Abstract
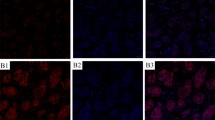
An increasing number of genes are being described in the context of non-syndromic male infertility. Linking the underlying genetic causes of non-syndromic male infertility with clinical data from patients is important to establish new genotype–phenotype correlations. This process can be facilitated by using universal nomenclature, but no standardized vocabulary is available in the field of non-syndromic male infertility. The International Male Infertility Genomics Consortium aimed at filling this gap, providing a standardized vocabulary containing nomenclature based on the Human Phenotype Ontology (HPO). The “HPO tree” was substantially revised compared with the previous version and is based on the clinical work-up of infertile men, including physical examination and hormonal assessment. Some causes of male infertility can already be suspected based on the patient’s clinical history, whereas in other instances, a testicular biopsy is needed for diagnosis. We assembled 49 HPO terms that are linked in a logical hierarchy and showed examples of morphological features of spermatozoa and testicular histology of infertile men with identified genetic diagnoses to describe the phenotypes. This work will help to record patients’ phenotypes systematically and facilitate communication between geneticists and andrologists. Collaboration across institutions will improve the identification of patients with the same phenotypes, which will promote the discovery of novel genetic causes for non-syndromic male infertility.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Claussnitzer, M. et al. A brief history of human disease genetics. Nature 577, 179–189 (2020).
Krausz, C. & Riera-Escamilla, A. Genetics of male infertility. Nat. Rev. Urol. 15, 369–384 (2018).
Oud, M. S. et al. A systematic review and standardized clinical validity assessment of male infertility genes. Hum. Reprod. 34, 932–941 (2019).
Agarwal, A., Mulgund, A., Hamada, A. & Chyatte, M. R. A unique view on male infertility around the globe. Reprod. Biol. Endocrinol. 13, 37 (2015).
Wyrwoll, M. J. et al. Genetic architecture of azoospermia-time to advance the standard of care. Eur. Urol. 83, 452–462 (2022).
Köhler, S. et al. The human phenotype ontology in 2017. Nucleic Acids Res. 45, D865–D876 (2017).
Köhler, S. et al. The human phenotype ontology in 2021. Nucleic Acids Res. 49, D1207–D1217 (2021).
Akawi, N. et al. Discovery of four recessive developmental disorders using probabilistic genotype and phenotype matching among 4,125 families. Nat. Genet. 47, 1363–1369 (2015).
Vissers, L. E. L. M. & Veltman, J. A. Standardized phenotyping enhances Mendelian disease gene identification. Nat. Genet. 47, 1222–1224 (2015).
Hamosh, A., Scott, A. F., Amberger, J., Valle, D. & McKusick, V. A. Online Mendelian inheritance in man (OMIM). Hum. Mutat. 15, 57–61 (2000).
Rath, A. et al. Representation of rare diseases in health information systems: the Orphanet approach to serve a wide range of end users. Hum. Mutat. 33, 803–808 (2012).
Köhler, S. et al. The human phenotype ontology project: linking molecular biology and disease through phenotype data. Nucleic Acids Res. 42, D966–D974 (2014).
Firth, H. V. et al. DECIPHER: database of chromosomal imbalance and phenotype in humans using Ensembl resources. Am. J. Hum. Genet. 84, 524–533 (2009).
Nieschlag, E., Behre, H. M. & Nieschlag, S. Andrology: male reproductive health and dysfunction (Springer, 2010).
McLachlan, R. I., Rajpert-De Meyts, E., Hoei-Hansen, C. E., de Kretser, D. M. & Skakkebaek, N. E. Histological evaluation of the human testis — approaches to optimizing the clinical value of the assessment: mini review. Hum. Reprod. 22, 2–16 (2007).
World Health Organization. WHO laboratory manual for examination and processing of human semen 6th edn (WHO, 2021).
Schlegel, P. N. et al. Diagnosis and treatment of infertility in men: AUA/ASRM guideline part II. J. Urol. 205, 44–51 (2021).
Robinson, P. N. et al. The human phenotype ontology: a tool for annotating and analyzing human hereditary disease. Am. J. Hum. Genet. 83, 610–615 (2008).
Pavan, S. et al. Clinical practice guidelines for rare diseases: the Orphanet database. PLoS One 12, e0170365 (2017).
Boehm, U. et al. European consensus statement on congenital hypogonadotropic hypogonadism — pathogenesis, diagnosis and treatment. Nat. Rev. Endocrinol. 11, 547–564 (2015).
Lenzi, A. et al. Epidemiology; diagnosis, and treatment of male hypogonadotropic hypogonadism. J. Endocrinol. Invest. 32, 934–938 (2009).
Chudnovsky, A. & Niederberger, C. S. Gonadotropin therapy for infertile men with hypogonadotropic hypogonadism. J. Androl. 28, 644–646 (2007).
Yabiku, R. S. et al. A search for disorders of sex development among infertile men. Sex. Dev. 12, 275–280 (2018).
Mohnach, L. et al. Nonsyndromic Disorders of Testicular Development Overview. GeneReviews [online] https://www.ncbi.nlm.nih.gov/books/NBK1547/ (updated 18 Aug 2022).
Young, J. Approach to the male patient with congenital hypogonadotropic hypogonadism. J. Clin. Endocrinol. Metab. 97, 707–718 (2012).
Young, J. et al. Clinical management of congenital hypogonadotropic hypogonadism. Endocr. Rev. 40, 669–710 (2019).
Salonia, A. et al. Sexual and Reproductive Health EAU Guidelines. Uroweb https://uroweb.org/guidelines/sexual-and-reproductive-health/chapter/male-infertility (2021).
Barratt, C. L. R. et al. The diagnosis of male infertility: an analysis of the evidence to support the development of global WHO guidance — challenges and future research opportunities. Hum. Reprod. Update 23, 660–680 (2017).
Björndahl, L. et al. Standards in semen examination: publishing reproducible and reliable data based on high-quality methodology. Hum. Reprod. 37, 2497–2502 (2022).
Oud, M. S. et al. Exome sequencing reveals novel causes as well as new candidate genes for human globozoospermia. Hum. Reprod. 35, 240–252 (2020).
Sironen, A., Shoemark, A., Patel, M., Loebinger, M. R. & Mitchison, H. M. Sperm defects in primary ciliary dyskinesia and related causes of male infertility. Cell. Mol. Life Sci. 77, 2029–2048 (2020).
Choy, J. T. & Amory, J. K. Nonsurgical management of oligozoospermia. J. Clin. Endocrinol. Metab. 105, e4194–e4207 (2020).
Vloeberghs, V. et al. How successful is TESE-ICSI in couples with non-obstructive azoospermia? Hum. Reprod. 30, 1790–1796 (2015).
Tournaye, H., Krausz, C. & Oates, R. D. Concepts in diagnosis and therapy for male reproductive impairment. Lancet Diabetes Endocrinol. 5, 554–564 (2017).
Krausz, C. Male infertility: pathogenesis and clinical diagnosis. Best. Pract. Res. Clin. Endocrinol. Metab. 25, 271–285 (2011).
Lotti, F. et al. The European Academy of Andrology (EAA) ultrasound study on healthy, fertile men: an overview on male genital tract ultrasound reference ranges. Andrology 10, 118–132 (2022).
Lotti, F. & Maggi, M. Ultrasound of the male genital tract in relation to male reproductive health. Hum. Reprod. Update 21, 56–83 (2015).
Schoor, R. A., Elhanbly, S., Niederberger, C. S. & Ross, L. S. The role of testicular biopsy in the modern management of male infertility. J. Urol. 167, 197–200 (2002).
Wosnitzer, M. S. & Goldstein, M. Obstructive azoospermia. Urol. Clin. North. Am. 41, 83–95 (2014).
Lotti, F. et al. The prevalence of midline prostatic cysts and the relationship between cyst size and semen parameters among infertile and fertile men. Hum. Reprod. 33, 2023–2034 (2018).
Schlegel, P. N. Causes of azoospermia and their management. Reprod. Fertil. Dev. 16, 561–572 (2004).
Anguiano, A. et al. Congenital bilateral absence of the vas deferens: a primarily genital form of cystic fibrosis. JAMA 267, 1794–1797 (1992).
Corona, G. et al. Sperm recovery and ICSI outcomes in men with non-obstructive azoospermia: a systematic review and meta-analysis. Hum. Reprod. Update 25, 733–757 (2019).
Bernie, A. M., Mata, D. A., Ramasamy, R. & Schlegel, P. N. Comparison of microdissection testicular sperm extraction, conventional testicular sperm extraction, and testicular sperm aspiration for nonobstructive azoospermia: a systematic review and meta-analysis. Fertil. Steril. 104, 1099–1103 (2015). e1–3.
Deruyver, Y., Vanderschueren, D. & Van der Aa, F. Outcome of microdissection TESE compared with conventional TESE in non-obstructive azoospermia: a systematic review. Andrology 2, 20–24 (2014).
Fietz, D. & Bergmann, M. in Endocrinology of the Testis and Male Reproduction (eds Simoni, M. & Huhtaniemi, I.) (Springer Cham, 2017).
Bergmann, M. & Kliesch, S. in Andrology (eds Nieschlag, E., Behre, H. M. & Nieschlag, S.) 155–167 (Springer Berlin Heidelberg, 2010).
Johnsen, S. G. Testicular biopsy score count — a method for registration of spermatogenesis in human testes: normal values and results in 335 hypogonadal males. Horm. Res. Paediatr. 1, 2–25 (1970).
O’Donnell, L. Mechanisms of spermiogenesis and spermiation and how they are disturbed. Spermatogenesis 4, e979623 (2014).
Zhengwei, Y., Wreford, N. G., Royce, P., de Kretser, D. M. & McLachlan, R. I. Stereological evaluation of human spermatogenesis after suppression by testosterone treatment: heterogeneous pattern of spermatogenic impairment. J. Clin. Endocrinol. Metab. 83, 1284–1291 (1998).
Aitken, R. J. & Lewis, S. E. M. DNA damage in testicular germ cells and spermatozoa. When and how is it induced? How should we measure it? What does it mean? Andrology. https://doi.org/10.1111/andr.13375 (2023).
Derijck, A. A. H. A. et al. Motile human normozoospermic and oligozoospermic semen samples show a difference in double-strand DNA break incidence. Hum. Reprod. 22, 2368–2376 (2007).
Sun, X. et al. The Catsper channel and its roles in male fertility: a systematic review. Reprod. Biol. Endocrinol. 15, 65 (2017).
Young, S. et al. Unexplained infertility is frequently caused by defective CatSper function preventing sperm from penetrating the egg coat. Preprint at medRxiv https://doi.org/10.1101/2023.03.23.23286813 (2023).
Bonte, D. et al. Assisted oocyte activation significantly increases fertilization and pregnancy outcome in patients with low and total failed fertilization after intracytoplasmic sperm injection: a 17-year retrospective study. Fertil. Steril. 112, 266–274 (2019).
Shefchek, K. A. et al. The Monarch Initiative in 2019: an integrative data and analytic platform connecting phenotypes to genotypes across species. Nucleic Acids Res. 48, D704–D715 (2020).
Köhler, S. et al. Expansion of the human phenotype ontology (HPO) knowledge base and resources. Nucleic Acids Res. 47, D1018–D1027 (2019).
Amer, M., Haggar, S. E., Moustafa, T., Abd El-Naser, T. & Zohdy, W. Testicular sperm extraction: impact of testicular histology on outcome, number of biopsies to be performed and optimal time for repetition. Hum. Reprod. 14, 3030–3034 (1999).
Tournaye, H. et al. Correlation between testicular histology and outcome after intracytoplasmic sperm injection using testicular spermatozoa. Hum. Reprod. 11, 127–132 (1996).
Acknowledgements
The authors thank C. Brenker for providing pictures of sperm phenotypes shown in Fig. 3 and C. Brennecka for language editing. This study was carried out within the framework of and supported by the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation) sponsored Clinical Research Unit ‘Male Germ Cells’ (CRU326, project number 329621271). C.K., F.T. and J.A.V. belong to Action CA20119 ‘ANDRONET’, which is supported by COST (European Cooperation in Science and Technology, https://www.cost.eu/).
Author information
Authors and Affiliations
Contributions
F.T., M.J.W. and G.W.v.d.H. researched data for the article. All authors contributed substantially to discussion of the content. F.T., M.J.W. and G.W.v.d.H. wrote the article. All authors reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Urology thanks Francesco Lotti, Sandro Esteves and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wyrwoll, M.J., van der Heijden, G.W., Krausz, C. et al. Improved phenotypic classification of male infertility to promote discovery of genetic causes. Nat Rev Urol 21, 91–101 (2024). https://doi.org/10.1038/s41585-023-00816-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41585-023-00816-0