Abstract
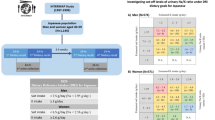
The association between the urinary sodium (Na)/potassium (K) ratio and hypertension is well recognized. We investigated whether the urinary Na/K ratio might be associated with hypertension in community-dwelling older adults and whether the association was influenced by habitual dietary patterns. We enrolled a total of 684 older adults (mean age, 76.8 years) and conducted health examinations at Kusatsu, Japan, in 2021. The urinary Na/K ratio was found to be independently associated with systolic blood pressure (SBP) (p < 0.0001), years of education (p = 0.0027), number of cohabitants (p = 0.0175), estimated glomerular filtrate rate (eGFR) (p = 0.0244), and Geriatric Depression Scale short-version (GDS15) score (p = 0.0366). In addition, an unsupervised hierarchical clustering analysis revealed a spectrum of habitual dietary patterns for higher and lower values of the urinary Na/K ratio. The decision tree indicated that the urinary Na/K ratio was associated with the history of milk consumption. A positive history of daily milk consumption predicted a mean urinary Na/K ratio of 2.8, and a negative history of daily milk consumption predicted a mean urinary Na/K ratio of 3.3. Furthermore, the frequency of fruit and vegetable consumption also predicted the urinary Na/K ratio. The relationship between the urinary Na/K ratio and hypertension was influenced by the frequency of consumption of milk, fruits, and vegetables in the subjects. This finding might be due to the influence of education and/or depression. The results suggested the importance of nutritional education in the development of hypertension.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Mente A, O’Donnell MJ, Rangarajan S, McQueen MJ, Poirier P, Wielgosz A, et al. PURE Investigators. Association of urinary sodium and potassium excretion with blood pressure. N Engl J Med. 2014;371:601–11.
Jackson SL, Cogswell ME, Zhao L, Terry AL, Wang CY, Wright J, et al. Association between urinary sodium and potassium excretion and blood pressure among adults in the United States: national health and nutrition examination survey, 2014. Circulation 2018;137:237–46.
Ma Y, He FJ, Sun Q, Yuan C, Kieneker LM, Curhan GC, et al. 24-Hour Urinary Sodium and Potassium Excretion and Cardiovascular Risk. N Engl J Med. 2022;386:252–63.
Oliveros E, Patel H, Kyung S, Fugar S, Goldberg A, Madan N, et al. Hypertension in older adults: Assessment, management, and challenges. Clin Cardiol. 2020;43:99–107.
Zemel MB, Sowers JR. Salt sensitivity and systemic hypertension in the elderly. Am J Cardiol. 1988;61:7H–12H.
Appel LJ, Moore TJ, Obarzanek E, Vollmer WM, Svetkey LP, Sacks FM, et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med. 1997;336:1117–24.
Morrissey E, Giltinan M, Kehoe L, Nugent AP, McNulty BA, Flynn A, et al. Sodium and Potassium Intakes and Their Ratio in Adults (18-90 y): Findings from the Irish National Adult Nutrition Survey. Nutrients 2020;12:938.
Mirmiran P, Gaeini Z, Bahadoran Z, Ghasemi A, Norouzirad R, Tohidi M, et al. Urinary sodium-to-potassium ratio: a simple and useful indicator of diet quality in population-based studies. Eur J Med Res. 2021;26:3.
Iwahori T, Ueshima H, Ohgami N, Yamashita H, Miyagawa N, Kondo K, et al. Effectiveness of a self-monitoring device for urinary sodium-to-potassium ratio on dietary improvement in freeliving adults: a randomized controlled trial. J Epidemiol. 2018;28:41–7.
Kogure M, Hirata T, Nakaya N, Tsuchiya N, Nakamura T, Narita A, et al. Multiple measurements of the urinary sodium-to-potassium ratio strongly related home hypertension: TMM Cohort Study. Hypertens Res. 2020;43:62–71.
Kogure M, Nakaya N, Hirata T, Tsuchiya N, Nakamura T, Narita A, et al. Sodium/potassium ratio change was associated with blood pressure change: possibility of population approach for sodium/potassium ratio reduction in health checkup. Hypertens Res. 2021;44:225–31.
Iwahori T, Miura K, Ueshima H. Time to Consider Use of the Sodium-to-Potassium Ratio for Practical Sodium Reduction and Potassium Increase. Nutrients. 2017;9:700.
Mendes J, Padrão P, Moreira P, Santos A, Borges N, Afonso C, et al. Handgrip strength and its association with hydration status and urinary sodium-to-potassium ratio in older adults. J Am Coll Nutr. 2020;39:192–9.
Li CL, Wang HJ, Si QJ, Zhou J, Li KL, Ding Y. Association between urinary sodium excretion and coronary heart disease in hospitalized elderly patients in China. J Int Med Res. 2018;46:3078–85.
Gonçalves C, Abreu S. Sodium and Potassium Intake and Cardiovascular Disease in Older People: A Systematic Review. Nutrients. 2020;12:3447.
Hsiao PY, Mitchell DC, Coffman DL, Craig Wood G, Hartman TJ, Still C, et al. Dietary patterns and relationship to obesity-related health outcomes and mortality in adults 75 years of age or greater. J Nutr Health Aging. 2013;17:566–72.
Kourlaba G, Polychronopoulos E, Zampelas A, Lionis C, Panagiotakos DB. Development of a diet index for older adults and its relation to cardiovascular disease risk factors: the Elderly Dietary Index. J Am Diet Assoc. 2009;109:1022–30.
Shinkai S, Yoshida H, Taniguchi Y, Murayama H, Nishi M, Amano H, et al. Public health approach to preventing frailty in the community and its effect on healthy aging in Japan. Geriatr Gerontol Int. 2016;16:87–97.
Yokoyama Y, Kitamura A, Nishi M, Seino S, Taniguchi Y, Amano H, et al. Frequency of Balanced-Meal Consumption and Frailty in Community-Dwelling Older Japanese: A Cross-Sectional Study. J Epidemiol. 2018;29:370–76.
Ogawa K, Fujiwara Y, Yoshida H, Nishi M, Fukaya T, Kim M, et al. The validity of the “Kihon Check-list” as an index of frailty and its biomarkers and inflammatory markers in elderly people. Nippon Ronen Igakkai Zasshi. 2011;48:545–52. (Japanese)
Burke WJ, Roccaforte WH, Wengel SP. The short form of the Geriatric Depression Scale: a comparison with the 30‐item form. J Geriatr Psychiatry Neurol. 1991;4:173–8.
Awata S, Bech P, Koizumi Y, Seki T, Kuriyama S, Hozawa A, et al. Validity and utility of the Japanese version of the WHO-Five Well-Being Index in the context of detecting suicidal ideation in elderly community residents. Int Psychogeriatr. 2007;19:77–88.
Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B. Screening for Undernutrition in Geriatric Practice: Developing the Short-Form Mini Nutritional. Assess (MNA-SF) J Geront. 2001;56A:M366–77.
Kumagai S, Watanabe S, Shibata H, Amano H, Fujiwara Y, Shinkai S, et al. Effects of dietary variety on declines in high-level functional capacity in elderly people living in a community. Nihon Koshu Eisei Zasshi. 2003;50:1117–24. (Japanese)
Adrogué HJ, Madias NE. Sodium and potassium in the pathogenesis of hypertension. N Engl J Med. 2007;356:1966–78.
Whelton PK, He J, Cutler JA. Effects of oral potassium on blood pressure. Meta-Anal randomized controlled Clinical trials. JAMA. 1997;277:1624–32.
Binia A, Jaeger J, Hu Y. Daily potassium intake and sodium-to-potassium ratio in the reduction of blood pressure: a meta-analysis of randomized controlled trials. J Hypertens. 2015;33:1509–20.
Cook NR, Obarzanek E, Cutler JA. Joint effects of sodium and potassium intake on subsequent cardiovascular disease: the Trials of Hypertension Prevention follow-up study. Arch Intern Med. 2009;169:32–40.
Segawa H, Higashi A, Masuda I, Yoshii K, Iwahori T, Ueshima H. Urinary sodium/potassium ratio as a screening tool for hyperaldosteronism in men with hypertension. Hypertens Res. 2021;44:1129–37.
Eudy RJ, Sahasrabudhe V, Sweeney K, Tugnait M, King-Ahmad A, Near K, et al. The use of plasma aldosterone and urinary sodium to potassium ratio as translatable quantitative biomarkers of mineralocorticoid receptor antagonism. J Transl Med. 2011;9:180.
Okuyama Y, Uchida HA, Iwahori T, Segawa H, Kato A, Takeuchi H, et al. The relationship between repeated measurement of casual and 24-h urinary sodium-to-potassium ratio in patients with chronic kidney disease. J Hum Hypertens. 2019;33:286–97.
Hattori H, Hirata A, Kubo S, Nishida Y, Nozawa M, Kawamura K, et al. Estimated 24 h Urinary Sodium-to-Potassium Ratio Is Related to Renal Function Decline: A 6-Year Cohort Study of Japanese Urban Residents. Int J Environ Res Public Health. 2020;17:5811.
Alencar de Pinho N, Kaboré J, Laville M, Metzger M, Lange C, Jacquelinet C, et al. CKD-REIN Study Group. Urinary Sodium-to-Potassium Ratio and Blood Pressure in CKD. Kidney Int Rep. 2020;5:1240–50.
Kimura Y, Wada T, Okumiya K, Ishimoto Y, Fukutomi E, Kasahara Y, et al. Eating alone among community-dwelling Japanese elderly: association with depression and food diversity. J Nutr Health Aging. 2012;16:728–31.
Wu EL, Chien IC, Lin CH, Chou YJ, Chou P. Increased risk of hypertension in patients with major depressive disorder: a population-based study. J Psychosom Res. 2012;73:169–74.
Alexander RW, Gill JR Jr, Yamabe H, Lovenberg W, Keiser HR. Effects of dietary sodium and of acute saline infusion on the interrelationship between dopamine excretion and adrenergic activity in man. J Clin Investig. 1974;54:194–200.
Grace AA. Dysregulation of the dopamine system in the pathophysiology of schizophrenia and depression. Nat Rev Neurosci. 2016;17:524–32.
Utsugi MT, Ohkubo T, Kikuya M, Kurimoto A, Sato RI, Suzuki K, et al. Fruit and vegetable consumption and the risk of hypertension determined by self measurement of blood pressure at home: the Ohasama study. Hypertens Res. 2008;31:1435–43.
Groziak SM, Miller GD. Natural bioactive substances in milk and colostrum: effects on the arterial blood pressure system. Br J Nutr. 2000;84:S119–125.
Moore TJ, Alsabeeh N, Apovian CM, Murphy MC, Coffman GA, Cullum-Dugan D, et al. Weight, blood pressure, and dietary benefits after 12 months of a Web-based Nutrition Education Program (DASH for health): longitudinal observational study. J Med Internet Res. 2008;10:e52.
Henchion M, Moloney AP, Hyland J, Zimmermann J, McCarthy S. Review: Trends for meat, milk and egg consumption for the next decades and the role played by livestock systems in the global production of proteins. Animal. 2021;15 S1:100287. https://doi.org/10.1016/j.animal.2021.100287.
Bennett G, Bardon LA, Gibney ER. A Comparison of Dietary Patterns and Factors Influencing Food Choice among Ethnic Groups Living in One Locality: A Systematic Review. Nutrients. 2022;14:941.
Acknowledgements
We would like to express our sincere appreciation to Toshiki Hata, Tomoya Sagara, and all other related parties in the Kusatsu Study who cooperated in this study.
Funding
All sources of support for this study were self-funded (Health Aging Innovation Center in Tokyo Metropolitan Geriatric Hospital and Institute of Gerontology).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamanaka, N., Itabashi, M., Fujiwara, Y. et al. Relationship between the urinary Na/K ratio, diet and hypertension among community-dwelling older adults. Hypertens Res 46, 556–564 (2023). https://doi.org/10.1038/s41440-022-01135-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-01135-4
Keywords
This article is cited by
-
2023 update and perspectives
Hypertension Research (2024)
-
Lifetime home BP-centered approach is the core from onset to aggravation of hypertension
Hypertension Research (2023)