are represented as mean ± SEM, **p = 0.0012 (day 13), ***p = 0.0005 (day 6), ***p = 0.0002 (day 11), ****p < 0.0001 (day 9), two-way ANOVA for multiple comparisons. b, Independent validation of the presence of inflammation in the DSS colitis model by quantifying iNOS expression during DSS treatment, weight loss, and the lipocalin-2 (LCN-2) biomarker, n = 10 animals per group. Data are represented as mean ± SEM, ****p < 0.0001, two-tailed unpaired Student’s t test. c, Histological scores of inflammation and necrosis, indicating the validity of the DSS model. Other indicators were observed but not quantified: bloody and loose stools, poor vigor, anal prolapse, and shortening of the colon upon dissection and gross morphological examination. Lines represent the mean. Error bars represent the SEM of independent biological replicates. d, Antibiotic-triggered redox imbalance measured by the NO sensor. NO Sensor 2 allowed us to detect an exacerbated inflammatory response after antibiotic treatment (carbenicillin and chloramphenicol) in a chronic DSS inflammation model, which implies multiple rounds of DSS treatment. Our biosensor for NO shows an increase of NO expression after 4 and 20–30 days of antibiotic treatment in both healthy and DSS-treated mice, with a significant switch activation on day 9 in the DSS-treated mice and on day 29 in the chronic DSS inflammation model, especially high for mouse #3. ‘DSS” samples, n = 5 and “Control” samples, n = 5. *p = 0.0408, **p = 0.0038, two-way ANOVA for multiple comparisons. e, Control for basal % of GFP+ over 4 days. After six rounds of re-growth of Sensor 1 and Sensor 2, the background signal of non-induced cells does not continue expanding over time, which validates them for use in animal models. Engineered bacteria were cultured in a selective media to measure NO detection, and the memory system was validated to ascertain that it accurately reflected, over multiple rounds of culturing (6 rounds, during 4 days) the initial input, n = 3 per group. Data are represented as mean ± SEM. f, Sensor validation in pigs. Experimental design: intestines were clamped to separate the different compartments (control vs. treated), and bacterial sensors were placed in the different compartments (left panel). All sensors registered significant activation in the presence of their respective inducers (300 uM H2O2, 30 mM TS, 3 mM TT, right panel). The bacteria were collected from the intestine after two hours of exposure to the analyte, and the percentage of GFP-positive cells was measured by flow cytometry. Lines represent the mean. The errors (SEM) are derived from flow cytometry experiments of three representative biological replicates, each of which involved n = 10,000 events. Here, we show data of three independent experiments (three animals [M, U, T, K] on different days, multiple compartments per animal). ****p < 0.0001, two-way ANOVA for multiple comparisons.
Extended Data Fig. 5 Design and manufacture of a bacteria-electronic pill casing compatible with ingestion.
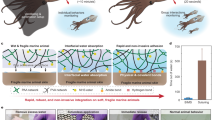
a, Size comparison of ingestible electronics and solid dosage forms with established safety rates. The safety of ingestible devices depends, in part, on ensuring that these devices will not damage, obstruct, or be retained in the GI tract. The current design was built to conform with the dimensions and form factors of solid dosage forms with known safety profiles and obstruction/retention rates (Procardia XL)55. Our system integration at the bacterial, electronics, and pill casing level allowed a significant reduction in size compared to a previously reported prototype (>9 mL to <1.4 mL)34. b, Pill casing manufacturing process. Casing blanks are 3D printed via selective laser sintering (Formlabs) with supports only on the top and bottom face to preserve the thin wall features. The top and bottom faces are then sanded to size. The filter membrane is cut to size with a punch and the double-sided adhesive film is laser cut with through holes aligned to the chambers. After pressing these outer layers together, the chambers are filled with bacterial suspensions from the inside and sealed off with a thin clear adhesive film to yield the fully sealed bacterial chamber/casing unibody. Scale bar = 5 mm.
Extended Data Fig. 6 Validation of semipermeable membranes and coatings for sealing and protection of on-board bacterial sensors.
a, Effect of membrane on analyte diffusion. The porous membranes, when placed in feces, did not interfere with detection of the target molecules. Fouling of the membrane by faecal matter may pose a problem, so we also screened several membrane materials, e.g., polyethersulfone (PES), polycarbonate (PC), and polyvinylidene fluoride (PVDF), to find which material allowed the highest diffusion of the analyte molecules across the membrane. Several porous membranes were tested in Franz Cells (inset on the right) in the presence of feces. All the membranes tested showed similar results, with a similar percentage of detection from the NO bacterial sensors after the analyte had passed through the membrane. The errors (SEM) are derived from flow cytometry experiments of three representative biological replicates, each of which involved n = 10,000 events. b–e, Manufacturing and performance of a pill casing protected from low pH ingress, compatible with ingestion. b, The assembled pill casing/chamber unibody can protect the sensor bacteria against low pH during stomach transit by inclusion of a film made of an enteric polymer (L100-55) attached via an adhesive layer (black). c, The enteric film hardens after exposure to simulated gastric fluid (SGF), but dissolves away after a brief exposure (< 1 hr) to neutral pH (PBS) allowing the bacteria to be exposed to the chemical environment of the small intestine. d, close-up view (red, dashed square in panel b) of enteric protected pill casings showing no membrane fouling after exposure to neutral pH (PBS). e, analysis of internal pH of fluid inside casing chambers by spotting contents onto pH paper. First two rows are control spots of the indicated fluids. Last two rows are spots from three chambers each from a protected or un-protected pill casing exposed to simulated gastric fluid (SGF) for 18 h. Bottom legend indicates corresponding pH of the resulting color change.
Extended Data Fig. 7 Enteric-protected pill casings preserve viability and luminescence of on-board bacterial sensors through simulated ingestion.
a, Un-protected or enteric-protected pill casings were loaded with constitutively luminescent bacterial cells and exposed to simulated intestinal fluid (SIF only, blue) or simulated ingestion with a 1-hour exposure to pH 1.2 simulated gastric fluid (SGF+SIF) at 37 C. b, At end of exposure the internal chamber contents were extracted and viability was measured through serial dilution and colony counting. As a control, an equivalent number of cells was directly resuspended in the exposure fluids (free cells) and pelleted between treatments. The viability of the common cell stock used to load the pill casings and for the free cell control was kept refrigerated during the exposures and its viability was also measured. Geometric mean and geometric 95% confidence intervals are plotted on top of individual replicate chambers. N = 8 (4 chambers x 2 pill casings), Multiple unpaired t-tests (two-tailed), *p = 0.0253 (unprotected), *p = 0.0195 (free cells), (ns) not significant. c, At end of exposure, the luminescence of the same chambers was also recorded (BioRad, ChemiDoc) from the inner side of the casings through the optically clear backing film. Total chamber luminescence was quantified (FIJI, Image J) and divided by the total chamber colony forming units (CFU) from panel b. The limit of detection (LOD) was set at 2.5x the standard deviation of the background signal divided by the largest viability value observed. Values below the LOD were set equal to the LOD and all values were normalized to set the LOD = 1. Geometric mean and geometric 95% confidence intervals are plotted on top of individual replicate chambers. N = 8 (4 chambers x 2 pill casings). d, Images used for luminescence quantification in panel c.
Extended Data Fig. 8 Kinetic response of the inflammatory biosensors with the luciferase readout.
a–b, E. coli Nissle biosensors were treated with their target analytes in LB (a) or in simulated intestinal fluid (b). The luminescence response was measured in a plate reader every 3 min for 10 h. The signal-to-noise ratio (SNR) was calculated by dividing the OD600-normalized luminescence values induced by the OD600-normalized luminescence values of uninduced samples. c, Response curve of the inflammatory biosensors with the luciferase readout. E. coli Nissle inflammatory sensor strains were treated with various concentrations of their target analytes; maximal luminescence values were measured thirty minutes to two hours post-exposure to the inducer and normalized to the optical density of the culture. Lines represent the mean. Error bars represent the SEM of three independent biological experiments. d, Nitric oxide (NO) detection and luciferase expression in anaerobiosis, replicating the gut environment. Luminescence values were measured aerobically in a plate reader after overnight aerobic or anaerobic growth and exposure to the inducer (DETA-NO 1mM) and normalized to the optical density of the culture. Lines represent the mean. Error bars denote the SEM for three independent biological replicates.
Extended Data Fig. 9 Electronic design and in vitro validation of the integrated bacterial-electronic pill.
a, Schematic of the miniaturized capsule PCB. The custom bioluminescence detector IC was fabricated in 65 nm CMOS technology2. The top PCB holds the custom-designed multi-channel and time-multiplexed bioluminescence detector, a 6.8 mm x 2.1 mm coin-cell battery, two 220 µF decoupling capacitors, and an 8-position female connector. The bottom PCB holds a microcontroller with an integrated transmitter, a crystal oscillator, an 8-position male connector, an antenna and other components for wireless data transmission. The components on the top and bottom PCB communicate through the two connectors. b–c, In vitro characterization of the device for miniaturized wireless sensing of NO and ROS with cell-based biosensors. Wireless signal over time from the NO (b) and ROS (c) sensors encapsulated in the device and immersed in bacterial growth media supplemented with 5 mM and 20 mM, respectively. Low-power CMOS-integrated photodiodes converted bioluminescence emitted from the bacterial sensor into a photocurrent, which was converted into quantifiable digital data and transmitted wirelessly to the external device. Lines represent the mean, and error bars denote the SEM for three independent replicates, conducted with one induced device (NO or ROS) and one uninduced device (Buffer); Rel. photocurrent, Relative Photocurrent.
Extended Data Fig. 10 In vivo validation of the integrated bacterial-electronic pill.
a,b, Individual replicates of TT sensing in the pig intestinal environment. The devices with the TT sensor were deposited in the intestinal compartments and TT (100 mM, blue) or buffer alone (black) were injected after temperature stabilization (~15 min, 37 °C). Readings from the device were wirelessly collected for 120 min following device deposition. Dark trace represents the mean of 3 replicates measurements (3 animals on different days, 2 devices per pig, in two different compartments) and pale traces indicate the individual current values for a given device (two channels measured per device). Photocurrents are provided relative to a one-time calibration value at t = 15 min. Non-induced sensor cells (black lines) decrease their luminescence output throughout the experiment (as shown in vitro, tested in simulated intestinal fluid, Extended Data Fig. 8b), while induced cells express higher levels of luciferase, compensating signal loss over time. For all the replicates, the response of the device placed in the compartment with TT was clearly distinguishable from that of the device in the compartment with the buffer control. b, For clarity, individual photocurrent values corresponding to different time points (15, 30, 60 and 120 min) for n = 3 or n = 5 samples for different set of conditions, including: TT sensor + TT, null sensor + TT, null sensor + buffer and TT sensor + buffer. Data are represented as mean ± SEM. c, Comparison of light detection between different chambers. E. coli Nissle strains containing a functional biosensor circuit for TT detection (TT sensor), and E coli Nissle without the gene for luciferase (null sensor) were loaded into the device. Devices were deposited in the intestine compartments and after temperature stabilization (~15 min), TT (100 mM, blue) or buffer alone (black) were injected. Compartmentalized intestines were kept inside the abdomen, at 37 °C, and wireless signals transmitted from inside the abdomen were collected for 120 min to analyze the kinetic response of the devices in the abdominal cavity of the pig. Photocurrents provided relative to a one-time calibration value at t = 15 min. Non-induced sensor cells (black lines) decrease their luminescence output throughout the experiment (as shown when tested in simulated intestinal fluid, Extended Data Fig. 8b), while induced cells express higher levels of luciferase compensating signal loss over time. The response of the device placed in the compartment with TT was clearly distinguishable from that of the device in the compartment with the buffer control. Null cells (light blue and grey traces) maintain constant values throughout. Error bars denote SEM for three experiments (3 animals on different days, 2 capsules per animal). d, Validation of the whole integrated device for miniaturized wireless biosensing in living pigs over time. The receiver operating characteristic (ROC) of the device sensing TT reached a sensitivity and specificity of 100% at 120 min.
Supplementary information
Supplementary Figures
Supplementary Fig. 1. Figure exemplifying the gating strategy. Statistics for each population are included at the bottom. This file also contains Supplementary Tables 2 and 3.
Supplementary Tables
This file contains Supplementary Table 1.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Inda-Webb, M.E., Jimenez, M., Liu, Q. et al. Sub-1.4 cm3 capsule for detecting labile inflammatory biomarkers in situ. Nature 620, 386–392 (2023). https://doi.org/10.1038/s41586-023-06369-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-023-06369-x
This article is cited by
-
End-to-end design of ingestible electronics
Nature Electronics (2024)
-
Engineered live bacteria as disease detection and diagnosis tools
Journal of Biological Engineering (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.