Abstract
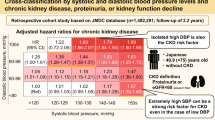
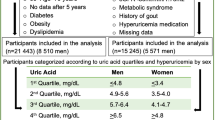
This study aimed to investigate the effect of hyperuricemia (HU) on the association of systolic blood pressure (SBP) with the prevalence of proteinuria and low estimated glomerular filtration rate (eGFR) in the general population. This cross-sectional study enrolled 24,728 Japanese individuals (11,137 men and 13,591 women) who underwent health checkups in 2010. The prevalence of proteinuria and low eGFR (< 60 mL/min/1.73 m2) among participants classified according to serum uric acid levels and SBP was compared. HU was defined as serum uric acid levels higher than the 75th percentile in male and female participants (> 7.2 and > 5.4 mg/dL, respectively). The odds ratio (OR) for proteinuria increased with elevated SBP. This trend was significantly evident in participants with HU. Moreover, there was an interactive effect of SBP and HU on the prevalence of proteinuria in the male (Pfor interaction = 0.04) and female (Pfor interaction = 0.04) participants. Next, we evaluated the OR for low eGFR (< 60 mL/min/1.73 m2) with and without proteinuria based on the presence of HU. The multivariate analysis revealed that the OR for low eGFR with proteinuria increased with elevated SBP, but that for low eGFR without proteinuria decreased. These trends of OR tended to be prevalent among those with HU. The association between SBP and the prevalence of proteinuria was more pronounced in participants with HU. However, the association between SBP and decreased renal function with and without proteinuria might be different regardless of HU.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Nishizawa H, Maeda N, Shimomura I. Impact of hyperuricemia on chronic kidney disease and atherosclerotic cardiovascular disease. Hypertens Res. 2022;45:635–40.
Iseki K, Oshiro S, Tozawa M, Iseki C, Ikemiya Y, Takishita S. Significance of hyperuricemia on the early detection of renal failure in a cohort of screened subjects. Hypertens Res. 2001;24:691–7.
Weiner DE, Tighiouart H, Elsayed EF, Griffith JL, Salem DN, Levey AS. Uric acid and incident kidney disease in the community. J Am Soc Nephrol. 2008;19:1204–11.
Takae K, Nagata M, Hata J, Mukai N, Hirakawa Y, Yoshida D, et al. Serum uric acid as a risk factor for chronic kidney disease in a Japanese community - The Hisayama study. Circ J. 2016;80:1857–62.
Suzuki K, Konta T, Kudo K, Sato H, Ikeda A, Ichikawa K, et al. The association between serum uric acid and renal damage in a community-based population: the Takahata study. Clin Exp Nephrol. 2013;17:541–8.
Chang HY, Lee PH, Lei CC, Tung CW, Hsu YC, Huang TJ, et al. Hyperuricemia is an independent risk factor for new onset micro-albuminuria in a middle-aged and elderly population: A prospective cohort study in Taiwan. PLoS One. 2013;8:e61450.
Obermayr RP, Temml C, Gutjahr G, Knechtelsdorfer M, Oberbauer R, Klauser-Braun R. Elevated uric acid increases the risk for kidney disease. J Am Soc Nephrol. 2008;19:2407–13.
Momoki K, Kataoka H, Moriyama T, Mochizuki T, Nitta K. Hyperuricemia as a predictive marker for progression of nephrosclerosis: Clinical assessment of prognostic factors in biopsy-proven Arterial/Arteriolar nephrosclerosis. J Atheroscler Thromb. 2017;24:630–42.
Kohagura K, Kochi M, Miyagi T, Kinjyo T, Maehara Y, Nagahama K, et al. An association between uric acid levels and renal arteriolopathy in chronic kidney disease: A biopsy-based study. Hypertens Res. 2013;36:43–9.
Hill GS, Heudes D, Jacquot C, Gauthier E, Bariéty J. Morphometric evidence for impairment of renal autoregulation in advanced essential hypertension. Kidney Int. 2006;69:823–31.
Remuzzi G, Bertani T. Pathophysiology of progressive nephropathies. N Engl J Med. 1998;339:1448–56.
Kohagura K, Kochi M, Zamami R, Ohya Y. Understanding the Complex Interaction Between Uric Acid and Hypertension. Am J Hypertens. 2020;33:822–4.
Tada K, Maeda T, Takahashi K, Ito K, Yasuno T, Funakoshi S, et al. Association between serum uric acid and new onset and progression of chronic kidney disease in a Japanese general population: Iki epidemiological study of atherosclerosis and chronic kidney disease. Clin Exp Nephrol. 2021;25:751–9.
Kohagura K, Kochi M, Miyagi T, Zamami R, Nagahama K, Yonemoto K, et al. Augmented association between blood pressure and proteinuria in hyperuricemic patients with non-nephrotic chronic kidney disease. 2017; Am J Hypertens. https://doi.org/10.1093/ajh/hpx166.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Kashiwagi A, Kasuga M, Araki E, Oka Y, Hanafusa T, Ito H, et al. International clinical harmonization of glycated hemoglobin in Japan: From Japan Diabetes Society to National Glycohemoglobin Standardization Program values. J Diabetes Investig. 2012;3:39–40.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y. et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res.2019;42:1235–481.
Inker LA, Astor BC, Fox CH, Isakova T, Lash JP, Peralta CA, et al. KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis. 2014;63:713–35.
Woodward M. Epidemiology: Study Design and Data Analysis, Second Edition, Chapman & Hall/CRC, 2005.
Mazzali M, Kanellis J, Han L, Feng L, Xia YY, Chen Q, et al. Hyperuricemia induces a primary renal arteriolopathy in rats by a blood pressure-independent mechanism. Am J Physiol Renal Physiol. 2002;282:F991–7.
Kang DH, Park SK, Lee IK, Johnson RJ. Uric acid-induced C-reactive protein expression: Implication on cell proliferation and nitric oxide production of human vascular cells. J Am Soc Nephrol. 2005;16:3553–62.
Tsioufis C, Dimitriadis K, Antoniadis D, Stefanadis C, Kallikazaros I. Inter-relationships of microalbuminuria with the other surrogates of the atherosclerotic cardiovascular disease in hypertensive subjects. Am J Hypertens. 2004;17:470–6.
Sánchez-Lozada LG, Tapia E, Avila-Casado C, Soto V, Franco M, Santamaría J, et al. Mild hyperuricemia induces glomerular hypertension in normal rats. Am J Physiol Renal Physiol. 2002;283:F1105–1110.
Matsukuma Y, Masutani K, Tanaka S, Tsuchimoto A, Haruyama N, Okabe Y, et al. Association between serum uric acid level and renal arteriolar hyalinization in individuals without chronic kidney disease. Atherosclerosis. 2017;266:121–7.
Hill GS, Heudes D, Bariéty J. Morphometric study of arterioles and glomeruli in the aging kidney suggests focal loss of autoregulation. Kidney Int. 2003;63:1027–36.
Uedono H, Tsuda A, Ishimura E, Yasumoto M, Ichii M, Ochi A, et al. Relationship between serum uric acid levels and intrarenal hemodynamic parameters. Kidney Blood Press Res. 2015;40:315–22.
Zamami R, Kohagura K, Miyagi T, Kinjyo T, Shiota K, Ohya Y. Modification of the impact of hypertension on proteinuria by renal arteriolar hyalinosis in nonnephrotic chronic kidney disease. J Hypertens. 2016;34:2274–9.
Kohagura K, Kochi M, Miyagi T, Zamami R, Nagahama K, Yonemoto K, et al. Augmented Association Between Blood Pressure and Proteinuria in Hyperuricemic Patients With Nonnephrotic Chronic Kidney Disease. Am J Hypertens. 2018;31:480–5.
Rule AD, Amer H, Cornell LD, Taler SJ, Cosio FG, Kremers WK, et al. The association between age and nephrosclerosis on renal biopsy among healthy adults. Ann Intern Med. 2010;152:561–7.
Glassock RJ, Denic A, Rule. AD. The physiology and pathophysiology of the kidneys in aging. In: Brenner & Rector’s THE KIDNEY. 11 Ed. edited by Alan S. L. Yu, Glenn M. Chertow, Philip A. Marsden, Valerie Luyckx, Maarten W. Taal, Karl Skorecki Philadelphia, Elsevier, 2020, 710–30
Freedman BI, Iskandar SS, Appel RG. The link between hypertension and nephrosclerosis. Am J Kidney Dis. 1995;25:207–21.
Messerli FH, Frohlich ED, Dreslinski GR, Suarez DH, Aristimuno GG. Serum uric acid in essential hypertension: An indicator of renal vascular involvement. Ann Intern Med. 1980;93:817–21.
Badve SV, Pascoe EM, Tiku A, Boudville N, Brown FG, Cass A, et al. Effects of allopurinol on the progression of chronic kidney disease. N Engl J Med. 2020;382:2504–13.
Doria A, Galecki AT, Spino C, Pop-Busui R, Cherney DZ, Lingvay I, et al. Serum urate lowering with allopurinol and kidney function in type 1 diabetes. N Engl J Med. 2020;382:2493–503.
Wright JT, Bakris G, Greene T, Agodoa LY, Appel LJ, Charleston J, et al. Effect of blood pressure lowering and antihypertensive drug class on progression of hypertensive kidney disease: results from the AASK trial. JAMA. 2002;288:2421–31.
Chen Q, Wang Z, Zhou J, Chen Z, Li Y, Li S, et al. Effect of urate-lowering therapy on cardiovascular and kidney outcomes: A systematic review and meta-analysis. Clin J Am Soc Nephrol. 2020;15:1576–86.
Tanaka H, Shiohira Y, Uezu Y, Higa A, Iseki K. Metabolic syndrome and chronic kidney disease in Okinawa, Japan. Kidney Int. 2006;69:369–74.
Feig DI, Soletsky B, Johnson RJ. Effect of allopurinol on blood pressure of adolescents with newly diagnosed essential hypertension: a randomized trial. JAMA. 2008;300:924–32.
Quiñones Galvan A, Natali A, Baldi S, Frascerra S, Sanna G, Ciociaro D, et al. Effect of insulin on uric acid excretion in humans. Am J Physiol. 1995;268:E1–5.
Acknowledgements
The authors are grateful to Dr. Kinjyo K, the chairman of the Okinawa General Health Association, Haebaru, Japan, for providing the data for analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Kohagura received personal fees for lecture from Teijin Pharma, Fuji Pharma, Sanwa Kagaku, Pfizer, and Mochida Pharma as well as obtained research funding from Teijin Pharma, outside the submitted work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kochi, M., Kohagura, K., Oshiro, N. et al. Association of blood pressure and hyperuricemia with proteinuria and reduced renal function in the general population. Hypertens Res 46, 1662–1672 (2023). https://doi.org/10.1038/s41440-023-01250-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-023-01250-w
Keywords
This article is cited by
-
Hyperuricemia: An Intriguing Connection to Metabolic Syndrome, Diabetes, Kidney Disease, and Hypertension
Current Hypertension Reports (2024)
-
Hyperuricemia: the third key player for nephrosclerosis with ischemia
Hypertension Research (2023)
-
Sympathetic nervous activation and hypertension
Hypertension Research (2023)