Abstract
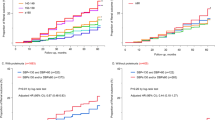
Little is known about the relationship between blood pressure (BP) and incident cardiovascular disease (CVD) in people with proteinuria and a preserved estimated glomerular filtration rate (eGFR). This study sought to investigate the association of BP with CVD risk in adults with proteinuria and preserved eGFR. We studied 188,837 individuals with proteinuria and preserved eGFR ≥60 mL/min/1.73 m2. We categorized individuals who were not taking BP-lowering medications into four groups based on the 2017 American College of Cardiology/American Heart Association BP guideline and categorized those who were taking BP-lowering medications using the same BP ranges. The primary outcome was a composite CVD endpoint that included myocardial infarction, angina pectoris, stroke, and heart failure. Over a mean follow-up of 1,050 days, 7,039 CVD events were identified. Compared with normal BP, stage 1 hypertension (hazard ratio [HR]: 1.30, 95% confidence interval [95% CI]: 1.21–1.40) and stage 2 hypertension (HR: 2.17, 95% CI: 2.01–2.34) were associated with an increased risk for CVD events among medication-naïve individuals. Only stage 2 hypertension range (HR: 1.19, 95% CI: 1.02–1.38) was associated with an increased CVD event risk among people taking BP-lowering medications. Restricted cubic spline analysis showed that the risk of CVD events increased monotonically with BP at an SBP/DBP > 120/80 mmHg among medication-naïve individuals, but risk increased only at an SBP/DBP > 140/90 mmHg among individuals taking BP-lowering medications. In conclusion, among people with proteinuria and preserved eGFR, stage 1 and stage 2 hypertension were associated with a greater risk of CVD among medication-naïve individuals, whereas only stage 2 hypertension was associated with an increased CVD risk among those taking BP-lowering medications.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
This database is available for anyone who purchases it from JMDC Inc. (https://www.jmdc.co.jp/en/).
References
Lawes CM, Vander Hoorn S, Rodgers A. International Society of Hypertension. Global burden of blood-pressure-related disease, 2001. Lancet. 2008;3:1513–8.
Virani SS, Alonso A, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP, et al. Heart disease and stroke statistics-2020 update: a report from the American Heart Association. Circulation. 2020;3:e139–e596.
Oparil S, Acelajado MC, Bakris GL, Berlowitz DR, Cífková R, Dominiczak AF, et al. Hypertension. Nat Rev Dis Prim. 2018;22:18014.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2018;23:e484–e594.
Kovesdy CP, Trivedi BK, Kalantar-Zadeh K, Anderson JE. Association of low blood pressure with increased mortality in patients with moderate to severe chronic kidney disease. Nephrol Dial Transpl. 2006;21:1257–62.
Weiner DE, Tighiouart H, Levey AS, Elsayed E, Griffith JL, Salem DN, et al. Lowest systolic blood pressure is associated with stroke in stages 3 to 4 chronic kidney disease. J Am Soc Nephrol. 2007;18:960–6.
Chiang HP, Lee JJ, Chiu YW, Tsai JC, Hung CC, Hwang SJ, et al. Systolic blood pressure and outcomes in stage 3-4 chronic kidney disease patients: evidence from a Taiwanese cohort. Am J Hypertens. 2014;27:1396–407.
Yamamoto T, Nakayama M, Miyazaki M, Matsushima M, Sato T, Taguma Y, et al. Relationship between low blood pressure and renal/cardiovascular outcomes in Japanese patients with chronic kidney disease under nephrologist care: the Gonryo study. Clin Exp Nephrol. 2015;19:878–86.
Sarnak MJ, Greene T, Wang X, Beck G, Kusek JW, Collins AJ, et al. The effect of a lower target blood pressure on the progression of kidney disease: long-term follow-up of the modification of diet in renal disease study. Ann Intern Med. 2005;1:342–51.
Appel LJ, Wright JT Jr, Greene T, Agodoa LY, Astor BC, Bakris GL, et al. Intensive blood-pressure control in hypertensive chronic kidney disease. N Engl J Med. 2010;2:918–29.
Ku E, Gassman J, Appel LJ, Smogorzewski M, Sarnak MJ, Glidden DV, et al. BP control and long-term risk of ESRD and mortality. J Am Soc Nephrol. 2017;28:671–7.
Cheung AK, Rahman M, Reboussin DM, Craven TE, Greene T, Kimmel PL, et al. Effects of intensive BP control in CKD. J Am Soc Nephrol. 2017;28:2812–23.
Aggarwal R, Petrie B, Bala W, Chiu N. Mortality outcomes with intensive blood pressure targets in chronic kidney disease patients. Hypertension. 2019;73:1275–82.
Fukui A, Kaneko H, Okada A, Yano Y, Itoh H, Matsuoka S, et al. Semiquantitative assessed proteinuria and risk of heart failure: analysis of a nationwide epidemiological database. Nephrol Dial Transpl. 2022;22:1691–9.
Currie G, Delles C. Proteinuria and its relation to cardiovascular disease. Int J Nephrol Renovasc Dis. 2013;21:13–24.
Kaneko H, Yano Y, Itoh H, Morita K, Kiriyama H, Kamon T, et al. Association of blood pressure classification using the 2017 American College of Cardiology/American Heart Association blood pressure guideline with risk of heart failure and atrial fibrillation. Circulation. 2021;8:2244–53.
Kaneko H, Itoh H, Kamon T, Fujiu K, Morita K, Michihata N, et al. Association of cardiovascular health metrics with subsequent cardiovascular disease in young adults. J Am Coll Cardiol. 2020;17:2414–6.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Suzuki Y, Kaneko H, Okada A, Itoh H, Morita K, Fujiu K, et al. Change in cardiovascular health metrics and risk for proteinuria development: analysis of a nationwide population-based database. Am J Nephrol. 2022;53:240–8.
Kaneko H, Morita H, Komuro I. Beautiful harmony of the Japanese precious healthcare legacies for the new imperial era. Circ J. 2020;25:371–3.
Itoh H, Kaneko H, Okada A, Yano Y, Morita K, Seki H, et al. Fasting plasma glucose and incident colorectal cancer: analysis of a nationwide epidemiological database. J Clin Endocrinol Metab. 2021;25:dgab466.
Shiozawa M, Kaneko H, Itoh H, Morita K, Okada A, Matsuoka S, et al. Association of Body Mass Index with ischemic and hemorrhagic stroke. Nutrients. 2021;9:2343.
Kaneko H, Itoh H, Yotsumoto H, Kiriyama H, Kamon T, Fujiu K, et al. Association of isolated diastolic hypertension based on the cutoff value in the 2017 American College of Cardiology/American Heart Association blood pressure guidelines with subsequent cardiovascular events in the general population. J Am Heart Assoc. 2020;20:e017963.
Matsuoka S, Kaneko H, Yano Y, Itoh H, Fukui A, Morita K, et al. Association between blood pressure classification using the 2017 ACC/AHA blood pressure guideline and retinal atherosclerosis. Am J Hypertens. 2021;27:1049–56.
Strazzullo P, D’Elia L, Kandala NB, Cappuccio FP. Salt intake, stroke, and cardiovascular disease: meta-analysis of prospective studies. BMJ. 2009;24:b4567.
Rozanski A, Blumenthal JA, Kaplan J. Impact of psychological factors on the pathogenesis of cardiovascular disease and implications for therapy. Circulation. 1999;99:2192–217.
Saito I, Yamagishi K, Kokubo Y, Yatsuya H, Iso H, Sawada N, et al. Association between mortality and incidence rates of coronary heart disease and stroke: the Japan Public Health Center-based prospective (JPHC) study. Int J Cardiol. 2016;1:281–6.
Miura K, Nakagawa H, Ohashi Y, Harada A, Taguri M, Kushiro T, et al. Four blood pressure indexes and the risk of stroke and myocardial infarction in Japanese men and women: a meta-analysis of 16 cohort studies. Circulation. 2009;14:1892–8.
Yamana H, Moriwaki M, Horiguchi H, Kodan M, Fushimi K, Yasunaga H. Validity of diagnoses, procedures, and laboratory data in Japanese administrative data. J Epidemiol. 2017;27:476–82.
Fujihara K, Yamada-Harada M, Matsubayashi Y, Kitazawa M, Yamamoto M, Yaguchi Y, et al. Accuracy of Japanese claims data in identifying diabetes-related complications. Pharmacoepidemiol Drug Saf. 2021;30:594–601.
Kario K, Chen CH, Park S, Park CG, Hoshide S, Cheng HM, et al. Consensus document on improving hypertension management in Asian patients, taking into account Asian characteristics. Hypertension. 2018;71:375–82.
Perkovic V, Huxley R, Wu Y, Prabhakaran D, MacMahon S. The burden of blood pressure-related disease: a neglected priority for global health. Hypertension. 2007;50:991–7.
Funding
This work was supported by grants from the Ministry of Health, Labour and Welfare, Japan (19AA2007 and H30-Policy- Designated-004) and the Ministry of Education, Culture, Sports, Sci-ence and Technology, Japan (17H04141). The funding sources had no role in the design or implementation of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Research funding and scholarship funds (HK and KF) were received from Medtronic Japan Co., Ltd., Boston Scientific Japan Co., Ltd., Biotronik Japan, Simplex QUANTUM Co., Ltd., and Fukuda Denshi, Central Tokyo Co., Ltd. The remaining authors declare no competing interests.
Ethics approval
IRB information: The Clinical Research Review Board of the University of Tokyo [2018–10862] approved this study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Suzuki, Y., Kaneko, H., Yano, Y. et al. The association of BP with cardiovascular outcomes in patients with dipstick proteinuria and preserved kidney function. Hypertens Res 46, 856–867 (2023). https://doi.org/10.1038/s41440-022-01146-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-01146-1
Keywords
This article is cited by
-
Which blood pressure threshold indicates a therapeutic benefit for patients with chronic kidney disease?
Hypertension Research (2023)
-
The importance of lifestyle modification for hypertension in Asia
Hypertension Research (2023)